Abstract
Multiple psychiatric disorders are characterized by a failure to suppress default-mode network (DMN) activity during tasks and by weaker anti-correlations between DMN and other brain networks at rest. However, the cellular and molecular mechanisms underlying this phenomenon are poorly understood. At the cellular level, neuronal activity is regulated by multiple neurochemical processes including cycling of glutamate and GABA, the major excitatory and inhibitory neurotransmitters in brain. By combining functional MRI and magnetic resonance spectroscopy techniques, it has been shown that the neurotransmitter concentrations in DMN modulate not only functional activity during cognitive tasks, but also the functional connectivity between DMN and other brain networks such as frontoparietal executive control network (CN) at rest in the healthy brain. In the current study, we extend previous research to first episode psychosis (FEP) patients and their relatives. We detected higher glutamate (Glu) levels in the medial prefrontal cortex (MPFC) in FEP compared to healthy controls without a significant difference in GABA. We also observed a significantly lower functional anti-correlated connectivity between critical nodes within the DMN (MPFC) and CN (DLPFC) in FEP. Furthermore, the relationship between MPFC Glu and GABA concentrations and the functional anti-correlation that is seen in healthy people was absent in FEP patients. These findings imply that both the DMN Glu level and the interaction between DMN and CN are affected by the illness, as is the association between neurochemistry and functional connectivity. A better understanding of this observation could provide opportunities for developing novel treatment strategies for psychosis.
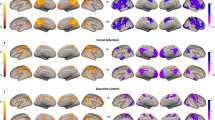
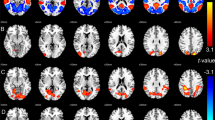
Similar content being viewed by others
Introduction
Psychotic disorders such as schizophrenia (SZ) and bipolar disorder with psychotic features (BD) are characterized by hallucinations, disorganized thought, impaired emotional and motivational processes, and cognitive dysfunction. Researchers have sought to identify the pathophysiology of these disorders for decades without great success. The development of novel neuroimaging techniques holds promise for the identification of biomarkers for psychosis based on brain function, structure, and metabolites. One promising direction of research has to do with the “disconnection syndrome” observed in psychotic disorders and characterized by abnormal within-network connectivity and between-network anticorrelation [1]. The presence of a default mode network (DMN), including the medial prefrontal cortex (MPFC), posterior cingulate cortex (PCC), and bilateral inferior parietal lobules (IPL), is one of the most reliable observations from neuroimaging studies. The DMN is active during internally oriented processing and is downregulated during task-related processing [2]. Failure to suppress DMN activity during tasks in various psychiatric disorders has been observed [3], as well as a reduced anti-correlation between DMN and task-related brain networks at rest in schizophrenia [4] and an opposite trend in major depressive disorder [5]. However, the cellular and molecular mechanisms underlying this phenomenon are poorly understood.
At the cellular level, neuronal activity is regulated by multiple neurochemical processes including cycling of glutamate (Glu) and GABA, the major excitatory and inhibitory neurotransmitters in the central nervous system. There has been considerable interest in the role of glutamatergic neurotransmission in the pathophysiology of psychosis [6]. Determining the nature of glutamatergic abnormalities in psychosis may prove useful in understanding symptomatology and in developing novel treatment strategies. Combined functional MRI (fMRI) and magnetic resonance spectroscopy (MRS)studies have demonstrated a role for regional neurotransmitter modulation of brain functional activity and connectivity in multiple brain regions [7, 8]. In previous studies, we found that neurotransmitter concentrations in the posterior cingulate cortex (PCC), a key component of the DMN, modulate DMN deactivation induced by an n-back working memory task and this association increases with cognitive load [9] and investigated the resting-state functional connectivity (rsFC) of DMN and task positive networks (TPNs) [10]. We studied the triple relationship between PCC neurotransmitters, resting-state FC and DMN deactivation during working memory tasks and found that the internetwork resting-state FC may mediate the relationship between neurotransmitters representing excitation-inhibition balance and task induced DMN deactivation. More recently, we measured Glu and GABA from medial prefrontal cortex (MPFC), another component of DMN, and dorsolateral prefrontal cortex (DLPFC), a critical node in frontoparietal executive control network (CN), as well as the functional connectivity between them under resting state and during Sternberg task, an alternative working memory paradigm [11]. We confirmed a relationship between MPFC neurotransmitters, FC between DMN-CN, and task-evoked DMN deactivation. On the other hand, it is striking that DLPFC neurotransmitter levels did not show significant association with functional MRI measures. These findings imply that MPFC and DLPFC transmission have an asymmetric relationship with task-related activation and inter-network functional connectivity, with MPFC neurotransmission playing a more important role. Recent studies by other groups have reported disrupted correlations between neurotransmitter levels and brain BOLD signals. The associations between cortical neurotransmitters and BOLD activations evoked by the Stroop [12] and working memory [13] tasks were found to be altered in SZ. A few studies have compared the relationship of resting-state connectivities in the ACC [14,15,16] and hippocampus [17] and neurotransmitter levels in SZ and HC and found alterations of this relationship in both regions. In another work, we have identified a relationship between brain energy metabolism and functional connectivity in psychotic disorders [18]. Specifically, we discovered significant correlations between MPFC energy metabolism rate and its functional connectivity with long-distance and large-scale brain networks in healthy controls, and a breakdown of this relationship in individuals with psychotic disorders.
