Abstract
Inactivation of the von Hippel-Lindau (VHL) tumor suppressor gene leads to the development of central nervous system hemangioblastomas, pheochromocytomas and renal cell carcinomas. The biological role of the VHL gene during development is poorly understood because of early lethality of VHL-null embryos. To overcome early embryo lethality observed in the conventional knockout mouse, we introduced a tamoxifen-inducible Cre (CreERTM) transgene for the stage specific inactivation of the VHL gene. Acute tamoxifen-induced inactivation of the VHL gene at E10.5 resulted in embryonic lethality between E14.5 and E15.0 with extensive hemorrhage and necrosis, while littermate controls showed normal development. Examination of the VHL-inactivated embryos between E10.5 and E14.5 revealed dilated blood vessels, hemorrhage and necrotizing liver damage. Concomitant with severe hemorrhage and abnormal vasculature at E15.0, blood circulation in the yolk sac was impaired in the VHL-inactivated embryos, which may be the cause of embryo death. Placental development looked normal before embryo death (E14.5); however, at E16.5 following embryo death, we observed reduced growth of the placental labyrinthine layer. Inactivation of the VHL gene resulted in hypoxia-inducible factor (HIF)-1α stabilization and induction of its target genes, VEGF and CAIX, in mouse embryonic fibroblasts (MEFs). In addition, we observed lactate overproduction and acidification of culture media by the inactivation of the VHL gene. Thus, by using a novel conditional VHL knockout mouse model, we could show that the VHL gene plays an important role in the developing vasculature and liver during embryogenesis through regulation of HIF-1α and its target genes. This mouse model will be useful for the screening of anti-HIF or anti-VEGF drugs in vivo. Additionally, this acute VHL inactivation system may provide a useful tool for the in vivo study of genes that cause early embryonic lethality.
Similar content being viewed by others
Main
von Hippel-Lindau (VHL) disease is a hereditary cancer syndrome, which is transmitted in an autosomal dominant manner and affects approximately 1 in 36 000 individuals.1 The VHL gene was mapped to 3p25 and isolated by positional cloning.1, 2 VHL germline mutations are responsible for the development of highly vascular tumors including hemangioblastomas of the retina and central nervous system, pheochromocytomas and renal cell carcinomas (RCC). pVHL is a component of an E3 ubiquitin ligase complex that recognizes and degrades the alpha subunits of hypoxia-inducible factor (HIF) under normoxic conditions.3, 4 Type 1, type 2A and type 2B VHL mutations, which disrupt regulation of HIF, lead to the accumulation of HIF under normoxic conditions.5 HIF target genes, such as vascular endothelial growth factor (VEGF), Glucose transporter 1 (Glut-1) and carbonic anhydrase IX (CAIX) are upregulated in response to the inactivation of the HIF regulatory activity of pVHL.6, 7, 8 It is likely that the HIF regulatory activity of pVHL is related to the development of hemangioblastomas and RCC in VHL patients. However, type 2C mutations in the VHL gene, which are responsible for pheochromocytoma development, retain the HIF regulatory activity, but are defective in promoting fibronectin matrix assembly.9 Recently pVHL has also been shown to bind microtubules and stabilize their structure.10 This activity is disrupted only in the type 2A VHL mutants that have diminished but not defective HIF regulatory activity. These biochemical analyses of pVHL function provide possible molecular clues to explain the phenotype–genotype correlations evident in VHL disease.
HIF regulation under normoxic condition is the most well-described function of pVHL. Oxygen is essential for oxidative phosphorylation, which satisfies the high energy demand of multicellular organisms. Cells maintain oxygen homeostasis and also generate necessary energy metabolites. HIF is a transcription factor that plays an essential role in modulating both cellular and systemic responses to changes in oxygen concentration. It regulates the expression of genes involved in angiogenesis, hematopoiesis, pH regulation and energy metabolism (glucose transporter and glycolytic enzymes). VHL inactivation results in oxygen-independent accumulation of HIF and thus, upregulation of its target genes under normoxic conditions. It has been demonstrated that HIF and its target genes are important for tumor progression.11
Several VHL-knockout (KO) mouse models have been developed to investigate the biological role of pVHL. Vascular hepatic tumors developed in the heterozygous VHL-KO mice and also in β-actin-promoter driven Cre-mediated conditional VHL-KO mice.12, 13 Upregulation of HIFs and their target genes were reported in these mouse models. Additional roles for pVHL in different organs have been suggested through the use of Cre-mediated VHL inactivation. VHL inactivation resulted in defects in spermatogenesis, thymus cell survival and bone development due to reduced cell proliferation and/or increased cell death.13, 14, 15 Contrary to expectation, VHL-inactivation did not increase cell proliferation in somatic and germ cells. Teratomas derived from VHL null embryonic stem (ES) cells displayed a highly vascular phenotype but showed severe reduction of tumor volume compared with heterozygous null ES cells.16 Reintroduction of VHL into VHL null ES cells restored tumor growth, so that the tumor volume was comparable to that of VHL heterozygous null ES cells. Specifically this growth disadvantage of teratomas was shown to be related to VHL type 2A mutations.17 Thus, it is likely that additional mutations in unknown gene(s), which can facilitate cell growth, might be necessary for the development of tumors in VHL patients.
VHL homozygous null mouse embryos died in utero at E10.5 to E12.5 due to defects in placental vasculogenesis.18 As a result of early embryo lethality, little is known about the role of the VHL gene in embryo development. Here, we explored the functions of the VHL gene during embryogenesis by inactivating the VHL gene at mid-gestation. We used an inducible system in which tamoxifen induced Cre recombinase (CreERTM)19 to inactivate the floxed VHL gene in an acute manner during embryo development. VHL inactivation occurred in a mosaic pattern and produced vascular defects and liver damage in the VHL inactivated embryos.
