- OUTLOOK
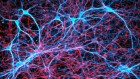
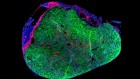
The mouth’s curative superpowers
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Rent or buy this article
Prices vary by article type
from$1.95
to$39.95
Prices may be subject to local taxes which are calculated during checkout
doi: https://doi.org/10.1038/d41586-021-02923-7
This article is part of Nature Outlook: Oral health, an editorially independent supplement produced with the financial support of third parties. About this content.
References
Iglesias-Bartolome, R. Sci. Transl. Med. 10, eaap8798 (2018).
Szpaderska, A. M., Zuckerman, J. D. & DiPietro, L. A. J. Dent. Res. 82, 621–626 (2003).
Szpaderska, A. M., Walsh, C. G., Steinberg, M. J. & DiPietro, L. A. J. Dent. Res. 84, 309–314 (2005).
Enoch, S. et al. J. Dent. Res. 88, 916–921 (2009).
Davies, L. C. et al. Stem Cells Dev. 19, 819–830 (2010).
Yang. Y., Knight, R., Stephens, P. & Zhang, Y. J. Oral Pathol. Med. 49, 342–349 (2020).
Kou, X. et al. Sci. Transl. Med. 10, eaai8524 (2018).

 Homing in on an oral link to inflammatory disease
Homing in on an oral link to inflammatory disease
 Dentists and doctors need to play on the same team
Dentists and doctors need to play on the same team
 Oral microbiome findings challenge dentistry dogma
Oral microbiome findings challenge dentistry dogma
 Lessons from the ancient oral microbiome
Lessons from the ancient oral microbiome
 Investigating the mouth–COVID connection
Investigating the mouth–COVID connection
 The fluoride wars rage on
The fluoride wars rage on
 Optics shine a light on dental imaging
Optics shine a light on dental imaging
 The advocacy frontier
The advocacy frontier
 Research round-up: oral health
Research round-up: oral health