Our findings regarding neurochemical characteristics of DMN have several important implications for DMN dysfunction in psychiatric disorders. In the current report, we extended our previous work [11] to first episode psychosis (FEP) patients and their first-degree unaffected relatives (siblings). Working with FEP patients, we can obviate long-term medication effects and the toxic effects of chronic psychosis. In parallel with our previous work [10, 11], we focused on the measurements of MPFC neurotransmitters and DMN (MPFC)-CN (DLPFC) rsFC. We hypothesized that abnormal excitatory and inhibitory neurotransmission would be associated with the well-known rsFC abnormalities in FEP.
Methods
Participants
43 subjects, including 15 FEP patients, 10 relatives (RL) and 18 healthy controls (HC), were recruited in the current study. 15 patients with all DSM-5 non-affective psychotic disorder diagnoses were allowed. Participants were men and women between the ages of 18–30 under the care of McLean OnTrack, an outpatient specialty program for those with new onset of psychosis within the past 12 months and with at most once hospitalization. At this stage, patients are minimally-treated during acute stabilization but have not been on long-term pharmacotherapy. We excluded first generation antipsychotic medications, clozapine, as well as NMDA-related medications such as memantine and amantadine. We did not exclude GABA-ergic medications since benzodiazepines are so commonly used in the care of FEP patients and it would have limited recruitment even further if we had excluded these medications. Medication doses were stable for 12 weeks at the time of the study. Patients who meet criteria for a DSM-5 substance use disorder, including tobacco and alcohol in the past 3 months were excluded. 10 first-degree unaffected relatives, all siblings, both men and women with no DSM diagnoses of any psychotic disorder (schizophrenia spectrum or bipolar disorder with psychotic features), psychiatric hospitalizations, nor psychoactive medication were enrolled. 18 control participants with no history of medical, neurological, psychiatric, substance use problems, and not taking medications and no history of the same in first degree relatives were also recruited from the community. Exclusion criteria for patients included history of head injury with loss of consciousness, seizure disorder, and MRI contraindications. Exclusion criteria for controls included the same as well personal history of psychiatric diagnosis or treatment, and first degree relative with a history of a psychotic disorder. All procedures were approved by the Mass General Brigham IRB and all participants provided written informed consent.
Clinical assessment
Clinical and community functioning were assessed using the Positive and Negative Syndrome Scale (PANSS), the Young Mania Rating Scale (YMRS), the Montgomery-Asberg Depression Rating Scale (MADRS) and the Multnomah Community Ability Scale (MCAS). The MCAS measures functioning in multiple domains including social interest/effectiveness, independence in daily living, and instrumental role functioning. The North American Adult Reading Test (NAART) was used as a measure of premorbid IQ. Information regarding current psychiatric medication use was collected by patient report, and chlorpromazine (CPZ) equivalents were calculated according to [19].
MRI
The following MRS and fMRI scans were performed on a Siemens 3 T Trio scanner using a 32-channel volume coil: a high-resolution anatomical scan (5 min), resting-state fMRI (6 min × 2 runs), followed by MRS (20 min for localized shimming, MEGA-PRESS and semi-LASER). Resting-state functional connectivity MPFC and DLPFC ROIs, MRS voxels, and representative MR spectra of semi-LASER and MEGA-PRESS of MPFC were presented in Fig. 1.
Single-voxel proton MRS was acquired at MPFC (30 × 20 × 30 mm3). A MEGA-PRESS [20, 21] optimized in house for GABA detection [22] was acquired with the following parameters: TE/TR = 68/3000 ms and total 192 averages (scan time = 10 min); the editing pulses applied alternatively at frequency of 1.9 or 7.5 ppm interleaved with the averages. A semi-LASER sequence [23, 24] with optimized TE = 28 ms [25] and TR = 3 s and 64 averages (scan time = 4 min) was used to measure Glu and Gln from the same regions as MEGA-PRESS. Fastmap shimming [26] was performed before MRS scans to ensure the full widths at half maxima (FWHM) of water resonance <12 Hz. A VAPOR (VAriable pulse Power and Optimized Relaxation delays) module [27] was utilized in both sequences to achieve water suppression. Spectra with unsuppressed water were also acquired for eddy-current correction and quantification reference.
Resting-state fMRI was collected using a single-shot gradient-echo echo-planar imaging sequence. The imaging parameters are: TR/TE = 2.5 s/30 ms; FA = 78°; slice thickness/gap = 4/0 mm; 39 slices; FOV = 220 × 220 mm2 (3.44 × 3.44 mm2 in-plane resolution). Two runs of resting-state fMRI were performed, with 124 time points each run for 5 min. The subjects were instructed to keep the eyes open and think of nothing in particular during the scan.
The anatomical data were acquired for structural reference using a MP-RAGE sequence (256 × 256 × 122 matrix size; 1 × 1 × 1.28 mm3 spatial resolution; TI/TR/TE = 1100/1600/2.25 ms; flip angle = 12°).
We also collected DTI data in the same scans. DTI data were acquired by axial, single-shot spin echo EPI sequence (TR = 6230 ms; TE = 84 ms; FA = 90°; FOV = 1540 × 1540 mm2; matrix = 1120 × 1120; slice thickness=3 mm; slice interval=3 mm; consecutive scanning of 45 slices). One control image without diffusion weighting and 6 images with noncolinear diffusion directions at b = 1000 sec/mm2 were acquired.
