Abstract
Analysis of the Gene Expression Profiling Interactive Analysis (GEPIA) database revealed that Kelch-like 17 (KLHL17) is overexpressed in non-small cell lung cancer (NSCLC) including adenocarcinoma (ADC) and squamous cell carcinoma (SCC). We therefore explored the role of KLHL17 in the development and progression of NSCLC. Immunohistochemistry and western blotting showed that KLHL17 expression was significantly higher in the tumor tissues from 173 patients with NSCLC, compared with the corresponding non-neoplastic tissue. In addition, upregulated KLHL17 expression was positively correlated with tumor size, lymph node metastasis and tumor node metastasis (TNM) stage, and affected the overall survival (OS) of patients with NSCLC. Consistent with clinical samples, in vitro studies demonstrated that KLHL17 expression was higher in various cell lines of NSCLC (A549, H1299, H460 and SK cells) as compared to normal human bronchial epithelial cells (HBE cells). Overexpression of KLHL17 in the cell lines of NSCLC with KLHL17-Flag plasmid promoted the proliferation and migration of tumor cells, which was associated with elevated activation of Rat sarcoma/Mitogen-activated protein kinases (Ras/MAPK) signaling and increased expression of cyclin D1, cyclin D-dependent kinases 4 (CDK4), matrix metalloproteinase 2 (MMP2) and Ras homolog gene family member A (RhoA). In contrast, knockdown of KLHL17 in the cell lines of NSCLC using KLHL17 small interfering RNA suppressed the proliferation and migration of tumor cells, in association with reduced activation of Ras/MAPK signaling and decreased expression of cyclin D1, CDK4, MMP2 and RhoA. Moreover, treatment of tumor cells with Ras inhibitor salirasib prevented KLHL17-induced Ras/MAPK activity as well as tumor proliferation and migration. These results suggest that upregulated KLHL17 in NSCLC promotes the proliferation and migration of tumor by activating Ras/MAPK signaling pathway. Therefore, KLHL17 may be a novel therapeutic target for the treatment of NSCLC.
Similar content being viewed by others
Introduction
Despite enhanced recognition and concerns regarding physical health, the incidence of lung cancer has continuously shown an upward trend1,2, which not only puts a burden on the affected families but also on society. Lung cancer accounts for 13% of all global cancer cases and 23% of all cancer-related deaths3. NSCLC is the most common type of lung cancer that accounts for 85% of all lung cancer4,5 and is associated with poor prognosis and limited treatment options6,7. Although standard surgical lobectomy has been and is currently the gold standard for early-stage NSCLC, not all patients are medically fit to undergo surgery. Additionally, a proportion of lung cancer patients develop local recurrence or systemic metastasis, even after curative resection. Over the past decade, advances in molecular targeted therapies and immunotherapies provide hope for patients with lung cancer including NSCLC4. Unfortunately, fewer than 25% of patients benefit from current targeted therapies or immunotherapies, and inherited/acquired resistance may eventually develop during treatment4. Thus, the identification of specific novel molecular targets and the development of matched targeted therapies remain urgently needed.
KLHL17 is one of the 42 known members of the Kelch protein family characterized by a broad-complex, tramtrack, bri-a-brac/poxvirus and zinc finger (BTB/POZ) domain, BTB and C-terminal Kelch (BACK) domain, and five Kelch repeats8,9. The BTB/POZ domain has multiple functions, including the maintenance of the cytoskeleton10, ion channel gating11, transcriptional repression12 and ubiquitination of targeted proteins via cullin E3 ligase13,14. Kelch repeats or domains are evolutionarily conserved structures from Drosophila melanogaster to humans15. Our team is committed to the study of the mechanism of the Kelch protein family in NSCLC. The previous results showed that Kelch-like 38 (KLHL38) and Kelch-like 18 (KLHL18) had an impact on the proliferation, migration and prognosis of NSCLC, and played a role in promoting or inhibiting the development of NSCLC16,17. What’s more, a previous study identified the methylation of KLHL17 gene in early-stage breast tumors compared with that in adjacent normal samples18. Intersection analysis indicated that KLHL17 was correlated with both overall survival (OS) and disease free interval (DFI) in prostate adenocarcinoma19. However, no study to date has reported the role of KLHL17 in lung cancer. In this study, we hypothesized that KLHL17 might play a role in the development and progression of NSCLC and examined whether KLHL17 exerts tumor-promoting function in NSCLC using clinical samples and NSCLC cells.