Materials and methods
Generation and Genotyping of VHLf/d/CreERTM Embryos
Previously, we generated mice harboring floxed (f) and deleted (d) VHL alleles on a C57BL6/129 mixed background.13 VHLd/+ mice were crossed with mice carrying a CreERTM transgene obtained from Dr Corrinne Lobe (University of Toronto) to produce VHLd/+/CreERTM mice. VHLd/+/CreERTM mice used in this study were either VHLd/+/CreERTM(tg/0) or VHLd/+/CreERTM(tg/tg) since they were maintained by backcrossing with either the CreERTM(tg/0) or CreERTM(tg/tg) transgenic mice. VHLd/+/CreERTM mice were crossed with VHLf/f mice to produce VHLf/d/CreERTM (VHLf/d/CreERTM(tg/0)) embryos, in which the floxed VHL allele could be excised by tamoxifen induced Cre recombinase activity. Tamoxifen dissolved in corn oil was injected intraperitoneally (0, 0.1, 1, 2, 4 and 8 mg) into pregnant females (25–30 g) at mid-gestation. Embryos and their placentas were collected 2–6 days after tamoxifen injection, photographed and fixed in neutral formalin for histological examination. For genotyping, genomic DNAs were isolated from the yolk sacs after proteinase K digestion. For VHL genotyping, three primers were used to amplify wild type (244 bp PCR product), floxed (277 bp PCR product) and deleted (161 bp PCR product) VHL alleles; P1 5′-GGCAAGCACTCTGTCACTGTTC-3′, which is specific to genomic sequence upstream of the 5′-loxP sequence; P2 5′-GGCTATGGCATTGGGTGAGCTA-3′, which is upstream of 3′-loxP sequence; P3 5′-CACCAGGACTCCTCTCGGACAT-3′, which is downstream of 3′-loxP sequence. For Cre genotyping, the forward (5′-GCAACATTTGGGCCAGCTAAAC-3′) and the reverse (5′-CCGGCATCAACGTTTTCTTTTTC-3′) primers were used for PCR amplification. DNAs isolated from embryos and their placentas were used for Southern blot analysis using a PCR-generated 250 bp probe specific to sequence upstream of the 5′ loxP site of VHL as described.13 Briefly, genomic DNAs were digested with HindIII restriction enzyme, electrophoresed in 0.8% agarose, blotted onto a HybondN+ membrane and probed with the 32P-labeled probe.
Evaluation of Cre Activity in the CreERTM Transgenic Embryos
Tamoxifen induced Cre activity was evaluated in embryos from crosses of the CreERTM transgenic mice with ROSA26 reporter mice,20 in which excision of the floxed neomycin cassette by Cre recombinase allows lacZ gene expression. Tamoxifen (2 mg/30 g mouse) was injected into pregnant females at E10.5 and embryos were harvested at E13.5 or E14.5. β-galactosidase activity was measured in situ in whole embryos, in dissected organs or in frozen sections using standard staining techniques. Tissue sections were counterstained with nuclear fast red (Sigma).
Generation of MEFs and Cell Culture
Mouse embryonic fibroblasts (MEFs) were generated from E13.5 mouse embryos. Embryos were harvested, minced and trypsinzed (0.25% trypsin) for 10–20 min at 37°C. Tissue culture media (DMEM containing 10% fetal bovine serum and penicillin/streptomycin) was added to cell suspensions and pipetted up and down for further disaggregation. Cell suspensions were cultured in T75 flasks containing 10 ml media in a CO2 incubator at 37°C. Confluent cultures were trypsinized and replated onto two 150 mm dishes. After 3 days of culture, cells were trypsinized and resuspended in DMEM containing 10% FBS and 10% DMSO for liquid nitrogen storage. Frozen vials were subsequently thawed and passaged every 3 days. Cells were seeded at 7.5 × 105 cells per 100 mm dish or equivalent. Early passage MEFs (P3–P10) were used for the experiments. 4-hydroxy tamoxifen (4OHT) dissolved in ethanol was used to induce CreERTM activity during MEF culture.
Measurement of Lactate Production
MEFs were plated on two 12-well plates (3.5 × 104 cells/well), and 4OHT (0, 5, 20 and 100 nM) was added to the culture media 1 day after plating. On the fourth day, media was changed and 4OHT was added again. On the seventh day, cell numbers were counted in one of the two replicative plates. Culture media in the second plate was replaced with fresh media and 1 day later 50 μl of media was collected for lactate measurement. Lactate concentration in the culture was measured as described with minor modifications.21 Briefly, 5 μl of culture media was added to the reaction mixture containing lactate oxidase, peroxidase and substrate, ABTS (Sigma). After 10 min of reaction at room temperature, absorbance was measured at 405 nm. Lactate production was normalized to the cell number.
