Abstract
Activated monocytes and macrophages secrete the inflammatory cytokine tumor necrosis factor-α (TNF-α). TNF-α is produced as a 26 kd transmembrane protein that is cleaved to release a 17 kd soluble protein. TNF-α in both forms is biologically active. The intracellular trafficking of membrane-associated TNF-α in lipopolysaccharide-activated mouse macrophages was assessed after treatment with the metalloprotease inhibitor BB-3103, which prevents the cleavage of pro–TNF-α. Immunoprecipitation and immunofluorescence studies showed sustained expression of cell-associated TNF-α in the presence of the inhibitor. Cell immunoreactivity and surface biotinylation revealed that uncleaved TNF-α accumulated on the cell surface and was endocytosed, appearing in intracellular vesicles. Perturbation of post-Golgi traffic blocked the surface expression of 26 kd TNF-α. Tracking a bolus of TNF-α over time in cycloheximide-treated cells confirmed that uncleaved TNF-α is first transported to the cell surface and subsequently endocytosed. Vesicular structures immunoreactive for TNF-α were identified as endosomes by double labeling. The secretory and membrane-associated endocytic trafficking of TNF-α provides a mechanism for modulating the quantity of biologically active 26 kd TNF-α expressed on macrophages, allowing regulation of paracrine and autocrine responses.
Similar content being viewed by others
Introduction
Tumor necrosis factor-α (TNF-α) is an important pro-inflammatory cytokine produced and secreted primarily from macrophages and monocytes in response to a bacterial challenge or tumor burden. It is capable of a broad range of immuno-responsive actions that are central to the pathophysiology of acute and chronic inflammation and cancer (Aggarwal and Natarajan, 1996; Fiers, 1991). Overproduction and secretion of TNF-α contributes to the acute symptoms of septic shock (Tracey, 1991), and to the more chronic effects of diseases such as rheumatoid arthritis and Crohn's disease (Beutler, 1999). The murine macrophage cell line RAW264 is widely used in studies of the regulation of TNF-α production (Darville et al, 1994; Kol et al, 1998). Exposure of RAW264 cells to bacterial lipopolysaccharide (LPS) leads to the rapid appearance of TNF-α mRNA (Chang et al, 1999) and a rapid accumulation of TNF-α protein in the Golgi complex (Shurety et al, 2000). The swift induction of relatively large quantities of this protein in mouse macrophages makes this an ideal system to dissect and characterize the intracellular trafficking of TNF-α.
TNF-α is synthesized as a type II transmembrane, 26 kd precursor (pro–TNF-α), which is then proteolytically cleaved to release a soluble, mature 17 kd subunit, which ultimately gains biological activity upon formation of a 52 kd homotrimer (Jue et al, 1990; Kriegler et al, 1988). Pro–TNF-α is processed by a membrane-associated metalloprotease, and the release of soluble TNF-α can be effectively inhibited by metalloprotease inhibitors (Black et al, 1997; Gearing et al, 1994; Kim et al, 1993; McGeehan et al, 1994; Mohler et al, 1994; Moss et al, 1997). The specific enzyme responsible for this cleavage has been identified as the TNF-α converting enzyme (TACE) ADAM 17, which is also a member of the ADAM family of disintegrin-proteinases (Black et al, 1997; Moss et al, 1997). More recently, TACE was also found to cleave several other membrane-anchored proteins (Peschon et al, 1998). The efficiency of TNF-α processing is normally high, up to 90% of pro–TNF-α is converted to the 17 kd form for acute release by activated monocytes (Solomon et al, 1997). The cleavage of pro–TNF-α is thought to occur at the cell surface (Black et al, 1997; Decoster et al, 1995; Glaser et al, 1999), although there is also evidence for earlier proteolytic processing at the level of the Golgi complex (Jue et al, 1990; Shurety et al, 2000; Solomon et al, 1997; Watanabe et al, 1998). Secreted 17 kd TNF-α can act locally in autocrine and paracrine modes and at long distances in an endocrine mode by binding to the two known TNF-α receptors (55 kd and 75 kd) to initiate the acute systemic effects of TNF-α (Vassalli, 1996).
TNF-α is also expressed on the cell surface of immune cells (Kinkhabwala et al, 1990). The 26 kd, membrane-anchored form of TNF-α is biologically active (Perez et al, 1990) and has distinct functions. This form mediates effects at the autocrine and local paracrine levels, in contrast to the long-range and systemic effects produced by the 17 kd subunits. The surface expression of 26 kd TNF-α can be enhanced experimentally in the presence of metalloprotease inhibitors or by expression of mutants with altered or deleted proteolytic cleavage sites. Under these conditions, the uncleaved 26 kd TNF-α is capable of killing tumor cells during cell-cell contact (Decoster et al, 1995, 1998; Perez et al, 1990). Membrane-associated TNF-α is also capable of interacting with the 55 and 75 kd TNF receptors, although with altered affinities. This interaction elicits additional cytokine and proliferative responses (Decoster et al, 1995) and initiates down-regulation of surface receptors during desensitization of cells preparing for endogenous production of TNF-α (Decoster et al, 1998). In activated cells treated with metalloprotease inhibitors there is a relatively modest or transient increase in the amount of uncleaved TNF-α on the cell surface (Gearing et al, 1994; McGeehan et al, 1994; Solomon et al, 1997). This observation suggests that there may be further processing or degradation of the pro–TNF-α. The mechanisms for delivery of pro–TNF-α to the cell surface and its removal from the cell surface have not been characterized.
In the present study we used the metalloprotease inhibitor BB-3103, which has been shown to inhibit the processing enzyme TACE, to block cleavage of pro–TNF-α in macrophages (Ancuta et al, 1997; Mitsiades et al, 1999; Sewter et al, 1999). Preventing the cleavage of 26 kd TNF-α enabled the characterization of the intracellular trafficking of membrane-associated TNF-α. Our results demonstrate that pro–TNF-α is trafficked from the Golgi complex to the cell surface where it can be either cleaved or endocytosed. Secretory and endocytic pathways are revealed as possible mechanisms for modulating the number and availability of biologically active pro–TNF-α molecules presented on the cell surface.
