Abstract
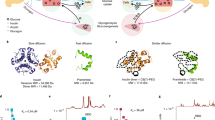
Stimulation of the glucagon-like peptide-1 (GLP1) receptor is a useful treatment strategy for type 2 diabetes due to pleiotropic effects, such as the regulation of islet hormones and the induction of satiety. However, the native ligand for the GLP1 receptor has a short half-life owing to enzymatic inactivation and rapid clearance. Here, we show that a subcutaneous depot formed after a single injection of GLP1 recombinantly fused to a thermosensitive elastin-like polypeptide results in zero-order release kinetics and circulation times of up to 10 days in mice and 17 days in monkeys. The optimized pharmacokinetics lead to 10 days of glycaemic control in three different mouse models of diabetes, as well as the reduction of glycosylated haemoglobin levels and weight gain in ob/ob mice treated once weekly for 8 weeks. Our results suggest that the optimized GLP1 formulation could enhance therapeutic outcomes by eliminating peak-and-valley pharmacokinetics and improving overall safety and tolerability. The design principles that we established should be broadly applicable for improving the pharmacological performance of other peptide and protein therapeutics.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 digital issues and online access to articles
$99.00 per year
only $8.25 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
References
National Diabetes Statistics Report: Estimates of Diabetes and Its Burden in the United States, 2014 (Centers for Disease Control and Prevention, 2014).
Bailey, C. J. The current drug treatment landscape for diabetes and perspectives for the future. Clin. Pharmacol. Therap. 98, 170–184 (2015).
Inzucchi, S. E. et al. Management of hyperglycaemia in type 2 diabetes, 2015: a patient-centred approach. Update to a position statement of the American Diabetes Association and the European Association for the Study of Diabetes. Diabetologia 58, 429–442 (2015).
Bell, G. I., Santerre, R. F. & Mullenbach, G. T. Hamster preproglucagon contains the sequence of glucagon and two related peptides. Nature 302, 716–718 (1983).
Mojsov, S. et al. Preproglucagon gene expression in pancreas and intestine diversifies at the level of post-translational processing. J. Biol. Chem. 261, 11880–11889 (1986).
Mortensen, K., Christensen, L. L., Holst, J. J. & Orskov, C. GLP-1 and GIP are colocalized in a subset of endocrine cells in the small intestine. Reg. Pept. 114, 189–196 (2003).
Flint, A., Raben, A., Astrup, A. & Holst, J. J. Glucagon-like peptide 1 promotes satiety and suppresses energy intake in humans. J. Clin. Invest. 101, 515–520 (1998).
Meeran, K. et al. Repeated intracerebroventricular administration of glucagon-like peptide-1-(7-36) amide or exendin-(9-39) alters body weight in the rat. Endocrinology 140, 244–250 (1999).
Drucker, D. J. Glucagon-like peptide-1 and the islet beta-cell: augmentation of cell proliferation and inhibition of apoptosis. Endocrinology 144, 5145–5148 (2003).
Qualmann, C., Nauck, M. A., Holst, J. J., Orskov, C. & Creutzfeldt, W. Insulinotropic actions of intravenous glucagon-like peptide-1 (GLP-1) [7-36 amide] in the fasting state in healthy subjects. Acta Diabet. 32, 13–16 (1995).
Meloni, A. R., DeYoung, M. B., Lowe, C. & Parkes, D. G. GLP-1 receptor activated insulin secretion from pancreatic beta-cells: mechanism and glucose dependence. Diabet. Obes. Metab. 15, 15–27 (2013).
Rachman, J. et al. Normalization of insulin responses to glucose by overnight infusion of glucagon-like peptide 1 (7-36) amide in patients with NIDDM. Diabetes 45, 1524–1530 (1996).
Rachman, J., Barrow, B. A., Levy, J. C. & Turner, R. C. Near-normalisation of diurnal glucose concentrations by continuous administration of glucagon-like peptide-1 (GLP-1) in subjects with NIDDM. Diabetologia 40, 205–211 (1997).
Quddusi, S., Vahl, T. P., Hanson, K., Prigeon, R. L. & D'Alessio, D. A. Differential effects of acute and extended infusions of glucagon-like peptide-1 on first- and second-phase insulin secretion in diabetic and nondiabetic humans. Diabet. Care 26, 791–798 (2003).
