Abstract
Pulmonary fibrosis triggered during the early stage of acute respiratory distress syndrome (ARDS) contributes to poor prognosis in patients. However, whether microRNAs (miRNAs) can serve as therapeutic targets for early pulmonary fibrosis during ARDS is still largely unknown. In this study, we evaluated the effects and mechanisms of miR-200s and its targets ZEB1/2 in lung tissue. An early pulmonary fibrosis mouse model caused by ARDS was established via a lipopolysaccharide (LPS) three-hit regimen. Lentiviral packaged miR-200b/c cDNA or ZEB1/2 shRNA was intratracheally administered into the lungs of C57BL/6 mice 1 day before an LPS injection was administered. In vitro, following a 30-min pretreatment with miR-200b/c or SB203580/SIS3, RLE-6TN cells were stimulated by LPS or LPS + transforming growth factor-β (TGF-β) for 24 h. miR-200b/c and E-cadherin protein expression declined, whereas ZEB1/2 mRNA and protein and vimentin and α-smooth muscle actin (α-SMA) protein levels gradually increased during the development of pulmonary fibrosis. Furthermore, both the overexpression of miR-200b/c and the silencing of ZEB1/2 significantly alleviated pulmonary inflammation and fibrosis, reduced vimentin and α-SMA expression, and increased E-cadherin protein levels. In RLE-6TN cells, LPS combined with TGF-β exerts synergistic effects of increasing vimentin and α-SMA protein levels, increasing p38 and smad3 phosphorylation and reducing E-cadherin protein levels, which were reversed by pretreatment with miR-200b/c or SB203580/SIS3. Our findings demonstrate that miR-200b/c was downregulated, whereas ZEB1/2 was upregulated in the development of LPS-induced early pulmonary fibrosis. miR-200b/c exerts a protective effect by targeting ZEB1/2, which may be associated with the inhibition of p38 MAPK and TGF-β /smad3 signaling pathways.
Similar content being viewed by others
Main
Acute respiratory distress syndrome (ARDS) is an acute and progressive respiratory failure with refractory hypoxemia caused by a variety of factors.1 Previous studies2 demonstrated that the pathological change in lung tissue is mainly exudative manifestation in the early stage of ARDS (<7d), whereas the collagen fibers increase 7 days later, and pulmonary fibrosis forms gradually. However, recent studies3 showed that pulmonary fibrosis may occur in the early stage of ARDS. Early pulmonary fibrosis is an important factor of poor prognosis in patients with ARDS.4 Therefore, exploring the mechanism of early pulmonary fibrosis may provide a theoretical and experimental basis for the development of effective treatment strategies and improvements in prognosis.
microRNA (miRNA) is a class of highly conserved RNA composed of ~22-nucleotide-long, single-stranded, non-coding, small endogenous RNA that can negatively regulate the expression of targets at the post-transcriptional level.5 miRNA causes the degradation of mRNA or inhibits translation by binding to the complementary sequences of target mRNA in the 3' untranslated region (3'-UTR).6 Existing research7 indicated that miRNA participated in pivotal steps of life, such as proliferation, differentiation, senescence, apoptosis, metabolism, and embryonic development and organ formation. A recent study8 also revealed that miRNA was associated with the onset and progression of some diseases, and the relationship between miRNA and diseases has recently been explored.
The miR-200 family (miR-200s) consists of miR-200a, miR-200b, miR-200c, miR-141, and miR-429.9 It has been shown that miR-200a, miR-200b, and miR-200c were significantly downregulated in mice with idiopathic pulmonary fibrosis (IPF) induced by bleomycin; similarly, miR-200a and miR-200c were also markedly reduced in patients with IPF.10 The zinc finger E-box-binding homeobox (ZEB) family includes ZEB1 and ZEB2.11 Current studies12 have confirmed that ZEB1/2 mRNA was the target of miR-200s and that its 3'-UTR comprised several binding sites of miR-200s.
Transforming growth factor-β (TGF-β), produced by lymphocytes, monocytes, epithelial cells, and fibroblasts, regulates proliferation, differentiation, migration, adhesion, and metabolism of extracellular matrix (ECM) by way of autocrine or paracrine mechanisms and participates in the process of embryonic development, injury and repair.13 In the development of fibrosis, the complicated regulatory system of various cytokines is imbalanced, and TGF-β is a key factor that contributes to fibrosis. Importantly, epithelial–mesenchymal transition (EMT) is considered to be crucial in the pathogenesis of fibrosis.14
Recent studies have indicated that miRNA play an important role in EMT by negatively regulating its target.15 Multiple studies confirmed that miR-200s increased the expression of the epithelial marker E-cadherin by targeting ZEB, thereby suppressing EMT.16 Researchers have found that ZEB1/2 is the target of miR-200s and that TGF-β can upregulate the expression of ZEB1/2, thereby forming a TGF-β/ZEB/miR-200 signaling network in renal tubular epithelial cells and human breast cancer cells.17, 18
In this study, we established an animal model of early pulmonary fibrosis caused by lipopolysaccharide (LPS) treatment to detect the expression of components of the miR-200s/ZEB signaling network and to examine the effect of miR-200b/c and ZEB1/2 on early pulmonary fibrosis. We also investigated whether LPS promotes EMT by activating the p38/MAPK and TGF-β/Smad signaling pathways.
Materials and methods
Animals and Reagents
C57BL/6 mice weighing 20~25 g were obtained from the Department of Laboratory Animal Science of Shanghai Jiaotong University, Shanghai, China. LPS (Escherichia coli 055: B5) was purchased from Sigma-Aldrich (St. Louis, MO, USA). Ham’s F12 medium was procured from Lonza (Basel, Switzerland). TGF-β was procured from Pepro Tech (Rocky Hill, NJ, USA). The rabbit anti-ZEB1 primary antibody was purchased from Santa Cruz Biotechnology (Delaware, CA, USA). The goat anti-ZEB2 primary antibody was procured from Novus, Inc. (Littleton, CO, USA). Rat anti-E-cadherin, rabbit anti-vimentin, rabbit anti-α-smooth muscle actin (α-SMA), mouse anti-E-cadherin, and rabbit anti-β-actin primary antibodies were purchased from Abcam (Cambridge, UK). Rabbit anti-p38, mouse anti-phosphorylated-p38, rabbit anti-smad3, and rabbit anti-phosphorylated-smad3 were purchased from Cell Signaling Technology (Danvers, MA, USA). Horseradish peroxidase-conjugated goat anti-rabbit, horse anti-rat, rabbit anti-goat, and goat anti-mouse secondary antibodies were all purchased from ComWin Biotech (Beijing, China). SB203580 (a specific inhibitor of p38 MAPK) and SIS3 (a selective inhibitor of smad3) were procured from Selleckchem (Houston, TX, USA) and Tocris Bioscience (Minneapolis, MN, USA), respectively.
