Abstract
Mutant forms of transthyretin (TTR) cause the most common type of autosomal-dominant hereditary systemic amyloidosis. In addition, wild-type TTR causes senile systemic amyloidosis, a sporadic disease seen in the elderly. Although spontaneous development of TTR amyloidosis had not been reported in animals other than humans, we recently determined that two aged vervet monkeys (Chlorocebus pygerythrus) spontaneously developed systemic TTR amyloidosis. In this study here, we first determined that aged vervet monkeys developed TTR amyloidosis and showed cardiac dysfunction but other primates did not. We also found that vervet monkeys had the TTR Ile122 allele, which is well known as a frequent mutation-causing human TTR amyloidosis. Furthermore, we generated recombinant monkey TTRs and determined that the vervet monkey TTR had lower tetrameric stability and formed more amyloid fibrils than did cynomolgus monkey TTR, which had the Val122 allele. We thus propose that the Ile122 allele has an important role in TTR amyloidosis in the aged vervet monkey and that this monkey can serve as a valid pathological model of the human disease. Finally, from the viewpoint of molecular evolution of TTR in primates, we determined that human TTR mutations causing the leptomeningeal phenotype of TTR amyloidosis tended to occur in amino acid residues that showed no diversity throughout primate evolution. Those findings may be valuable for understanding the genotype–phenotype correlation in this inherited human disease.
Similar content being viewed by others
Main
Amyloidosis is a protein conformational disorder characterized by extracellular accumulation of amyloid fibrils derived from various proteins.1, 2 Thus far, 27 distinct protein precursors of amyloid fibrils have been identified as causing different kinds of amyloidosis, such as Alzheimer's disease, prion disease, and type 2 diabetes.3 In each type of amyloidosis, certain characteristics, such as aging, genetic mutation, inflammation, and tumors, can stimulate disease-causing polymerization of functional soluble proteins in the body.
Mutant forms of transthyretin (TTR) cause the most common type of autosomal-dominant hereditary systemic amyloidosis.4, 5, 6 In addition, wild-type TTR causes senile systemic amyloidosis, a sporadic disease seen in the elderly.7 TTR is mainly synthesized by the liver, forms a homotetramer that has a dimer of dimers configuration in the bloodstream, and acts as a plasma transport protein for thyroid hormone and retinol-binding protein with vitamin A.8 Destabilization of TTR tetramers is widely believed to be a critical step in amyloid formation.9, 10 To date, 120 TTR mutations have been identified.6, 7 Although 14 TTR mutations are nonamyloidogenic, other TTR mutations induce amyloidosis, which can be classified into several phenotypes such as neuropathy (peripheral neuropathy (PN) type), commonly known as familial amyloidotic polyneuropathy (FAP); cardiomyopathy (C type), also known as familial amyloidotic cardiomyopathy; vitreous opacity (V type); and leptomeningeal amyloidosis (LM type), which causes central nervous symptoms. Of those pathogenic TTR mutations, Val30Met was the first to be identified and is the most well-known mutation causing the PN type of amyloidosis found throughout the world, including Portugal, Sweden, and Japan.4, 5 In the United States, however, the most prevalent TTR mutation is Val122Ile. Approximately 3–4% of African Americans have this mutation, which causes late-onset cardiac amyloidosis.11
Various kinds of animals other than humans are well known to develop several kinds of amyloidosis, such as amyloid A, amyloid β (Aβ), and islet amyloid polypeptide (IAPP) amyloidosis.3 Although papers indicating that several transgenic rodents possessing mutant human TTRs developed human TTR deposits in different tissues have been published,12, 13 spontaneous development of TTR amyloidosis in animals other than humans had not been reported. We recently determined, however, that two aged vervet monkeys (Chlorocebus pygerythrus) spontaneously developed systemic TTR amyloidosis.14, 15 However, the pathogenesis of TTR amyloidosis in vervet monkeys was still unclear.
This study therefore investigated the clinicopathological features of TTR amyloidosis in vervet monkeys, elucidated the pathogenesis of TTR amyloidosis in these monkeys, and verified a pathological relationship between TTR amyloidosis in vervet monkeys and the disease in humans. The rationale for this study relates to our need in medical research for valid animal models of pathological conditions that mimic human diseases.
