Abstract
Objective
Perinatal palliative care (PPC) is the coordinated application of palliative care principles to the care of families, fetuses and newborns with suspected life-limiting conditions. This approach relies on continuity of care that spans pregnancy, birth and beyond. The goal of this retrospective cohort study was to evaluate outcomes and PPC continuity in infants born to families who received PPC at a quaternary care pediatric hospital, and to identify targets to improve care continuity.
Study design
PPC patients seen between July 2018 and June 2021 were identified via local PPC registry. Demographic, outcome, and continuity data were gathered from the electronic medical record. Descriptive statistics were used to calculate the rate of postnatal palliative consult and infant mortality rates.
Results
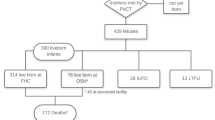
181 mother-infant dyads were identified as having a PPC consultation and had available data following birth. Overall perinatal mortality was 65%; 59.6% of all liveborn infants died prior to discharge. Only 47.6 % of liveborn infants, who did not die in the perinatal period, received postnatal palliative care. Location of birth (primary versus non-network hospital) was significantly associated with postnatal PPC consult rate (p = 0.007).
Conclusion
Continuation of palliative care after birth in families who received perinatal palliative care is inconsistently achieved. Creating reliable systems for PPC continuity will depend on location of care.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
Data availability
The dataset generated during and/or analyzed during the current study are not publically available due to concerns in maintaining private health data, but are available from corresponding author upon reasonable request.
References
Murphy SL, Xu J, Kochanek KD, Arias E, Tejada-Vera B. Deaths: Final Data for 2018. Natl Vital Stat Rep. 2021;69:1–83.
Care PP. ACOG committee opinion. Obstet Gynecol. 2019;134:e84–9.
Carter BS, Parravicini E, Benini F, Lago P. perinatal palliative care comes of age. Front Pediatr. 2021;9:555.
Benini F, Congedi S, Rusalen F, Cavicchiolo ME, Lago P. Barriers to perinatal palliative care consultation. Front Pediatr. 2020;8:590616.
Rocha Catania T, Stein Bernardes L, Guerra Benute GR, Bento Cicaroni Gibeli MA, Bertolassi do Nascimento N, Aparecida Barbosa TV, et al. When one knows a fetus is expected to die: palliative care in the context of prenatal diagnosis of fetal malformations. J Palliat Med. 2017;20:1020–31.
Tosello B, Dany L, Bétrémieux P, Le Coz P, Auquier P, Gire C, et al. Barriers in referring neonatal patients to perinatal palliative care: a French multicenter survey. PLoS ONE. 2015;10:e0126861.
Marc-Aurele KL, Hull AD, Jones MC, Pretorius DH. A fetal diagnostic center’s referral rate for perinatal palliative care. Ann Palliat Med. 2017;7:177–85.
Rogers MM, Friebert S, Williams CS, Humphrey L, Thienprayoon R, Klick JC. Pediatric palliative care programs in US hospitals. Pediatrics. 2021;148:e2020021634.
Tucker MH, Ellis K, Linebarger J. Outcomes following perinatal palliative care consultation: a retrospective review. J Perinatol. 2021;41:2196–200.
Quinn M, Gephart S. Evidence for implementation strategies to provide palliative care in the neonatal intensive care unit. Adv Neonatal Care. 2016;16:430–8.
Hancock HS, Pituch K, Uzark K, Bhat P, Fifer C, Silveira M, et al. A randomised trial of early palliative care for maternal stress in infants prenatally diagnosed with single-ventricle heart disease. Cardiol Young. 2018;28:561–70.
Thienprayoon R, Alessandrini E, Frimpong-Manso M, Grossoehme D. Defining provider-prioritized domains of quality in pediatric home-based hospice and palliative care: a study of the Ohio pediatric palliative care and end-of-life network. J Palliat Med. 2018;21:1414–35.
Thienprayoon R, San Julian Mark M, Grossoehme D. Provider-prioritized domains of quality in pediatric home-based hospice and palliative care: a study of the Ohio pediatric palliative care and end-of-life network. J Palliat Med. 2018;21:290–6.
Acknowledgements
The authors would like to acknowledge Drs. Lilli Ding and Qing Duan for their assistance with statistical modeling and data support. We would also like to acknowledge Dr. Jennifer Linebarger for her communication and willingness to share her team’s experiences.
Author information
Authors and Affiliations
Contributions
KN, HF, RT and BW conceptualized the initial project and design was further developed in coordination with ZF and SPL. ZF and SPL were responsible for primary data collection, analysis and writing the paper. HF, KN assisted with data collection. SPL was responsible for figure and table creation, paper editing, communication with journals and submission.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Farmer, Z.J., Palmaccio-Lawton, S.J., Flint, H.A. et al. Fetal outcomes and continuity in perinatal palliative care patients at a quaternary care pediatric hospital. J Perinatol 43, 889–894 (2023). https://doi.org/10.1038/s41372-023-01664-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-023-01664-x