- OUTLOOK
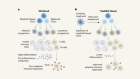
Diet should be a tool for researchers, not a treatment
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Rent or buy this article
Prices vary by article type
from$1.95
to$39.95
Prices may be subject to local taxes which are calculated during checkout
Nature 577, S23 (2020)
doi: https://doi.org/10.1038/d41586-020-00202-5
This article is part of Nature Outlook: The gut microbiome, an editorially independent supplement produced with the financial support of third parties. About this content.
References
Johnston, B. C. et al. Ann. Intern. Med. 171, 756–764 (2019).
David, L. A. et al. Nature 505, 559–563 (2014).
Carmody, R. N. et al. Nature Microbiol. 4, 2052–2063 (2019).
Wolf, A. R. et al. Cell Host Microbe 26, 463–477 (2019).
Gehrig, J. L. et al. Science 365, eaau4732 (2019).
Competing Interests
P.J.T. is on the scientific advisory boards for Kaleido Biosciences, Pendulum Therapeutics, Seres Therapeutics and Snipr Biome.


 The hunt for a healthy microbiome
The hunt for a healthy microbiome
 Homing in on the molecules from microbes
Homing in on the molecules from microbes
 The complex relationship between drugs and the microbiome
The complex relationship between drugs and the microbiome
 Could a bacteria-stuffed pill cure autoimmune diseases?
Could a bacteria-stuffed pill cure autoimmune diseases?
 Could the gut microbiome be linked to autism?
Could the gut microbiome be linked to autism?
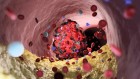
 Fighting cancer with microbes
Fighting cancer with microbes
 Rich data sets could end costly drug discovery
Rich data sets could end costly drug discovery
 Therapeutic microbes to tackle disease
Therapeutic microbes to tackle disease
 Highlights from studies on the gut microbiome
Highlights from studies on the gut microbiome