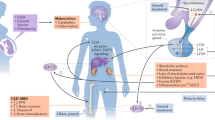
Abstract
The introduction of recombinant DNA-derived human growth hormone (rhGH) in the mid-1980s allowed studies to be undertaken in a number of growth disorders other than the classic indication—growth-hormone deficiency (GHD). In patients with GHD, optimizing the dose and frequency of rhGH administration, and early instigation of therapy, has led to near-normalization of final height. The use of rhGH in the treatment of Turner syndrome, Prader–Willi syndrome, intrauterine growth restriction, and chronic renal failure demonstrated the efficacy of therapy, although the increase in final height (5–7 cm) is less than that achieved in GHD. Cost–benefit implications need to be considered in the next phases of evaluating the role of rhGH therapy in these indications. To date, rhGH has only received approval for the management of idiopathic short stature in the US; as with the other wider growth indications, the lack of formal randomized, controlled trials hampers the full evaluation of efficacy, and a cautious approach should, therefore, be adopted for this particular indication. rhGH has a good safety record, although there are current concerns about the possible long-term increased risk of colonic and lymphatic malignancy, which will require monitoring through national cancer registries.
Key Points
-
Recombinant DNA-derived human growth hormone (rhGH) therapy is effective in growth-hormone deficiency; if rhGH is used at a daily dose of 0.025–0.035 mg/kg body weight, administered by subcutaneous injection from an early age, normalization of final height to within the target height of the family can be achieved
-
At the end of therapy, all patients with isolated growth-hormone deficiency should be retested and rhGH therapy continued into adulthood in the most severely affected; for individuals with reduced GH secretion, careful follow-up by an adult endocrinologist is warranted
-
Data from the only randomized, controlled trial of rhGH therapy in patients with Turner syndrome showed a net gain of 7.3 cm with therapy: at a daily dose of rhGH of 0.05 mg/kg body weight, six patients needed to be treated in order that one would reach a height of over 150 cm
-
The other indications for rhGH therapy—chronic renal failure and intrauterine growth restriction—require similar doses to Turner syndrome, but efficacy remains to be demonstrated in formal studies
-
There is insufficient information from randomized, controlled studies to advise on the use of rhGH therapy in patients with idiopathic short stature
-
rhGH has a good safety record to date, but ongoing pharmacologic vigilance is required, particularly in the uncertain area of long-term risk of malignancy
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Raben MS (1958) Treatment of a pituitary dwarf with human growth hormone. J Clin Endocrinol Metab 18: 901–903
Prader A et al. (1967) Long term treatment with human growth hormone (Raben) in small doses. Evaluation of 18 hypopituitary patients. Helv Paediatr Acta 22: 423–439
Tanner JM et al. (1971) Effect of human growth hormone treatment for 1 to 7 years on growth of 100 children with growth hormone deficiency, low birth weight, inherited smallness, Turner syndrome and other complaints. Arch Dis Child 45: 745–779
GH Research Society (2000) Consensus guidelines for the diagnosis and treatment of growth hormone (GH) deficiency in childhood and adolescence: summary statement of the GH Research Society. J Clin Endocrinol Metab 85: 3990–3993
Dattani MT and Preece MA (2004) Growth hormone deficiency and related disorders: insights into causation, diagnosis and treatment. Lancet 363: 1977–1987
Wit JM et al. (1996) Spontaneous growth and response to growth hormone treatment in children with growth hormone deficiency and idiopathic short stature. Pediatr Res 39: 295–302
Tanaka T et al. (2002) Diagnosis and management of growth hormone deficiency in childhood and adolescence: part 2—growth hormone treatment in growth hormone deficient children. Growth Horm IGF Res 12: 323–341
Saenger P (2002) Growth hormone in growth hormone deficiency. BMJ 325: 58–59
Preece MA et al. (1976) Dose dependence of growth response to human growth hormone in growth hormone deficiency. J Clin Endocrinol Metab 42: 477–483
