Abstract
Endothelial barrier disruption is a hallmark of tissue injury, edema, and inflammation. Vascular endothelial cells express the G protein-coupled receptor (GPCR) protease acctivated receptor 1 (PAR1) and the ion channel transient receptor potential vanilloid 4 (TRPV4), and these signaling proteins are known to respond to inflammatory conditions and promote edema through remodeling of cell–cell junctions and modulation of endothelial barriers. It has previously been established that signaling initiated by the related protease activated receptor 2 (PAR2) is enhanced by TRPV4 in sensory neurons and that this functional interaction plays a critical role in the development of neurogenic inflammation and nociception. Here, we investigated the PAR1–TRPV4 axis, to determine if TRPV4 plays a similar role in the control of edema mediated by thrombin-induced signaling. Using Evans Blue permeation and retention as an indication of increased vascular permeability in vivo, we showed that TRPV4 contributes to PAR1-induced vascular hyperpermeability in the airways and upper gastrointestinal tract of mice. TRPV4 contributes to sustained PAR1-induced Ca2+ signaling in recombinant cell systems and to PAR1-dependent endothelial junction remodeling in vitro. This study supports the role of GPCR–TRP channel functional interactions in inflammatory-associated changes to vascular function and indicates that TRPV4 is a signaling effector for multiple PAR family members.
Similar content being viewed by others
Introduction
The microvasculature provides important homeostatic functions including the exchange of gas, fluid, and micro- or macro-molecules from the circulation to the interstitial space and surrounding tissues. As the main component of this vascular barrier, endothelial cells regulate blood flow, fluidity, perfusion, as well as vascular permeability. Dysfunction of the endothelium can result in a loss of barrier integrity, prolonged hyperpermeability, and unregulated fluid extravasation, leading to edema and inflammation [1, 2].
Inflammatory signaling in endothelial cells is regulated by a variety of mediators, including the serine proteases thrombin and trypsin. These proteases can bind and cleave the amino terminal sequence of specific G protein-coupled receptors (GPCRs) known as protease-activated receptors (PARs). This is a unique activation mechanism for GPCRs and once cleaved, the newly exposed N-terminus functions as a tethered ligand that can rapidly engage with, and activate the receptor [3, 4]. Furthermore, the N-terminus of these receptors has also evolved to contain recognition and cleavage sequences for multiple proteases, and cleavage at distinct sites can promote a range of signaling outcomes [5]. Endothelial cells express all four PAR family subtypes (PAR1–PAR4), and these receptors play roles in maintaining vascular homeostasis through promoting adhesion, chemotaxis, coagulation, proliferation, and excretion of cytokines [6]. The proteolytic cleavage of PAR1 by thrombin mediates thrombosis in the coagulation pathway [7]. In addition, PAR1 activation can lead to increased vascular permeability in response to injury and inflammation. This occurs through phosphorylation of myosin light chain proteins, leading to cytoskeletal contraction, junctional remodeling, and disruption of the endothelial barrier [8].
Transient receptor potential (TRP) ion channels are expressed by a variety of cell types including endothelial and smooth muscle cells and contribute to signaling pathways that regulate vasculature processes, by promoting rapid cellular uptake of divalent cations, including Ca2+. The TRP Vanilloid 4 (TRPV4) ion channel, for example, is a polymodal protein that can respond to changes in thermal, chemical, and mechanical stimuli such as shear stress and osmotic pressure [9]. TRPV4 is expressed by endothelial and vascular smooth muscle cells, and regulates vascular tone, cytoskeletal architecture, and junctional remodeling of endothelial barriers [10,11,12].
GPCRs including PARs can indirectly activate and sensitize TRP channels by upregulating intracellular signaling pathways that lead to increased phosphorylation, to ultimately lower TRP channel activation thresholds. This GPCR–TRP transactivation axis plays a pivotal role in sensory neuron signaling processes to regulate pain, itch, cough, and inflammation [13]. For example, PAR2-mediated sensitization of TRPV4 has been implicated in hyperalgesia [14], inflammation [15], and edema [16]. Given the overlap in downstream signaling pathways mediated by PARs, TRPV4 may also act as a downstream mediator of vascular tone through PAR1-dependent transactivation, either directly, or via the activity of growth factor receptors [17]. Given that PAR1 and TRPV4 both perform critical functions in the vasculature, we investigated whether PAR1–TRPV4 functional interactions are involved in the regulation of endothelial barrier integrity and vascular permeability. Focusing on isolated airway and gastrointestinal (GI) tissues, our data support a role for TRPV4 as a facilitator of PAR1-dependent vascular endothelial barrier permeability.
Experimental procedures
Mice
Wild Type C57Bl/6J, TRPV4−/−, and littermate control mice (6–12 weeks) were obtained from Animal Resources Centre (Canning Vale, WA), or were purpose-bred by the Monash Animal Research Platform, Monash University. All animals were maintained in a temperature-controlled environment with a 12 h light/dark cycle and free access to food and water. All animal experiments are reported in accordance with the ARRIVE guidelines [18]. This study was approved by the respective Animal Ethics Committees of RMIT and Monash Institute of Pharmaceutical Sciences.