SUBJECTS AND METHODS
Animals
Vervet monkeys and cynomolgus monkeys were maintained at the Tsukuba Primate Research Center for Medical Science at the National Institute of Biomedical Innovation (NIBIO, Ibaraki, Japan). Those monkeys were individually housed in stainless steel cages under temperature conditions between 23 and 27 °C, humidity between 50 and 70%, 12 air changes/h, and a 12/12-h light/dark cycle, and were fed 70 g of commercial monkey chow (Type AS, Oriental Yeast, Chiba, Japan) and 200 g of fruits daily. Ketamine hydrochloride (Ketalar, 10 mg/kg; Daiichi-Sankyo, Tokyo, Japan) was used to induce anesthesia for clinical procedures such as blood sampling and clinical examinations. Tissue specimens were collected at necropsy immediately after their deaths and were fixed in 10% buffered formalin for histopathological examinations. Tissue specimens for evaluating mRNA levels were immediately frozen with liquid nitrogen and were kept at −80 °C. Necropsied cases in zoos were also employed for histopathological examinations (Supplementary Tables S1 and S2).
Histological and Immunohistochemical Studies
Tissue specimens from the primates studied (Supplementary Tables S1 and S2) stained with alkaline Congo red and hematoxylin. For immunohistochemistry, a polyclonal rabbit anti-human TTR antibody (Dako, Glostrup, Denmark) (1:100 dilution), a monoclonal mouse anti-human IAPP antibody (Dako) (1:100 dilution), and a monoclonal mouse anti-human IAPP antibody (Abcam, Cambridge, UK) (1:100 dilution) were utilized, as described previously.13
Electron Microscopy
Post-mortem cardiac samples were fixed first in 4% paraformaldehyde and 1% glutaraldehyde solution and then in 1% OsO4, after which they were embedded in Epon. Ultrathin sections were stained with 4% uranyl acetate and lead citrate and were examined with a transmission electron microscope (H-7500; Hitachi, Tokyo, Japan), as described previously.16
Extraction of Amyloid Proteins and Immunoblotting
We used the biochemical methods of Kaplan et al17 to extract amyloid proteins from 30 formalin-fixed, paraffin-embedded, amyloid-containing cardiac tissue specimens that had been sectioned at a thickness of 3 μm. Isolated tissue pellets incubated at 90 °C for 15 min in Laemmli sample buffer (Bio-Rad, Hercules, CA, USA) containing 8 M urea were subjected to SDS-PAGE and were then transferred to nitrocellulose membranes (Bio-Rad). Immunoblotting with the polyclonal rabbit anti-human TTR antibody (Dako) (1:1000 dilution) was performed as described previously.13
Echocardiography and Thoracic Radiography
All living vervet monkeys, which were kept in the Tsukuba Primate Research Center, and age- and sex-matched cynomolgus monkeys were used for echocardiographic studies. Echocardiographic images were obtained with the ProSound SSD-5000 (Aloka, Tokyo, Japan), as described previously.18 Thoracic radiographs were obtained by using the C-arm Radiography System (Siemens, Erlangen, Germany).
Measurements of TTR and Atrial Natriuretic Peptide Concentrations
Serum TTR concentrations were measured by means of nephelometry. Plasma atrial natriuretic peptide (ANP) concentrations were measured by a chemiluminescent enzyme immunoassay (Shionogi, Osaka, Japan).
TTR Gene Analyses in Primates
PCR amplification by direct DNA sequencing was accomplished with the use of ABI BigDye Terminator reagents (Applied Biosystems, Foster City, CA, USA) on the 3130 Genetic Analyzer (Applied Biosystems). We utilized specific primers to evaluate sequences of TTR genes in these primates (Supplementary Table S3). We inferred an evolutionary tree for the TTR gene by using the neighbor-joining method with the MEGA5 program.19
Mass Spectrometric Analysis of Serum TTR
Serum samples diluted 1:50 with 50 mM Tris-HCl pH 7.0 were used for evaluation. Surface-enhanced laser desorption/ionization time-of-flight mass spectrometry (SELDI-TOF MS) (Bio-Rad) analyses with a strong anion exchange surface Q10 chip were performed as described previously.20
Real-Time PCR to Evaluate TTR mRNA Levels in Tissues
Total RNA was isolated from frozen tissue specimens by use of the RNeasy Kit (Qiagen, Hilden, Germany). Then, reverse transcription (RT) was performed with the PrimeScript RT reagent Kit (Takara Bio, Shiga, Japan). Real-time PCR was performed with SYBR Premix DimerEraser (Takara Bio) and the LightCycler 480 system (Roche Diagnostics GmbH, Penzberg, Germany). The primers for detecting TTR and GAPDH are provided in Supplementary Table S3.
