Abstract
The renin–angiotensin–aldosterone system (RAAS) has a central function in the regulation of blood pressure. Aliskiren, the first direct renin inhibitor to be approved for the treatment of hypertension, blocks the RAAS at its point of activation. As renin inhibition acts at the top of the RAAS cascade, this mechanism has been proposed to offer advantages over existing modes of RAAS blockade. The RAAS is also considered to be a major factor in the pathogenesis of many renal diseases, especially diabetic nephropathy (DN), the main cause of end-stage renal disease. Existing therapies to block the RAAS slow the progression of DN, but they do not halt the disease. Therefore, more effective modes of interventions are needed. Studies to determine the efficacy of aliskiren in human renal disease are in progress. This review summarizes in vivo studies in which the efficacy of aliskiren was tested in experimental models of renal disease, and presents in vitro studies that provide insights into the possible mechanisms by which aliskiren confers renoprotection in animals. These works are discussed in the framework of the intrarenal RAAS and suggest that aliskiren may act by unique renoprotective mechanisms.
Similar content being viewed by others
Introduction
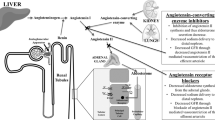
The renin–angiotensin–aldosterone system (RAAS) is an ancient pathway1 that has evolved into a central mechanism by which mammalian blood pressure (BP) and fluid homeostasis are regulated. Research in this field started with the discovery in 1898 by Tigerstedt and Berman2 that a renal extract when injected into rabbits induced a rapid increase in systemic BP. Subsequent work over many years established the RAAS as a pivotal contributor to cardio-renal diseases. Hence, inhibitors of the middle and distal portions of the RAAS pathway, angiotensin-converting enzyme (ACE) inhibitors (ACEI) and AT1 receptor blockers, respectively, have become mainstay therapies for treating hypertension. In 2007, aliskiren, the first direct renin inhibitor (DRI), was approved for the treatment of hypertension. This heralded the therapeutic control of BP by inhibiting the RAAS at its first and rate-limiting step. However, RAAS blockade is also effective for treating renal disease3, 4, 5, 6 and the efficacy of aliskiren for this purpose is currently being investigated. Accordingly, the subject of this review is to summarize the preclinical evidence for renoprotection by aliskiren, and to discuss recently published information on the possible mechanism(s) for these benefits. As it is well recognized that there is a tissue as well as circulating RAAS,7 the preclinical actions of aliskiren will be discussed in the context of the intrarenal RAAS and the potential for its inhibition by aliskiren.
Intrarenal RAAS
Goormaghtigh8 first proposed that renin was produced just outside of the glomerulus in juxtaglomerular (JG) cells. However, work over the past several decades indicates a broader pattern of intra-glomerular RAAS expression. Indeed, the kidney possesses a fully functional tissue RAAS9, 10, 11 with expression along virtually the entire nephron.
Gene and protein expression of angiotensinogen (Aogen), renin and ACE has been reported in cultured glomerular mesangial cells12, 13, 14, 15, 16, 17, 18, 19, 20, 21, 22, 23, 24 and podocytes.25, 26, 27, 28 Mesangial expression of Aogen and ACE has also been documented in renal tissue sections.19, 23
Mesangial cells synthesize Ang II22, 24 and aldosterone, the latter apparently through an Ang II-dependent mechanism.29 Podocytes also produce Ang II25, 26, 28 and aldosterone.30 Angiotensin type 1 receptors are expressed on mesangial cells19, 24, 31 and podocytes26, 28, 32 and mineralocorticoid receptors are also expressed by both cell types.29, 33, 34
The likely importance of the local glomerular RAAS relates to the pathogenesis of glomeruloscleorsis and the loss of glomerular permselectivity observed in many glomerular diseases. In cultured mesangial cells, Ang II35, 36, 37 and aldosterone38, 39 provoke synthesis of extracellular matrix (ECM) proteins that accumulate in glomerulosclerosis. In podocytes, Ang II has been shown to induce apoptosis,40, 41 cytoskeletal rearrangement42 and nephrin loss43 in podocytes, alterations that have been linked to albuminuria.44 Aldosterone can also damage podocytes by inducing apoptosis and reducing nephrin gene expression.30, 33, 45 Thus, through autocrine or endocrine mechanisms, Ang II and aldosterone may induce damage and/or pro-fibrotic pathways in mesangial cells or podocytes, and thus contribute to glomerular damage.
Renal tubular cells express all of the components of the RAAS. Renin mRNA and protein are expressed in the proximal and connecting tubules, as well as the collecting ducts.19, 46, 47, 48, 49, 50, 51, 52, 53, 54 Interestingly, mechanisms for regulating tubular renin seem to be independent of those in the JG cell.47, 48, 50, 52 Proximal tubular cells express mRNA54, 55, 56 and protein53, 57 for ACE and Aogen.58, 59, 60, 61 In vivo evidence that proximal tubular cells may synthesize Ang II has also been reported.62
The above studies indicate the presence of a functional renal tubular RAAS, which likely has an important function in regulating sodium and fluid balance, and hence BP. However, the tubular RAAS may also be linked to the pathogenesis of tubulo-interstitial fibrosis. For instance, Ang II induces epithelial-mesenchymal transformation in tubular cells,63 a process thought to presage renal fibrosis.64
Renoprotective effects of renin inhibition with aliskiren
Aliskiren is a competitive inhibitor of renin; it binds to the active site of the enzyme and thereby prevents access to its substrate, Aogen. In turn, activation of the RAAS cascade is blocked. Given the above evidence that the primary and damaging effector molecule (Ang II) of the RAAS is made at many sites throughout the kidney, and that inhibition of renin blocks the RAAS at the first and rate-limiting step in Ang II formation, it is reasonable to propose that a DRI may provide distinct renoprotective benefits in a variety of renal diseases. The ensuing discussion will outline the evidence that the DRI aliskiren ameliorates renal damage in experimental renal disease. However, let us first consider some aspects of aliskiren that bear on its use in experimental settings.
Testing aliskiren in animal models
Certain important characteristics of aliskiren impact its use in animal models. First, because aliskiren is a human renin inhibitor, it is a less potent inhibitor of rodent renin than human renin65 (Table 1). Thus, although rodent models of renal disease are very commonly used, models that express rat renin are not ideal for testing aliskiren. This issue can be circumvented by using a transgenic rat model with an activated RAAS. The so-called double transgenic rat66 expresses the human genes for renin and Aogen, and thereby provides a model in which a human DRI can inhibit human renin in a rodent. A second model, the TG(mRen-2)27 (mRen-2) rat expresses the mouse ren-2 gene,67 and takes advantage of the capacity of mouse renin to cleave rat Aogen. Aliskiren is effective in this model as the IC50 of the drug against mouse renin is relatively low (Table 1). The organ damage seen in dTGR68 and mRen-2 rats69 is ameliorated by RAAS blockade, giving relevance to testing aliskiren in these models.
A second relevant property of aliskiren is its low oral bioavailability in rodents, in which oral dosing of this DRI does not result in good efficacy. Rather, consistent efficacy is seen when aliskiren is administered to rodents by subcutaneously implanted osmotic minipumps.
Aliskiren protects against experimental renal disease
Hypertensive renal disease
The first evidence for renoprotection by aliskiren was reported in dTGR. The activated RAAS in these animals leads to severe hypertension with renal damage, including albuminuria, elevated serum creatinine, renal infiltration of macrophages, and ECM deposition.68, 70 In this model, aliskiren (0.3 or 3 mg kg–1 per day) normalized the BP and reversed existing renal damage, evidenced by normalizing albuminuria and serum creatinine levels. Furthermore, glomerular collagen IV accumulation and renal macrophage and lymphocyte contents were lowered.71 This paper also showed a reduction in renal cortical Ang I and Ang II levels in aliskiren-treated dTGR, thus documenting an inhibitory effect of this DRI on the intrarenal RAAS. Moreover, Ang I-forming capacity of the sera from these rats was also significantly reduced. A subsequent report by this group72 showed that treatment with aliskiren inhibited complement activation and cellular infiltration in kidneys of dTGR. These studies showed the efficacy of aliskiren in high Ang II-induced renal injury and suggested a beneficial effect of the drug in complement-dependent renal disease. Notably, an earlier study of dTGR showed that when the renin inhibitor remikiren and a non-RAAS blocking anti-hypertensive therapy were compared at comparable BP-lowering doses, remikiren showed stronger renoprotection,70 suggesting BP-independent effects of renin inhibition.