Reagents
Reagents were obtained from the following suppliers: Evans Blue dye, TFLLR-NH2, bovine plasma thrombin, tetracycline hydrochloride, poly-L-lysine, and GSK1016790A were purchased from Sigma-Aldrich (Castle Hill, Australia); Fura2-AM was purchased from (ThermoFisher Scientific, Scoresby, Victoria). Vorapaxar (SCH-530348) was purchased from Axon Medchem (Groningen, The Netherlands) and HC067047 was purchased from Tocris Bioscience (Bristol, UK).
Evans Blue extravasation
Mice were anesthetized with a combination of ketamine (100 mg/kg i.p.) and xylazine (10 mg/kg i.p.) and kept on a warming pad throughout the experiment. The skin on the neck was then removed to expose the jugular veins. Substances were administered i.v. by passing the injection needle through the pectoralis major muscle to prevent bleeding on withdrawal. Evans Blue dye (20 mg/kg) was administered via the jugular vein 1 min before injection of agonist (0.03–1 mg/kg GSK1016790A or 3 µmol/kg TFLLR) or vehicle (0.9% saline or 1% DMSO in 0.9% saline). The TRPV4-selective antagonist (0.1–10 mg/kg HC067047) was injected i.p. (prepared in 1% DMSO/0.9% saline) 60 min prior to anesthetics, Evans Blue and agonist administration. After 5 min post-agonist injection, the animal was exsanguinated, and the systemic circulation perfused with 0.9% saline to remove all remaining blood and dye. Tissue samples were collected, weighed, and placed immediately in 0.2 ml formamide. The airways were removed en bloc, before being separated. Lung parenchyma was removed from the bronchi and intrapulmonary airways (IPA). Tissues were then incubated in formamide (≥18 h at 37 °C) to facilitate dye extraction. Absorbance of the resulting extracts was determined against standard concentrations of Evans Blue at 620 nm using a CLARIOstar® microplate reader (BMG Labtech, Ortenberg, Germany). Results were expressed as the mass of Evans Blue dye relative to tissue mass (ng/mg of wet weight tissue).
Cell lines
Human Embryonic Kidney 293 (HEK293) cell lines stably expressing wildtype human TRPV4 (hTRPV4) were generated using a tetracycline-inducible system as previously described [15]. Briefly, Flp-InTM T-RexTM HEK293 cells (ThermoFisher Scientific) were transfected with pcDNA5/FRT/TO containing hTRPV4 (TRPV4-HEK). TRPV4-HEK were grown in Dulbecco’s Modified Eagle’s Medium (DMEM, ThermoFisher Scientific) containing 10% tetracycline-free fetal bovine serum (FBS), blasticidin (5 µg/ml), and hygromycin (100 µg/ml). Non-transfected control HEK293 cells (NT-HEK) were grown under the same conditions, but without hygromycin. HUVEC were grown in endothelial growth medium (EGM, Lonza) containing 2% FBS.
Intracellular Ca2+ assay
TRPV4-HEK and NT-HEK were seeded onto poly-L-lysine (100 µg/ml) coated 96-well plates (60,000 cells/well) and cultured for 48 h. Wildtype and TRPV4 HEK cells were treated with tetracycline (1 µg/ml) for 4 h to induce TRPV4 expression. NT-HEK were treated with the same tetracycline induction conditions. HUVEC were seeded onto non-coated 96-well plates (15,000 cells/well) and cultured for 48 h. Cells were loaded with Fura2-AM ester (2.5 µM) in HBSS containing probenecid (2 mM) and pluronic acid (0.5 µM) (pH 7.4, 37 °C, 45–60 min). Fluorescence was measured at 340/380 nm excitation and 510 nm emission wavelengths using a FlexStation 3 plate reader (Molecular Devices, Sunnyvale, CA) as previously described [19]. Fluorescence was recorded for 15 s prior to compound addition to establish a baseline reading. Agonist and antagonist treatments are indicated in results and data were expressed as the 340/380 nm fluorescence ratio, to determine fluctuations in free intracellular calcium ([Ca2+]i).
Immunofluorescence
Human umbilical vein endothelial cells (HUVEC) were seeded on glass coverslips coated with Matrigel (1:10 dilution, Corning). Once cells formed a confluent monolayer, they were treated as described in the results. Media was then removed and HUVEC were washed with PBS before fixation (4% paraformaldehyde, 15 min). HUVEC were washed (3 × 10 min PBS) then incubated in permeabilization/blocking buffer (5% normal horse serum in PBS containing 0.1% sodium azide and 0.1% saponin) for 1 h at room temperature (RT). Cells were incubated with a polyclonal anti-VE-cadherin antibody (rabbit, #ab33168, Abcam RRID:AB_870662, 1:400) in blocking buffer overnight at 4 °C. Cells were then washed (3× PBS) and incubated with secondary antibody (donkey anti-rabbit Alexa594, 1:500; ThermoFisher) and phalloidin Alexa488 (1:1,000; Abcam) in PBS for 2 h at RT. Nuclei were detected with Hoechst 33342 (1:2,000; ThermoFisher; 10 min at RT). Coverslips were mounted using ProLong Diamond Antifade Mountant (ThermoFisher) and images were captured on a Leica TCS-SP8 confocal system as described [20] using an HC PLAN APO 1.4 NA 63× oil objective. Three regions for each treatment were captured at 16-bit depth and 1024 × 1024-pixel resolution in four independent experiments.