Animal Model
The animal model of early pulmonary fibrosis caused by LPS-induced ARDS was established via a modified approach of previously published methods19 In brief, 48 mice were randomly divided into six groups, and the eight mice in each group were anesthetized via an intraperitoneal injection of pentobarbital (0.8%) at a dosage of 200 μl/10 g body weight and subjected to oral endotracheal intubation using an arterial puncture needle (22G). LPS (1.5 mg/kg) was injected into the lung by the endotracheal tube, and then, the mouse was bristled up and whirled in order to evenly distribute the liquid drug into the lung. The endotracheal tube was then removed. LPS (3 mg/kg) was administered by intraperitoneal injection after 24 h and was administered via endotracheal tube after 48 h. An equivalent amount of normal saline was used for solvent comparison, and the control group received nothing. Mice were sacrificed on the 3rd, 7th, 14th, and 21st day after LPS treatment. Alveolar lavage was performed before the lung tissues were harvested. The left lobe of lung tissues was used for histology and the right lobe for miRNA microarray, mRNA and protein analysis.
Microarray Analysis
Microarray analysis of lung tissues was accomplished with the help of OE Biotech. Co., Ltd. in Shanghai, China. In brief, total RNA from the lung tissue of the animal model was quantified by the NanoDrop ND-2000 (Thermo Scientific), and RNA integrity was assessed with the Agilent Bioanalyzer 2100 (Agilent Technologies). The sample labeling, microarray hybridization and washing were performed based on the manufacturer’s standard protocols. In brief, total RNA was dephosphorylated, denatured, and then labeled with Cyanine-3-CTP. After purification, the labeled RNAs were hybridized onto the microarray. After washing, the arrays were scanned with the Agilent Scanner G2505C (Agilent Technologies).
Feature Extraction software (version 10.7.1.1, Agilent Technologies) was used to analyze array images to obtain raw data. Next, Genespring software (version 13.1, Agilent Technologies) was employed to finish the basic analysis of the raw data. Initially, the raw data were normalized with the quantile algorithm. The probes in at least 100% of samples in any one condition out of two conditions that had flags in 'Detected' were chosen for further data analysis. Differentially expressed miRNAs were then identified through fold change and P-values calculated via t-tests. The threshold set for up- and downregulated genes was a ⩾2.0-fold change and a P-value of ⩽0.05. Target genes of differentially expressed miRNAs were the intersection predicted with three databases (Targetscan, microRNAorg, pita). GO analysis and KEGG analysis were applied to determine the roles of these target genes. Hierarchical Clustering was performed to show the distinguishable miRNA expression patterns among samples.
Recombinant Lentiviral miR-200b/c cDNA or ZEB1/2 shRNA Vectors were Transduced into Mice
Both lentivirus over-expressing miR-200b or miR-200c and lentiviral vector carrying ZEB1 shRNA or ZEB2 shRNA were generated by Genomeditech Inc. (Shanghai, China). The recombinant lentiviral vector packaged miR-200b and miR-200c were designated 'Lv-miR-200b' and 'Lv-miR-200c'. Three shRNA sequences targeting the mouse ZEB1 or ZEB2 coding region were designed, and the corresponding lentiviral vectors (Lv-ZEB1 shRNA and Lv-ZEB2 shRNA) were constructed. An invalid RNA sequence was used as the negative control (Lv-NC). Lv-miR-200b, Lv-miR-200c, Lv-ZEB1 shRNA, Lv-ZEB2 shRNA, and Lv-NC were intratracheally administered into the lungs of C57BL/6 mouse, and eight mice was used for each group. One day after gene transfer, animals received LPS injections as described. Mice were killed on the 21st day after LPS treatment, and lung tissues were harvested.
Pathological Staining
The left lobes of lung tissues were immersed in 4% paraformaldehyde for 24 h and transferred to 70% ethanol. Then, the samples were dehydrated through a serial alcohol gradient, embedded in paraffin, and sectioned at 4-μm thickness. Before immunostaining, sections were dewaxed in xylene, rehydrated through decreasing concentrations of ethanol, and washed in PBS. Sections were then stained with either hematoxylin and eosin or Masson's trichrome per the manufacturer’s standard procedures. Light microscopy was used to observe the morphology of plaques, and the Image-Pro Plus Image analysis system was used to acquire and analyze histologic images. The semi-quantitative scoring on the degree of lung injury for edema, inflammation, and hemorrhage was performed according to the method of Murakami and colleagues,20 and pulmonary fibrosis for blue collagen fibers was assayed via the standard Aschoff score as previously described.21 Degrees of lung injury and pulmonary fibrosis were graded on a scale of 0~4: 0, absent, appears normal (−); 1, light (+); 2, moderate (++); 3, strong (+++); 4, intense (++++). Three sections collected from each lung were analyzed, and the analysis was conducted by two independent observers.
Cell Culture and Treatment
RLE-6TN (rat lung epithelial-T-antigen negative) cells, purchased from ATCC (American Type Culture Collection), were cultured in Ham’s F12 medium with 10% FBS in 5% CO2 and humidified air at 37 °C. The cell culture medium was replaced every 2–3 days. Upon reaching 80–90% confluency, cells were subcultured at a 1:5 ratio as recommended and seeded into six-well plates. One day after seeding, cells were exposed to LPS (0.1 mg/ml) or TGF-β (0.5 ng/ml) for 24 h.
RLE-6TN cells were pretreated with SB203580, SIS3, miR-200b/c mimic, or ZEB-shRNA for 30 min prior to LPS or TGF-β stimulation to investigate the p38/MAPK and TGF-β/smad3 signaling pathways, respectively.
ELISA
Serum, supernatants of bronchoalveolar lavage fluid (BALF) and cell culture media were collected. TGF-β levels were measured with an ELISA kit (R&D Systems) according to the procedure described by the manufacturer. Absorbance was determined at 450 nm with a microplate reader (Bio-Rad Laboratory), and concentration was calculated from a linear standard curve. ELISA measurements were performed in triplicate.
Real-Time PCR
Total RNA was extracted from lung tissue with Trizol reagent according to the manufacturer’s protocol. RNA was reverse-transcribed with the PrimeScript RT reagent Kit (RR036A, Takara, Japan) for miRNA or the PrimeScript RT Master Mix kit (RR037A) for mRNA per the manufacturer’s instructions. SYBR Green quantitative RT-PCRs were performed on the Applied Biosystems 7500 RT-PCR system. For each sample, the amplification reaction was performed in triplicate. The primers were purchased from Ribobio Biotechnolog (Guangzhou, China). The ZEB1 and ZEB2 primers used in this study were as follows: ZEB1 (GenBank accession No. NM_011546.3): forward: 5′-ACACGCCCACAGATACGA-3′; reverse: 5′-TTGATTCCTGAAGCAACCA-3′; ZEB2 (GenBank accession No. NM_001289521.1): forward: 5′-CAGGTAACCGCAAGTTCAA-3′; reverse: CAGTTTGGGCATTCGTAAG; β-actin (GenBank accession No. NM_007393.5): forward: 5′-CCTCTATGCCAACACAGT-3′; reverse: 5′-AGCCACCAATCCACACAG-3′. Relative RNA quantification was performed via the comparative 2−ΔΔCt method. miRNA expression was normalized to U6, and ZEB1/2 was normalized to β-actin mRNA levels.