Isolation of RNAs from MEFs and Quantitative RT-PCR
Total RNAs were isolated from MEFs using Trizol reagent (Invitrogen) according to the manufacturer's instruction. To remove genomic DNA contamination, RNAs were digested with DNase I for 1 h at 37°C followed by heat denaturation at 70°C for 20 min. Total RNAs (2.5 μg) were primed with 100 ng random primers and reverse-transcribed by Superscript II reverse transcriptase (Invitrogen) at 42°C for 1 h. The same reactions were performed without reverse transcriptase to generate negative controls. The following PCR primers were generated by using Primer 3 software:22 VEGF forward, 5′-CAGGCTGCTGTAACGATGAA-3′; VEGF reverse, 5′-TATGTGCTGGCTTTGGTGAG-3′; VHL forward, 5′-TGTGCCATCCCTCAATGTCG-3′; VHL reverse, 5′-AGGCTCCGCACAACCTGAAG-3′; β-actin forward, 5′-GACAGGATGCAGAAGGAGATTACTG-3′; β-actin reverse, 5′-GCTGATCCACATCTGCTGGAA-3′; CAIX forward, 5′-CCTCTCCCGGAACTGAGCCTAT-3′; CAIX reverse, 5′-TGTTCTGAGCCTGGGTGATCTG-3′. Quantitative RT-PCR was performed with SYBR-Green reagent (Applied Biosystems) with the ABI PRISM sequence detection system (Applied Biosystems) following the manufacturer's instruction. All reactions were run in triplicate using the β-actin gene as an internal control since β-actin mRNA levels do not change across the VHL genotypes. The relative level of a particular gene expression was evaluated according to the function described previously.23 All expression levels reported were expressed relative to the expression levels determined for VHLf/+ MEFs.
Immunoblots
MEFs incubated with tamoxifen were harvested and lysed in RIPA buffer. Cell lysates were resolved by 8–16% SDS PAGE and blotted onto PVDF membrane. Equal protein loading was confirmed by Ponceau S staining. Antibodies for HIF-1α, HIF-2α (Novus biologicals Inc.) and pVHL (Santa Cruz Biotechnology Inc.) were used for Western-blot analysis. Immunoblots were processed by ECL (Pierce) according to the manufacturer's instruction.
Phenotype Evaluation and Histopathology
Embryos and placentas were dissected at E12.5–E18.5 and gross morphological changes were examined under a dissection microscope. They were fixed in 10% formalin, embedded in paraffin, and 5 μm sections were prepared. The sections were deparaffinized and rehydrated through an ethanol dilution series into water. Sections were stained with hematoxylin and eosin.
Results
Evaluation of Tamoxifen Toxicity and Tamoxifen-Induced Excision of the Floxed Sequence
To inactivate the VHL gene during embryogenesis, we used mice carrying the CreERTM transgene, in which introduction of tamoxifen induces Cre recombinase to excise the floxed gene. CreERTM transgenic mice exhibit highest Cre activity in embryos from pregnant females injected with 8 mg of tamoxifen, although some toxicity to the mother was observed.19 To avoid any harmful effects of tamoxifen, we determined the least toxic concentration of tamoxifen that was still effective in inducing Cre recombination. We evaluated tamoxifen toxicity in embryos by injecting 1, 2, 4 or 8 mg of tamoxifen into the pregnant female (25–30 g) intraperitoneally at E10.5 and evaluating gross morphological changes in the embryos at E13.5. We found that 8 mg of tamoxifen caused hemorrhage in every embryo examined (8/8). However, 1, 2 and 4 mg of tamoxifen induced morphological changes in only 1/20 embryos (data not shown). We selected 2 mg tamoxifen as the maximum dose that produced no morphologic changes.
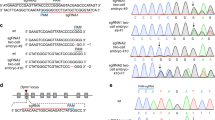
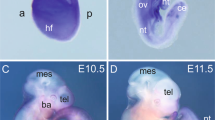
We asked whether 2 mg of tamoxifen (per 25–30 g body weight) could excise the floxed gene sequence in the embryos by crossing CreERTM mice with ROSA26 reporter mice and measuring β-galactosidase staining in the embryos as a measure of Cre recombinase activity. CreERTM/ROSA26 double transgenic embryos exhibited positive lacZ staining while their ROSA26 embryo littermates showed negative staining (Figure 1a and b). LacZ positive staining was observed in a mosaic pattern in most of the tissues and organs to varying degrees (Figure 1c, d and e). In the heart, liver and brain, approximately 50, 10 and 20% of the cells, respectively, were positive for lacZ, indicating that the efficiency of deletion may be 10–50% in these embryonic organs. We also examined Cre recombinase activity in the placenta. CreERTM/ROSA26 double transgenic placentas exhibited lacZ positive staining primarily in the chorionic plate and the umbilical vessels (Figure 1f). However, a limited number of cells in the labyrinthine layer showed lacZ staining. CreERTM/ROSA26 placentas from the corn oil injected (no Tam) female did not show any lacZ positive staining (Figure 1g). Depending upon the Cre transgene expression and the accessibility to tamoxifen, the Cre-mediated excision rate may be different for different organs. Based on these results, we decided to inject 2 mg of tamoxifen into pregnant females to induce CreERTM-mediated excision of the floxed VHL gene.
Tamoxifen-induced Cre excision of floxed allele in CreERTM/Rosa26 embryos. LacZ staining of the double transgenic CreERTM/Rosa26 embryos from a pregnant female injected with 2 mg tamoxifen is shown. Tamoxifen was injected at E10.5 and embryos were collected at E13.5 or E14.5. Positive lacZ staining was found in CreERTM/Rosa26 embryos (a), but not in Rosa26 littermate embryos (b). LacZ staining of the brain (c), heart (d), and liver (e) of the CreERTM/Rosa26 embryo. Mosaic pattern of lacZ staining represents mosaic deletion of floxed sequences by Cre recombinase. LacZ staining of the CreERTM/Rosa26 placentas from a tamoxifen treated female (f) and from an untreated female (no Tam, g). LacZ positive staining was seen in the chorionic plate of the placenta and the umbilical vessels (arrow). A mosaic pattern of lacZ staining was also seen in the yolk sac (asterisks). However, lacZ staining in the labyrinthine layer was limited. Placentas derived from corn oil injected females exhibited no lacZ positive staining. Tissue sections were counterstained with nuclear fast red.
