Abstract
Background
Telomere length (TL) is a biomarker of genomic aging. The evidence on the association between TL and air pollution was inconsistent. Besides, the modification effect of genetic susceptibility on the air pollution-TL association remains unknown.
Objective
We aimed to evaluate the association of ambient air pollution with TL and further assess the modification effect of genetic susceptibility.
Methods
433,535 participants with complete data of TL and air pollutants in UK Biobank were included. Annual average exposure of NO2, NOx, PM10 and PM2.5 was estimated by applying land use regression models. Genetic risk score (GRS) was constructed using reported telomere-related SNPs. Leukocyte TL was measured by quantitative polymerase chain reaction (qPCR). Multivariable linear regression models were employed to conduct associational analyses.
Results
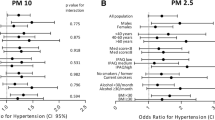
Categorical exposure models and RCS models both indicated U-shaped (for NO2 and NOx) and L-shaped (for PM10 and PM2.5) correlations between air pollution and TL. In comparison to the lowest quartile, the 2nd and 3rd quartile of NO2 (q2: −1.3% [−2.1%, −0.4%]; q3: −1.2% [−2.0%, −0.3%], NOx (q2: −1.3% [−2.1%, −0.5%]; q3: −1.4% [−2.2%, −0.5%]), PM2.5 (q2: −0.8% [−1.7%, 0.0%]; q3: −1.3% [−2.2%, −0.5%]), and the third quartile of PM10 (q3: −1.1% [−1.9%, −0.2%]) were inversely associated with TL. The highest quartile of NO2 was positively correlated with TL (q4: 1.0% [0.0%, 2.0%]), whereas the negative correlation between the highest quartile of other pollutants and TL was also attenuated and no longer significant. In the genetic analyses, synergistic interactions were observed between the 4th quartile of three air pollutants (NO2, NOx, and PM2.5) and genetic risk.
Impact statement
Our study for the first time revealed a non-linear trend for the association between air pollution and telomere length. The genetic analyses suggested synergistic interactions between air pollution and genetic risk on the air pollution-TL association. These findings may shed new light on air pollution’s health effects, offer suggestions for identifying at-risk individuals, and provide hints regarding further investigation into gene-environment interactions.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 6 print issues and online access
$259.00 per year
only $43.17 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
Data availability
All data are available on the aforementioned public repository and are accessible with permission from the corresponding data committee. No restrictions on data availability other than those imposed by the corresponding data committee.
References
Blackburn EH. Telomere states and cell fates. Nature. 2000;408:53–6.
Rossiello F, Jurk D, Passos JF, d’Adda di Fagagna F. Telomere dysfunction in ageing and age-related diseases. Nat Cell Biol. 2022;24:135–47.
Brouilette S, Singh RK, Thompson JR, Goodall AH, Samani NJ. White cell telomere length and risk of premature myocardial infarction. Arterioscler Thrombosi, Vasc Biol. 2003;23:842–6.
Fitzpatrick AL, Kronmal RA, Gardner JP, Psaty BM, Jenny NS, Tracy RP, et al. Leukocyte telomere length and cardiovascular disease in the cardiovascular health study. Am J Epidemiol. 2007;165:14–21.
Pejenaute Á, Cortés A, Marqués J, Montero L, Beloqui Ó, Fortuño A, et al. NADPH oxidase overactivity underlies telomere shortening in human atherosclerosis. Int J Mol Sci. 2020;21:1434.
van der Harst P, van der Steege G, de Boer RA, Voors AA, Hall AS, Mulder MJ, et al. Telomere length of circulating leukocytes is decreased in patients with chronic heart failure. J Am Coll Cardiol. 2007;49:1459–64.
Demissie S, Levy D, Benjamin EJ, Cupples LA, Gardner JP, Herbert A, et al. Insulin resistance, oxidative stress, hypertension, and leukocyte telomere length in men from the Framingham Heart Study. Aging cell. 2006;5:325–30.
Health Effects Institute. State of global air. Boston, MA: Health Effects Institute; 2020.
Lelieveld J, Evans JS, Fnais M, Giannadaki D, Pozzer A. The contribution of outdoor air pollution sources to premature mortality on a global scale. Nature. 2015;525:367–71.
Zare Sakhvidi MJ, Lequy E, Goldberg M, Jacquemin B. Air pollution exposure and bladder, kidney and urinary tract cancer risk: a systematic review. Environ Pollut. 2020;267:115328.
White AJ, Gregoire AM, Niehoff NM, Bertrand KA, Palmer JR, Coogan PF, et al. Air pollution and breast cancer risk in the Black Women’s Health Study. Environ Res. 2021;194:110651.