Western Blotting
Total protein was extracted with M-PER mammalian protein extraction reagents (Pierce, Rockford, IL, USA) in accordance with the manufacturer’s instructions. Equivalent amounts of protein sample (50 μg) were separated by gel electrophoresis on a 10% SDS-PAGE gel and then transferred onto a polyvinylidenedifluoride membrane (Millipore, Billerica, MA, USA). Blots were blocked at room temperature for 2 h with 5% bovine serum albumin (BSA). The membranes were subsequently incubated at 4 °C overnight with primary antibodies (1:500 dilution for rabbit a-ZEB1, 1:400 dilution for goat a-ZEB2, 1:2000 dilution for rabbit a-vimentin, 1:1000 dilution for rat a-E-cadherin, 1:2000 dilution for rabbit a-α-SMA, 1:1000 dilution for mouse a-E-cadherin, 1:500 dilution for rabbit a-p38, 1:500 dilution for mouse a-p-p38, 1:400 dilution for rabbit a-smad3, 1:400 dilution for rabbit a-p-smad3), followed by an appropriate HRP-conjugated secondary antibody (1:4000 dilution) at room temperature for 2 h. Next, ECL plus detection reagents (Pierce) were used to detect immunoblotting. The protein levels were normalized to β-actin.
Immunofluorescence Staining
A total of 4-μm thick sections were cut from paraffin blocks of lung tissue. After deparaffinization and rehydration, endogenous peroxidase activity was blocked by immersing the slides in absolute methanol solution containing 0.3% hydrogen peroxide for 30 min. Slides were then permeabilized with 0.5% Triton X-100 for 20 min and washed in PBS. Non-specific sites were blocked by incubation with PBS containing 1% BSA for 30 min at room temperature. Heat-induced antigen retrieval by autoclave pretreatment (120 °C for 5 min) in citrate buffer solution (pH 6.0) was performed. The sections were then incubated with rat anti-E-cadherin antibody (1:200 dilution), rabbit anti-vimentin antibody (1:200 dilution) and rabbit anti-α-SMA (1:300 dilution) overnight at 4 °C followed by appropriate Cy3-conjugated goat anti-rabbit or anti-rat IgG secondary antibodies (1:400; Jackson ImmunoResearch, West Grove, PA) for 1 h at room temperature. Nuclei were counterstained with DAPI (1:500; Invitrogen). All reactions were performed with appropriate positive and negative controls, and no significant staining was observed in the negative control sections. Fluorescence imaging was conducted with excitation at 488 nm and emission at 510 nm at room temperature.
Statistical Analysis
All data were presented as the mean±standard deviation. The significant differences between two groups were determined via t-tests. Comparisons between treatment groups and the control group were executed via a one-way analysis of variance followed by Dunnett’s test. Comparisons among multiple groups were performed with one-way analysis of variance followed by Bonferroni’s test. Statistical analysis was performed with GraphPad Prism version 5.0 (San Diego, CA, USA). A P-value of <0.05 was considered statistically significant.
Results
In vivo Studies
The pathology of lung tissue in the development of early pulmonary fibrosis
HE staining results showed that the morphology of lung tissue is normal in the control group. Alveolar walls were slightly widened, and inflammatory cells leaked into the alveolar cavity on the third day after the LPS injection. Alveolar septa thickened, alveolar collapse occurred, and a large number of inflammatory cells had infiltrated on the 7th day. The alveolar inflammation subsided, and alveolar septa were destroyed, resulting in a loss of normal alveolar structure at the 14th and 21st days (Figure 1a). Lung injury scores revealed that the edema, inflammation and hemorrhage were significantly higher on the 3rd and 7th days after LPS injection, compared with the control group and NS group. Then, lung edema and hemorrhage were markedly lower on the 14th and 21st days after LPS injection, but the inflammation score was still higher than in the control and NS group. There was no significant difference in the lung injury score between the control group and the NS group (Figure 1b).
Pathological changes in lung tissue and the levels of TGF-β in BALF and serum during the development of early pulmonary fibrosis HE staining (a) and Masson staining (c) of lung tissue in an animal model of early pulmonary fibrosis. The lung injury score (b) and pulmonary fibrosis score (d). The levels of TGF-β in BALF (e) and serum (f) in an animal model of early pulmonary fibrosis were quantified by ELISA. All data are expressed as the mean±s.d. from at least three replicate experiments. *P<0.05 and **P<0.01 vs the control group.
Masson staining results indicated that a small amount of blue collagen fiber, the main component of the extracellular matrix, was observed in the control group. A few collagen fibers appeared in lung tissue on the third day after LPS treatment. The amount of collagen fiber markedly increased and concentrated around the vessels and bronchi on the 7th day. The amount of blue collagen fibers increased, and fibrosis was gradually aggravated over time. Many collagen fibers were deposited, and typical pulmonary fibrosis formed on the 21st day (Figure 1c). Similarly, the fibrosis score also showed a gradually increased trend in lung tissue after LPS stimulation (Figure 1d).
The levels of TGF-β in BALF and serum in the development of early pulmonary fibrosis
ELISA results showed that the TGF-β levels in the BALF and serum of LPS treatment animals were significantly greater than those in the control or NS group. LPS led to a gradual increase in TGF-β levels over time. Compared with the control group, the levels of TGF-β were approximately 1.3-fold higher in BALF (P<0.05) and in serum (P<0.01) in the 3d group. Moreover, there was a significant increase in TGF-β levels in BALF and serum in the 7d, 14d, and 21d groups (P<0.01). The level of TGF-β was almost three times higher in BALF and two times higher in serum than in the control group on the 21st day after LPS injection (Figures 1e and f).
Microarray analysis in the development of early pulmonary fibrosis
Microarray assay revealed that compared with the control group, different miRNAs were upregulated or downregulated in the NS, 3d, 7d, 14d, and 21d groups (Figure 2a). Furthermore, miR-429, miR-141, miR-21, miR-200a, miR-200b, miR-200c, miR-29a, miR-29b, and miR-29c were expressed abnormally. Importantly, members of the miR-200 family were significantly downregulated, especially miR-200b and miR-200c, in lung tissue during the development of LPS-induced early pulmonary fibrosis (Figure 2b).
Microassay analysis during the development of early pulmonary fibrosis. The microassay analysis (a) of miRNA in lung tissue in an animal model of LPS-induced early pulmonary fibrosis. The heat map of miRNAs (b) that were associated with early pulmonary fibrosis. All data are expressed as the mean±s.d. from at least three replicate experiments.
The expression of miR-200b/c, ZEB1/2 mRNA,and protein in the development of early pulmonary fibrosis
Real-time PCR results showed that the expression of miR-200b and miR-200c was downregulated during the development of early pulmonary fibrosis. Compared with the control group, miR-200b and miR-200c were significantly decreased on the 3rd day after LPS injection and had continuously declined on the 7th, 14th, and 21st days. At the 21st day after LPS injection, the expression level of miR-200b dropped to ~66%, and miR-200c was reduced by almost 50% compared with the control group (Figures 3a and b).
The expression of miR-200b/c, ZEB1/2 mRNA, and protein during the development of early pulmonary fibrosis. The expression levels of miR-200b (a), miR-200c (b), ZEB1 mRNA (c), and ZEB2 mRNA (d) in lung tissue in animal model of early pulmonary fibrosis were detected by real-time PCR. The protein levels of ZEB1 (e) and ZEB2 (f) in lung tissue in animal model of early pulmonary fibrosis were examined by western blotting. All data are expressed as the mean±s.d. from at least three replicate experiments. *P<0.05 and **P<0.01 vs the control group.
