Abstract
The ankle-brachial blood pressure index (ABPI) has been recognized to have a predictive value for cardiovascular (CV) events and mortality in general or dialysis populations. However, the associations between ABPI and those outcomes have not been fully investigated in predialysis patients. The present study aimed to clarify the relationships between ABPI and both CV events and mortality in Japanese chronic kidney disease (CKD) patients not on dialysis. In this prospective observational study, we enrolled 320 patients with CKD stages 3–5 who were not on dialysis. At baseline, ABPI was examined and a low ABPI was defined as <0.9. CV events and all-cause deaths were examined in each patient. A Cox proportional hazards model was applied to determine the risk factors for CV events, as well as for mortality from CV and all causes. The median follow-up period was 30 months. CV events occurred in 56 patients and all-cause deaths occurred in 48, including 20 CV deaths. Multivariate analysis showed that age and low ABPI were risk factors for CV events. It was demonstrated that age, a history of cerebrovascular disease and low ABPI were determined as independent risk factors for CV mortality. In addition, age, body mass index and low ABPI were independently associated with all-cause mortality. In patients with CKD, low ABPI during the predialysis period is independently associated with poor survival and CV events, suggesting the usefulness of measuring ABPI for predicting CV events and patient survival in CKD.
Similar content being viewed by others
Introduction
Patients with chronic kidney disease (CKD) have high cardiovascular (CV) morbidity and mortality.1 Manifestations of CKD, such as hyperphosphatemia, hyperparathyroidism and chronic inflammation, are implicated in atherosclerosis in addition to traditional risk factors, such as smoking, diabetes, dyslipidemia and hypertension.2 CKD patients had more advanced arterial wall stiffness compared with healthy subjects,3 which is strongly associated with atherosclerosis.4 Therefore, the presence of CKD worsens CV disease outcomes because of advanced atherosclerosis in CKD patients.
The ankle-brachial blood pressure index (ABPI) is a simple, noninvasive and reliable method of evaluating systemic atherosclerosis and peripheral artery disease.5, 6 It was demonstrated that low ABPI levels, particularly those <0.90, are indicative of generalized atherosclerosis.7 An ABPI <0.9 is also associated with increased CV and all-cause mortality in non-CKD populations.8, 9, 10, 11, 12, 13 Several studies have also shown that a low ABPI monitored during a maintenance dialysis period is associated with the outcome of CV morbidity and mortality.14, 15, 16, 17, 18, 19 However, very few studies have documented the relationship between ABPI during the predialysis period and either CV events or mortality in predialysis patients.20, 21 Moreover, there have been very few studies investigating the relationship between low ABPI and CV events or mortality in Japanese CKD patients not on dialysis.20 The present study aimed to determine whether ABPI during the predialysis period is associated with CV events and with both CV and all-cause mortality in Japanese CKD patients.
Materials and Methods
In this prospective observational study, we enrolled 320 consecutive Japanese patients with CKD stages 3–5 not on dialysis, who were admitted to our hospital for evaluation of and education about CKD between January 2005 and September 2012. Patients with any malignancy or history of treatment for peripheral artery disease were excluded from this study. All patients provided written informed consent to the protocol, which was approved by the Ethics Committee of the National Kyushu Medical Center Hospital.
Blood samples (serum creatinine (SCr), C-reactive protein, hemoglobin, serum albumin and serum phosphorus levels) were obtained in the early morning after an overnight fast. Daily proteinuria was also measured. The estimated glomerular filtration rate (eGFR; ml min−1 per 1.73 m2) was calculated using the following new Japanese equation: 194 × SCr−1.094 × age−0.287 × 0.739 (if female).22
All enrolled patients were interviewed and clinically examined at presentation. Their medical histories and outpatient records were also evaluated in detail. Demographic information (age and sex), medication history and atherosclerotic risk factors (hypertension, history of smoking, dyslipidemia and diabetes mellitus) at presentation were recorded for each patient. Hypertension was defined as systolic blood pressure ⩾140 mm Hg or diastolic blood pressure ⩾90 mm Hg, or the current use of antihypertensive drugs. Dyslipidemia was defined as plasma triglycerides ⩾150 mg dl−1, plasma low-density lipoprotein cholesterol ⩾140 mg dl−1, plasma high-density lipoprotein cholesterol <40 mg dl−1 or the use of lipid-lowering drugs based on a history of dyslipidemia. Diabetes mellitus was defined as previous or current plasma fasting glucose ⩾126 mg dl−1 or the use of hypoglycemic agents. Present or past cigarette smoking was distinguished. Body mass index was calculated as weight in kg divided by height in m2. Blood pressure was measured at three separate times in a sitting position on the second day of hospitalization; the average of the three readings was recorded. Pulse pressures were calculated as the difference between systolic and diastolic blood pressures.