In both the above studies,71, 72 AT1 receptor blockers were included as positive controls; they were not intended to be comparator agents. These drugs were administered at different dosages and by different routes of administration than aliskiren. Although comparable renoprotective effects were observed with aliskiren and its comparator in each of these studies, conclusions on comparative efficacy vs. aliskiren could not be made.
In this regard, we tested in mRen-2 rats the effects of 4 weeks of treatment with aliskiren or enalapril, both administered through osmotic minipumps to achieve constant plasma levels of each drug, at doses that achieved comparable tail cuff BP control (Figure 1a) (Avigdor, Hu, Jen, and Feldman, unpublished data). Compared with vehicle controls, albuminuria was reduced similarly by both therapies (Figure 1b), as were plasma levels of Ang II and aldosterone (Table 2) at the end of the experiment. This study indicated that when drug delivery and BP lowering were similar, aliskiren induced comparable reductions in albuminuria and blockade of the circulating RAAS, including lowering plasma aldosterone.
Effect of aliskiren and enalapril on blood pressure (a) and albumin excretion (b) in mRen-2 rats. mRen-2 rats were treated with aliskiren or enalapril by subcutaneous osmotic minipumps. Blood pressure was measured by the tail cuff method and urinary albumin levels were measured by ELISA. *P<0.05 vs. vehicle.
Endothelial nitric oxide synthase (eNOS) regulates renal hemodynamics and renal function.73 Deficiencies in eNOS lead to accelerated renal damage in models of renal disease,74 highlighting the importance of nitric oxide in renal health. Recently, aliskiren was shown to inhibit the renal disease that develops in eNOS−/− mice.75 Increases in albuminuria, glomerulosclerosis and renal macrophage infiltration observed in the vehicle-treated knockout mice were significantly reduced by aliskiren treatment (25 mg kg–1), as were levels of glomerular superoxide and renal NADPH oxidase. Importantly, hydralazine given at a dose that lowered tail cuff BP similarly to aliskiren did not show these beneficial effects. This work showed that the renoprotective actions of aliskiren do not require eNOS-mediated pathways. Moreover, this protection seems to result at least partially from effects that are beyond BP control, possibly by inhibiting Ang II-induced damaging effects in the kidney.
The anti-inflammatory effect of aliskiren observed in the kidneys of dTGR71 and eNOS−/− 75 mice is not a renal-specific effect. Recently, Ino and coworkers76 reported that at a non-BP-lowering dose, aliskiren reduced leukocyte adhesion in a murine vascular injury model. Furthermore, this effect of aliskiren was associated with a reduction in the injury-induced up-regulation of adhesion molecules on the vascular endothelium, pointing toward a possible mechanism for the reductions in inflammatory infiltrates noted above in the kidneys of dTGR71 and mice.75
Diabetic nephropathy
Diabetic nephropathy (DN) is the leading cause of end-stage renal disease in the developed world.77 The RAAS is thought to have a central function in the pathogenesis of this disease, evidenced by numerous studies showing that RAAS blockade by ACEIs and AT1 receptor blockers slows the progression of DN.3, 4, 5, 6 However, these treatments do not halt the progression of this disease. Thus, the underlying mechanisms for progression of DN continue even in patients treated with accepted therapies. The intrarenal RAAS is thought to be activated during diabetes, based on in vitro and in vivo evidence.21, 22, 24, 25, 48, 54, 55, 69, 78 Therefore, the effect of renin inhibition in diabetic conditions is of great interest.
In vitro effects of aliskiren in high glucose conditions
Albuminuria is the first clinically detectable change in renal function in DN, resulting from a reduction in permselectivity of the glomerular capillary wall. The glomerular permeability barrier consists of three layers, the outer most glomerular visceral epithelial cells (podocytes) that cover the (middle) glomerular basement membrane, which is lined on its luminal side by the inner layer, the fenestrated endothelium. Podocytes seem to have a key function in preventing the escape of plasma proteins across the glomerular capillary wall into the urine. Their involvement in the development of albuminuria and glomerulosclerosis in DN is increasingly accepted.44, 79
During diabetes, podocytes are exposed in vivo to high glucose levels and stretch forces, the latter because of glomerular hypertrophy and hyperfiltration. When these conditions are modeled in vitro in mouse podocytes, the RAAS becomes activated. Indeed, podocytes subjected to mechanical stretch show Ang II-mediated apoptosis.41 Aliskiren was tested for its effects on cultured mouse podocytes exposed to high glucose levels.25 In such podocytes, high glucose induced increased expression of renin mRNA and protein, and Ang II formation was detected. The latter was not inhibited by the ACEI captopril, but it was suppressed by aliskiren and the non-selective chymase inhibitor chymostatin. These findings suggest that high glucose conditions activated the podocyte RAAS at the level of renin, leading to increased Ang II formation. If we can assume that captopril actually entered the podocytes in this study, the results further indicate that Ang II formation in these cells was mediated primarily by non-ACE pathways (that is, chymase). To the extent that the up-regulation of glomerular chymase in diabetic kidneys18 may suggest a function for ACE-independent Ang II formation in DN, renin inhibition may have a protective advantage over ACEI in this disease. Thus, these in vitro results may be an example in which blocking the RAAS at the top of the cascade (that is, at renin) may achieve different outcomes than by inhibiting elsewhere in the pathway.
The loss of podocytes from the glomerular capillary wall is associated with the development of albuminuria80 and glomerulosclerosis,81 and apoptosis of podocytes has been suggested as a mechanism for such loss.44 Phillips and coworkers82 reported that aliskiren attenuated the high glucose-induced increase in cleaved caspase-3 in cultured mouse podocytes, suggesting a protective effect of aliskiren against podocyte apoptosis in a high glucose milieu. Moreover, these authors showed that aliskiren inhibited the high glucose-induced increase in fibronectin mRNA and protein in these cells.
The above two in vitro studies in podocytes have potential clinical significance because they suggest that aliskiren can induce effects that relate directly to protecting the glomerular filtration barrier. Aliskiren has a molecular weight (551.8) small enough to be filtered by the glomerulus, and indeed the drug appears in the urine.83 Thus, in vivo exposure of podocytes to aliskiren is predicted. As podocytes express a functional RAAS,25, 26, 27, 28 renin inhibition in these cells by aliskiren may provide a cellular mechanism (that is, podocyte protection) for the anti-albuminuric effect observed in human beings84, 85 as well as animals.71, 75, 86, 87, 88
In vivo effects of aliskiren in experimental DN
Transgenic mRen-2 rats with superimposed STZ-induced diabetes develop albuminuria, glomerulosclerosis and tubulo-interstitial fibrosis,69 similar features as in human DN. Aliskiren (10 mg kg–1 per day) and the ACEI perindopril (0.2 mg kg–1 per day) were compared for their renoprotective effects in this model.88 The chosen dose of perindopril lowered tail cuff BP 36 mm Hg more than in aliskiren-treated STZ-mRen-2 rats. However, despite this difference, aliskiren attenuated albuminuria and glomerulosclerosis to similar degrees as perindopril. Interestingly, levels of albuminuria correlated well with BP in vehicle- and perindopril-treated mRen-2 rats, but not in aliskiren-treated rats. Moreover, histological evaluation showed that aliskiren conferred significantly greater protection against tubulo-interstitial fibrosis than perindopril. These two differential effects of aliskiren vs. perindopril may reflect a BP-independent renoprotective effect of aliskiren, possibly by inhibiting the intrarenal RAAS to a greater extent than the ACEI.
In another study with diabetic mRen-2 rats in which BP was monitored continuously by telemetry, aliskiren at 10, 30 and 60 mg kg–1 per day dose dependently reversed existing hypertension and prevented the development of albuminuria over the 10 weeks study.87 At the end of this study, renal cortical gene expression of collagen I and the pro-fibrotic growth factor, transforming growth factor-β (TGF-β), in the mRen-2 rats were significantly reduced in the aliskiren vs. the vehicle group.
