Abstract
Vitamin D is necessary for the healthy growth and development of bone and muscle. Vitamin D deficiency, which is present in 42% of the US population, is often undiagnosed as symptoms may not manifest for several years and long-term deficiency has been linked to osteoporosis, diabetes and cancer. Currently the majority of vitamin D testing is performed in large-scale commercial laboratories which have high operational costs and long times-to-result. Development of a low-cost point-of-need assay could be transformative to deficiency analysis in limited-resource settings. The best biomarker of vitamin D status, 25hydroxyvitamin D3 (25(OH)D3), however, is particularly challenging to measure in such a format due to complexities involved in sample preparation, including the need to separate the marker from its binding protein. Here we present a rapid diagnostic test for the accurate, quantitative assessment of 25(OH)D3 in finger-stick blood. The assay is accompanied by a smartphone-assisted portable imaging device that can autonomously perform the necessary image processing. To achieve accurate quantification of 25(OH)D3, we also demonstrate a novel elution buffer that separates 25(OH)D3 from its binding protein in situ, eliminating the need for sample preparation. In human trials, the accuracy of our platform is 90.5%.
Similar content being viewed by others
Introduction
Vitamin D refers to a group of fat soluble secosteroids responsible for promoting absorption of calcium, phosphate and zinc in the body1,2. It is also essential for the healthy growth and maintenance of bone and muscle3MEP_L_bib3. Vitamin D deficiency causes rickets in children4MEP_L_bib4 and low levels of vitamin D have been attributed to diabetes, heart disease, cancer and osteoporosis in adults5MEP_L_bib5. Vitamin D is also critical for ensuring optimal immune function; for example, vitamin D is required for producing antimicrobial peptides such as cathelicidin, necessary to combat pathogens such as Mycobacterium tuberculosis in human macrophages6MEP_L_bib6. Deficiency is defined by evaluating the serum concentrations of 25-hydroxyvitamin D, or 25(OH)D, a pro-hormone that is produced in the liver by hydroxylation of cholecalciferol, the biologically inert form of vitamin D that is produced in the skin. 25(OH)D is the major circulating form of vitamin D and is considered the best indicator of holistic vitamin D status. Supplemental vitamin D is available in two forms: ergocalciferol (vitamin D2) and cholecalciferol (vitamin D3). Even though commonly prescribed supplements contain either vitamin D2 or vitamin D3, it has been demonstrated that cholecalciferol has a higher efficacy at raising the total serum 25(OH)D status in individuals7,8. As a result, many of the supplements now on the market contain cholecalciferol. The Endocrine Society guidelines suggest that individuals with serum concentration of 25(OH)D greater than 75 nmol/L can be considered healthy while those with values between 50 and 75 nmol/L are insufficient and lower than 50 nmol/L are deficient9MEP_L_bib9.
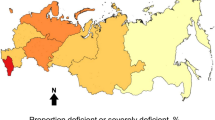
In the United States, the prevalence of vitamin D deficiency rate is estimated at 42%, with a higher incidence amongst the African American (82%) and Hispanic (69%) population10MEP_L_bib10. Deficiency can be corrected with supplementation and dietary changes particularly when detected early; however, many people are unaware of their status due to the lack of easy to access methods for quantifying 25(OH)D3 levels in human serum. Point-of-care vitamin D deficiency testing remains a significant challenge due to the presence of vitamin D binding protein, a carrier protein that helps transport 25(OH)D in blood. 95–99% of available 25(OH)D in blood is bound to vitamin D binding protein11,12 and due to the nature of the strong hydrophobic bond between them, it is not possible to assess an individual’s vitamin D status without separating the two from each other. Furthermore, vitamin D binding protein is always present in significant molar excess in blood and has no correlation with the amount of circulating 25(OH)D13,14,15. As a result, it cannot be used as a target itself, a scheme which has been adopted for targets such as vitamin A16,17,18,19.