For the measurement of ABPI, bilateral arm systolic blood pressure and bilateral ankle systolic blood pressure (posterior tibial artery) were taken with the subject in a supine position, and the measurement for each leg and ipsilateral arm was used to calculate ABPI. Patients who had ABPI <0.9 in either leg were categorized as having low ABPI.23
CV events were defined as follows: procedures of percutaneous coronary intervention or coronary artery bypass grafting for ischemic heart disease, congestive heart failure or cerebrovascular disease (such as brain infarction and hemorrhage); procedures of carotid endarterectomy for internal carotid artery stenosis; and procedures of percutaneous transcatheter angioplasty, lower-limb amputation or bypass surgery for peripheral artery disease; dissecting aneurysm of the thoracic and/or abdominal aorta, rupture of thoracic and/or abdominal aortic aneurysm, pulmonary embolism or sudden death.
Statistical analysis
Continuous data are expressed as either the mean±s.d. or the median (interquartile range), depending on their distribution. Categorical data are expressed as numbers (with %). The significance of differences between ABPI <0.9 and ⩾0.9 was examined using the χ2 test for categorical data, the Wilcoxon’s rank-sum test for nonparametric data and the unpaired Student’s t-test for parametric data. A logistic regression analysis was performed to elucidate the associations between low ABPI and traditional and nontraditional CV risk factors. Covariates associated with low ABPI in univariate analysis were analyzed by multivariate analysis to determine the independent risk factors for low ABPI. A Cox proportional hazards model was also applied to elucidate the traditional and nontraditional CV risk factors associated with CV events and both mortality and all-cause mortality. Covariates associated with these outcomes that were significant in univariate analysis were selected as risk factors in multivariate analysis. The odds and hazard ratios and the 95% confidence interval were calculated for each variable. Survival curves were estimated by the Kaplan–Meier method and evaluated by the log-rank test. Data were analyzed using the JMP10 statistics package (SAS Institute, Cary, NC, USA). A P-value below 0.05 indicated a significant difference.
Results
The median age of the 320 patients (218 men and 102 women) in this study was 72 years (range, 30–92 years). The primary causes of renal disease were diabetic nephropathy (35%, 113 patients), hypertensive nephrosclerosis (33%, 104 patients), chronic glomerulonephritis (21%, 67 patients), other defined causes (8%, 27 patients) and unknown (3%, 9 patients). The median follow-up period was 30 months (range, 2–104 months). At the end of follow-up, 48 all-cause deaths were recorded. The causes of death were as follows: CV deaths in 20 patients, infection in 13, malignancy in 5, other defined causes in 8 and unknown in 2. In addition, CV events occurred in 56 patients.
The clinical characteristics of the patients with and without low ABPI are summarized in Table 1. Low ABPI was found in 42 patients (13%). The median age of patients with low ABPI was significantly higher than that of patients without low ABPI. The prevalences of smoking, diabetes mellitus and a history of ischemic heart disease or cerebrovascular disease were significantly higher in patients with low ABPI. Systolic, diastolic and pulse pressures were also significantly higher in patients with low ABPI, whereas body mass index was significantly lower. There were no significant differences in the values of serum albumin, C-reactive protein, hemoglobin, serum phosphorus, proteinuria and eGFR between the two groups.