Real-time PCR analysis also showed that the expression level of ZEB1/2 mRNA was gradually upregulated after LPS treatment during the development of early pulmonary fibrosis and increased significantly at the 21st day compared with the control group. Interestingly, the increase in the ZEB2 mRNA level was greater than that for ZEB1 mRNA in the process of early pulmonary fibrosis. The expression of ZEB2 mRNA was almost three times higher than that of the control group, whereas the ZEB1 mRNA level showed only an ~1.3-fold increase at the 21st day after LPS treatment (Figures 3c and d).
In addition, western blotting results revealed that the changes in ZEB1 and ZEB2 protein were consistent with their mRNA levels in the development of early pulmonary fibrosis. ZEB1 and ZEB2 proteins increased along with the aggravation of pulmonary fibrosis, and the increase of ZEB2 protein was more than that of ZEB1 protein (Figures 3e and f).
The expression of E-cadherin, vimentin, α-SMA protein in the development of early pulmonary fibrosis
Western blotting results showed that the epithelial marker E-cadherin reduced, while the expression levels of mesenchymal markers vimentin and α-SMA increased after LPS treatment. Compared with control group, there is a significant difference in the decreased E-cadherin level on the third day (P<0.01), whereas vimentin and α-SMA protein levels were increased slightly (P>0.05). The E-cadherin protein level declined, and vimentin and α-SMA were further upregulated on the 7th, 14th, and 21st days. The expression level of E-cadherin in the 21d group was almost half of that in the control group. In contrast, the level of vimentin increased significantly, and the α-SMA protein showed a threefold increase in the 21d group (P<0.01) (Figure 4a).
The expression of E-cadherin, vimentin, α-SMA protein during the development of early pulmonary fibrosis. The expression of E-cadherin, vimentin and α-SMA protein in lung tissue in an animal model of early pulmonary fibrosis was detected by western blotting (a) and immunofluorescence (b). All data are expressed as the mean±s.d. from at least three replicate experiments. *P<0.05 and **P<0.01 vs the control group.
Immunofluorescence assay also revealed that E-cadherin protein decreased and vimentin and α-SMA increased gradually in the development of early pulmonary fibrosis, which was consistent with the western blot results (Figure 4b).
Effects of Lv-miR-200b/c cDNA and Lv-ZEB1/2 shRNA on the expression of miR-200b/c, ZEB1/2 mRNA, and protein in lung tissue
Real-time PCR results showed that Lv-miR-200b/c transfection effectively upregulated miR-200b or miR-200c expression ~1.6-fold (Figures 5a and b), as well as significantly reduced ZEB1 and ZEB2 mRNA and protein levels in lung tissue. Compared with LPS group, there was significant decreased in ZEB2 mRNA level (P<0.05), whereas the ZEB1 mRNA level declined slightly (P>0.05) in the miR-200b overexpression group. Both ZEB1 and ZEB2 mRNA levels in the miR-200c overexpression group were significantly lower than those in the LPS group, and the differences were statistically significant (P<0.01) (Figures 5c and d). Similarly, ZEB1 and ZEB2 protein levels also reduced after miR-200b and miR-200c overexpression in lung tissue (P<0.05) (Figures 5e and f).
Effects of miR-200b/c overexpression or ZEB1/2 silencing on the expression of miR-200b/c and ZEB1/2. After the overexpression of miR-200b or miR-200c in local lung tissue, the levels of miR-200b (a), miR-200c (b), ZEB1 mRNA (c), and ZEB2 mRNA (d) in lung tissue were detected by real-time PCR. The protein levels of ZEB1 (e) and ZEB2 (f) in lung tissue were examined by western blotting. In addition, after the silencing of ZEB1 and ZEB2 in local lung tissue, ZEB1 mRNA (g) and ZEB2 mRNA (h) in lung tissue were detected by real-time PCR, and the levels of ZEB1 protein (I) and ZEB2 protein (j) were examined by western blotting. Real-time PCR was also used to detect miR-200b (k) and miR-200c (l) levels. All data are expressed as the mean±s.d. from at least three replicate experiments. *P<0.05 and **P<0.01 vs the LPS group.
In addition, transducing Lv-ZEB1 shRNA into local lung tissue markedly reduced the expression of ZEB1 mRNA and protein (P<0.05). ZEB1 mRNA and protein reduced to almost half of that in the LPS group (Figures 5g and h). Similarly, the mRNA and protein levels of ZEB2 also declined significantly after silencing ZEB2 in lung tissue (P<0.01). The expression level of ZEB2 mRNA reduced to 30%, and protein reduced to half of that in the LPS group (Figures 5i and j). Interestingly, silencing of ZEB1 and ZEB2 upregulated miR-200b and miR-200c markedly. The expression levels of miR-200b in Lv-ZEB1 shRNA+LPS group and Lv-ZEB2 shRNA+LPS group were significantly higher than those in the LPS group (P<0.05). Compared with the LPS group, miR-200c increased 1.8-fold in the Lv-ZEB1 shRNA+LPS group and 2.2-fold in the Lv-ZEB2 shRNA+LPS group (Figures 5k and l).
Effects of miR-200b/c overexpression and ZEB1/2 silencing on BALF TGF-β secretion and early pulmonary fibrosis
ELISA results showed that both the overexpression of miR-200b/c and the silencing of ZEB1/2 markedly decreased TGF-β levels in BALF. Compared with the LPS group, the levels of TGF-β were reduced by almost half, and a significant difference was detected (P<0.01) (Figures 6a and b). Interestingly, the effects of silencing ZEB1 and ZEB2 on the levels of TGF-β in BALF were slightly stronger than in the miR-200b and miR-200c overexpression groups.
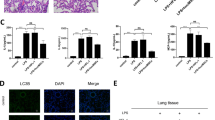
Effects of miR-200b/c overexpression and ZEB1/2 silencing on the level of TGF-β in BALF and the pathology of lung tissue. The levels of TGF-β in BALF were examined by ELISA after the overexpression of miR-200b and miR-200c (a) or the silencing of ZEB1 and ZEB2 (b) in local lung tissue. After the overexpression of miR-200b and miR-200c, HE and Masson staining of lung tissue (c) was performed, and the lung injury score (e) and pulmonary fibrosis score (f) were calculated. Similarly, after the silencing of ZEB1 and ZEB2, HE and Masson staining of lung tissue (d) was performed, and then, the lung injury score (g) and pulmonary fibrosis score (h) were calculated. All data are expressed as the mean±s.d. from three replicate experiments. *P<0.05 and **P<0.01 vs the LPS group.
Both the overexpression of miR-200b and miR-200c alleviated the LPS-induced inflammatory response and pulmonary fibrosis (Figure 6c), and the lung injury score and fibrosis score were significantly lower than in the LPS group (P<0.05) (Figures 6e and f). Similarly, silencing ZEB1 and ZEB2 in local lung tissue also reduced LPS-induced pulmonary inflammation and fibrosis. The pulmonary interstitial edema, infiltration of inflammatory cells, alveolar hemorrhage and blue collagen fibers were almost invisible (Figure 6d), and the lung injury score and fibrosis score were also lower than in the LPS group (P<0.01) (Figures 6g and h).