In this experiment, treatment of diabetic mRen-2 rats with the high-dose (60 mg kg–1 per day) aliskiren was discontinued about 3 weeks into the study, but the animals were monitored for the remainder of the 10 weeks experiment (Webb, Zhou, Feldman, unpublished data). Withdrawal of aliskiren treatment was accompanied by an increase in BP and the development of albuminuria. The rise in BP was gradual, taking about 10 days to reach vehicle-control levels. Moreover, at the end of 10 weeks, gene expression of renal cortical TGF-β was still suppressed, despite stopping treatment with aliskiren about 7 weeks earlier. It is unknown whether this suppression of TGF-β reflects a continued presence or persistent effect of aliskiren in the kidneys, or whether RAAS inhibition early in the development of the hypertensive phenotype of this model confers long-term effects on growth factor expression.
Aliskiren has also shown renoprotective effects in db/db mice, a model of type 2 diabetes.86 In this study, treatment with aliskiren ameliorated the albuminuria and glomerulosclerosis seen in the vehicle-treated mice. These benefits were accompanied by reductions in expression of TGF-β, collagen IV and nephrin, as well as p22phox and NADPH oxidase activity.
Collectively, the above in vitro and in vivo studies suggest that the functional and structural renoprotection conferred by aliskiren in experimental renal disease may be explained by inhibition of the intrarenal RAAS, which may result in BP-independent renoprotective mechanisms (for example, anti-inflammatory, anti-oxidant) that reduce ECM accumulation and possibly mitigate against cellular (for example podocyte) damage. These studies also provide hints of persistent renoprotective effects of this DRI.
Potential novel mechanisms of aliskiren's renoprotective actions
Given that aliskiren blocks renin, it is not surprising that this drug has renoprotective effects in the experimental settings described above. Rather, the intriguing question is: ‘does a DRI, by blocking the RAAS at the first and rate-limiting step, impart a specific renoprotective mechanism?’ New evidence is emerging that suggests this may be the case.
Aliskiren localizes in the kidney
The kidney is the main source of renin; this organ contains a fully functional RAAS distributed over virtually all regions of the nephron, as described earlier. Consequently, as this pathway has been linked closely with renal damage, a distinct renoprotective advantage is expected from blocking the intrarenal RAAS. For a drug to inhibit the intrarenal RAAS and protect against organ damage, an obvious requirement is that it partitions to an appropriate renal compartment. On the basis of the experiments discussed below, this requirement seems to be met by aliskiren.
Sprague–Dawley rats were treated with 10 mg kg–1 per day aliskiren for 2 weeks by osmotic minipumps, and their plasmas and kidneys were studied for the presence of the drug. Renal levels of aliskiren were 46-fold over plasma levels, indicating that renal localization of aliskiren occurred, but was not due simply to equilibration from the plasma.87 Other renin inhibitors have shown a similar renophilic property.89 Although this study showed that aliskiren partitions to the kidney, it did not indicate the renal compartment in which aliskiren localized.
Therefore, in another experiment, the renal topographical localization of aliskiren was explored by administering 14C-aliskiren intravenously to normotensive rats and harvesting their kidneys 2 h afterward. By light microscopy, cryostat sections revealed heavy autoradiographic labeling in 100% of glomeruli on each renal section, indicating extensive partitioning of aliskiren throughout these structures87 (Figure 2a). Moreover, images suggestive of the presence of aliskiren in JG cells of the afferent arterioles were obtained, although such localization was not identified conclusively in these relatively thick cryostat sections. However, the possibility that aliskiren can enter vascular structures was shown clearly by the presence of label in larger caliber intrarenal arteries in these kidneys (Figure 2b), and preliminary evidence from recent studies suggests that in fact, aliskiren may localize in the afferent arterioles (Feldman et al., paper in preparation). However, in contrast to glomeruli, autoradiographic evidence for the presence of aliskiren in the tubulo-interstitium was not observed within the short duration of exposure in this experiment.87
Autoradiographic localization of aliskiren in rat kidneys. Hanover–Wistar rats were injected intravenously with 14C-aliskiren and 2 h later the kidneys were removed for autoradiography. (a) Two glomeruli (G) show extensive autoradiographic labeling, indicating the presence of aliskiren. (b) A renal cortical artery (arrow) shows extensive autoradiographic labeling in vascular wall. (Reproduced with permission from Lippincott Williams & Wilkins.87)
The above studies show that aliskiren partitions to the kidneys and localizes in the renal vasculature, possibly in structures known to contain renin. Moreover, extensive partitioning of aliskiren to the glomeruli suggests that it can access mesangial cells and podocytes, potentially inhibiting the RAAS in these cells and conferring structural and functional renoprotection observed in rodents.71, 75, 86, 87, 88 Light microscopic studies with labeled aliskiren have not been conducted in disease models in which changes in (extraglomerular) vascular permeability may facilitate permeation of the drug to the tubulo-interstitium, with potential access to tubular cells and fibroblasts. However, it seems reasonable to speculate that this may occur, and it may have relevance to the extent that enhanced expression of tubular renin may be linked to the development of tubulo-interstitial fibrosis.47
Not only does aliskiren partition to the kidneys in rats, its renal presence is prolonged. Two lines of evidence support this concept. First, dTGR were treated with aliskiren (3 mg kg–1 per day) for 2 weeks, during which time BP (tail cuff) and albuminuria were significantly reduced vs. vehicle controls. After a 3-week washout period, renal and plasma levels of aliskiren were measured. Aliskiren was not detectable in the plasma from these rats, but drug levels in the kidney were still above the IC50 for inhibiting human renin.90 Second, Vaneckova and coworkers91 treated mRen-2 rats with aliskiren (10 mg kg–1 per day) for 4 weeks, during which time BP (telemetry) was normalized. At the end of this treatment period, plasma and renal Ang II levels were lowered to those in non-hypertensive vehicle controls, confirming the observations in dTGR71 that treatment with aliskiren reduces renal Ang II content. At this time, aliskiren treatment of mRen-2 rats was stopped for 12 days washout. Importantly, after the washout period, plasma and renal Ang II levels were still reduced to vehicle-control levels.
Taken together, the above studies showed that aliskiren partitions to the kidney and exhibits a prolonged renal residence. These studies also suggest that aliskiren inhibits the intrarenal RAAS, and that such inhibition is enduring. In view of the growing evidence that 24-h BP control predicts better outcomes for target organ protection,92, 93, 94 such long-acting inhibition of the intrarenal RAAS may be especially important in conditions in which this pathway is activated, such as believed to occur in DN.78
Aliskiren may bind to intrarenal renin
The autoradiographic images discussed above87 provoke questions regarding the intracellular fate of aliskiren. Whether labeled aliskiren found in the kidneys of rats represents renin-bound inhibitor is an important issue. It seems doubtful that all of the labeled aliskiren observed in glomeruli in these studies was bound to renin: it is highly unlikely that so much renin was present in the glomeruli of the normotensive rats used in this study.69, 95, 96 Moreover, it seems similarly implausible that exposure to aliskiren for 2 h in normotensive rats could have induced recruitment of such high levels of glomerular renin, as has been shown in pre-glomerular vessels after chronic RAAS blockade,97 especially as aliskiren is a relatively weak inhibitor of rat renin (Table 1). However, some of the label seen in glomeruli may have reflected aliskiren bound to renin that possibly was present in the mesangial matrix. In addition, as aliskiren can penetrate cultured cardiomyocytes,98 the drug may have entered mesangial cells and podocytes, both of which express renin20, 24, 25, 26 to which aliskiren could bind. Furthermore, the unequivocal evidence for labeled aliskiren in the walls of renal vessels prompts the proposal that this DRI can enter JG cells, and possibly incorporate into forming or formed renin granules. Recent in vitro studies provide evidence for the latter possibility.