Materials and methods
Oncomine database analysis
The Gene Expression Profiling Interactive Analysis (GEPIA) database (http://gepia.cancer-pku.cn/) was used to analyze the difference between the KLHL17 expression of NSCLC tissue and non-neoplastic tissue. The analysis data originated from The Cancer Genome Atlas (TCGA) and Genotype-Tissue Expression (GTEx) databases, which reflected the gene expression. Oncomine public cancer microarray database (https://www.oncomine.org/resource/login.html) was used to analyze the data information of gene expression array of NSCLC20. The data set was defined as p < 0.01 and log2FC > 1.5, and the mRNA expression level of KLHL17 was analyzed and compared between tumor tissue and non-neoplastic tissue.
Patients and specimens
In this study, tissue samples were obtained from 173 randomly selected patients who were diagnosed with lung cancer and underwent tumor resection surgery between 2010 and 2018. None of the patients had received radiotherapy or chemotherapy before the surgery, which was confirmed by reviewing the patients’ medical records. The clinical and pathological characteristics of the cases are summarized in Table 1. This study was approved by the Ethics Committee of China Medical University, and all patients signed an informed consent form.
NSCLC cell culture
All cell lines were purchased from Shanghai Cell Bank (Shanghai, China) and cultured in a medium containing 10% fetal bovine serum (FBS; FB15015; Clark Biosciences, Richmond, VA, USA). HBE cells were cultured in high-glucose Dulbecco’s modified Eagle’s medium (Gibco, New York, USA), whereas NSCLC cell lines A549, H1299, H460, and H292 were cultured in Roswell Park Memorial Institute 1640 medium (Gibco, New York, USA). The SK cell line was cultured in minimal essential medium (Gibco, New York, USA).
Plasmid construction and transfection
KLHL17 small interfering RNA (siKLHL17) and its negative control (negative control) were purchased from RiboBio Co., Ltd. (Guangzhou, China). KLHL17-Flag and its negative control plasmid pCMV6 were purchased from Origene (Rockville, MD, USA). siKLHL17 and KLHL17-Flag were transfected into A549 and H1299 lung cancer cells using Lipofectamine 3000 (Invitrogen, Carlsbad, CA, USA) according to the manufacturer’s instructions to downregulate or upregulate KLHL17 expression, respectively.
Tissue immunohistochemistry
NSCLC tissue sections were incubated with anti-KLHL17 antibody (HPA031251, Sigma-Aldrich, St. Louis, MO, USA) at 4 °C overnight at a dilution of 1:100. After tissue sections were developed, the expression of KLHL17 was analyzed based on the color and staining intensity (brown denoted high expression, yellow moderate expression, light yellow low expression, and colorless indicated negative expression), and expression levels were compared between normal and adjacent tissue samples.
Cellular immunohistochemistry
Round glass slides of suitable sizes for each well of a 24-well plate were placed in a cell culture dish, on which 103 cells were seeded. After incubation at 37 °C overnight, the glass slides were washed three times with phosphate-buffered saline (PBS), and the cells were fixed with pre-cooled methanol. The slides containing the cells were then incubated overnight at 4 °C with anti-KLHL17 antibody (HPA031251, Sigma-Aldrich) at a 1:100 dilution. The next day, the cells were stained with crystal violet solution, and the expression of KLHL17 was observed.
Immunofluorescence
Round glass slides of suitable sizes for each well of a 24-well plate were placed in a cell culture dish, on which 103 cells were added. After incubating at 37 °C overnight, the cells were fixed with 4% paraformaldehyde followed by treatment with 0.1% Triton X-100 for 10 min. The glass slides were washed with PBS three times followed with 3% bovine serum albumin treatment (A8010, Solarbio, Beijing, China) to block the cells for 2 h. The cells were then incubated with anti-KLHL17 antibody and incubated overnight at 4 °C as described above for immunohistochemistry. The next day, glass slides were incubated with a fluorescent secondary antibody (A0562, Beyotime, China) in the dark for 2 h, and the cells were imaged using a confocal microscope (FV3000, Olympus, Fukuoka, Japan).
