Abstract
An increasing body of research indicates that stroma surrounding cancer cells plays an important role in the development and subsequent behavior of the tumor. Studies using a wide range of techniques, including stromal cell isolation, modification of stromal-specific gene expression, and recreation of specific microenvironment conditions in culture, have demonstrated that stroma can promote cancer and that the expression patterns within the stroma can influence clinical outcome. Major hurdles in the study of the cancer stroma revolve around the cellular complexity of the tumor microenvironment, both in modeling the microenvironment and discovering/isolating pure populations of stromal cell types.
Similar content being viewed by others
Analysis and manipulations of tumor stroma
The majority of cancer research has focused on the neoplastic cells and as a result, the vast majority of therapies available to oncologists are therapeutic agents that act on these cancer cells. The cancers often develop resistance to these therapies, in large part due to their inherent genomic instability.1 An alternative, emerging, avenue of therapy focuses on targeting various non-neoplastic cells that are associated with the tumor microenvironment, such as endothelial cells.2 Since stromal cells within the tumor are thought to be ‘normal’ and less genetically labile than the neoplastic cells, development of acquired resistance to therapy may be less likely. As such, the tumor stroma may be an excellent target for directed therapy.
The rapidly growing field of stroma–cancer interaction has been advanced by a number of elegant and useful studies. A number of studies used isolated stromal cells from carcinomas to demonstrate that these cells have developed increased ability to support cancerous growth compared to normal stromal cells. Several examples stand out in this area. Olumi et al3 showed that fibroblasts isolated from prostatic tumor stroma significantly increased growth of prostate epithelium. This supporting effect of carcinoma-associated fibroblasts (CAF) was not seen when these fibroblasts were isolated from normal prostatic stroma. Similarly, a study by Orimo et al4 used CAF isolated from different patients in a model system in which an MCF7-ras breast carcinoma tumor cell line was co-injected with CAF into immunodeficient mice. The CAF provided better support for MCF7 cell growth than fibroblasts derived from areas that were not intimately associated with invasive carcinoma. Krtolica et al5 showed that senescent human stromal cells can stimulate pre-malignant and malignant, but not normal, epithelial cells to proliferate in culture and form tumors in mice. These findings suggest that senescent fibroblasts could promote cancer in certain circumstances.
Another approach has been to selectively modify stromal cell gene expression and observe the effect on oncogenesis. In a study by Bhowmick et al,6 fibroblasts had the TGF-β type II receptor gene conditionally inactivated. This resulted in prostatic intraepithelial neoplasia and invasive squamous cell carcinoma of the forestomach. This result suggests that TGF-β signaling involving fibroblasts can modulate the oncogenic potential of adjacent epithelium.
Other groups have altered fibroblast culture conditions to simulate specific aspects of stromal environments. Exposure of serum-starved cultured fibroblasts to serum led to a change in expression of a large number of genes, many of which are known to be involved in wound healing.7 Serum exposure of fibroblasts occurs in wounds in vivo and activates a wound-healing response and a similar reaction had been hypothesized to occur in cancers.8 Using the wound-healing response gene set identified in fibroblast cultures, the authors could identify a similar response in a subset of breast tumors and this was associated with a poor clinical outcome. The influence on progression of these wound-healing signatures was not only restricted to breast carcinomas but was also seen in a variety of other tumors including lung and gastric carcinoma. Similarly, a response to hypoxic conditions was examined in a variety of cultured cell types in a different set of experiments.9 The expression patterns of the hypoxia response in culture were also represented in several carcinomas and predicted a worse outcome.
