Abstract
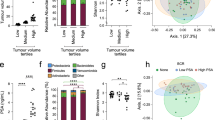
Benign prostatic hyperplasia (BPH) is the most common urologic disease in men over age 50. Symptoms include acute urinary retention, urgency to urinate and nocturia. For patients with severe symptoms, surgical treatment is used to remove the affected tissue. Interestingly, the presence of histologic BPH does not always correlate with symptoms. The molecular basis of symptomatic BPH and how it differs from asymptomatic BPH is unknown. Investigation into the molecular players involved in symptomatic BPH will likely give insight into novel therapeutic, and potentially preventative, targets. We determined the expression of genes involved in the innate anti-viral immune response in tissues from patients undergoing surgery to alleviate the symptoms of BPH, and compared the results with prostate tissue with histologic BPH, but from patients with few urinary issues (asymptomatic BPH). We found that expression of complement factor I, apolipoprotein B mRNA-editing enzyme, catalytic polypeptide-like protein 3G, oligoadenylate synthetase 2 and interferon-induced tetratricopeptide 1, four genes whose protein products are involved in the innate anti-viral immune response, was significantly transcriptionally upregulated in symptomatic BPH. Additionally, we observe hypomethylation and concomitant expression of ancient retroviral-like sequences, the long interspersed nuclear element 1 retrotransposons, in symptomatic BPH when compared with normal prostate tissue. These findings merit further investigation into the anti-viral immune response in symptomatic BPH.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 6 digital issues and online access to articles
$119.00 per year
only $19.83 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
References
Saigal CS, Joyce G . Economic costs of benign prostatic hyperplasia in the private sector. J Urol 2005; 173: 1309–1313.
Blanker MH, Bohnen AM, Groeneveld FP, Bernsen RM, Prins A, Ruud Bosch JL . Normal voiding patterns and determinants of increased diurnal and nocturnal voiding frequency in elderly men. J Urol 2000; 164: 1201–1205.
Ventura S, Oliver V, White CW, Xie JH, Haynes JM, Exintaris B . Novel drug targets for the pharmacotherapy of benign prostatic hyperplasia (BPH). Br J Pharmacol 2011; 163: 891–907.
Ropiquet F, Giri D, Lamb DJ, FGF7 Ittmann M . and FGF2 are increased in benign prostatic hyperplasia and are associated with increased proliferation. J Urol 1999; 162: 595–599.
Dong G, Rajah R, Vu T, Hoffman AR, Rosenfeld RG, Roberts CT et al. Decreased expression of Wilms’ tumor gene WT-1 and elevated expression of insulin growth factor-II (IGF-II) and type 1 IGF receptor genes in prostatic stromal cells from patients with benign prostatic hyperplasia. J Clin Endocrinol Metab 1997; 82: 2198–2203.
Nicholson TM, Ricke WA . Androgens and estrogens in benign prostatic hyperplasia: past, present and future. Differentiation 2011; 82: 184–199.
Schauer IG, Rowley DR . The functional role of reactive stroma in benign prostatic hyperplasia. Differentiation 2011; 82: 200–210.
Zhao H, Ramos CF, Brooks JD, Peehl DM . Distinctive gene expression of prostatic stromal cells cultured from diseased versus normal tissues. J Cell Physiol 2007; 210: 111–121.
Janeway C, Travers P, Walport M, Shlomchik M . Immunobiology, The Immune System in Health and Disease 5th edn Garland Science: New York, 2001.
Santourlidis S, Florl A, Ackermann R, Wirtz HC, Schulz WA . High frequency of alterations in DNA methylation in adenocarcinoma of the prostate. Prostate 1999; 39: 166–174.
Bhutani N, Burns DM, Blau HM . DNA demethylation dynamics. Cell 2011; 146: 866–872.
Chiu YL, Greene WC . APOBEC3G: an intracellular centurion. Philos Trans R Soc Lond B Biol Sci 2009; 364: 689–703.
Fensterl V, Sen GC . The ISG56/IFIT1 gene family. J Interferon Cytokine Res 2011; 31: 71–78.