Western blotting
Approximately 106 cells were placed in a centrifugal tube and centrifuged at 4 °C (3000 rpm; 5 min). After obtaining the pellet, four times the volume of the cell lysate was treated with a protease inhibitor (P0013; Beyotime Biosciences, Shanghai, China) and phosphatase inhibitor (B14002 and B15002, respectively; Biotool, Shanghai, China) at a 100:1:1 ratio, and a 35-μg sample was prepared. Next, the proteins were separated using SDS-PAGE, transferred to a polyvinylidene difluoride membrane (Millipore, Billerica, MA, USA), and blocked with 5% skim milk (232100; BD Co., Franklin Lakes, NJ, USA) for 2 h. Membranes were incubated with primary antibodies at 4 °C overnight, followed by incubation with a peroxidase-conjugated secondary antibody (A0208, A0216, Beyotime, China) for 2 h at 37 °C. The antibodies used in this experiment were as follows: anti-MMP2 (409904 s, 1:1,000), anti-β-actin (3700 s, 1:2000), anti-CDK4 (12790 s, 1:1,000), anti-Cyclin D1 (55506 s, 1:1,000), anti-phospho-MAPK (4370 s, 1:1,000), and anti-RhoA (2117 s, 1:1,000) were obtained from Cell Signaling Technology (Danvers, MA, USA), and anti-PanRas (60309-1-lg, 1:1,000) was obtained from Proteintech Group (Chicago, IL, USA). Proteins were visualized using enhanced chemiluminescence (ECL 34080; Thermo Fisher Scientific, Waltham, MA, USA). The ImageJ software was used to quantitatively evaluate the grayscale integral value of each band.
Proliferation assay
Cells (A549, H1299 and SK) transfected with siKLHL17 or KLHL17-Flag were added to a 96-well culture plate at 3,000 cells/well with five replicates and cultured with 10% FBS for 5 days. One culture plate was removed per day, to which 20 μL of 3-(4,5-dimethylthiazol-2-yl)-5-(3-carboxymethoxyphenyl)-2-(4-sulfophenyl)-2H-tetrazole salt (MTS; G3580, Promega, Madison, WI, USA) solution was added to measure cell viability and proliferation. The cells were cultured at 37 °C for 1 h in the dark, and cell proliferation was measured at a wavelength of 490 nm.
Colony formation assay
Cells (A549, H1299 and SK) transfected with siKLHL17 or KLHL17-Flag were plated in a 6-well culture plate at 800 cells/well and incubated with 10% FBS at 37 °C for 2 weeks. The cell culture plate was then washed with PBS three times and the cells were fixed in pre-chilled methanol. The cells were stained with crystal violet staining solution, and images were acquired to determine the number of colonies.
Migration assay
Cells (A549, H1299 and SK) transfected with siKLHL17 or KLHL17-Flag were added to the upper chamber of a transwell chamber at 5 × 104 cells/100 μL and cultured in presence of 2% FBS; 600 μL of 20% FBS was added to the lower chamber and the cells were incubated at 37 °C for 24 h. The transwell chamber was then washed with PBS three times and fixed with pre-chilled methanol followed by staining with crystal violet solution. The number of migrating cells was counted from the images of stained cells.
Inhibitor treatments
The cells were treated with KLHL17-Flag followed by 20 μM of the Ras inhibitor salirasib (HY-14754, MCE) for 24 h.
Gene set enrichment analysis
To reveal the unique biological significance and key pathways associated with KLHL17, we used Gene Set Enrichment Analysis (GSEA) (version 6.2) for analysis and selected the enrichment items with the absolute value of normalized enrichment score (NES) > 1, P < 0.05 and false discovery rate (FDR) < 0.25 as the potential biological function and carcinogenic mechanism of the target gene. Kyoto Encyclopedia of Genes and Genomes (KEGG) information was included in the analysis.
Statistical analysis
All data were analyzed using SPSS version 24.0 (Beijing, China) and GraphPad Prism 5 (La Jolla, CA, USA). χ2 test was used to assess the correlation between clinicopathological factors and KLHL17 expression. Differences between two groups were analyzed with Student’s t test. Overall survival was assessed using Kaplan–Meier survival analysis and the log rank test. All experiments were repeated independently at least three times under the same conditions. The sample size chosen for each experiment was based on a previous study21. Results with P < 0.05 were considered statistically significant.
Results
Increased KLHL17 expression in the tumor tissues is associated with poor prognosis of patients with NSCLC
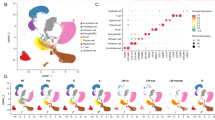
We first evaluated the expression of KLHL17 by screening the GEPIA database (http://gepia.cancer-pku.cn/) and searching the public cancer microarray database (Oncomine), the results showed that we found that KLHL17 expression was significantly higher in lung cancer tissues, particularly in lung adenocarcinoma and squamous cell carcinoma, compared with that in normal lung tissues (Fig. 1).
A Analysis of the Gene Expression Profiling Interactive Analysis (GEPIA) database showing the expression of KLHL17 in lung adenocarcinoma (LUAD) and lung squamous cell carcinoma (LUSC). Red: the tumor tissue; gray: the adjacent normal tissue. *P < 0.05. B–E Data retrieving from Garber Lung oncomine database, Selamat Lung oncomine database, Hou Lung oncomine database and the Cancer Genome Atlas (TCGA) oncomine database showing high expression of KLHL17 in most non-small cell lung cancer samples.
