Abstract
To understand the role of the proinflammatory cytokine interleukin-1 (IL-1) in mycobacterial inflammation, IL-1 α/β double-knockout (KO) mice were produced. These mice were infected with either Mycobacterium tuberculosis H37Rv by the airborne route using an airborne infection apparatus, and their capacities to control mycobacterial growth, granuloma formation, cytokine, and nitric oxide (NO) production were examined. The IL-1 α/β mice developed significantly larger (p < 0.01) granulomatous, but not necrotic, lesions in their lungs than wild-type (WT) mice after infection with H37Rv. Inflammatory lesions, but not granulomas, were observed in spleen and liver tissues from both IL-1 α/β KO and wild-type mice. Granulomatous lesion development in IL-1 α/β KO mice was not significantly inhibited by treatment with exogenous recombinant IL-1α/β. Compared with wild-type mice, splenic IFN-γ and IL-12 levels were within the normal range. NO production by cultured alveolar macrophages from IL-1 α/β KO mice was lower than in wild-type mice but were increased by the addition of recombinant IL-1 α/β. Our data clearly indicate that IL-1 is important for the generation of early-phase protective immunity against mycobacterial infection.
Similar content being viewed by others
Introduction
Interleukin (IL)-1 (IL-1α and IL-1β) is the prototypic multifunctional cytokine. Unlike lymphocyte and colony-stimulating factors, IL-1 affects nearly all cell types. Wide variety of biologic effects of IL-1 have been reported to date (Dinarello, 1996; Durum and Oppenheim, 1993; Zheng et al, 1995), and these include induction of fever, hypotension, neutrophilia, hyperlipidemia, and hypoferremia, among others. The changes in immunologic responses produced by IL-1 are interesting: IL-1 increases antibody production and lymphokine synthesis, up-regulates IL-2 receptors, and enhances spleen cell mitogenic responses to bacterial lipopolysaccharides (LPS). Its inflammatory effects are well known and include proliferation of fibroblasts, smooth muscle cells, and mesangial cells (Lonnemann et al, 1995), increased HIV-1 expression, neutrophil and albumin influx into the lungs after intratracheal instillation, increased nonspecific resistance to infection (pretreatment), and increased hepatic acute-phase protein synthesis (refer to Dinarello, 1996 for review).
We are currently studying the mechanisms underlying Mycobacterium tuberculosis-induced granuloma formation at the molecular level. We have previously found that granulomas are induced in mice with a disrupted interferon (IFN)-γ gene by avirulent forms of Mycobacterium, but not by virulent strains of M. tuberculosis (Sugawara et al, 1998). IFN-γ may be primarily responsible for macrophage activation in murine experimental tuberculosis (Cooper et al, 1993; Dalton et al, 1993; Flynn et al, 1993; Sugawara et al, 1998). Using tumor necrosis factor (TNF-α) gene-knockout mice, we and other researchers have also shown that TNF-α plays an important role in protective immunity against virulent mycobacteria (Bean et al, 1999; Kaneko et al, 1999). Very recently, it has been shown that IL-18 (IFN-γ inducing factor) is important for the generation of protective immunity against mycobacteria, and that its main function is the induction of IFN-γ expression (Sugawara et al, 1999). Many cytokines other than IFN-γ, TNF-α, IL-18, and IL-12 may be involved in the development of protective immunity against infectious diseases, including mycobacterial infection.
IL-1 is a major mediator of inflammation and exerts pleiotropic effects on the neuro-immuno-endocrine system. Various pathophysiological roles of IL-1 have been described, including involvement in inflammation, acute-phase responses, host defense against bacterial and viral infection, activation of the immune system (including thymocyte maturation (Zuniga-Pflücker et al, 1995) and T helper 2 cell proliferation), bone metabolism (including osteoclast activation and secretion of metalloproteases), the development of fever, and effects on the hypothalamic-pituitary-adrenal axis (Dinarello, 1996; Durum and Oppenheim, 1993). The physiological role of IL-1 in acute and chronic inflammation is, however, still unclear. Thus, it is very important to clarify the physiologic role of IL-1 in the development of protective immunity. We therefore produced IL-1 α/β doubly deficient knockout (KO) mice (Horai et al, 1998). Using these KO mice, we studied the effects of IL-1 in M. tuberculosis-induced experimental tuberculosis.