Table 2 shows the results of logistic regression analysis of determinant factors for low ABPI. Univariate analysis demonstrated that age, smoking, pulse pressure, diabetes mellitus, history of ischemic heart disease and of cerebrovascular disease, and body mass index were significantly associated with low ABPI. Multivariate analysis showed that age, pulse pressure and history of cerebrovascular disease remained as independent determinant factors for low ABPI.
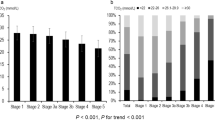
We analyzed the risk factors for CV events and both mortality and all-cause mortality using a Cox hazards analysis, as shown in Table 3. In multivariate analysis, age and low ABPI were independently associated with CV events. Age, a history of cerebrovascular disease and low ABPI were identified as independent risk factors for CV mortality. In addition, age, body mass index and low ABPI were independently associated with all-cause mortality. Figure 1 shows Kaplan–Meier curves of freedom from CV events (Figure 1a) and mortality (Figure 1b), as well as all-cause mortality (Figure 1c) in subjects with ABPI <0.9 and ⩾0.9. Patients with low ABPI experienced more CV events as well as both CV deaths and all-cause deaths.
The associations between ankle-brachial blood pressure index (ABPI) and cardiovascular (CV) events, as well as with mortality from CV and all causes. Kaplan–Meier curves with log-rank tests of freedom from CV events (a) and deaths (b), and all-cause deaths (c) according to groups with ABPI <0.9 and ⩾0.9.
Discussion
Previous studies demonstrated the relationships between low ABPI and both CV events and mortality in predialysis patients. One report addressed the association of low ABPI with CV and all-cause mortality, but not with CV events.21 In another report, clinical end points were defined as composite events of all-cause deaths or CV events.20 On the other hand, the present study investigated separately the effects of low ABPI on CV events as well as on CV and all-cause mortality; it was demonstrated that low ABPI is independently associated with all these clinical end points. Additionally, although there have been limited data regarding the risk factors for having low ABPI in CKD patients,24 our study simultaneously investigated those factors using a multivariate analysis to further explore the relationship between low ABPI and outcomes. In addition, given that very few studies regarding the association of low ABPI with outcomes have been conducted in Japanese predialysis patients,20 the results of the present study may contribute to the clarification of the relationship between low ABPI and outcomes in this population.
In previous studies, old age, diabetes mellitus, a history of ischemic heart disease or cerebrovascular disease, increased pulse pressure, low serum albumin and low eGFR levels were identified as risk factors for atherosclerosis in patients with CKD.25, 26, 27 In the present study, multivariate logistic regression analysis showed that pulse pressure, old age and a history of cerebrovascular disease were independent determinant factors for low ABPI. A previous study demonstrated that pulse pressure was a determinant factor for low ABPI in non-CKD patients.28, 29 On the other hand, patients with CKD exhibit vascular abnormalities, including arterial stiffness and early wave reflection, that contribute to elevated pulse pressure.30, 31 Pulse pressure was also positively and significantly associated with low ABPI in CKD patients.32 In addition, higher levels of pulse pressure have been associated with carotid stenosis,33 left ventricular hypertrophy,34 myocardial infarction,35 CV death36 and congestive heart failure37 in both normotensive and hypertensive populations. However, in the present study multivariate analysis showed that low ABPI, but not pulse pressure, was an independent risk factor for CV events and mortality. Taken together, these previous and present findings suggested that ABPI, rather than pulse pressure, was a useful method to predict CV events and mortality in CKD patients.