Then we evaluated the expression of KLHL17 in the tumor tissues from 173 patients with NSCLC using immunohistochemistry. Our results showed that no KLHL17 expression was observed in either normal bronchial epithelium or normal alveoli of the lung tissues, whereas positive staining for KLHL17 was detected in both lung squamous cell carcinoma and lung adenocarcinoma tissues (Fig. 2A). To quantitatively analyze protein levels of KLHL17 in tumor tissues, eight pairs of fresh tissue samples were randomly selected from these 173 tissue samples for western blotting analysis and the results showed that the protein levels of KLHL17 were markedly higher in the tumor tissues than in the adjacent normal tissues for six pairs of the eight pairs of tissue samples (Fig. 2B). These data are consistent with the observation from immunohistochemistry.
A Representative immunohistochemistry images of KLHL17 staining in normal bronchial epithelium (a), normal alveolar epithelium (b), highly differentiated lung squamous cell carcinoma (c), highly differentiated lung adenocarcinoma(d), poorly differentiated lung squamous cell carcinoma(e), and poorly differentiated lung adenocarcinoma (f). B Western blotting analysis of KLHL17 expression in eight paired non-small cell lung cancer tissues and their corresponding adjacent normal tissues. *P < 0.05 vs corresponding adjacent normal tissues. C Kaplan–Meier plotter analysis showing the correlation between KLHL17 expression and the prognosis of patients with lung cancer. Red line: high KLHL17 expression; black line: low KLHL17 expression (P = 8.8e−05). Data were from the Kaplan–Meier plotter database (https://kmplot.com/analysis/index.php?p=service&cancer=lung).
Kaplan-Meier plotter analysis revealed that KLHL17 expression was significantly associated with the degree of NSCLC differentiation (P = 0.022), tumor size (P < 0.001), lymph node migration (P = 0.004), and TNM stage (P = 0.004). Moreover, the survival of patients with lung cancer who had high KLHL17 expression was significantly shorter than that of those with low KLHL17 expression (Fig. 2C).
KLHL17 is highly expressed in NSCLC cells
We next evaluated the protein levels of KLHL17 in five commonly used NSCLC cell lines and normal HBE cell line using western blotting. As shown in Fig. 3A, KLHL17 protein levels were significantly higher in four NSCLC cell lines as compared to normal HBE cell line. Consistent with western blotting data, subsequent immunohistochemical analysis (Fig. 3B) and confocal imaging (Fig. 3C) showed abundant expression of KLHL17 in four NSCLC cell lines, which was predominantly located in the nucleus of tumor cells. These in vitro results confirmed the findings from clinical samples.
A Western blotting analysis showing expression of KLHL17 in normal human bronchial epithelial (HBE) cells and various NSCLC cell lines. B Immunocytochemistry images showing abundant KLHL17 expression in different NSCLC cell lines. C Confocal microscopy images showing the localization of KLHL17 in various NSCLC cell lines.
KLHL17 promotes the proliferation and migration of NSCLC cells
Based on the results of western blotting, immunohistochemical and immunofluorescence studies showing that A549, H1299 and SK cell lines had more abundant expression of KLHL17, we selected these cell lines to further examine the role of KLHL17 in the proliferation and migration of NSCLC cells.
MTS assay showed that A549, H1299 and SK cells transfected with KLHL17-Flag plasmid to overexpress KLHL17 had significantly enhanced proliferation ability, whereas these cells transfected with siKLHL17 to knock down KLHL17 expression exhibited decreased cell proliferation than respective control cells (Fig. 4A, P < 0.05). Additionally, cells overexpressing KLHL17 with KLHL17-Flag plasmid showed increased colony-forming ability, whereas suppressing KLHL17 using siRNA decreased the colony-forming ability of both A549, H1299 and SK cells (Fig. 4B, P < 0.05). Similarly, the Transwell assay revealed that high expression of KLHL17 promoted the migration ability but downregulated KLHL17 reduced the migration ability in all three selected NSCLC cell lines (Fig. 5, P < 0.05).
A MTS assay showing effects of KLHL17 overexpression with KLHL17-Flag plasmid (KLHL17) or KLHL17 knockdown with small interfering RNA (siKLHL17) on the proliferation ability of A549, H1299 and SK cells. *P < 0.05 vs negative control (NC), #P < 0.05 vs Empty. B Colony formation assay showing the effects of KLHL17 overexpression or KLHL17 knockdown on colony formation ability of A549, H1299 and SK cells. Quantitative analysis of the numbers of colonies is shown on the right. *P < 0.05, **P < 0.01 vs negative control (NC) or Empty.