Expression and Purification of TTR in Escherichia Coli
Recombinant TTRs of vervet and cynomolgus monkeys were used in this study. We isolated and cloned full-length cDNAs of vervet and cynomolgus monkey TTR from liver samples and used these cDNAs for generating the pQE plasmid (Qiagen) containing cDNA for each TTR. The sequences of the inserted DNA segments were verified by DNA sequencing with a DNA sequencing kit (Applied Biosystems) with pQE30 sequencing primers (Qiagen). The plasmids were transformed into competent M15 cells (Qiagen). The recombinant TTRs were expressed and purified as described elsewhere.21
Evaluation of the Stability of TTR Tetramers
To evaluate the stability of TTR tetramers to urea denaturation, samples were incubated (25 °C, 12 h) with buffers containing concentrations of urea as described previously.21 TTR was detected by silver staining with the ProteoSilver Silver Stain Kit (Sigma, St Louis, MO, USA). Band intensities were quantified by using the NIH ImageJ program (http://rsbweb.nih.gov/ij/).22
Amyloid Fibril Formation and Thioflavin T (ThT)-Binding Assay
Amyloid fibril formation of recombinant TTR was evaluated as described previously.23 Recombinant proteins were diluted in 50 mM glycine-HCl (pH 3.0 or pH 4.0) containing 100 mM NaCl. TTR samples were prepared to a final concentration of 20 μM and were then incubated at 37 °C. Aliquots were collected for measurement of the extent of ThT fluorescence, which was measured with a Hitachi F-2000 spectrofluorimeter (Hitachi). An excitation wavelength of 442 nm and an emission wavelength of 489 nm were used for all assays. The reaction mixture contained 5 mM ThT and 50 mM glycine-NaOH buffer (pH 9.5); 5 μl of 20 μM TTR solution was added to 1 ml of this reaction mixture.
Ethics
The studies described herein were performed in accordance with the recommendations of the Weatherall Report, ‘The use of non-human primates in research’ (http://www.mrc.ac.uk/Utilities/Documentrecord/index.htm?d=MRC003440), and were approved by the ethics review committees of Kumamoto University, National Institute of Biomedical Innovation, and Azabu University.
Statistical Analysis
Data were evaluated with Pearson's χ2 test or Student's t-test and ANOVA. All analyses were performed with JMP version 5.1 (SAS Institute Japan, Tokyo, Japan). P-values of <0.05 were regarded as statistically significant.
RESULTS
Amyloid Deposits in Various Nonhuman Primates: Histopathological Findings
Histopathological investigations using 124 post-mortem cardiac specimens obtained from nonhuman primates revealed that three of six aged vervet monkeys had amyloid deposits derived from TTR (Figures 1a and b, Supplementary Table S1), whereas the other primate species did not. Electron microscopy revealed haphazardly arranged rigid amyloid fibrils in the heart in these vervet monkeys (Figure 1c). Vervet monkeys also developed TTR amyloid deposits in systemic organs and tissues including the gastrointestinal tract (Figure 1d), subcutaneous adipose tissue (Figure 1e), lung, tongue, and vascular walls (Figures 1g and h). Amyloid deposits were not found in the kidney glomerulus (Figures 1g and h), however, a site with severe amyloid deposits in most types of systemic amyloidosis. We also confirmed by means of immunoblotting that amyloid proteins extracted from cardiac specimens reacted with anti-TTR antibody (Figure 1f). In this study, we did not find lesions in monkey tissues that were positive for TTR and negative for Congo red. In addition, Aβ amyloid deposits in the brain and IAPP amyloid deposits in the pancreatic islet developed with age in both vervet monkeys and cynomolgus monkeys (Figures 1i and j, Supplementary Table S2), but TTR amyloid deposits developed only in vervet monkeys.