The present study also showed that low ABPI was an independent risk factor for all-cause mortality. No report thus far has explained clearly the association between low ABPI and all-cause mortality. Results of the National Health and Nutrition Examination Survey demonstrated that there are high prevalences of both traditional and nontraditional CV risk factors among persons with peripheral artery disease.38 In addition, the Atherosclerosis Risk In Communities (ARIC) study reported that more patients with peripheral artery disease had hypertension, diabetes and a smoking habit.39 In the present study, patients with low ABPI also had significantly higher prevalences of hypertension, diabetes, smoking, high pulse pressure and a history of ischemic heart and cerebrovascular disease compared with patients having normal ABPI. Previous studies demonstrated that hypertension,40 diabetes41 and smoking42 are independent risk factors for all-cause mortality in general populations. Other studies also showed that pulse pressure was an independent risk factor for all-cause mortality in patients with CKD stages 4 and 5,43 peritoneal dialysis44 and hemodialysis.45 All these clinical features might explain why patients with low ABPI had a higher mortality rate from CKD. However, risk factors such as pulse pressure and a history of cerebrovascular disease independently related to low ABPI were not associated with all-cause mortality in multivariate analysis. Therefore, the precise reason for the association between low ABPI and all-cause mortality has remained uncertain.
The present study has some limitations. First, the study subjects were in only one regional hospital; thus, the selection of patients was limited and the sample size was relatively small. Second, our study had an imbalanced gender ratio. Our study recruited the consecutive patients who were admitted to our hospital, and the number of male patients was two times the number of female patients. In general, male-predominant study groups tend to have a high risk of CV outcomes46, 47 and all-cause mortality. In patients on dialysis, previous studies with male predominance (>60%) have addressed the association between male gender and mortality; one report showed a significant association between male gender and all-cause mortality in a multivariate analysis,15 but another study did not observe such a relationship.16 In our present study, the univariate analysis showed that male gender was not associated with CV outcomes or all-cause mortality. Third, it has been reported that abnormally high ABPI (⩾1.3) predicts both CV mortality and all-cause mortality in CKD and hemodialysis patients.18, 19 However, we could not find an association between an abnormally high ABPI and CV events or death from CV or all causes, because only 18 patients had ABPI ⩾1.3 in the present study. A larger cohort study will be needed to avoid study bias and to document more precisely the association between low ABPI and CV events, as well as mortality from CV and all causes.
In conclusion, the present study demonstrated that low ABPI was independently associated with CV events as well as with mortality from CV and all causes. This finding suggests that ABPI measurement could have a predictive value for CV disease outcome and patient survival.
References
Herzog CA, Asinger RW, Berger AK, Charytan DM, Díez J, Hart RG, Eckardt KU, Kasiske BL, McCullough PA, Passman RS, DeLoach SS, Pun PH, Ritz E . Cardiovascular disease in chronic kidney disease. A clinical update from Kidney Disease: Improving Global Outcomes (KDIGO). Kidney Int 2011; 80: 572–586.
DeLoach SS, Mohler ER III . Peripheral arterial disease: a guide for nephrologists. Clin J Am Soc Nephrol 2007; 2: 839–846.
Shinohara K, Shoji T, Tsujimoto Y, Kimoto E, Tahara H, Koyama H, Emoto M, Ishimura E, Miki T, Tabata T, Nishizawa Y . Arterial stiffness in predialysis patients with uremia. Kidney Int 2004; 65: 936–943.
van Popele NM, Grobbee DE, Bots ML, Asmar R, Topouchian J, Reneman RS, Hoeks AP, van der Kuip DA, Hofman A, Witteman JC . Association between arterial stiffness and atherosclerosis: the Rotterdam Study. Stroke 2001; 32: 454–460.
Carter SA . Clinical measurement of systolic pressures in limbs with arterial occlusive disease. JAMA 1969; 207: 1869–1874.
Yao ST, Hobbs JT, Irvine WT . Ankle systolic pressure measurements in arterial disease affecting the lower extremities. Br J Surg 1969; 56: 676–679.
Zheng ZJ, Sharrett AR, Chambless LE, Rosamond WD, Nieto FJ, Sheps DS, Dobs A, Evans GW, Heiss G . Associations of ankle-brachial index with clinical coronary heart disease, stroke and preclinical carotid and popliteal atherosclerosis: the Atherosclerosis Risk in Communities (ARIC) Study. Atherosclerosis 1997; 131: 115–125.
Newman AB, Sutton-Tyrrell K, Vogt MT, Kuller LH . Morbidity and mortality in hypertensive adults with a low ankle/arm blood pressure index. JAMA 1993; 270: 487–489.