KLHL17 exerts its tumor-promoting effect by activating Ras/MAPK signaling pathway
Using GSEA for possible pathways and genes related to NSCLC enrichment, we found that the KLHL17 and Ras/MAPK signaling pathway have a close relationship with NSCLC (Fig. 6A, B). Rho A, cyclins and MMPs play important roles in tumor proliferation and migration21,22. Ras/MAPK signaling has been shown to contribute to tumor proliferation and migration by regulating Rho A, cyclins and MMPs23. To determine the molecular mechanism by which KLHL17 promotes tumor proliferation and migration of NSCLC, we assessed activation of Ras/MAPK signaling and expression of Rho A, cyclin D1, CDK4 and MMP2 in the cell lines of NSCLC treated with KLHL17-Flag plasmid and siKLHL17.
A and B Analysis of Kyoto Encyclopedia of Genes and Genomes (KEGG) and Gene Set Enrichment Analysis (GSEA) databases showing the association between KLHL17 and Ras/MAPK signaling pathway. C–E Effects of KLHL17 overexpression with KLHL17-Flag plasmid (KLHL17) or KLHL17 knockdown with small interfering RNA (siKLHL17) on Ras/MAPK signaling pathway and expression of cyclin D1, CDK4, MMP2 and RhoA in A549, H1299 and SK cells.
Western blotting analysis showed that overexpression of KLHL17 with KLHL17-Flag plasmid elevated expression of Ras, phosphorylated extracellular regulated protein kinases (ERK) 1/2, Rho A, cyclin D1, CDK4 and MMP2, whereas knockdown of KLHL17 with siKLHL17 reduced expression of Ras, phosphorylated ERK 1/2, Rho A, cyclin D1, CDK4 and MMP2 in A549 (Fig. 6C), H1299 (Fig. 6D) and SK cells (Fig. 6E).
To further confirm the effect of KLHL17 on Ras/MAPK signaling pathway, we treated KLHL17-Flag-transfected A549, H1299 and SK cells with salirasib, a specific inhibitor of Ras. As presented in Fig. 7, salirasib treatment prevented KLHL17-induced increase in expression of phosphorylated ERK1/2, which was accompanied by reduction in expression of Rho A, cyclin D1, CDK4 and MMP2 in A549, H1299 and SK cells (Fig. 7A). In addition, salirasib treatment also suppressed the ability of KLHL17 to promote cell proliferation (Fig. 7B), colony formation (Fig. 7C) and cell migration (Fig. 7D) in A549, H1299 and SK cells.
A Effect of Ras inhibitor salirasib treatment on KLHL17-induced expression of phosphorylated ERK1/2, cyclin D1, CDK4, MMP2 and RhoA in A549, H1299 and SK cells. B–D Effect of Ras inhibitor salirasib treatment on KLHL17-induced proliferation ability, colony formation ability and migration ability of A549, H1299 and SK cells. *P < 0.05, **P < 0.01 vs E + D. E + D: Empty+DSMO; K17 + D: KLHL17 + DMSO; E + S: Empty+salirasib; K17 + S: KLHL17 + salirasib.
Discussion
The novel findings of this study are: (1) KLHL17 expression is significantly higher in the tumor tissues from patients with NSCLC, compared with normal lung tissues; upregulated KLHL17 expression is positively correlated with tumor size, lymph node metastasis and TNM stage, and affected the overall survival of patients with NSCLC. (2) KLHL17 expression is higher in various cell lines of NSCLC (A549, H1299, H460 and SK cells) as compared to normal human bronchial epithelial cells. (3) Overexpression of KLHL17 in the cell lines of NSCLC promotes the proliferation and migration of tumor cells, which is associated with elevated activation of Ras/MAPK signaling and increased expression of cyclin D1, CDK4, MMP2 and RhoA. In contrast, knockdown of KLHL17 in the cell lines of NSCLC suppresses the proliferation and migration of tumor cells, in association with reduced activation of Ras/MAPK signaling and decreased expression of cyclin D1, CDK4, MMP2 and RhoA. (4) Treatment of tumor cells with Ras inhibitor salirasib prevents KLHL17-induced Ras/MAPK activity as well as tumor proliferation and migration.
