Abstract
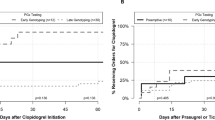
We examined clinical outcomes with proton pump inhibitors (PPI) use within CYP2C19 genotype groups during clopidogrel treatment following acute myocardial infarction (AMI). 2062 patients were genotyped for CYP2C19*2 and *17 variants in TRIUMPH. 12 month clinical outcomes were analyzed among patients discharged on clopidogrel within CYP2C19*2 carrier, CYP2C19*17 carrier, and CYP2C19*1 homozygote genotype groups. PPI use was not associated with a difference in mortality. Among clopidogrel-treated Caucasians following AMI, PPI use was associated with a significantly higher rate of cardiac rehospitalization (HR 1.62, 95% CI 1.19–2.19; P=0.002) compared with no PPI use. PPI users who were carriers of the CYP2C19*17 variant experienced significantly higher rates of cardiac rehospitalization (HR 2.05, 95% CI 1.26–3.33; P=0.003), carriers of the CYP2C19*2 variant had a trend toward increased 1-year cardiac rehospitalization (HR 1.69, 95% CI 0.95–2.99; P=0.07), while no significant differences were observed among CYP2C19*1 homozygotes. These results indicate that the risks associated with PPI use among clopidogrel-treated Caucasian post-MI patients are impacted by CYP2C19 genotype, and suggest knowledge of genotype may be useful for personalizing PPI use among patients following AMI to reduce rehospitalization.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 6 print issues and online access
$259.00 per year
only $43.17 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Go AS, Mozaffarian D, Roger VL, Benjamin EJ, Berry JD, Borden WB et al. Heart disease and stroke statistics—2013 update: a report from the American Heart Association. Circulation 2013; 127: e6–e245.
Bhatt DL . Role of antiplatelet therapy across the spectrum of patients with coronary artery disease. Am J Cardiol 2009; 103: 11A–19A.
Depta JP, Bhatt DL . Aspirin and platelet adenosine diphosphate receptor antagonists in acute coronary syndromes and percutaneous coronary intervention: role in therapy and strategies to overcome resistance. Am J Cardiovasc Drugs 2008; 8: 91–112.
Somma KA, Bhatt DL, Fonarow GC, Cannon CP, Cox M, Laskey W et al. Guideline adherence after ST-segment elevation versus non-ST segment elevation myocardial infarction. Am J Cardiovasc Drugs 2012; 5: 654–661.
Bonello L, Tantry US, Marcucci R, Blindt R, Angiolillo DJ, Becker R et al. Consensus and future directions on the definition of high on-treatment platelet reactivity to adenosine diphosphate. J Am Coll Cardiol 2010; 56: 919–933.
Depta JP, Bhatt DL . Antiplatelet therapy and proton pump inhibition: cause for concern? Curr Opin Cardiol 2012; 27: 642–650.
Depta JP, Bhatt DL . Omeprazole and clopidogrel: Should clinicians be worried? Cleve Clin J Med 2010; 77: 113–116.
Mega JL, Close SL, Wiviott SD, Shen L, Hockett RD, Brandt JT et al. Cytochrome p-450 polymorphisms and response to clopidogrel. N Engl J Med 2009; 360: 354–362.
Shi S, Klotz U . Proton pump inhibitors: an update of their clinical use and pharmacokinetics. Eur J Clin Pharmacol 2008; 64: 935–951.
Frelinger AL 3rd, Lee RD, Mulford DJ, Wu J, Nudurupati S, Nigam A et al. A randomized, 2-period, crossover design study to assess the effects of dexlansoprazole, lansoprazole, esomeprazole, and omeprazole on the steady-state pharmacokinetics and pharmacodynamics of clopidogrel in healthy volunteers. J Am Coll Cardiol 2012; 59: 1304–1311.
O’Donoghue ML, Braunwald E, Antman EM, Murphy SA, Bates ER, Rozenman Y et al. Pharmacodynamic effect and clinical efficacy of clopidogrel and prasugrel with or without a proton-pump inhibitor: an analysis of two randomised trials. Lancet 2009; 374: 989–997.
O’Donoghue ML . CYP2C19 genotype and proton pump inhibitors in clopidogrel-treated patients: does it take two to tango? Circulation 2011; 123: 468–470.