Acute Inactivation of the VHL Gene Leads to Embryo Lethality
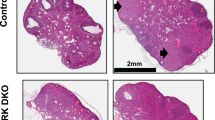
Previously, we developed mice harboring either a floxed or a deleted VHL allele by using genetically altered murine embryonic stem cells.13 The floxed VHL allele encodes the wild-type VHL protein but the deleted VHL allele does not produce functional protein.13 In this study, we generated VHLd/+/CreERTM mice and crossed them with VHLf/f mice to produce VHLf/d/CreERTM embryos. Based on the CreERTM/ROSA26 results, tamoxifen treatment was predicted to produce mosaically distributed VHL-inactivated (VHLd/d) cells in the VHLf/d/CreERTM embryos. In order to inactivate VHL during the mid-gestational stage, we injected 2 mg of tamoxifen into pregnant females at E10.5. At 6 days after tamoxifen injection (E16.5), embryos were collected and their morphological changes were noted. All the VHLf/d/CreERTM embryos were dead (8/8, Figure 2a), while their littermate controls showed normal development (7/7, Figure 2b). VHL inactivated embryos (VHLf/d/CreERTM) were smaller than their littermates and were pale. The diameter of the VHLf/d/CreERTM placenta was comparable to that of VHLf/+/CreERTM (Figure 2a and b). However, the thickness of the VHLf/d/CreERTM placenta, especially the labyrinthine layer, was reduced compared with littermate controls (Figure 2d and f). In addition, dilated blood vessels and spongiotrophoblast cells were frequently observed in the labyrinthine layer of the VHLf/d/CreERTM placenta (Figure 2g).
Embryonic lethality and abnormal placental development by the acute and mosaic inactivation of the VHL gene. Acute Cre-mediated excision of the VHL floxed allele by the administration of tamoxifen at E10.5 resulted in lethality of the embryos at E16.5. (a) All the VHL-inactivated VHLf/d/CreERTM embryos (8/8, from two litters) were found dead 6 days after tamoxifen administration, but (b) their littermate VHLf/+/CreERTM, VHLf/d, and VHLf/+ controls (7/7, from two litters) showed normal development. (c) Histological analysis of the VHL inactivated embryos showed extensive necrosis in the brain and other parts of the body. The placentas of the VHL inactivated embryos (f) showed a thinner labyrinthine layer (La) compared with their littermate controls (d). The labyrinthine layer of the VHL-inactivated placentas often showed dilated blood vessels (arrow heads) and spongiotrophoblast cells (asterisks) (g), whereas the controls showed well-organized vasculature (e). PCR genotyping of the DNAs from embryos and placentas (h) at E15.5. (*) indicates genotyping using tail DNA from a VHLf/d mouse. Southern blot analysis of HindIII digested mouse embryo and placental genomic DNA using a VHL probe (i and j). The VHL deleted allele (12.4 kb) was observed in the VHLf/+/CreERTM embryo treated with tamoxifen (i, lane 2), but was not detected in the VHLf/+/CreERTM placenta (i, lane 4). Tail genomic DNA from a VHLf/d mouse (i, lane 5) was used as a control. Decrease of floxed (flox) and increase of deleted (del) allele intensities were observed in tamoxifen treated VHLf/d/CreERTM embryos (j, lane 2, 3 and 4) compared with the allele intensities of the VHLf/d embryo (j, lane 1).
We measured the efficiency of VHL inactivation in the embryos and placentas by Southern blot analysis of genomic DNAs extracted from these tissues. We detected the deleted VHL allele in the VHLf/+/CreERTM embryos at about one third the band intensity of the floxed allele band (Figure 2i). By comparing the band intensity of the floxed VHL allele and the deleted VHL allele in the VHLf/d/CreERTM embryos, we determined that on average about 25% of the floxed alleles were converted to deleted alleles (Figure 2j), supporting a mosaic pattern of VHL inactivation in the embryos. On the other hand, the deleted VHL allele was barely detectable in the VHLf/+/CreERTM placenta suggesting that VHL inactivation occurred at a much lower frequency in placentas compared with embryos (Figure 2i).
Hemorrhage and Liver Necrosis in the VHL-Inactivated Embryos
To ascertain the cause of embryonic death, 64 embryos from a total of seven pregnant females were collected at different time points between E12.5 and E15.5 following tamoxifen-induced VHL inactivation at E10.5. Morphological changes in the VHLf/d/CreERTM embryos were observed from E13.5 (Figure 3a) and were distinct at E14.5 (Figure 3b), while littermate controls, including VHLf/+/CreERTM embryos, showed normal development (Figure 3e–h). Hemorrhage was found in the embryos at E14.5 and became extensive afterwards. All the affected embryos (12/12, 100%) died between E14.5 and E15.5 with severe hemorrhage in the dorsolateral region and extensive necrosis in the body (Figure 3c and d), while most of littermates showed normal development (22/24, 92%). The head and limbs of the affected embryos turned pale and blood circulation in the yolk sac was impaired at E14.7 indicating embryo death (Figure 3j and k). Corn oil injection without tamoxifen and low tamoxifen dosage (0.1 mg) did not result in pathological changes in VHLf/d/CreERTM embryos dissected at E15.5 (Figure 3i, 3/3) and E18.5 (4/4), respectively, or in littermate controls (Figure 3m, 13/13).