Cultured JG cells do not store renin,99 making them unsuitable for studying the intracellular renin-binding capacity of aliskiren. However, a human mast cell line synthesizes and secretes (pro)renin.100 Krop and coworkers101 used these cells to ask whether aliskiren can incorporate into renin granules. They found that mast cells that had been incubated for 7 days with aliskiren secreted renin that displayed inhibited enzyme activity (that is, inhibited Ang I-forming capacity). These data show that aliskiren can access intracellular renin, bind or incorporate into renin granules, and remain associated with the enzyme through the secretory process. Similar results were seen with prorenin, which is constitutively released from HMC-1 cells.102 This study lays the groundwork for understanding the intracellular fate of aliskiren. Moreover, the implications from this work and the autoradiographic data are that aliskiren may provide an unusual example in which an inhibitor incorporates into its (still intracellular) target even before the latter is secreted. In this case, (pro)renin would be secreted from JG cells to the plasma or the tubulo-interstitium103 in an already inhibited state. The renin activity in this (pro)renin-aliskiren complex would be inhibited: this renin (or prorenin, which may undergo activation at tissue sites) could not cleave Aogen, and the tissue and systemic RAAS cascades would not be activated. As this mechanism should operate independently of plasma drug levels,101 it may help to explain the prolonged BP benefits observed in rats discussed earlier, and in patients in whom aliskiren treatment has been stopped.104
Aliskiren, prorenin and the (pro)renin receptor
The recent discovery of a receptor for renin and prorenin, the (P)RR,105 has added an important new dimension to the tissue RAAS.106, 107, 108 In the kidney, gene and/or protein expression of the (P)RR has been reported in the glomerular mesangium,109 vascular wall87, 109 and tubular cells.87, 110 Gene and protein expression for the (P)RR has also been reported in podocytes.111, 112, 113
Stimulation of the (P)RR initiates Ang II-dependent and -independent effects. The former include a gain in catalytic activity for renin bound to the (P)RR (vs. unbound renin). This effect amplifies the formation of Ang II at the cell surface.109 Furthermore, on binding to the (P)RR, prorenin, which is normally inactive, becomes catalytically active (it can cleave Aogen to form Ang I), possibly because of a conformational change induced by the binding.109, 114, 115, 116 The Ang II-independent effects of (P)RR stimulation include activation of extracellular signal-regulated kinase1/2,109, 117, 118 and heat shock protein 27119 and phosphatidylinositol-3 kinase p85α120 pathways. The production of TGF-β and plasminogen-activator-1 is also increased, as are gene expression and production of collagen I and fibronectin, respectively.117, 121 Thus, through the (P)RR, renin and prorenin can induce direct effects on cells. Continuing work on this receptor has led to the isolation and characterization of a soluble form of the (P)RR,111 the significance of which remains to be elucidated.
As the (P)RR can activate prorenin, it has been suggested that this receptor may have an important function in the activation of prorenin at tissue sites, with consequent Ang II-mediated tissue damage.122 Prorenin is inactive because a 43 amino-acid prosegment covers the enzyme's active site. Incubation of prorenin with a renin inhibitor under the appropriate conditions permits access of the inhibitor to the active site of prorenin, while the prosegment, in equilibrium between ‘covering’ and ‘lifted’ conformations, is lifted from its position covering the active site.123 In vitro studies showed that when incubated with prorenin, aliskiren binds to the active site of the enzyme87 and can inhibit Ang I formation that would normally occur from non-proteolytic [(P)RR-mediated] activation of prorenin.116 This finding is significant because activation of prorenin at tissue sites might occur by (P)RR-mediated mechanisms or by proteolytic cleavage of the prosegment. The latter may occur in tissues in which inflammatory or dead/dying parenchymal cells may release proteases such as cathepsin G or elastase,124 which are capable of cleaving the prosegment. In either case, the Ang I-forming capacity of prorenin and the subsequent formation of Ang II (in the presence of ACE or chymase) would be blocked by bound aliskiren. The ability of aliskiren to inhibit prorenin activation has additional relevance because circulating levels of prorenin are about 10-fold those of renin.125 This represents high potential renin activity. In addition, plasma prorenin levels can be substantially elevated in diabetes126 and are strongly associated with microvascular complications of this disease.127 Thus, to the extent that activation of prorenin at tissue sites may contribute to local Ang II formation and tissue damage, aliskiren may provide tissue-protective effects. However, it must be noted that the concept of prorenin-induced tissue injury is not fully established; in two models of prorenin over-expressing mice, cardio-renal damage was not observed.128, 129
The potential clinical significance of the (P)RR is highlighted in a set of studies by Ichihara and coworkers (reviewed elsewhere130) that suggest a central function for this receptor in the pathogenesis of DN. This body of work is particularly provocative because the authors have reported dramatic benefits in STZ-diabetic rats with a putative (P)RR blocker. However, attempts by other investigators to reproduce the cellular effects of the blocker, and its in vivo benefits (although in non-diabetic models of renal damage), have largely been unsuccessful.115, 118, 131, 132 Replication by others of the experimental designs used by Ichihara and coworkers may clarify some of the questions on the function of the (P)RR in DN and in tissue damage in general.
What is the effect of aliskiren on the function of the renal (P)RR? Aliskiren does not inhibit binding of (pro)renin to the (P)RR,87, 118 nor does it prevent (pro)renin-induced cell signaling.87, 118, 120 However, in STZ-diabetic mRen-2 rats treated with aliskiren for 10 weeks, in situ hybridization on renal sections revealed a clear reduction in gene expression of the (P)RR in the glomeruli and tubular cells compared with vehicle-control diabetic mRen-2 rats.87 Interestingly, in vitro studies showed that aliskiren did not affect gene expression of (P)RR in mesangial cells. These data suggest that aliskiren can suppress mesangial cell gene expression of the (P)RR in vivo, but probably not through a direct cellular effect. Regardless, if this reduced gene expression also leads to lower (P)RR density at the cell surface, a reduction in Ang II-dependent and -independent effects could be expected from administration of aliskiren. This topic deserves more investigation.
In addition to suppressing gene expression of the (P)RR, treatment of diabetic mRen-2 rats with aliskiren also led to a reduction in renal cortical mRNA abundance for TGF-β and collagen I.87 It is tempting to invoke a causative relationship between reductions in gene expression of the (P)RR, TGF-β and collagen I in the above study. Indeed, elegant in vitro experiments by Huang and coworkers18 established a strong link between renin-induced production of TGF-β and ECM production in cultured mesangial cells, whereas blockade of the (P)RR with siRNA significantly inhibited this response. However, a similar causative conclusion from the in vivo study87 awaits a more robust proof.
Working model of renoprotective mechanism of action of aliskiren
From the data presented heretofore, it is possible to propose a working model for the mechanism(s) by which aliskiren protects the kidneys in experimental settings (Figure 3). Although this model is necessarily speculative, it provides testable hypotheses.
In this working model of the renoprotective actions of aliskiren, outcomes for which in vitro or in vivo evidence exists are referenced (see References); no reference indicates a logical, but still speculative outcome. Solid arrows indicate the existence of in vitro or in vivo evidence to support a causal link between the events. Dotted lines denote a logical, but as yet, unproven causal link between events. * indicates Feldman DL et al., manuscript in preparation. Once aliskiren localizes in the kidney (for example, JG cells), it may incorporate into renin granules or prorenin and stay in these cells until released with (pro)renin. This renal localization would lead to a longer renal residence time than if unbound, and ultimately would lead to prolonged local RAAS blockade. Aliskiren that deposits in the glomeruli may inhibit mesangial and podocyte renin, inhibiting Ang II-mediated glomerular ECM accretion and loss of permselectivity. Renin or prorenin bound to aliskiren in JG cells would be released as inhibited enzymes and would theoretically have no abilities to cleave Aogen. The formation of Ang II would be inhibited, maintaining a quiescent local (tissue) and systemic RAAS. If aliskiren reduces synthesis of the (P)RR as a result of suppressing its gene expression, lower receptor density on the cell surface would be expected, reducing the opportunity for (pro)renin to bind to diminished numbers of receptors. Once released from JG cells, inhibited renin could still bind to the (P)RR, but could not gain the amplified catalytic activity that has been described after such binding. Similarly, prorenin released as bound to aliskiren could not become activated by proteolytic or non-proteolytic mechanisms. These actions on renin and prorenin would reduce Ang II formation at the cell surface. Extrarenal tissues that take up already inhibited renin would also theoretically derive protection from these mechanisms. Finally, in addition to the mechanisms described here, renoprotection would also derive from aliskiren binding to (pro)renin in the plasma.
Summary
Although the idea to inhibit renin as a means of blocking the RAAS originated from studies that were conducted over 100 years ago,2 it is only recently that the effects of inhibiting this enzyme have been studied in depth. There is still much to learn about the mechanism of action of renin inhibition, and how it differs from those of ACEI and AT1 receptor blockers. The possibility that aliskiren binds to intracellular (pro)renin, leading to release of already inhibited enzyme seems to be a novel mechanism. However, it still must be documented that this occurs in vivo, and in fact that such a mechanism confers a benefit for organ protection. Toward this end, preclinical studies offer the means by which aliskiren's mode of action can be revealed more fully, thus generating hypotheses that can be tested in patients.
References
Nishimura H . Angiotensin receptors—evolutionary overview and perspectives. Comp Biochem Physiol A Mol Integr Physiol 2001; 128: 11–30.