Processing
The processing of MRS and rsfMRI followed the previous strategies described in [11]. Briefly, MRS averages were saved individually for all spectra and phase and frequency corrections were applied using FID-A [28]. Quantifications of metabolite concentrations were performed with LCModel [29] with eddy current correction using water as reference. Home-simulated basis spectra of metabolites were used in both MRS sequences. An experimental acquired macromolecule (MM) basis set was used for semi-LASER. The GABA signal measured by MEGA-PRESS contained a MM co-editing contribution which was removed using the MM basis set [30]. The partial volume effect was corrected with the same strategy as in [11]. We also calculated the Glu and GABA concentrations without normalization of gray and white matter (Fig. S2). To confirm the measurement consistency between MEGA-PRESS and semi-LASER, we also performed the correlation between Glx measured by semi-LASER and MEGA-PRESS. The two measures well agree with each other with r = 0.81, p < 0.001 (Fig. S1).
Preprocessing of the rsfMRI data was carried out in DPARSFA [31] and included removing first 5 time points, slice-timing correction, realignment, head motion correction, Gaussian spatial smoothing (FWHM = 4 mm), linear detrending, and spatial normalization to MNI space with a resampling resolution of 3 × 3 × 3 mm3. Nuisance signal regressions and band-pass temporal filtering (passband: 0.01–0.1 Hz) were also performed. The nuisance regressors included Friston’s 24 head motion parameters (6 head motion parameters, 6 head motion parameters one time point before, and the 12 corresponding squared items) [32] and 5 principal components of principal time courses extracted from respective white matter and cerebral spinal fluid (CSF) fluctuations using the anatomical CompCor (aCompCor) method [33]. To minimize the influence of head motion in the rsFC analysis, data points with the instantaneous head motion, defined by framewise displacement (FD) [34] was larger than 0.25 mm, as well as the one time points before and after these “bad” time points were used as regressors in the nuisance regression. Subjects with mean FD > 0.3 mm were excluded from analysis. The global signal regression (GSR) was performed. The MPFC and DLPFC ROIs obtained from the working memory activation/deactivation map in the previous study [11] were used to extract functional connectivity between the two regions. The ROI information including MNI coordinates, volumes etc were presented in Table S1. The importance of including both type of analyses, with and without GSR in rsFC has been shown in [5], therefore the analysis without GSR was also performed.
Statistics
All statistical analyses were performed using IBM SPSS Statistics Version 25. One-way ANOVA was performed to compare the differences of MPFC GABA and Glu concentrations as well as the MPFC-DLPFC functional connectivity between the FEP, RL and HC groups. Bonferroni post hoc tests were performed for significant findings from the one-way ANOVA.
Pearson correlation coefficients were computed between MPFC-DLPFC functional connectivity and MPFC GABA and Glu levels within each group. The age of the participants was within a very narrow range so it was not included as a coefficient in the analysis. Gender was not controlled in the analysis either as our previous study did not show gender as a significant contributor [11]. The relation between GM percentage and measured metabolite concentrations is non-linear and therefore not appropriate to be included as a coefficient. Instead, we calculated the metabolite concentrations in MPFC and DLPFC in pure gray matter with the information of tissue percentages and the prior knowledge of metabolite WM/GM concentration ratios in the same way as our previous publication [11] and suggested by others [35, 36].
Results
Neurotransmitters in MPFC
Two subjects (one HC, one RL) were excluded because of the low SNR of the MEGA-PRESS spectrum caused by the eddy current. The spectral quality metrics, including Cramer-Rao lower bounds (CRLBs), signal of noise ratio (SNR) and the linewidth full-width at half-maximum (FWHM) of the three subject groups, as well as the tissue percentages of the MPFC voxel, are presented in Table S2. All these measures indicate the high MRS data quality stably acquired at our 3 T clinical scanner. There is no significant difference in these measures between the three groups by one-way ANOVA.
Regarding the MPFC neurotransmitters (Fig. 2), a significant group-wise difference was observed on the Glu concentrations (F = 5.6, p = 0.004). Bonferroni post hoc tests showed an elevated Glu level in the MPFC in FEP (9.6 ± 0.6 mM) compared to the control group (8.8 ± 0.6 mM). The Glu level of the relative group (9.1 ± 0.7 mM) is between FEP and HC. There was no significant difference in GABA between the three groups (1.04 ± 0.11 mM, 1.01 ± 0.09 mM and 1.06 ± 0.13 mM for FEP, RL and HC groups respectively).
MPFC-DLPFC resting-state functional connectivity
One subject in the FEP group was excluded because of motions (mean FD > 0.3 mm). Based on MPFC and DLPFC ROIs obtained from the working memory activation/deactivation map in our previous study [11], we extracted rsFC between these two regions; this rsFC is typically an anti-correlation (Fig. 3). A significant group-wise difference in MPFC-DLPFC rsFC was observed in the one-way ANOVA (F = 7.2, p = 0.002). The Bonferroni post hoc test showed the functional anti-correlation between MPFC and DLPFC in FEP was significantly reduced to −0.097 ± 0.184 compared to the control group (−0.250 ± 0.096). The difference between RL (0.302 ± 0.138) and FEP was also significant (p = 0.005).
