Abstract
Objective
To compare the length of stay (LOS) against the expected date of delivery (EDD) and to describe mortality and LOS outcomes by gestational age (GA) categories over the years.
Study design
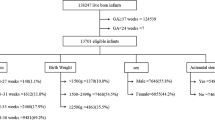
Healthcare Cost and Utilization Project Kids’ Inpatient database discharge records for years 2003, 2006, 2009, 2012, and 2016 were analyzed. For premature infants after inclusion–exclusion, actual, and calculated LOS were compared. Mortality and LOS outcomes were analyzed by GA and years.
Results
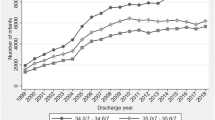
The majority (99%) of infants >28 weeks were discharged by EDD while, for neonate ≤28 weeks, about three-quarters (75%) of infants were discharged by calculated EDD. LOS is increasing while mortality is decreasing by GA categories in recent years.
Conclusions
This is the largest study of mortality and LOS in the United States. Our study provides evidence-based numbers comparing actual LOS against EDD, which can be used in perinatal settings to counsel parents.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Aly H, Hoffman H, El-Dib M, Said L, Mohamed M. Factor affecting length of stay in late preterm infants: an US national database study. J Matern Fetal Neonatal Med. 2015;28:598–604.
Hinchliffe SR, Seaton SE, Lambert PC, Draper ES, Field DJ, Manktelow BN. Modelling time to death or discharge in neonatal care: an application of competing risks. Paediatr Perinat Epidemiol. 2013;27:426–33.
Korvenranta E, Linna M, Hakkinen U, Peltola M, Andersson S, Gissler M, et al. Differences in the length of initial hospital stay in very preterm infants. Acta Paediatr. 2007;96:1416–20.
Mohamed MA, Nada A, Aly H. Day-by-day postnatal survival in very low birth weight infants. Pediatrics. 2010;126:e360–6.
Phibbs CS, Schmitt SK. Estimates of the cost and length of stay changes that can be attributed to one-week increases in gestational age for premature infants. Early Hum Dev. 2006;82:85–95.
Seaton SE, Barker L, Jenkins D, Draper ES, Abrams KR, Manktelow BN. What factors predict length of stay in a neonatal unit: a systematic review. BMJ Open. 2016;6:e010466.
Stoll BJ, Hansen NI, Bell EF, Shankaran S, Laptook AR, Walsh MC, et al. Neonatal outcomes of extremely preterm infants from the NICHD Neonatal Research Network. Pediatrics. 2010;126:443–56.
Stoll BJ, Hansen NI, Bell EF, Walsh MC, Carlo WA, Shankaran S, et al. Trends in care practices, morbidity, and mortality of extremely preterm neonates, 1993–2012. JAMA. 2015;314:1039–51.
Tyson JE, Parikh NA, Langer J, Green C, Higgins RD. Intensive care for extreme prematurity–moving beyond gestational age. N Engl J Med. 2008;358:1672–81.
Seaton SE, Barker L, Draper ES, Abrams KR, Modi N, Manktelow BN, et al. Estimating neonatal length of stay for babies born very preterm. Arch Dis Child Fetal Neonatal Ed. 2019;104:F182–F186.
Richardson DK, Corcoran JD, Escobar GJ, Lee SK. SNAP-II and SNAPPE-II: simplified newborn illness severity and mortality risk scores. J Pediatr. 2001;138:92–100.
Richardson DK, Gray JE, McCormick MC, Workman K, Goldmann DA. Score for Neonatal Acute Physiology: a physiologic severity index for neonatal intensive care. Pediatrics. 1993;91:617–23.
Author information
Authors and Affiliations
Contributions
JP did data analysis with help from JD. JP prepared an initial draft, which was revised based on feedback from MP, RK, LT, and JD.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Patel, J., Patel, M., Tucker, L. et al. Do most premature babies get discharged by the expected date of delivery?. J Perinatol 40, 798–805 (2020). https://doi.org/10.1038/s41372-020-0653-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-020-0653-x