Tigerstedt R, Bergman P . Niere und Kreislauf. Skand Arch Physiol 1898; 8: 223–270.
Brenner BM, Cooper ME, de ZD, Keane WF, Mitch WE, Parving HH, Remuzzi G, Snapinn SM, Zhang Z, Shahinfar S . Effects of losartan on renal and cardiovascular outcomes in patients with type 2 diabetes and nephropathy. N Engl J Med 2001; 345: 861–869.
Lewis EJ, Hunsicker LG, Bain RP, Rohde RD . The effect of angiotensin-converting-enzyme inhibition on diabetic nephropathy. The Collaborative Study Group. N Engl J Med 1993; 329: 1456–1462.
Lewis EJ, Hunsicker LG, Clarke WR, Berl T, Pohl MA, Lewis JB, Ritz E, Atkins RC, Rohde R, Raz I . Renoprotective effect of the angiotensin-receptor antagonist irbesartan in patients with nephropathy due to type 2 diabetes. N Engl J Med 2001; 345: 851–860.
Parving HH, Lehnert H, Brochner-Mortensen J, Gomis R, Andersen S, Arner P . The effect of irbesartan on the development of diabetic nephropathy in patients with type 2 diabetes. N Engl J Med 2001; 345: 870–878.
Dzau VJ . Circulating versus local renin-angiotensin system in cardiovascular homeostasis. Circulation 1988; 77: I4–13.
Goormaghtigh N . Existence of an endocrine gland in the media of the renal arterioles. Proc Soc Exp Biol Med 1939; 42: 688–693.
Carey RM, Siragy HM . The intrarenal renin-angiotensin system and diabetic nephropathy. Trends Endocrinol Metab 2003; 14: 274–281.
Kobori H, Nangaku M, Navar LG, Nishiyama A . The intrarenal renin-angiotensin system: from physiology to the pathobiology of hypertension and kidney disease. Pharmacol Rev 2007; 59: 251–287.
Velez JC . The importance of the intrarenal renin-angiotensin system. Nat Clin Pract Nephrol 2009; 5: 89–100.
Andrade AQ, Casarini DE, Schor N, Boim MA . Characterization of renin mRNA expression and enzyme activity in rat and mouse mesangial cells. Braz J Med Biol Res 2002; 35: 17–24.
Andrade MC, Quinto BM, Carmona AK, Ribas OS, Boim MA, Schor N, Casarini DE . Purification and characterization of angiotensin I-converting enzymes from mesangial cells in culture. J Hypertens 1998; 16: 2063–2074.
Becker BN, Yasuda T, Kondo S, Vaikunth S, Homma T, Harris RC . Mechanical stretch/relaxation stimulates a cellular renin-angiotensin system in cultured rat mesangial cells. Exp Nephrol 1998; 6: 57–66.
Casarini DE, Boim MA, Stella RC, Krieger-Azzolini MH, Krieger JE, Schor N . Angiotensin I-converting enzyme activity in tubular fluid along the rat nephron. Am J Physiol 1997; 272: F405–F409.
Chansel D, Dussaule JC, Ardaillou N, Ardaillou R . Identification and regulation of renin in human cultured mesangial cells. Am J Physiol 1987; 252: F32–F38.
Dzau VJ, Kreisberg J . Cultured glomerular mesangial cells contain renin: influence of calcium and isoproterenol. J Cardiovasc Pharmacol 1986; 8 (Suppl 10): S6–S10.
Huang XR, Chen WY, Truong LD, Lan HY . Chymase is upregulated in diabetic nephropathy: implications for an alternative pathway of angiotensin II-mediated diabetic renal and vascular disease. J Am Soc Nephrol 2003; 14: 1738–1747.
Lai KN, Leung JC, Lai KB, To WY, Yeung VT, Lai FM . Gene expression of the renin-angiotensin system in human kidney. J Hypertens 1998; 16: 91–102.
Leite CA, Cristovam PC, Leitao AA, Miranda A, Andrade MC, Di MG, Casarini DE, Boim MA . Renin similar to the submaxillary gland form is expressed in mouse mesangial cells: subcellular localization and all generation under control and glucose-stimulated conditions. Cell Physiol Biochem 2003; 13: 357–366.
Singh R, Singh AK, Alavi N, Leehey DJ . Mechanism of increased angiotensin II levels in glomerular mesangial cells cultured in high glucose. J Am Soc Nephrol 2003; 14: 873–880.
Singh R, Leehey DJ . Effect of ACE inhibitors on angiotensin II in rat mesangial cells cultured in high glucose. Biochem Biophys Res Commun 2007; 357: 1040–1045.
Takamatsu M, Urushihara M, Kondo S, Shimizu M, Morioka T, Oite T, Kobori H, Kagami S . Glomerular angiotensinogen protein is enhanced in pediatric IgA nephropathy. Pediatr Nephrol 2008; 23: 1257–1267.
Vidotti DB, Casarini DE, Cristovam PC, Leite CA, Schor N, Boim MA . High glucose concentration stimulates intracellular renin activity and angiotensin II generation in rat mesangial cells. Am J Physiol Renal Physiol 2004; 286: F1039–F1045.
Durvasula RV, Shankland SJ . Activation of a local renin angiotensin system in podocytes by glucose. Am J Physiol Renal Physiol 2008; 294: F830–F839.
Liebau MC, Lang D, Bohm J, Endlich N, Bek MJ, Witherden I, Mathieson PW, Saleem MA, Pavenstadt H, Fischer KG . Functional expression of the renin-angiotensin system in human podocytes. Am J Physiol Renal Physiol 2006; 290: F710–F719.
Velez JC, Bland AM, Arthur JM, Raymond JR, Janech MG . Characterization of renin-angiotensin system enzyme activities in cultured mouse podocytes. Am J Physiol Renal Physiol 2007; 293: F398–F407.
Yoo TH, Li JJ, Kim JJ, Jung DS, Kwak SJ, Ryu DR, Choi HY, Kim JS, Kim HJ, Han SH, Lee JE, Han DS, Kang SW . Activation of the renin-angiotensin system within podocytes in diabetes. Kidney Int 2007; 71: 1019–1027.
Lai LY, Gu Y, Chen J, Yu SQ, Ma J, Yang HC, Lin SY . Production of aldosterone by rat mesangial cell and the accumulation of extracellular matrix induced by aldosterone]. Zhonghua Yi Xue Za Zhi 2003; 83: 1900–1905.
Lee SH, Yoo TH, Nam BY, Kim DK, Li JJ, Jung DS, Kwak SJ, Ryu DR, Han SH, Lee JE, Moon SJ, Han DS, Kang SW . Activation of local aldosterone system within podocytes is involved in apoptosis under diabetic conditions. Am J Physiol Renal Physiol 2009; 297: F1381–F1390.
Ardaillou R, Chansel D, Chatziantoniou C, Dussaule JC . Mesangial AT1 receptors: expression, signaling, and regulation. J Am Soc Nephrol 1999; 10 (Suppl 11): S40–S46.
Sharma M, Sharma R, Greene AS, McCarthy ET, Savin VJ . Documentation of angiotensin II receptors in glomerular epithelial cells. Am J Physiol 1998; 274: F623–F627.
Shibata S, Nagase M, Yoshida S, Kawachi H, Fujita T . Podocyte as the target for aldosterone: roles of oxidative stress and Sgk1. Hypertension 2007; 49: 355–364.
Terada Y, Kobayashi T, Kuwana H, Tanaka H, Inoshita S, Kuwahara M, Sasaki S . Aldosterone stimulates proliferation of mesangial cells by activating mitogen-activated protein kinase 1/2, cyclin D1, and cyclin A. J Am Soc Nephrol 2005; 16: 2296–2305.
Amiri F, Shaw S, Wang X, Tang J, Waller JL, Eaton DC, Marrero MB . Angiotensin II activation of the JAK/STAT pathway in mesangial cells is altered by high glucose. Kidney Int 2002; 61: 1605–1616.
Kagami S, Border WA, Miller DE, Noble NA . Angiotensin II stimulates extracellular matrix protein synthesis through induction of transforming growth factor-beta expression in rat glomerular mesangial cells. J Clin Invest 1994; 93: 2431–2437.
Wolf G, Haberstroh U, Neilson EG . Angiotensin II stimulates the proliferation and biosynthesis of type I collagen in cultured murine mesangial cells. Am J Pathol 1992; 140: 95–107.