Current clinical methods for quantitation of 25(OH)D can be broadly divided into chromatographic methods with (LC/MS-MS: Liquid Chromatography Tandem Mass Spectrometry) and without (HPLC: High Performance Liquid Chromatography) mass spectrometric detection and competitive immunoassays such as RadioImmunoAssay (RIA). These techniques are expensive and time consuming due to the need for specialized equipment and personnel and the necessity to separate and remove vitamin D binding protein presents further complications by requiring elaborate sample preparation. Usually the sample is treated and incubated (for ~1 hour) with large amounts of organic solvents such as acetonitrile to perform the separation step. Further, organic solvents cannot be used directly with blood as they cause lysis of blood cells, and require that the blood be centrifuged into serum. Standard protocols also require an additional centrifugation step after the organic solvents are added in order to remove the precipitated protein. These tedious sample preparation requirements combined with the need for specialized equipment pose a severe limitation for the development of point-of-need tests for the assessment of vitamin D status.
In recent years, several research groups have employed microfluidic techniques to develop low cost methods to assess micronutrient status at the point-of-need. A microfluidic chip that was able to perform the detection of ferritin and CRP in human serum samples was demonstrated by Kartalov et al.20MEP_L_bib20. Similarly, Dimov et al. exhibited the “stand-alone self-powered integrated microfluidic blood analysis system (SIMBAS)” for detection of vitamin B6 21MEP_L_bib21. While these works have demonstrated excellent proof of concepts for use at the point of care, they are limited by their inability to perform blood processing on chip and the need for expensive imaging equipment. Lee et al.22MEP_L_bib22 demonstrated the vitamin AuNP-based Immunoassay Device (vitaAID), a system for quantification of vitamin D levels using a smartphone. In that work, a novel gold nanoparticle based immunoassay architecture was developed and analyzed by a smartphone camera, enabling quantification of serum samples without the need for expensive lab equipment. Even though the method helped transition vitamin D testing out of the lab, the technique was limited by its inability to perform blood processing on chip and non-trivial incubation time (~6 hours).
In this work, we present a rapid diagnostic test that is capable of accurate, quantitative assessment of vitamin D status. Our test focuses on quantification of 25(OH)D3, the largest component of circulating 25(OH)D, in the deficient range ( < 50nmol/L), as that is where the greatest need is. Quantitative ability is necessary in the deficient range to help distinguish between individuals who are severely and moderately deficient. In order to maintain compatibility with existing manufacturing techniques, we developed our diagnostic test as a lateral flow assay. Furthermore, our diagnostic test is integrated into a smartphone-assisted imaging platform which allows for easy operation and hassle-free access to test results. In addition to being capable of processing blood on strip, our test incorporates a novel elution buffer that is compatible with lateral flow assays to achieve separation of 25(OH)D3 from its binding protein in situ, eliminating the need for any sample preparation. We show reliable quantification of physiologically relevant vitamin D3 levels in standard solutions, commercial calibrators, human serum and finger stick blood.
Results
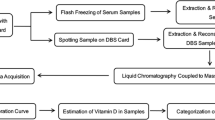
Vitamin D3 diagnostic test protocol: The system consists of a vitamin D3 diagnostic test, custom made cassette that houses the test and a portable reader (TIDBIT) (See Fig. 1). The TIDBIT has been designed so that when the cassette is inserted into the device, it is aligned with a CMOS camera that automatically captures an image of the test area. The TIDBIT can be operated via a smartphone or computer application and can be controlled with the help of the Nutriphone application. Once the image is taken, a custom python script automatically crops the image and deduces the ratio of intensities of the test line to the control line, or T/C ratio (See Fig. 2B and C). The T/C ratio is correlated to a value of 25(OH)D3 by using a calibration curve, that is determined prior to testing by analyzing samples of known 25(OH)D3 values.
To run a vitamin D3 test, the user starts the Nutriphone application on the device of choice and follows the instructions. First the user applies a small amount (4 µL) of elution buffer on the edge of the sample pad. The user then collects 40 µL of blood from a finger prick and places it onto the sample collection pad. After allowing for the blood to separate into serum and mix with the elution buffer, the user is prompted by the smartphone application to apply 15 µL of running buffer for the filtered serum to enter the conjugate pad. After another short period of incubation, the user is again prompted to add 25 µL of running buffer to start the test. Following this step, the user must place the cassette in the TIDBIT, which automatically images and analyzes the test strip when the test and control lines are fully developed. Briefly, a grayscale image is taken using the TIDBIT and processed by a python script to filter out the noise using a Gaussian filter. The noisy 2D image is filtered and converted to the grayscale, followed by a median filtering process to convert the 2D image into a 1D array, reducing the task to analyzing a 1D digital signal. The test and control lines of concentrated AuNP – anti 25(OH)D3 are detected as local minima on the intensity plot. The respective peak values can be used to calculate a T/C ratio.