Transwell permeability assay
HUVEC were seeded on non-coated Transwell inserts (6.5 mm diameter, 0.4 µm pore size, Corning, Mulgrave, Victoria) and grown for up to 72 h, until a HUVEC confluent monolayer had been achieved. Cells were then treated with antagonists (as indicated in results) in serum-free cell culture media, followed by co-addition of agonist and FITC-labeled dextran (100 µg/ml, average MW = 70 kDa, Sigma-Aldrich) to the Transwell insert. After 30 min, 100 µL samples from the bottom chamber of the Transwell system were removed and FITC fluorescence was measured (excitation/emission wavelengths 492/520 nm) in a CLARIOstar® microplate reader. Results were expressed as fluorescence intensity normalized to the vehicle control treatment group (0.1% DMSO).
Statistical analysis
A p value of < 0.05 was considered to be significantly different to the null hypothesis of no difference in means at the 95% confidence level. All treatments comparing three or more variables were analyzed using one-way ANOVA with Sidak’s multiple comparison tests. Comparisons of two variables were analyzed using an unpaired Student’s t test. For cell-based assays, sigmoidal curves were fitted to agonist concentration responses. Due to the higher baseline fluorescence (F340/F380 ratio) observed in TRPV4-HEK compared with NT-HEK cells, agonist peaks and coupling analysis were determined based on normalized data by subtracting the baseline fluorescence (average fluorescence from 0–15 s).
Results
Activation of TRPV4-induced vascular hyperpermeability in the airways and upper GI tract
To assess the effect of TRPV4 activation on vascular permeability, we examined the tissue distribution of Evans Blue dye in mice following the administration of the selective TRPV4 agonist GSK1016790A (GSK101). GSK101 elicited dose-dependent extravasation of Evans Blue in the airways (lung parenchyma, bronchi, IPA, and trachea) and upper GI tract (esophagus and stomach) (Fig. 1a). To further confirm that the GSK101-induced vascular hyperpermeability was TRPV4 specific, animals received increasing doses of the TRPV4-selective antagonist HC067047 (HC06; 0.1, 1, or 10 mg/kg) 60 min prior to Evans Blue and a moderate dose of GSK101 (0.1 mg/kg). Comparison of dye retention in these tissues reveals a HC06 dose-dependent reduction in GSK101-induced vascular hyperpermeability (Fig. 1b).
a Vascular hyperpermeability assessed by presence of Evans Blue in tissue, following i.v. administration of increasing doses of TRPV4 agonist GSK101, relative to control treatment (Veh, 1% DMSO in 0.9% saline). b Inhibition of TRPV4-mediated, GSK101-dependent Evans Blue permeability by co-administration of GSK101 (0.1 mg/kg) with increasing doses of TRPV4 antagonist, HC067047 (HC06, concentrations indicated on x-axes), or by co-administration of HC06 (10 mg/kg) with vehicle control. Each data point represents a measurement from the indicated tissue, harvested from an individual animal. Column graphs represent mean ± s.e.m., n = 7–9. *, #p< 0.05; **, ##p < 0.01; ***, ###p < 0.001; ****, ####p < 0.0001; one-way ANOVA with Sidak’s multiple comparisons test, comparing treatments to Vehicle only control (*) or relative to GSK101 only control (#).
TRPV4 mediates PAR1-induced vascular hyperpermeability in the airways and upper GI tract
We have previously demonstrated that TRPV4 promotes PAR2-dependent signaling and edema [15]. We therefore investigated whether TRPV4 plays a similar role in PAR1-induced hyperpermeability. To confirm that activation of PAR1 leads to vascular hyperpermeability, we administered the PAR1-selective activating peptide TFLLR-NH2 (TFLLR), using the same mouse model. Relative to the canonical protease thrombin, which activates PAR1 as well as other PARs and extracellular proteins [3], the perfusion of free peptide agonist TFLLR was chosen due to its selectivity for the receptor. TFLLR-treated (3 µmol/kg) mice also exhibited significant Evans Blue retention compared with the vehicle control in the same tissues, as demonstrated by a mean 1.68-fold dye uptake increase in airway tissue, and 2.34-fold increase in upper GI tissue and jejunum (Fig. 2).
Evans Blue retention measured in regions involved in the airways (a) or upper GI tract and jejunum (b). Animals were treated with vehicle alone, HC06 (10 mg/kg) with Vehicle (0.9% saline) or HC06 with TFLLR PAR1 agonist peptide (3 µmol/kg). Each data point represents a measurement from an individual animal, column graphs represent mean ± s.e.m., n = 6–11. *, #p < 0.05; **, ##p < 0.01; ***, ###p < 0.001; ****, ####p < 0.0001; two-way ANOVA with Sidak’s multiple comparisons test; relative to vehicle only control (*) or vehicle + TFLLR treatment (#).