Leng GC, Fowkes FG, Lee AJ, Dunbar J, Housley E, Ruckley CV . Use of ankle brachial pressure index to predict cardiovascular events and death: a cohort study. BMJ 1996; 313: 1440–1444.
Newman AB, Tyrrell KS, Kuller LH . Mortality over four years in SHEP participants with a low ankle-arm index. J Am Geriatr Soc 1997; 45: 1472–1478.
Newman AB, Shemanski L, Manolio TA, Cushman M, Mittelmark M, Polak JF, Powe NR, Siscovick D . Ankle-arm index as a predictor of cardiovascular disease and mortality in the Cardiovascular Health Study. The Cardiovascular Health Study Group. Arterioscler Thromb Vasc Biol 1999; 19: 538–545.
Xu Y, Li J, Luo Y, Wu Y, Zheng L, Yu J, Ma J, Gu J, Hu D . The association between ankle-brachial index and cardiovascular or all-cause mortality in metabolic syndrome of elderly Chinese. Hypertens Res 2007; 30: 613–619.
Ankle Brachial Index Collaboration Fowkes FG, Murray GD, Butcher I, Heald CL, Lee RJ, Chambless LE, Folsom AR, Hirsch AT, Dramaix M, deBacker G, Wautrecht JC, Kornitzer M, Newman AB, Cushman M, Sutton-Tyrrell K, Fowkes FG, Lee AJ, Price JF, d'Agostino RB, Murabito JM, Norman PE, Jamrozik K, Curb JD, Masaki KH, Rodríguez BL, Dekker JM, Bouter LM, Heine RJ, Nijpels G, Stehouwer CD, Ferrucci L, McDermott MM, Stoffers HE, Hooi JD, Knottnerus JA, Ogren M, Hedblad B, Witteman JC, Breteler MM, Hunink MG, Hofman A, Criqui MH, Langer RD, Fronek A, Hiatt WR, Hamman R, Resnick HE, Guralnik J, McDermott MM . Ankle brachial index combined with Framingham Risk Score to predict cardiovascular events and mortality: a meta-analysis. JAMA 2008; 300: 197–208.
Fishbane S, Youn S, Flaster E, Adam G, Maesaka JK . Ankle-arm blood pressure index as a predictor of mortality in hemodialysis patients. Am J Kidney Dis 1996; 27: 668–672.
Ono K, Tsuchida A, Kawai H, Matsuo H, Wakamatsu R, Maezawa A, Yano S, Kawada T, Nojima Y . Ankle-brachial blood pressure index predicts all-cause and cardiovascular mortality in hemodialysis patients. J Am Soc Nephrol 2003; 14: 1591–1598.
Kitahara T, Ono K, Tsuchida A, Kawai H, Shinohara M, Ishii Y, Koyanagi H, Noguchi T, Matsumoto T, Sekihara T, Watanabe Y, Kanai H, Ishida H, Nojima Y . Impact of brachial-ankle pulse wave velocity and ankle-brachial blood pressure index on mortality in hemodialysis patients. Am J Kidney Dis 2005; 46: 688–696.
Kato A, Takita T, Furuhashi M, Kumagai H, Hishida A . A small reduction in the ankle-brachial index is associated with increased mortality in patients on chronic hemodialysis. Nephron Clin Pract 2010; 114: c29–c37.
Chen SC, Chang JM, Hwang SJ, Tsai JC, Liu WC, Wang CS, Lin TH, Su HM, Chen HC . Ankle brachial index as a predictor for mortality in patients with chronic kidney disease and undergoing haemodialysis. Nephrology (Carlton) 2010; 15: 294–299.
Tanaka M, Ishii H, Aoyama T, Takahashi H, Toriyama T, Kasuga H, Takeshita K, Yoshikawa D, Amano T, Murohara T . Ankle brachial pressure index but not brachial-ankle pulse wave velocity is a strong predictor of systemic atherosclerotic morbidity and mortality in patients on maintenance hemodialysis. Atherosclerosis 2011; 219: 643–647.