Results
Effective Control of Bacterial Replication by IL-1
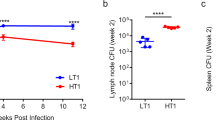
IL-1 α/β KO and wild-type (WT) littermates were infected by the airborne route (105 to 106 CFU) with the virulent H37Rv strain. All of the IL-1 α/β KO and WT mice survived until the date of sacrifice (up to 100 days after infection). First, we measured the weights of the spleens, lungs, and livers of groups of IL-1 KO and WT mice sacrificed at weekly intervals for organ colony forming unit (CFU) assay. As shown in Figure 1, the lungs of the IL-1 KO mice became heavier 5 weeks postinfection and there was a significant difference in lung weight between the KO and WT mice (p < 0.01). However, there were no significant differences in the weights of the livers and spleens between the WT and IL-1 α/β KO mice. The number of mycobacterial colonies in the lungs increased from 3 weeks postinfection onward, and there was a significant difference in lung CFU counts at 7 weeks postinfection between the IL-1 KO and WT mice (Fig. 2, p < 0.01). No colonies were found in the spleens of the IL-1 KO and WT mice for the first 2 weeks and subsequently there was no significant difference in spleen CFU counts between the IL-1 KO and WT mice.
Histologic Features of Infections
When 106 CFU of the H37Rv strain was given to the IL-1 α/β KO mice by the airborne route, larger granulomas were developed in the lungs of IL-1 KO mice than in those of the WT controls (Fig. 3). No Langhans-like giant cells were found in the granulomatous lesions. The average diameter of 10 granulomas in the lungs of IL-1 KO mice was 1412 + 132 μm, whereas that in WT mice was 403 + 29 μm (Table 1). This difference was significant (p < 0.01). No necrotic lesions were present in these granulomas. When exogenous recombinant IL-1 was administered to the IL-1 KO mice infected with H37Rv subcutaneously, the sizes of the granulomatous lesions were not reduced significantly (mean diameter, 1295 + 13 μm) and the difference between the treated and untreated group was not significant (p < 0.01) (Fig. 3D). IL-1 treatment did not reduce the mycobacterial burden significantly as assessed by spleen tissue CFU assay (data not shown).
Histologic examination of lung tissues. The KO and WT mice were sacrificed 7 weeks after infection, and formalin-fixed sections were stained with hematoxylin and eosin (A, C, and D) and for acid-fast bacilli (B). A, Lung tissue from IL-1 KO mouse infected with H37Rv strain. A large granuloma with several foamy macrophages is noted. Magnification, ×100. B, Lung tissue from IL-1 KO mouse infected with H37Rv strain. Mycobacteria stain red and are recognized in the granuloma by Ziehl-Neelsen staining. Magnification, ×600. C, Lung tissue from WT mouse infected with H37Rv strain. A small, discrete granuloma is formed. Magnification, ×100. D, Lung tissue from IL-1 KO mice infected with H37Rv strain and treated four times subcutaneously with recombinant IL-1α/β (5×104 units each time). The granulomatous scar is recognized. Magnification, ×100. E, Lung tissue without vehicle. The typical granulomatous lesion is recognized. Magnification, ×100.
Using electron microscope, the epithelioid macrophages in the granulomas of the IL-1 KO mice showed less incorporation of H37Rv into phagosomes. No ultrastructural changes resulting from the uptake of M. tuberculosis were apparent in epithelioid macrophages from either KO or WT mice (Fig. 4). Neutrophil infiltration was not found in the granulomatous lesion.
Electron micrographs of lung tissue infected with H37Rv strain, obtained at necropsy (7 weeks after infection). A, Epithelioid macrophage in the lung from a IL-1 KO mouse. Phagosomes incorporating tubercle bacilli are not prominent. Original magnification, ×6,500. B, Epithelioid macrophage in the lung from WT mouse infected with H37Rv strain. Also, note many phagosomes ingesting tubercle bacilli. Original magnification, ×6,500.