Design and implementation of a protein elution buffer
Vitamin D binding protein interferes with the capture and quantification of 25(OH)D3 via traditional immunoassay techniques. Commercial tests such as the DiaSorin RIA call for mixing the sample with 10X the amount of acetonitrile, an organic solvent, in order to liberate all 25(OH)D3 in the sample from the binding protein23MEP_L_bib23. This method cannot be directly translated for application with a low-cost point-of-need lateral flow platform for several reasons. Firstly, organic solvents cause lysis of red blood cells24MEP_L_bib24, making it unsuitable for use with blood samples; the sample must be first spun down into serum via centrifugation, a process that is difficult to perform in point-of-need settings. Secondly, if not neutralized or removed prior to running the test, acetonitrile could negatively affect the conjugated gold nanoparticles and the dispensed reagents on the test and control lines as the antibodies present are prone to denaturation themselves. Finally, adding large amounts of organic solvent is particularly unsuitable for lateral flow platforms, as they may adsorb to the nitrocellulose membrane and alter its wetting properties25MEP_L_bib26. It was therefore necessary to develop an elution buffer that could denature binding protein in the sample without lysing blood cells while maintaining compatibility with the nitrocellulose membrane, the conjugated nanoparticles and the dispensed reagents.
In order to perform the separation of 25(OH)D3 from its binding protein, our diagnostic test takes advantage of carefully optimized organic solvents and low pH buffers, which are known to be effective at denaturing proteins. After assessing a number of possible combinations, we decided on a combination of Dimethyl sulfoxide (DMSO), ethanol and a low pH acetate buffer. We hypothesize that DMSO and ethanol are able to unfold vitamin D binding protein while also serving as organic solvents to stabilize the liberated 25(OH)D3 26MEP_L_bib25. This unfolding effect is further enhanced in the presence of a low pH buffer as most proteins undergo destabilization at low pH25MEP_L_bib26. As seen in Fig. 3B, there is no relationship between [25(OH)D3] and the T/C ratio when samples are tested for vitamin D3 without the use of any elution buffer.
Elution Buffer. (A) Elution of 25(OH)D3 from binding protein with the help of organic solvents and low pH buffer and (B) Calibration curve obtained from analyzing samples without the use of elution buffer. As seen, there is no relationship between [25(OH)D3] and T/C ratio without the use of the elution buffer.
Vitamin D3 diagnostic test architecture and principles
The vitamin D3 diagnostic test seen in Fig. 2 consists of a: blood filtration membrane, a conjugate pad that dry stores gold nanoparticle conjugates (AuNP – anti 25(OH)D3), a spacer pad that allows for incubation of the sample with the elution buffer and the conjugates, a nitrocellulose membrane that houses immobilized 25(OH)D3-BSA and secondary antibodies and a cellulose fiber absorbent pad respectively. When applicable, the blood filtration membrane can be substituted for a cellulose fiber pad to perform testing in human serum. Our test strip adopts a competitive type architecture as 25(OH)D3 is unable to bind to more than one antibody at a time due to its small size (~350 Daltons).
The architecture of the diagnostic test was designed in order to prevent any need for specialized sample preparation. Prior to starting the test, the user dispenses a small amount of elution buffer onto the front edge of the blood filtration membrane to prevent the interaction of the elution buffer and the red blood cells present in the blood sample. Once the user dispenses the blood on the sample pad, it automatically flows forward through the filtration paper and separates into serum while simultaneously mixing with the elution buffer. This causes bound 25(OH)D3 to be released from the binding protein present in the sample. After the first instance of running buffer is applied, the sample enters the conjugated pad and the unbound 25(OH)D3 interacts with the AuNP-anti 25(OH)D3 conjugates. This step is critical for the proper functioning of the assay. Based on the amount of 25(OH)D3 in the sample, there is a competitive interaction between the immobilized 25(OH)D3-BSA on the nitrocellulose and the 25(OH)D3 in the sample for binding sites on the AuNP-antibody conjugates as the sample flows through the nitrocellulose. As seen in Fig. 2B, an individual with vitamin D3 deficiency will observe a T/C ratio that is high as most binding sites on the conjugates will be empty and free to bind to the immobilized 25(OH)D3. Conversely, an individual with healthy levels of 25(OH)D3 will observe a T/C ratio that is low as most of the binding sites on the conjugates are occupied with 25(OH)D3 from the sample which prevents them from binding at the test line (Fig. 2C).