Results
BB-3103 Increases Cell-Associated 26 kd TNF-α
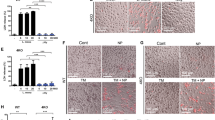
RAW264 cells were stimulated with 100 ng/ml of LPS in the absence or presence of the metalloprotease inhibitor, BB-3103, to measure the effect on TNF-α secretion. The effect of BB-3103 on the release of TNF-α from RAW 264 cells into the extracellular medium was determined first by an ELISA assay. Results showed a concentration-dependent inhibition of TNF-α release in the presence of BB-3103, with 80% to 95% inhibition at concentrations of 0.1 μm to > 1 μm (Fig. 1).
Treatment of macrophages with BB-3103 prevented the release of tumor necrosis factor α (TNF-α) into the medium. Adherent RAW264 cells were treated with 100 ng/ml of lipopolysaccharide (LPS) and various concentrations of BB-3103 for 2 hours (0.1 to 100 μm). The release of soluble TNF-α into the medium was measured using an ELISA assay. The inhibitor had a concentration-dependent effect of TNF-α release. Assays were performed in triplicate and data points are expressed as mean ± sem.
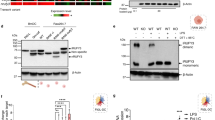
Immunoblotting of cell lysates was carried out to investigate the effect of BB-3103 on cell-associated TNF-α and its precursors. After 2 hours in the presence of the inhibitor, increased amounts of the 26 kd membrane-bound form of TNF-α were found in cell lysates (Fig. 2a). Cells tested at longer intervals (up to 16 hours) after LPS treatment continued to show increased retention of TNF-α in the presence of BB-3103 (data not shown). The effect of BB-3103 on the various intracellular TNF-α forms was tested by pulse-chase labeling and immunoprecipitation of 35S–TNF-α (Fig. 2b). The addition of 1 μm BB-3103 during the chase times resulted in a significant increase in the amount of 26 kd TNF-α in the cell extracts at the 60 minutes time point. In the absence of BB-3103, the 26 kd form was fully cleaved. A small amount of the 26 kd TNF-α was still visible in extracts of BB-3103–treated cells after a chase time of 120 minutes. These results show that BB-3103 is an effective inhibitor of TNF-α release and that BB-3103 prolongs the intracellular half-life of 26 kd TNF-α in macrophages.
BB-3103 increases cell-associated pro–TNF-α. a, Adherent RAW264 cells were treated with either 100 ng/ml of LPS or LPS and 1 μm BB-3103 for 2 hours. Equivalent aliquots of cell lysates were subjected to SDS-PAGE and immunoblotted for TNF-α. b, Adherent RAW264 cells were pulse-labeled for 15 minutes with 35S-translabel in the presence of LPS. Cells were chased for 0.5, 1, and 2 hours in the absence and presence of 1 μm BB-3103. Cell lysates were analyzed for 35S–TNF-α by immunoprecipitation. The inhibitor prolonged the appearance of 26 kd TNF-α. These data are representative of three separate labeling experiments.
BB-3103 Enhances Plasma Membrane and Vesicular Immunoreactivity in RAW264 Cells
Several approaches were taken to determine the location of the retained 26 kd TNF-α in inhibitor-treated cells. First, biotinylation was used to detect TNF-α on the cell surface. After surface biotinylation, the labeled proteins were collected on streptavidin beads and TNF-α was immunoprecipitated from the bead eluate and from the non-biotinylated supernatant. The 26 kd TNF-α was recovered in the biotinylated and non-biotinylated fractions, which served as a crude separation of cell surface and intracellular proteins, respectively. There was significantly more biotinylated 26 kd TNF-α on the surface of inhibitor-treated cells. This is consistent with prevention of proteolytic release (Fig. 3). There was also more 26 kd TNF-α in the non-biotinylated fraction in inhibitor-treated cells, indicating that the intracellular stores were also increased by BB-3103. This result shows that BB-3103 causes an increase in cell-surface 26 kd TNF-α and causes an accumulation of 26 kd TNF-α in the intracellular pool, which was not accessible to surface biotinylation.
Surface biotinylation of TNF-α. Biotinylation was performed to detect surface (biotinylated) and intracellular (nonbiotinylated) pools of TNF-α. Adherent RAW264 cells were treated with 100 ng/ml of LPS in the presence or absence of 10 μm BB-3103. The cell surface was biotinylated, the cells were lysed, and surface biotinylated proteins were collected on streptavidin beads. Nonbiotinylated proteins in the supernatant were also sampled. Pro–TNF-α was detected in LPS and LPS plus inhibitor treated samples by immunoblotting. These data are representative of three separate experiments.
Immunofluorescence studies of TNF-α on the cell surface of activated macrophages were visualized most effectively in non-permeabilized cells. Very low levels of TNF-α were observed on the surface of most cells treated with LPS alone (Fig. 4). Distinct immunoreactivity at the cell periphery was first observed after 30 minutes of BB-3103 treatment and strong cell surface immunoreactivity was visible after 1 hour of treatment. This cell surface immunoreactivity continued for sustained times and started to have a punctate appearance after 4 hours, consistent with clustering of uncleaved TNF-α. Immunoreactivity was more sensitive than immunoprecipitation (Fig. 2) in detecting retention of uncleaved TNF-α.
Immunofluorescence of TNF-α on the surface of nonpermeabilized cells. After LPS or LPS plus inhibitor treatment for various times, RAW264 macrophages grown on coverslips were fixed with 4% paraformaldehyde and immunoreacted with a polyclonal antibody to TNF-α. Immunofluorescence of only surface-accessible TNF-α is shown at different times. Uniform (d) or punctate (f) immunoreactivity was detected after inhibitor treatment.
