- NEWS AND VIEWS
CRISPR tool scales up to interrogate a huge line-up of viral suspects
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Rent or buy this article
Prices vary by article type
from$1.95
to$39.95
Prices may be subject to local taxes which are calculated during checkout
Nature 582, 188-189 (2020)
doi: https://doi.org/10.1038/d41586-020-01447-w
References
Smolinski, M. S., Hamburg, M. A. & Lederberg, J. (eds) Microbial Threats to Health in the 21st Century (National Academies Press, 2003).
Morens, D. M. & Fauci, A. S. PLoS Pathog. 9, e1003467 (2013).
Ackerman, C. M. et al. Nature 582, 277–282 (2020).
Myhrvold, C. et al. Science 360, 444–448 (2014).
Terns, M. P. Mol. Cell 72, 404–412 (2018).
Broughton, J. P. et al. Nature Biotechnol. https://doi.org/10.1038/s41587-020-0513-4 (2020).
Wang D. et al. Proc. Natl Acad. Sci. USA 99, 15687–15692 (2002).
Hanson, K. E. & Couturier, M. R. Clin. Infect. Dis. 63, 1361–1367 (2016).
Wu, G., Miller, S. & Chiu, C. Y. Annu. Rev. Pathol. 14, 319–338 (2019).

 Read the paper: Massively multiplexed nucleic acid detection using Cas13
Read the paper: Massively multiplexed nucleic acid detection using Cas13
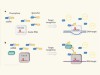 From CRISPR scissors to virus sensors
From CRISPR scissors to virus sensors
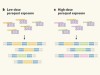 CRISPR tool puts RNA on the record
CRISPR tool puts RNA on the record