Time course experiment shows lethality of the VHL inactivated embryos between E14.5 and E15.0. Embryos were collected at different time points between E12.5 and E15.5 after tamoxifen (2 mg) injection of pregnant females at E10.5. No significant changes were observed in the VHLf/d/CreERTM embryos (a, 4/4 from two litters) before E14.5. Hemorrhage was observed in the VHLf/d/CreERTM embryos at E14.5 (b, 2/2 embryos) and became extensive at E14.7 (c, 5/5 embryos) and later (d, 7/7 embryos). All the VHLf/d/CreERTM embryos (12/12 embryos from four litters) were dead after E14.5. However, most of their littermate controls showed normal development (22/24 embryos from four litters, 92%). Blood circulation was normal in the VHLf/d/CreERTM yolk sac up to E14.5 (j), but was impaired at E14.7 (k) and later (l). The VHLf/+/CreERTM controls showed normal development (e–h) and normal blood circulation in the yolk sac (n–p). Higher magnification of the VHLf/d/CreERTM embryo at E14.7 showed abnormal vasculature in the body (box in c). Both VHLf/d/CreERTM and VHLf/+/CreERTM embryos at E15.5 from the tamoxifen untreated (corn oil only) females showed normal development (i and m, respectively).
Histological analysis of the VHL-inactivated embryos before death (E14.5) showed blood cell leakage from blood vessels, particularly in subcutaneous tissues, dilated blood vessels including blood vessels in the heart, and focal necrosis in the liver (Figure 4). However, we did not detect significant histological defects in the placenta of the affected embryos. The placental vasculature and labyrinthine layer thickness of the VHLf/d/CreERTM embryos were comparable to those of their littermate controls. To look for any changes in cell proliferation or cell death preceding embryonic death, we performed Ki-67 and TUNEL staining of the embryos at E14.5. We did not find significant increase in cell death or decrease in cell proliferation in the affected embryos (data not shown). Thus, it is likely that vascular leakage induced by VHL inactivation is a major cause of embryo death.
Histological analysis of the embryos showed hemorrhage, dilated blood vessels and necrotizing liver damage in the VHL-inactivated embryos. H&E staining of VHLf/d/CreERTM embryos (b, e, and h) and placenta (k) before embryo death (E14.5) and comparison with VHLf/+/CreERTM controls (a, d, g and j). Dilated blood vessels (arrow head), vascular lesion (arrow head) and blood cell leakage to surrounding tissues were often observed in the dorso-lateral region of the embryo (b and c). Focal necrotizing liver damage (asterisks in e and g), dilated blood vessels in heart (arrow head in h and i) and hemorrhage in the forebrain (white arrow in l) were observed. No significant developmental defects were observed in the VHLf/d/CreERTM placenta (k) compared with the VHLf/+/CreERTM placenta (j). VHL-inactivated embryo immediately following death (E14.7) displays large distended blood vessels (arrow heads in n) and hemorrhage (n) while the control (VHLf/+/CreERTM) shows normal development (m). Higher magnification of the spinal cords in ‘n’ reveals extensive necrosis (o).
We also inactivated VHL by tamoxifen injection to pregnant females at E9.0 and E12.5 to see the developmental stage specific effect of VHL-inactivation. Injection of 2 mg of tamoxifen was toxic to the embryos at E9.0 since 30% (4/12) of embryos showed lethality irrespective of their genotypes. When VHL was inactivated at E12.5 by injecting 2–4 mg of tamoxifen, we saw no pathological defects in dissected E17.5 or E18.5 VHLf/d/CreERTM embryos (3/3) or in the placentas. However, 5–6 mg of tamoxifen injection induced embryo lethality in all the VHLf/d/CreERTM embryos (4/4, 100%) at E17.5 or E18.5 and some of the control embryos (6/15, 40%). Gross morphological defects were also observed in the control embryos (2/15, 13%). Thus injection of high doses of tamoxifen at E12.5 induced toxicity to embryos.
Upregulation of HIF-1α and VEGF by the Inactivation of the VHL Gene
In order to study biochemical changes induced by homozygous VHL inactivation, we established and analyzed mouse embryo fibroblast (MEF) cell lines from E13.5 embryos harboring different VHL genotypes (VHLf/+, VHLf/+/CreERTM, VHLf/d and VHLf/d/CreERTM). During MEF cell culture, we inactivated the VHL gene in an acute manner in the VHLf/d/CreERTM cells by addition of 4-hydroxy tamoxifen (4OHT) to the culture media. The VHL gene was inactivated in more than 90% of the cells by the action of CreERTM recombinase after 3 days of culture with tamoxifen (Figure 5a). As a result of VHL inactivation, VHL protein and mRNA expression were greatly reduced (Figure 5c left panel). As expected, HIF-1α accumulated in the VHL-inactivated cells (Figure 5b). However, we could not detect HIF-2α in the MEFs (data not shown). HIF-1α accumulation resulted in upregulation of its downstream target, VEGF, in MEFs (Figure 5c right panel). Thus, we have established primary cells, in which the VHL gene could be inactivated in an acute manner by 4OHT providing an in vitro system for dissecting biochemical changes resulting from VHL inactivation.