Histopathological features of aged vervet monkeys. TTR amyloid deposits in the heart (a–c), duodenum (d), subcutaneous fat (e), and kidney (g, h) of an aged vervet monkey. (a, g) Congo red staining under polarized light; (b, d, e, h) immunohistochemical staining using anti-TTR antibody; and (c) electron micrograph of amyloid fibrils in the cardiac specimen. Arrowheads: amyloid deposits in the vascular wall; arrows: absence of amyloid deposits in the kidney glomerulus. (f) Silver stain (lane 1) and immunoblotting using anti-TTR antibody (lane 2) of amyloid proteins extracted from cardiac amyloid deposits. Aged monkeys also developed amyloid β (Aβ) amyloid deposits in the brain (i; immunohistochemical staining using anti-Aβ antibody) and IAPP amyloid deposits in the pancreas (j; immunohistochemical staining using anti-IAPP antibody). is, islet IAPP amyloid deposit; p, Aβ amyloid deposits in senile plaques; v, vascular Aβ amyloid deposits.
Cardiac Function of Living Vervet Monkeys and Cynomolgus Monkeys
We investigated the functioning of the heart in living vervet monkeys and cynomolgus monkeys that lived in captivity in an experimental facility. As Table 1 shows, almost half of the aged vervet monkeys had abnormal cardiac findings, such as arrhythmia, increased cardiothoracic ratio, increased plasma ANP concentrations, and reduced ejection fraction (EF) (Figures 2a–c), but cynomolgus monkeys did not have those abnormal findings. Cardiac diastolic function could not be evaluated by means of echocardiography, because these monkeys generally had rapid heart rates and much smaller hearts than humans. In vervet monkeys, the occurrence of cardiac symptoms correlated with sex (P=0.016) (Table 1).
TTR Sequences in the Vervet Monkey and Other Primates
All of the vervet monkeys and one malbrouck monkey (Chlorocebus cynosuros), which belongs to the same genus as the vervet monkey, had the TTR Ile122 allele (Figures 3 and 4), which is well known as a mutation-causing TTR amyloidosis in humans, whereas other primates had the TTR Val122 allele (Figure 3). Except for the change at position 122, the other amino acid sequences of vervet monkey TTR were identical to TTR sequences in three other species of Old World monkeys: the cynomolgus monkey, rhesus macaque, and hamadryas baboon (Figure 3). Studies utilizing SELDI-TOF MS revealed that the measured mass of serum TTR was almost identical to the theoretical mass of TTR calculated on the basis of the TTR sequences in each monkey species (Figures 4c and d). We also investigated TTR gene sequences in 17 vervet monkeys and 15 cynomolgus monkeys and found the polymorphism Val/Ile at position 5 in both monkey species (Figure 4e), but this polymorphism had no correlation with TTR amyloidosis. In addition, cynomolgus monkeys possessed several other TTR gene polymorphisms (Figure 4e).
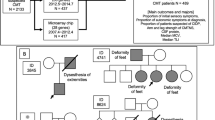
TTR amino acid sequence alignment for the 15 primate species, and human TTR mutations. The shaded area indicates conserved sequences in the primates. *Conserved amino acid residues in all 15 primates; †sequence data examined in this study; ‡sequence data cited from GenBank; ND, not determined. §Mutation-causing amyloid PN type; ¶mutation-causing amyloid C type; ∥mutation developing LM amyloid deposits causing CNS symptoms; **mutation developing V-type amyloid deposits causing visual disturbance; and ††with shading: nonamyloidogenic mutation. Del, deletion of amino acid residue.
Analyses of TTR gene sequences and serum TTR in monkeys. (a, c) TTR gene sequence at position 122. Cynomolgus monkeys had the TTR Val122 allele coded by GTC, which was identical to the allele in healthy humans, but vervet monkeys had the TTR Ile122 allele coded by ATC, which is a well-known mutation-causing TTR amyloidosis in humans. (b, d) SELDI-TOF MS analyses of serum TTR in the cynomolgus monkey (c) and the vervet monkey (d). (e) Polymorphism of TTR sequences in vervet monkeys and cynomolgus monkeys. *According to Pearson's χ2 test, comparing each group with the other groups.