Importantly, experimental results indicated that the effects of silencing ZEB1 and ZEB2 on pulmonary inflammation and fibrosis were greater than in the miR-200b and miR-200c overexpression groups. Correspondingly, the lung injury score and fibrosis score in the Lv-ZEB1 shRNA+LPS and Lv-ZEB2 shRNA+LPS groups were lower than those in the Lv-miR-200b+LPS and Lv-miR-200c+LPS groups.
Effects of miR-200b/c overexpression and ZEB1/2 silencing on the expression of E-cadherin, vimentin, α-SMA protein
Western blotting results demonstrated that both the overexpression of miR-200b/c and the silencing of ZEB1/2 in local lung tissue upregulated the expression level of E-cadherin and significantly suppressed the expression of vimentin and α-SMA protein (Figures 7a and b).
Effects of miR-200b/c overexpression and ZEB1/2 silencing on the expression of E-cadherin, vimentin, α-SMA protein. The protein levels of E-cadherin, vimentin and α-SMA in lung tissue were detected by western blotting after the overexpression of miR-200b or miR-200c (a) and the silencing of ZEB1 and ZEB2 (b). In addition, the expression of E-cadherin, vimentin and α-SMA protein in lung tissue was also detected via immunofluorescence assays after the overexpression of miR-200b or miR-200c (c) and the silencing of ZEB1 or ZEB2 (d). All data are expressed as the mean±s.d. from at least three replicate experiments. *P<0.05 and **P<0.01 vs the LPS group.
Immunofluorescence assays also revealed that the expression of E-cadherin protein increased, while the expression of vimentin and α-SMA decreased after the overexpression of miR-200b/c or the silencing of ZEB1/2 in local lung tissue, which was consistent with western blot results (Figures 7c and d).
In vitro Studies
Effects of LPS on the TGF-β level and EMT in RLE-6TN cells
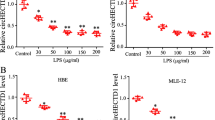
ELISA results revealed that LPS induced an increase in TGF-β levels in the supernatant of cultured RLE-6TN cells. The level of TGF-β in the LPS group was nearly three times higher than that in the control group, and there was a significant difference between the two groups (P<0.01) (Figure 8a).
Effect of LPS on TGF-β levels and EMT in RLE-6TN cells. The level of TGF-β in the supernatants of cultured RLE-6TN cells was examined by ELISA (a). The protein levels of ZEB1, ZEB2 (b), E-cadherin, vimentin, and α-SMA (c) in RLE-6TN cells were detected by western blotting. In addition, the p38 (d) and smad3 (e) phosphorylation levels in RLE-6TN cells were also detected by western blotting after RLE-6TN cells were stimulated with LPS and TGF-β for 24 h. All data are expressed as the mean±s.d. from at least three replicate experiments. *P<0.05 and **P<0.01 vs the control group; #P<0.05 and ##P<0.01 vs the LPS group; &P<0.05 vs the TGF-β group.
Western blotting showed that the expression of ZEB1 and ZEB2 protein increased slightly when RLE-6TN cells were treated with LPS or TGF-β for 24 h, and no significant difference was detected (P>0.05). However, ZEB1 and ZEB2 protein levels increased significantly when cells were treated with LPS combined with TGF-β (P<0.05) (Figure 8b).
LPS downregulated E-cadherin expression and upregulated vimentin and α-SMA protein levels in RLE-6TN cells. E-cadherin protein expression was reduced by ~30%, whereas vimentin and α-SMA protein levels increased slightly. TGF-β triggered a more significant decrease in E-cadherin (P<0.01) and a remarkable increase in vimentin and α-SMA protein levels (P<0.05). Treatment with LPS combined with TGF-β produced an additive or synergistic effect. Compared with the control group, there was a significant difference in the levels of E-cadherin, vimentin and α-SMA protein (P<0.01). Moreover, there was a significant difference in E-cadherin, vimentin, and α-SMA protein expression between the LPS+ TGF-β and LPS groups (Figure 8c).
Western blotting results also indicated that LPS or TGF-β treatment led to increased p38 and smad3 phosphorylation levels in RLE-6TN cells. LPS combined with TGF-β caused an additive or synergistic effect on p38 and smad3 phosphorylation. Compared with the control group, the p38 phosphorylation level increased slightly after RLE-6TN cells were treated with LPS or TGF-β alone. However, treatment with LPS combined with TGF-β markedly increased the p38 phosphorylation level. The p38 phosphorylation level in the LPS+TGF-β group was significantly higher than in the control group (P<0.01). Compared with the LPS and TGF-β group, the phosphorylation level of p38 in the LPS+TGF-β group was also significantly increased (P<0.05) (Figure 8d). LPS triggered a slight increase in smad3 phosphorylation, and TGF-β caused a significant increase in smad3 phosphorylation levels. Smad3 phosphorylation levels increased further after treatment with LPS combined with TGF-β (Figure 8e).
Effects of specific inhibitors of p38 and smad3 on miR-200b/c expression and LPS/TGF-β-induced EMT in RLE-6TN cells
Pretreatment with p38-specific inhibitors SB203580 in RLE-6TN cells noticeably reduced p38 phosphorylation levels. In addition, the p38 phosphorylation level in the LPS+TGF-β+SB203580 group was significantly lower than in the LPS+TGF-β group (P<0.05) (Figure 9a). Similarly, pretreatment with SIS3, the selective inhibitor of smad3, markedly suppressed smad3 phosphorylation (Figure 9b).
Effects of specific p38 inhibitors and selective smad3 inhibitors on miR-200b/c in RLE-6TN cells. The p38 (a) and smad3 (b) phosphorylation levels in RLE-6TN cells were examined by western blotting and miR-200b (c) and miR-200c (d) were detected by real-time PCR after RLE-6TN cells were stimulated with LPS and TGF-β for 24 h following pretreatment with the specific p38 inhibitor SB203580 or the selective smad3 inhibitor SIS3. All data are expressed as the mean±s.d. from at least three replicate experiments. *P<0.05 and **P<0.01 vs the control group; #P<0.05 vs the LPS group; &P<0.05 vs the TGF-β group; $P<0.05 and $$P<0.01 vs the LPS+TGF-β group.
In addition, real-time PCR analysis also showed that LPS reduced miR-200b and miR-200c levels (P<0.05). LPS combined with TGF-β led to a further decrease in the expression of miR-200b and miR-200c (P<0.01). However, treatment with specific inhibitors of p38 and smad3 reversed the decrease in miR-200b/c, and this difference was statistically significant (Figures 9c and d).
The p38-specific inhibitors reduced ZEB1 and ZEB2 protein levels slightly (Figure 10a). Moreover, pretreatment with SB203580 in RLE-6TN cells significantly upregulated E-cadherin and downregulated vimentin and α-SMA protein expression (Figure 10c).
Effects of p38-specific inhibitors and smad3 selective inhibitors on LPS or TGF-β-induced EMT in RLE-6TN cells. The protein levels of ZEB1 and ZEB2 in RLE-6TN cells were detected by western blotting after RLE-6TN cells were stimulated with LPS and TGF-β for 24 h following pretreatment with the specific p38 inhibitor SB203580 (a) or the selective smad3 inhibitor SIS3 (b). The levels of E-cadherin, vimentin and α-SMA proteins in RLE-6TN cells were detected by western blotting after RLE-6TN cells were stimulated with LPS and TGF-β for 24 h following pretreatment with the specific p38 inhibitor SB203580 (c) or the selective smad3 inhibitor SIS3 (d). All data are expressed as the mean±s.d. from at least three replicate experiments. *P<0.05 and **P<0.01 vs the control group; #P<0.05 vs the LPS group; &P<0.05 vs the TGF-β group; $P<0.05 and $$P<0.01 vs the LPS+TGF-βgroup.