Relationship between MPFC neurotransmitters and MPFC-DLPFC anti-correlation
The group-wise correlations were presented in Fig. 4. In the control group we replicated the previous finding [11] that GABA and Glu concentrations in the MPFC were significantly associated with anti-correlation between DMN and CN at rest: R2 = 0.42, p = 0.005 (GABA) and R2 = 0.34, p = 0.01 (Glu). The relationship between MPFC neurotransmitter concentrations and functional anti-correlation was absent in FEP: R2 = 7.1e–4, p = 0.93 (GABA) and R2 = 0.011, p = 0.71 (Glu) and in RL: R2 = 0.05, p = 0.56 (GABA) and R2 = 0.13, p = 0.34 (Glu). The removal of GSR reduced the functional anti-correlation but didn’t change the associations with neurotransmitters in different groups (Fig. S3).
DTI
There was no significant difference in global FA between the groups. Furthermore, including the mean FA values as covariates did not change the results of the correlation analysis between neurotransmitters and FC in any group.
Discussion
The prefrontal cortex plays a key role in higher-order cognition and emotional processing through its regulation of cortical and limbic regions and its involvement in higher-order executive function [37, 38]. We do not yet have a detailed picture of how neurochemicals modulate cognition and behavior in psychiatric diseases, one emerging principle is that there is a balance and coordinated activity between excitatory glutamatergic and inhibitory GABAergic neurons. The imbalance of cortical cellular excitation and inhibition could give rise to many abnormalities observed in psychosis [39,40,41,42]. In the current study we measured Glu and GABA levels using dedicated semi-LASER and MEGA-PRESS MRS sequences respectively in the human brain at 3 T. We observed elevated Glu levels in the MPFC in FEP, without a significant change in MPFC GABA. Glutamatergic dysfunction is known to occur in psychosis. The increased Glu observed in the cingulate cortex in our study is consistent with many previous reports. For example, a study by Egerton et al. [43] showed that the Glu/Cr ratio in the ACC of 15 patients with FEP was significantly higher compared to patients in remission. Another MRS study using a 3 T MR scanner revealed that absolute Glu concentrations in the dorsal-caudate of antipsychotic naïve FEP patients were elevated compared with HC subjects [44]. A recent study by our group, using TE-averaged MRS, a different sequence to measure Glu on 4 T, also observed an elevated Glu in the MPFC in FEP [45]. There are several other lines of evidence that implicate the glutamatergic system in the pathophysiology of schizophrenia. Dissociative anesthetics such as phencyclidine (PCP) and ketamine block the glutamate N-methyl-d-aspartate receptor (NMDAR), and the administration of these drugs produces a state in adults that is phenomenologically similar to schizophrenia [46]. Ketamine also increases prefrontal glutamatergic metabolites in human [46, 47] and in rat [48]. On the other hand, a recent review and meta-analysis did not show any significant group differences in MPFC GABA between individuals with schizophrenia and health controls [49]. This is in line with our current findings, although not with our previous report of elevated GABA in schizophrenia [50].
The reduced anticorrelations between DMN and positive task-related activation networks has been widely observed [4, 51,52,53]. DMN is characterized by increased activation during task-free resting periods but becomes deactivated during externally-oriented processing; the latter engages the frontoparietal executive control network (CN) [54], one critical note of which is the DLPFC. There is a report of an association between magnitude of MPFC-DLPFC anti-correlation and working memory capacity for young adults [55], as well as findings of reduced MPFC-DLPFC resting-state anti-correlation and reduced working memory capacity in schizophrenia patients [4] and older healthy subjects [56]. In our previous study, we found that MPFC neurotransmitter concentrations modulate not only the MPFC deactivation during a working memory task, but also the MPFC-DLPFC anticorrelation during resting state and working memory task in heathy young adults [11]. To follow up on our previous study, we targeted the MPFC and DLPFC here to measure their rsFC. The loss of MPFC-DLPFC anticorrelation in FEP in the current study is in line with the literature and may reflect insufficient segregation of internally and externally focused states and disturbance of cognition in psychotic disorders [53].
We find that MPFC Glu modulates the MPFC-DLPFC connectivity positively in healthy young adults, i.e., higher MPFC Glu level predicts weaker anticorrelation, as well as an opposite trend of the correlation between GABA and the MPFC-DLPFC connectivity. This finding replicates our previous study [11] in a new cohort of healthy subjects and in line with other studies [57,58,59,60]. In FEP, we found that both GABA-FC and Glu-FC correlations have broken down. The results of this study suggest that the relationship between GABA and Glu and inter-network functional connectivity between DMN and CN is significantly reduced in FEP. Given the elevated Glu level which may reflect an abnormal glutamatergic system in FEP, it appears that the neurotransmission abnormality is accompanied by a breakdown of normal circuit modulation. On the other hand, though we find no MPFC GABA abnormalities in FEP, the GABA system is known to be abnormal in schizophrenia [61, 62] and an abnormal GABA system could lead to disturbances in FC in FEP. Recent studies have reported a disrupted correlation between regional neurotransmitter levels and task evoked BOLD activation in SZ [12, 13]. Furthermore, a few studies have compared the relationship of rsFC in the ACC [14, 15] and hippocampus [17] and neurotransmitter levels in SZ and HC and found alterations of this relationship in both regions. To our knowledge, the current investigation is the first one to study the association of DMN neurotransmitters and internetwork connection between DMN and task activated networks in psychotic disorders. According to our previous study, MPFC neurotransmitters could be more involved in orchestrating between-network brain activity at rest and during task performance than DLPFC neurotransmitters [11], suggesting a special role for MPFC in this system.
