Abstract
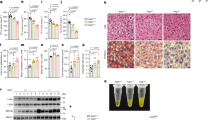
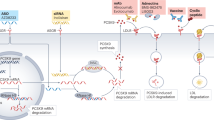
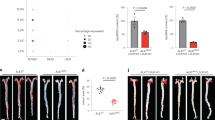
Recent large-scale genetic sequencing efforts have identified rare coding variants in genes in the triglyceride-rich lipoprotein (TRL) clearance pathway that are protective against coronary heart disease (CHD), independently of LDL cholesterol (LDL-C) levels1. Insight into the mechanisms of protection of these variants may facilitate the development of new therapies for lowering TRL levels. The gene APOC3 encodes apoC-III, a critical inhibitor of triglyceride (TG) lipolysis and remnant TRL clearance2. Here we report a detailed interrogation of the mechanism of TRL lowering by the APOC3 Ala43Thr (A43T) variant, the only missense (rather than protein-truncating) variant in APOC3 reported to be TG lowering and protective against CHD3,4,5. We found that both human APOC3 A43T heterozygotes and mice expressing human APOC3 A43T display markedly reduced circulating apoC-III levels. In mice, this reduction is due to impaired binding of A43T apoC-III to lipoproteins and accelerated renal catabolism of free apoC-III. Moreover, the reduced content of apoC-III in TRLs resulted in accelerated clearance of circulating TRLs. On the basis of this protective mechanism, we developed a monoclonal antibody targeting lipoprotein-bound human apoC-III that promotes circulating apoC-III clearance in mice expressing human APOC3 and enhances TRL catabolism in vivo. These data reveal the molecular mechanism by which a missense variant in APOC3 causes reduced circulating TG levels and, hence, protects from CHD. This protective mechanism has the potential to be exploited as a new therapeutic approach to reduce apoC-III levels and circulating TRL burden.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Musunuru, K. & Kathiresan, S. Surprises from genetic analyses of lipid risk factors for atherosclerosis. Circ. Res. 118, 579–585 (2016).
Khetarpal, S.A., Qamar, A., Millar, J.S. & Rader, D.J. Targeting ApoC-III to reduce coronary disease risk. Curr. Atheroscler. Rep. 18, 54 (2016).
Jørgensen, A.B., Frikke-Schmidt, R., Nordestgaard, B.G. & Tybjærg-Hansen, A. Loss-of-function mutations in APOC3 and risk of ischemic vascular disease. N. Engl. J. Med. 371, 32–41 (2014).
Crosby, J. et al. Loss-of-function mutations in APOC3, triglycerides, and coronary disease. N. Engl. J. Med. 371, 22–31 (2014).
Pollin, T.I. et al. A null mutation in human APOC3 confers a favorable plasma lipid profile and apparent cardioprotection. Science 322, 1702–1705 (2008).
Aalto-Setälä, K. et al. Mechanism of hypertriglyceridemia in human apolipoprotein (apo) CIII transgenic mice. Diminished very low density lipoprotein fractional catabolic rate associated with increased apo CIII and reduced apo E on the particles. J. Clin. Invest. 90, 1889–1900 (1992).
Aalto-Setälä, K. et al. Further characterization of the metabolic properties of triglyceride-rich lipoproteins from human and mouse apoC-III transgenic mice. J. Lipid Res. 37, 1802–1811 (1996).
de Silva, H.V. et al. Overexpression of human apolipoprotein C-III in transgenic mice results in an accumulation of apolipoprotein B48 remnants that is corrected by excess apolipoprotein E. J. Biol. Chem. 269, 2324–2335 (1994).
Eisenberg, S., Patsch, J.R., Sparrow, J.T., Gotto, A.M. & Olivecrona, T. Very low density lipoprotein. Removal of apolipoproteins C-II and C-III-1 during lipolysis in vitro. J. Biol. Chem. 254, 12603–12608 (1979).
Masucci-Magoulas, L. et al. A mouse model with features of familial combined hyperlipidemia. Science 275, 391–394 (1997).
Chan, D.C., Watts, G.F., Nguyen, M.N. & Barrett, P.H. Apolipoproteins C-III and A-V as predictors of very-low-density lipoprotein triglyceride and apolipoprotein B-100 kinetics. Arterioscler. Thromb. Vasc. Biol. 26, 590–596 (2006).