Reverse Transcription Polymerase Chain Reaction
To examine the major cytokine mRNA expression profiles of IL-1 KO mice infected with H37Rv, we examined mRNA expression levels of IFN-γ, TNF-α, IL-12 p40, iNOS, IL-4, and IL-10 in their lungs by reverse transcription polymerase chain reaction (RT-PCR). The expression levels of these cytokine mRNAs increased with the progression of infection, except for those of IL-4 and IL-10, and there were no significant differences between IL-1 KO and WT mice (Figure 5). IL-4 and IL-10 mRNAs were expressed to a mild degree in the lungs of IL-1 KO mice.
Secretion of Monokines
We also examined the monokine secretion capacities of alveolar macrophages from IL-1 KO mice after in vitro stimulation with either LPS or BCG because alveolar macrophages are targets of mycobacterial infection. As shown in Table 2, the alveolar macrophages secreted TNF-α in response to both BCG and LPS. However, after stimulation with BCG, the alveolar macrophages of IL-1 KO mice secreted TNF-α to a significantly greater extent than those of WT mice. Alveolar macrophages from IL-1 KO mice secreted less IL-12 than those from WT mice after stimulation with either BCG or LPS.
NO Production
NO levels in the supernatants of alveolar macrophage cultures were determined using the Griess reagent and reference to a standard NaNO2 curve. The levels of NO produced by unstimulated alveolar macrophages from both WT and IL-1 KO mice were low. However, when the alveolar macrophages were stimulated overnight with H37Rv (103 CFU/well), NO levels increased to 43 μm (KO mice) and 51 μm (WT control). When 1,000 units recombinant IL-1 α/β were added to the cultures of alveolar macrophages from KO mice, NO production increased to a moderate degree (50 μm) (Fig. 6). Addition of recombinant IFN-γ did not promote NO secretion activity by H37Rv-stimulated alveolar macrophages of IL-1 KO mice.
Discussion
In the present study, we found that large granulomas lacking a central necrotic area were induced by infecting IL-1α/β deficient mice with a virulent M. tuberculosis strain. Although mice deficient in IL-1β, IL-1 receptor antagonist, or IL-1 receptor I have been generated previously (Fantuzzi and Dinarello, 1996; Labow et al, 1997; Schormick et al, 1996; Zheng et al, 1995), IL-1α and IL-1 α/β double-KO mice have not been available until now, and were produced for the first time by one of the present authors (Horai et al, 1998). It has previously been shown that inflammatory responses and cytokine synthesis are defective in IL-1β KO mice, and that these KO mice become resistant to the induction of fever. Their acute-phase response is also impaired (Dinarello, 1996). However, the role of IL-1 in chronic specific inflammation remains unclear. It is, therefore, interesting that IL-1 played a protective role during the development of chronic inflammation in our experimental model.
IL-1 has been reported to induce fibroblast proliferation (Lonnemann et al, 1995). Therefore, we speculated that IL-1 would play an important role in granuloma formation. Our data clearly show that the granulomas formed in the present study were surrounded by proliferating fibroblasts. Collagen deposition was demonstrated in these granulomas by collagen staining (Masson Trichrome stain). Thus, other unknown cytokine(s) may be involved in the mechanism underlying granuloma formation.
Necrotic lesions are induced to a marked extent in IFN-γ, TNF-α, and IL-12 KO mice (Cooper et al, 1993; 1997; Flynn et al, 1993; Kaneko et al, 1999; Sugawara et al, 1998). However, necrotic lesions were not induced in our IL-1 α/β double KO mice. We examined IFN-γ, TNF-α, and IL-12 mRNA levels in the infected lung tissues of the IL-1 α/β KO mice, and strong expression was noted. This explains the development of granulomas without central necrosis. The fact that granulomatous lesions were induced in IL-1 KO mice with high-level IL-12, TNF-α and IFN-γ mRNA expression reveals that IL-1 is also important in generating protective immunity against mycobacterial infection.