Intracellular TNF-α was localized in adherent, permeabilized RAW264 macrophages by immunofluorescence (Fig. 5). In unstimulated cells and in cells exposed only to the inhibitor BB-3103, faint diffuse immunoreactivity was detected. This may represent low constitutive levels of TNF-α in or on the cells (Shurety et al, 2000). After exposure to 100 ng/ml of LPS for 30 minutes to 2 hours, intense immunoreactivity of TNF-α appeared in the Golgi region. In cells treated with both LPS and BB-3103, plasma membrane immunoreactivity was also apparent, and inhibitor-treated cells had distinct cell surface immunoreactivity and a flatter appearance by 1 hour (Fig. 5d). TNF-α immunoreactivity in the Golgi persisted for approximately 2 to 4 hours in both cells treated with LPS and cells treated with LPS plus BB-3103. Additionally, numerous vesicular structures containing TNF-α appeared in cells treated with BB-3103. These labeled organelles were not present in cells treated with LPS alone and were most prominent after 2 hours of BB-3103 treatment. Plasma membrane TNF-α immunoreactivity was present on inhibitor-treated cells from 30 minutes to more than 4 hours. With either treatment, TNF-α immunoreactivity was diminished in most cells by 8 hours. Immunofluorescence confirmed the presence of TNF-α on the cell surface and showed the de novo appearance of an intracellular vesicular pool of TNF-α that was induced by BB-3103. The immunoreactivity of both unpermeabilized (Fig. 4) and permeabilized (Fig. 5) cells concurs in showing that the inhibitor BB-3103 causes an accumulation of TNF-α at the cell surface followed by clustering of TNF-α into vesicles.
Immunofluorescence of TNF-α in permeabilized cells. RAW264 cells, grown on coverslips, were treated with either 100 ng/ml of LPS or LPS plus 1 μm BB-3103 for various times. Cells were fixed with 4% paraformaldehyde, permeabilized with 0.1% Triton X-100, and immunoreacted with a polyclonal antibody to TNF-α. TNF-α was prominent in the perinuclear Golgi complex after activation with LPS for 0.5 hours (c). TNF-α immunoreactivity in the Golgi persisted for approximately 2 to 4 hours and was diminished in most cells by 8 hours. BB-3103 increased surface immunoreactivity (f, h, and j) and induced vesicular immunoreactivity at late times (h and j).
The 26 kd Form of TNF-α Travels Directly from the Golgi to the Plasma Membrane
Treatments aimed at disrupting the secretory pathway were effective in preventing TNF-α from reaching the plasma membrane in RAW264 cells treated with LPS and the inhibitor. Typically, TNF-α immunoreactivity in the Golgi was present after 30 minutes of LPS stimulation followed by a 90 minutes chase. When BB-3103 was present during the chase, TNF-α was retained on the plasma membrane and appeared in vesicles (Fig. 6). Brefeldin A (BFA) treatment induces fusion of Golgi membranes with the ER and endosomal compartments, thereby disrupting the organization of the Golgi complex and blocking protein secretion (Lippincott-Schwartz et al, 1991). When cells were chased in the presence of BFA, TNF-α immunoreactivity in the Golgi was disrupted (Fig. 6c). Furthermore, the plasma membrane and vesicular TNF-α immunoreactivity induced by BB-3103 were no longer seen, indicating that BFA treatment blocked transport of TNF-α to the cell surface (Fig. 6d).
Treatment of cells with Brefeldin A (BFA) and cell immunoreactivity. RAW264 cells were treated with 100 ng/ml of LPS for 30 minutes to accumulate TNF-α at the level of the Golgi. Cells were then further incubated for 90 minutes in the presence of control medium, causing a decrease in TNF-α immunoreactivity in some cells (a). In the presence of 1 μm BB-3103, cell surface immunoreactivity was apparent (b). BFA (5 μg/ml) caused dispersal of the Golgi immunoreactivity (c). Cell surface immunoreactivity did not appear after treatment with both BB-3103 and BFA (d).
N-ethyl malemide (NEM) is another agent that disrupts the post-Golgi trafficking of secretory proteins. NEM prevents the fusion of secretory vesicles with their target membrane by blocking NEM-dependent ATPases, including the NEM sensitive fusion protein NSF (Beckers and Balch, 1989). Using an experimental method adapted from Galli et al (1998), RAW264 cells were incubated with 1 mm NEM for 15 minutes at 4° C after 30 minutes of LPS stimulation. Cells were then incubated for 60 minutes at 37° C in the absence or presence of BB3103 to follow the fate of TNF-α. In the presence of BB-3103, TNF-α was trafficked from the Golgi to the cell surface, where it accumulated (Fig. 7). NEM prevented cell-surface immunoreactivity, consistent with a block in post-Golgi transport (Fig. 7). These treatments indicate that TNF-α is transported directly from the Golgi to the plasma membrane and suggest that vesicular immunoreactivity arising from BB-3103 treatment is a subsequent event.
Treatment of cells with N-ethyl malemide (NEM) and cell immunoreactivity. RAW264 cells were stimulated with 100 ng/ml of LPS for 30 minutes and then incubated in the absence or presence of 1 mm NEM for 15 minutes at 4° C. Cells were then incubated for 60 minutes with or without 1 μm BB-3103. Without NEM and BB-3103 treatments, cells exhibited TNF-α immunoreactivity in the Golgi region, as expected (a). In the presence of BB-3103, there was distinct labeling at the cell surface and in vesicular compartments (b). NEM treatment had no effect on Golgi immunoreactivity (c), although in the presence of both NEM and BB-3103, cell surface labeling was absent (d).
To further follow the post-Golgi trafficking of TNF-α, we examined the cells over time in the presence of cycloheximide, which blocks protein synthesis. After stimulation with LPS for 30 minutes to accumulate TNF-α in the Golgi, a bolus of TNF-α protein was followed in the presence of cycloheximide (Fig. 8). After 15 minutes of chase, Golgi immunoreactivity persisted in both control and BB-3103–treated cells. However, marked plasma membrane immunoreactivity was present in the BB-3103–treated cells (Fig. 8d; arrowhead). By 30 minutes, some of the TNF-α in the LPS-stimulated cells was still present in the Golgi complex. In inhibitor-treated cells, however, the TNF-α was mostly on the cell surface (Fig. 8f; arrowhead). Prominently labeled vesicular structures appeared in the cytoplasm between the 60 to 90 minutes chase times in BB-3103–treated cells (Fig. 8h; arrow). Thus, the bolus of TNF-α seems to move from the Golgi to the cell surface, and then to intracellular vesicles. Cell-associated TNF-α immunoreactivity was depleted from all cells by 120 minutes (see also Fig. 2b). These findings support the hypothesis that pro–TNF-α is delivered directly to the plasma membrane from the Golgi complex. When cleavage of the membrane-bound form of TNF-α is prevented in the presence of BB-3103, cell surface pro–TNF-α is then endocytosed into vesicular structures.