Although there’s substantial evidence of abnormalities in white matter in FEP [63], our current findings cannot be explained by white matter abnormalities. The DTI findings in frontal brain regions of FEP are inconsistent [64,65,66,67]. This picture could be caused by highly variable DTI data acquisition, processing and analysis protocols, and the heterogeneity of subject populations [68]. In the current study, we did not find any statistically significant difference in DTI between HC and FEP. Including the mean FA values as covariate did not significantly change the correlation between neurochemical levels and FC. The absence of DTI findings strengthens our interpretation that neurotransmission abnormalities account for rsFC abnormalities in FEP.
We were able to study a small sample of unaffected siblings as a RL group in this study. These individuals were not siblings of the patients in the study, but they all have siblings with FEP themselves. The RL group provides the advantage of examining psychosis risk without the confounding factors of medication and disease effects. In this study, Glu levels and the rsFC results in the RL group were somewhere between those of the FEP and the HC groups and this is broadly consistent with other observations in the literature. This pattern suggests that our findings reflect the pathophysiology of FEP and cannot be fully explained by confounding factors.
Potential limitations of the current study include a relatively small sample size because of the narrow inclusion criteria; thus patients with different diagnoses were not separated into different groups. The observation of correlation was in the context of a small sample and a “noisy” signal. The correlation directions could vary across studies, as different brain regions are studied. Future studies with a significantly larger sample size and an improved MRSI measurement may further validate the correlations observed in the previous and current studies. Additionally, patients were taking medication. In the current study we did not uncover a relationship between CPZ equivalents and neurotransmitter levels or functional connectivity, suggesting that the dose of antipsychotic medication did not have an effect on our measures. Nonetheless, we cannot rule out medication effects and this needs to be addressed in future studies. Thirdly, the GABA measurement is challenging, and it is subject to MM co-editing. The degree of MM signal contamination varies with sequences and parameters [30, 69, 70]. The symmetric editing method [30] can suppress the co-edited MM signal but it was shown that the MM-suppressed GABA signal is very sensitive to frequency drift [71]. On the other hand, previous studies [72, 73] suggested that the MM concentrations in cortical regions of healthy adults are very stable with respect to age and gender. Therefore, individual differences in the contaminated GABA levels are likely to reflect differences in GABA itself. Lastly, using 1H-MRS to detect synaptic Glu is an unsolved issue. The 1H MRS signal arises from all “free” Glu and not only that at the synapse. It cannot distinguish Glu packed in synaptic vesicles (20–30% of total) from the metabolic pool in cytosol (~50%) [74]. Therefore, total tissue levels of metabolites may not solely reflect neurotransmission. And it should be noted that it is Glu signal instead of Glx that was reported here, as most Glu signal quantified using semi-LASER comes from glutamate. However the glutamate signal is not completely resolved from glutamine, and we cannot rule out the contributions from glutamine or other metabolites.
In the current study, we observed that the relationship between MPFC neurotransmitter concentrations and the functional anti-correlation seen in healthy people was compromised in FEP patients. Coordinated activity within and differential activity between DMN and CN is a critical feature of brain organization. These findings imply that DMN glutamatergic neurotransmission dysfunction has an adverse impact on the interaction between DMN and CN in FEP, and it is important to better understand this dysregulation. They also provide opportunities for developing novel treatment strategies for psychotic disorders.
References
Friston K, Brown HR, Siemerkus J, Stephan KE. The dysconnection hypothesis (2016). Schizophr Res. 2016;176:83–94.
Raichle ME, MacLeod AM, Snyder AZ, Powers WJ, Gusnard DA, Shulman GL. A default mode of brain function. Proc Natl Acad Sci USA. 2001;98:676–82.
Anticevic A, Cole MW, Murray JD, Corlett PR, Wang XJ, Krystal JH. The role of default network deactivation in cognition and disease. Trends Cogn Sci. 2012;16:584–92.
Whitfield-Gabrieli S, Thermenos HW, Milanovic S, Tsuang MT, Faraone SV, McCarley RW, et al. Hyperactivity and hyperconnectivity of the default network in schizophrenia and in first-degree relatives of persons with schizophrenia. Proc Natl Acad Sci USA. 2009;106:1279–84.
Scalabrini A, Vai B, Poletti S, Damiani S, Mucci C, Colombo C, et al. All roads lead to the default-mode network-global source of DMN abnormalities in major depressive disorder. Neuropsychopharmacol: Off Publ Am Coll Neuropsychopharmacol. 2020;45:2058–69.
Moghaddam B, Javitt D. From revolution to evolution: the glutamate hypothesis of schizophrenia and its implication for treatment. Neuropsychopharmacol: Off Publ Am Coll Neuropsychopharmacol. 2012;37:4–15.
Duncan NW, Wiebking C, Northoff G. Associations of regional GABA and glutamate with intrinsic and extrinsic neural activity in humans-a review of multimodal imaging studies. Neurosci Biobehav Rev. 2014;47:36–52.
Kiemes A, Davies C, Kempton MJ, Lukow PB, Bennallick C, Stone JM, et al. GABA, glutamate and neural activity: a systematic review with meta-analysis of multimodal (1)H-MRS-fMRI studies. Front psychiatry. 2021;12:644315.
Hu Y, Chen X, Gu H, Yang Y. Resting-state glutamate and GABA concentrations predict task-induced deactivation in the default mode network.J Neurosci: Off J Soc Neurosci. 2013;33:18566–73.
Gu H, Hu Y, Chen X, He Y, Yang Y. Regional excitation-inhibition balance predicts default-mode network deactivation via functional connectivity. Neuroimage 2019;185:388–97.