Multinucleated giant cells have been recognized in granulomas of IFN-γ KO mice, but not in TNF-α or IL-18 KO mice (Bean et al, 1999; Kaneko et al, 1999; Sugawara et al, 1998; 1999). IFN-γ may be involved in macrophage fusion and the recruitment of epithelioid macrophages to form multinucleated giant cells (Sugawara et al, 1998). Because no multinucleated giant cells were found in our IL-1 KO mice, this effect may be specific to IFN-γ.
Our data also show that activated alveolar macrophages from IL-1 KO mice produce IL-12 and TNF-α, despite the lack of IL-1 secretion. TNF-α may increase compensatorily in IL-1 KO mice. Further study will be required to elucidate this. IL-1 has been reported to increase the synthesis of various lymphokines, including IL-1, IL-2, IL-3, IL-4, IL-5, IL-6, IL-7, IL-10, and IL-12 (Dinarello, 1996). It has also been reported to induce increased expression of IL-1 receptor antagonist, TNF, GM-CSF, TGF-β3, G-CSF and M-CSF, IL-8, and macrophage inflammatory protein-1α (Dinarello, 1996). In our IL-1 KO mice, IL-4 and IL10 mRNA expression was low, but IL-12 and TNF mRNA were expressed to a significantly higher extent. Thus, there may be a yet unknown mechanism that maintains IL-12 and TNF mRNA expression within the normal range in IL-1 KO mice.
NO production was impaired to a mild degree in our IL-1 KO mice. Addition of exogenous recombinant IL-1 did not restore NO production fully, suggesting possible dysfunction of the IL-1 receptor. In contrast, the iNOS system is regulated normally in IL-1 KO mice, because iNOS mRNA is expressed to a significant extent in the lung tissues of these mice.
Subcutaneous injection of IL-1 α/β failed to cure the granulomatous lesions in the IL-1 KO mice completely. These mice are regarded as a form of hereditary IL-1 deficiency because the IL-1 gene was disrupted, which might be difficult to treat effectively with recombinant IL-1 α/β alone. We have experienced a similar situation with IFN-γ α and TNF-α KO mice (Kaneko et al, 1999; Sugawara et al, 1998). However, we recently reported that treatment with exogenous IL-18 reduced the mycobacterial load significantly in IL-18 KO mice, suggesting that IL-18 plays an important role in the immune response against M. tuberculosis (Sugawara et al, 1999). The total dose of IL-1 injected during the present study may have been too low. Alternatively, combination therapy consisting of different cytokines may be required to cure the granulomatous lesions completely.
Materials and Methods
Mice
IL-1α and IL-1β genomic clones were isolated from mouse 129 genomic phage libraries. For the IL-1α targeting vector, a 1.5 kb DNA fragment lying between the Sau3AI and KpnI sites in exon 5 and intron 5, including the NH2 terminal coding region for mature IL-1α, was deleted, and a lacZ-pA-PGK-hpn-pA cassette was inserted in its place. For the IL-1β targeting vector, a 2.45 kb DNA fragment situated between the HincII and BstXI sites in exons 3 and 5 including the NH2 terminal coding region for mature IL-1β, was deleted, and a lacZ-pA-PGK-neo-pA cassette was inserted in its place (Horai et al, 1998). ES cells were electrophorated with 20–25 μg of the linearized IL-1α and IL-1β targeting vectors per 107 cells, as described previously (Asano et al, 1997). Mice heterozygous for the resulting IL-1α and IL-1β mutations were intercrossed to yield mice homozygous for the mutation. All of the KO mice were fertile, and the pups were born healthy. After birth, the IL-1α/β KO mice developed normally. They were kept under specific pathogen-free conditions in an environmentally controlled clean room at the Laboratory Animal Research Center, Institute of Medical Science, University of Tokyo. All experiments were carried out according to institutional ethical guidelines for animal experiments and safety guidelines for gene manipulation experiments.