Sahu A, Isaacs SN, Soulika AM, Lambris JD . Interaction of vaccinia virus complement control protein with human complement proteins: factor I-mediated degradation of C3b to iC3b1 inactivates the alternative complement pathway. J Immunol 1998; 160: 5596–5604.
Johnson JB, Grant K, Parks GD . The paramyxoviruses simian virus 5 and mumps virus recruit host cell CD46 to evade complement-mediated neutralization. J Virol 2009; 83: 7602–7611.
Mold C, Bradt BM, Nemerow GR, Cooper NR . Epstein-Barr virus regulates activation and processing of the third component of complement. J Exp Med 1988; 168: 949–969.
Okroj M, Hsu YF, Ajona D, Pio R, Blom AM . Non-small cell lung cancer cells produce a functional set of complement factor I and its soluble cofactors. Mol Immunol 2008; 45: 169–179.
Gasque P, Julen N, Ischenko AM, Picot C, Mauger C, Chauzy C et al. Expression of complement components of the alternative pathway by glioma cell lines. J Immunol 1992; 149: 1381–1387.
Minta JO, Fung M, Paramaswara B . Transcriptional and post-transcriptional regulation of complement factor I (CFI) gene expression in Hep G2 cells by interleukin-6. Biochim Biophys Acta 1998; 1442: 286–295.
Timár KK, Junnikkala S, Dallos A, Jarva H, Bhuiyan ZA, Meri S et al. Human keratinocytes produce the complement inhibitor factor I: Synthesis is regulated by interferon-gamma. Mol Immunol 2007; 44: 2943–2949.
Pichlmair A, Lassnig C, Eberle CA, Górna MW, Baumann CL, Burkard TR et al. IFIT1 is an antiviral protein that recognizes 5'-triphosphate RNA. Nat Immunol 2011; 12: 624–630.
Sutcliffe S, Rohrmann S, Giovannucci E, Nelson KE, De Marzo AM, Isaacs WB et al. Viral infections and lower urinary tract symptoms in the third national health and nutrition examination survey. J Urol 2007; 178: 2181–2185.
Breyer BN, Van den Eeden SK, Horberg MA, Eisenberg ML, Deng DY, Smith JF et al. HIV status is an independent risk factor for reporting lower urinary tract symptoms. J Urol 2011; 185: 1710–1715.
Mavragani CP, Crow MK . Activation of the type I interferon pathway in primary Sjogren's syndrome. J Autoimmun 2010; 35: 225–231.
Zisman A, Zisman E, Lindner A, Velikanov S, Siegel YI, Mozes E . Autoantibodies to prostate specific antigen in patients with benign prostatic hyperplasia. J Urol 1995; 154: 1052–1055.
Yang AS, Estécio MR, Doshi K, Kondo Y, Tajara EH, Issa JP . A simple method for estimating global DNA methylation using bisulfite PCR of repetitive DNA elements. Nucleic Acids Res 2004; 32: e38.
Acknowledgements
Thank you to Dr Saumendra Sarkar for helpful scientific discussion. Special thanks to Jennifer Gregg and Katherine Semmler for insightful suggestions. Thank you to the University of Pittsburgh HSTB for the symptomatic and asymptomatic BPH specimens. AAM and this work were funded by the T32 post-doctoral fellowship NIHT32DK007774. DOK, DJB and JLC are funded by NIHR01CA138444 and KMS by DOD Award PC101949. The US Army Medical Research Acquisition Activity, 820 Chandler Street, Fort Detrick MD 21702-5014 is the awarding and administering acquisition office. The content of this publication does not necessarily reflect the position or policy of the government, and no official endorsement should be inferred. This work was funded by the University of Pittsburgh Urologic Training Program for Scientists T32 5T32DK007774-12, Cancer Center Support Grant P30CA047904 and RO1CA138444.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies the paper on Genes and Immunity website
Supplementary information
Rights and permissions
About this article
Cite this article
Madigan, A., Sobek, K., Cummings, J. et al. Activation of innate anti-viral immune response genes in symptomatic benign prostatic hyperplasia. Genes Immun 13, 566–572 (2012). https://doi.org/10.1038/gene.2012.40
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/gene.2012.40