Genetic analyses also revealed that TTRs of apes, Old World monkeys, and New World monkeys had 95–98%, 93–94%, and 76–81% amino acid homologies to human TTR, respectively (Figure 3). Furthermore, we found that all five species of New World monkeys showed a deficiency of three amino acids in the N-terminal side of mature TTR (from position 4 to position 6) compared with TTRs of the other primates. An evolutionary tree based on these primate TTR gene sequences was also developed (Supplementary Figure S1).
Expression and Serum Concentration of TTR in Vervet Monkeys and Cynomolgus Monkeys
Real-time PCR revealed that vervet monkeys expressed the TTR gene in the liver, choroid plexus, eye, and pancreas (Figure 5a), which are locations of TTR gene expression in humans and rodents. Cynomolgus monkeys also expressed the TTR gene in the liver to the same degree as did vervet monkeys (Figure 5a). However, serum TTR concentrations in vervet monkeys were less than half of those in cynomolgus monkeys (Figure 5b). Serum TTR concentrations in vervet monkeys with and without cardiac dysfunction did not differ (Figure 5c). Serum TTR concentrations also showed no significant sex differences (male: 75.2±6.8, female: 82.3±16.8 mg/l, P = 0.494) in this study.
TTR gene expression and serum TTR concentrations in cynomolgus monkeys and vervet monkeys. (a) TTR gene expression in cynomolgus monkeys in the liver (n=5) and in vervet monkeys in various tissues including the liver. (b, c) Serum TTR concentrations measured by means of nephelometry. (b) Comparison of serum TTR concentrations in 15 cynomolgus monkeys (male: n=6, female: n=9) and 13 vervet monkeys (male: n=4, female: n=9). *P<0.0001. (c) Serum TTR concentrations of vervet monkeys with (EF <50%, n=4) and without (EF >50%, n=9) cardiac dysfunction. Error bars show the s.d.
Stability and Amyloid Formation of Recombinant Monkey TTRs
To investigate the role of the TTR Ile122 allele on TTR stability and amyloid formation in the vervet monkey, we generated recombinant monkey TTRs. The recombinant TTR of the vervet monkey showed a significantly greater tendency to dissociate to monomers under the influence of urea-mediated denaturation stress than recombinant TTR of the cynomolgus monkey, which had the Val122 allele (Figures 6a–c). Furthermore, the ThT-binding assay revealed that the recombinant TTR protein of the vervet monkey formed more amyloid fibrils in vitro than did that of the cynomolgus monkey (Figure 6d).
Stability and amyloid fibril formation of recombinant monkey TTRs. (a–c) Stability of the tertiary structure of recombinant monkey TTRs to urea-mediated denaturation stress. (a) Silver staining of recombinant monkey TTRs cross-linked by glutaraldehyde after denaturation stress induced by different urea concentrations (0, 4.5, and 9 M). (b) Relative intensities of each molecular form of TTR after denaturation stress induced by 9 M urea. (c) Relative intensities of each molecular form of TTR after denaturation stress induced by 4.5 M urea. (d) In vitro fibril formation of recombinant monkey TTRs. Samples were incubated for 120 h at pH 3.0 or pH 4.0. *P<0.05 (vs cynomolgus monkey). Error bars show the s.d.
Human TTR Mutations and the Diversity of TTR Amino Acid Sequences in Primates
In Figure 3, we provided human TTR mutations and compared those mutations with the TTR sequences of nonhuman primates. Although as many as 120 TTR mutations have been reported in humans, nonhuman primates evidenced only three amyloidogenic TTR alleles—Thr81 in two New World monkeys (common marmoset (Callithrix jacchus) and black-bearded saki (Chiropotes satanas)), Val107 in all New World monkeys, and Ile122 in the vervet monkey—and one nonamyloidogenic TTR allele—His104 in all Old and New World monkeys.