Chen X, Fan X, Hu Y, Zuo C, Whitfield-Gabrieli S, Holt D, et al. Regional GABA concentrations modulate inter-network resting-state functional connectivity. Cereb cortex. 2019;29:1607–18.
Overbeek G, Gawne TJ, Reid MA, Salibi N, Kraguljac NV, White DM, et al. Relationship between cortical excitation and inhibition and task-induced activation and deactivation: a combined magnetic resonance spectroscopy and functional magnetic resonance imaging study at 7T in first-episode psychosis. Biol Psychiatry Cogn Neurosci Neuroimaging. 2019;4:121–30.
Kaminski J, Gleich T, Fukuda Y, Katthagen T, Gallinat J, Heinz A, et al. Association of cortical glutamate and working memory activation in patients with schizophrenia: a multimodal proton magnetic resonance spectroscopy and functional magnetic resonance imaging study. Biol psychiatry. 2020;87:225–33.
Shukla DK, Wijtenburg SA, Chen H, Chiappelli JJ, Kochunov P, Hong LE, et al. Anterior cingulate glutamate and GABA associations on functional connectivity in schizophrenia. Schizophr Bull. 2019;45:647–58.
Overbeek G, Gawne TJ, Reid MA, Kraguljac NV, Lahti AC. A multimodal neuroimaging study investigating resting-state connectivity, glutamate and GABA at 7 T in first-episode psychosis. J Psychiatry Neurosci. 2021;46:E702–E10.
Maximo JO, Briend F, Armstrong WP, Kraguljac NV, Lahti AC. Salience network glutamate and brain connectivity in medication-naive first episode patients - a multimodal magnetic resonance spectroscopy and resting state functional connectivity MRI study. Neuroimage Clin. 2021;32:102845.
Nelson EA, Kraguljac NV, Maximo JO, Briend F, Armstrong W, Ver Hoef LW, et al. Hippocampal dysconnectivity and altered glutamatergic modulation of the default mode network: a combined resting-state connectivity and magnetic resonance spectroscopy study in schizophrenia. Biol Psychiatry Cogn Neurosci Neuroimaging. 2022;7:108–18.
Song X, Chen X, Yuksel C, Yuan J, Pizzagalli DA, Forester B, et al. Bioenergetics and abnormal functional connectivity in psychotic disorders. Mol Psychiatry. 2021;26:2483–92.
Baldessarini RJ. Chemotherapy in Psychiatry. 2013.
Mescher M, Merkle H, Kirsch J, Garwood M, Gruetter R. Simultaneous in vivo spectral editing and water suppression. NMR Biomed. 1998;11:266–72.
Rothman DL, Behar KL, Hetherington HP, Shulman RG. Homonuclear 1H double-resonance difference spectroscopy of the rat brain in vivo. Proc Natl Acad Sci USA. 1984;81:6330–4.
Marjanska M, Lehericy S, Valabregue R, Popa T, Worbe Y, Russo M, et al. Brain dynamic neurochemical changes in dystonic patients: a magnetic resonance spectroscopy study. Mov Disord. 2013;28:201–9.
Oz G, Tkac I. Short-echo, single-shot, full-intensity proton magnetic resonance spectroscopy for neurochemical profiling at 4 T: validation in the cerebellum and brainstem. Magn Reson Med: Off J Soc Magn Reson Med / Soc Magn Reson Med. 2011;65:901–10.
Scheenen TW, Klomp DW, Wijnen JP, Heerschap A. Short echo time 1H-MRSI of the human brain at 3T with minimal chemical shift displacement errors using adiabatic refocusing pulses. Magn Reson Med: Off J Soc Magn Reson Med / Soc Magn Reson Med. 2008;59:1–6.
Terpstra M, Cheong I, Lyu T, Deelchand DK, Emir UE, Bednarik P, et al. Test-retest reproducibility of neurochemical profiles with short-echo, single-voxel MR spectroscopy at 3T and 7T. Magn Reson Med: Off J Soc Magn Reson Med / Soc Magn Reson Med. 2016;76:1083–91.
Gruetter R. Automatic, localized in vivo adjustment of all first- and second-order shim coils. Magn Reson Med: Off J Soc Magn Reson Med / Soc Magn Reson Med. 1993;29:804–11.
Tkac I, Starcuk Z, Choi IY, Gruetter R. In vivo H-1 NMR spectroscopy of rat brain at 1 ms echo time. Magn Reson Med. 1999;41:649–56.
Simpson R, Devenyi GA, Jezzard P, Hennessy TJ, Near J. Advanced processing and simulation of MRS data using the FID appliance (FID-A)-An open source, MATLAB-based toolkit. Magn Reson Med: Off J Soc Magn Reson Med / Soc Magn Reson Med. 2017;77:23–33.
Provencher SW. Automatic quantitation of localized in vivo 1H spectra with LCModel. NMR Biomed. 2001;14:260–4.
Henry PG, Dautry C, Hantraye P, Bloch G. Brain GABA editing without macromolecule contamination. Magn Reson Med. 2001;45:517–20.
Yan CG, Zang YF. DPARSF: A MATLAB Toolbox for “Pipeline” Data Analysis of Resting-State fMRI. Front Syst Neurosci. 2010;4:13.
Friston KJ, Williams S, Howard R, Frackowiak RS, Turner R. Movement-related effects in fMRI time-series. Magn Reson Med: Off J Soc Magn Reson Med / Soc Magn Reson Med. 1996;35:346–55.
