Abstract
Objective:
The relationship between weight status, adenotonsillar hypertrophy and obstructive sleep apnea (OSA) in children has not yet been well studied. As the sleep parameters may show a disparity in different weight statuses, this study examined the relationship between the data of over-night polysomnography and different weight statuses, as well as the impact of adenotonsillar hypertrophy on children with OSA.
Methods:
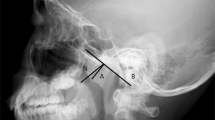
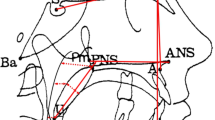
Children with sleep disturbances were recruited from our clinics. Standard physical examinations, history taking, lateral neck roentgenography, and full-night polysomnography were obtained. Children were divided into four groups based on the age- and gender-corrected body mass index (BMI): underweight, normal weight, overweight and obese. An adenoidal/nasopharyngeal ratio of more than 0.67 was considered adenoidal hypertrophy. Tonsillar hypertrophy was defined as having Grade III tonsils or above.
Results:
From July 2006 to January 2009, 197 children were included in this study. Obese children had a significantly higher apnea–hypopnea index (AHI), obstructive apnea index and lower minimum oxygen saturation (MinSaO2) than those of the other groups. Underweight children had the second highest AHI. A negative correlation was also found between BMI z scores and MinSaO2 (r=−0.194; P=0.007). Children with tonsillar hypertrophy (P=0.001) were associated with a higher risk of having OSA. The risk of having OSA was significantly higher in obese children (P=0.001) and underweight children (P=0.043) than in those with a normal weight.
Conclusion:
Obesity, underweight status and tonsillar hypertrophy are associated with children having OSA, and obese children have a significantly higher risk than children with underweight status.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Ebbeling CB, Pawlak DB, Ludwig DS . Childhood obesity: public-health crisis, common sense cure. Lancet 2002; 360: 473–482.
Lobstein T . Obesity in children and young people: a crisis in public health. Obes Rev 2004; 5 (s1): 4–85.
American Thoracic Society. Standards and indications for cardiopulmonary sleep studies in children. Am J Respir Crit Care Med 1996; 153: 866–878.
Schechter MS . Technical report: diagnosis and management of childhood obstructive sleep apnea syndrome. Pediatrics 2002; 109: e69.
American Academy of Pediatrics. Section on Pediatric Pulmonology, Subcommittee on Obstructive Sleep Apnea Syndrome. Clinical practice guideline: diagnosis and management of childhood obstructive sleep apnea syndrome. Pediatrics 2002; 109: 704–712.
Arens R, Marcus CL . Pathophysiology of upper airway obstruction: a developmental perspective. Sleep 2004; 27: 997–1019.
Redline S, Tishler PV, Schluchter M, Aylor J, Clark K, Graham G . Risk factors for sleep-disordered breathing in children: associations with obesity, race, and respiratory problems. Am J Respir Crit Care Med 1999; 159: 1527–1532.
Marcus CL, Carroll JL, Koerner CB, Hamer A, Lutz J, Loughlin GM . Determinants of growth in children with the obstructive sleep apnea syndrome. J Pediatr 1994; 125: 556–562.
Isono S, Shimada A, Utsugi M, Konno A, Nishino T . Comparison of static mechanical properties of the passive pharynx between normal children and children with sleep-disordered breathing. Am J Respir Crit Care Med 1998; 157: 1204–1212.
Brodsky L, Moore L, Stanievich JF . A comparison of tonsillar size and oropharyngeal dimensions in children with obstructive adenotonsillar hypertrophy. Int J Pediatr Otorhinolaryngol 1987; 13: 149–156.
Kemaloglu YK, Goksu N, Inal E, Akyildiz N . Radiographic evaluation of children with nasopharyngeal obstruction due to the adenoid. Ann Otol Rhinol Laryngol 1999; 108: 67–72.
Major MP, Flores-Mir C, Major PW . Assessment of lateral cephalometric diagnosis of adenoid hypertrophy and posterior upper airway obstruction: a systematic review. Am J Orthod Dentofacial Orthop 2006; 130: 700–708.
Huang YC . Body mass index reference for Taiwanese children and adolescents. J Med Sci 2002; 22: 221–226.