Tracking of TNF-α in cycloheximide-treated cells. RAW264 cells were incubated with 100 ng/ml of LPS in the absence (a) or presence (b) of 1 μm BB-3103 for 30 minutes, followed by an incubation with 0.5 mm cycloheximide for various times (0 to 120 minutes). In cells treated with LPS, TNF-α immunoreactivity in the Golgi persisted for 30 minutes (a, c, and e), and from 60 minutes, TNF-α was cleared and no cellular immunoreactivity was visible (g, i, and k). However, in BB-3103–treated cells, Golgi immunoreactivity persisted for 15 minutes (b and d), and the cell surface immunoreactivity of TNF-α was seen until 90 minutes (b, d, f, h, and j). Vesicular immunoreactivity appeared after 30 minutes (f) and remained until after 90 minutes (h and j; arrowheads). These patterns are consistent with the sequential appearance of TNF-α in the Golgi complex, cell surface, and endosomes of inhibitor-treated cells.
Uncleaved TNF-α Is Found in the Endocytic Pathway of RAW264 Cells
Internalization of uncleaved TNF-α from the cell surface was also confirmed by surface biotinylation at 4° C followed by internalization at 37° C. After one hour of LPS and BB-3103 treatment, a large pool of 26 kd TNF-α could be biotinylated at the cell surface (Fig. 9). After incubation at 37° C to allow internalization, surface biotin was stripped and the endocytosed pool was assayed. The internalized pool of 26 kd TNF-α diminished over time, because of either delivery into a degradation pathway or recycling back to the cell surface.
TNF-α (26 kd) at the cell surface is internalized. Biotinylation of adherent RAW264 cells was performed to detect surface and internalized pools of TNF-α. Cells were first treated with 100 ng/ml of LPS in the presence of 10 μm BB-3103, and cell surface proteins were biotinylated at 4° C. Biotinylated proteins were internalized by transferring the cells to 37° C for 20 and 60 minutes. Using the glutathione stripping solution, biotinylated proteins were removed from the cell surface. Cells were then lysed and all biotinylated proteins collected on streptavidin beads. Pro–TNF-α was detected in cell surface and intracellular pools by immunoblotting. These data are representative of three separate experiments.
The presence of TNF-α in the endocytic pathway of RAW264 cells was confirmed by colocalizing intracellular TNF-α with endosomal markers. Double-labeling experiments were performed with an antibody to EEA1, a protein that associates with the membrane of early endosomes (Mu et al, 1995). Newly synthesized TNF-α in cells treated for 30 minutes or 1 hour with LPS and BB-3103 did not colocalize with EEA1 (Fig. 10). However, in cells treated for 2 hours with LPS and BB-3103, TNF-α was colocalized in some of the same vesicular structures as EEA1 (Figs. 10 and 11; arrowheads). This confirms that surface 26 kd TNF-α is internalized and accumulates in early endosomes. From this location, TNF-α could either be transported to the degradative pathway or recycled to the cell surface in other nonEEA1-labeled endosomes.
Labeling of TNF-α and early endosomes. RAW264 cells grown on coverslips were treated with 100 ng/ml of LPS and 1 μm BB-3103 for 30 (a and d), 60 (b and e), or 120 minutes (c and f), fixed with paraformaldehyde, and permeabilized. Cells were double labeled with antibodies against TNF-α and the early endosome marker, EEA1, as indicated. There was separate labeling of Golgi (TNF-α) and other vesicles and of vesicular endosomes (EEA1) at 30-minute and 1-hour time points. At 2 hours, there are some endosomes where TNF-α and EEA1 are colocalized, as indicated by arrowheads.
Localization of TNF-α in early endosomes. RAW264 cells grown on coverslips were treated with 100 ng/ml of LPS and 1 μm BB-3103 for 2 hours, fixed with paraformaldehyde, and permeabilized. Cells were double labeled with antibodies against TNF-α (a) and the early endosome marker, EEA1 (b). This image shows colocalization of TNF-α in EEA1-marked early endosomes (arrowheads).
Discussion
We determined the fate of 26 kd TNF-α in activated macrophages treated with the metalloprotease inhibitor BB-3103, providing evidence that this uncleaved form of TNF-α is trafficked from the Golgi complex to the plasma membrane. This hydroxamic acid-based inhibitor was shown to block more than 95% of the production of soluble TNF-α, causing retention of the 26 kd pro–TNF-α for relatively long periods. Results of TNF-α immunoreactivity, particularly in the presence of cycloheximide, showed that the TNF-α proform does not seem to accumulate in any other cellular compartment after leaving the Golgi complex, but travels directly to the cell surface. At the cell surface, pro–TNF-α accumulates transiently and is then endocytosed back into the cell. A proportion of the internalized 26 kd protein was localized in vesicular structures, identified as early endosomes by the presence of EEA1, wherein internalized proteins are typically sorted for further trafficking into either degradative or recycling endosomes (Bucci et al, 1992; Rubino et al, 2000). Other vesicular pools of endocytosed TNF-α may represent protein further down these pathways or protein retrieved from the surface by additional pathways. This is the first direct demonstration that uncleaved TNF-α is endocytosed from the cell surface. Although we have demonstrated endocytosis of 26 kd TNF-α sustained experimentally in the presence of inhibitors, we anticipate that similar trafficking of constitutive levels of uncleaved TNF-α occur under physiologic conditions. The post-cleavage, membrane-anchor of pro–TNF-α may also be cleared from the cell surface via a similar endocytic pathway (Decoster et al, 1998; Pocsik et al, 1995).