Experimental Infections
The virulent H37Rv strain (ATCC 25618) of M. tuberculosis was grown in Middlebrook 7H9 medium (Difco) to the mid-log phase (Sugawara et al, 1998). The cultures were filtered through a 4-μm pore-size membrane filter (Millipore) before use so that they were dispersed evenly. Mice (both IL-1α/β KO and control wild-type mice) were infected by the airborne route by placing them in the exposure chamber of a Middlebrook airborne infection apparatus (Model 099CA4212; Glas-Col, Inc., Terre Haute, Indiana) (Cooper et al, 1993). The nebulizer compartment was filled with 5 ml of a suspension of 105–6 colony-forming unit (CFU) of H37Rv, a concentration calculated to result in uptake of ca. 200–500 viable bacilli by the lungs just after inhalation exposure for 75 minutes under the experimental conditions for this study (Sugawara et al, 1999). The infected mice were divided into groups of five animals, and the survival of each group was recorded for 100 days after infection with M. tuberculosis.
Survival curves were plotted. The lungs and spleens from the infected IL-1α/β knockout and WT mice were retrieved on Day 0, or 1, 2, 3, 4, 5, 6 and 7 weeks after infection, homogenized, diluted with physiological saline, plated on Ogawa slant agar, and incubated at 37° C for 21 days. The resulting CFU were counted.
Histopathology
Some IL-1 α/β KO and WT mice were sacrificed 7 weeks after infection, while others were monitored for up to 100 days postinfection. For light microscopy, tissue sections (5 μm thick) cut from paraffin blocks containing lung, liver, and spleen tissues were stained with hematoxylin and eosin or by the Ziehl-Neelsen method for acid-fast bacilli. We prepared sections from every lung tissue sample with white nodular lesions. The sizes of 10 granulomas per group consisting of five mice were measured with a micrometer (Nikon Optical Company, Tokyo, Japan) (Sugawara et al, 1999). For electron microscopy, the fresh lung tissues were cut into pieces, fixed with 2.5% glutaraldehyde, postfixed with 1% osmium tetroxide, and embedded in Epon 815 resin. (Nakamura et al, 1990).
Cytokine Assays
Because alveolar macrophages are targets of infection in our experiments, alveolar macrophages were prepared from IL-1 α/β KO and WT mice to determine whether they secreted various monokines (IL-12, TNF-α, and IL-1). After the mice had been anesthetized with 100 μl pentobarbital, alveolar macrophages were obtained by bronchoalveolar lavage. Briefly, the murine trachea was cannulated and 1 ml physiological saline was poured in. The saline was recovered using a 1 ml disposable syringe. The cells thus obtained contained more than 99% macrophages as assessed by phagocytosis of BCG. The cell suspensions were plated (1×105 cells/well) in 96-well culture plates and incubated for 12 hours at 37°C in 5% CO2 in air, and the cells were stimulated with either medium alone or medium containing LPS (Sigma Chemical, St. Louis, Missouri; 10 μg/ml) or live BCG organisms (103 CFU/well). The concentrations of IL-12, TNF-α, and IL-1β in the culture supernatants of these cells were measured by sandwich enzyme-linked immunosorbent assay (ELISA) (Biosource International, Camarillo, California).
Alveolar Macrophage Nitric Oxide Assay
Alveolar macrophages (5×105/well) in RPMI 1640 supplemented with 10% (vol/vol) fetal calf serum were plated in 96-well culture plates, left unstimulated or stimulated with recombinant IL-1α/β (1000 units each, Genzyme, Cambridge, Massachusetts), then cultured with BCG or H37Rv overnight. The supernatants were collected 24 hours after culture seeding and filtering, and their nitrite concentrations were determined by the Griess assay, as described previously (Green et al, 1990; Kaneko et al, 1999).
Reverse Transcriptase-Polymerase Chain Reaction
Lung tissue samples were taken from infected mice 1, 3, 5, or 7 weeks after infection, frozen in liquid nitrogen, and stored at −85°C until required for use, when RNA was extracted as described previously. RT-PCR was carried out using gene-specific primer sets for inducible NO synthase (iNOS), TNF-α, IFN-γ, IL-12 p40, IL-1β, IL-4, and IL-10 (CLP Inc., California), the respective sizes of which were 306, 276, 405, 850, 447, 441, and 324 bp. The β-actin RNA from the spleen tissues was used as an internal control for size comparison in the RT-PCR analysis (Kaneko et al, 1999; Sugawara et al, 1998).