Nauck, M. A. et al. Normalization of fasting hyperglycaemia by exogenous glucagon-like peptide 1 (7-36 amide) in type 2 (non-insulin-dependent) diabetic patients. Diabetologia 36, 741–744 (1993).
Vilsboll, T., Agerso, H., Krarup, T. & Holst, J. J. Similar elimination rates of glucagon-like peptide-1 in obese type 2 diabetic patients and healthy subjects. J. Clin. Endocrinol. Metab. 88, 220–224 (2003).
Deacon, C. F., Johnsen, A. H. & Holst, J. J. Degradation of glucagon-like peptide-1 by human plasma in vitro yields an N-terminally truncated peptide that is a major endogenous metabolite in vivo. J. Clin. Endocrinol. Metab. 80, 952–957 (1995).
Gilroy, C. A., Luginbuhl, K. M. & Chilkoti, A. Controlled release of biologics for the treatment of type 2 diabetes. J. Con. Rel. 240, 151–164 (2015).
Drucker, D. J. & Nauck, M. A. The incretin system: glucagon-like peptide-1 receptor agonists and dipeptidyl peptidase-4 inhibitors in type 2 diabetes. Lancet 368, 1696–1705 (2006).
Jimenez-Solem, E., Rasmussen, M. H., Christensen, M. & Knop, F. K. Dulaglutide, a long-acting GLP-1 analog fused with an Fc antibody fragment for the potential treatment of type 2 diabetes. Curr. Opin. Mol. Therap. 12, 790–797 (2010).
Matthews, J. E. et al. Pharmacodynamics, pharmacokinetics, safety, and tolerability of albiglutide, a long-acting glucagon-like peptide-1 mimetic, in patients with type 2 diabetes. J. Clin. Endocrinol. Metab. 93, 4810–4817 (2008).
Yu, L. et al. In vitro and in vivo evaluation of a once-weekly formulation of an antidiabetic peptide drug Exenatide in an injectable thermogel. J. Pharm. Sci. 102, 4140–4149 (2013).
Chen, Y. P. et al. Injectable and thermosensitive hydrogel containing Liraglutide as a long-acting antidiabetic system. ACS Appl. Mater. Inter. 8, 30703–30713 (2016).
Gedulin, B. R. et al. Dose-response for glycaemic and metabolic changes 28 days after single injection of long-acting release exenatide in diabetic fatty Zucker rats. Diabetologia 48, 1380–1385 (2005).
Kim, D. et al. Effects of once-weekly dosing of a long-acting release formulation of exenatide on glucose control and body weight in subjects with type 2 diabetes. Diab. Care 30, 1487–1493 (2007).
Schwendeman, S. P., Shah, R. B., Bailey, B. A. & Schwendeman, A. S. Injectable controlled release depots for large molecules. J. Con. Rel. 190, 240–253 (2014).
DeYoung, M. B., MacConell, L., Sarin, V., Trautmann, M. & Herbert, P. Encapsulation of exenatide in poly-(d,l-lactide-co-glycolide) microspheres produced an investigational long-acting once-weekly formulation for type 2 diabetes. Diab. Technol. Ther. 13, 1145–1154 (2011).
MacEwan, S. R. & Chilkoti, A. Elastin-like polypeptides: biomedical applications of tunable biopolymers. Biopolymers 94, 60–77 (2010).
Chilkoti, A., Christensen, T. & MacKay, J. A. Stimulus responsive elastin biopolymers: applications in medicine and biotechnology. Curr. Opin. Chem. Biol. 10, 652–657 (2006).
Cho, Y. H. et al. Effects of Hofmeister anions on the phase transition temperature of elastin-like polypeptides. J. Phys. Chem. B 112, 13765–13771 (2008).
Amiram, M., Luginbuhl, K. M., Li, X., Feinglos, M. N. & Chilkoti, A. A depot-forming glucagon-like peptide-1 fusion protein reduces blood glucose for five days with a single injection. J. Con. Rel. 172, 144–151 (2013).