VHL inactivation in MEFs. (a) The VHL gene was inactivated in VHLf/d/CreERTM MEFs but not control MEFs by addition of 4OHT (1 μM) as revealed by Southern blot analysis of the genomic tail DNA with a VHL-specific probe. (b) HIF-1α accumulated in the VHL inactivated MEFs. (c) VHL protein and mRNA expression were abolished and VEGF mRNA expression was induced by VHL inactivation. (d) Culture media was acidified upon inactivation of the VHL gene by 5–400 nM 4OHT treatment as indicated by the color change of the phenol red indicator in media. MEFs were plated on six-well plates (7 × 104 cells/well) and 4OHT was added 24 h later. Media color change was monitored 7 days after 4OHT treatment. (e) 24 h lactate accumulation in the culture media was measured 7 days after 4 OHT treatment and normalized to cell number as described in the Materials and methods. Lactate production (per 1 × 106 cells) was increased upon inactivation of VHL. (f) However cell growth, based on cell counts performed 7 days after 4OHT addition and normalized to untreated control cultures, was decreased upon VHL inactivation. (g) CAIX mRNA expression was induced by the inactivation of VHL as revealed by semi-quantitative RT-PCR. flox, floxed VHL allele; del, deleted VHL allele; +, wild-type.
Acidification of Culture Media by the Inactivation of the VHL Gene in the MEFs
We found that VHL inactivation of VHLf/d/CreERTM MEFs by 4OHT induced acidification of the culture media based on phenol red indicator color change observed 7 days after tamoxifen addition. However, the media pH of the control MEFs (VHLf/+/CreERTM) was maintained neutral with or without 4OHT treatment (Figure 5d). Upregulation of HIF mimics the hypoxic state, and glycolytic rate and lactate production were shown to be elevated in VHL−/− embryonic stem cells.16 As in the VHL−/− embryonic stem cells, lactate production was increased in MEFs with VHL inactivation (Figure 5e). Lactate production was not related to increased cell growth of the VHL-inactivated MEFs. Cell growth, determined by cell count 7 days after tamoxifen treatment, was actually decreased by VHL inactivation (Figure 5f). Decreased cell growth of the VHL−/− MEFs has also been reported.24 In addition to lactate production, the expression of CAIX, which regulates extracellular pH and is a target gene of HIF, was increased after VHL inactivation in the MEFs (Figure 5g).
Discussion
In this study, we inactivated the VHL gene at the mid-gestational stage of embryogenesis using a tamoxifen-inducible CreERTM system to avoid the early embryo lethality (E10.5–E12.5) seen in conventional VHL-KO mouse models. The conventional VHL-KO mouse reported by Gnarra et al18 died during early embryogenesis due to placental defects. Using the inducible CreERTM system, we have overcome early embryonic lethality by inactivating the VHL gene at mid-gestation (E10.5), circumventing early placental defects, and have observed the effect of VHL inactivation specifically in the embryos at E14.5 or later.
We saw differential effects of tamoxifen-induced VHL inactivation in the embryo and in the placenta. Although we observed dramatic pathological changes in the embryos, we were unable to detect gross placental defects at the time of embryo death. One possible explanation is the restricted Cre recombinase expression in the placenta. Cre recombinase activity was primarily observed in the chorionic plate and umbilical vessels, and was nearly absent from the labyrinthine layer (Figure 1f), where VHL expression was high.18 In support of these observations the overall VHL-allele excision rate was much lower in the placenta compared with the embryo (Figure 2i). Thus, the phenotypes in the embryos most likely resulted from inactivation of the VHL gene in the embryo rather than from the indirect effect of VHL inactivation in the placenta. However, we cannot completely exclude possible involvement of the placenta in the defects of the embryos. Although we could not observe significant pathological changes at the time of embryo death, dilated blood vessels were often observed in the labyrinthine layer in the VHL-inactivated placenta at E16.5 (Figure 2g). Thus, it is likely that the limited effect of VHL-inactivation on the placenta at the time of embryo death becomes more pronounced later following a longer duration of time.
As in the conventional VHL-KO mouse model, VHL inactivation at mid-gestation led to embryonic death. However, in contrast to the conventional mouse model, VHL-inactivation at mid-gestation delayed embryo death until E14.5 and caused extensive hemorrhage, vascular defects and liver damage in the embryos but did not cause placental defects prior to embryo death. The technical improvement provided by the inducible CreERTM system allowed us to evaluate for the first time specific VHL-null-associated defects observed in the mid-gestational stage embryos. As with the VHL gene, inactivation of a number of genes has been found to cause early embryo lethality. Therefore, it is difficult to study the function of these genes at later stages of embryo development. However, as we report in this study, early embryonic lethality may be overcome by inactivating the gene of interest at mid-gestation through the use of inducible Cre/lox technology. To our knowledge, this is the first study showing the application of the CreERTM system to the analysis of a gene's function during embryogenesis. We found the CreERTM system to be useful for the study of genes, specifically VHL, which cause embryonic lethality when inactivated in mice.
In addition, we established MEF cell lines, in which the VHL gene could be inactivated in an acute manner. In vitro analysis of the VHL-null MEFs revealed HIF-1α accumulation and VEGF overproduction. We also could observe metabolic and physiological changes in the VHL-null MEFs. VHL-null MEFs produced more lactate, indicating increased glycolysis, and overexpressed CAIX, which contributed to acidification of the culture media. The biochemical analyses of the VHL-inactivated MEFs provide indirect evidence that the VHL gene plays an important role in the maintenance of vascular structure and integrity, and in protecting against liver damage during embryogenesis by regulating HIF-1α and its target genes. However, a more direct way to test whether the highly vascular phenotype in the VHL-inactivated embryos is a consequence of HIFα activation would be to perform these experiments in a conditional VHL knockout mouse model in which HIF activation was conditionally suppressed during VHL inactivation and observe the subsequent effects on the vascular phenotype.