To assess a potential role for TRPV4 in PAR1-mediated hyperpermeability, TRPV4 function was blocked either pharmacologically (Fig. 2) or by genetic ablation (Fig. 3). PAR1-induced vascular hyperpermeability in the airways and upper GI tract were reversed by pretreatment with HC06 (10 mg/kg) (Fig. 2). Furthermore, comparable inhibition of TFLLR-induced Evans Blue retention was observed when examined in TRPV4−/− mice (Fig. 3). HC06 alone did not reduce Evans Blue retention relative to the vehicle control, thus indicating that the antagonist reduced vascular hyperpermeability specifically following PAR1 activation. Similarly, there was no basal difference in dye retention in TRPV4−/− mice compared with wild type controls.
Evans Blue retention measured in regions involved in the airways (a–c) or upper GI tract and jejunum (d–f). Wildtype or TRPV4−/− mice were treated with vehicle alone or with the PAR1 agonist peptide TFLLR (3 µmol/kg). Each data point represents a measurement from an individual animal, column graphs represent mean ± s.e.m., n = 5–6. *, #p < 0.05; **, ##p < 0.01; two-way ANOVA with Sidak’s multiple comparisons test; relative to Vehicle only control (*) or Vehicle + TFLLR treatment (#).
TRPV4 promotes sustained Ca2+ responses following PAR1 activation
TRPV4 has previously been reported to enhance the duration and magnitude of PAR2-dependent Ca2+ signaling in immortalized cells and has also been associated with enhanced edema in an acute model of inflammation [15]. Consistent with this, PAR1-dependent disruption of the endothelial barrier also has the potential to involve rapid changes in free intracellular Ca2+ ([Ca2+]i) levels and can be readily investigated in cells co-expressing PAR1 and TRPV4. Utilizing stable TRPV4-HEK cells and non-transfected control HEK cells (NT-HEK) that endogenously express human PAR1, the temporal Ca2+ profiles were compared for responses to PAR1 activation with the TFLLR peptide or canonical protease, thrombin (Fig. 4). In control NT-HEK cells, PAR1 stimulation with thrombin (3 U/ml) or TFLLR (30 µM) resulted in a rapid transient [Ca2+]i mobilization, consistent with activation of Gαq-mediated pathways, and returned to basal levels within 40 s post stimulation (Fig. 4a, b). In contrast, the equivalent treatment in TRPV4-HEK cells resulted in a rapid and relatively more sustained elevation in [Ca2+]i. This observation was consistent with the nonlinear regression curves (80 s post stimulation) of Ca2+ responses from different TFLLR and thrombin concentrations. The concentration response curves, determined by plotting peak responses, showed no significant difference between the two agonists (Fig. 4c, d), whereas those based on area under the curve (AUC) indicated that TRPV4 promotes a significant increase in sustained Ca2+ flux (Fig. 4e, f). Together, these data suggest that TRPV4 activity does not affect the maximum transient Ca2+ release from intracellular stores, but does contribute to the global PAR1-mediated Ca2+ response in transfected HEK cells.
[Ca2+]i was measured in NT-HEK (control) or TRPV4-HEK cells, that both endogenously express PAR1. a, b Time course of effects of thrombin (3 U/ml) and TFLLR peptide (30 μM) on both cell types. c, d Effects of graded concentrations of thrombin and TFLLR on the maximal Ca2+ response, to determine the contribution of TRPV4 to PAR1-mediated transient Ca2+-mobilization from intracellular stores. e, f Effects of graded concentrations of thrombin and TFLLR on the total Ca2+ response (AUC, 60 s post stimulation) to reveal the contribution of TRPV4 to sustained PAR1-mediated Ca2+ signaling. Data are presented as mean ± s.e.m., n = 5–6.
TRPV4 contributes to PAR1-induced endothelial hyperpermeability in HUVEC
The roles of PAR1 and TRPV4 in Ca2+ signaling and permeability were subsequently examined in HUVEC, a well characterized and commonly used cell model system representative of signaling responses in the vasculature. Stimulation of HUVEC with either GSK101 or TFLLR caused a concentration-dependent increase in [Ca2+]i, thus demonstrating that TRPV4 and PAR1 are both endogenously expressed and functional in these cells. The time traces of [Ca2+]i show that TRPV4 activation resulted in a sustained response, while PAR1 activation resulted in a transient Ca2+ response, which is characteristic for Gαq coupled responses (Fig. 5a, c). To determine whether PAR1 sensitizes TRPV4, HUVEC pretreated with TFLLR 15 min prior, were stimulated with GSK101 (Fig. 5a). The leftwards shift of the curve was positively associated with TFLLR concentration, suggesting that activation of PAR1 sensitizes TRPV4, particularly at lower GSK101 concentrations (Fig. 5b). To determine the relative contribution of TRPV4 activity to PAR1-mediated responses, cells were pretreated with vehicle, the selective PAR1 antagonist Vorapaxar, (VPX, 100 nM) or the TRPV4 antagonist HC06 (1 µM), followed by stimulation with increasing concentrations of TFLLR (Fig. 5c). By comparing the total Ca2+ response (AUC, 130 s post stimulation), these TFLLR-evoked Ca2+ responses in HUVEC were abolished in the presence of VPX, but were unaffected by TRPV4 inhibition (Fig. 5d). Similarly, HC06 did not have a significant effect on the sustained phase of the PAR1-mediated calcium responses (Fig. 5c). It is possible that the differences in TRPV4 contribution to PAR1 signaling in HUVEC and NT-HEK results from variations in receptor quantity or compensatory mechanisms originating from cell type-specific differences.