Fajersztajn L, Veras M, Barrozo LV, Saldiva P. Air pollution: a potentially modifiable risk factor for lung cancer. Nat Rev Cancer. 2013;13:674–8.
Wang M, Zhou T, Song Y, Li X, Ma H, Hu Y, et al. Joint exposure to various ambient air pollutants and incident heart failure: a prospective analysis in UK Biobank. Eur Heart J. 2021;42:1582–91.
Brook RD, Rajagopalan S, Pope CA 3rd, Brook JR, Bhatnagar A, Diez-Roux AV, et al. Particulate matter air pollution and cardiovascular disease: an update to the scientific statement from the American Heart Association. Circulation. 2010;121:2331–78.
Guarnieri M, Balmes JR. Outdoor air pollution and asthma. Lancet. 2014;383:1581–92.
Martens DS, Nawrot TS. Air pollution stress and the aging phenotype: the telomere connection. Curr Environ Health Rep. 2016;3:258–69.
Kelly FJ, Fussell JC. Linking ambient particulate matter pollution effects with oxidative biology and immune responses. Ann N Y Acad Sci. 2015;1340:84–94.
Masi S, Salpea KD, Li K, Parkar M, Nibali L, Donos N, et al. Oxidative stress, chronic inflammation, and telomere length in patients with periodontitis. Free Radic Biol Med. 2011;50:730–5.
Pieters N, Janssen BG, Dewitte H, Cox B, Cuypers A, Lefebvre W, et al. Biomolecular markers within the core axis of aging and particulate air pollution exposure in the elderly: a cross-sectional study. Environ Health Perspect. 2016;124:943–50.
Zhao B, Vo HQ, Johnston FH, Negishi K. Air pollution and telomere length: a systematic review of 12,058 subjects. Cardiovasc Diagn Ther. 2018;8:480–92.
Njajou OT, Cawthon RM, Damcott CM, Wu SH, Ott S, Garant MJ, et al. Telomere length is paternally inherited and is associated with parental lifespan. Proc Natl Acad Sci USA. 2007;104:12135–9.
Broer L, Codd V, Nyholt DR, Deelen J, Mangino M, Willemsen G, et al. Meta-analysis of telomere length in 19,713 subjects reveals high heritability, stronger maternal inheritance and a paternal age effect. Eur J Hum Genet. 2013;21:1163–8.
Codd V, Nelson CP, Albrecht E, Mangino M, Deelen J, Buxton JL, et al. Identification of seven loci affecting mean telomere length and their association with disease. Nat Genet. 2013;45:422–7, 7e1-2.
Mangino M, Hwang SJ, Spector TD, Hunt SC, Kimura M, Fitzpatrick AL, et al. Genome-wide meta-analysis points to CTC1 and ZNF676 as genes regulating telomere homeostasis in humans. Hum Mol Genet. 2012;21:5385–94.
Haycock PC, Burgess S, Nounu A, Zheng J, Okoli GN, Bowden J, et al. Association between telomere length and risk of cancer and non-neoplastic diseases: a Mendelian randomization study. JAMA Oncol. 2017;3:636–51.
Codd V, Wang Q, Allara E, Musicha C, Kaptoge S, Stoma S, et al. Polygenic basis and biomedical consequences of telomere length variation. Nat Genet. 2021;53:1425–33.
Eeftens M, Beelen R, de Hoogh K, Bellander T, Cesaroni G, Cirach M, et al. Development of Land Use Regression models for PM(2.5), PM(2.5) absorbance, PM(10) and PM(coarse) in 20 European study areas; results of the ESCAPE project. Environ Sci Technol. 2012;46:11195–205.
Beelen R, Hoek G, Vienneau D, Eeftens M, Dimakopoulou K, Pedeli X, et al. Development of NO2 and NOx land use regression models for estimating air pollution exposure in 36 study areas in Europe—The ESCAPE project. Atmos Environ. 2013;72:10–23.
Sheridan C, Klompmaker J, Cummins S, James P, Fecht D, Roscoe C. Associations of air pollution with COVID-19 positivity, hospitalisations, and mortality: Observational evidence from UK Biobank. Environ Pollut. 2022;308:119686.
Cui F, Sun Y, Xie J, Li D, Wu M, Song L, et al. Air pollutants, genetic susceptibility and risk of incident idiopathic pulmonary fibrosis. Eur Respir J. 2023;61:2200777.
Codd V, Denniff M, Swinfield C, Warner SC, Papakonstantinou M, Sheth S, et al. Measurement and initial characterization of leukocyte telomere length in 474,074 participants in UK Biobank. Nat Aging. 2022;2:170–9.
