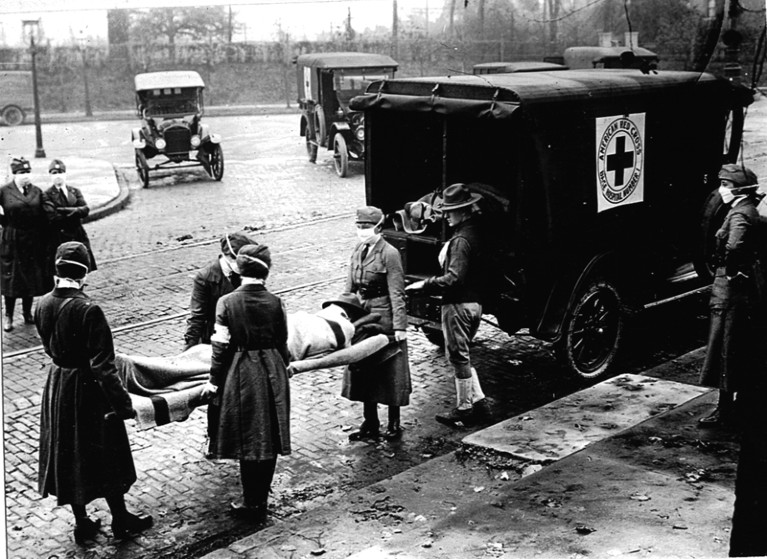
The global flu pandemic of 1918–19 should help to focus minds on the current threat.Credit: PhotoQuest/Getty
One hundred years ago this month, the 1918 influenza virus was just starting to spread. It would become the greatest public-health crisis of the twentieth century, claiming some 50 million to 100 million lives. The centenary has raised questions over whether such a severe flu pandemic could happen today, and whether the world is prepared.
There are few data points to go on — flu pandemics happen only three or four times a century — but one risk is certainly higher: 7.6 billion people share the planet in 2018, up from 1.9 billion in 1918. Feeding all those extra people has also meant a huge rise in livestock numbers, intensive farming and the numbers of animals being transported around the world. Scientists say that the genetic mixing and evolution of animal flu viruses is thus being amplified, increasing the chance of viruses gaining the potential to jump to humans and, if they can spread easily between people, causing a human pandemic. Our just-in-time global production systems and service economies are also exquisitely vulnerable to the quickly cascading disruption that a severe pandemic would cause.
The case-fatality rate in the 1918 pandemic was around 2.5% (compared with less than 0.1% in other flu pandemics), and a comparable or worse rate in a future pandemic cannot be discounted. There are two hypotheses to explain the 1918 strain’s high lethality: cytokine storms and secondary bacterial infection. (In a cytokine storm, the body’s immune system overreacts, causing tissue and organ damage, and even death.)
But in an intriguing 2008 paper (D. M. Morens, J. K. Taubenberger and A. S. Fauci J. Infect. Dis. 198, 962–970; 2008), researchers went through data from almost 8,500 post-mortem records from the 1918–19 pandemic and discovered what doctors knew at the time, but which was subsequently forgotten — that most people in the pandemic probably died of secondary pneumonia from common bacterial pathogens.
Were this latter pattern to dominate in any severe future pandemic, the availability of antibiotics, which didn’t exist in 1918, would dent death rates, provided that sufficient stockpiles were available. More broadly, the importance of robust public-health systems and surge capacity in hospitals as a basic bulwark against epidemic and pandemic threats of all kinds cannot be overstated. Yet health systems remain weak in many countries.
Speak to scientists, and they all agree on what must be the number one research goal for effective mitigation of any future pandemic: a universal flu vaccine. At present, the seasonal flu vaccine usually has to be updated every year or so to match the circulating virus strains — which are continually evolving — and these vaccines provide no protection against an altogether new pandemic subtype.
The 2009 swine flu pandemic showed that it takes months to start producing a vaccine against a pandemic flu virus. In many countries, substantial amounts of vaccine arrived only after the first wave of infection had already passed. Fortunately, the 2009 virus was relatively mild.
A universal vaccine, ideally offering lifelong protection against all flu subtypes, would improve the effectiveness of seasonal flu vaccines and offer protection against novel pandemic threats. Even a vaccine that is around 75% effective in preventing disease symptoms would be a huge public advance, scientists reckon (C. I. Paules et al. Immunity 47, 599–603; 2017).
A major international workshop on developing such a vaccine was held last year in Rockville, Maryland, and identified many research gaps — including the complexity of the immune response to infection and vaccination — and a road map for addressing them. Yet the United States, one of the largest flu-research funders, last year invested just US$75 million on universal flu vaccine research and development.
Whether the world will again ever see the likes of the 1918–19 flu pandemic cannot be reliably predicted, but given the stakes, it is best for society, as a whole, to plan for worst-case scenarios. And advocates rightly argue that the research and development of a universal flu vaccine — ultimately the only effective defence against future pandemics — merits a programme equivalent in scale to the Manhattan Project.

 How to beat the next Ebola
How to beat the next Ebola
 Mutations explain poor showing of 2012 flu vaccine
Mutations explain poor showing of 2012 flu vaccine
 Study revives bird origin for 1918 flu pandemic
Study revives bird origin for 1918 flu pandemic
 Book review of Pale Rider: The Spanish Flu of 1918 and How it Changed the World
Book review of Pale Rider: The Spanish Flu of 1918 and How it Changed the World