Abstract
The developmental origins of health disease (DOHaD) hypothesis proposes that altered environmental influences (nutrition, metabolism, pollutants, stress and so on) during critical stages of fetal growth predisposes individuals to diabetes and other non-communicable disease in later life. This phenomenon is thought to reflect permanent effects (‘programming’) of unbalanced fetal development on physiological systems. Intrauterine programming may underlie the characteristic Indian ‘thin–fat’ phenotype and the current unprecedented epidemic of diabetes on the backdrop of multigenerational maternal undernutrition in the country. India has been at the forefront of the DOHaD research for over two decades. Both retrospective and prospective birth cohorts in India provide evidence for the role of impaired early-life nutrition on the later diabetes risk. These studies show that in a transitioning country such as India, maternal undernutrition (of micronutrients) and overnutrition (gestational diabetes) co-exist, and expose the offspring to disease risk through multiple pathways. Currently, the Indian scientists are embarking on complex mechanistic and intervention studies to find solutions for the diabetes susceptibility of this population. However, a few unresolved issues in this context warrant continued research and a cautious approach.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Neel JV . Diabetes mellitus: a ‘thrifty’ genotype rendered detrimental by ‘progress’? Am J Hum Genetics 1962; 14: 353–362.
Banerji MA, Faridi N, Atluri R, Chaiken RL, Lebovitz HE . Body composition,visceral fat, leptin, and insulin resistance in Asian Indian men. J Clin Endocrinol Metab 1999; 84: 137–144.
Chandalia M, Abate N, Garg A, Stray-Gundersen J, Grundy SM . Relationship between generalized and upper body obesity to insulin resistance in Asian Indian men. J Clin Endocrinol Metab 1999; 84: 2329–2335.
Yajnik CS, Fall CHD, Coyaji KJ, Hirve SS, Rao S, Barker DJP et al. Neonatal anthropometry: the thin-fat Indian baby; the Pune Maternal Nutrition Study. Int J Obes Relat Metab Disord 2003; 27: 173–180.
Barker DJP . Mothers, babies and health in later life, 2nd edition. Churchill Livingstone: Edinburgh, UK, 1998.
Barker DJP, Hales CN, Fall CHD, Osmond C, Phipps K, Clark PMS . Type 2 (non-insulin-dependent) diabetes mellitus, hypertension and hyperlipidaemia (syndrome X): relation to reduced foetal growth. Diabetologia 1993; 36: 62–67.
Wells JC, Pomeroy E, Walimbe SR, Popkin BM, Yajnik CS . The elevated susceptibility to diabetes in india: an evolutionary perspective. Front Public Health 2016; 4: 145.
Yajnik CS, Fall CH, Vaidya U, Pandit AN, Bavdekar A, Bhat DS et al. Foetal growth and glucose and insulin metabolism in four-year old Indian children. Diabet Med 1995; 12: 330–336.
Bavdekar A, Yajnik CS, Fall CH, Bapat S, Pandit AN, Deshpande V et al. Insulin resistance syndrome in 8-year-old Indian children. Small at birth, Big at 8 years, or both? Diabetes 1999; 48: 2422–2429.
Joshi SM, Katre PA, Kumaran K, Joglekar C, Osmond C, Bhat DS et al. Tracking of cardiovascular risk factors from childhood to young adulthood - the Pune Children's Study. Int J Cardiol 2014; 175: 176–178.
Yajnik CS, Katre PA, Joshi SM, Kumaran K, Bhat DS, Lubree HG et al. Higher glucose, insulin and insulin resistance (HOMA-IR) in childhood predict adverse cardiovascular risk in early adulthood: the Pune Children's Study. Diabetologia 2015; 58: 1626–1636.
Bhargava SK, Sachdev HS, Fall CH, Osmond C, Lakshmy R, Barker DJ et al. Relation of serial changes in childhood body-mass-index to impaired glucose tolerance in young adulthood. N Engl J Med 2004; 350: 865–875.
Raghupathy P, Antonisamy B, Geethanjali FS, Saperia J, Leary SD, Priya G et al. Glucose tolerance, insulin resistance and insulin secretion in young south Indian adults: relationships to parental size, neonatal size and childhood body mass index. Diabetes Res Clin Pract 2010; 87: 283–292.