Kelch-like proteins that are encoded by 42 Kelch-like gene family members consist of the prominent class of substrate adaptors of cullin3-RING ligases8,9,24. Cullin3-RING ligases play essential roles in cancer progression by regulating protein hemostasis24. Structurally, substrate binding pockets that are composed by six kelch repeat domain of KLHLs differ from each other25. KLHLs exert different biological function via specificities of substrate recognizing in many diseases26. Accumulating evidence shows that KLHLs display aberrant alterations in the tumor progression including dysregulation of KLHL expression27,28,29,30, indicating that alteration in KLHLs might contribute to cancer progression. For example, increased KLHL22 expression promotes malignant melanoma growth in vitro and in vivo31. KLHL14 is specially upregulated in ovarian or endometrial cancer and upregulation of KLHL14 is positively associated with worse outcome in patients with ovarian or endometrial cancer32. However, the role of KLHL17 in the pathogenesis of cancer remains unclear. In this study, expression of KLHL17 in the tumor samples from 173 patients with NSCLC was assessed. We found that KLHL17 expression is significantly higher in the tumor tissues compared with normal lung tissues. In addition, upregulated KLHL17 expression is positively correlated with tumor size, lymph node metastasis and TNM stage as well as worsened survival among patients with NSCLC. In vitro study showed that various cell lines of NSCLC (A549, H1299, H460 and SK cells) had higher KLHL17 expression than normal human bronchial epithelial cells, which confirmed the finding from clinical samples. Overexpression of KLHL17 in the cell lines of NSCLC promoted the proliferation and migration of tumor cells, whereas knockdown of KLHL17 in the cell lines of NSCLC suppressed the proliferation and migration of tumor cells. These results provide direct evidence that KLHL17 is overexpressed in the NSCLC and that overexpression of KLHL17 contributes to proliferation, migration and invasion of NSCLC. These findings also suggest that KLHL17 expression in the tumor tissues predicts the poor prognosis in patients with NSCLC.
The Ras/MAPK pathway is known to play an important role in cell cycle progression, protein synthesis, differentiation, migration, survival and senescence33. Additionally, the Ras/MAPK pathway has been considered as a major driver of oncogenesis and is dysregulated in nearly 30% of human cancers, primarily by mutation in the Ras genes34. The direct inhibition of Ras/MAPK ERK1/2 pathway has been suggested to provide valuable therapeutic options for cancers driven by Ras mutation34. An early study has demonstrated that ERK1/2 is activated in NSCLC and that ERK1/2 activation is positively correlated with tumor stage and lymph node metastases35. Our present data showed that overexpression of KLHL17 elevated expression of Ras and phosphorylated ERK1/2 in cells of NSCLC, which was associated with increased expression of Rho A, cyclin D1, CDK4 and MMP2, the major factors for tumor proliferation and migration21,22. In contrast, knockdown of KLHL17 reduced expression of Ras and phosphorylated ERK 1/2 in cells of NSCLC, leading to decreased expression of Rho A, cyclin D1, CDK4 and MMP2. More importantly, we found that inhibition of Ras/MAPK pathway with a Ras inhibitor suppressed the ability of KLHL17 to promote cell proliferation, colony formation and cell migration in cells of NSCLC. These results suggest that upregulated KLHL17 in NSCLC promotes tumor proliferation and migration by activating Ras/MAPK pathway to increase expression of Rho A, cyclin D1, CDK4 and MMP2.
In conclusion, the present study demonstrates for the first time that KLHL17 is upregulated in NSCLC and that upregulated KLHL17 is associated with poor prognosis in patients with NSCLC. KLHL17 promotes tumor proliferation and migration in NSCLC by activating Ras/MAPK signaling pathway. The findings suggest that KLHL17 may be a novel therapeutic target for the treatment of NSCLC.
Data availability
The data that support the findings of this study are available from the corresponding author upon reasonable request.