Behzadi Y, Restom K, Liau J, Liu TT. A component based noise correction method (CompCor) for BOLD and perfusion based fMRI. Neuroimage 2007;37:90–101.
Power JD, Barnes KA, Snyder AZ, Schlaggar BL, Petersen SE. Spurious but systematic correlations in functional connectivity MRI networks arise from subject motion. Neuroimage 2012;59:2142–54.
Porges EC, Woods AJ, Lamb DG, Williamson JB, Cohen RA, Edden RAE, et al. Impact of tissue correction strategy on GABA-edited MRS findings. Neuroimage 2017;162:249–56.
Harris AD, Puts NA, Edden RA. Tissue correction for GABA-edited MRS: considerations of voxel composition, tissue segmentation, and tissue relaxations. J Magn Reson Imaging: JMRI. 2015;42:1431–40.
Goldstein RZ, Volkow ND. Dysfunction of the prefrontal cortex in addiction: neuroimaging findings and clinical implications. Nat Rev Neurosci. 2011;12:652–69.
Kalivas PW, Volkow N, Seamans J. Unmanageable motivation in addiction: a pathology in prefrontal-accumbens glutamate transmission. Neuron 2005;45:647–50.
Yizhar O, Fenno LE, Prigge M, Schneider F, Davidson TJ, O’Shea DJ, et al. Neocortical excitation/inhibition balance in information processing and social dysfunction. Nature 2011;477:171–8.
Jocham G, Hunt LT, Near J, Behrens TE. A mechanism for value-guided choice based on the excitation-inhibition balance in prefrontal cortex. Nat Neurosci. 2012;15:960–1.
Cocchi L, Zalesky A, Fornito A, Mattingley JB. Dynamic cooperation and competition between brain systems during cognitive control. Trends Cogn Sci. 2013;17:493–501.
Gipson CD, Reissner KJ, Kupchik YM, Smith AC, Stankeviciute N, Hensley-Simon ME, et al. Reinstatement of nicotine seeking is mediated by glutamatergic plasticity. Proc Natl Acad Sci USA. 2013;110:9124–9.
Egerton A, Brugger S, Raffin M, Barker GJ, Lythgoe DJ, McGuire PK, et al. Anterior cingulate glutamate levels related to clinical status following treatment in first-episode schizophrenia. Neuropsychopharmacol: Off Publ Am Coll Neuropsychopharmacol. 2012;37:2515–21.
de la Fuente-Sandoval C, Leon-Ortiz P, Favila R, Stephano S, Mamo D, Ramirez-Bermudez J, et al. Higher levels of glutamate in the associative-striatum of subjects with prodromal symptoms of schizophrenia and patients with first-episode psychosis. Neuropsychopharmacol: Off Publ Am Coll Neuropsychopharmacol. 2011;36:1781–91.
Kim SY, Kaufman MJ, Cohen BM, Jensen JE, Coyle JT, Du F, et al. In vivo brain glycine and glutamate concentrations in patients with first-episode psychosis measured by echo time-averaged proton magnetic resonance spectroscopy at 4T. Biol psychiatry. 2018;83:484–91.
Rowland LM, Bustillo JR, Mullins PG, Jung RE, Lenroot R, Landgraf E, et al. Effects of ketamine on anterior cingulate glutamate metabolism in healthy humans: A 4-T Proton MRS Study. Am J Psychiatry. 2005;162:394–96.
Stone JM, Dietrich C, Edden R, Mehta MA, De Simoni S, Reed LJ, et al. Ketamine effects on brain GABA and glutamate levels with 1H-MRS: relationship to ketamine-induced psychopathology. Mol Psychiatry. 2012;17:664–5.
Moghaddam B, Adams B, Verma A, Daly D. Activation of glutamatergic neurotransmission by ketamine: a novel step in the pathway from NMDA receptor blockade to dopaminergic and cognitive disruptions associated with the prefrontal cortex. J Neurosci: Off J Soc Neurosci. 1997;17:2921–7.
Egerton A, Modinos G, Ferrera D, McGuire P. Neuroimaging studies of GABA in schizophrenia: a systematic review with meta-analysis. Transl Psychiatry. 2017;7:e1147.
Ongur D, Prescot AP, McCarthy J, Cohen BM, Renshaw PF. Elevated gamma-aminobutyric acid levels in chronic schizophrenia. Biol psychiatry. 2010;68:667–70.
Hu ML, Zong XF, Mann JJ, Zheng JJ, Liao YH, Li ZC, et al. A review of the functional and anatomical default mode network in schizophrenia. Neurosci Bull. 2017;33:73–84.
Williamson P. Are anticorrelated networks in the brain relevant to schizophrenia? Schizophr Bull. 2007;33:994–1003.
Wotruba D, Michels L, Buechler R, Metzler S, Theodoridou A, Gerstenberg M, et al. Aberrant coupling within and across the default mode, task-positive, and salience network in subjects at risk for psychosis. Schizophr Bull. 2014;40:1095–104.
Buckner RL, Andrews-Hanna JR, Schacter DL. The brain’s default network: anatomy, function, and relevance to disease. Ann N Y Acad Sci. 2008;1124:1–38.
Hampson M, Driesen N, Roth JK, Gore JC, Constable RT. Functional connectivity between task-positive and task-negative brain areas and its relation to working memory performance. Magn Reson Imaging. 2010;28:1051–7.