In addition, to determine the genotype–phenotype correlation for human hereditary TTR amyloidosis, we investigated the relationship between the distribution of pathogenic mutations in human TTR and the diversity of amino acid sequences in primate TTRs (Figure 3). As Figure 7a demonstrates, the ratios of the number of human TTR mutations causing two amyloidosis phenotypes, PN and LM, to the number of uniform TTR amino acid residues were higher than the ratios for diverse amino acid residues, whereas for the other phenotypes, these ratios were almost equal. All mutations causing LM amyloidosis were found only in uniform amino acid residues in the primates (Figure 7b).
Difference in occurrence of human pathogenic TTR mutations in diverse and uniform amino acid residues in primates. (a) Difference in the ratio of the number of TTR mutations causing various human phenotypes to the number of diverse and uniform TTR amino acid residues. (b) TTR mutations causing different human phenotypes as related to diverse and uniform TTR amino acid residues. Non-amy, nonamyloidogenic. P-values according to Pearson's χ2 test, comparing each group with the other groups. *P<0.05.
DISCUSSION
To our knowledge, the vervet monkey is the first species other than humans to develop TTR amyloidosis spontaneously. We initially determined that only vervet monkeys developed TTR amyloidosis and that almost half of the aged vervet monkeys showed cardiac dysfunctions, such as arrhythmia, increased cardiothoracic ratio, increased plasma ANP concentration, and reduced EF. The occurrence of cardiac symptoms in the aged vervet monkeys correlated with sex (P=0.016), as is the case in human TTR amyloidosis.7, 24 In addition, all the vervet monkeys studied had the TTR Ile122 allele, which is known to be the mutation that causes TTR amyloidosis in humans, whereas other primates had the TTR Val122 allele. Except for Ile122, the amino acid sequence of vervet monkey TTR was identical to that of the cynomolgus monkey, which did not have TTR amyloid deposits or cardiac symptoms. These results suggest that the Ile122 allele has a critical role in TTR amyloidosis in the vervet monkey.
With regard to amyloidosis in humans, that 3–4% of African Americans have a heterozygous amino acid substitution from valine to isoleucine at position 122 (Val122Ile) of TTR is well known, and elderly individuals with this substitution are at high risk of developing TTR amyloidosis that affects mainly cardiac function.11 Several patients with a homozygous Val122Ile mutation reportedly showed more severe clinical symptoms of amyloidosis than did patients with the heterozygous mutation.24, 25 Although the reason why the TTR Ile122 allele occurs only in vervet monkeys remains to be determined, we suggest that the this allele may be subjected to positive selection through the evolution—both vervet monkeys, which originated in Africa and African Americans—and may provide certain functional advantages for living in Africa. Further studies should be undertaken to answer this question.
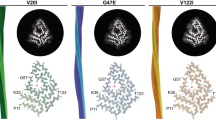
We also determined that the recombinant TTR of the vervet monkey carrying Ile122 allele was less stable and tended to form more amyloid fibrils than that of the cynomolgus monkey carrying Val122 allele. In the human TTR, residue Ile122 is located on the periphery of the H strand, which makes an antiparallel–sheet interaction with strand H of another monomer, stabilizing the dimer interface. It is also one of the residues involved in dimer-dimer interactions. Based on results from X-ray crystallography, Damas et al26 reported that the human TTR Val122Ile variant indicated an elongation of the dimer–dimer interactions present in the tetrameric molecule and consequently less stable molecules, with a higher propensity to dissociation. Jiang et al27 also reported that the human TTR Val122Ile mutation enhanced the rate of dissociation from tetramer to monomer, thus enhancing amyloid fibril formation, in vitro. Together, all these findings strongly support our working hypothesis that the Ile residue at position 122 has a critical role in TTR amyloid formation in the vervet monkey.
In addition, we determined that, compared with cynomolgus monkeys, vervet monkeys had lower TTR concentrations in the blood, whereas both species had identical TTR gene expression in the liver, which is the major organ that secretes TTR entering the bloodstream. Buxbaum et al28 reported that human TTR Val122Ile carriers had significantly lower serum TTR concentrations than did age-matched controls although the majority of such individuals did not have clinical symptoms. A recent in vitro study also indicated that highly destabilized mutant TTRs are subject to processing by intracellular quality control systems and are not efficiently secreted into the bloodstream.29 In view of these findings, we speculate that the TTR in vervet monkeys may also be degraded by intracellular quality control systems. Together, all these findings led us to conclude that aged vervet monkeys developed TTR amyloidosis because of the Ile122 allele and had pathological conditions mimicking those of patients with TTR Val122Ile amyloidosis.