Roure N, Gomez S, Mediano O, Duran J, Pena Mde L, Capote F et al. Daytime sleepiness and polysomnography in obstructive sleep apnea patients. Sleep Med 2008; 9: 727–731.
Rechtschaffen A, Kales A . A Manual of Standardized Terminology, Techniques and Scoring System for Sleep Stages of Human Subjects. UCLA Brain Information Service/Brain Research Institute: Los Angeles, 1968.
Kushida CA, Littner MR, Morgenthaler T, Alessi CA, Bailey D, Coleman J et al. Practice parameters for the indications for polysomnography and related procedures: an update for 2005. Sleep 2005; 28: 499–521.
Lee P, Su YN, Yu CJ, Yang PC, Wu HD . Phox2b mutation-confirmed congenital central hypoventilation syndrome in a Chinese family: Presentation from newborn to adulthood. Chest 2009; 135: 537–544.
Gozal D . Sleep-disordered breathing and school performance in children. Pediatrics 1998; 102: 616–620.
Malhotra A, Huang Y, Fogel RB, Pillar G, Edwards JK, Kikinis R et al. The male predisposition to pharyngeal collapse: importance of airway length. Am J Respir Crit Care Med 2002; 166: 1388–1395.
Ronen O, Malhotra A, Pillar G . Influence of gender and age on upper-airway length during development. Pediatrics 2007; 120: e1028–e1034.
Lin CM, Davidson TM, Ancoli-Israel S . Gender differences in obstructive sleep apnea and treatment implications. Sleep Med Rev 2008; 12: 481–496.
Tsai HH, Ho CY, Lee PL, Tan CT . Sex differences in anthropometric and cephalometric characteristics in the severity of obstructive sleep apnea syndrome. Am J Orthod Dentofacial Orthop 2009; 135: 155–164.
Lumeng JC, Chervin RD . Epidemiology of pediatric obstructive sleep apnea. Proc Am Thorac Soc 2008; 5: 242–252.
Wing YK, Hui SH, Pak WM, Ho CK, Cheung A, Li AM et al. A controlled study of sleep related disordered breathing in obese children. Arch Dis Child 2003; 88: 1043–1047.
Sardon O, Perez-Yarza EG, Aldasoro A, Bordoy A, Mintegui J, Emparanza JI . Obstructive sleep apnea-hypopnea syndrome in children is not associated with obesity. Arch Bronconeumol 2006; 42: 583–587.
Xu Z, Jiaqing A, Yuchuan L, Shen K . A case-control study of obstructive sleep apnea-hypopnea syndrome in obese and nonobese Chinese children. Chest 2008; 133: 684–689.
Friedman M, Wilson M, Lin HC, Chang HW . Updated systematic review of tonsillectomy and adenoidectomy for treatment of pediatric obstructive sleep apnea/hypopnea syndrome. Otolaryngol Head Neck Surg 2009; 140: 800–808.
Tauman R, Gulliver TE, Krishna J, Montgomery-Downs HE, O’Brien LM, Ivanenko A et al. Persistence of obstructive sleep apnea syndrome in children after adenotonsillectomy. J Pediatr 2006; 149: 803808.
Guilleminault C, Huang Y, Glamann C, Li KK, Chan A . Adenotonsillectomy and obstructive sleep apnea in children: a prospective survey. Otolaryngol Head Neck Surg 2007; 136: 169–175.
Acknowledgements
We thank the staff of the Center of Sleep Disorder, National Taiwan University Hospital for their technical support.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Kang, KT., Lee, PL., Weng, WC. et al. Body weight status and obstructive sleep apnea in children. Int J Obes 36, 920–924 (2012). https://doi.org/10.1038/ijo.2012.5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ijo.2012.5
Keywords
This article is cited by
-
Analyzing sleep status in children with acute leukemia
Italian Journal of Pediatrics (2023)
-
Obstructive sleep apnea (OSA) is associated with the impairment of beta-cell response to glucose in children and adolescents with obesity
International Journal of Obesity (2023)
-
Analysis of possible risk factors for the severity of paediatric obstructive sleep apnoea syndrome
European Archives of Oto-Rhino-Laryngology (2023)
-
The association between obesity and hyperactivity/anxiety among elementary school students in Japan
International Journal of Behavioral Medicine (2020)
-
Correlations between obstructive sleep apnea and adenotonsillar hypertrophy in children of different weight status
Scientific Reports (2019)