In cells treated with TGF-β alone, smad3 inhibitor pretreatment significantly suppressed the expression of both ZEB1 and ZEB2 proteins. However, in the cells treated by LPS combined with TGF-β, the inhibition of smad3 significantly decreased the ZEB2 protein level. (Figure 10b). In addition, pretreatment with SIS3 also increased E-cadherin and decreased vimentin and α-SMA protein levels (Figure 10d).
Effects of a miR-200b/c mimic or ZEB1/2 shRNA on LPS/ TGF-β-induced EMT in RLE-6TN cells
Treatment with miR-200b and miR-200c mimics significantly suppressed ZEB1/2 protein expression in RLE-6TN cells (P<0.01) (Figures 11a and b). E-cadherin protein expression was upregulated, while vimentin and α-SMA levels were downregulated by exposure to the miR-200b/c mimic in the cells treated with LPS combined with TGF-β (Figure 11c). In addition, exposure to the miR-200b/c mimic also reduced the p38 and smad3 phosphorylation levels in RLE-6TN cells (Figures 11d and e).
Effects of a miR-200b/c mimic on LPS/ TGF-β-induced EMT in RLE-6TN cells. The levels of ZEB1 (a) and ZEB2 (b) proteins, E-cadherin, vimentin, and α-SMA proteins (c), and p38 (d), and smad3 (e) phosphorylation levels in RLE-6TN cells were detected by western blotting after RLE-6TN cells were stimulated with LPS and TGF-β for 24 h following pretreatment with miR-200b or miR-200c. All data are expressed as the mean±s.d. from at least three replicate experiments. *P<0.05 and **P<0.01 vs the control group; $P<0.05 and $$P<0.01 vs the LPS+TGF-β group.
Compared with the LPS+TGF-β group, miR-200b, and miR-200c were upregulated by ZEB1/2 shRNA in RLE-6TN cells (Figures 11a and b). E-cadherin protein expression increased, whereas vimentin, α-SMA protein and p38 and smad3 phosphorylation levels decreased in response to ZEB1 shRNA and ZEB2 shRNA treatment in RLE-6TN cells (Figures 11c–e).
Discussion
Sepsis is a prominent cause in ICU patients with ARDS.22 LPS is a major component of endotoxin and is considered to be an important factor of sepsis that can promote the development of acute lung injury directly or indirectly.23 The application of LPS in animal studies successfully simulated the clinical pathological changes in patients with ARDS, which lays the foundation for exploring the pathogenesis and effective treatments. Previous research24 suggested that acute lung injury may develop into pulmonary fibrosis and that early pulmonary fibrosis is the key pathological process. The pathological manifestations of early pulmonary fibrosis included the injury of alveolar epithelial cells, the proliferation of fibroblasts and the deposition of ECM.25 Consistent with a previous study,19 our results also showed that LPS induced obvious pulmonary fibrosis. HE and Masson staining showed that inflammation was present in the early stage, and collagen fibers deposited in pulmonary interstitial in the later stage after LPS treatment.
After LPS stimulation in the lung tissue of mice, epithelial cells and alveolar structure were damaged. In addition, a large number of cytokines were released by the damaged epithelial cells and macrophages.26 In this experiment, we found that TGF-β levels in BALF and plasma were significantly greater than those in the control group after LPS treatment and gradually increased during the development of early pulmonary fibrosis. Thus, TGF-β was associated with pulmonary fibrosis and promoted the development of early pulmonary fibrosis after LPS-induced ARDS.
EMT is considered an important mechanism for the development of fibrosis and is usually accompanied by some changes in molecular markers.27 For example, the expression of the epithelial marker E-cadherin dropped and the expression of the mesenchymal markers vimentin and α-SMA increased significantly.28 Our experimental results showed that the expression of E-cadherin was decreased, while vimentin and α-SMA protein levels were increased during the development of early pulmonary fibrosis. These results suggested that EMT occurred after ARDS and thereby contributed to the development of early pulmonary fibrosis.
miRNA is an endogenous, non-coding, single-stranded small RNA that suppressed translation or degraded mRNA by targeting the 3'-UTR of mRNA.29 In this study, the results of the microarray assay showed that miR-200s were closely associated with LPS-induced early pulmonary fibrosis.
In recent years, scholars have found that miR-200s play an important role in the process of fibrosis and tumor development. It has been shown that miR-200a, miR-200b, and miR-200c were significantly downregulated in mice with IPF induced by bleomycin; similarly, miR-200a and miR-200c were also markedly reduced in patients with IPF.10 In addition, a previous study30 also revealed that the miR-200 family participated in a variety of pathological processes and negatively regulated mRNA and protein expression by targeting the 3'-UTR of ZEB1/2. The expression of miR-200 family proteins was increased and targeted multiple markers, including ZEB1 and ZEB2, in a metastatic non-small cell lung cancer cell line.31 However, miR-200c was decreased and targeted ZEBs in leiomyoma and endometrial cancer.32, 33 The results of this experiment demonstrated that the expression of miR-200b and miR-200c decreased, whereas the mRNA and protein levels of their targets ZEB1 and ZEB2 gradually increased during the development of early pulmonary fibrosis. Interestingly, the expression of miR-200b/c decreased from day 3 onwards. However, the mRNA expression of their targets, ZEB1/2, had increased 21 days after LPS treatment. The complex regulatory mechanisms lead to differences in time. Moreover, the overexpression of miR-200b/c in local lung tissue significantly decreased ZEB1/2 mRNA and protein levels. These results suggested that miR-200b/c and their targets ZEB1/2 were closely related to early pulmonary fibrosis, and miR-200b/c play a key role in the development of early pulmonary fibrosis by negatively regulating ZEB1 and ZEB2.
Importantly, researchers also discovered that regulation of the miR-200 family could alleviate fibrosis or suppress the development of tumors. Treatment with a miR-200b precursor can ameliorate renal tubule-interstitial fibrosis.34 The overexpression of miR-200a inhibited the migration and invasion of CD133/1+ ovarian stem cells and NPC cells by targeting ZEB2.35, 36 The up-regulation of miR-200b suppressed cell growth, migration, invasion, and metastasis by targeting ZEB2 in human gastric cancer cell lines.37 Our experimental results showed that the overexpression of miR-200b/c in local lung tissue reduced ZEB1 and ZEB2 expression, markedly decreased TGF-β levels in BALF, reduced LPS-induced pulmonary inflammation and fibrosis, upregulated the expression of E-cadherin, and significantly suppressed the expression of vimentin and α-SMA proteins. Consequently, our study demonstrated that miR-200b/c attenuated LPS-induced early pulmonary fibrosis by inhibiting ZEB1/2.
