Key Points
-
Helps clinicians understand the possible aetiologies for inadequate tooth display.
-
Provides advice on what to look for clinically to make a correct diagnosis of the aetiology.
-
Suggests when restorative dentistry may correct the inadequate tooth display.
-
Helps in the understanding of when non-restorative options will be necessary to achieve the desired outcomes.
Abstract
Some of the most challenging patients to produce a pleasing smile for are those who present with inadequate tooth display (either due to tooth position, the patient has normal size teeth, but they aren't exposed adequately to fill out the smile) or due to tooth size (the teeth are small, often due to tooth wear). The key to understanding how to manage these patients is to learn to understand the possible aetiologies that could produce the condition, and learn how to diagnose which aetiologies exist for your patient. Potential aetiologies for inadequate tooth display in patients with normal length unworn anterior teeth: excessive lip length; inadequate lip mobility; inadequate vertical eruption of the anterior teeth; inadequate facial prominence of the maxillary anterior teeth; vertical maxillary deficiency; and anterior maxillary deficiency.
This article, the first in a British Dental Journal series on the topic of aesthetic dentistry, reviews the clinical findings consistent with diagnosing each of the above etiologies, and then reviews the treatment options available for correcting the inadequate tooth display.
Similar content being viewed by others
Background and aim
The desire for a full and beautiful smile continues to increase as more and more patients are exposed to the possibilities of aesthetic dentistry. One of the most challenging patients to produce an ideal smile for is one who presents with inadequate tooth display, either due to tooth position (ie the patient has normal size teeth but they aren't exposed adequately to fill out the smile) or due to tooth size (ie the teeth are small, often due to tooth wear).
The key to understanding how to manage these patients is to learn to understand the possible aetiologies that could produce the condition, and learn how to diagnose which aetiologies exist for your patient. Once the diagnosis is made, it is critical to know which treatment options exist to manage the given problem, understanding that for most dental problems, there are multiple treatment plans that can produce an improvement, depending upon the level of compromise the patient is willing to accept.
In starting to discuss the diagnosis and treatment planning of patients with inadequate tooth display, it is helpful to describe what the desired outcome is for most patients, understanding that this outcome describes a range of acceptability, not an absolute that applies to all patients.
This paper will focus on achieving acceptable central incisor display, understanding that the remaining teeth in the arch are then positioned relative to the central incisors to produce the desired smile line and fullness of the buccal corridor.1 When we consider maxillary central incisor display, it is common to discuss the amount of tooth that shows at rest (repose), and the amount of tooth that shows in a full smile.
Introduction
Research has shown that the amount of central incisor display at rest varies from male to female, and also changes over time with ageing.2,3,4 However, using absolute values of how much of the central incisors show at rest to determine the central incisor incisal edge position has significant limitations, ie all 30-year-olds should not get 3.5 mm of central showing at rest, just as all 50-year-olds should not show 1.5 mm at rest, even though the 3–3.5 mm display in a 30-year-old, and the 1–1.5 mm display in a 50-year-old, would fit the average amounts found in Vig and Brundo's classic study. Ultimately, it is important aesthetically that the edges of the centrals are at least visible at rest. If they are not, regardless of the age of the patient, there will be inadequate tooth display, not just when the patient's lip is at rest, but also when they are speaking.5
What the lip at rest does help with understanding is how much change will have to be made if the centrals are not visible at rest. In other words, it is possible to measure from the lip to the incisal edge of the centrals and know that if the incisal edges are 3 mm under the lip, it will be necessary to make at least a 3.5–4 mm change in the relationship of the lip to the edges of the teeth to allow for the incisal edges to be visible at rest (Fig. 1).