25(OH)D3 quantification in standard solution and commercial calibrators
In Fig. 4A, we demonstrate that the T/C ratio can be correlated to a 25(OH)D3 concentration in standard solutions. At each concentration, two strips were used and the maximum lower and upper deviations from the average T/C values were shown. The coefficient of variation of our assay ranges from 1.7% at 100 nmol/L to 14.7% at 125 nmol/L. We then fitted a linear curve such that [25(OH)D3] = f(T/C). We also tested the performance our assay with standard solutions that were spiked with 25(OH)D2 in order to evaluate the cross-reactivity of the assay (inset in Fig. 4A). To verify the accuracy of the assay in serum, 25(OH)D3 levels were also quantified in commercially available serum based standards (ChromSystems Inc). The calibrators are based on pooled human serum and contain artificially spiked values of 25(OH)D3 that lie in the physiologically relevant range. As seen in Fig. 4B, our assay is able to reliably distinguish between a deficient, insufficient and healthy sample. These standards did not require the use of the elution buffer as these samples were prepared by artificially introducing 25(OH)D3 into the sample. The coefficient of variation of our assay ranges from 2.63% at 85 nmol/L to 11.2% at 0 nmol/L.
Calibration curve in standards. (A) T/C ratios of the colorimetric signals at different 25(OH)D3 concentration in standard buffers. T/C ratio = a[25(OH)D3] + b, where a = −0.0251 and b = 3.983. Linear logistic curve was fitted with R2 = 0.95. The inset demonstrates a calibration curve performed with standard buffers that were spiked with 25(OH)D2 to verify cross-reactivity. A linear logistic curve was fitted with R2 = 0.0059 indicating no dependence of T/C ratio on [25(OH)D2] (B) T/C ratios of the colorimetrics signals at different 25(OH)D3 concentrations in commercial serum based calibrators. T/C ratio \(={\boldsymbol{d}}+\frac{{\boldsymbol{a}}-{\boldsymbol{d}}}{1+{(\frac{[25({\boldsymbol{OH}}){\boldsymbol{D}}3]}{{\boldsymbol{c}}})}^{{\boldsymbol{b}}}}\), where a = 2.81, b = 2.63, c = 26.2 and d = 1.52. A four parameter logistic curve was fitted with R2 = 0.99. At each concentration two strips were used and the maximum and minimum deviation from the average is shown as error bars.
Vitamin D3 deficiency testing in human serum
Our assay was used to quantify the vitamin D3 levels in human serum samples that were collected from a human trial to demonstrate the assay’s applicability in the clinical setting (Fig. 5A,B and C). Native serum samples required the use of elution buffer to separate 25(OH)D3 from vitamin D binding protein. As expected of our competitive type architecture, the T/C ratio for a participant with vitamin D deficiency appears to be significantly greater than that of a participant with vitamin D insufficiency. Actual serum 25(OH)D3 values were quantified using tandem liquid chromatography/mass spectrometry (LC/MS-MS). Figure 5B shows a ROC curve for the serum tests based on a linear calibration curve that was determined from the same batch of test strips (Fig. 5A). We used the DeLong method27MEP_L_bib27 to obtain an asymptotically exact method to evaluate the area under curve (auc) using 300,000 iterations with a cutoff of 50 nmol/L. A similar method was used to evaluate the performance of the assay at a cutoff of 30 nmol/L28MEP_L_bib28 that can be seen in Fig. 5C. Diagnostic accuracy, defined as the proportion of correctly classified subjects to all subjects, was evaluated as 90.5% and 100% for the two cutoffs respectively. Both cutoffs are based on recommendations made by the Institute of Medicine. The root mean square error was assessed to be 5.4 nmol/L. The coefficient of variation ranged from 0.05% at 43 nmol/L to 16.6% at 57 nmol/L.
