- NEWS
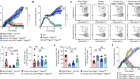
How can countries stretch COVID vaccine supplies? Scientists are divided over dosing strategies
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Rent or buy this article
Prices vary by article type
from$1.95
to$39.95
Prices may be subject to local taxes which are calculated during checkout
Nature 589, 182 (2021)
doi: https://doi.org/10.1038/d41586-021-00001-6

 The lightning-fast quest for COVID vaccines — and what it means for other diseases
The lightning-fast quest for COVID vaccines — and what it means for other diseases
 Could new COVID variants undermine vaccines? Labs scramble to find out
Could new COVID variants undermine vaccines? Labs scramble to find out
 The underdog coronavirus vaccines that the world will need if front runners stumble
The underdog coronavirus vaccines that the world will need if front runners stumble
 How anti-ageing drugs could boost COVID vaccines in older people
How anti-ageing drugs could boost COVID vaccines in older people
 How COVID vaccines are being divvied up around the world
How COVID vaccines are being divvied up around the world