a Time trace of TRPV4 agonist GSK101 (3 nM) pretreated with three different concentrations of PAR1 agonist TFLLR. b Effect of graded concentrations of GSK101 (AUC) following pretreatment with TFLLR demonstrated the functional presence of TRPV4 in HUVEC, and indicated that TFLLR induces a leftwards shift in the GSK101 curve. c Time trace of TFLLR following pretreatment of cells with the TRPV4 antagonist HC06 or the PAR1 antagonist VPX. d Graded concentrations of TFLLR following treatment with vehicle, HC06 or VPX (AUC) confirmed a role for functional TRPV4 and PAR1 in the TFLLR Ca2+ response. Calcium signaling data are presented as mean ± s.e.m., n = 6–7.To determine the role of TRPV4 and PAR1 in endothelial permeability, the passage of a fluorescent reporter dye (FITC-Dextran) was measured across confluent HUVEC monolayers grown on a porous membrane. e Stimulation with vehicle or GSK101 (3 nM, 30 min) was used to confirm a role for TRPV4 activity in HUVEC permeability, which was significantly reduced following pretreatment with HC06. f Stimulation with vehicle or TFLLR (10 µM, 30 min) was used to confirm a role for PAR1 in HUVEC permeability. Effect of pretreatment with HC06 (10 µM, 60 min) and VPX (100 nM, 60 min) reveals a role for TRPV4 in the TFLLR-induced hyperpermeability and confirms that TFLLR is mediating effects selectively via PAR1, respectively. Column graphs for permeability data represent mean ± s.e.m., n = 6–8. *, #p < 0.05; **p < 0.01; ****, ####p < 0.0001; one-way ANOVA with Sidak’s multiple comparison tests; relative to the vehicle only control (*), vehicle + GSK101 (e) or vehicle + TFLLR (f) (#).
Evans Blue studies in animals indicated that TRPV4 may be functionally important for promoting PAR1-mediated changes in vascular permeability (Figs. 2, 3). To investigate whether the Ca2+ signals match functional responses as well as the influence of PAR1 and TRPV4 on endothelial permeability in vitro, PAR1 and TRPV4-mediated HUVEC permeability was assessed by growing cells to confluence on Transwell® porous membrane inserts followed by measurement of FITC-labeled dextran (fluorescent macromolecule reporter) transfer from the upper insert to the bottom chamber. Activation of TRPV4 (GSK101, 3 nM) significantly increased permeability of FITC-dextran (100 µg/ml; 70 kDa) across the monolayer relative to vehicle treatment (4.1-fold increase in FITC intensity), thus suggesting that TRPV4 signaling can promote junctional changes in endothelia. To further demonstrate a functional role for TRPV4 in modulating barrier integrity, GSK101-mediated FITC-dextran permeation was abolished in cells pretreated with HC06 (Fig. 5e). PAR1 activation (TFLLR, 10 µM) also increased permeability of FITC-dextran relative to vehicle treatment (4.02-fold increase), and this was blocked by 30 min pretreatment with Vorapaxar (100 nM), a potent PAR1-selective competitive antagonist of TFLLR. To investigate the contribution of TRPV4 in PAR1-mediated permeability, cells were pretreated for 30 min with the TRPV4 antagonist HC06 (1 µM). This resulted in a significant reduction in TFLLR-mediated FITC-dextran permeability (2.6-fold increase relative to vehicle, Fig. 5f). Together, these observations demonstrate that TRPV4 contributes to PAR1-stimulated signaling and vascular permeability, but are not essential for PAR1-mediated Ca2+ mobilization. While further studies are required to understand the precise cell signaling pathways involved, these data support a role for Gαq-mediated signaling for PAR1–TRPV4 functional interactions in HEK cells, and Gαq-independent signaling processes to modulate barrier integrity in endothelial cells.
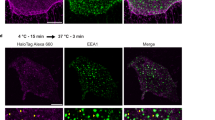
To further support these endothelial monolayer permeability studies, cell–cell junction integrity was also assessed by fluorescence imaging. Cells were treated, fixed and stained to reveal the localization of the endothelial junctional protein VE-cadherin, the actin cytoskeleton, and nucleus. Consistent with previous studies [21], PAR1 activation for 30 min induced a destabilization of cell–cell junctions, shown by elongation of adherens junctions and presence of inter-endothelial gaps, when compared with vehicle treatment. Pretreatment with the TRPV4 antagonist HC06 prevented the TFLLR-induced extension of adherens junctions, but did not prevent the presence of gaps (Fig. 6). Consistent with the FITC-dextran permeability findings (Fig. 5b), TRPV4 inhibition reduces PAR1-mediated junction elongation and destabilization, and therefore supports a role for TRPV4 activity in the modulation of cell–cell junctions. However, the presence of TFLLR-induced inter-endothelial gaps with HC06 pretreatment suggests that PAR1-mediated junctional remodeling is also likely to be driven by TRPV4-independent signaling.
Confluent HUVEC were treated with TFLLR (10 µM) for 30 min after pretreatment with HC06 (1 µM, 1 h), or vehicle control. Cells were stained to reveal the localization of VE-cadherin (magenta), F-actin (green), and the nucleus (blue). Dashed boxes indicate a region of interest enlarged to show the localization and structure of VE-cadherin. Fluorescence intensity profiles correspond to dashed lines in ROI images. Scale bar, 20 µm. The images are representative of three regions from four independent experiments.