Analysis of human trial samples (A) Linear calibration curve for 21 human serum samples with R2 = 0.91. T/C ratio = a[25(OH)D3] + b where a = −0.075 and b = 5.689 (B) ROC curve obtained with Delong method with n = 300000 and auc 0.836 at a cutoff of 50nmol/L (C) ROC curve obtained from Delong method with n = 300000 and auc 1 at a cutoff of 30 nmol/L (D) Calibration curve from 6 human finger stick blood samples with R2 = 0.94. T/C ratio = a[25(OH)D3] + b where a = −0.033 and b = 2.9925.
Vitamin D3 deficiency testing in finger prick blood samples
We used our assay to quantify vitamin D3 levels in finger prick blood from volunteers after obtaining informed consent, as per a protocol approved by the Institutional Review Board at Cornell University. Samples were run and analyzed at the site of the trial. Figure 5D demonstrates a calibration curve for the sample set with R2 value of 0.94. From Fig. 5D, it is apparent that our assay demonstrates a linear correlation between the T/C ratio and [25(OH)D3]. Additionally, by observing the change in T/C ratio, we are able to demonstrate that our test can distinguish between a severely deficient, deficient and insufficient participant with reasonable certainty. The coefficient of variation ranged from 0.5% at 39 nmol/L to 17.2% at 48 nmol/L.
Discussion
In this work, we demonstrate a rapid and easy to use microfluidic platform for the assessment of vitamin D status. We showed the quantification of 25(OH)D3 in the physiologically relevant range within minutes. This was achieved by using a competitive type lateral flow assay that incorporates a novel elution buffer which separates 25(OH)D3 from its binding protein on the strip, therefore eliminating the need for tedious sample preparation. The assay produces a colorimetric image that can be analyzed to obtain a T/C ratio that can be correlated to a concentration of 25(OH)D3 in the sample (serum or blood). We further validate the system by quantifying levels in trivial amounts of human serum and a finger prick of blood. Given the limitations of traditional clinical diagnostic methods, our assay has the potential to make an immediate impact in the point-of-need setting as an accurate tool for the assessment of vitamin D3 status.
Our work presented here is the first quantitative, point-of-need diagnostic test for the assessment of vitamin D3 status and represents a critical step towards transitioning vitamin D deficiency testing out of the lab and into the hands of individuals. Unlike commercial platforms that have been developed for micronutrient testing, our test is able to process finger stick blood, denature vitamin D binding protein in situ and quantify levels of 25(OH)D3 in the sample in a few minutes without the need for expensive equipment. These unique traits coupled with a high diagnostic accuracy (90.5%) make our test sufficient for application at the point of need. Our assay is designed specifically for assessing 25(OH)D3 status in the deficient range ( < 50 nmol/L) as this is where differentiation is most important. However, we have also demonstrated that our test is able to reliably quantify concentrations in the complete physiologically relevant range (0–150nmol/L). Since our assay is unable to detect 25(OH)D2, the quantitative ability is limited when used in settings where ergocalciferol is the preferred supplement. However, the recent uptake in vitamin D3 supplementation suggests that our diagnostic test is practical for use in many point-of-need settings29,30. Given the minimal amount of expertise needed to run the assay, our test enables individuals to evaluate their own vitamin D status irrespective of their medical training or knowledge. The low cost and portability of the testing platform will also make monitoring and evaluation of the efficacy of nutritional interventions feasible in both research and programmatic settings. Furthermore, we have developed a protein elution buffer that could be adopted to improve several other diagnostic tests that require specialized sample preparation because of the presence of a binding protein (vitamins A, B7 and B12).
Materials and Methods
The monoclonal anti-25(OH)D3 IgG produced in mouse (GenScript Inc) was conjugated with 40 nm Gold Nanoparticles using the InnovaCoat Gold Conjugation Kit (Innova Biosciences Ltd). For the conjugation, 0.23 µg AuNP in freeze dried form was mixed with 1ug anti 25(OH)D3 IgG in 0.01 M amine free phosphate buffer saline at pH 7.4. The anti-25(OH)D3 IgG is attached to the surface of AuNP via lysine residues during a 15-minute incubation and the reaction was terminated by adding 0.1 M tris-buffered saline (TBS) with 0.1% Tween 20. To remove excess antibodies, DI water was added in 10 times the volume of the conjugate mixture as centrifuged at 9000 g for 10 min. Upon removal of the supernatant, the final gold nanoparticle concentration was reconstituted in 0.01 M TBS containing 2% BSA and the final optical density was verified by using Spectramax 384 to measure absorbance of the conjugates at a wavelength of 530 nm. The conjugates were stored at 4 °C until use. Conjugate pads were prepared by first diluting the conjugates to roughly 0.7–0.8 OD (depending on application) in a conjugate buffer (2 mM Borate buffer with 5% sucrose) which contained appropriate preservatives. Glass Fiber conjugate pads (EMD Millipore) with 30cmx5 cm dimensions were soaked in diluted conjugate solution for 2 minutes followed by drying at 37 °C for a minimum of 12 h.