Reconstitution of IL-1 α/β KO Mice with Exogenous IL-1
KO mice were injected subcutaneously with 100 μl recombinant IL-1 α and β (5×104 units each, Genzyme) in PBS or with PBS alone, on four occasions at weekly intervals. The lungs from the infected IL-1 α/β KO mice treated subcutaneously with recombinant IL-1 were retrieved 7 weeks after infection. The lung tissues were used for CFU assay and histopathological analysis.
Statistical Analysis
All values were expressed as means + se and compared by Student's t test. For all statistical analyses, a p value of < 0.01 was considered significant.
In summary, the results presented in this report indicate the importance of IL-1 in generating early protective immunity against mycobacterial infection.
References
Asano M, Furukawa K, Kido M, Matsumoto S, Umesaki Y, Kochibe N, and Iwakura Y (1997). Growth retardation and early death of β-1,4- galactosyltransferase knockout mice with augmented proliferation and abnormal differentiation of epithelial cells. EMBO J 16:1850–1857.
Bean AG, Roach DR, Briscoe H, France MP, Korner H, Sedgwick JD, and Britton WJ (1999). Structural deficiencies in granuloma formation in TNF gene-targeted mice underlie the heightened susceptibility to aerosol Mycobacterium tuberculosis infection, which is not compensated for by lymphotoxin. J Immunol 162:3504–3511.
Cooper AM, Dalton DK, Stewart TA, Griffin JP, Russell DG, and Orme IM (1993). Disseminated tuberculosis in interferon-γ gene-disrupted mice. J Exp Med 178:2243–2247.
Cooper AM, Magram J, Ferrante J, and Orme IM (1997). Interleukin 12 (IL-12) is crucial to the development of protective immunity in mice intravenously infected with Mycobacterium tuberculosis. J Exp Med 186:39–45.
Dalton DK, Pitts-Meek S, Keshav S, Figari IS, Bradley A, and Stewart TA (1993). Multiple defects of immune cell function in mice with disrupted interferon-γ genes. Science 259:1739–1742.
Dinarello CA (1996). Biologic basis for interleukin-1 in disease. Blood 87:2095–2147.
Durum SK and Oppenheim JJ (1993). Proinflammatory cytokines and immunity. In: Paul WE, editor. Fundamental immunology, 3rd ed. New York:Raven Press, Ltd, 801–835.
Fantuzzi G and Dinarello CA (1996). The inflammatory response in interleukin-1 β-deficient mice: comparison with other cytokine- related knock-out mice. J Leukoc Biol 59:489–493.
Flynn J, Chan J, Triebold KJ, Dalton DK, Stewart TA, and Bloom BR (1993). An essential role for interferon γ in resistance to Mycobacterium tuberculosis infection. J Exp Med 178:2249–2254.
Green SJ, Crawford RM, Hockmeyer JT, Meltzer MS, and Nacy CA (1990). Leishmania major amastigotes initiate the L- arginine-dependent killing mechanism in IFN-γ-stimulated macrophages by induction of tumor necrosis factor-α. J Immunol 145:4290–4297.
Hirsch E, Irikura VM, Paul SM, and Hirsch D (1996). Functions of interleukin 1 receptor antagonist in gene knockout and overproducing mice. Pro Natl Acad Sci U S A 93:11008–11013.
Horai R, Asano M, Sudo K, Kanuka H, Suzuki M, Nishihara M, Takahashi M, and Iwakura Y (1998). Production of mice deficient in genes for interleukin (IL)-1α, IL-1β, IL-1 α/β, and IL-1 receptor antagonist shows that IL-1β is crucial in turpentine-induced fever development and glucocorticoid secretion. J Exp Med 187:1463–1475.
Kaneko H, Yamada H, Mizuno S, Udagawa T, Kazumi Y, Sekikawa K, and Sugawara I (1999). Role of tumor necrosis factor-α in Mycobacterium-induced granuloma formation in tumor necrosis factor-α-deficient mice. Lab Invest 79:379–386.