Discussion
PARs have evolved to respond to extracellular proteases to regulate diverse physiological and pathophysiological processes [4]. As the major receptor for the coagulation protease thrombin, PAR1 has been extensively studied for its role in hemostasis, platelet aggregation and immune cell chemotaxis, and is known to be a dynamic receptor that can initiate downstream signaling by coupling to the Gαq, Gα12/13, and Gαi protein subunits [4, 7, 22]. This diversity of PAR1-mediated signaling outcomes can be further modulated according to proteolytic activity. Specifically, protease-dependent cleavage at different sites within the N-terminus can reveal distinct tethered ligand sequences, and each of these tethered ligands favors activation of specific signaling processes to achieve unique physiological outcomes [5].
In addition to their well-characterized function in platelet activation, thrombin and PAR1 are known to control endothelial permeability via downstream modulation of junctional proteins that perform essential roles in barrier formations and cytoskeleton dynamics [4, 21]. PAR1 coupling to Gαq/11 and PLC-mediated release of intracellular calcium stores, for example, is required for the activation of myosin light chain kinase (MLCK), and when combined with Gα12/13-mediated RhoA activity, this leads to cytoskeletal contraction and post-translational modification of endothelial junction proteins such as VE-cadherin, p120-catenin, and β-catenin [23]. Sustained PAR1 activation promotes transient disruption of these protein complexes, leading to increased endothelial permeability and plasma extravasation.
Functional interactions between GPCRs and TRP channels have previously been explored in a variety of cell settings, and while many PAR1-mediated intracellular signaling networks have been revealed, the potential for PAR1 signaling to utilize TRP channels to achieve edema has not been explored in detail. TRPV4 was proposed to be a downstream effector of PAR1-stimulated signaling pathways due to its known functional interactions with the related receptor PAR2, in inflammatory pathways, and its central role in vascular processes [14,15,16]. Influx of Ca2+ through TRP channels can contribute to, or amplify edema-associated signaling pathways and indirectly modulate MLCK-dependent contraction of smooth muscle cells [24]. In physiological states, TRPV4 responds to mechanical stimuli (e.g., shear stress, membrane stretch) or the release of endogenous arachidonic lipid metabolites, to regulate endothelial homeostasis, vascular tone and endothelial orientation by regulating [Ca2+]i and nitric oxide synthase activity to promote niric oxide production [9, 25]. TRPV4 has also recently been shown to modulate phosphorylation and trafficking of vascular endothelial growth factor signaling via VEGF receptor-2 [26]. In environments where elevated or chronic TRPV4 activity is likely to occur, TRPV4-mediated increases in [Ca2+]i cause junctional and cytoskeletal reorganization [12] and previous findings have revealed that sustained activation of TRPV4 by intravenous administration of GSK101 can cause irreversible endothelial barrier disruption and circulatory collapse [27]. Hence, TRPV4 is proposed to be an important regulator of barrier function and a contributor to pathophysiological conditions where edema is observed and may therefore be a valuable therapeutic target. Indeed, orally active TRPV4 antagonists have previously been shown to effectively reverse pulmonary edema and associated pathologies, induced by high pulmonary venous pressure or myocardial infarction [28,29,30]. Furthermore, chronic treatment with a TRPV4 inhibitor in animal models did not affect osmoregulation or interfere with the activity of diuretics, which are often used as a therapy to help resolve edema in the clinic [30].
Thrombin and TFLLR-NH2 have previously been shown to increase vascular permeability in the pulmonary microvasculature, and jejunum of wild-type but not PAR1 knockout mice [31, 32]. To further explore the potential for TRPV4 to function as a downstream effector of thrombin-PAR1-induced edema, we explored Evans Blue uptake and retention in tissues of the airways and upper GI tract and supported these studies with in vitro characterization of endothelia. PAR1 or TRPV4 stimulation resulted in increased Evans Blue permeability in tissues associated with the airways and upper GI tract, as determined by Evans Blue uptake following intravenous administration of PAR1- and TRPV4-selective pharmacological agents, thus suggesting that the observed edema is endothelial-specific, yet may also affect smooth muscle cell layers. The importance of TRPV4-mediated signaling in PAR1-mediated vessel hyperpermeability of the airways and upper GI tract were supported with the use of the selective TRPV4 antagonist HC06 and in TRPV4−/− mice. Together, these data indicate that TRPV4 functions as a component of PAR1-mediated changes in vascular permeability, which is consistent with previous studies demonstrating a role for TRPV4 as a downstream effector of trypsin/PAR2-mediated edema [15].