VEGF, one of the most studied targets of HIF, is a key regulator of vasculogenesis, angiogenesis, hematopoiesis and recruitment of leukocytes to inflammation sites.25 The VEGF gene family consists of at least five members, including VEGF-A, VEGF-B, VEGF-C, VEGF-D and placental growth factor (PlGF). These ligands bind distinct receptor tyrosine kinases, including VEGFR-1 (Flt-1), VEGFR-2 (Flk-1/KDR), VEGFR-3 (Flt-4) and Neuropilin-1. VEGF receptors are expressed by both hematopoietic stem cells and angioblasts, which are precursors of blood cells and endothelial cells, respectively. VEGF signaling was shown to be critical to both hematopoiesis and vasculogenesis in studies with knockout mouse models of the ligand and its receptors. Embryos heterozygous for the VEGF gene die in utero between E11 and E12 showing defective vascular development and reduced blood cells within the blood island in the yolk sac.26, 27 Gene targeting of the VEGFR-2 displayed a phenotype similar to the VEGF mutant with almost complete lack of endothelial cells and hematopoietic cells.28
In this study, we inactivated the VHL gene at mid-gestation (E10.5) in an acute manner. Vasculogenesis and hematopoiesis begin as early as E7.5 and blood circulation in the embryo and yolk sac can be seen from E9.0. During mid-gestation the pre-existing vasculature, through which nutrients and oxygen are supplied to the developing embryo, becomes extensive by means of active angiogenesis. VHL inactivation at mid-gestation affected vascular stability and vascular structure in the developing embryos. VEGF, known as vascular permeability factor (VPF), increases vascular permeability during pathogenic blood vessel growth.29 Increased permeability leads to leakage of small and large molecules, and often blood cells, into adjacent tissues. Hemorrhage is a consequence of blood cell leakage from blood vessels. Thus, the extensive hemorrhage of the VHL-inactivated embryos is most likely a result of increased vascular permeability by overproduced VEGF. The dilated blood vessels and disorganized vasculature are also probable consequences of uncontrolled growth of endothelial cells by overproduced VEGF.
In addition to the vascular phenotype, we observed focal liver damage in the developing embryos after VHL inactivation. Such localized focal damage can be explained by the low Cre activity seen in the liver of the CreERTM/ROSA26 transgenic embryos. During embryogenesis, hematopoiesis shifts from yolk sac to liver by E11.5. Thus, fetal liver generates blood cells as well as hepatocytes. As VEGF receptors are expressed by hematopoietic stem cells, it is intriguing to consider whether unbalanced production of VEGF induces this phenotype through VEGF signaling. We cannot rule out the possibility that other HIF-regulated cytokines, such as EPO, PDGF and TGF-α, are involved in liver damage. Of note, VHL heterozygous null mice develop hemangiomas in the liver spontaneously.12, 13 Thus, the liver appears to be the organ most susceptible to VHL inactivation.
A common characteristic of tumors is their acidic environment. It has been shown that the low pH of the tumor environment is caused by excessive lactate production in tumor cells as well as by hydration of CO2 to carbonic acid by carbonic anhydrase. As glycolysis is a dominating metabolic pathway in cancer cells, lactate is produced even under aerobic conditions. Generally tumors are in a hypoxic state, in which the glycolytic rate is increased by upregulation of the expression of glycolytic enzymes. CAIX and CAXII are induced by hypoxia.8 HIF is responsible for the expression of glycolytic enzymes and carbonic anhydrases under hypoxic conditions. Thus, acidification of culture media by VHL inactivation is regarded as a consequence of HIF stabilization in the MEFs caused by lactate overproduction and increased CAIX expression in these VHL-inactivated MEFs.
The results of our study support a role for the VHL gene in maintenance of vascular integrity and protecting liver function for hematopoeisis during mouse embryogenesis. This report is the first to provide a functional analysis of the VHL gene in the embryo during development. As many pathological processes involve increased vascular permeability and angiogenesis, our study suggests a possible involvement of the VHL gene in those processes. This inducible VHL-inactivation system should prove useful as an in vivo model for evaluating drugs that can inhibit vascular permeability and/or target HIF and HIF-regulated genes such as VEGF.
References
Maher ER, Bentley E, Yates JR, et al. Mapping of the von Hippel-Lindau disease locus to a small region of chromosome 3p by genetic linkage analysis. Genomics 1991;10:957–960.
Latif F, Tory K, Gnarra J, et al. Identification of the von Hippel-Lindau disease tumor suppressor gene. Science 1993;260:1317–1320.
Iliopoulos O, Levy AP, Jiang C, et al. Negative regulation of hypoxia-inducible genes by the von Hippel-Lindau protein. Proc Natl Acad Sci USA 1996;93:10595–10599.
Maxwell PH, Wiesener MS, Chang GW, et al. The tumour suppressor protein VHL targets hypoxia-inducible factors for oxygen-dependent proteolysis. Nature 1999;399:271–275.
Clifford SC, Cockman ME, Smallwood AC, et al. Contrasting effects on HIF-1alpha regulation by disease-causing pVHL mutations correlate with patterns of tumourigenesis in von Hippel-Lindau disease. Hum Mol Genet 2001;10:1029–1038.
Flamme I, Krieg M, Plate KH . Up-regulation of vascular endothelial growth factor in stromal cells of hemangioblastomas is correlated with up-regulation of the transcription factor HRF/HIF-2alpha. Am J Pathol 1998;153:25–29.
Pioli PA, Rigby WF . The von Hippel-Lindau protein interacts with heteronuclear ribonucleoprotein a2 and regulates its expression. J Biol Chem 2001;276:40346–40352.
Ivanov S, Liao SY, Ivanova A, et al. Expression of hypoxia-inducible cell-surface transmembrane carbonic anhydrases in human cancer. Am J Pathol 2001;158:905–919.