Two recent reports show that mature TACE is found both on the cell surface and in intracellular compartments (Doedens and Black, 2000; Schlöndorff et al, 2000). This evidence suggests a scenario where TNF-α may be cleaved in intracellular compartments. In studying down-regulation of TACE, Doedens and Black (2000) demonstrated that TACE is removed from the cell surface by endocytosis, a process that is induced by phorbol esters and inhibited by the presence of hydroxamates. It is of interest to find that both TACE and TNF-α can be endocytosed and, furthermore, that hydroxamate inhibitors act to retain both proteins on the surface, promoting uptake of uncleaved TNF-α but not of TACE. A role for endocytosis in regulating TNF-α cleavage and release is further implied by the reciprocal fates of substrate and enzyme in this situation.
The significant, albeit transient, buildup of uncleaved, cell surface TNF-α shown herein by immunofluorescence and biotinylation studies is consistent with similar observations made in previous studies using FACS analysis (Glaser et al, 1999; Solomon et al, 1997). It is likely that this sustained pool of membrane pro–TNF-α is biologically active as demonstrated in other studies where uncleaved TNF-α has been shown to be competent in target cell killing (Decoster et al, 1995; Solomon et al, 1997). The quantity of 26 kd TNF-α present on the cell surface at any one time could significantly influence its paracrine and tumoricidal action and is thus likely to be regulated by the cell (Decoster et al, 1995, 1998; Kriegler et al, 1988; Perez et al, 1990). TNF-α has also been discovered in vesicles in mast cells from where it can be released upon activation (Walsh et al, 1991). Endocytosis and recycling of pro–TNF-α is a possible mechanism for modulating levels and functions of surface exposed TNF-α and of TNF-α available for cleavage. In support of this concept, we have previously shown that macrophages activated by the distinct cascades associated with either LPS and interferon-γ or LPS alone have different trafficking of TNF-α (Shurety et al, 2000). Interferon-γ induces the trafficking of some TNF-α to endosomal structures that may be used to sequester or reroute surface TNF-α to produce a different biological action. The appearance of TNF-α in endosomes in response to disparate manipulations, interferon-γ or BB-3103, further suggests that these treatments serve to upregulate a constitutive endocytosis pathway for TNF-α.
Our immunoblotting and ELISA data are consistent with studies carried out on monocyte cell-lines with the metalloprotease inhibitor GI 129471. In these studies, cell-associated pro–TNF-α was increased two-fold and secretion of the mature 17 kd form into the media was prevented (Glaser et al, 1999; McGeehan et al, 1994). Additionally, in monocytes it has been demonstrated that pro–TNF-α normally has a relatively short half-life of approximately 15 minutes, but in the presence of inhibitor its half-life in cell extracts is extended for up to one hour (Solomon et al, 1997). However, our pulse-chase and immunofluorescence studies in RAW macrophages show that pro–TNF-α has a half-life of at least 30 minutes under physiologic conditions (Shurety et al, 2000). Furthermore, in inhibitor-treated macrophages a significant pool of pro–TNF-α is retained for much longer times on the surface and in endosomes. Thus, degradation of TNF-α may occur at a slower rate in macrophages than in monocytes. Interestingly, a large cell surface buildup of pro–TNF-α with a relatively long half-life has been reported in T lymphocytes treated with the metalloprotease inhibitor TAPI (Crowe et al, 1995). Thus, there are cell type differences in the handling of pro–TNF-α that may reflect differences in the specific functions of surface TNF-α.
Careful analysis of a post-activation time course in macrophages shows that the presence of the inhibitor did not alter or block the normal post-Golgi trafficking of TNF-α to the cell surface (Shurety et al, 2000 and this study). A previous study demonstrated TNF-α immunoreactivity appearing in the Golgi complex of Mono Mac-6 cells in the presence of the inhibitor but not with LPS alone, although a time course was not shown (McGeehan et al, 1994). In this case, the inhibitor could be interpreted as causing a block in movement of pro–TNF-α out of the Golgi. In RAW cells we observe TNF-α Golgi immunoreactivity soon after activation with LPS (Shurety et al, 2000) and have now shown that the inhibitor does not increase TNF-α immunoreactivity in the Golgi. It has also been proposed that unprocessed pro–TNF-α is not sorted to another cell compartment but is rapidly moved from the Golgi complex and directed to lysosomes for degradation in inhibitor-treated monocytes (Solomon et al, 1997). Although some molecules are trafficked from the trans-Golgi network to late endosomes or lysosomes (Deng et al, 1996; reviewed in Le Borgne and Hoflack, 1998), our data now shows clearly that, for uncleaved TNF-α, access to the endosomal system occurs via the cell surface. Biochemical and cell immunofluorescence results taken together suggest that TNF-α is trafficked to and accumulated on the cell surface in its 26 kd form.
We conclude that a direct pathway exists for the transfer of TNF-α from the Golgi to the plasma membrane of macrophages. Excess TNF-α is then internalized and is processed through compartments of the endocytic pathway including early endosomes. Although the majority of uncleaved TNF-α stored in these compartments may be targeted for degradation over time, it is important to elucidate whether endocytosed, biologically active TNF-α also recycles to replenish the cell surface. Endocytosis may also be a route for redirecting surface TNF-α to other intracellular sites, such as the mitochondria (Ledgerwood et al, 1998), or to trigger transcriptional regulation in an autocrine manner. The ability to prevent the secretion of the mature 17 kd TNF-α and to prolong the appearance and half-life of the 26 kd form in macrophages could have important clinical implications for metalloprotease inhibitors as potential therapeutics. Previous findings have demonstrated metalloprotease inhibitors prevent hepatic injury in endotoxemic mice (Murakami et al, 1998) and protected mice from a lethal dose of endotoxin by inhibiting TNF-α release (Mohler et al, 1994). Thus, in addition to controlling the release of mature TNF-α, metalloprotease inhibitors could regulate paracrine and autocrine responses by modifying the presence of biologically active pro–TNF-α in and on various cell-types for longer times. Several therapeutic strategies designed to combat excess secretion of TNF have been tried in the treatment of sepsis, rheumatoid arthritis, and congestive heart disease. Most of these strategies focus on mopping up secreted TNF-α with humanized TNF antibodies or other binding proteins (Eigler et al, 1997). By characterizing the intracellular trafficking of membrane-associated TNF-α, our study provides the basis for alternative strategies aimed at selectively controlling the trafficking and cell surface exposure of TNF-α.