Chan, D.C., Watts, G.F., Redgrave, T.G., Mori, T.A. & Barrett, P.H. Apolipoprotein B-100 kinetics in visceral obesity: associations with plasma apolipoprotein C-III concentration. Metabolism 51, 1041–1046 (2002).
Olivieri, O. et al. Apolipoprotein C-III, metabolic syndrome, and risk of coronary artery disease. J. Lipid Res. 44, 2374–2381 (2003).
Ooi, E.M., Barrett, P.H., Chan, D.C. & Watts, G.F. Apolipoprotein C-III: understanding an emerging cardiovascular risk factor. Clin. Sci. (Lond.) 114, 611–624 (2008).
Caron, S. et al. Transcriptional activation of apolipoprotein CIII expression by glucose may contribute to diabetic dyslipidemia. Arterioscler. Thromb. Vasc. Biol. 31, 513–519 (2011).
Ginsberg, H.N. & Brown, W.V. Apolipoprotein CIII: 42 years old and even more interesting. Arterioscler. Thromb. Vasc. Biol. 31, 471–473 (2011).
Ooi, E.M. et al. Plasma apolipoprotein C-III metabolism in patients with chronic kidney disease. J. Lipid Res. 52, 794–800 (2011).
Qamar, A. et al. Plasma apolipoprotein C-III levels, triglycerides, and coronary artery calcification in type 2 diabetics. Arterioscler. Thromb. Vasc. Biol. 35, 1880–1888 (2015).
Cohn, J.S. et al. Plasma turnover of HDL apoC-I, apoC-III, and apoE in humans: in vivo evidence for a link between HDL apoC-III and apoA-I metabolism. J. Lipid Res. 44, 1976–1983 (2003).
Nguyen, M.N. et al. Use of Intralipid for kinetic analysis of HDL apoC-III: evidence for a homogeneous kinetic pool of apoC-III in plasma. J. Lipid Res. 47, 1274–1280 (2006).
Ginsberg, H.N. & Ramakrishnan, R. Kinetic studies of the metabolism of rapidly exchangeable apolipoproteins may leave investigators and readers with exchangeable results. Arterioscler. Thromb. Vasc. Biol. 28, 1685–1686 (2008).
Ginsberg, H.N. & Ramakrishnan, R. Investigations of apoC-III metabolism using stable isotopes: what information can you acquire and how can you interpret your results? J. Lipid Res. 52, 1071–1072 (2011).
Mauger, J.F., Couture, P., Bergeron, N. & Lamarche, B. Apolipoprotein C-III isoforms: kinetics and relative implication in lipid metabolism. J. Lipid Res. 47, 1212–1218 (2006).
Shin, M.J. & Krauss, R.M. Apolipoprotein CIII bound to apoB-containing lipoproteins is associated with small, dense LDL independent of plasma triglyceride levels in healthy men. Atherosclerosis 211, 337–341 (2010).
Yang, X. et al. Reduction in lipoprotein-associated apoC-III levels following volanesorsen therapy: phase 2 randomized trial results. J. Lipid Res. 57, 706–713 (2016).
Pechlaner, R. et al. Very-low-density lipoprotein-associated apolipoproteins predict cardiovascular events and are lowered by inhibition of APOC-III. J. Am. Coll. Cardiol. 69, 789–800 (2017).
Wyler von Ballmoos, M.C., Haring, B. & Sacks, F.M. The risk of cardiovascular events with increased apolipoprotein CIII: a systematic review and meta-analysis. J. Clin. Lipidol. 9, 498–510 (2015).
Nagashima, K. et al. Effects of the PPARγ agonist pioglitazone on lipoprotein metabolism in patients with type 2 diabetes mellitus. J. Clin. Invest. 115, 1323–1332 (2005).
Willer, C.J. et al. Discovery and refinement of loci associated with lipid levels. Nat. Genet. 45, 1274–1283 (2013).
Graham, M.J. et al. Antisense oligonucleotide inhibition of apolipoprotein C-III reduces plasma triglycerides in rodents, nonhuman primates, and humans. Circ. Res. 112, 1479–1490 (2013).