Cohen P et al. (2002) Effects of dose and gender on the growth and growth factor response to GH in GH-deficient children: implications for efficacy and safety. J Clin Endocrinol Metab 87: 90–98
Radetti G et al. (2003) Treatment of GH-deficient children with two different GH doses: effect on final height and cost–benefit implications. Eur J Endocrinol 148: 515–518
Ranke MB et al. (1994) Prediction of growth in response to treatment with growth hormone. In Progress in Growth Hormone Therapy—5 Years of KIGS, 97–111 (Eds Ranke MB and Gunnarsson R) Mannheim: JJ Verlag
Burns EC et al. (1981) Final height and pubertal development in 55 children with idiopathic growth hormone deficiency, treated for between 2 and 15 years with human growth hormone. Eur J Pediatr 137: 155–164
Blethen SL et al. (1993) Factors predicting the response to growth hormone (GH) therapy in prepubertal children with GH deficiency. J Clin Endocrinol Metab 74: 574–579
Adan L et al. (1997) Adult height in 24 patients treated for growth hormone deficiency and early puberty. J Clin Endocrinol Metab 82: 229–233
Mericq MV et al. (2000) Near final height in pubertal growth hormone (GH)-deficient patients treated with GH alone or in combination with luteinizing hormone-releasing hormone analog: results of a prospective, randomized trial. J Clin Endocrinol Metab 85: 569–573
Tanaka T et al. (1997) GH and GnRH analog treatment in children who enter puberty at short stature. J Pediatr Endocrinol Metab 10: 623–628
Mul D et al. (2005) Final height after treatment of early puberty in short adopted girls with gonadotrophin releasing hormone agonist with or without growth hormone. Clin Endocrinol 63: 185–190
Clayton PE et al. (2005) Consensus statement on the management of the GH-treated adolescent in the transition to adult care. Eur J Endocrinol 152: 165–170
Salomon F et al. (1989) The effects of treatment with recombinant human growth hormone on body composition and metabolism in adults with growth hormone deficiency. N Engl J Med 321: 1797–1803
Tomlinson JW et al. (2001) Association between premature mortality and hypopituitarism: West Midlands Prospective Hypopituitary Study Group. Lancet 357: 425–431
Yuen KCJ et al. (2005) Improvement in insulin sensitivity without concomitant changes in body composition and cardiovascular risk markers following fixed administration of a very low growth hormone (GH) dose in adults with severe GH deficiency. Clin Endocrinol 63: 428–436
Saenger P et al. (2001) Recommendations for the diagnosis and treatment of Turner syndrome. J Clin Endocrinol Metab 86: 3061–3069
van Pareren YK et al. (2003) Final height in girls with Turner syndrome after long-term growth hormone treatment in three dosages and low dose estrogens. J Clin Endocrinol Metab 88: 1119–1125
Stephure K et al. (2005) Impact of growth hormone supplementation on adult height in Turner syndrome: results of the Canadian randomized controlled trial. J Clin Endocrinol Metab 90: 3360–3366
Vimalachandra D et al. (2001) Growth hormone treatment in children with chronic renal failure: a meta-analysis of randomized controlled trials. J Pediatr 139: 560–567
Paterson WF and Donaldson MD (2003) Growth hormone therapy in the Prader–Willi syndrome. Arch Dis Child 88: 283–285
Myers SE et al. (2000) Sustained benefit after 2 years of growth hormone on body composition, fat utilization, physical strength and agility, and growth in Prader–Willi syndrome. J Pediatr 137: 42–49
Carrel AL et al. (2004) Growth hormone improves mobility and body composition in infants and toddlers with Prader–Willi syndrome. J Pediatr 145: 744–749
von Pareren Y et al. (2003) Adult height after long-term, continuous growth hormone (GH) treatment in short children born small for gestational age: results of a randomized, double blind, dose-response GH trial. J Clin Endocrinlon Metab 88: 3584–3590
Ranke MB (1996) Towards a consensus on the definition of idiopathic short stature. Horm Res 45 (Suppl 2): 64–66
Leschek EW et al. (2004) Effect of growth hormone treatment on adult height in peripubertal children with idiopathic short stature: a randomized, double blind, placebo-controlled trial. J Clin Endocrinol Metab 89: 3140–3148