Itaya H, Shiba M, Joki N, Nakamura M . Combined assessment of chronic kidney disease and subclinical peripheral artery disease used to predict future cardiac events. Nephrology (Carlton) 2010; 15: 230–235.
Wang Y, Guo X, Li J, Hu D, Zhao D, Ma H, Mou Q, Liu J, Xu Y . Predictive value of ankle-brachial index to all-cause mortality and cardiovascular mortality in Chinese patients with chronic kidney disease. Vasa 2012; 41: 205–213.
Matsuo S, Imai E, Horio M, Yasuda Y, Tomita K, Nitta K, Yamagata K, Tomino Y, Yokoyama H, Hishida A, Collaborators developing the Japanese equation for estimated GFR. Revised equations for estimated GFR from serum creatinine in Japan. Am J Kidney Dis 2009; 53: 982–992.
Resnick HE, Lindsay RS, McDermott MM, Devereux RB, Jones KL, Fabsitz RR, Howard BV . Relationship of high and low ankle brachial index to all-cause and cardiovascular disease mortality: the Strong Heart Study. Circulation 2004; 109: 733–739.
Chen SC, Chang JM, Hwang SJ, Chen JH, Lin FH, Su HM, Chen HC . Comparison of ankle-brachial index and brachial-ankle pulse wave velocity between patients with chronic kidney disease and hemodialysis. Am J Nephrol 2009; 29: 374–380.
de Vinuesa SG, Ortega M, Martinez P, Goicoechea M, Campdera FG, Luño J . Subclinical peripheral arterial disease in patients with chronic kidney disease: prevalence and related risk factors. Kidney Int Suppl 2005; 93: S44–S47.
Cheung AK, Sarnak MJ, Yan G, Dwyer JT, Heyka RJ, Rocco MV, Teehan BP, Levey AS . Atherosclerotic cardiovascular disease risks in chronic hemodialysis patients. Kidney Int 2000; 58: 353–362.
Nakagawa N, Takahashi F, Chinda J, Kobayashi M, Hayashi Y, Abe M, Saijo Y, Kikuchi K, Hasebe N . A newly estimated glomerular filtration rate is independently associated with arterial stiffness in Japanese patients. Hypertens Res 2008; 31: 193–201.
Zhan Y, Yu J, Chen R, Sun Y, Fu Y, Zhang L, Li S, Zhang F, Hu D . Prevalence of low ankle brachial index and its association with pulse pressure in an elderly Chinese population: a cross-sectional study. J Epidemiol 2012; 22: 454–461.
Korhonen P, Kautiainen H, Aarnio P . Pulse pressure and subclinical peripheral artery disease. J Hum Hypertens 2013; 28: 242–245.
London GM, Marchais SJ, Safar ME, Genest AF, Guerin AP, Metivier F, Chedid K, London AM . Aortic and large artery compliance in end-stage renal failure. Kidney Int 1990; 37: 137–142.
Barenbrock M, Spieker C, Laske V, Heidenreich S, Hohage H, Bachmann J, Hoeks AP, Rahn KH . Studies of the vessel wall properties in hemodialysis patients. Kidney Int 1994; 45: 1397–1400.
Chen J, Mohler ER 3rd, Xie D, Shlipak MG, Townsend RR, Appel LJ, Raj DS, Ojo AO, Schreiber MJ, Strauss LF, Zhang X, Wang X, He J, Hamm LL, CRIC Investigators. Risk factors for peripheral arterial disease among patients with chronic kidney disease. Am J Cardiol 2012; 110: 136–141.
Franklin SS, Sutton-Tyrrell K, Belle SH, Weber MA, Kuller LH . The importance of pulsatile components of hypertension in predicting carotid stenosis in older adults. J Hypertens 1997; 15: 1143–1150.
Girerd X, Laurent S, Pannier B, Asmar R, Safar M . Arterial distensibility and left ventricular hypertrophy in patients with sustained essential hypertension. Am Heart J 1991; 122: 1210–1214.