Materials and Methods
Antibodies and Reagents
Unless otherwise stated, all chemicals used were obtained from Sigma Chemical Company (Castle Hill, Australia). The rabbit anti-mouse TNF-α polyclonal serum was purchased from Genzyme (Cambridge, Massachusetts) and the antibody to the early endosome marker EEA1, was purchased from Transduction Laboratories (Lexington, Kentucky). The metalloprotease inhibitor BB-3101 was kindly provided by British Biotech Pharmaceuticals (Oxford, United Kingdom).
Cell Culture
RAW264 murine macrophages were grown in RPMI 1640 medium (BioWhittaker, Walkersville, Maryland) supplemented with 10% heat-inactivated (56° C, 30 minutes) serum supreme (BioWhittaker) and 1% L-glutamine (GIBCO, Grand Island, New York). Cells were stimulated with 100 ng/ml of LPS (from Salmonella minnesota Re 595; Sigma Chemical Company) in the presence or absence of BB-3103.
Immunofluorescence
RAW264 cells, plated at a low density, were grown for 2 days on coverslips. Cells were fixed in 4% paraformaldehyde then permeabilized for 5 minutes in PBS containing 0.1% Triton X-100. Fixed cells were incubated with primary antibodies followed by FITC- or Cy3-conjugated secondary antibodies using BSA in blocking/washing buffers. Coverslips were mounted on glass slides in a solution of 50% glycerol and 1% n-propyl gallate in PBS and examined using an Olympus AX70 microscope fitted for epifluorescence. Digital images were collected on a Dage 300ET-RC 0.5” cooled CCD camera with a SCION LG-3 frame-grabbing card using NIH-image software.
Pulse-Chase Labeling and Immunoprecipitation
RAW264 cells grown to 90% confluence in 6 cm plates were washed in cysteine/methionine free (cys−/met−) medium containing 1% L-glutamine. Cells were then incubated with 1.5 ml of labeling medium consisting of cys−/met− medium, ± 100 ng/ml of LPS, 5% serum supreme, and 0.5 mCi/ml of 35S-Translabel (ICN Pharmaceuticals Inc., Costa Mesa, California; specific activity: 43.48 TBq/mmol) for 15 minutes at 37° C. Cells were either washed in PBS then lysed with RIPA buffer (1% Triton X-100, 1% deoxycholate, 0.1% SDS, 0.15 M NaCl, and 25 mm Tris-HCl pH 7.4) containing Complete protease inhibitors (Boehringer Mannheim, Mannheim, Germany) or were washed then chased for various times at 37° C in culture medium in the presence or absence of 1 μm BB-3103. The medium was collected before the cells were lysed in RIPA buffer. RIPA extracts of cells or aliquots of culture medium were incubated with TNF-α antibody and incubated with protein A beads (Pierce Chemical Company, Rockford, Illinois). Beads were pelleted and washed five times in RIPA buffer and then boiled in SDS-PAGE sample buffer. Proteins were separated using SDS-PAGE. Gels were fluored with sodium salicylate, dried, and exposed to X-ray film.
SDS-PAGE and Immunoblotting
Cell lysates to be analyzed were separated by SDS-PAGE on 15% Laemmli denaturing gels under reducing conditions. For immunodetection, the proteins were transferred onto polyvinylidene difluoride Immobilon P membrane (Millipore, Bedford, Massachusetts) and stained in 0.1% Coomassie blue (in 50% methanol and 10% acetic acid) to check protein loading. Membranes were blocked and washed in Blotto (20 mm Tris-HCl buffer pH 7.5, containing 0.15 M NaCl, 0.1% Triton X-100, and 5% nonfat milk) and incubated with primary antibody for 2 hours. Bound specific antibody was detected by incubation using a horseradish peroxidase-conjugated secondary antibody (Sigma Chemical Company) and ECL Western blotting detection reagent (Amersham International, Buckinghamshire, United Kingdom).
Cell Surface Biotinylation and Endocytosis Assay
The following procedures were adapted from Le et al (1999). RAW264 cells grown on tissue culture plates were incubated with either 100 ng/ml of LPS or LPS plus 10 μm BB-3103 for 2 hours, then incubated with 1.5 mg/ml of sulfosuccinimidyl 2-(biotinamido) ethyl-dithioproprionate (sulfo-NHS-SS-biotin; Pierce Chemical Company) at 4° C for 1 hour, and washed with 50 mm NH4Cl in PBS to quench any free sulfo-NHS-SS-biotin. This was followed by several further washes with PBS. To measure cell surface biotinylated proteins, cells were then lysed in 1 ml of RIPA buffer (20 mm Tris-HCl pH 7.4, with 150 mm NaCl, 0.1% SDS, 1% Triton X-100, 1% deoxycholate, 5 mm EDTA) containing protease inhibitors. To measure internalized biotinylated proteins, PBS was replaced with complete RPMI medium at 37° C for 20 and 60 minutes. Cells were incubated in two 20-minute washes of glutathione stripping solution (60 mm glutathione and 0.83 mm NaCl, with 0.83 mm NaOH and 1% BSA added before use) at 4° C, which removed all cell surface biotin groups. Remaining biotinylated proteins were sequestered inside cells by endocytosis and were therefore protected from glutathione stripping. Cell extracts were centrifuged to remove cell debris and obtain a detergent soluble supernatant, which was incubated with streptavidin beads (Sigma Chemical Company) to collect bound, biotinylated proteins. These samples were then analyzed by SDS-PAGE and immunoblotting to identify TNF-α.
ELISA
RAW264 cells were grown for 2 days on 12 well plates (to approximately 90% confluence). TNF-α concentration in the culture medium was determined by ELISA using the Quantikine M ELISA kit for TNF-α (R and D Systems, Minneapolis, Minnesota), according to the manufacturer's instructions. Samples were measured in triplicate.