Furthermore, we investigated a relationship between the diversity of amino acid sequences of TTR in primates and the distribution of human TTR mutations, and we determined that all TTR mutations causing the LM amyloidosis phenotype occurred in uniform amino acid residues in these primates. Certain studies suggested that some TTR mutations causing the LM amyloidosis phenotype were more unstable than were the other TTR mutations.29, 30 Also from the viewpoint of molecular evolution of primates, human TTR mutations causing the LM phenotype may occur in functionally and/or conformationally important amino acid residues, because those amino acid residues are maintained throughout primate evolution. These findings may be valuable for understanding the genotype–phenotype correlation in this inherited human disease.
In conclusion, we propose that vervet monkeys develop TTR amyloidosis because of the Ile122 allele and serve as a valid animal model of this inherited human disease. Moreover, we suggest that the genotype–phenotype correlation in TTR amyloidosis can be investigated from the viewpoint of molecular evolution in primates.
References
Merlini G, Seldin DC, Gertz MA . Amyloidosis: pathogenesis and new therapeutic options. J Clin Oncol 2011;29:1924–1933.
Benson MD . Genetics: clinical implications of TTR amyloidosis. In: Richardson SJ, Cody V (eds). Recent Advances in Transthyretin Evolution, Structure and Biological Functions. Springer: Heidelberg, 2009, pp 173–189.
Sipe JD, Benson MD, Buxbaum JN, et al. Amyloid fibril protein nomenclature: 2010 recommendations from the nomenclature committee of the International Society of Amyloidosis. Amyloid 2010;17:101–104.
Ando Y, Nakamura M, Araki S . Transthyretin-related familial amyloidotic polyneuropathy. Arch Neurol 2005;62:1057–1062.
Zeldenrust S, Benson MD . Familial and senile amyloidosis caused by transthyretin. In: Alvarado M, Kelly JW, Dobson CM (eds). Protein Misfolding Diseases: Current and Emerging Principles and Therapies. John Wiley and Sons: Hoboken, NJ, 2010, pp 795–815.
Connors LH, Lim A, Prokaeva T, et al. Tabulation of human transthyretin (TTR) variants, 2003. Amyloid 2003;10:160–184.
Westermark P, Bergström J, Solomon A, et al. Transthyretin-derived senile systemic amyloidosis: clinicopathologic and structural considerations. Amyloid 2003;10:48–54.
Buxbaum JN, Reixach N . Transthyretin: the servant of many masters. Cell Mol Life Sci 2009;66:3095–3101.
Colón W, Kelly JW . Partial denaturation of transthyretin is sufficient for amyloid fibril formation in vitro. Biochemistry 1992;31:8654–8660.
Lai Z, Colón W, Kelly JW . The acid-mediated denaturation pathway of transthyretin yields a conformational intermediate that can self-assemble into amyloid. Biochemistry 1996;35:6470–6482.
Jacobson DR, Pastore R, Pool S, et al. Revised transthyretin Ile 122 allele frequency in African-Americans. Hum Genet 1996;98:236–238.
Teng MH, Yin JY, Vidal R, et al. Amyloid and nonfibrillar deposits in mice transgenic for wild-type human transthyretin: a possible model for senile systemic amyloidosis. Lab Invest 2001;81:385–396.
Ueda M, Ando Y, Hakamata Y, et al. A transgenic rat with the human ATTR V30M: a novel tool for analyses of ATTR metabolisms. Biochem Biophys Res Commun 2007;352:299–304.
Nakamura S, Okabayashi S, Ageyama N, et al. Transthyretin amyloidosis and two other aging-related amyloidoses in an aged vervet monkey. Vet Pathol 2008;45:67–72.
Chambers JK, Kanda T, Shirai A, et al. Senile systemic amyloidosis in an aged savannah monkey (Chlorocebus aethiops) with tenosynovial degeneration. J Vet Med Sci 2010;72:657–659.