The most significant factor impacting tooth display is not the position of the incisal edge relative to the lip at rest, but how much the lip moves from rest position to its highest position during a spontaneous smile, what I will refer to as 'lip mobility'. Notice the reference to a spontaneous smile, often a posed smile, does not provide an accurate view of a patients full smile, especially if they are uncomfortable with the appearance of their teeth. Research has shown the spontaneous smile to have significantly greater lip mobility than the typical posed smile.6
Having measured lip mobility in patients for over 25 years, my conclusion is that the average patient has between 6–8 mm of movement from their resting lip position to the highest position the lip moves in a spontaneous smile. This makes sense when we evaluate the average tooth size and tooth display in a 30-year-old with a pleasing smile. They would have around 3.5 mm of central incisors showing at rest, which given the average central incisor length of 10.5 mm, would leave 7 mm of the central incisor not exposed. With a high smile, if they had 6 mm of lip mobility they would show all but 1 mm of the centrals, and if they had 8 mm of lip mobility they would show all of the centrals and 1 mm of gingiva.
We could describe the outcome for the 30-year-old above as a description of an ideal goal for tooth display, centrals showing at rest, and all or most of the centrals exposed in a high smile. The challenge of course is that not all patients have 6–8 mm of lip mobility. Patients with very low levels of lip mobility, 2–5 mm, could have 3 mm of their central incisors showing at rest, and only show half the centrals in a full smile, not the smile most patients desire. In patients with low levels of lip mobility, it is frequently necessary to have an increased tooth display at rest, sometimes 4-6 mm, so that they have the level of tooth display we would consider pleasing in a full smile (Fig. 2).
The other extreme are patients with high levels of lip mobility, over 10 mm; if a patient with 10 mm of lip mobility has 3 mm of centrals showing at rest, and they have average 10.5 mm long centrals, they will show almost 3 mm of gingiva in a high smile. If the patient is bothered by the gingival display, it will be necessary to reduce the lip mobility with botulinum toxin, or lip repositioning surgery, or to consider repositioning the teeth and gingiva in a superior direction. In which case the desire would be to move the centrals so only 1 mm showed at rest, leaving 9.5 mm covered by the lip, and so then with 10 mm of lip mobility, during a high smile, the full central incisors would show and only 0.5 mm of gingiva. Botulinum toxin has been shown to predictably, although temporarily, reduce lip mobility 3–5 mm, while lip repositioning surgery has been shown to be effective at reducing excessive gingival display from lip hypermobility long term.7,8,9
The main point in using these examples is simple; there is not one correct answer for how teeth should be positioned because of the significant variations between patients' levels of lip mobility, and their varying desires for how much tooth display is appropriate in a full smile. As a general rule, patients with low levels of lip mobility will need to show more tooth at rest to achieve the desired amount of tooth display in a smile, and those with high levels of lip mobility will need to show very little central incisor at rest if they desire minimising the amount of gingiva displayed in a full smile.
As mentioned previously, the two primary aetiologies for inadequate tooth display are tooth position and tooth size, each of which has subsets that can be identified. It is helpful to describe these subsets as they aid in understanding what treatment options are available.
Inadequate tooth display
Potential etiologies for inadequate tooth display in patients with normal length unworn anterior teeth
These include:
-
Excessive lip length
-
Inadequate lip mobility
-
Inadequate vertical eruption of the anterior teeth
-
Inadequate facial prominence of the maxillary anterior teeth
-
Vertical maxillary deficiency
-
Anterior maxillary deficiency.
Excessive lip length
A critical element relating to tooth display is the length and character of the upper lip. The longer lip significantly reduces tooth display at rest, during speech, and in a full smile. Research has shown that upper lip length is one of the most variable elements between individuals, and can change significantly with age, getting longer as the patient gets older.10,11,12 For diagnostic purposes the lip can be measured at repose from the base of the nose to the inferior border of the lip, with 20–22 mm being average for a 30-year-old female, and 22–24 mm for a male (Fig. 3).
Surgery to reduce the length of an excessively long lip can significantly improve tooth display, while requiring no dental intervention.13
Inadequate lip mobility
Patients with inadequate lip mobility can be very challenging, unlike patients with hypermobile lips, who can be treated with Botox or lip repositioning surgery, patients with low levels of lip mobility don't have an option for increasing it. This means all treatment options must address the position of the teeth relative to the lip, which means the incisal edges of the anterior teeth need to be moved in a coronal direction relative to the lip, through orthodontic eruption, restorative lengthening, or orthognathic surgery. It is important to note that often more than one form of treatment is necessary to achieve an acceptable result. Any of the above movements will also require potentially significant alterations in the mandibular teeth to satisfy the occlusal considerations for the patient.