Madhavan S, Ooi WL, Cohen H, Alderman MH . Relation of pulse pressure and blood pressure reduction to the incidence of myocardial infarction. Hypertension 1994; 23: 395–401.
Lee ML, Rosner BA, Weiss ST . Relationship of blood pressure to cardiovascular death: the effects of pulse pressure in the elderly. Ann Epidemiol 1999; 9: 101–107.
Chae CU, Pfeffer MA, Glynn RJ, Mitchell GF, Taylor JO, Hennekens CH . Increased pulse pressure and risk of heart failure in the elderly. JAMA 1999; 281: 634–639.
Selvin E, Erlinger TP . Prevalence of and risk factors for peripheral arterial disease in the United States: results from the National Health and Nutrition Examination Survey, 1999–2000. Circulation 2004; 110: 738–743.
Weatherley BD, Nelson JJ, Heiss G, Chambless LE, Sharrett AR, Nieto FJ, Folsom AR, Rosamond WD . The association of the ankle-brachial index with incident coronary heart disease: the Atherosclerosis Risk In Communities (ARIC) study, 1987–2001. BMC Cardiovasc Disord 2007; 7: 3.
Murakami Y, Hozawa A, Okamura T, Ueshima H, Evidence for Cardiovascular Prevention From Observational Cohorts in Japan Research Group (EPOCH-JAPAN). Relation of blood pressure and all-cause mortality in 180,000 Japanese participants: pooled analysis of 13 cohort studies. Hypertension 2008; 51: 1483–1491.
Wei M, Gaskill SP, Haffner SM, Stern MP . Effects of diabetes and level of glycemia on all-cause and cardiovascular mortality. The San Antonio Heart Study. Diabetes Care 1998; 21: 1167–1172.
Hara M, Sobue T, Sasaki S, Tsugane S . Smoking and risk of premature death among middle-aged Japanese: ten-year follow-up of the Japan Public Health Center-based prospective study on cancer and cardiovascular diseases (JPHC Study) cohort I. Jpn J Cancer Res 2002; 93: 6–14.
Banerjee D, Brincat S, Gregson H, Contreras G, Streather C, Oliveira D, Nelson S . Pulse pressure and inhibition of renin–angiotensin system in chronic kidney disease. Nephrol Dial Transplant 2006; 21: 975–978.
Fang W, Yang X, Bargman JM, Oreopoulos DG . Association between pulse pressure and mortality in patients undergoing peritoneal dialysis. Perit Dial Int 2009; 29: 163–170.
Tozawa M, Iseki K, Iseki C, Takishita S . Pulse pressure and risk of total mortality and cardiovascular events in patients on chronic hemodialysis. Kidney Int 2002; 61: 717–726.
Lawlor DA, Ebrahim S, Davey Smith G . Sex matters: secular and geographical trends in sex differences in coronary heart disease mortality. BMJ 2001; 323: 541–545.
Pilote L, Dasgupta K, Guru V, Humphries KH, McGrath J, Norris C, Rabi D, Tremblay J, Alamian A, Barnett T, Cox J, Ghali WA, Grace S, Hamet P, Ho T, Kirkland S, Lambert M, Libersan D, O'Loughlin J, Paradis G, Petrovich M, Tagalakis V . A comprehensive view of sex-specific issues related to cardiovascular disease. CMAJ 2007; 176: S1–44.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Yoshitomi, R., Nakayama, M., Ura, Y. et al. Ankle-brachial blood pressure index predicts cardiovascular events and mortality in Japanese patients with chronic kidney disease not on dialysis. Hypertens Res 37, 1050–1055 (2014). https://doi.org/10.1038/hr.2014.120
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/hr.2014.120
Keywords
This article is cited by
-
Association of aortic valve calcification with carotid artery lesions and peripheral artery disease in patients with chronic kidney disease: a cross-sectional study
BMC Nephrology (2020)
-
Automated plethysmographic measurement of the ankle-brachial index: a comparison with the doppler ultrasound method
Hypertension Research (2016)