Comparable TFLLR-stimulated changes in barrier integrity were also observed when measuring permeation of a fluorescent reporter across a porous membrane with a confluent endothelial cell monolayer. Consistent with these findings, thrombin and TFLLR have previously been shown to decrease trans-endothelial electrical resistance in a myosin light chain-dependent manner [33]. It was also noted that the FITC-dextran permeation was more effectively blocked by antagonism of PAR1 relative to pretreatment with a selective TRPV4 antagonist. This role for TRPV4 was also supported by immunofluorescence imaging, where PAR1 activation resulted in junctional remodeling in HUVEC monolayers, yet this destabilization effect was prevented by pharmacological inhibition of TRPV4 activity. VE-cadherin is the main component of adherens junctions between endothelial cells and plays a major role in the regulation of vascular permeability. Cadherins are calcium dependent proteins and the phosphorylation, internalization, and actin-mediated contraction of VE-cadherin are known to modulate permeability in endothelial cells [34,35,36]. While the mechanisms remain unclear, these data suggest that inhibition of TRPV4 Ca2+ influx is not sufficient for preventing PAR1-mediated junction destabilization, but may be necessary for PAR1 to achieve its complete signaling repertoire to promote sustained edema. Further, the observation that HC06 could more effectively prevent Evans Blue permeation and retention in animals suggests that TRPV4 may play additional roles in complex cell systems and indicates the potential for PAR1 signaling to promote TRPV4 activity through additional mechanisms in mice, including through localized production of lipid mediators or mechanical activation that may occur through PAR1-mediated processes [9, 21].
In conclusion, we have demonstrated that TRPV4 functionally contributes to PAR1 signaling in the airways, upper GI tract and endothelial monolayers. The findings of this study suggest that TRPV4 is a signaling effector for multiple PAR family members and while pharmacological inhibition of TRPV4 diminishes PAR1-induced hyperpermeability, it may also contribute to other PAR1-mediated signaling processes that require further investigation.
References
Esper RJ, Nordaby RA, Vilarino JO, Paragano A, Cacharrón JL, Machado RA. Endothelial dysfunction: a comprehensive appraisal. Cardiovasc Diabetol. 2006;5:4.
Pober JS, Sessa WC. Evolving functions of endothelial cells in inflammation. Nat Rev Immunol. 2007;7:803–15.
Coughlin SR. Thrombin signalling and protease-activated receptors. Nature. 2000;407:258–64.
Ossovskaya VS, Bunnett NW. Protease-activated receptors: contribution to physiology and disease. Physiol Rev. 2004;84:579–621.
Zhao P, Metcalf M, Bunnett NW. Biased signaling of protease-activated receptors. Front Endocrinol. 2014;5:67.
Soh UJ, Dores MR, Chen B, Trejo J. Signal transduction by protease-activated receptors. Br J Pharmacol. 2010;160:191–203.
Coughlin SR. Protease-activated receptors in hemostasis, thrombosis and vascular biology. J Thromb Haemost. 2005;3:1800–14.
Bogatcheva NV, Garcia JG, Verin AD. Molecular mechanisms of thrombin-induced endothelial cell permeability. Biochemistry. 2002;67:75–84.
White JP, Cibelli M, Urban L, Nilius B, McGeown JG, Nagy I. TRPV4: molecular conductor of a diverse orchestra. Physiol Rev. 2016;96:911–73.
Filosa JA, Yao X, Rath G. TRPV4 and the regulation of vascular tone. J Cardiovasc Pharmacol. 2013;61:113–9.
Mendoza SA, Fang J, Gutterman DD, Wilcox DA, Bubolz AH, Li R, et al. TRPV4-mediated endothelial Ca2+ influx and vasodilation in response to shear stress. Am J Physiol Heart Circ Physiol. 2010;298:H466–76.
Phuong TTT, Redmon SN, Yarishkin O, Winter JM, Li DY, Krizaj D. Calcium influx through TRPV4 channels modulates the adherens contacts between retinal microvascular endothelial cells. J Physiol. 2017;595:6869–85.
Veldhuis NA, Poole DP, Grace M, McIntyre P, Bunnett NW. The G protein-coupled receptor-transient receptor potential channel axis: molecular insights for targeting disorders of sensation and inflammation. Pharmacol Rev. 2015;67:36–73.
Grant AD, Cottrell GS, Amadesi S, Trevisani M, Nicoletti P, Materazzi S, et al. Protease-activated receptor 2 sensitizes the transient receptor potential vanilloid 4 ion channel to cause mechanical hyperalgesia in mice. J Physiol. 2007;578(Pt 3):715–33.
Poole DP, Amadesi S, Veldhuis NA, Abogadie FC, Lieu T, Darby W, et al. Protease-activated receptor 2 (PAR2) protein and transient receptor potential vanilloid 4 (TRPV4) protein coupling is required for sustained inflammatory signaling. J Biol Chem. 2013;288:5790–802.
Zhao P, Lieu T, Barlow N, Sostegni SH, Korbmacher C, et al. Neutrophil elastase activates protease-activated receptor-2 (PAR2) and transient receptor potential vanilloid 4 (TRPV4) to cause inflammation and pain. J Biol Chem. 2015;290:13875–87.
Saifeddine M, El-Daly M, Mihara K, Bunnett NW, McIntyre P, Altier C, et al. GPCR-mediated EGF receptor transactivation regulates TRPV4 action in the vasculature. Br J Pharmacol. 2015;172:2493–506.
McGrath JC, Drummond GB, McLachlan EM, Kilkenny C, Wainwright CL. Guidelines for reporting experiments involving animals: the ARRIVE guidelines. Br J Pharmacol. 2010;160:1573–6.