Another treatment option that can increase anterior tooth display, in addition to the coronal movement of the incisal edges, is to increase the facial prominence of the maxillary teeth. Consider the upper lip as a flap of tissue attached at the vestibule; the position of the lip at rest is strongly affected by the underlying bone and tooth position. If the maxillary teeth are retracted, the position of the lip moves coronally and the amount of tooth display at rest decreases, although the lip mobility may not change significantly. The inverse is also true, if the maxillary teeth are moved facially; the position of the lip moves in an apical direction, exposing more tooth at rest, and occasionally resulting in a small increase in lip mobility as well. However, even if the lip mobility doesn't increase, since the movement of the lip starts from a more apical position on the anterior teeth, there is a subsequent increase in the total amount of tooth displayed in the smile.
Inadequate vertical eruption of the anterior teeth
The next aetiology to consider is the possibility that the anterior teeth did not erupt to the correct position in an inferior dimension. This is different to the entire maxilla having an anterior and vertical deficiency. When the anterior teeth are inadequately erupted, there is a visible step between the anterior and posterior teeth when looking at the plane of occlusion. This step in the occlusal plane indicates a normal posterior eruption and vertical dimension, but a lack of normal anterior eruption.
There are two common causes for the lack of anterior eruption, the first being a potential tongue posture problem, where the tongue did not allow the teeth to erupt into their normal position. The hallmark of these patients is typically an anterior open bite and a significantly reversed smile line across the anterior. Assuming the anterior teeth are in good condition and unworn due to the open bite, orthodontics is the most logical treatment, but it requires the tongue posture be addressed and managed.14
If the tongue is not an issue, and the anterior teeth are normal sized, unworn, in occlusion, and under-erupted, the most common cause is a lack of adequate overjet. For the maxillary anteriors to reach their normal position in the face, overjet is necessary, and consequently anything that reduces overjet during growth and development will reduce the ability of the maxillary anteriors to erupt in a coronal direction.
Causes for the lack of overjet may be skeletal, being Class III, or having a skeletal Class III tendency. Other causes include arch length issues, where the mandibular arch may be long due to supernumerary teeth, or having retained primary molars, which are wider mesial distally then the permanent premolars. Another problem might be arch length issues where the maxillary arch is short, such as congenitally missing lateral incisors. Issues of tooth inclination, such as retroclined maxillary anteriors or proclined mandibular anteriors, can also reduce overjet.
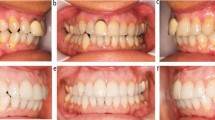
The treatment for inadequate anterior eruption with a step in the occlusal plane can be orthodontics, levelling the maxillary arch by extruding the anterior teeth after first correcting the lack of overjet;15 orthodontics and orthognathic surgery, particularly when the patient is a full skeletal Class III; or restorative dentistry, with or without orthodontic or orthognathic assistance. However, in most instances where there is a step in the occlusal plane due to a lack of overjet, restorative dentistry alone is a difficult option because it is rarely capable of producing an acceptable overbite and overjet relationship. Often this requires increasing the vertical dimension in order to lengthen teeth which are already normal in length, just not in the correct position (Figs 4,5,6,7,8,9).
Inadequate facial prominence of the anterior teeth
As described previously in discussing patients with low levels of lip mobility, the facial prominence of the anterior teeth can have an impact on where the lip is positioned at rest, and also on how it moves during a smile. Think of this as being similar to the concept of providing adequate lip support with the flange of a denture for an edentulous patient. This need for increased lip support can also be true for patients with normal levels of lip mobility, not just those with low levels of lip mobility. A common example might be a patient who has normal levels of lip mobility, but had been previously treated with the removal of upper first premolars, followed by the retraction of the maxillary anteriors to correct a Class II occlusal relationship.16,17
In some patients the aesthetic result can be excellent, particularly patients whose maxillary teeth were too prominent. However if the maxillary teeth were correctly positioned before the retraction, it is not uncommon for these patients to have a decrease in their overall tooth display. Again, this is due to the lip now moving more coronally at rest, which results in a decreased tooth display, but since the lip now starts its movement from a more coronal position, there is less overall tooth display in a full smile.