A number of groups have successfully undertaken technically demanding studies to isolate and evaluate cancer stroma expression. For example, Allinen et al10 used flow cytometry to separate different cell populations followed by SAGE to generate gene expression profiles of different components of the tumor microenvironment, including neoplastic and stromal cell types. The authors could identify many genes that were highly and specifically expressed at high levels in each cell compartment. Owing to the complexity of this method only a few breast cancers could be studied. More importantly, the ‘sort by subtraction technique’ for isolating stromal cells did not tease out possible different fibroblast subtypes or activation states but instead treated all stromal cells as a uniform population. In another study, a mouse model of prostatic adenocarcinoma was used to generate microdissected-purified stroma from both prostatic adenocarcinoma and prostatic intraepithelial neoplasia. The differences in gene expression profiles of these two types of stroma were found to predict outcome in both prostate and breast cancer.11
The conclusions drawn from these and many other studies indicate that tumor stroma does play a supporting and, according to some studies, perhaps even an initiating role in malignant epithelial tumor growth.12, 13 But some of these studies also suggest that there is a variety of stromal responses that can occur in the tumor microenvironment.
Using soft tissue tumors as a model system to study tumor stroma
Given the intense interest in stroma, there is little knowledge about normal stromal components and their expression. Yet it has been shown that ‘normal’ fibroblasts can show markedly different expression patterns. Therefore, it is possible that there are as yet to be determined activation states or even fibroblast subtypes. The study of normal connective tissue and tumor stroma is hampered by a lack of markers that can distinguish subtypes of stromal spindle cells (fibroblasts, myofibroblasts, and possible unknown variants). These cells are histologically quite similar and morphologic studies have struggled to find correlation between form and function. Experimental approaches to the study of connective tissue components are thus complicated by the intimate coexistence of many different cell types within the tissue. One approach to this problem is to study the expression profiles of soft tissue tumors (STTs) as surrogates for unrecognized cell types in a variety of stromal responses, including cancer. STTs, whether clinically benign or malignant, form a relatively pure population of transformed normal connective tissue constituents. We believe that STT-based studies can contribute in an essential manner to this field by discovering new markers that recognize distinct subtypes of these normal connective tissue and tumor stroma spindle cells, allowing us to recognize the diversity of cell types that hide under the terms ‘fibroblast’ or ‘myofibroblast’. A large number (over 100) of distinct STTs exist and there are numerous examples of markers specific for a particular tumor that can identify a subpopulation of morphologically identical normal stromal components.
Similar to lymphomas where each tumor is a clonal outgrowth of a particular lymphoid cell subtype, each STT type may also be regarded as a clonal outgrowth of a particular connective tissue cell type. In the past, lymphomas have been used as ‘discovery tools’ for new monoclonal antibodies.14, 15 Mice were immunized with lymphoma cells and the resulting monoclonal antibodies often led to the discovery of distinct lymphocyte subtypes. The lymphocyte differentiation antigens would have been hard to identify if normal lymphoid tissue, which includes a mixture of lymphocyte types, was injected into mice as an immunogen. For example, T-helper cells constitute a minority of the total lymphocyte population and, in an immunization challenge with normal lymphoid tissue, antibodies specific to T-helper cells would likely be lost among antibodies to proteins from other lymphocyte types. Therefore, to find markers that are expressed on a small subset of cells, it is very useful to use tumors derived from this subset of cells as immunogen. In our case, rather than immunize mice with STT tissue, a more direct approach is to perform gene expression profiling to find candidate markers. This ‘in silico’ alternative to immunization generates many more candidate markers, allows direct comparison of expression profiles for different STTs, is independent of the complexities of the mouse immune system, and allows an immediate assessment of expression in many situations, such as the tumor microenvironment, by application to existing gene expression profile data sets (Figure 1).