Wit JM et al. (2005) Growth hormone (GH) treatment to final height in children with idiopathic short stature: evidence for a dose effect. J Pediatr 146: 45–53
Finkelstein BS et al. (2002) Effect of growth hormone therapy on height in children with idiopathic short stature: a meta-analysis. Arch Pediatr Adolesc Med 156: 230–240
Ulph F et al. (2004) Personality functioning: the influence of stature. Arch Dis Child 89: 17–21
Sandberg DE and Voss LD (2002) The psychosocial consequences of short stature: a review of the evidence. Best Pract Res Clin Endocrinol Metab 16: 449–463
Lai KYC et al. (1994) Cognitive abilities associated with Silver–Russell syndrome. Arch Dis Child 71: 490–496
Skuse DH et al. (1997) Evidence from Turner's syndrome of an imprinted X-linked locus affecting cognitive function. Nature 387: 705–708
Takala J et al. (1999) Increased mortality associated with growth hormone treatment in critically ill adults. N Engl J Med 341: 785–792
Cutfield WS et al. (2000) Incidence of diabetes mellitus and impaired glucose tolerance in children and adolescents receiving growth-hormone treatment. Lancet 355: 610–613
Rivkees SA et al. (1994) Prednisone dose limitation of growth hormone treatment of steroid-induced growth failure. J Pediatr 125: 322–325
Toogood AA et al. (2000) Modulation of cortisol metabolism by low-dose growth hormone replacement in elderly hypopituitary patients. J Clin Endocrinol Metab 85: 1727–1730
Moore JS et al. (1999) Modulation of 11β-hydroxysteroid dehydrogenase isozymes by growth hormone and insulin-like growth factor: in vivo and in vitro studies. J Clin Endocrinol Metab 84: 4172–41774
Watanabe S et al. (1989) Risk factors for leukemia occurrence among growth hormone users. Jpn J Cancer Res 80: 822–825
Blethen SL et al. (1996) Safety of recombinant DNA-derived growth hormone (rhGH): the National Cooperative Growth Study experience. J Clin Endocrinol Metab 81: 1704–1710
Swerdlow AJ et al. (2002) Risk of cancer in patients treated with human pituitary growth hormone in the UK, 1959–1985: a cohort study. Lancet 360: 273–277
Furstenberger G and Senn HJ (2002) Insulin-like growth factors and cancer. Lancet Oncol 5: 298–302
Gravholt CH (2005) Clinical practice in Turner syndrome. Nat Clin Pract Endocrinol Metab 1: 41–52
Allen DB (1999) Issues in the transition from childhood to adult growth hormone therapy. Pediatrics 104: 1004–1010
Donaubauer J et al. (2003) Re-assessment of growth hormone secretion in young adult patients with childhood-onset growth hormone deficiency. Clin Endocrinol (Oxf) 58: 456–463
Mullis PE et al. (2005) Isolated autosomal dominant growth hormone deficiency: an evolving pituitary deficit? A multicenter follow-up study. J Clin Endocrinol Metab 90: 2089–2096
Saggese G et al. (1998) Diagnosis and treatment of growth hormone deficiency in children and adolescents: towards a consensus. Ten years after the Availability of Recombinant Human Growth Hormone Workshop held in Pisa, Italy, 27–28 March 1998. Horm Res 50: 320–340
Shalet SM et al. (1998) The diagnosis of growth hormone deficiency in children and adults. Endocr Rev 19: 203–223
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Rights and permissions
About this article
Cite this article
Hindmarsh, P., Dattani, M. Use of growth hormone in children. Nat Rev Endocrinol 2, 260–268 (2006). https://doi.org/10.1038/ncpendmet0169
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1038/ncpendmet0169
This article is cited by
-
An updated view of hypothalamic–vascular–pituitary unit function and plasticity
Nature Reviews Endocrinology (2017)
-
Short-term, supra-physiological rhGH administration induces transient DNA damage in peripheral lymphocytes of healthy women
Journal of Endocrinological Investigation (2017)
-
Kleinwuchs
Monatsschrift Kinderheilkunde (2015)
-
A Follow-up Study to Monitor Adult Height Among Spanish Children with Growth Hormone Deficiency Who Received Biosimilar Human Recombinant Growth Hormone (Omnitrope®) During a Phase III Clinical Trial
Advances in Therapy (2015)
-
Prediction of response to growth hormone treatment in pre-pubertal children with growth hormone deficiency
Journal of Endocrinological Investigation (2011)