Lai L, Chen J, Hao CM, Lin S, Gu Y . Aldosterone promotes fibronectin production through a Smad2-dependent TGF-beta1 pathway in mesangial cells. Biochem Biophys Res Commun 2006; 348: 70–75.
Zhang M, Chen J, Lai L, You L, Lin S, Hao C, Gu Y . Aldosterone promotes fibronectin synthesis in rat mesangial cells via ERK1/2-stimulated Na-H(+) exchanger isoform 1. Am J Nephrol 2009; 31: 75–82.
Ding G, Reddy K, Kapasi AA, Franki N, Gibbons N, Kasinath BS, Singhal PC . Angiotensin II induces apoptosis in rat glomerular epithelial cells. Am J Physiol Renal Physiol 2002; 283: F173–F180.
Durvasula RV, Petermann AT, Hiromura K, Blonski M, Pippin J, Mundel P, Pichler R, Griffin S, Couser WG, Shankland SJ . Activation of a local tissue angiotensin system in podocytes by mechanical strain. Kidney Int 2004; 65: 30–39.
Sharma R, Lovell HB, Wiegmann TB, Savin VJ . Vasoactive substances induce cytoskeletal changes in cultured rat glomerular epithelial cells. J Am Soc Nephrol 1992; 3: 1131–1138.
Doublier S, Salvidio G, Lupia E, Ruotsalainen V, Verzola D, Deferrari G, Camussi G . Nephrin expression is reduced in human diabetic nephropathy: evidence for a distinct role for glycated albumin and angiotensin II. Diabetes 2003; 52: 1023–1030.
Shankland SJ . The podocyte's response to injury: role in proteinuria and glomerulosclerosis. Kidney Int 2006; 69: 2131–2147.
Nagase M, Fujita T . Aldosterone and glomerular podocyte injury. Clin Exp Nephrol 2008; 12: 233–242.
Chen M, Harris MP, Rose D, Smart A, He XR, Kretzler M, Briggs JP, Schnermann J . Renin and renin mRNA in proximal tubules of the rat kidney. J Clin Invest 1994; 94: 237–243.
Gilbert RE, Wu LL, Kelly DJ, Cox A, Wilkinson-Berka JL, Johnston CI, Cooper ME . Pathological expression of renin and angiotensin II in the renal tubule after subtotal nephrectomy. Implications for the pathogenesis of tubulointerstitial fibrosis. Am J Pathol 1999; 155: 429–440.
Kang JJ, Toma I, Sipos A, Meer EJ, Vargas SL, Peti-Peterdi J . The collecting duct is the major source of prorenin in diabetes. Hypertension 2008; 51: 1597–1604.
Moe OW, Ujiie K, Star RA, Miller RT, Widell J, Alpern RJ, Henrich WL . Renin expression in renal proximal tubule. J Clin Invest 1993; 91: 774–779.
Prieto-Carrasquero MC, Harrison-Bernard LM, Kobori H, Ozawa Y, Hering-Smith KS, Hamm LL, Navar LG . Enhancement of collecting duct renin in angiotensin II-dependent hypertensive rats. Hypertension 2004; 44: 223–229.
Rohrwasser A, Morgan T, Dillon HF, Zhao L, Callaway CW, Hillas E, Zhang S, Cheng T, Inagami T, Ward K, Terreros DA, Lalouel JM . Elements of a paracrine tubular renin-angiotensin system along the entire nephron. Hypertension 1999; 34: 1265–1274.
Tank JE, Moe OW, Star RA, Henrich WL . Differential regulation of rat glomerular and proximal tubular renin mRNA following uninephrectomy. Am J Physiol 1996; 270: F776–F783.
Taugner R, Hackenthal E, Rix E, Nobiling R, Poulsen K . Immunocytochemistry of the renin-angiotensin system: renin, angiotensinogen, angiotensin I, angiotensin II, and converting enzyme in the kidneys of mice, rats, and tree shrews. Kidney Int Suppl 1982; 12: S33–S43.
Zimpelmann J, Kumar D, Levine DZ, Wehbi G, Imig JD, Navar LG, Burns KD . Early diabetes mellitus stimulates proximal tubule renin mRNA expression in the rat. Kidney Int 2000; 58: 2320–2330.
Anderson S, Jung FF, Ingelfinger JR . Renal renin-angiotensin system in diabetes: functional, immunohistochemical, and molecular biological correlations. Am J Physiol 1993; 265: F477–F486.
Mizuiri S, Yoshikawa H, Tanegashima M, Miyagi M, Kobayashi M, Sakai K, Hayashi I, Aikawa A, Ohara T, Hasegawa A . Renal ACE immunohistochemical localization in NIDDM patients with nephropathy. Am J Kidney Dis 1998; 31: 301–307.
Metzger R, Bohle RM, Pauls K, Eichner G, Alhenc-Gelas F, Danilov SM, Franke FE . Angiotensin-converting enzyme in non-neoplastic kidney diseases. Kidney Int 1999; 56: 1442–1454.
Darby IA, Congiu M, Fernley RT, Sernia C, Coghlan JP . Cellular and ultrastructural location of angiotensinogen in rat and sheep kidney. Kidney Int 1994; 46: 1557–1560.
Darby IA, Sernia C . In situ hybridization and immunohistochemistry of renal angiotensinogen in neonatal and adult rat kidneys. Cell Tissue Res 1995; 281: 197–206.
Ingelfinger JR, Zuo WM, Fon EA, Ellison KE, Dzau VJ . In situ hybridization evidence for angiotensinogen messenger RNA in the rat proximal tubule. An hypothesis for the intrarenal renin angiotensin system. J Clin Invest 1990; 85: 417–423.
Richoux JP, Cordonnier JL, Bouhnik J, Clauser E, Corvol P, Menard J, Grignon G . Immunocytochemical localization of angiotensinogen in rat liver and kidney. Cell Tissue Res 1983; 233: 439–451.
Braam B, Mitchell KD, Fox J, Navar LG . Proximal tubular secretion of angiotensin II in rats. Am J Physiol 1993; 264: F891–F898.
Carvajal G, Rodriguez-Vita J, Rodrigues-Diez R, Sanchez-Lopez E, Ruperez M, Cartier C, Esteban V, Ortiz A, Egido J, Mezzano SA, Ruiz-Ortega M . Angiotensin II activates the Smad pathway during epithelial mesenchymal transdifferentiation. Kidney Int 2008; 74: 585–595.
Neilson EG . Mechanisms of disease: fibroblasts—a new look at an old problem. Nat Clin Pract Nephrol 2006; 2: 101–108.
Wood JM, Maibaum J, Rahuel J, Grutter MG, Cohen NC, Rasetti V, Ruger H, Goschke R, Stutz S, Fuhrer W, Schilling W, Rigollier P, Yamaguchi Y, Cumin F, Baum HP, Schnell CR, Herold P, Mah R, Jensen C, O′Brien E, Stanton A, Bedigian MP . Structure-based design of aliskiren, a novel orally effective renin inhibitor. Biochem Biophys Res Commun 2003; 308: 698–705.
Ganten D, Wagner J, Zeh K, Bader M, Michel JB, Paul M, Zimmermann F, Ruf P, Hilgenfeldt U, Ganten U . Species specificity of renin kinetics in transgenic rats harboring the human renin and angiotensinogen genes. Proc Natl Acad Sci USA 1992; 89: 7806–7810.
Mullins JJ, Peters J, Ganten D . Fulminant hypertension in transgenic rats harbouring the mouse Ren-2 gene. Nature 1990; 344: 541–544.
Mervaala EM, Muller DN, Park JK, Schmidt F, Lohn M, Breu V, Dragun D, Ganten D, Haller H, Luft FC . Monocyte infiltration and adhesion molecules in a rat model of high human renin hypertension. Hypertension 1999; 33: 389–395.
Kelly DJ, Wilkinson-Berka JL, Allen TJ, Cooper ME, Skinner SL . A new model of diabetic nephropathy with progressive renal impairment in the transgenic (mRen-2)27 rat (TGR). Kidney Int 1998; 54: 343–352.
Mervaala E, Muller DN, Schmidt F, Park JK, Gross V, Bader M, Breu V, Ganten D, Haller H, Luft FC . Blood pressure-independent effects in rats with human renin and angiotensinogen genes. Hypertension 2000; 35: 587–594.