Gaudet, D. et al. Antisense inhibition of apolipoprotein C-III in patients with hypertriglyceridemia. N. Engl. J. Med. 373, 438–447 (2015).
Sundaram, M. et al. Functional analysis of the missense APOC3 mutation Ala23Thr associated with human hypotriglyceridemia. J. Lipid Res. 51, 1524–1534 (2010).
Millar, J.S., Cromley, D.A., McCoy, M.G., Rader, D.J. & Billheimer, J.T. Determining hepatic triglyceride production in mice: comparison of poloxamer 407 with Triton WR-1339. J. Lipid Res. 46, 2023–2028 (2005).
Malmendier, C.L., Lontie, J.F., Grutman, G.A. & Delcroix, C. Metabolism of apolipoprotein C-III in normolipemic human subjects. Atherosclerosis 69, 51–59 (1988).
Malmendier, C.L. et al. Apolipoproteins C-II and C-III metabolism in hypertriglyceridemic patients. Effect of a drastic triglyceride reduction by combined diet restriction and fenofibrate administration. Atherosclerosis 77, 139–149 (1989).
Gordts, P.L. et al. ApoC-III inhibits clearance of triglyceride-rich lipoproteins through LDL family receptors. J. Clin. Invest. 126, 2855–2866 (2016).
Kathiresan, S. Developing medicines that mimic the natural successes of the human genome: lessons from NPC1L1, HMGCR, PCSK9, APOC3, and CETP. J. Am. Coll. Cardiol. 65, 1562–1566 (2015).
Dewey, F.E. et al. Inactivating variants in ANGPTL4 and risk of coronary artery disease. N. Engl. J. Med. 374, 1123–1133 (2016).
Stitziel, N.O. et al. Coding variation in ANGPTL4, LPL, and SVEP1 and the risk of coronary disease. N. Engl. J. Med. 374, 1134–1144 (2016).
Do, R. et al. Exome sequencing identifies rare LDLR and APOA5 alleles conferring risk for myocardial infarction. Nature 518, 102–106 (2015).
Peloso, G.M. et al. Association of low-frequency and rare coding-sequence variants with blood lipids and coronary heart disease in 56,000 whites and blacks. Am. J. Hum. Genet. 94, 223–232 (2014).
MacLean, B. et al. Skyline: an open source document editor for creating and analyzing targeted proteomics experiments. Bioinformatics 26, 966–968 (2010).
Mucaki, E.J., Shirley, B.C. & Rogan, P.K. Prediction of mutant mRNA splice isoforms by information theory–based exon definition. Hum. Mutat. 34, 557–565 (2013).
Ibrahim, S., Somanathan, S., Billheimer, J., Wilson, J.M. & Rader, D.J. Stable liver-specific expression of human IDOL in humanized mice raises plasma cholesterol. Cardiovasc. Res. 110, 23–29 (2016).
Somanathan, S. et al. AAV vectors expressing LDLR gain-of-function variants demonstrate increased efficacy in mouse models of familial hypercholesterolemia. Circ. Res. 115, 591–599 (2014).
Chen, S.J. et al. Biodistribution of AAV8 vectors expressing human low-density lipoprotein receptor in a mouse model of homozygous familial hypercholesterolemia. Hum. Gene Ther. Clin. Dev. 24, 154–160 (2013).
Kassim, S.H. et al. Adeno-associated virus serotype 8 gene therapy leads to significant lowering of plasma cholesterol levels in humanized mouse models of homozygous and heterozygous familial hypercholesterolemia. Hum. Gene Ther. 24, 19–26 (2013).
Rader, D.J., Castro, G., Zech, L.A., Fruchart, J.C. & Brewer, H.B. Jr. In vivo metabolism of apolipoprotein A-I on high density lipoprotein particles LpA-I and LpA-I,A-II. J. Lipid Res. 32, 1849–1859 (1991).
Cain, W.J. et al. Lipoprotein [a] is cleared from the plasma primarily by the liver in a process mediated by apolipoprotein [a]. J. Lipid Res. 46, 2681–2691 (2005).