The treatment options to correct this issue are designed to recreate the correct facial prominence of the anterior teeth. Orthodontics is one option, and can be done two ways. Firstly, if the problem is due to the removal of maxillary premolars, it is possible to consider reopening the premolar spaces to provide room for implants, essentially repositioning the teeth into the position they would have been in before removing the premolars. The primary risk in this movement concerns the facial bone and gingiva on the anterior teeth; however with surgically-assisted orthodontics, where bone grafting is done on the facials before surgery, some facial movement without recession can be achieved.
The one problem with the approach of re-opening spaces is the Class II skeletal relationship will need to be addressed, as there will now be excess overjet and a lack of anterior contact. This potentially means a mandibular advancement, or significant orthodontic movement, to procline the mandibular anterior teeth.
Another alternative for the patient missing premolars whose anterior teeth have been retracted and now has inadequate tooth display, is not to reopen the premolar spaces, but to orthodontically expand the arch creating diastemas between the teeth. This requires restoration of the teeth to close the spaces, and also requires managing the lower arch to correct the excess overjet created by the maxillary expansion.
An additional option, which does not require alterations to the mandibular arch for patients missing maxillary premolars with inadequate tooth display, is to consider using restorations to increase the length of the maxillary teeth and also their prominence facially, but leave the teeth in their existing position, so no orthodontic intervention is used. This technique cannot produce the same change in the facial prominence of the teeth that the orthodontic options can, but when combined with minor increases in tooth length can be very successful. This allows for a significant aesthetic improvement, without dramatically increasing the overbite or altering the occlusion (Figs 10,11,12,13,14,15).
Vertical maxillary deficiency
Just as it is possible for the anterior teeth to not erupt to a normal vertical position, resulting in a step in the maxillary occlusal plane between the anterior and posterior teeth, it is also possible for the maxilla to not develop adequately to produce a normal level of tooth display. The hallmark of these patients is typically normal length anterior teeth, a level occlusal plane, normal levels of lip mobility, but a short lower face, creating the classic square brachycephalic appearance. From a lateral perspective, the mandible is characterised by a long ramus, acute gonial angle, and flat mandibular plane angle.18,19
Since most general practitioners don't take cephalometric radiographs, frontal and lateral photographs of the face can be very helpful in aiding a diagnosis. Start by identifying the glabella (the prominence between the eyebrows), then the base of the nose, and measuring the distance between them – this provides the length of the mid-face. Then measure from the base of the nose to the base of the chin which provides the length of the lower face. A normal face will have a proportion where the mid-face is 45 to 50% of the total length of the mid face and lower face combined, and the lower face is 50 to 55% of the total combined lengths.
A typical brachycephalic face with inadequate maxillary tooth display may have a mid face proportion of 55% or more, and a lower face proportion of 45% or less. They also may have relatively deep overbites. Their maxilla needs to be moved in an inferior direction to increase their facial vertical dimension and increase their tooth display; however, down-fracturing the maxilla and grafting bone has a high degree of postsurgical relapse.20,21,22,23
A much more stable procedure is to use orthognathic surgery to rotate the maxilla down in front in order to achieve the desired level of maxillary tooth display, grafting bone to fill in the gap created by the rotation. Then the mandible is also operated on, rotating it down in the anterior so the occlusion fits. This approach leaves the molars in a position similar to where they were pre-surgically, and does not increase the length of the masseter and medial pterygoid muscles, which is why it produces a much more stable result.
The overall outcome is an increase in tooth display, a normalising of the facial vertical proportions, and a much more pleasing overall aesthetic result. Attempting to treat these individuals without orthognathic surgery is usually a significant compromise in both tooth display and facial aesthetics (Figs 16,17,18,19).
Anterior maxillary deficiency
In addition to the potential for the maxilla to not develop vertically to a normal level, it is also possible for it to be deficient in its anterior development. This results in a concave facial profile and a tendency towards a Class III occlusal relationship. From the perspective of tooth display, the amount of tooth displayed at rest and in a full smile is highly dependent upon the severity of the deficiency, and whether the deficiency is just anterior or there is a vertical deficiency as well.
