- NEWS FEATURE
Why do COVID death rates seem to be falling?
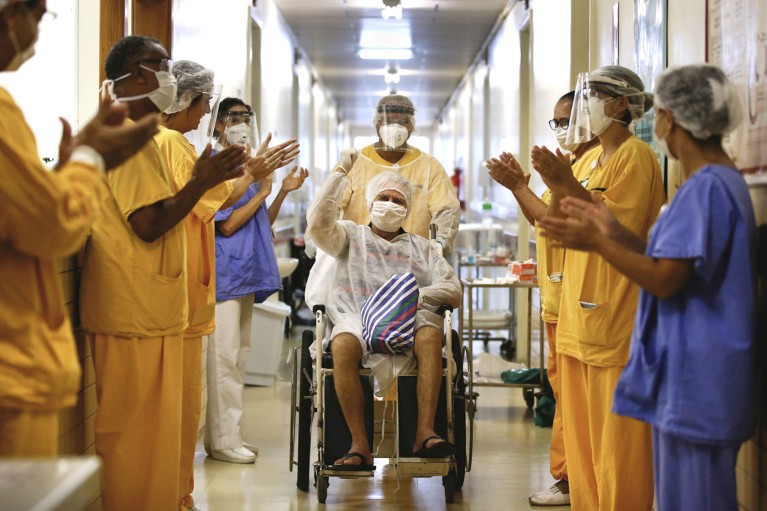
More individuals treated for severe COVID-19 seem to be surviving now than in the early weeks of the pandemic. Credit: Diego Vara/Reuters
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Rent or buy this article
Prices vary by article type
from$1.95
to$39.95
Prices may be subject to local taxes which are calculated during checkout
Nature 587, 190-192 (2020)
doi: https://doi.org/10.1038/d41586-020-03132-4
References
Dennis, J. M., McGovern, A. P., Vollmer, S. J. & Mateen, B. A. Crit. Care Med. https://doi.org/10.1097/CCM.0000000000004747 (2020).
The RECOVERY Collaborative Group. N. Engl. J. Med. https://doi.org/10.1056/NEJMoa2022926 (2020).
Bessière, F. et al. JAMA Cardiol. 5, 1067–1069 (2020).
Sinha, P., Matthay, M. A. & Calfee, C. S. JAMA Intern. Med. 180, 1152–1154 (2020).
Stone, J. H. et al. N. Engl. J. Med. https://doi.org/10.1056/NEJMoa2028836 (2020).
The RECOVERY Collaborative Group. N. Engl. J. Med. https://doi.org/10.1056/NEJMoa2021436 (2020).
Beigel, J. H. et al. N. Engl. J. Med. https://doi.org/10.1056/NEJMoa2007764 (2020).
Agarwal, A. et al. Br. Med. J. 371, m3939 (2020).

 Hopes rise for coronavirus drug remdesivir
Hopes rise for coronavirus drug remdesivir
 Chloroquine hype is derailing the search for coronavirus treatments
Chloroquine hype is derailing the search for coronavirus treatments
 Evidence lags behind excitement over blood plasma as a coronavirus treatment
Evidence lags behind excitement over blood plasma as a coronavirus treatment
 Coronavirus blood-clot mystery intensifies
Coronavirus blood-clot mystery intensifies