Amiram, M. Glucagon-Like Peptide-1 Depots for the Treatment of Type-2 Diabetes. PhD thesis, Duke Univ. (2012).
Trammell, R. A., Cox, L. & Toth, L. A. Markers for heightened monitoring, imminent death, and euthanasia in aged inbred mice. Compar. Med. 62, 172–178 (2012).
Runge, S. et al. Differential structural properties of GLP-1 and exendin-4 determine their relative affinity for the GLP-1 receptor N-terminal extracellular domain. Biochemistry 46, 5830–5840 (2007).
Baggio, L. L., Huang, Q., Brown, T. J. & Drucker, D. J. A recombinant human glucagon-like peptide (GLP)-1-albumin protein (albugon) mimics peptidergic activation of GLP-1 receptor-dependent pathways coupled with satiety, gastrointestinal motility, and glucose homeostasis. Diabetes 53, 2492–2500 (2004).
Madsbad, S. et al. An overview of once-weekly glucagon-like peptide-1 receptor agonists-available efficacy and safety data and perspectives for the future. Diab. Obes. Metab 13, 394–407 (2011).
Chae, S. Y. et al. Pharmacokinetic and pharmacodynamic evaluation of site-specific PEGylated glucagon-like peptide-1 analogs as flexible postprandial-glucose controllers. J. Pharm. Sci. 98, 1556–1567 (2009).
McDaniel, J. R., Radford, D. C. & Chilkoti, A. A unified model for de novo design of elastin-like polypeptides with tunable inverse transition temperatures. Biomacromolecules 14, 2866–2872 (2013).
Brenner, B. M., Hostetter, T. H. & Humes, H. D. Glomerular permselectivity: barrier function based on discrimination of molecular size and charge. Am. J. Physiol. 234, 455–460 (1978).
Waldmann, T. A., Strober, W. & Mogielnicki, R. P. The renal handling of low molecular weight proteins. II. Disorders of serum protein catabolism in patients with tubular proteinuria, the nephrotic syndrome, or uremia. J. Clin. Invest. 51, 2162–2174 (1972).
Pisal, D. S., Kosloski, M. P. & Balu-Iyer, S. V. Delivery of therapeutic proteins. J. Pharm. Sci. 99, 2557–2575 (2010).
Caliceti, P. & Veronese, F. M. Pharmacokinetic and biodistribution properties of poly(ethylene glycol)-protein conjugates. Adv. Drug Deliv. Rev. 55, 1261–1277 (2003).
Yamaoka, T., Tabata, Y. & Ikada, Y. Distribution and tissue uptake of poly(ethylene glycol) with different molecular weights after intravenous administration to mice. J. Pharm. Sci. 83, 601–606 (1994).
Armstrong, J. K., Wenby, R. B., Meiselman, H. J. & Fisher, T. C. The hydrodynamic radii of macromolecules and their effect on red blood cell aggregation. Biophys. J. 87, 4259–4270 (2004).
Purtell, J. N., Pesce, A. J., Clyne, D. H., Miller, W. C. & Pollak, V. E. Isoelectric point of albumin: effect on renal handling of albumin. Kidney Int. 16, 366–376 (1979).
Dubuc, P. U., Scott, B. K. & Peterson, C. M. Sex-differences in glycated hemoglobin in diabetic and nondiabetic C57bl/6 mice. Diab. Res. Clin. Pr. 21, 95–101 (1993).
Vanputten, L. M. The life span of red cells in the rat and the mouse as determined by labeling with Dfp32 in vivo. Blood 13, 789–794 (1958).
Shemin, D. & Rittenberg, D. The life span of the human red blood cell. J. Biol. Chem. 166, 627–636 (1946).
Mahmood, I. Application of allometric principles for the prediction of pharmacokinetics in human and veterinary drug development. Adv. Drug Deliv. Rev. 59, 1177–1192 (2007).
Lapin, B. A., Gvozdik, T. E. & Klots, I. N. Blood glucose levels in rhesus monkeys (Macaca mulatta) and cynomolgus macaques (Macaca fascicularis) under moderate stress and after recovery. Bull. Exp. Biol. Med. 154, 497–500 (2013).