Again, since most general practitioners are not routinely taking cephalometric radiographs, the use of photographs can be helpful in diagnosis, particularly a lateral image of the face.24 To evaluate the profile, identify three landmarks on the photograph, the glabella (the prominent point between the eyebrows), subnasale (the point at the base of the nose as it transitions onto the upper lip) and finally, the pogonion (the most prominent point of the chin). Instead of measuring the distance between the points, this time draw a line from glabella to subnasale, and a second line from subnasale to pogonion, and then measure the angle formed by the two lines.
While there are multiple variations of what a normal or ideal facial profile is, noting that it varies significantly based upon ethnicity, a Class I facial profile will typically have an angle of between 165 to 175 degrees. An angle which is less than 165 degrees means the patient has a more convex profile, and potentially a deficient mandible or chin; angles over 180 degrees means the patient has a flat to concave profile, and either a deficient maxilla, or a protrusive mandible. The more exaggerated the variation from normal the more likely orthognathic surgery may be required to correct it if ideal tooth display and facial appearance is the goal.
If the profile tends towards flat to concave, and the occlusal relationship and the facial profile are acceptable but the tooth display is unacceptable, then lengthening the teeth and/or making them more prominent through a combination of orthodontics and restorative dentistry (or orthodontics alone, or restorative dentistry alone) as described previously can often result in a level of tooth display that is pleasing to the patient without any orthognathic surgery.
If, however, the profile is strongly concave, the occlusal relationship unacceptable, because it is full or strongly Class III, and the patient desires a much fuller smile, then orthognathic surgery to advance the maxilla is the only option that can produce an ideal result.25 The good news is, more often than not, the surgery does not need to address the mandible, just the position of the maxilla, moving it to correct the anterior tooth position and display, while conventional orthodontics can then be used to finalise the occlusion (Figs 20,21,22).
The other major aetiology for inadequate tooth display, besides incorrect tooth position, is inadequate tooth length. There are several reasons the teeth can small, and of course the tooth position must be taken into account when making a diagnosis and developing a treatment plan.
Inadequate tooth length
Potential aetiologies for inadequate tooth display in patients with inadequate tooth length
These include:
-
Tooth wear without compensatory eruption
-
Tooth wear with compensatory eruption
-
Abnormal eruption patterns, altered passive or active eruption.
Tooth wear without compensatory eruption
A common reason for inadequate tooth display in adults is tooth wear without compensatory eruption, simply put, as the teeth get shorter, the amount of tooth display decreases to match the amount of wear. For tooth wear to occur without compensatory eruption of the maxillary anterior teeth, one of three things has to occur: the patient develops an anterior open bite which increases as the teeth wear, not a very common finding; or the mandibular anterior teeth erupt to maintain occlusal contact, now becoming more visible aesthetically; or the patient loses vertical dimension to maintain occlusal contact.
Some keys to understanding what has happened for your patient is to understand that for the patient to lose vertical dimension, there has to have been wear or loss of the posterior teeth. If you see a patient with unworn posterior teeth, but severe anterior wear, and the anterior teeth are in occlusion, it is almost guaranteed that there has been some compensatory eruption of either the maxillary or mandibular anterior teeth, or both.
The classic example of a patient with inadequate tooth display from tooth wear, who has not had compensatory eruption, is the patient who has wear on all their teeth, and when you determine how much tooth structure will need to be added to the incisal edges to correct the inadequate tooth display, the teeth end up the correct length. In other words no changes in gingival position are necessary to create acceptable length anterior teeth.
This finding is strong evidence for a lack of compensatory eruption. In these patients it is often necessary to increase the vertical dimension to accommodate the increased tooth length (Figs 23,24,25).26,27,28
Not all cases of anterior tooth wear without eruption have wear on all teeth, but if they have not lost vertical dimension there will have to be an anterior open bite, or eruption of the mandibular anteriors. In the case of the open bite, the wear is usually from acid erosion, and there is room to restore the teeth, so the restoration is generally easy and predictable. In the case where the worn anterior teeth are in occlusion, due to the secondary eruption of the mandibular anteriors, it will be necessary to correct the mandibular anterior position with orthodontic intrusion, or alter their length with crown lengthening followed by restoration to create the necessary room to restore the maxillary anterior teeth.