Vitamin D3 lateral flow assay preparation
Hi Flow Plus 180 membrane Cards (EMD Milipore) were used as the assay platform. The membrane cards have a 2mm clear polyester film backing that contains the nitrocellulose membrane and the adhesive that allows for assembly of conjugate and sample pads. The nitrocellulose part of the assay extends for 2.5 cm in length and has a nominal capillary flowrate of 45 seconds/cm. This is the slowest flow rate offered by the manufacturers and was chosen to allow for maximum reaction time between the sample and the conjugates due to the relatively low detection range. The test and control lines were prepared by using a Lateral Flow Reagent Dispenser (Claremont Bio) to dispense 0.4 mg/mL of anti-mouse IgG produced in goat and 1 mg/mL of 25(OH)D3-BSA. The two lines are separated by 3mm and have line widths of 1mm. These lines were dispensed using the Legato 200 Dual Syringe Pump (Claremont Bio) at 6.7 µL/min. Once the reagents were dispensed, they were dried for a minimum of 12 hours at 37 °C. The final assay was assembled by first applying the spacer pad onto the bottom of the nitrocellulose portion with 2–3mm overlap followed by a dried conjugate pad. The sample pad, which is the final component, varies based on the sample that is to be tested. Cellulose pads (EMD Milipore) were used for serum samples and FR1 blood filtration membranes (MDI membrane technologies) were used for blood samples. In both cases, the sample pad was attached below the conjugate pad with 2mm overlap. The FR-1 membrane has a thickness of 0.35 mm and capacity of 30 µL/cm2 and measured to be 30 cm × 2.5 cm while the Cellulose pad measured to be 30 cm × 1 cm. Another cellulose fiber sample pad was attached at the top of the nitrocellulose card to serve as an absorbent pad to collect any waste from the assay. The assembled assay was then cut into 4mm strips using a rotary paper trimmer. The strips were then kept sealed in a plastic container and wrapped in aluminum foil in a humidity controlled chamber (Secador) for a few days to prevent adverse effects of exposure to varying temperature and humidity. Test strips remain integral for up to several weeks while stored in these conditions. However, their shelf life can be extended up to a year if they are sealed in light safe mylar pouches and stored at room temperature.
Elution buffer preparation
A combination of organic solvents and low pH buffers was used to ensure the separation of vitamin D binding protein and 25(OH)D3 on strip. We mixed 4.7 parts of 1:1 mixture of Dimethyl sulfoxide (VWR) and Pure Ethanol (Acros Organics) with 1 part of pH 4.0 acetate buffer (VWR). In the case of finger prick blood testing, 4 µL of this mixed buffer was added to the area of overlap between the blood filtration membrane and the conjugate pad to allow for the filtered serum to interact with the elution buffer prior to the reaction with the conjugates. Elution buffer cannot be added directly to whole blood as the organic solvents cause lysing of blood cells. As for serum, the same amount of elution buffer was mixed in with the sample in a plastic 1.5 mL micro-centrifuge vial prior to applying the sample to the strip.
Vitamin D3 test strip protocol and human trials
Capillary tubes were used for the collection of constant amount of blood from the participants. First, 4 µL of elution buffer was pipetted onto the area of overlap between the sample pad and the conjugate pad. This allows for the filtered serum to interact with the elution buffer prior to the conjugates. Elution buffer is added prior to the interaction of the sample with the AuNP-anti 25(OH)D3 conjugates to avoid affecting the performance of the gold nanoparticles. Nanoparticle aggregation was observed when the conjugates are mixed directly with elution buffer. Additionally, adding elution buffer to the sample prior to incubation reduces the adverse effects of the elution buffer on the conjugates. After allowing for 4 minutes for the sample to filter into serum, 15 µL of running buffer is added to flow the sample and elution buffer mixture into the conjugate pad. After allowing for an additional four minutes of incubation, 25 µL of running buffer is added to start the flow onto the nitrocellulose membrane. At this point, the user inserts the cartridge into the imaging device. The imaging device automatically images the diagnostic test when the test and control lines are fully developed.