References
Aggarwal BB and Natarajan K (1996). Tumor necrosis factors: Development during the last decade. Eur Cytokine Netw 7: 93–124.
Ancuta P, Fahmi H, Pons JF, Le Blay K, and Chaby R (1997). Involvement of the membrane form of tumour necrosis factor-alpha in lipopolysaccharide-induced priming of mouse peritoneal macrophages for enhanced nitric oxide response to lipopolysaccharide. Immunology 92: 259–266.
Beckers CJM and Balch WE (1989). Calcium and GTP: Essential components in vesicular trafficking between the endoplasmic reticulum and Golgi apparatus. J Cell Biol 108: 1245–1256.
Beutler BA (1999). The role of tumour necrosis factor in health and disease. J Rheumatol 26: 16–21.
Black RA, Rauch CT, Kozlosky CJ, Peschon JJ, Slack JL, Wolfson MF, Castner BJ, Stocking KL, Reddy P, Srinivasan S, Nelson N, Boiani N, Schooley KA, Gerhart M, Davis R, Fitzner JN, Johnson RS, Paxton RJ, March CJ, and Cerretti DP (1997). A metalloprotease disintegrin that releases tumour-necrosis factor-α from cells. Nature 385: 729–733.
Bucci C, Parton RG, Mather IH, Stunnenberg H, Simons K, Hoflack B, and Zerial M (1992). The small GTPase rab5 functions as a regulatory factor in the early endocytic pathway. Cell 70: 715–728.
Chang S, Stacey KJ, Costelloe EO, Aderem A, and Hume DA (1999). Mechanisms of regulation of the MacMarcks gene in macrophages. J Leukoc Biol 66: 528–534.
Crowe PD, Walter BN, Mohler KM, Otten-Evans C, Black RA, and Ware CF (1995). A metalloprotease inhibitor blocks shedding of the 80-kD TNF receptor and TNF processing in T lymphocytes. J Exp Med 181: 1205–1210.
Darville T, Tabor D, Simpson K, and Jacobs RF (1994). Intravenous immunoglobulin modulates human mononuclear phagocyte tumor necrosis factor-alpha production in vitro. Pediatr Res 35: 397–403.
Decoster E, Vanhaesebroeck B, Boone E, Plaisance S, De Vos K, Haegeman G, Grooten J, and Fiers W (1998). Induction of unresponsiveness to tumor necrosis factor (TNF) after autocrine TNF expression requires TNF membrane retention. J Biol Chem 273: 3271–3277.
Decoster E, Vanhaesebroeck B, Vandenbeele P, Grooten G, and Fiers W (1995). Generation and biological characterization of membrane-bound, uncleavable murine tumor necrosis factor. 270: 18473–18478.
Deng J, Rudick V, and Dory L (1996). Lysosomal degradation and sorting of apolipoprotein E in macrophages. J Lipid Res 36: 2129–2140.
Doedens JR and Black RA (2000). Stimulation-induced down-regulation of tumor necrosis factor-α converting enzyme. J Biol Chem 275: 14598–14607.
Eigler A, Sinha B, Hartmann G, and Endres S (1997). Taming TNF: Strategies to restrain this proinflammatory cytokine. Immunol Today 18: 487–492.
Fiers W (1991). Tumor necrosis factor: Characterization at the molecular, cellular and in vivo level. FEBS Lett 285: 199–212.
Galli T, Zahraoui A, Vaidyanathan VV, Raposo G, Tian JM, Karin M, Niemann H, and Louvard D (1998). A novel tetanus neurotoxin-insensitive vesicle-associated membrane protein in SNARE complexes of the apical plasma membrane of epithelial cells. Mol Biol Cell 9: 1437–1448.
Gearing AJ, Beckett P, Christodoulou M, Churchill M, Clements J, Davidson AH, Drummond AH, Galloway WA, Gilbert R, Gordon JL, Leber TM, Mangan M, Miller K, Nayee P, Owen K, Patel S, Thomas W, Wells G, Wood LM, and Woolley K (1994). Processing of tumour necrosis factor-alpha precursor by metalloproteases. Nature 370: 555–557.
Glaser KB, Pease L, Li J, and Morgan DW (1999). Enhancement of the surface expression of tumor necrosis factor α (TNFα) but not the p55 TNFα receptor in the THP-1 monocytic cell line by matrix metalloprotease inhibitors. Biochem Pharmacol 57: 291–302.
Jue D-M, Sherry B, Luedke C, Manogue KR, and Cerami A (1990). Processing of newly synthesized cachectin/tumor necrosis factor in endotoxin-stimulated macrophages. Biochemistry 29: 8371–8377.
Kim K-U, Kwon O-J, and Jue D-M (1993). Pro-tumour necrosis factor cleavage enzyme in macrophage membrane/particulate. Immunol 80: 134–139.
Kinkhabwala M, Sehajpal P, Scolnik E, Smith D, Shrma K, Vlassara H, Cerami A, and Suthanthiran M (1990). A novel addition to the T cell repertory: Cell surface expression of tumor necrosis factor/cachectin by activated normal human T cells. J Exp Med 171: 941–946.
Kol A, Sukhova GK, Lichtman AH, and Libby P (1998). Chlamydial heat shock protein 60 localizes in human atheroma and regulates macrophage tumor necrosis factor-alpha and matrix metalloproteinase expression. Circulation 98: 300–307.
Kriegler M, Perez C, DeFay K, Albert I, and Lu SD (1988). A novel form of TNF-α/cachectin is a cell surface cytotoxic transmembrane protein: Ramification for the complex physiology of TNF-α. Cell 53: 45–53.
Le TL, Yap AS, and Stow JL (1999). Recycling of E-cadherin: A potential mechanism for regulating cadherin dynamics. J Cell Biol 146: 219–232.
Le Borgne R and Hoflack B (1998). Protein transport from the secretory to the endocytic pathway in mammalian cells. Biochim Biophys Acta 1404: 195–209.
Ledgerwood EC, Prins JB, Bright NA, Johnson DR, Wolfreys K, Pober JS, O'Rahilly S, and Bradley JR (1998). Tumor necrosis factor is delivered to mitochondria where a tumor necrosis factor-binding protein is localized. Lab Invest 78: 1583–1589.