Pilz B, Shagdarsuren E, Wellner M, Fiebeler A, Dechend R, Gratze P, Meiners S, Feldman DL, Webb RL, Garrelds IM, Jan Danser AH, Luft FC, Muller DN . Aliskiren, a human renin inhibitor, ameliorates cardiac and renal damage in double-transgenic rats. Hypertension 2005; 46: 569–576.
Shagdarsuren E, Wellner M, Braesen JH, Park JK, Fiebeler A, Henke N, Dechend R, Gratze P, Luft FC, Muller DN . Complement activation in angiotensin II-induced organ damage. Circ Res 2005; 97: 716–724.
Bachmann S, Mundel P . Nitric oxide in the kidney: synthesis, localization, and function. Am J Kidney Dis 1994; 24: 112–129.
Nakayama T, Sato W, Kosugi T, Zhang L, Campbell-Thompson M, Yoshimura A, Croker BP, Johnson RJ, Nakagawa T . Endothelial injury due to eNOS deficiency accelerates the progression of chronic renal disease in the mouse. Am J Physiol Renal Physiol 2009; 296: F317–F327.
Yamamoto E, Kataoka K, Dong YF, Nakamura T, Fukuda M, Tokutomi Y, Matsuba S, Nako H, Nakagata N, Kaneko T, Ogawa H, Kim-Mitsuyama S . Aliskiren enhances the protective effects of valsartan against cardiovascular and renal injury in endothelial nitric oxide synthase-deficient mice. Hypertension 2009; 54: 633–638.
Ino J, Kojima C, Osaka M, Nitta K, Yoshida M . Dynamic observation of mechanically-injured mouse femoral artery reveals an antiinflammatory effect of renin inhibitor. Arterioscler Thromb Vasc Biol 2009; 29: 1858–1863.
Rossing P . Diabetic nephropathy: worldwide epidemic and effects of current treatment on natural history. Curr Diab Rep 2006; 6: 479–483.
Hollenberg NK, Price DA, Fisher ND, Lansang MC, Perkins B, Gordon MS, Williams GH, Laffel LM . Glomerular hemodynamics and the renin-angiotensin system in patients with type 1 diabetes mellitus. Kidney Int 2003; 63: 172–178.
Tryggvason K, Patrakka J, Wartiovaara J . Hereditary proteinuria syndromes and mechanisms of proteinuria. N Engl J Med 2006; 354: 1387–1401.
White KE, Bilous RW, Marshall SM, El NM, Remuzzi G, Piras G, De CS, Viberti G . Podocyte number in normotensive type 1 diabetic patients with albuminuria. Diabetes 2002; 51: 3083–3089.
Sato Y, Wharram BL, Lee SK, Wickman L, Goyal M, Venkatareddy M, Chang JW, Wiggins JE, Lienczewski C, Kretzler M, Wiggins RC . Urine podocyte mRNAs mark progression of renal disease. J Am Soc Nephrol 2009; 20: 1041–1052.
Phillips LM, Dai T, Feldman DL, LaPage J, Adler SG . Aliskiren attenuates high glucose induced extracelllular matrix and protects against cell death in cultured podocytes (Pods). J Am Soc Nephrol 2007; 18: 169 (Abstract).
Waldmeier F, Glaenzel U, Wirz B, Oberer L, Schmid D, Seiberling M, Valencia J, Riviere GJ, End P, Vaidyanathan S . Absorption, distribution, metabolism, and elimination of the direct renin inhibitor aliskiren in healthy volunteers. Drug Metab Dispos 2007; 35: 1418–1428.
Parving HH, Persson F, Lewis JB, Lewis EJ, Hollenberg NK . Aliskiren combined with losartan in type 2 diabetes and nephropathy. N Engl J Med 2008; 358: 2433–2446.
Persson F, Rossing P, Schjoedt KJ, Juhl T, Tarnow L, Stehouwer CD, Schalkwijk C, Boomsma F, Frandsen E, Parving HH . Time course of the antiproteinuric and antihypertensive effects of direct renin inhibition in type 2 diabetes. Kidney Int 2008; 73: 1419–1425.
Dong YF, Kataoka K, Nakamura T, Fukuda M, Tokutomi Y, Nako H, Liu L, Ogawa H, Kim-Mitsuyama S . Non-depressor dosage of renin inhibitor enhances protective effects of ARB on type 2 diabetic nephropathy. 2009. The 32nd Annual Scientific Meeting of the Japanese Society of Hypertension, October 1-3, 2009 Program and Abstracts, PL1-1, Page 153 (In Japanese).
Feldman DL, Jin L, Xuan H, Contrepas A, Zhou Y, Webb RL, Mueller DN, Feldt S, Cumin F, Maniara W, Persohn E, Schuetz H, Jan Danser AH, Nguyen G . Effects of aliskiren on blood pressure, albuminuria, and (pro)renin receptor expression in diabetic TG(mRen-2)27 rats. Hypertension 2008; 52: 130–136.
Kelly DJ, Zhang Y, Moe G, Naik G, Gilbert RE . Aliskiren, a novel renin inhibitor, is renoprotective in a model of advanced diabetic nephropathy in rats. Diabetologia 2007; 50: 2398–2404.
Richter WF, Whitby BR, Chou RC . Distribution of remikiren, a potent orally active inhibitor of human renin, in laboratory animals. Xenobiotica 1996; 26: 243–254.
Feldman DL, Persohn E, Schuetz H, Jin L, Miserindino-Moltini R, Xuan H, Zhuang S, Zhou W . Renal localization of the renin inhibitor aliskiren. J Clin Hypertens 2006; 8: 80–81 (Abstract).
Vaneckova I, Cervenka L, Huskova Z, Vanourkova Z, Kopkan L . The effect of aliskiren on the development of hypertension and angiotensin II levels in heterozygous Ren-2 transgenic rats. J Hypertens 2008; S521 (Abstract).
Frattola A, Parati G, Cuspidi C, Albini F, Mancia G . Prognostic value of 24-h blood pressure variability. J Hypertens 1993; 11: 1133–1137.
Kario K, Lowy A, Munck VC, Annemans L . 24-h blood pressure control- a predictor for clinical outcomes. Curr Hypertens Rev 2009; 5: 102–122.
Parati G, Pomidossi G, Albini F, Malaspina D, Mancia G . Relationship of 24-h blood pressure mean and variability to severity of target-organ damage in hypertension. J Hypertens 1987; 5: 93–98.
Rosenberg ME, Correa-Rotter R, Inagami T, Kren SM, Hostetter TH . Glomerular renin synthesis and storage in the remnant kidney in the rat. Kidney Int 1991; 40: 677–683.
Toma I, Kang J, Peti-Peterdi J . Imaging renin content and release in the living kidney. Nephron Physiol 2009; 103: 71–74.
Tufro-McReddie A, Johns DW, Geary KM, Dagli H, Everett AD, Chevalier RL, Carey RM, Gomez RA . Angiotensin II type 1 receptor: role in renal growth and gene expression during normal development. Am J Physiol 1994; 266: F911–F918.
Singh VP, Baker KM, Kumar R . Activation of the intracellular renin-angiotensin system in cardiac fibroblasts by high glucose: role in extracellular matrix production. Am J Physiol Heart Circ Physiol 2008; 294: H1675–H1684.
Schweda F, Friis U, Wagner C, Skott O, Kurtz A . Renin release. Physiology (Bethesda) 2007; 22: 310–319.
Silver RB, Reid AC, Mackins CJ, Askwith T, Schaefer U, Herzlinger D, Levi R . Mast cells: a unique source of renin. Proc Natl Acad Sci USA 2004; 101: 13607–13612.
Krop M, Garrelds IM, de Bruin RJ, van Gool JM, Fisher ND, Hollenberg NK, Jan Danser AH . Aliskiren accumulates in renin secretory granules and binds plasma prorenin. Hypertension 2008; 52: 1076–1083.
Krop M, van VR, Garrelds IM, de Bruin RJ, van Gool JM, van den Meiracker AH, Thio M, van Daele PL, Danser AH . Cardiac renin levels are not influenced by the amount of resident mast cells. Hypertension 2009; 54: 315–321.
Peti-Peterdi J, Fintha A, Fuson AL, Tousson A, Chow RH . Real-time imaging of renin release in vitro. Am J Physiol Renal Physiol 2004; 287: F329–F335.