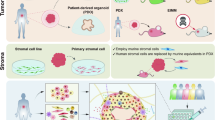
The effect of clustering breast carcinomas with stroma-specific genes. Generally, gene microarray data on breast carcinomas are clustered with genes that pass a number of quality criteria. In this process (a), genes that are expressed in carcinoma cells tend to play a predominant role in clustering breast cancer cases based on similarities between tumor cells from different patients. For example, patient samples with ‘red’ tumor cells will co-cluster independently of the type of fibroblasts (blue vs orange) that surround them. It is caused by the fact that the number of genes that are expressed by the different fibroblast types and stroma is relatively low. A list of genes specific for different types of stromal fibroblasts can be discovered by performing gene expression profiles on two types of fibroblast-like soft tissue tumors resulting in a list of approximately 400 genes that are expressed in a mutually exclusive manner between the soft tissue tumors (b). When breast carcinomas are next clustered using the information for these 400 genes only, as only shown in (c), breast carcinomas will tend to cluster there based on the type of fibroblasts that surround them. For example, the breast carcinomas in the left most branch of the dendrogram, in orange, are surrounded by the ‘orange’-type fibroblasts driven by the high expression levels of genes specific for the ‘orange’ soft tissue tumor-type fibroblast; see bar on the right-hand side of (c). In contrast, carcinoma specimens where the ‘blue’ type of fibroblast surrounds the tumor cells will be co-clustered based on the high level of expression found in the specimens of genes specific for the ‘blue’ type of soft tissue tumor.
In our first investigation toward this goal, we used gene expression profiles from two different STTs, desmoid-type fibromatosis (DTF) and solitary fibrous tumor (SFT), thought to be derived from ‘fibroblasts’, to identify their counterparts, and possibly new subtypes, in normal connective tissue.16 The two similar ‘fibroblastic’ tumors, SFT and DTF, are quite distinct tumors despite being composed of cells with very similar morphology and yet have dramatically different clinical behavior. Comparing the SFT and DTF gene expression profiles, we found a remarkably large number of differentially expressed genes from different functional categories. The distinguishing genes showed great differences in function with genes involved in the fibrotic response being highly expressed in DTF, whereas many genes associated with basement membrane synthesis being highly expressed in SFT. Tissue staining show that tumor-specific markers are also differentially expressed in normal connective tissue cells, including inflammatory responses that lead to scar formation, such as a fistula tract, and specialized stroma around dermal sweat glands. Based on these differences in expression we hypothesized that the cells of origin for each lesion may perform different functions in normal connective tissue.
We found that these markers are also differentially expressed in the tumor microenvironment. These markers were often mutually exclusively expressed in the stroma of different breast carcinoma cases. We analyzed the expression of these genes in a large gene expression profile data set of breast cancer. When the breast carcinomas were clustered based on the SFT and DTF sets of positively expressed genes only, a subset of DTF-associated genes defined a distinct group of breast carcinomas. Interestingly, a previous study used serial analysis of gene expression on sorted components of the breast cancer microenvironment.10 Some of the genes found to be highly expressed in their ‘myoepithelial/myofibroblast’ cell population are also present in the DTF gene list. A subsequent study examining the expression differences between prostatic intraepithelial neoplasia and invasive prostatic adenocarcinoma also found genes present in the DFT gene list.11 In addition, two groups of genes associated with SFT defined a second group of breast carcinomas. Not all DTF genes contributed equally to the separation of breast carcinomas with a DTF-like stroma for the rest of the tumors. Thus, the breast carcinoma gene expression data set can be seen as a ‘filter’ to highlight genes that are most important in describing the stromal subtypes in carcinoma. The two groups of breast carcinoma, distinguished by expression of genes in the stroma but not in the tumor cells, showed a remarkable difference in clinical outcome. Because the genes are discovered in STTs, we expect that the majority of these genes will be expressed in the stromal cells and not expressed in the neoplastic epithelial cells of the carcinoma. This assumption has so far been supported by histological analysis of expression of five markers and by GO-term analysis. Almost all ‘discovery-type’ gene expression studies use unsupervised expression data to cluster the tumors, which results in the tumors being clustered based mainly on the gene expression patterns of the neoplastic cells. More subtle variations in gene expression patterns of the tumor stroma can be lost in the analysis, overwhelmed by the neoplastic cell expression patterns. By analyzing these carcinoma data sets with a gene set restricted to connective tissue-related genes, such as those derived from STT gene signatures, we can uncover these latent tumor stroma expression patterns.