Some researchers proposed that ZEB1 and ZEB2 could bind to the E-box region of the miR-200 gene promoter and inhibit the expression of miR-200s. Thus, miR-200s and their targets ZEB1/2 formed a reciprocal, negative feedback loop and maintained the balance of the body.31, 38 However, the ZEB/miR-200 feedback loop was also the molecular motor of cellular plasticity at the crossroads of signal transduction in development and disease.39, 40 In this study, miR-200b/c and ZEB1/2 were negatively correlated in LPS-induced early pulmonary fibrosis. Moreover, we also found that the overexpression of miR-200b/c decreased ZEB1/2 mRNA and protein levels, whereas the silencing of ZEB1/2 increased miR-200b and miR-200c expression in lung tissue and RLE-6TN cells. The silencing of ZEB1/2 led to similar effects as the overexpression of miR-200b/c in the development of pulmonary fibrosis. Therefore, the ZEB/miR-200 feedback loop might have a critical role in the development of early pulmonary fibrosis, and the regulation of the ZEB/miR-200 feedback loop could relieve pulmonary fibrosis.
ZEB is known as a transcriptional inhibitor of E-cadherin. ZEB inhibited the expression of E-cadherin via direct binding of its zinc finger to the E-box of the E-cadherin gene promoter, thereby inducing the epithelial–mesenchymal transition.41 Our experimental results showed that ZEB1/2 mRNA and protein expression increased, while E-cadherin protein levels were reduced in lung tissue and RLE-6TN cells after LPS treatment. The overexpression of miR-200b/c in local lung tissue or RLE-6TN cells resulted in decreased ZEB1/2 and increased E-cadherin expression. In addition, the protein level of E-cadherin was upregulated after the silencing of ZEB1/2. These results suggested that ZEB is negatively correlated to E-cadherin and promotes the development of early pulmonary fibrosis.
In addition, our in vitro study also found that LPS increased TGF-β levels in the supernatants of cultured RLE-6TN cells. The expression of E-cadherin was decreased, and the expression of ZEB1/2, vimentin and α-SMA protein increased when RLE-6TN cells were treated with LPS or TGF-β for 24 h. Treatment with LPS and TGF-β also upregulated the p38 and smad3 phosphorylation levels. Pretreatment with p38 or smad3 inhibitors in RLE-6TN cells suppressed p38 and smad3 phosphorylation, reversed miR-200b, and miR-200c expression, decreased ZEB1 and ZEB2 protein expression, upregulated E-cadherin levels and downregulated vimentin and α-SMA levels. Treatment with a miR-200b/c mimic downregulated ZEB1/2 protein expression, and treatment with ZEB1/2 shRNA negatively regulated miR-200b and miR-200c in RLE-6TN cells. Importantly, treatment with a miR-200b/c mimic or ZEB1/2 shRNA reduced LPS/TGF-β-induced EMT and decreased p38 and smad3 phosphorylation levels. These results suggested that LPS-induced EMT may be associated with the miR-200/ZEBs network and p38 MAPK and TGF-β/smad3 signaling pathways. Treatment with miR-200b/c mimics or ZEB-shRNA and the inhibition of p38 MAPK, and TGF-β/smad3 signaling pathways can reverse EMT.
In summary, the present study confirmed that the expression of miR-200b/c was decreased and involved in EMT by negatively regulating ZEB1/2, thereby promoting the development of LPS-induced early pulmonary fibrosis. The overexpression of miR-200b/c or silencing of ZEB1/2 expression can alleviate early pulmonary fibrosis and provide a novel treatment for patients. LPS-induced EMT in the process of early pulmonary fibrosis may be associated with p38 MAPK and TGF-β/smad3 signaling pathways and the inhibition of p38 MAPK and TGF-β/smad3 signaling pathways can reverse EMT.
Effects of ZEB1/2 shRNA on miR-200b/c and LPS/ TGF-β-induced EMT in RLE-6TN cells. miR-200b (a) and miR-200c (b) were examined by real-time PCR. The protein levels of E-cadherin, vimentin, and α-SMA (c), and p38 (d) and smad3 (e) phosphorylation levels in RLE-6TN cells were detected by western blotting after RLE-6TN cells were stimulated with LPS and TGF-β for 24 h following pretreatment with ZEB1 shRNA or ZEB2 shRNA. All data are expressed as the mean±s.d. from at least three replicate experiments. *P<0.05 and **P<0.01 vs the control group; $P<0.05 and $$P<0.01 vs the LPS+TGF-β group.
Accession codes
References
Luce JM . Acute lung injury and the acute respiratory distress syndrome. Crit Care Med 1998;26:369–376.
Cunningham AJ . Acute respiratory distress syndrome-two decades later. Yale J Biol Med 1991;64:387–402.
Marshall RP, Bellingan G, Webb S et al. Fibroproliferation occurs early in the acute respiratory distress syndrome and impacts on outcome. Am J Respir Crit Care Med 2000;162:1783–1788.
Burnham EL, Janssen WJ, Riches DWH et al. The fibroproliferative response in acute respiratory distress syndrome: mechanisms and clinical significance. Eur Respir J 2013;43:276–285.
Sun W, Julie Li YS, Huang HD et al. microRNA: a master regulator of cellular processes for bioengineering systems. Annu Rev Biomed Eng 2010;12:1–27.
Guo H, Ingolia NT, Weissman JS et al. Mammalian microRNAs predominantly act to decrease target mRNA levels. Nature 2010;466:835–840.
Bartel DP . MicroRNAs: genomics,biogenesis, mechanism, and function. Cell 2004;116:281–297.
Hammond SM . RNAi, microRNAs, and human disease. Cancer Chemother Pharmacol 2006;58:63–68.
Korpal M, Lee ES, Hu G et al. The miR-200 family inhibits epithelial-mesenchymal transition and cancer cell migration by direct targeting of E-cadherin transcriptional repressors ZEB1 and ZEB2. J Biol Chem 2008;283:14910–14914.
Yang S, Banerjee S, de Freitas A et al. Participation of miR-200 in pulmonary fibrosis. Am J Pathol 2012;180:484–493.
Park SM, Gaur AB, Lengyel E et al. The miR-200 family determines the epithelial phenotype of cancer cells by targeting the E-cadherin repressors ZEB1 and ZEB2. Genes Dev 2008;22:894–907.
Bendoraite A, Knouf EC, Garg KS et al. Regulation of miR-200 family microRNAs and ZEB transcription factors in ovarian cancer: evidence supporting a mesothelial-to-epithelial transition. Gynecol Oncol 2010;116:117–125.
Wilson MS, Wynn TA . Pulmonary fibrosis: pathogenesis, etiology and regulation. Mucosal Immunol 2009;2:103–121.
Chapman HA . Epithelial-mesenchymal Interactions in pulmonary fibrosis. Annu Rev Physiol 2011;73:413–435.
Ding XM . MicroRNAs: regulators of cancer metastasis and epithelial-mesenchymal transition (EMT). Chin J Cancer 2014;33:140–147.
Mongroo PS, Rustgi AK . The role of the miR-200 family in epithelial-mesenchymal transition. Cancer Biol Ther 2010;10:219–222.
Gregory PA, Bracken CP, Smith E et al. An autocrine TGF- /ZEB/miR-200 signaling network regulates establishment and maintenance of epithelial-mesenchymal transition. Mol Biol Cell 2011;22:1686–1698.
