Abstract
Objective:
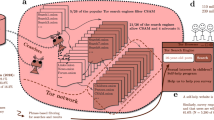
This study examined whether adopting a standardized prenatal substance use protocol (protocol) in a hospital labor and delivery unit reduced racial disparities in reporting to child protective services (CPS) related to maternal drug use during pregnancy.
Study design:
This study used an interrupted time series design with a non-equivalent control. One hospital adopted a protocol and another hospital group serving a similar geographic population did not change protocols. Data on CPS reporting disparities from these hospitals over 3.5 years were analyzed using segmented regression.
Result:
In the hospital that adopted the protocol, almost five times more black than white newborns were reported during the study period. Adopting the protocol was not associated with reduced disparities.
Conclusion:
Adopting a protocol cannot be assumed to reduce CPS reporting disparities. Efforts to encourage hospitals to adopt protocols as a strategy to reduce disparities may be misguided. Other strategies to reduce disparities are needed.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Neuspiel DR, Zingman TM, Templeton VH, DiStabile P Drucker E . Custody of cocaine-exposed newborns: determinants of discharge decisions. Am J Public Health 1993; 83 (12): 1726–1729.
Chasnoff IJ, Landress HJ Barrett ME . The prevalence of illicit-drug or alcohol use during pregnancy and discrepancies in mandatory reporting in Pinellas County, Florida. N Engl J Med 1990; 322 (17): 1202–1206.
Roberts SC, Nuru-Jeter A . Universal screening for alcohol and drug use and racial disparities in child protective services reporting. J Behav Health Serv Res 2012; 39 (1): 3–16.
Osterling KL, D’Andrade A, Austin MJ . Understanding and addressing racial/ethnic disproportionality in the front end of the child welfare system. J Evid Based Soc Work 2008; 5 (1-2): 9–30.
Nair P, Schuler ME, Black MM, Kettinger L, Harrington D . Cumulative environmental risk in substance abusing women: early intervention, parenting stress, child abuse potential and child development. Child Abuse Negl 2003; 27 (9): 997–1017.
Mikton C, Butchart A . Child maltreatment prevention: a systematic review of reviews. Bull World Health Organ 2009; 87 (5): 353–361.
McCann KJ, Twomey JE, Caldwell D, Soave R, Fontaine LA, Lester BM . Services used by perinatal substance-users with child welfare involvement: a descriptive study. Harm Reduct J 2010; 7: 19.
Jansson LM, Svikis DS, Beilenson P . Effectiveness of child case management services for offspring of drug-dependent women. Subst Use Misuse 2003; 38 (14): 1933–1952.
Roberts SC, Pies C . Complex calculations: how drug use during pregnancy becomes a barrier to prenatal care. Matern Child Health J 2011; 15 (3): 333–341.
PSAP. Making Change Happen: A Year in Review. http://cchealth.org/psap/pdf/2008_annual_report.pdf. CCHS (ed). Perinatal Substance Abuse Partnership: Martinez, CA, 2008.
Drescher-Burke K, Price A . Identifying, Reporting, and Responding to Substance Exposed Newborns: An Exploratory Study of Policies and Practices. National Abandoned Infants Assistance Resource Center, University of California at Berkeley: Berkeley, CA, 2005.
California Department of Alcohol and Drug Problems. Fact Sheet: Substance Exposed Infants (Senate Bill 2669) 2006.
Albert V, Klein D, Noble A, Zahnd E, Holtby S . Identifying substance abusing delivering women: consequences for child maltreatment reports. Child Abuse Negl 2000; 24 (2): 173–183.
Zellman GL, Fair C, Hoube J, Wong M . A search for guidance: examining prenatal substance exposure protocols. Matern Child Health J 2002; 6 (3): 205–212.
Ellsworth MA, Stevens TP, D’Angio CT . Infant race affects application of clinical guidelines when screening for drugs of abuse in newborns. Pediatrics 2010; 125 (6): e1379–e1385.
Keppel K, Bilheimer L, Gurley L . Improving population health and reducing health care disparities. Health Aff (Millwood) 2007; 26 (5): 1281–1292.