Tooth wear with compensatory eruption
The strongest evidence that a patient has had compensatory eruption of their maxillary anterior teeth as their teeth have worn is when you find that correcting the position of the teeth for ideal tooth display results in teeth that are still too short in length. In other words, it will be necessary to alter the gingival levels and, often, the papilla levels to correct the length of the teeth, not just add to the incisal edges.
The amount of compensatory eruption varies dramatically from patient to patient, with some teeth erupting to the extent that even with severe wear their incisal edge position stays level with the unworn posterior occlusal plane. In these individuals their smile transforms from being normal when they are young, to displaying shorter and shorter teeth, but more and more gingiva as they age and experience dentoalveolar extrusion due to the tooth wear. In these individuals the challenge is correcting the eruption/extrusion, most commonly through orthodontic intrusion or crown lengthening surgery, although sometimes orthognathic surgery can be used as well.
In cases of extreme compensatory eruption, four things should be looked at in determining whether orthodontic intrusion or crown lengthening surgery might be the better choice:
-
Root length – clinically determine how many millimetres of gingival change will be necessary to correct the tooth length. Go to a radiograph and identify the existing osseous crest, then move apically the distance you would need to crown lengthen. Evaluate the amount of root that would be left in bone following the surgery; my general rule is to always try and leave at least 8 mm of root in bone on anterior teeth following surgery. If the roots are not long enough to achieve that, orthodontic intrusion is probably a better choice than surgery
-
Remaining tooth structure – evaluate the amount of exposed tooth structure relative to your ability to create retention and resistance form for a restoration. In severe wear cases there is often very little tooth structure left, this creates a challenge if orthodontic intrusion is used. Not that the orthodontics can't be done, but after the orthodontics is completed it will be necessary to determine how you will restore the teeth, often considering crown lengthening to expose more tooth structure, which will now make the teeth too long due to the prior intrusion. In cases where minimal tooth structure is available, if the root length is adequate, crown lengthening may be the preferred treatment, as it not only repositions the gingiva and papilla, but provides the necessary tooth structure for a restoration as well (Figs 26,27,28)
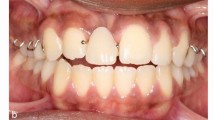
Figure 26 Figure 27: The patient's incisal edges show 3 mm at rest, and are level with the occlusal plane. -
Tooth inclination – evaluate whether the over-erupted anterior teeth are proclined or retroclined in the alveolar housing. Crown lengthening is very predictable on well aligned teeth, with the only long-term issue being a rebound of tissue over time. However, crown lengthening teeth that are proclined or retroclined is far less predictable relative to the position of the final gingival margins.29,30,31 In addition orthodontic correction of the tooth inclination can accompany the necessary intrusion to correct the gingival levels, and often also improves the anterior occlusal relationships, particularly when the maxillary anterior teeth are retroclined
-
Contact length – this variable is both an aesthetic and restorative technique issue. In unworn, well aligned, anterior teeth, the length of the contact between the central incisors, defined as the distance from the papilla to the bottom of the incisal embrasure, is equal to the height of the papilla, defined as the distance from the gingival margin to the tip of the papilla.32 For the purposes of treatment planning worn teeth, since the incisal embrasure is frequently worn away, I try to plan for the tip of the papilla to be 5–6 mm from the incisal edges of the restorations on the centrals, with the other anterior papillae at the same level, and a papilla height of 4.5 to 5 mm between the centrals.
As teeth wear the contact length decreases, so in cases of teeth which have worn and erupted it is necessary to apically position both the gingival margin and the papilla, but the outcome is vastly different if it is treated with orthodontic intrusion rather than crown lengthening. If intrusion is carried out, the normal relationship of the gingiva to the cementoenamel junction (CEJ) and bone is maintained both interproximally and facially, meaning there are no open embrasures, and the restorations can be prepped conservatively and on enamel. If crown lengthening is carried out, on the facial there will be root exposure, and interproximally there will be open embrasures, meaning the preps will have to go through the interproximal and onto the root. This does not mean crown lengthening should not be used, but if a patient is willing to do the orthodontics and there is adequate tooth structure to restore, it allows for a more conservative, restorative approach.