Xiong M, Jiang L, Zhou Y et al. The miR-200 family regulates TGF-beta1-induced renal tubular epithelial to mesenchymal transition through Smad pathway by targeting ZEB1 and ZEB2 expression. Am J Physiol Renal Physiol 2012;302:F369–F379.
Hui L, Shaohui D, Lina Y et al. Rapid pulmonary fibrosis induced by acute lung injury via a lipopolysaccharide three-hit regimen. Innate Immun 2009;15:143–154.
Li Y, Zeng Z, Li Y et al. Angiotensin-converting enzyme inhibition attenuates lipopolysaccharide-induced lung injury by regulating the balance between angiotensin-converting enzyme and angiotensin-converting enzyme 2 and inhibiting mitogen-activated protein kinase activation. Shock 2015;43:395–404.
Chen Q, Yang Y, Huang Y et al. Angiotensin-(1-7) attenuates lung fibrosis by way of Mas receptor in acute lung injury. J Surg Res 2013;185:740–747.
Ning F, Wang X, Shang L et al. Low molecular weight heparin may prevent acute lung injury induced by sepsis in rats. Gene 2015;557:88–91.
Takaoka Y, Goto S, Nakano T et al. Glyceraldehyde-3-phosphate dehydrogenase (GAPDH) prevents lipopolysaccharide (LPS)-induced, sepsis-related severe acute lung injury in mice. Sci Rep 2014;4:5204.
Du S, Li H, Cui Y et al. Houttuynia cordata inhibits lipopolysaccharide-induced rapid pulmonary fibrosis by up-regulating IFN-gamma and inhibiting the TGF-beta1/Smad pathway. Int Immunopharmacol 2012;13:331–340.
Barkauskas CE, Noble PW . Cellular mechanisms of tissue fibrosis. 7. New insights into the cellular mechanisms of pulmonary fibrosis. Am J Physiol Cell Physiol 2014;306:C987–C996.
Kim KK, Kugler MC, Wolters PJ et al. Alveolar epithelial cell mesenchymal transition develops in vivo during pulmonary fibrosis and is regulated by the extracellular matrix. Proc Natl Acad Sci USA 2006;103:13180–13185.
Tellez CS, Juri DE, Do K et al. EMT and stem cell-like properties associated with miR-205 and miR-200 epigenetic silencing are early manifestations during carcinogen-induced transformation of human lung epithelial cells. Cancer Res 2011;71:3087–3097.
Vyas-Read S, Wang W, Kato S et al. Hyperoxia induces alveolar epithelial-to-mesenchymal cell transition. Am J Physiol Lung Cell Mol Physiol 2014;306:L326–L340.
He L, Hannon GJ . MicroRNAs: small RNAs with a big role in gene regulation. Nat Rev Genet 2004;5:522–531.
Magenta A, Cencioni C, Fasanaro P et al. miR-200c is upregulated by oxidative stress and induces endothelial cell apoptosis and senescence via ZEB1 inhibition. Cell Death Differ 2011;18:1628–1639.
Pacurari M, Addison JB, Bondalapati N et al. The microRNA-200 family targets multiple non-small cell lung cancer prognostic markers in H1299 cells and BEAS-2B cells. Int J Oncol 2013;43:548–560.
Chuang TD, Panda H, Luo X et al. miR-200c is aberrantly expressed in leiomyomas in an ethnic-dependent manner and targets ZEBs, VEGFA, TIMP2, and FBLN5. Endocr Relat Cancer 2012;19:541–556.
Panda H, Pelakh L, Chuang TD et al. Endometrial miR-200c is altered during transformation into cancerous states and targets the expression of ZEBs, VEGFA, FLT1, IKKbeta, KLF9, and FBLN5. Reprod Sci 2012;19:786–796.
Oba S, Kumano S, Suzuki E et al. miR-200b precursor can ameliorate renal tubulointerstitial fibrosis. PloS ONE 2010;5:e13614.
Wu Q, Guo R, Lin M et al. MicroRNA-200a inhibits CD133/1+ ovarian cancer stem cells migration and invasion by targeting E-cadherin repressor ZEB2. Gynecol Oncol 2011;122:149–154.
Xia H, Ng SS, Jiang S et al. miR-200a-mediated downregulation of ZEB2 and CTNNB1 differentially inhibits nasopharyngeal carcinoma cell growth, migration and invasion. Biochem Biophys Res Commun 2010;391:535–541.
Kurashige J, Kamohara H, Watanabe M et al. MicroRNA-200b regulates cell proliferation, invasion, and migration by directly targeting ZEB2 in gastric carcinoma. Ann Surg Oncol 2012;19:S656–S664.
Reddy MA, Jin W, Villeneuve L et al. Pro-inflammatory role of microrna-200 in vascular smooth muscle cells from diabetic mice. Arterioscler Thromb Vasc Biol 2012;32:721–729.
Brabletz S, Brabletz T . The ZEB/miR-200 feedback loop—a motor of cellular plasticity in development and cancer? EMBO Rep 2010;11:670–677.
Chua HL, Bhat-Nakshatri P, Clare SE et al. NF-kappaB represses E-cadherin expression and enhances epithelial to mesenchymal transition of mammary epithelial cells: potential involvement of ZEB-1 and ZEB-2. Oncogene 2007;26:711–724.
Das S, Becker BN, Hoffmann FM et al. Complete reversal of epithelial to mesenchymal transition requires inhibition of both ZEB expression and the Rho pathway. BMC Cell Biol 2009;10:94.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
The pulmonary fibrosis triggered in the early stage of acute respiratory distress syndrome (ARDS) contributes to poor prognosis. An early pulmonary fibrosis mouse model of this syndrome was developed via a lipopolysaccharide three-hit regimen. His study demonstrates that miR-200b/c is down-regulated while ZEB1/2 is up-regulated in this model. miR-200b/c exerts a protective effect by targeting ZEB//2, which may be associated with inhibitiom of p38 MAPK and TGF-β/mad3 signaling pathways.
Rights and permissions
About this article
Cite this article
Cao, Y., Liu, Y., Ping, F. et al. miR-200b/c attenuates lipopolysaccharide-induced early pulmonary fibrosis by targeting ZEB1/2 via p38 MAPK and TGF-β/smad3 signaling pathways. Lab Invest 98, 339–359 (2018). https://doi.org/10.1038/labinvest.2017.123
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/labinvest.2017.123
This article is cited by
-
Differential DNA methylation landscape of miRNAs genes in mice liver fibrosis
Molecular Biology Reports (2024)
-
Mesenchymal stem cell-derived extracellular vesicles prevent the formation of pulmonary arterial hypertension through a microRNA-200b-dependent mechanism
Respiratory Research (2023)
-
Knockdown of lncRNA-ASLNC12002 alleviates epithelial–mesenchymal transition of type II alveolar epithelial cells in sepsis-induced acute respiratory distress syndrome
Human Cell (2022)
-
MSC-derived exosomes carrying a cocktail of exogenous interfering RNAs an unprecedented therapy in era of COVID-19 outbreak
Journal of Translational Medicine (2021)
-
MiR-200b in heme oxygenase-1-modified bone marrow mesenchymal stem cell-derived exosomes alleviates inflammatory injury of intestinal epithelial cells by targeting high mobility group box 3
Cell Death & Disease (2020)