- NEWS AND VIEWS
- Retraction 27 September 2021
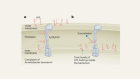
RETRACTED ARTICLE: A two-pronged attack on antibiotic-resistant microbes
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Rent or buy this article
Prices vary by article type
from$1.95
to$39.95
Prices may be subject to local taxes which are calculated during checkout
Nature 589, 517-518 (2021)
doi: https://doi.org/10.1038/d41586-020-03660-z
Updates & Corrections
-
Retraction 27 September 2021: In view of the fact that the authors of the article ‘IspH inhibitors kill Gram-negative bacteria and mobilize immune clearance’ (K. S. Singh et al. Nature 589, 597–602; 2021) are retracting their report, the authors of this News & Views wish to retract their article, which dealt with this study and was based on the accuracy and reproducibility of the data in the study.
References
Singh, K. S. et al. Nature 589, 597–602 (2021).
Zhao, L., Chang, W.-C., Xiao, Y., Liu, H. W. & Liu, P. Annu. Rev. Biochem. 82, 497–530 (2013).
Janthawornpong, K. et al. J. Am. Chem. Soc. 135, 1816–1822 (2013).
Jomaa, H. et al. Science 285, 1573–1576 (1999).
McAteer, S., Coulson, A., McLennan, N. & Masters, M. J. Bacteriol. 183, 7403–7407 (2001).
Wang, K. et al. J. Am. Chem. Soc. 132, 6719–6727 (2010).
Zinglé, C., Kuntz, L., Tritsch, D., Grosdemange-Billiard, C. & Rohmer, M. J. Org. Chem. 75, 3203–3207 (2010).
Morita, C. T., Jin, C., Sarikonda, G. & Wang, H. Immunol. Rev. 215, 59–76 (2007).
Willcox, C. R., Mohammed, F. & Willcox, B. E. Immunol. Rev. 298, 25–46 (2020).
Silva-Santos, B., Mensurado, S. & Coffelt, S. B. Nature Rev. Cancer 19, 392–404 (2019).

 Read the paper: IspH inhibitors kill Gram-negative bacteria and mobilize immune clearance
Read the paper: IspH inhibitors kill Gram-negative bacteria and mobilize immune clearance
 Modular synthesis enables molecular ju-jitsu in the fight against antibiotic resistance
Modular synthesis enables molecular ju-jitsu in the fight against antibiotic resistance
 New antibiotics target the outer membrane of bacteria
New antibiotics target the outer membrane of bacteria