Tanigawa, H. et al. Expression of cholesteryl ester transfer protein in mice promotes macrophage reverse cholesterol transport. Circulation 116, 1267–1273 (2007).
Ota, T., Gayet, C. & Ginsberg, H.N. Inhibition of apolipoprotein B100 secretion by lipid-induced hepatic endoplasmic reticulum stress in rodents. J. Clin. Invest. 118, 316–332 (2008).
McCoy, M.G. et al. Characterization of the lipolytic activity of endothelial lipase. J. Lipid Res. 43, 921–929 (2002).
Larsson, M., Vorrsjö, E., Talmud, P., Lookene, A. & Olivecrona, G. Apolipoproteins C-I and C-III inhibit lipoprotein lipase activity by displacement of the enzyme from lipid droplets. J. Biol. Chem. 288, 33997–34008 (2013).
Acknowledgements
The authors thank A. Wilson, E. Edouard, J. McParland, M. McCoy, K. Trindade, S. DerOrhannessian, M. Risman, K. Burton, and M. Sun for technical expertise and M. Lazar, M. Bucan, Z. Arany, B. Garcia, N. Hand, D. Marchadier, D. Conlon, and R. Bauer for helpful discussions. This work was supported in part by NIH grants R01HL133502 and R37HL055323 and a grant from the Foundation Leducq CVGeneF(x) Transatlantic Network of Excellence to D.J.R. and by NIH grant F30HL124967 to S.A.K. This project also used the UPCI Cancer Proteomics Facility, which is supported in part by NIH award P30CA047904. Recruitment to the Penn Medicine BioBank was supported by the Penn Cardiovascular Institute, the Perelman School of Medicine of the University of Pennsylvania, and a gift from the Smilow family.
Author information
Authors and Affiliations
Contributions
S.A.K., J.S.M., C.V., A.V.H.S., and P.Z. performed experiments on the A43T variant. S.A.K., X.Z., Z.S., and N.A.Y. performed selective reaction monitoring measurements from human plasma samples. S.A.K., P.D.-J., J.A.L., N.B., W.J.Z., I.T., and H.d.H. designed and performed experiments on anti-apoC-III monoclonal antibodies. G.M.P., P.N., M.C., S.L.-K., M.C.P., A.R.T., and S.K. provided guidance with study design. S.A.K. and D.J.R. secured funding, conceived and designed experiments, interpreted all results, and wrote the manuscript. All authors provided input on the manuscript.
Corresponding author
Ethics declarations
Competing interests
D.J.R. has previously been paid as a consultant for the following companies: Aegerion, Alnylam, Eli Lily, Pfizer, and Novartis. P.D.J., A.R.T., and D.J.R. are cofounders of Staten Biotechnology BV. In addition, J.A.L., N.B., and W.J.Z. are employees of and hold equity in Staten Biotechnology BV. I.T. is an employee of FairJourney Biologics. H.d.H. is an employee of and holds equity in argenX BVBA. The other authors declare no competing financial interests.
Supplementary information
Supplementary Figures and Tables
Supplementary Figures 1–13 and Supplementary Tables 1–4. (PDF 3185 kb)
Rights and permissions
About this article
Cite this article
Khetarpal, S., Zeng, X., Millar, J. et al. A human APOC3 missense variant and monoclonal antibody accelerate apoC-III clearance and lower triglyceride-rich lipoprotein levels. Nat Med 23, 1086–1094 (2017). https://doi.org/10.1038/nm.4390
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nm.4390
This article is cited by
-
Hyperlipidaemia in diabetes: are there particular considerations for next-generation therapies?
Diabetologia (2024)
-
Apolipoprotein C-III itself stimulates the Syk/cPLA2-induced inflammasome activation of macrophage to boost anti-tumor activity of CD8+ T cell
Cancer Immunology, Immunotherapy (2023)
-
APOC-III: a Gatekeeper in Controlling Triglyceride Metabolism
Current Atherosclerosis Reports (2023)
-
Causes, clinical findings and therapeutic options in chylomicronemia syndrome, a special form of hypertriglyceridemia
Lipids in Health and Disease (2022)
-
A Tale of Two New Targets for Hypertriglyceridaemia: Which Choice of Therapy?
BioDrugs (2022)