Hoffman MA, Ohh M, Yang H, et al. von Hippel-Lindau protein mutants linked to type 2C VHL disease preserve the ability to downregulate HIF. Hum Mol Genet 2001;10:1019–1027.
Hergovich A, Lisztwan J, Barry R, et al. Regulation of microtubule stability by the von Hippel-Lindau tumour suppressor protein pVHL. Nat Cell Biol 2003;5:64–70.
Semenza GL . Targeting HIF-1 for cancer therapy. Nat Rev Cancer 2003;3:721–732.
Haase VH, Glickman JN, Socolovsky M, et al. Vascular tumors in livers with targeted inactivation of the von Hippel-Lindau tumor suppressor. Proc Natl Acad Sci USA 2001;98:1583–1588.
Ma W, Tessarollo L, Hong SB, et al. Hepatic vascular tumors, angiectasis in multiple organs, and impaired spermatogenesis in mice with conditional inactivation of the VHL gene. Cancer Res 2003;63:5320–5328.
Biju MP, Neumann AK, Bensinger SJ, et al. Vhlh gene deletion induces Hif-1-mediated cell death in thymocytes. Mol Cell Biol 2004;24:9038–9047.
Pfander D, Kobayashi T, Knight MC, et al. Deletion of Vhlh in chondrocytes reduces cell proliferation and increases matrix deposition during growth plate development. Development 2004;131:2497–2508.
Mack FA, Rathmell WK, Arsham AM, et al. Loss of pVHL is sufficient to cause HIF dysregulation in primary cells but does not promote tumor growth. Cancer Cell 2003;3:75–88.
Rathmell WK, Hickey MM, Bezman NA, et al. In vitro and in vivo models analyzing von Hippel-Lindau disease-specific mutations. Cancer Res 2004;64:8595–8603.
Gnarra JR, Ward JM, Porter FD, et al. Defective placental vasculogenesis causes embryonic lethality in VHL-deficient mice. Proc Natl Acad Sci USA 1997;94:9102–9107.
Guo C, Yang W, Lobe CG . A Cre recombinase transgene with mosaic, widespread tamoxifen-inducible action. Genesis 2002;32:8–18.
Soriano P . Generalized lacZ expression with the ROSA26 Cre reporter strain. Nat Genet 1999;21:70–71.
Lin CY, Chen SH, Kou GH, et al. An enzymatic microassay for lactate concentration in blood and hemolymph. Acta Zool Taiwan 1999;10:91–101.
Rozen S, Skaletsky H . Primer3 on the WWW for general users and for biologist programmers. Methods Mol Biol 2000;132:365–386.
Boley SE, Wong VA, French JE, et al. p53 heterozygosity alters the mRNA expression of p53 target genes in the bone marrow in response to inhaled benzene. Toxicol Sci 2002;66:209–215.
Mack FA, Patel JH, Biju MP, et al. Decreased growth of Vhl−/− fibrosarcomas is associated with elevated levels of cyclin kinase inhibitors p21 and p27. Mol Cell Biol 2005;25:4565–4578.
Ferrara N . Molecular and biological properties of vascular endothelial growth factor. J Mol Med 1999;77:527–543.
Carmeliet P, Ferreira V, Breier G, et al. Abnormal blood vessel development and lethality in embryos lacking a single VEGF allele. Nature 1996;380:435–439.
Ferrara N, Carver-Moore K, Chen H, et al. Heterozygous embryonic lethality induced by targeted inactivation of the VEGF gene. Nature 1996;380:439–442.
Shalaby F, Rossant J, Yamaguchi TP, et al. Failure of blood-island formation and vasculogenesis in Flk-1-deficient mice. Nature 1995;376:62–66.
Bates DO, Harper SJ . Regulation of vascular permeability by vascular endothelial growth factors. Vascul Pharmacol 2002;39:225–237.
Acknowledgements
This publication has been funded in whole or in part with federal funds from the National Cancer Institute, National Institutes of Health, under contract N01-CO-12400. The content of this publication does not necessarily reflect the views or policies of the Department of Health and Human Services, nor does mention of trade names, commercial products, or organizations imply endorsement by the US Government. This research was supported in part by the Intramural Research Program of the NIH, National Cancer Institute, Center for Cancer Research. NCI-Frederick is accredited by AAALAC International and follows the Public Health Service Policy for the Care and Use of Laboratory Animals. Animal care was provided in accordance with the procedures outlined in the ‘Guide for the Care and Use of Laboratory Animals’ (National Research Council; 1996; National Academy Press; Washington, DC).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Hong, SB., Furihata, M., Baba, M. et al. Vascular defects and liver damage by the acute inactivation of the VHL gene during mouse embryogenesis. Lab Invest 86, 664–675 (2006). https://doi.org/10.1038/labinvest.3700431
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/labinvest.3700431
Keywords
This article is cited by
-
Endothelial cells by inactivation of VHL gene direct angiogenesis, not vasculogenesis via Twist1 accumulation associated with hemangioblastoma neovascularization
Scientific Reports (2017)
-
Complex cellular functions of the von Hippel–Lindau tumor suppressor gene: insights from model organisms
Oncogene (2012)
-
Increased expression of the von Hippel–Lindau gene in the implantation site of human tubal pregnancy
Molecular and Cellular Biochemistry (2012)
-
Uncoupling hypoxia signaling from oxygen sensing in the liver results in hypoketotic hypoglycemic death
Oncogene (2011)
-
The VHL-dependent regulation of microRNAs in renal cancer
BMC Medicine (2010)