Keller JB, Hedden T, Thompson TW, Anteraper SA, Gabrieli JD, Whitfield-Gabrieli S. Resting-state anticorrelations between medial and lateral prefrontal cortex: association with working memory, aging, and individual differences. Cortex 2015;64:271–80.
Kapogiannis D, Reiter DA, Willette AA, Mattson MP. Posteromedial cortex glutamate and GABA predict intrinsic functional connectivity of the default mode network. Neuroimage 2013;64:112–9.
Duncan NW, Enzi B, Wiebking C, Northoff G. Involvement of glutamate in rest-stimulus interaction between perigenual and supragenual anterior cingulate cortex: a combined fMRI-MRS study. Hum brain Mapp. 2011;32:2172–82.
Duncan NW, Wiebking C, Tiret B, Marjanska M, Hayes DJ, Lyttleton O, et al. Glutamate concentration in the medial prefrontal cortex predicts resting-state cortical-subcortical functional connectivity in humans. PloS one. 2013;8:e60312.
Schmaal L, Goudriaan AE, van der Meer J, van den Brink W, Veltman DJ. The association between cingulate cortex glutamate concentration and delay discounting is mediated by resting state functional connectivity. Brain Behav. 2012;2:553–62.
Benes FM, Berretta S. GABAergic interneurons: implications for understanding schizophrenia and bipolar disorder. Neuropsychopharmacol: Off Publ Am Coll Neuropsychopharmacol. 2001;25:1–27.
Guidotti A, Auta J, Davis JM, Di-Giorgi-Gerevini V, Dwivedi Y, Grayson DR, et al. Decrease in reelin and glutamic acid decarboxylase67 (GAD67) expression in schizophrenia and bipolar disorder: a postmortem brain study. Arch Gen Psychiatry. 2000;57:1061–9.
Du F, Ongur D. Probing myelin and axon abnormalities separately in psychiatric disorders using MRI techniques. Front Integr Neurosci. 2013;7:24.
Scheel M, Prokscha T, Bayerl M, Gallinat J, Montag C. Myelination deficits in schizophrenia: evidence from diffusion tensor imaging. Brain Struct Funct. 2013;218:151–56.
Kumar J, Iwabuchi S, Oowise S, Balain V, Palaniyappan L, Liddle PF. Shared white-matter dysconnectivity in schizophrenia and bipolar disorder with psychosis. Psychological Med. 2015;45:759–70.
Mamah D, Ji A, Rutlin J, Shimony JS. White matter integrity in schizophrenia and bipolar disorder: tract- and voxel-based analyses of diffusion data from the connectom scanner. NeuroImage Clin. 2019;21:101649.
Boos HB, Mandl RC, van Haren NE, Cahn W, van Baal GC, Kahn RS, et al. Tract-based diffusion tensor imaging in patients with schizophrenia and their non-psychotic siblings. Eur Neuropsychopharmacol: J Eur Coll Neuropsychopharmacol. 2013;23:295–304.
Kubicki M, McCarley R, Westin CF, Park HJ, Maier S, Kikinis R, et al. A review of diffusion tensor imaging studies in schizophrenia. J Psychiatr Res. 2007;41:15–30.
Terpstra M, Ugurbil K, Gruetter R. Direct in vivo measurement of human cerebral GABA concentration using MEGA-editing at 7 Tesla. Magn Reson Med: Off J Soc Magn Reson Med / Soc Magn Reson Med. 2002;47:1009–12.
Near J, Simpson R, Cowen P, Jezzard P. Efficient gamma-aminobutyric acid editing at 3T without macromolecule contamination: MEGA-SPECIAL. NMR Biomed. 2011;24:1277–85.
Edden RA, Oeltzschner G, Harris AD, Puts NA, Chan KL, Boer VO, et al. Prospective frequency correction for macromolecule-suppressed GABA editing at 3T. J Magn Reson Imaging: JMRI. 2016;44:1474–82.
Hofmann L, Slotboom J, Boesch C, Kreis R. Characterization of the macromolecule baseline in localized (1)H-MR spectra of human brain. Magn Reson Med: Off J Soc Magn Reson Med / Soc Magn Reson Med. 2001;46:855–63.
Mader I, Seeger U, Karitzky J, Erb M, Schick F, Klose U. Proton magnetic resonance spectroscopy with metabolite nulling reveals regional differences of macromolecules in normal human brain. J Magn Reson Imaging: JMRI. 2002;16:538–46.
Nedergaard M, Takano T, Hansen AJ. Beyond the role of glutamate as a neurotransmitter. Nat Rev Neurosci. 2002;3:748–55.
Funding
This research work was partially supported by National Institutes of Health (NIH) grants: R01MH114982, P50MH115846, R01AG066670 and R01MH095809.
Author information
Authors and Affiliations
Contributions
XC: Analysis of data and interpretation of result. Drafting of paper. XS: Analysis of data. Revision of paper. DÖ: Conception of idea and design of the study. Interpretation of result. Revision of paper and final approval of the submission. FD: Conception of idea and design of the study. Acquisition of data. Revision of paper.
Corresponding author
Ethics declarations
Competing interests
DÖ received honoraria from Neumora Inc and Guggenheim LLC for scientific presentation. The remaining authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Chen, X., Song, X., Öngür, D. et al. Association of default-mode network neurotransmitters and inter-network functional connectivity in first episode psychosis. Neuropsychopharmacol. 48, 781–788 (2023). https://doi.org/10.1038/s41386-023-01546-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41386-023-01546-y