Oh BH, Mitchell J, Herron JR, Chung J, Khan M, Keefe DL . Aliskiren, an oral renin inhibitor, provides dose-dependent efficacy and sustained 24-h blood pressure control in patients with hypertension. J Am Coll Cardiol 2007; 49: 1157–1163.
Nguyen G, Delarue F, Berrou J, Rondeau E, Sraer JD . Specific receptor binding of renin on human mesangial cells in culture increases plasminogen activator inhibitor-1 antigen. Kidney Int 1996; 50: 1897–1903.
Danser AH . (Pro)renin receptors: are they biologically relevant? Curr Opin Nephrol Hypertens 2009; 18: 74–78.
Ichihara A, Sakoda M, Kurauchi-Mito A, Kaneshiro Y, Itoh H . Renin, prorenin and the kidney: a new chapter in an old saga. J Nephrol 2009; 22: 306–311.
Nguyen G, Contrepas A . The (pro)renin receptors. J Mol Med 2008; 86: 643–646.
Nguyen G, Delarue F, Burckle C, Bouzhir L, Giller T, Sraer JD . Pivotal role of the renin/prorenin receptor in angiotensin II production and cellular responses to renin. J Clin Invest 2002; 109: 1417–1427.
Nguyen G . Increased cyclooxygenase-2, hyperfiltration, glomerulosclerosis, and diabetic nephropathy: put the blame on the (pro)renin receptor? Kidney Int 2006; 70: 618–620.
Cousin C, Bracquart D, Contrepas A, Corvol P, Muller L, Nguyen G . Soluble form of the (pro)renin receptor generated by intracellular cleavage by furin is secreted in plasma. Hypertension 2009; 53: 1077–1082.
Hamming I, Contrepas A, Nguyen G, Huitema S, Navis J, van Goor H . Regulation of the renal renin/(pro)renin receptor (RPR) by ACE inhibition and sodium restriction. J Am Soc Nephrol 2005; 16: 120 (Abstract).
Ichihara A, Kaneshiro Y, Takemitsu T, Sakoda M, Itoh H . The (pro)renin receptor and the kidney. Semin Nephrol 2007; 27: 524–528.
Nabi AH, Kageshima A, Uddin MN, Nakagawa T, Park EY, Suzuki F . Binding properties of rat prorenin and renin to the recombinant rat renin/prorenin receptor prepared by a baculovirus expression system. Int J Mol Med 2006; 18: 483–488.
Batenburg WW, Krop M, Garrelds IM, de VR, de Bruin RJ, Burckle CA, Muller DN, Bader M, Nguyen G, Danser AH . Prorenin is the endogenous agonist of the (pro)renin receptor. Binding kinetics of renin and prorenin in rat vascular smooth muscle cells overexpressing the human (pro)renin receptor. J Hypertens 2007; 25: 2441–2453.
Batenburg WW, de Bruin RJ, van Gool JM, Muller DN, Bader M, Nguyen G, Danser AH . Aliskiren-binding increases the half life of renin and prorenin in rat aortic vascular smooth muscle cells. Arterioscler Thromb Vasc Biol 2008; 28: 1151–1157.
Huang Y, Noble NA, Zhang J, Xu C, Border WA . Renin-stimulated TGF-beta1 expression is regulated by a mitogen-activated protein kinase in mesangial cells. Kidney Int 2007; 72: 45–52.
Feldt S, Batenburg WW, Mazak I, Maschke U, Wellner M, Kvakan H, Dechend R, Fiebeler A, Burckle C, Contrepas A, Jan Danser AH, Bader M, Nguyen G, Luft FC, Muller DN . Prorenin and renin-induced extracellular signal-regulated kinase 1/2 activation in monocytes is not blocked by aliskiren or the handle-region peptide. Hypertension 2008; 51: 682–688.
Saris JJ, ‘t Hoen PA, Garrelds IM, Dekkers DH, den Dunnen JT, Lamers JM, Danser AHJ . Prorenin induces intracellular signaling in cardiomyocytes independently of angiotensin II. Hypertens 2006; 48: 564–571.
Schefe JH, Neumann C, Goebel M, Danser J, Kirsch S, Gust R, Kintscher U, Unger T, Funke-Kaiser H . Prorenin engages the (pro)renin receptor like renin and both ligand activities are unopposed by aliskiren. J Hypertens 2008; 26: 1787–1794.
Huang Y, Wongamorntham S, Kasting J, McQuillan D, Owens RT, Yu L, Noble NA, Border W . Renin increases mesangial cell transforming growth factor-beta1 and matrix proteins through receptor-mediated, angiotensin II-independent mechanisms. Kidney Int 2006; 69: 105–113.
Ichihara A, Hayashi M, Kaneshiro Y, Suzuki F, Nakagawa T, Tada Y, Koura Y, Nishiyama A, Okada H, Uddin MN, Nabi AH, Ishida Y, Inagami T, Saruta T . Inhibition of diabetic nephropathy by a decoy peptide corresponding to the ‘handle’ region for nonproteolytic activation of prorenin. J Clin Invest 2004; 114: 1128–1135.
Derkx FH, Deinum J, Lipovski M, Verhaar M, Fischli W, Schalekamp MA . Nonproteolytic ‘activation’ of prorenin by active site-directed renin inhibitors as demonstrated by renin-specific monoclonal antibody. J Biol Chem 1992; 267: 22837–22842.
Dzau VJ, Gonzalez D, Kaempfer C, Dubin D, Wintroub BU . Human neutrophils release serine proteases capable of activating prorenin. Circ Res 1987; 60: 595–601.
Danser AH, Derkx FH, Schalekamp MA, Hense HW, Riegger GA, Schunkert H . Determinants of interindividual variation of renin and prorenin concentrations: evidence for a sexual dimorphism of (pro)renin levels in humans. J Hypertens 1998; 16: 853–862.
Deinum J, Ronn B, Mathiesen E, Derkx FH, Hop WC, Schalekamp MA . Increase in serum prorenin precedes onset of microalbuminuria in patients with insulin-dependent diabetes mellitus. Diabetologia 1999; 42: 1006–1010.
Luetscher JA, Kraemer FB, Wilson DM, Schwartz HC, Bryer-Ash M . Increased plasma inactive renin in diabetes mellitus. A marker of microvascular complications. N Engl J Med 1985; 312: 1412–1417.
Mercure C, Prescott G, Lacombe MJ, Silversides DW, Reudelhuber TL . Chronic increases in circulating prorenin are not associated with renal or cardiac pathologies. Hypertension 2009; 53: 1062–1069.
Peters B, Grisk O, Becher B, Wanka H, Kuttler B, Ludemann J, Lorenz G, Rettig R, Mullins JJ, Peters J . Dose-dependent titration of prorenin and blood pressure in Cyp1a1ren-2 transgenic rats: absence of prorenin-induced glomerulosclerosis. J Hypertens 2008; 26: 102–109.
Ichihara A, Kaneshiro Y, Suzuki F . Prorenin receptor blockers: effects on cardiovascular complications of diabetes and hypertension. Expert Opin Investig Drugs 2006; 15: 1137–1139.
Feldt S, Maschke U, Dechend R, Luft FC, Muller DN . The putative (pro)renin receptor blocker HRP fails to prevent (pro)renin signaling. J Am Soc Nephrol 2008; 19: 743–748.
Muller DN, Klanke B, Feldt S, Cordasic N, Hartner A, Schmieder RE, Luft FC, Hilgers KF . (Pro)renin receptor peptide inhibitor ‘handle-region’ peptide does not affect hypertensive nephrosclerosis in Goldblatt rats. Hypertension 2008; 51: 676–681.
Acknowledgements
Unpublished data included in this review were contributed by Mr M Avigdor, Mss C-W Hu and J Leung-Chu, and Drs A Jeng, E Persohn and H Schuetz. Ms Therese Johnsen provided invaluable assistance in preparing the paper.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
David L Feldman is a full-time employee of Novartis Pharmaceuticals.
Rights and permissions
About this article
Cite this article
Feldman, D. New insights into the renoprotective actions of the renin inhibitor aliskiren in experimental renal disease. Hypertens Res 33, 279–287 (2010). https://doi.org/10.1038/hr.2010.19
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/hr.2010.19
Keywords
This article is cited by
-
Protective Effects of Aliskiren on Atrial Ionic Remodeling in a Canine Model of Rapid Atrial Pacing
Cardiovascular Drugs and Therapy (2014)
-
Mechanistic insights into the antifibrotic activity of aliskiren in the kidney
Hypertension Research (2012)