Blane D, Townsend P, Phillimore P, Beattie A. Health and deprivation: inequality and the North. Br J Sociol. 1988;40:344.
Song L, Zhang B, Liu B, Wu M, Zhang L, Wang L, et al. Effects of maternal exposure to ambient air pollution on newborn telomere length. Environ Int. 2019;128:254–60.
Rosa MJ, Hsu HL, Just AC, Brennan KJ, Bloomquist T, Kloog I, et al. Association between prenatal particulate air pollution exposure and telomere length in cord blood: Effect modification by fetal sex. Environ Res. 2019;172:495–501.
Martens DS, Cox B, Janssen BG, Clemente DBP, Gasparrini A, Vanpoucke C, et al. Prenatal air pollution and newborns’ predisposition to accelerated biological aging. JAMA Pediatrics. 2017;171:1160–7.
Lee AG, Cowell W, Kannan S, Ganguri HB, Nentin F, Wilson A, et al. Prenatal particulate air pollution and newborn telomere length: effect modification by maternal antioxidant intakes and infant sex. Environ Res. 2020;187:109707.
Harnung Scholten R, Møller P, Jovanovic Andersen Z, Dehlendorff C, Khan J, Brandt J, et al. Telomere length in newborns is associated with exposure to low levels of air pollution during pregnancy. Environ Int. 2021;146:106202.
Clemente DBP, Vrijheid M, Martens DS, Bustamante M, Chatzi L, Danileviciute A, et al. Prenatal and childhood traffic-related air pollution exposure and telomere length in european children: the HELIX project. Environ health Perspect. 2019;127:87001.
Moslem A, Rad A, de Prado Bert P, Alahabadi A, Ebrahimi Aval H, Miri M, et al. Association of exposure to air pollution and telomere length in preschool children. Sci total Environ. 2020;722:137933.
Lee EY, Oh SS, White MJ, Eng CS, Elhawary JR, Borrell LN, et al. Ambient air pollution, asthma drug response, and telomere length in African American youth. J Allergy Clin Immunol. 2019;144:839–45.e10.
Hautekiet P, Nawrot TS, Janssen BG, Martens DS, De Clercq EM, Dadvand P, et al. Child buccal telomere length and mitochondrial DNA content as biomolecular markers of ageing in association with air pollution. Environ Int. 2021;147:106332.
Everson F, Martens DS, Nawrot TS, Goswami N, Mthethwa M, Webster I, et al. Personal exposure to NO(2) and benzene in the Cape Town region of South Africa is associated with shorter leukocyte telomere length in women. Environ Res. 2020;182:108993.
Dioni L, Hoxha M, Nordio F, Bonzini M, Tarantini L, Albetti B, et al. Effects of short-term exposure to inhalable particulate matter on telomere length, telomerase expression, and telomerase methylation in steel workers. Environ Health Perspect. 2011;119:622–7.
Hou L, Wang S, Dou C, Zhang X, Yu Y, Zheng Y, et al. Air pollution exposure and telomere length in highly exposed subjects in Beijing, China: a repeated-measure study. Environ Int. 2012;48:71–7.
Walton RT, Mudway IS, Dundas I, Marlin N, Koh LC, Aitlhadj L, et al. Air pollution, ethnicity and telomere length in east London schoolchildren: an observational study. Environ Int. 2016;96:41–7.
Shlush LI, Skorecki KL, Itzkovitz S, Yehezkel S, Segev Y, Shachar H, et al. Telomere elongation followed by telomere length reduction, in leukocytes from divers exposed to intense oxidative stress-implications for tissue and organismal aging. Mechanisms Ageing Dev. 2011;132:123–30.
Gangwar RS, Bevan GH, Palanivel R, Das L, Rajagopalan S. Oxidative stress pathways of air pollution mediated toxicity: recent insights. Redox Biol. 2020;34:101545.
Acknowledgements
We are grateful to all the staff and participants in the UK Biobank for their contributions to this study. This research has been conducted using the UK Biobank resource under application number 69741.
Author information
Authors and Affiliations
Contributions
YHT and LXT conceived and designed the study. DKL prepared the data. LXT conducted the data analysis and drafted the manuscript. YHT, BBS and JNW revised the manuscript. All authors agreed on the final version of the manuscript and take responsibility for its content.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethical approval
UK Biobank received ethical approval from the North West Multi-centre Research Ethics Committee (REC reference: 16/NW/0274).
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Tang, L., Li, D., Wang, J. et al. Ambient air pollution, genetic risk and telomere length in UK biobank. J Expo Sci Environ Epidemiol (2023). https://doi.org/10.1038/s41370-023-00587-1
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41370-023-00587-1