Abnormal eruption patterns
The final reason, under discussion in this article, for a smile that is not as full and pretty as a patient may desire, is also one of the easiest to correct – namely, teeth that are correctly positioned and unworn but which are small due to a lack of the normal apical migration of the gingiva. There are two aetiologies which produce abnormal gingival levels: one is altered passive eruption, the bone and CEJ levels are in a normal relationship, approximately 1.5–2 mm apart, but there is excess sulcus depth due to a lack of normal gingival recession to within 1–2 mm of the CEJ.
In these patients the key diagnostic feature is that the CEJ is easily felt at the base of the sulcus, and there is excess sulcus depth, perhaps 3-5 mm. Treatment is generally a simple gingivectomy, removing the excess tissue and leaving a normal sulcus depth after surgery. This condition is particularly common following orthodontics, where there may be gingival hyperplasia that occurs.
The second aetiology is altered active eruption, where the teeth do not erupt to a normal level relative to the crest of bone, leaving the CEJ at or below the osseous crest. The hallmark of these patients is the inability to feel the CEJ through the sulcus with a probe or explorer. In addition a radiograph will show interproximally that the CEJ and bone are at the same level. In these patients the only way to correct the tooth size long term is to lay a flap and remove facial bone so it is 2 mm apical to the CEJ, and then replace the flap so it is 3 mm coronal to the bone, 1 mm coronal to the CEJ. This produces normal sized teeth, which provides the desired full smile, assuming they are correctly positioned.
Conclusions
The purpose of this paper has been to identify many of the common aetiologies which can produce inadequate tooth display, recognising that often, for the restorative dentist, the belief is that inadequate tooth display is thought of as the teeth being too small, and therefore correctable with restorations. It is my hope that this paper can aid in the diagnosis and treatment choices clinicians consider when treating this challenging problem.
References
Zachrisson B U . Esthetic factors involved in anterior tooth display and the smile. J Clin Orthod 1998; 32: 432–445.
Vig R G, Brundo G C . The kinetics of anterior tooth display. J Prosthet Dent 1978; 39: 502–504.
Al Wazzan K A . The visible portion of anterior teeth at rest. J Contemp Dent Pract 2004; 5: 53–62.
Al-Habahbeh R, Al-Shammout R, Al-Jabrah O, Al-Omari F . The effect of gender on tooth and gingival display in the anterior region at rest and during smiling. Eur J Esthet Dent 2009; 4: 382–395.
Sackstein M . Display of mandibular and maxillary anterior teeth during smiling and speech: age and sex correlations. Int J Prosthodont 2008; 21: 149–151.
Van Der Geld P, Oosterveld P, Berge S J, Kuijpers-Jagtman A M . Tooth display and lip position during spontaneous and posed smiling in adults. Acta Odontol Scand 2008; 66: 207–213.
Polo M . Botulinum toxin type A in the treatment of excessive gingival display. Am J Orthod Dentofac Orthop 2005; 127: 214–218.
Polo M . Botulinum toxin type A (Botox) for the neuromuscular correction of excessive gingival display on smiling (gummy smile). Am J Orthod Dentofacial Orthop 2008; 133: 195–203.
Silva C O, Ribeiro-Júnior N V, Campos T V, Rodrigues J G, Tatakis D N . Excessive gingival display: treatment by a modified lip repositioning technique. J Clin Periodontol 2013; 40: 260–265.
Van der Geld P, Oosterveld P, Kuijpers-Jagtman A M . Age-related changes of the dental aesthetic zone at rest and during spontaneous smiling and speech. Eur J Orthod. 2008; 30: 366–373.
Woelfel J B, Igarashi T, Dong J K . Faculty-supervised measurements of the face and of mandibular movements on young adults. J Adv Prosthodont 2014; 6: 483–490.
Patel J R, Prajapati P, Sethuraman R, Naveen Y G . A comparative evaluation of effect of upper lip length, age and sex on amount of exposure of maxillary anterior teeth. J Contemp Dent Pract 2011; 12: 24–29.