Labow M, Shuster D, Zetterstrom M, Nunes P, Terry R, Cullinan EB, Bartfai T, Solorzano C, Moldawer LL, Chizzonite R, and McIntyre KW (1997). Absence of IL-1 signaling and reduced inflammatory response in IL-1 type I receptor-deficient mice. J Immunol 159:2452–2461.
Lonnemann G, Shapiro L, Engler-Blum G, Müller GA, Koch KM, and Dinarello CA (1995). Cytokines in human renal interstitial fibrosis. I. Interleukin-1 is a paracrine growth factor for cultured fibrosis-derived kidney fibroblasts. Kidney Int 47:837–844.
Nakamura H, Morishita Y, Sugawara I, Fujii Y, Hasumi K, and Mori S (1990). Ultrastructural localization of antigens recognized by 5D-4 monoclonal antibody reactive with islets of Langerhans. J Electron Microsc 23:393–398.
Schormick LP, De Togni PD, Mariathasan S, Goellner J, Strauss-Schoenberger J, Karr RW, Ferguson TA, and Chaplin DD (1996). Mice deficient in IL-1β manifest impaired contact hypersensitivity to trinitrochlorobenzene. J Exp Med 183:1427–1436.
Sugawara I, Yamada H, Kaneko H, Mizuno S, Takeda K, and Akira S (1999). Role of interleukin-18 (IL-18) in mycobacterial infection in IL-18–gene–disrupted mice. Infect Immun 67:2585–2589.
Sugawara I, Yamada H, Kazumi Y, Doi N, Otomo K, Aoki T, Mizuno S, Udagawa T, Tagawa Y, and Iwakura Y (1998). Induction of granulomas in interferon-γ gene-disrupted mice by avirulent but not by virulent strains of Mycobacterium tuberculosis. J Med Microbiol 47:871–877.
Tocci MJ, and Schmidt JA (1997). Interleukin-1: structure and function. In: Remick DG, and Friedland JS, editors. Cytokines in health and disease, 2nd ed. New York:Marcel Dekker, Inc., 1–27.
Zheng H, Fletcher D, Kozak W, Jiang M, Hofmann KJ, Conn CA, Soszynski D, Grabiec C, Trumbauer ME, and Shaw A (1995). Resistance to fever induction and impaired acute-phase response in interleukin-1β-deficient mice. Immunity 3:9–19.
Zuniga-Pflücker AM, Jiang D, and Leonardo MJ (1995). Requirement for TNFα and IL-1α in fetal thymocyte commitment and differentiation. Science 268:1906–1909.
Acknowledgements
This study was supported in part by an International Collaborative Study Grant to the chief investigator, Isamu Sugawara, from the Ministry of Health and Welfare, Japan. Part of this work was presented at the 73rd Annual Meeting of The Japanese Society for Tuberculosis at Tochigi, Japan, in 1999.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Yamada, H., Mizumo, S., Horai, R. et al. Protective Role of Interleukin-1 in Mycobacterial Infection in IL-1 α/β Double-Knockout Mice. Lab Invest 80, 759–767 (2000). https://doi.org/10.1038/labinvest.3780079
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1038/labinvest.3780079
This article is cited by
-
Early alveolar macrophage response and IL-1R-dependent T cell priming determine transmissibility of Mycobacterium tuberculosis strains
Nature Communications (2022)
-
Type I interferon-driven susceptibility to Mycobacterium tuberculosis is mediated by IL-1Ra
Nature Microbiology (2019)
-
Patients with type 1 diabetes mellitus have impaired IL-1β production in response to Mycobacterium tuberculosis
European Journal of Clinical Microbiology & Infectious Diseases (2018)
-
Clash of the Cytokine Titans: counter-regulation of interleukin-1 and type I interferon-mediated inflammatory responses
Cellular & Molecular Immunology (2017)
-
Inflammasomes-dependent regulation of IL-1β secretion induced by the virulent Mycobacterium bovis Beijing strain in THP-1 macrophages
Antonie van Leeuwenhoek (2015)