The human trials were approved by the Institutional Review Board for Human Subjects at Cornell University and carried out in accordance with their regulations. Informed consent was obtained from all participants prior to testing. For the trial, the participants were subjected to a finger prick (UniStik) for a drop of blood which was collected using a capillary tube and dispensed onto the sample pad. A trained and certified phlebotomist then drew 5 mL of blood via venipuncture which was used for tandem mass spectrometry analysis. Following 1 hour incubation at room temperature, serum was separated by centrifugation at 2000 g for 10 min. Serum 25(OH)D levels were characterized using tandem mass spectrometry (LC/MS-MS).
TIDBIT and image processing
Test strips were imaged using a portable imaging device designed specifically for colorimetric detection and quantification. The device consists of a 5 megapixel 1080p HD CMOS camera (Rasbperry Pi), focusing lens and LEDs (Thorlabs Inc), raspberry Pi computer board, rechargeable lithium ion battery pack (Adafruit Industries) and slide out cassette tray, all surrounded by a 3D printed light tight container. Once the cassette is inserted into the imaging device, it is automatically imaged and processed using a custom python script.
Data availability
All data generated or analyzed during the current study are available from the corresponding author on reasonable request.
References
Institute of Medicine. Dietary Reference Intakes for Calcium and Vitamin D. National Academies Press, Washington, DC; 2011.
Norman, A. W. From vitamin D to hormone D: fundamentals of the vitamin D endocrine system essential for good health. Am. J. Clin. Nutr. 88, 491S–499S (2008).
Calvo, M. S., Whiting, S. J. & Barton, C. N. Vitamin D Intake: A Global Perspective of Current Status. J. Nutr. 135, 310–316 (2005).
Wagner, C. L. & Greer, F. R. Prevention of Rickets and Vitamin D Deficiency in Infants, Children, and Adolescents. Pediatrics 122, 1142–1152 (2008).
Holick, M. F. Vitamin D: importance in the prevention of cancers, type 1 diabetes, heart disease, and osteoporosis. Am. J. Clin. Nutr. 79, 362–371 (2004).
Fabri, M. et al. Vitamin D Is Required for IFN-γ–Mediated Antimicrobial Activity of Human Macrophages. Sci. Transl. Med. 3, 104ra102–104ra102 (2011).
Houghton, L. A. & Vieth, R. The case against ergocalciferol (vitamin D2) as a vitamin supplement. Am. J. Clin. Nutr. 84, 694–697 (2006).
Tripkovic, L. et al. Comparison of vitamin D2 and vitamin D3 supplementation in raising serum 25-hydroxyvitamin D status: a systematic review and meta-analysis. Am. J. Clin. Nutr. 95, 1357–1364 (2012).
Holick, M. F. et al. Evaluation, Treatment, and Prevention of Vitamin D Deficiency: an Endocrine Society Clinical Practice Guideline. J. Clin. Endocrinol. Metab. 96, 1911–1930 (2011).
Forrest, K. Y. Z. & Stuhldreher, W. L. Prevalence and correlates of vitamin D deficiency in US adults. Nutr. Res. N. Y. N 31, 48–54 (2011).
Wootton, A. M. Improving the Measurement of 25-hydroxyvitamin D. Clin. Biochem. Rev. 26, 33 (2005).
Carter, G. D. Accuracy of 25-Hydroxyvitamin D Assays: Confronting the Issues. Curr. Drug Targets 12, 19–28 (2011).
Edelstein, S. Vitamin D Binding Proteins. Vitam. Horm. 32, 407–428 (1975).
Bikle, D. D. et al. Assessment of the Free Fraction of 25-Hydroxyvitamin D in Serum and Its Regulation by Albumin and the Vitamin D-Binding Protein. J. Clin. Endocrinol. Metab. 63, 954–959 (1986).