Veldhuis NA, Lew MJ, Abogadie FC, Poole DP, Jennings IE, Ivanusic JJ, et al. N-glycosylation determines ionic permeability and desensitization of the TRPV1 capsaicin receptor. J Biol Chem. 2012;287:21765–72.
Poole DP, Lieu T, Pelayo JC, Eriksson EM, Veldhuis NA, Bunnett NW. Inflammation-induced abnormalities in the subcellular localization and trafficking of the neurokinin 1 receptor in the enteric nervous system. Am J Physiol Gastrointest Liver Physiol. 2015;309:G248–59.
Timmerman I, Heemskerk N, Kroon J, Schaefer A, van Rijssel J, Hoogenboezem M, et al. A local VE-cadherin and Trio-based signaling complex stabilizes endothelial junctions through Rac1. J Cell Sci. 2015;128:3041–54.
Alberelli MA, De Candia E. Functional role of protease activated receptors in vascular biology. Vasc Pharmacol. 2014;62:72–81.
Thennes T, Mehta D. Heterotrimeric G proteins, focal adhesion kinase, and endothelial barrier function. Microvasc Res. 2012;83:31–44.
Earley S, Brayden JE. Transient receptor potential channels in the vasculature. Physiol Rev. 2015;95:645–90.
Earley S, Pauyo T, Drapp R, Tavares MJ, Liedtke W, Brayden JE. TRPV4-dependent dilation of peripheral resistance arteries influences arterial pressure. Am J Physiol Heart Circ Physiol. 2009;297:H1096–102.
Kanugula AK, Adapala RK, Midha P, Cappelli HC, Meszaros JG, Paruchuri S, et al. Novel noncanonical regulation of soluble VEGF/VEGFR2 signaling by mechanosensitive ion channel TRPV4. FASEB J. 2019;33:195–203.
Willette RN, Bao W, Nerurkar S, Yue TL, Doe CP, Stankus G, et al. Systemic activation of the transient receptor potential vanilloid subtype 4 channel causes endothelial failure and circulatory collapse: Part 2. J Pharmacol Exp Ther. 2008;326:443–52.
Balakrishna S, Song W, Achanta S, Doran SF, Liu B, Kaelberer MM, et al. TRPV4 inhibition counteracts edema and inflammation and improves pulmonary function and oxygen saturation in chemically induced acute lung injury. Am J Physiol Lung Cell Mol Physiol. 2014;307:16.
Huh D, Leslie DC, Matthews BD, Fraser JP, Jurek S, Hamilton GA, et al. A human disease model of drug toxicity-induced pulmonary edema in a lung-on-a-chip microdevice. Sci Transl Med. 2012;4:159ra147.
Thorneloe KS, Cheung M, Bao W, Alsaid H, Lenhard S, Jian MY, et al. An orally active TRPV4 channel blocker prevents and resolves pulmonary edema induced by heart failure. Sci Transl Med. 2012;4:159ra148.
de Garavilla L, Vergnolle N, Young SH, Ennes H, Steinhoff M, Ossovskaya VS, et al. Agonists of proteinase-activated receptor 1 induce plasma extravasation by a neurogenic mechanism. Br J Pharmacol. 2001;133:975–87.
Vogel SM, Gao X, Mehta D, Ye RD, John TA, Andrade-Gordon P, et al. Abrogation of thrombin-induced increase in pulmonary microvascular permeability in PAR-1 knockout mice. Physiol Genomics. 2000;4:137–45.
Hirano M, Hirano K. Myosin di-phosphorylation and peripheral actin bundle formation as initial events during endothelial barrier disruption. Sci Rep. 2016;6:20989.
Gavard J, Gutkind JS. VEGF controls endothelial-cell permeability by promoting the beta-arrestin-dependent endocytosis of VE-cadherin. Nat Cell Biol. 2006;8:1223–34.
Giannotta M, Trani M, Dejana E. VE-cadherin and endothelial adherens junctions: active guardians of vascular integrity. Dev Cell. 2013;26:441–54.
Dejana E, Orsenigo F, Lampugnani MG. The role of adherens junctions and VE-cadherin in the control of vascular permeability. J Cell Sci. 2008;121:2115–22.
Acknowledgements
The authors thank Dr Wolfgang Liedtke (Duke University) for providing TRPV4−/− mice.
Funding
Australian Research Council Centre of Excellence in Convergent Bio-Nano Science and Technology (NWB, TPD), NHMRC Australia 1046860 (PM, NWB), 1083480 (DPP).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The laboratories of NWB, DPP and NAV receive funding from Takeda Pharmaceuticals. The remaining authors declare no conflict of interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Peng, S., Grace, M.S., Gondin, A.B. et al. The transient receptor potential vanilloid 4 (TRPV4) ion channel mediates protease activated receptor 1 (PAR1)-induced vascular hyperpermeability. Lab Invest 100, 1057–1067 (2020). https://doi.org/10.1038/s41374-020-0430-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41374-020-0430-7
This article is cited by
-
Diversification of PAR signaling through receptor crosstalk
Cellular & Molecular Biology Letters (2022)
-
Serotonin-induced vascular permeability is mediated by transient receptor potential vanilloid 4 in the airways and upper gastrointestinal tract of mice
Laboratory Investigation (2021)