Arnold SV, Chan PS, Jones PG, Decker C, Buchanan DM, Krumholz HM et al. Translational Research Investigating Underlying Disparities in Acute Myocardial Infarction Patients’ Health Status (TRIUMPH): design and rationale of a prospective multicenter registry. Circ Cardiovasc Qual Outcomes 2011; 4: 467–476.
Cresci S, Wu J, Province MA, Spertus JA, Steffes M, McGill JB et al. Peroxisome proliferator-activated receptor pathway gene polymorphism associated with extent of coronary artery disease in patients with type 2 diabetes in the bypass angioplasty revascularization investigation 2 diabetes trial. Circulation 2011; 124: 1426–1434.
Lanfear DE, Jones PG, Cresci S, Tang F, Rathore SS, Spertus JA . Factors influencing patient willingness to participate in genetic research after a myocardial infarction. Genome medicine 2011; 3: 39.
Sim SC, Risinger C, Dahl ML, Aklillu E, Christensen M, Bertilsson L et al. A common novel CYP2C19 gene variant causes ultrarapid drug metabolism relevant for the drug response to proton pump inhibitors and antidepressants. Clin Pharmacol Ther 2006; 79: 103–113.
Wang H, An N, Wang H, Gao Y, Liu D, Bian T et al. Evaluation of the effects of 20 nonsynonymous single nucleotide polymorphisms of CYP2C19 on S-mephenytoin 4′-hydroxylation and omeprazole 5'-hydroxylation. Drug Metab Dispos 2011; 39: 830–837.
Yan AT, Yan RT, Tan M, Eagle KA, Granger CB, Dabbous OH et al. In-hospital revascularization and one-year outcome of acute coronary syndrome patients stratified by the GRACE risk score. Am J Cardiol 2005; 96: 913–916.
Tang EW, Wong CK, Herbison P . Global Registry of Acute Coronary Events (GRACE) hospital discharge risk score accurately predicts long-term mortality post acute coronary syndrome. Am Heart J 2007; 153: 29–35.
Ohbuchi M, Noguchi K, Kawamura A, Usui T . Different effects of proton pump inhibitors and famotidine on the clopidogrel metabolic activation by recombinant CYP2B6, CYP2C19 and CYP3A4. Xenobiotica 2012; 42: 633–640.
Zvyaga T, Chang SY, Chen C, Yang Z, Vuppugalla R, Hurley J et al. Evaluation of six proton pump inhibitors as inhibitors of various human cytochromes P450: focus on cytochrome P450 2C19. Drug Metab Dispos 2012; 40: 1698–1711.
Fernando H, Bassler N, Habersberger J, Sheffield LJ, Sharma R, Dart AM et al. Randomized double-blind placebo-controlled crossover study to determine the effects of esomeprazole on inhibition of platelet function by clopidogrel. J Thromb Haemost 2011; 9: 1582–1589.
Furuta T, Iwaki T, Umemura K . Influences of different proton pump inhibitors on the anti-platelet function of clopidogrel in relation to CYP2C19 genotypes. Br J Clin Pharmacol 2010; 70: 383–392.
Hulot JS, Wuerzner G, Bachelot-Loza C, Azizi M, Blanchard A, Peyrard S et al. Effect of an increased clopidogrel maintenance dose or lansoprazole co-administration on the antiplatelet response to clopidogrel in CYP2C19-genotyped healthy subjects. J Thromb Haemost 2010; 8: 610–613.
Liu Q, Dang DS, Chen YF, Yan M, Shi GB, Zhao QC . The influence of omeprazole on platelet inhibition of clopidogrel in various CYP2C19 mutant alleles. Genet Test Mol Biomarkers 2012; 16: 1293–1297.
Simon T, Steg PG, Gilard M, Blanchard D, Bonello L, Hanssen M et al. Clinical events as a function of proton pump inhibitor use, clopidogrel use, and cytochrome P450 2C19 genotype in a large nationwide cohort of acute myocardial infarction: results from the French Registry of Acute ST-Elevation and Non-ST-Elevation Myocardial Infarction (FAST-MI) registry. Circulation 2011; 123: 474–482.