References
Hong QY, Wu GM, Qian GS, Hu CP, Zhou JY, Chen LA, et al. Prevention and management of lung cancer in China. Cancer, 121 Suppl 17, 3080-8 (2015)
Sung H, Ferlay J, Siegel RL, Laversanne M, Soerjomataram I, Jemal A, et al. Global Cancer Statistics 2020: GLOBOCAN Estimates of Incidence and Mortality Worldwide for 36 Cancers in 185 Countries. CA Cancer J Clin, 71(3), 209-49 (2021)
Ji X, Bosse Y, Landi MT, Gui J, Xiao X, Qian D, et al. Identification of susceptibility pathways for the role of chromosome 15q25.1 in modifying lung cancer risk. Nat Commun, 9(1), 3221 (2018)
Wang M, Herbst RS, Boshoff C. Toward personalized treatment approaches for non-small-cell lung cancer. Nat Med, 27(8), 1345-56 (2021)
Siegel RL, Miller KD, Jemal A. Cancer Statistics, 2017. CA Cancer J Clin, 67(1), 7-30 (2017)
Hassanein SS, Abdel-Mawgood AL, Ibrahim SA. EGFR-Dependent Extracellular Matrix Protein Interactions Might Light a Candle in Cell Behavior of Non-Small Cell Lung Cancer. Front Oncol, 11, 766659 (2021)
Hassanein SS, Ibrahim SA, Abdel-Mawgood AL. Cell Behavior of Non-Small Cell Lung Cancer Is at EGFR and MicroRNAs Hands. Int J Mol Sci, 22(22), (2021)
Dhanoa BS, Cogliati T, Satish AG, Bruford EA, Friedman JS. Update on the Kelch-like (KLHL) gene family. Hum Genomics, 7, 13 (2013)
Hu H-T, Huang T-N, Hsueh Y-P. KLHL17/Actinfilin, a brain-specific gene associated with infantile spasms and autism, regulates dendritic spine enlargement. J Biomed Sci, 27(1), 103 (2020)
Kang MI, Kobayashi A, Wakabayashi N, Kim SG, Yamamoto M. Scaffolding of Keap1 to the actin cytoskeleton controls the function of Nrf2 as key regulator of cytoprotective phase 2 genes. Proc Natl Acad Sci U S A, 101(7), 2046-51 (2004)
Minor DL, Lin YF, Mobley BC, Avelar A, Jan YN, Jan LY, et al. The polar T1 interface is linked to conformational changes that open the voltage-gated potassium channel. Cell, 102(5), 657-70 (2000)
Melnick A, Ahmad KF, Arai S, Polinger A, Ball H, Borden KL, et al. In-depth mutational analysis of the promyelocytic leukemia zinc finger BTB/POZ domain reveals motifs and residues required for biological and transcriptional functions. Mol Cell Biol, 20(17), 6550-67 (2000)
Furukawa M, He YJ, Borchers C, Xiong Y. Targeting of protein ubiquitination by BTB-Cullin 3-Roc1 ubiquitin ligases. Nat Cell Biol, 5(11), 1001-7 (2003)
Xu L, Wei Y, Reboul J, Vaglio P, Shin TH, Vidal M, et al. BTB proteins are substrate-specific adaptors in an SCF-like modular ubiquitin ligase containing CUL-3. Nature, 425(6955), 316-21 (2003)
Adams J, Kelso R, Cooley L. The kelch repeat superfamily of proteins: propellers of cell function. Trends Cell Biol, 10(1), 17-24 (2000)
Xu Y, Wang C, Jiang X, Zhang Y, Su H, Jiang J, et al. KLHL38 involvement in non-small cell lung cancer progression via activation of the Akt signaling pathway. Cell Death Dis, 12(6), 556 (2021)
Jiang X, Xu Y, Ren H, Jiang J, Wudu M, Wang Q, et al. KLHL18 inhibits the proliferation, migration, and invasion of non-small cell lung cancer by inhibiting PI3K/PD-L1 axis activity. Cell Biosci, 10(1), 139 (2020)
Titus AJ, Way GP, Johnson KC, Christensen BC. Deconvolution of DNA methylation identifies differentially methylated gene regions on 1p36 across breast cancer subtypes. Sci Rep, 7(1), 11594 (2017)
Zheng X, Xu H, Yi X, Zhang T, Wei Q, Li H, et al. Tumor-antigens and immune landscapes identification for prostate adenocarcinoma mRNA vaccine. Mol Cancer, 20(1), 160 (2021)
Chae HS, Gil M, Saha SK, Kwak HJ, Park HW, Vellingiri B, et al. Sestrin2 Expression Has Regulatory Properties and Prognostic Value in Lung Cancer. J Pers Med, 10(3), (2020)
Zhou H, Cai L, Zhang X, Li A, Miao Y, Li Q, et al. ARHGEF39 promotes tumor progression via activation of Rac1/P38 MAPK/ATF2 signaling and predicts poor prognosis in non-small cell lung cancer patients. Lab Invest, 98(5), 670-81 (2018)
Zhang X, Luo Y, Li Q. TMED3 Promotes Proliferation and Migration in Breast Cancer Cells by Activating Wnt/beta-Catenin Signaling. Onco Targets Ther, 13, 5819-30 (2020)