Misumi Y, Ando Y, Ueda M, et al. Chain reaction of amyloid fibril formation with induction of basement membrane in familial amyloidotic polyneuropathy. J Pathol 2009;219:481–490.
Kaplan B, Hrncic R, Murphy CL, et al. Microextraction and purification techniques applicable to chemical characterization of amyloid proteins in minute amounts of tissue. Methods Enzymol 1999;309:67–81.
Koie H, Ageyama N, Ono F, et al. Echocardiographic diagnosis of muscular ventricular septal defect in a cynomolgus monkey (Macaca fascicularis). Contemp Top Lab Anim Sci 2005;44:26–28.
Tamura K, Dudley J, Nei M, et al. MEGA4: Molecular Evolutionary Genetics Analysis (MEGA) software version 4.0. Mol Biol Evol 2007;24:1596–1599.
Ueda M, Misumi Y, Mizuguchi M, et al. SELDI-TOF mass spectrometry evaluation of variant transthyretins for diagnosis and pathogenesis of familial amyloidotic polyneuropathy. Clin Chem 2009;55:1223–1227.
Matsubara K, Mizuguchi M, Kawano K . Expression of a synthetic gene encoding human transthyretin in Escherichia coli. Protein Expr Purif 2003;30:55–61.
Abramoff MD, Magelhaes PJ, Ram SJ . Image processing with ImageJ. Biophotonics Int 2004;11:36–42.
Misumi Y, Ueda M, Fujimori H, et al. Transthyretin forms amyloid fibrils at physiological pH with ultrasonication. Amyloid 2008;15:234–239.
Connors LH, Prokaeva T, Lim A, et al. Cardiac amyloidosis in African Americans: comparison of clinical and laboratory features of transthyretin V122I amyloidosis and immunoglobulin light chain amyloidosis. Am Heart J 2009;158:607–614.
Hamour IM, Lachmann HJ, Goodman HJ, et al. Heart transplantation for homozygous familial transthyretin (TTR) V122I cardiac amyloidosis. Am J Transplant 2008;8:1056–1059.
Damas AM, Ribeiro S, Lamzin VS, et al. Structure of the Val122Ile variant transthyretin - a cardiomyopathic mutant. Acta Crystallogr D Biol Crystallogr 1996;52:966–972.
Jiang X, Buxbaum JN, Kelly JW . The V122I cardiomyopathy variant of transthyretin increases the velocity of rate-limiting tetramer dissociation, resulting in accelerated amyloidosis. Proc Natl Acad Sci USA 2001;98:14943–14948.
Buxbaum J, Koziol J, Connors LH . Serum transthyretin levels in senile systemic amyloidosis: effects of age, gender and ethnicity. Amyloid 2008;15:255–261.
Sekijima Y, Wiseman RL, Matteson J, et al. The biological and chemical basis for tissue-selective amyloid disease. Cell 2005;121:73–85.
Hammarström P, Sekijima Y, White JT, et al. D18G transthyretin is monomeric, aggregation prone, and not detectable in plasma and cerebrospinal fluid: a prescription for central nervous system amyloidosis? Biochemistry 2003;42:6656–6663.
Acknowledgements
We thank Hiroko Katsura for her technical support during histopathological investigations. The authors’ work was partially supported by a Grant-in-Aid for Scientific Research (B) 21253742 (Y Ando) and by Grants-in-Aid for Young Scientists (B) 21790541 (M Ueda) from the Ministry of Education, Culture, Sports, Science and Technology.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
The first animal model for senile systemic transthyretin (TTR) amyloidosis, a sporadic disease of the elderly, is described. Aged vervet monkeys can spontaneously develop systemic TTR amyloidosis and show cardiac dysfunction. Vervet monkeys have the TTR Ile122 allele, which is a frequent mutation causing human hereditary systemic TTR amyloidosis.
Rights and permissions
About this article
Cite this article
Ueda, M., Ageyama, N., Nakamura, S. et al. Aged vervet monkeys developing transthyretin amyloidosis with the human disease-causing Ile122 allele: a valid pathological model of the human disease. Lab Invest 92, 474–484 (2012). https://doi.org/10.1038/labinvest.2011.195
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/labinvest.2011.195