Harmsze AM, van Werkum JW, Souverein PC, Breet NJ, Bouman HJ, Hackeng CM et al. Combined influence of proton-pump inhibitors, calcium-channel blockers and CYP2C19*2 on on-treatment platelet reactivity and on the occurrence of atherothrombotic events after percutaneous coronary intervention. J Thromb Haemost 2011; 9: 1892–1901.
Gladding P, Webster M, Zeng I, Farrell H, Stewart J, Ruygrok P et al. The pharmacogenetics and pharmacodynamics of clopidogrel response: an analysis from the PRINC (Plavix Response in Coronary Intervention) trial. JACC Cardiovasc Interv 2008; 1: 620–627.
Frere C, Cuisset T, Morange PE, Quilici J, Camoin-Jau L, Saut N et al. Effect of cytochrome p450 polymorphisms on platelet reactivity after treatment with clopidogrel in acute coronary syndrome. Am J Cardiol 2008; 101: 1088–1093.
Brandt JT, Close SL, Iturria SJ, Payne CD, Farid NA, Ernest CS 2nd et al. Common polymorphisms of CYP2C19 and CYP2C9 affect the pharmacokinetic and pharmacodynamic response to clopidogrel but not prasugrel. J Thromb Haemost 2007; 5: 2429–2436.
Frere C, Cuisset T, Gaborit B, Alessi MC, Hulot JS . The CYP2C19*17 allele is associated with better platelet response to clopidogrel in patients admitted for non-ST acute coronary syndrome. J Thromb Haemost 2009; 7: 1409–1411.
Muhlestein JB, Horne BD, Bair TL, Li Q, Madsen TE, Pearson RR et al. Usefulness of in-hospital prescription of statin agents after angiographic diagnosis of coronary artery disease in improving continued compliance and reduced mortality. Am J Cardiol 2001; 87: 257–261.
Acknowledgements
This work and S. Cresci’s effort are supported in part by the National Institutes of Health (Cresci R01 NR013396). TRIUMPH was sponsored by the National Institutes of Health: Washington University School of Medicine SCCOR Grant P50 HL077113.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
TY Wang has received research grants from Lilly USA (significant), Daiichi Sankyo (significant) and Gilead Science (significant), and is a consultant to Astra Zeneca (modest), American College of Cardiology Foundation (significant). JA Spertus has received research grants from Eli Lilly, EveHeart, Genentech and Gilead, and is a consultant to St Jude Medical (modest), United Healthcare (modest), Amgen (modest), Gilead (modest), Genentech (modest), Janssen (modest) and Novartis (modest). Copyrights/Patents apply to Seattle Angina Questionnaire, Kansas City Cardiomyopathy Questionnaire and Peripheral Artery Questionnaire. US Patents: 7,643,969; 7,853,456; 12/965,656; and 13/615,401. RG Bach has received research grants from AstraZeneca, Eli Lilly, Bristol-Myers Squibb and Merck/Schering-Plough, and is a consultant (CEC activity only) to Roche (significant), Pfizer (modest). The remaining authors declare no conflict of interest.
Additional information
Supplementary Information accompanies the paper on the The Pharmacogenomics Journal website
Supplementary information
PowerPoint slides
Rights and permissions
About this article
Cite this article
Depta, J., Lenzini, P., Lanfear, D. et al. Clinical outcomes associated with proton pump inhibitor use among clopidogrel-treated patients within CYP2C19 genotype groups following acute myocardial infarction. Pharmacogenomics J 15, 20–25 (2015). https://doi.org/10.1038/tpj.2014.28
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/tpj.2014.28
This article is cited by
-
Risk of major adverse cardiovascular events for concomitant use of clopidogrel and proton pump inhibitors in patients inheriting CYP2C19 loss-of-function alleles: meta-analysis
International Journal of Clinical Pharmacy (2021)
-
Drug–drug–gene interactions and adverse drug reactions
The Pharmacogenomics Journal (2020)
-
Effect of cytochrome P450 2C19 polymorphism on adverse cardiovascular events after drug-eluting stent implantation in a large Hakka population with acute coronary syndrome receiving clopidogrel in southern China
European Journal of Clinical Pharmacology (2018)
-
Association between CYP2C19 extensive metabolizer phenotype and childhood anti-reflux surgery following failed proton pump inhibitor medication treatment
European Journal of Pediatrics (2018)
-
A novel genetic marker of decreased inflammation and improved survival after acute myocardial infarction
Basic Research in Cardiology (2018)