Roberts SC, Nuru-Jeter A . Universal alcohol/drug screening in prenatal care: a strategy for reducing racial disparities? Questioning the assumptions. Matern Child Health J 2011; 15 (8): 1127–1134.
Oral R, Strang T . Neonatal illicit drug screening practices in Iowa: the impact of utilization of a structured screening protocol. J Perinatol 2006; 26 (11): 660–666.
Shadish WR, Cook TD, Campbell DT . Experimental and Quasi-Experimental Designs for Generalized Causal Inference. Houghton Mifflin Company: New York, 2002.
Hospital protocol for evaluating and reporting cases involving prenatal drug/alcohol exposure. Retrieved on 6 February 2014 from http://ican4kids.org/documents/CANProtocol/ap15.Hospital.pdf. Los Angeles, CA, 2009.
Census US. 2012 Community Survey 1-Year Estimates. Retrieved on 16 July 2014 from http://www.census.gov/acs/www/.
Harper S, Lynch J, Meersman SC, Breen N, Davis WW, Reichman ME . An overview of methods for monitoring social disparities in cancer with an example using trends in lung cancer incidence by area-socioeconomic position and race-ethnicity, 1992-2004. Am J Epidemiol 2008; 167 (8): 889–899.
Wagner AK, Soumerai SB, Zhang F, Ross-Degnan D . Segmented regression analysis of interrupted time series studies in medication use research. J Clin Pharm Ther 2002; 27 (4): 299–309.
Zhang F, Wagner AK, Ross-Degnan D . Simulation-based power calculation for designing interrupted time series analyses of health policy interventions. J Clin Epidemiol 2011; 64 (11): 1252–1261.
Roberts DE . Shattered Bonds: The Color of Child Welfare. Basic Books: New York, 2002.
Martin JA . Preterm births—United States, 2007. MMWR Morb Mortal Wkly Rep 2011; 60 (01): 78–79.
Alexander GR, Kogan MD, Nabukera S . Racial differences in prenatal care use in the United States: are disparities decreasing? Am J Public Health 2002; 92 (12): 1970–1975.
Roberts DE . Killing the black Body: Race, Reproduction, and the Meaning of Liberty. Vintage: New York, 1999.
MacMahon JR . Perinatal substance abuse: the impact of reporting infants to Child Protective Services. Pediatrics 1997; 100 (5): E1.
Roberts SC . Re-contextualizing Universal Screening for Alcohol and Drug Use in Prenatal Care: The (Not So) Hidden Connections Between Universal Screening and Reporting to Child Protective Services. University of California, Berkeley: Berkeley, CA, 2009.
Kerker BD, Horwitz SM, Leventhal JM . Patients’ characteristics and providers’ attitudes: predictors of screening pregnant women for illicit substance use. Child Abuse Negl 2004; 28 (2): 209–223.
Kerker BD, Leventhal JM, Schlesinger M, Horwitz SM . Racial and ethnic disparities in medical history taking: detecting substance use among low-income pregnant women. Ethn Dis 2006; 16 (1): 28–34.
Petrini J, Damus K, Roy S, Johnson K Johnston RB Jr . The effect of using ‘race of child’ instead of ‘race of mother’ on the black-white gap in infant mortality due to birth defects. Public Health Rep 1998; 113 (3): 263–267.
Acknowledgements
This study was supported by a grant from the University of California, San Francisco’s Academic Senate Committee on Research.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Roberts, S., Zahnd, E., Sufrin, C. et al. Does adopting a prenatal substance use protocol reduce racial disparities in CPS reporting related to maternal drug use? A California case study. J Perinatol 35, 146–150 (2015). https://doi.org/10.1038/jp.2014.168
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jp.2014.168
This article is cited by
-
The Government’s Involvement in Prenatal Drug Testing May Be Toxic
Maternal and Child Health Journal (2022)
-
Black Women’s Perspectives on Structural Racism across the Reproductive Lifespan: A Conceptual Framework for Measurement Development
Maternal and Child Health Journal (2021)