Fall CHD, Stein CE, Kumaran K, Cox V, Osmond C, Barker DJ et al. Size at birth, maternal weight, and non-insulin-dependent diabetes (NIDDM) in South Indian adults. Diabet Med 1998; 15: 220–227.
Yada KK, Gupta R, Gupta A, Gupta M . Insulin levels in low birth weight neonates. Indian J Med Res 2003; 118: 197–203.
Rao S, Yajnik CS, Kanade A, Fall CH, Margetts BM, Jackson AA et al. Intake of micronutrient-rich foods in rural Indian mothers is associated with the size of their babies at birth: Pune Maternal Nutrition Study. J Nutr 2001; 131: 1217–1224.
Yajnik CS, Deshpande SS, Jackson AA, Refsum H, Rao S, Fisher DJ et al. Vitamin B12 and folate concentrations during pregnancy and insulin resistance in the offspring: the Pune Maternal Nutrition Study. Diabetologia 2008; 51: 29–38.
Yajnik CS, Chandak GR, Joglekar C, Katre P, Bhat DS, Singh SN et al. Maternal homocysteine in pregnancy and offspring birthweight: epidemiological associations and Mendelian randomization analysis. Int J Epidemiol 2014; 43: 1487–1497.
Yajnik CS . Nutrient-mediated teratogenesis and fuel-mediated teratogenesis: two pathways of intrauterine programming of diabetes. Int J Gynaecol Obstet 2009; 104 (Suppl), S27–S31.
Kumar KA, Lalitha A, Pavithra D, Padmavathi IJ, Ganeshan M, Rao KR et al. Maternal dietary folate and/or vitamin B12 restrictions alter body composition (adiposity) and lipid metabolism in Wistar rat offspring. J Nutr Biochem 2013; 24: 25–31.
Kumar KA, Lalitha A, Reddy U, Chandak GR, Sengupta S, Raghunath M . Chronic maternal vitamin B12 restriction induced changes in body composition & glucose metabolism in the Wistar rat offspring are partly correctable by rehabilitation. PLoS ONE 2014; 9: e112991.
Freinkel N . Of pregnancy and progeny. Diabetes 1980; 29: 1023–1035.
Hill JC, Krishnaveni GV, Annamma I, Leary SD, Fall CHD . Glucose tolerance in pregnancy in South India: Relationships to neonatal anthropometry. Acta Obstet Gynecol Scand 2005; 84: 159–165.
Krishnaveni GV, Veena SR, Hill JC, Kehoe S, Karat SC, Fall CH . Intra-uterine exposure to maternal diabetes is associated with higher adiposity and insulin resistance and clustering of cardiovascular risk markers in Indian children. Diabetes Care 2010; 33: 402–404.
Krishnaveni GV, Veena SR, Karat SC, Yajnik CS, Fall CH . Association between maternal folate concentrations during pregnancy and insulin resistance in Indian children. Diabetologia 2014; 57: 110–121.
Kulkarni SR, Kumaran K, Rao SR, Chougule SD, Deokar TM, Bhalerao AJ et al. Maternal lipids are as important as glucose for fetal growth: findings from the Pune Maternal Nutrition Study. Diabetes Care 2013; 36: 2706–2713.
Krishnaveni GV, Hill JC, Veena SR, Bhat DS, Wills AK, Karat CLS et al. Low plasma vitamin B12 in pregnancy is associated with gestational ‘diabesity’ and later diabetes. Diabetologia 2009; 52: 2350–2358.
Yajnik CS, Lubree HG, Rege SS, Naik SS, Deshpande JA, Deshpande SS et al. Adiposity and hyperinsulinemia in Indians are present at birth. J Clin Endocrinol Metab 2002; 87: 5575–5580.
Modi N, Thomas EL, Uthaya SN, Umranikar S, Bell JD, Yajnik C . Whole body magnetic resonance imaging of healthy newborn infants demonstrates increased central adiposity in Asian Indians. Pediatr Res 2009; 65: 584–587.