Bouillon, R., Assche, F. A. V., Baelen, H. V., Heyns, W. & Moor, P. D. Influence of the Vitamin D-binding Protein on the Serum Concentration of 1,25-Dihydroxyvitamin D3: Significance of the Free 1,25-Dihydroxyvitamin D3 Concentration. J. Clin. Invest. 67, 589 (1981).
Pee, Sde & Dary, O. Biochemical Indicators of Vitamin A Deficiency: Serum Retinol and Serum Retinol Binding Protein. J. Nutr. 132, 2895S–2901S (2002).
Hix, J. et al. Validation of a rapid enzyme immunoassay for the quantitation of retinol-binding protein to assess vitamin A status within populations. Eur. J. Clin. Nutr. 60, 1299–1303 (2006).
Craft, N. E. Innovative Approaches to Vitamin A Assessment. J. Nutr. 131, 1626S–1630S (2001).
Gamble, M. V. et al. Retinol binding protein as a surrogate measure for serum retinol: studies in vitamin A–deficient children from the Republic of the Marshall Islands. Am. J. Clin. Nutr. 73, 594–601 (2001).
Kartalov, E. P. et al. Internally calibrated quantification of protein analytes in human serum by fluorescence immunoassays in disposable elastomeric microfluidic devices. Electrophoresis 29, 5010 (2008).
Dimov, I. K. et al. Stand-alone self-powered integrated microfluidic blood analysis system (SIMBAS). Lab. Chip 11, 845–850 (2011).
Lee, S., Oncescu, V., Mancuso, M., Mehta, S. & Erickson, D. A smartphone platform for the quantification of vitamin D levels. Lab. Chip 14, 1437–1442 (2014).
Laboratory Procedure Manual for Diasorin(formerly Incstar) 25-OH-D assay.
Tan, S. C. & Yiap, B. C. DNA, RNA, and Protein Extraction: The Past and The Present. J. Biomed. Biotechnol. 2009, (2009).
Tanford, C. Protein Denaturation. Adv. Protein Chem. 23, 121–282 (1968).
Arakawa, T., Kita, Y. & Timasheff, S. N. Protein precipitation and denaturation by dimethyl sulfoxide. Biophys. Chem. 131, 62–70 (2007).
DeLong, E. R., DeLong, D. M. & Clarke-Pearson, D. L. Comparing the areas under two or more correlated receiver operating characteristic curves: a nonparametric approach. Biometrics 44, 837–845 (1988).
Institute of Medicine. Dietary Reference Intakes for Calcium and Vitamin D. National Academies Press, Washington, DC; 1997.
Norman, A. W. Vitamin D: The Calcium Homeostatic Steroid Hormone. Academic Press (1979).
Erdman, J. W., MacDonald, I. A., Zeisel, S. H. Present Knowledge in Nutrition. International Life Sciences Institute (2012).
Acknowledgements
D.E. and S.M. acknowledge primary funding support for this effort from the National Science Foundation Award 1430092. The authors would also like to thank Olga Malyshev of the College of Human Ecology at Cornell for conducting tandem mass spectrometry diagnostics. The authors also thank Erica Bender for performing finger pricks and venipunctures for the human trials.
Author information
Authors and Affiliations
Contributions
Sasank Vemulapati (Principal Author) – Performed assay development, data collection, analysis and interpretation. Elizabeth Rey and Dakota O’Dell (Secondary Author) – Assisted in data collection and analysis in addition to designing imaging software. All co-authors contributed to writing and editing the paper.
Corresponding authors
Ethics declarations
Competing Interests
The authors declare the following competing financial interests(s): D.E., S.M. and D.O. have an equity interest in VitaScan which is commercializing similar micronutrient diagnostic technology that is described herein.
Additional information
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Vemulapati, S., Rey, E., O’Dell, D. et al. A Quantitative Point-of-Need Assay for the Assessment of Vitamin D3 Deficiency. Sci Rep 7, 14142 (2017). https://doi.org/10.1038/s41598-017-13044-5
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-017-13044-5
This article is cited by
-
An AuNPs-based electrochemical aptasensor for the detection of 25-hydroxy vitamin D3
Analytical Sciences (2024)
-
Graphene oxide and fluorescent aptamer based novel biosensor for detection of 25-hydroxyvitamin D3
Scientific Reports (2021)
-
Personalized stress monitoring: a smartphone-enabled system for quantification of salivary cortisol
Personal and Ubiquitous Computing (2018)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.