Park JH, Han HJ. Caveolin-1 plays important role in EGF-induced migration and proliferation of mouse embryonic stem cells: involvement of PI3K/Akt and ERK. Am J Physiol Cell Physiol, 297(4), C935-44 (2009)
Xiang S, Shi X, Chen P, Chen Y, Bing S, Jin X, et al. Targeting Cul3-scaffold E3 ligase complex via KLHL substrate adaptors for cancer therapy. Pharmacol Res, 169, 105616 (2021)
Canning P, Cooper CDO, Krojer T, Murray JW, Pike ACW, Chaikuad A, et al. Structural basis for Cul3 protein assembly with the BTB-Kelch family of E3 ubiquitin ligases. J Biol Chem, 288(11), 7803-14 (2013)
Shi X, Xiang S, Cao J, Zhu H, Yang B, He Q, et al. Kelch-like proteins: Physiological functions and relationships with diseases. Pharmacol Res, 148, 104404 (2019)
Lin Z, Li S, Feng C, Yang S, Wang H, Ma D, et al. Stabilizing mutations of KLHL24 ubiquitin ligase cause loss of keratin 14 and human skin fragility. Nat Genet, 48(12), 1508-16 (2016)
Chen J, Ou Y, Yang Y, Li W, Xu Y, Xie Y, et al. KLHL22 activates amino-acid-dependent mTORC1 signalling to promote tumorigenesis and ageing. Nature, 557(7706), 585-9 (2018)
Chen JC, Alvarez MJ, Talos F, Dhruv H, Rieckhof GE, Iyer A, et al. Identification of causal genetic drivers of human disease through systems-level analysis of regulatory networks. Cell, 159(2), 402-14 (2014)
Yuan W-C, Lee Y-R, Huang S-F, Lin Y-M, Chen T-Y, Chung H-C, et al. A Cullin3-KLHL20 Ubiquitin ligase-dependent pathway targets PML to potentiate HIF-1 signaling and prostate cancer progression. Cancer Cell, 20(2), 214-28 (2011)
Liu XR, Wang W, Li HM. KLHL22 promotes malignant melanoma growth in vitro and in vivo by activating the PI3K/Akt/mTOR signaling pathway. Neoplasma, 67(5), 1106-13 (2020)
Han M, Yang HJ, Lin Q. KLHL14, an ovarian and endometrial-specific gene, is over-expressed in ovarian and endometrial cancer. Math Biosci Eng, 17(2), 1702-17 (2019)
Hanahan D, Weinberg RA. Hallmarks of cancer: the next generation. Cell, 144(5), 646-74 (2011)
Ward RA, Anderton MJ, Bethel P, Breed J, Cook C, Davies EJ, et al. Discovery of a Potent and Selective Oral Inhibitor of ERK1/2 (AZD0364) That Is Efficacious in Both Monotherapy and Combination Therapy in Models of Nonsmall Cell Lung Cancer (NSCLC). J Med Chem, 62(24), 11004-18 (2019)
Vicent S, López-Picazo JM, Toledo G, Lozano MD, Torre W, Garcia-Corchón C, et al. ERK1/2 is activated in non-small-cell lung cancer and associated with advanced tumours. Br J Cancer, 90(5), 1047-52 (2004)
Acknowledgements
We would like to thank Editage (www.editage.cn) for their English language editing service.
Funding
This study was supported by Shengjing Hospital of China Medical University and the First Hospital of China Medical University.
Author information
Authors and Affiliations
Contributions
ZL designed the study, conducted experiments, acquired and analyzed data, and wrote the manuscript. MZ, XJ, YZ, SZ, YX, HR, HS, and HW conducted the experiments and acquired data. XQ was responsible for the conception and supervision of the study and wrote the manuscript. All authors corrected drafts and approved the final version of the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval and consent to participate
This research was approved by the Human Research Ethics Committee of China Medical University, which is accredited by the National Council on Ethics in Human Research.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Liu, Z., Zhao, M., Jiang, X. et al. Upregulation of KLHL17 promotes the proliferation and migration of non-small cell lung cancer by activating the Ras/MAPK signaling pathway. Lab Invest 102, 1389–1399 (2022). https://doi.org/10.1038/s41374-022-00806-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41374-022-00806-7
This article is cited by
-
Cordyceps sinensis relieves non-small cell lung cancer by inhibiting the MAPK pathway
Chinese Medicine (2024)
-
Routine radiology-pathology concordance evaluation of CT-guided percutaneous lung biopsies increases the number of cancers identified
European Radiology (2023)
-
Fer-mediated activation of the Ras-MAPK signaling pathway drives the proliferation, migration, and invasion of endometrial carcinoma cells
Molecular and Cellular Biochemistry (2023)