In conclusion, there is ample evidence that the stroma within the tumor microenvironment plays an important role in cancer biology. The specific interactions remain to be elucidated. In the future, this field may uncover novel therapeutic approaches that target the cancer–stroma interaction.
References
Rajagopalan H, Nowak MA, Vogelstein B, et al. The significance of unstable chromosomes in colorectal cancer. Nat Rev Cancer 2003;3:695–701.
Folkman J . Angiogenesis. Annu Rev Med 2006;57:1–18.
Olumi AF, Grossfeld GD, Hayward SW, et al. Carcinoma-associated fibroblasts direct tumor progression of initiated human prostatic epithelium. Cancer Res 1999;59:5002–5011.
Orimo A, Gupta PB, Sgroi DC, et al. Stromal fibroblasts present in invasive human breast carcinomas promote tumor growth and angiogenesis through elevated SDF-1/CXCL12 secretion. Cell 2005;121:335–348.
Krtolica A, Parrinello S, Lockett S, et al. Senescent fibroblasts promote epithelial cell growth and tumorigenesis: a link between cancer and aging. Proc Natl Acad Sci USA 2001;98:12072–12077.
Bhowmick NA, Chytil A, Plieth D, et al. TGF-beta signaling in fibroblasts modulates the oncogenic potential of adjacent epithelia. Science 2004;303:848–851.
Chang HY, Sneddon JB, Alizadeh AA, et al. Gene expression signature of fibroblast serum response predicts human cancer progression: similarities between tumors and wounds. PLoS Biol 2004;2:E7.
Dvorak HF . Tumors: wounds that do not heal. Similarities between tumor stroma generation and wound healing. N Engl J Med 1986;315:1650–1659.
Chi JT, Wang Z, Nuyten DS, et al. Gene expression programs in response to hypoxia: cell type specificity and prognostic significance in human cancers. PLoS Med 2006;3:e47.
Allinen M, Beroukhim R, Cai L, et al. Molecular characterization of the tumor microenvironment in breast cancer. Cancer Cell 2004;6:17–32.
Bacac M, Provero P, Mayran N, et al. A mouse stromal response to tumor invasion predicts prostate and breast cancer patient survival. PLoS ONE 2006;1:e32.
Mueller MM, Fusenig NE . Friends or foes—bipolar effects of the tumour stroma in cancer. Nat Rev Cancer 2004;4:839–849.
Bissell MJ, Radisky D . Putting tumours in context. Nat Rev Cancer 2001;1:46–54.
Ritz J, Pesando JM, Notis-McConarty J, et al. A monoclonal antibody to human acute lymphoblastic leukaemia antigen. Nature 1980;283:583–585.
Nadler LM, Stashenko P, Hardy R, et al. Characterization of a human B cell-specific antigen (B2) distinct from B1. J Immunol 1981;126:1941–1947.
West RB, Nuyten DS, Subramanian S, et al. Determination of stromal signatures in breast carcinoma. PLoS Biol 2005;3:e187.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
West, R., van de Rijn, M. Experimental approaches to the study of cancer–stroma interactions: recent findings suggest a pivotal role for stroma in carcinogenesis. Lab Invest 87, 967–970 (2007). https://doi.org/10.1038/labinvest.3700666
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/labinvest.3700666
Keywords
This article is cited by
-
Next generation sequencing-based expression profiling identifies signatures from benign stromal proliferations that define stromal components of breast cancer
Breast Cancer Research (2013)
-
Transcription Factor Networks in Invasion-Promoting Breast Carcinoma-Associated Fibroblasts
Cancer Microenvironment (2013)
-
Gene expression analysis identifies two groups of ovarian high-grade serous carcinomas with different prognosis
Modern Pathology (2011)
-
Stroma–epithelium crosstalk in prostate cancer
Asian Journal of Andrology (2009)
-
The fibromatosis signature defines a robust stromal response in breast carcinoma
Laboratory Investigation (2008)