Lippincott-Schwartz J, Yuan L, Tipper C, Amherdt M, Orci L, and Klausner RD (1991). Brefeldin A's effects on endosomes, lysosomes, and the TGN suggest a general mechanism for regulating organelle structure and membrane traffic. Cell 67: 601–616.
McGeehan GD, Becherer JD, Bast RJ, Boyer CM, Champion B, Connolly KM, Conway JG, Furdon P, Karp S, Kidao S, McElroy AB, Nichols J, Pryzwansky KM, Schoenen F, Sekut L, Truesdale A, Verghese M, Warner J, and Ways JP (1994). Regulation of tumour necrosis factor-alpha processing by a metalloprotease inhibitor. Nature 370: 558–561.
Mitsiades N, Poulaki V, Leone A, and Tsokos M (1999). Fas-mediated apoptosis in Ewing's sarcoma cell lines by metalloproteinase inhibitors. J Natl Cancer Inst 91: 1678–1684.
Mohler KM, Sleath PR, Fitzner JN, Cerretti DP, Alderson M, Kerwar SS, Torrance DS, Otten EC, Greenstreet T, Weerawarna K, Kronheim SR, Petersen M, Gerhart M, Kozlosky CJ, March CJ, and Black RA (1994). Protection against a lethal dose of endotoxin by an inhibitor of tumour necrosis factor processing. Nature 370: 218–220.
Moss ML, Catherine Jin S-L, Milla ME, Burkhart W, Carter HL, Chen W-J, Clay WC, Didsbury JR, Hassler D, Hoffman CR, Kost TA, Lambert MH, Leesnitzer MA, McCauley P, McGeehan G, Mitchell J, Moyer M, Pahel G, Rocque W, Overton LK, Schoenen F, Seaton T, Su J-L, Warner J, Willard D, and Becherer JD (1997). Cloning of a disintegrin metalloprotease that processes precursor tumour-necrosis factor-α. Nature 385: 733–736.
Mu FT, Callaghan JM, Steele-Mortimer O, Stenmark H, Parton R, Campbell PL, McCluskey J, Yeo JP, Tock EP, and Toh BH (1995). EEA1, an early endosome-associated protein. EEA1 is a conserved alpha-helical peripheral membrane protein flanked by cysteine “fingers” and contains a calmodulin-binding IQ motif. J Biol Chem 270: 13503–13511.
Murakami K, Kobayashi F, Ikegawa R, Koyama M, Shintani N, Yoshida T, Nakamura N, and Kondo T (1998). Metalloproteinase inhibitor prevents hepatic injury in endotexemic mice. Eur J Pharmacol 341: 105–110.
Perez C, Albert I, DeFay K, Zachariades N, Gooding L, and Kriegler M (1990). A nonsecretable cell surface mutant of tumor necrosis factor (TNF) kills by cell-cell contact. Cell 63: 251–258.
Peschon JJ, Slack JL, Reddy P, Stocking KL, Sunnarborg SW, Lee DC, Russell WE, Castner BJ, Johnson RS, Fitzner JN, Boyce RW, Nelson N, Kozlosky CJ, Wolfson MF, Rauch CT, Cerretti DP, Paxton RJ, March CJ, and Black RA (1998). An essential role for ectodomain shedding in mammalian development. Science 282: 1281–1284.
Pocsik E, Duda E, and Wallach D (1995). Phosphorylation of the 26 kDa TNF precursor in monocytic cells and in transfected HeLa cells. J Inflamm 45: 152–159.
Rubino M, Miaczynska M, Lippe R, and Zerial M (2000). Selective membrane recruitment of EEA1 suggests a role in directional transport of clathrin-coated vesicles to early endosomes. J Biol Chem 275: 3745–3748.
Schlöndorff J, Becherer JD, and Blobel CP (2000). Intracellular maturation and localization of the tumour necrosis factor α convertase (TACE). Biochem J 347: 131–138.
Sewter CP, Digby JE, Blows F, Prins JB, and O'Rahilly S (1999). Regulation of tumor necrosis factor-alpha release from human adipose tissue in vitro. J Endocrinol 163: 33–38.
Shurety W, Merino-Trigo A, Brown D, Hume DA, and Stow JL (2000). Localization and post-Golgi trafficking of TNF-α in macrophages. J Interferon Cytokine Res 20: 427–438.
Solomon KA, Covington MB, DeCicco CP, and Newton RC (1997). The fate of pro–TNF-α following inhibition of metalloprotease-dependent processing to soluble TNF-α in human monocytes. J Immunol 159: 4524–4531.
Tracey KJ (1991). Tumour necrosis factor (cachectin) in the biology of septic shock syndrome. Circ Shock 35: 123–128.
Vassalli P (1996). The tumour necrosis factor ligand and receptor families. N Engl J Med 334: 1717–1725.
Walsh LJ, Trinchieri G, Waldorf HA, Whittaker D, and Murphy GF (1991). Human dermal mast cells contain and release tumor necrosis factor α which induces leucocyte adhesion molecule-1. Proc Natl Acad Sci USA 86: 4220–4224.
Watanabe N, Nakadas K, and Kobayashi Y (1998). Processing and release of tumor necrosis factor α. Eur J Biochem 253: 576–582.
Acknowledgements
We thank Tatiana Khromykh and Juliana Venturato for their excellent technical assistance and Tam Luan Le for help with the biotinylation assays.
Author information
Authors and Affiliations
Corresponding author
Additional information
This work was supported by grants from the National Health and Medical Research Council to JLS and from the Diabetes Australia Research Trust to JBP. JLS and JBP are both Wellcome Trust Senior Research Fellows. The Institute for Molecular Bioscience is a special research center of the Australian Research Council.
Rights and permissions
About this article
Cite this article
Shurety, W., Pagan, J., Prins, J. et al. Endocytosis of Uncleaved Tumor Necrosis Factor-α in Macrophages. Lab Invest 81, 107–117 (2001). https://doi.org/10.1038/labinvest.3780216
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1038/labinvest.3780216