Maloney B P . Cosmetic surgery of the lips. Facial Plast Surg 1996; 12: 265–278.
Ngan P, Fields H W . Open bite: a review of aetiology and management. Paediatr Dent 1997; 19: 91–98.
Kokich V G . Esthetics and vertical tooth position: orthodontic possibilities. Compend Contin Educ Dent 1997; 18: 1225–1231.
Zachrisson B U . Making the premolar extraction smile full and radiant. World J Orthod 2002; 3: 260–265.
Zachrisson B U . Premolar extraction and smile esthetics. Am J Orthod Dentofacial Orthop 2003; 124: 11A–12A.
Arnett G W, Bergman R T . Facial keys to orthodontic diagnosis and treatment planning. Part I. Am J Orthod Dentofacial Orthop 103: 299–312.
Arnett G W, Bergman R T . Facial keys to orthodontic diagnosis and treatment planning. Am J Orthod Dentofacial Orthop 103: 395–411.
Costa F, Robiony M, Politi M . Stability of Le Fort I osteotomy in maxillary inferior repositioning: review of the literature. Int J Adult Orthodon Orthognath Surg 2000; 15: 197–204.
Convens J M, Kiekens R M, Kuijpers-Jagtman A M, Fudalej P S . Stability of Le Fort I maxillary inferior repositioning surgery with rigid internal fixation: a systematic review. Int J Oral Maxillofac Surg 2015; 44: 609–614.
Costa F, Robiony M, Zerman N, Zorzan E, Politi M . Bone biological plate for stabilization of maxillary inferior repositioning. Minerva Stomatol 2005; 54: 227–236.
Mehra P, Castro V, Freitas R Z, Wolford L M . Stability of the Le Fort I osteotomy for maxillary advancement using rigid fixation and porous block hydroxyapatite grafting. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2002; 94: 18–23.
Rustemeyer J, Martin A . Soft tissue response in orthognathic surgery patients treated by bimaxillary osteotomy: cephalometry compared with 2D photogrammetry. Oral Maxillofac Surg 2013; 17: 33–41.
Ghassemi M, Hilgers RD, Jamilian A et al. Effect of maxillary advancement on the change in the soft tissues after treatment of patients with class III malocclusion. Br J Oral Maxillofac Surg 2015; 10.1016/j.bjoms.2015.06.001.
Tallgren A . Changes in adult face height due to ageing, wear and loss of teeth and prosthetic treatment. Acta Odontol Scand 1957; 15(Supp 24): 73.
Gross M D, Nissan J, Ormianer Z, Dvori S, Shifman A . The effect of increasing occlusal vertical dimension on face height gross. Int J Prosth 2002 15: 353–357.
Dahl B L, Krogstad O . Long-term observations of an increased occlusal face height obtained by a combined orthodontic/prosthetic approach. J Oral Rehabil 1985; 12: 173–176.
Deas DE, Moritz A J, McDonnell H T, Powell C A, Mealey B L . Osseous surgery for crown lengthening: a 6month clinical study. J Periodontol 2004; 75: 1288–1294.
Arora R, Narula S C, Sharma R K, Tewari S . Evaluation of supracrestal gingival tissue after surgical crown lengthening: a 6month clinical study. J Periodontol 2013; 84: 934–940.
Hämmerle C H, Giannobile W V . Biology of soft tissue wound healing and regenerationconsensus report of Group 1 of the 10th European Workshop on Periodontology. J Clin Periodontol 2014; 41 (Suppl 15): S1–S5.
Raj V, Heymann H O, Hershey H G, Ritter A V, Casko J S . The apparent contact dimension and covariates among orthodontically treated and nontreated subjects. J Esthet Restor Dent 2009; 21: 96–111.
Author information
Authors and Affiliations
Corresponding author
Additional information
Refereed Paper
Rights and permissions
About this article
Cite this article
Spear, F. Diagnosing and treatment planning inadequate tooth display. Br Dent J 221, 463–472 (2016). https://doi.org/10.1038/sj.bdj.2016.773
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.bdj.2016.773
This article is cited by
-
Matrix transfer techniques for direct paste composite resins
British Dental Journal (2022)