Phillips DI, Jones A, Goulden PA . Birth weight, stress, and the metabolic syndrome in adult life. Ann N Y Acad Sci 2006; 1083: 28–36.
Kajantie E . Fetal origins of stress-related adult disease. Ann N Y Acad Sci 2006; 1083: 11–27.
Ward AM, Fall CH, Stein CE, Kumaran K, Veena SR, Wood PJ et al. Cortisol and the metabolic syndrome in South Asians. Clin Endocrinol (Oxf) 2003; 58: 500–505.
Krishnaveni GV, Veena S, Dhube A, Karat S, Phillips D, Fall CHD . Size at birth, morning cortisol and cardiometabolic risk markers in healthy Indian children. Clin Endocrinol (Oxf) 2014; 80: 73–79.
Krishnaveni GV, Veena SR, Jones A, Srinivasan K, Osmond C, Karat SC et al. Exposure to maternal gestational diabetes is associated with higher cardiovascular responses to stress in adolescent Indians. J Clin Endocrinol Metab 2015; 100: 986–993.
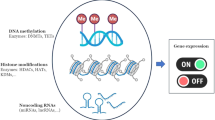
Weinhold B . Epigenetics: the science of change. Environ Health Perspect 2006; 114: A160–A167.
Vickers MH . Early life nutrition, epigenetics and programming of later life disease. Nutrients 2014; 6: 2165–2178.
Perkins E, Murphy SK, Murtha AP, Schildkraut J, Jirtle RL, Demark-Wahnefried W et al. Insulin like growth factor 2/H19 methylation at birth and risk of overweight and obesity in children. J Pediatr 2012; 161: 31–39.
Potdar RD, Sahariah SA, Gandhi M, Kehoe SH, Brown N, Sane H et al. Improving women's diet quality preconceptionally and during gestation: effects on birth weight and prevalence of low birth weight—a randomized controlled efficacy trial in India (Mumbai Maternal Nutrition Project). Am J Clin Nutr 2014; 100: 1257–1268.
Barker DJ, Lampl M, Roseboom T, Winder N . Resource allocation in utero and health in later life. Placenta 2012; 33 (Supp 2), e30–e34.
Jackson AA, Langley-Evans SC, McCarthy HD . Nutritional influences in early life upon obesity and body proportions. Ciba Found Symp 1996; 201: 118–129.
Krishnaveni GV, Veena SR, Srinivasan K, Osmond C, Fall CH . Linear growth and fat and lean tissue gain during childhood: associations with cardiometabolic and cognitive outcomes in adolescent Indian children. PLoS ONE 2015; 10: e0143231.
Bayo J, Dalvi MP, Martinez ED . Successful strategies in the discovery of small-molecule epigenetic modulators with anticancer potential. Future Med Chem 2015; 7: 2243–2261.
Joss-Moore LA, Lane RH . Epigenetics and the developmental origins of disease: the key to unlocking the door of personalized medicine. Epigenomics 2012; 4: 471–473.
Richardson SS, Daniels CR, Gillman MW, Golden J, Kukla R, Kuzawa C et al. Society: don’t blame the mothers. Nature 2014; 512: 131–132.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Krishnaveni, G., Yajnik, C. Developmental origins of diabetes—an Indian perspective. Eur J Clin Nutr 71, 865–869 (2017). https://doi.org/10.1038/ejcn.2017.87
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ejcn.2017.87
This article is cited by
-
Comparison of Anthropometry and Body Composition Using Air Displacement Plethysmography in Term Small for Gestational Age and Appropriate for Gestational Age Neonates
Indian Pediatrics (2023)
-
Pathophysiology, phenotypes and management of type 2 diabetes mellitus in Indian and Chinese populations
Nature Reviews Endocrinology (2022)
-
Effects of dietary and physical activity interventions on the risk of type 2 diabetes in South Asians: meta-analysis of individual participant data from randomised controlled trials
Diabetologia (2019)
-
Gestational diabetes and ultrasound-assessed fetal growth in South Asian and White European women: findings from a prospective pregnancy cohort
BMC Medicine (2018)
-
Contrasting patterns of overweight and thinness among preschool children of different ethnic groups in Norway, and relations with maternal and early life factors
BMC Public Health (2018)