Ponce, R. et al. Immunogenicity of biologically-derived therapeutics: assessment and interpretation of nonclinical safety studies. Regul. Toxicol. Pharm. 54, 164–182 (2009).
Glaesner, W. et al. Engineering and characterization of the long-acting glucagon-like peptide-1 analogue LY2189265, an Fc fusion protein. Diab. Metab. Res. Rev. 26, 287–296 (2010).
Williams, D. L., Baskin, D. G. & Schwartz, M. W. Leptin regulation of the anorexic response to glucagon-like peptide-1 receptor stimulation. Diabetes 55, 3387–3393 (2006).
Enriori, P. J. et al. Diet-induced obesity causes severe but reversible leptin resistance in arcuate melanocortin neurons. Cell Metab. 5, 181–194 (2007).
Glaesner, W. et al. Engineering and characterization of the long-acting glucagon-like peptide-1 analogue LY2189265, an Fc fusion protein. Diab. Metab. Res. 26, 287–296 (2010).
Young, M. A. et al. Clinical pharmacology of albiglutide, a GLP-1 receptor agonist. Postgrad. Med. 126, 84–97 (2014).
Painter, N. A., Morello, C. M., Singh, R. F. & McBane, S. E. An evidence-based and practical approach to using Bydureon in patients with type 2 diabetes. J. Am. Board Fam. Med. 26, 203–210 (2013).
Wang, J., Wang, B. M. & Schwendeman, S. P. Characterization of the initial burst release of a model peptide from poly(D,L-lactide-co-glycolide) microspheres. J. Control. Rel. 82, 289–307 (2002).
Zou, P. et al. Applications of human pharmacokinetic prediction in first-in-human dose estimation. AAPS J. 14, 262–281 (2012).
McDaniel, J. R., MacKay, J. A., Quiroz, F. G. & Chilkoti, A. Recursive directional ligation by plasmid reconstruction allows rapid and seamless cloning of oligomeric genes. Biomacromolecules 11, 944–952 (2010).
Burcelin, R., Dolci, W. & Thorens, B. Long-lasting antidiabetic effect of a dipeptidyl peptidase IV-resistant analog of glucagon-like peptide-1. Metab. Clin. Exp. 48, 252–258 (1999).
de Meester, I., Lambeir, A. M., Proost, P. & Scharpe, S. Dipeptidyl peptidase IV substrates. An update on in vitro peptide hydrolysis by human DPPIV. Adv. Exp. Med. Biol. 524, 3–17 (2003).
Holst, J. J. The physiology of glucagon-like peptide 1. Physiol. Rev. 87, 1409–1439 (2007).
Miranda, L. P. et al. Design and synthesis of conformationally constrained glucagon-like peptide-1 derivatives with increased plasma stability and prolonged in vivo activity. J. Med. Chem. 51, 2758–2765 (2008).
Amiram, M., Luginbuhl, K. M., Li, X., Feinglos, M. N. & Chilkoti, A. Injectable protease-operated depots of glucagon-like peptide-1 provide extended and tunable glucose control. Proc. Natl Acad. Sci. USA 110, 2792–2797 (2013).
Meyer, D. E. & Chilkoti, A. Purification of recombinant proteins by fusion with thermally-responsive polypeptides. Nat. Biotechnol. 17, 1112–1115 (1999).
Chizzonite, R. et al. IL-12: monoclonal antibodies specific for the 40-kDa subunit block receptor binding and biologic activity on activated human lymphoblasts. J. Immunol. 147, 1548–1556 (1991).
Goke, R. & Conlon, J. M. Receptors for glucagon-like peptide-1(7-36) amide on rat insulinoma-derived cells. J. Endocrinol. 116, 357–362 (1988).
Chan, H. M., Jain, R., Ahren, B., Pacini, G. & D'Argenio, D. Z. Effects of increasing doses of glucagon-like peptide-1 on insulin-releasing phases during intravenous glucose administration in mice. Am. J. Physiol. Regul. Integr. Comp. Physiol. 300, 1126–1133 (2011).
Ahren, B., Holst, J. J., Martensson, H. & Balkan, B . Improved glucose tolerance and insulin secretion by inhibition of dipeptidyl peptidase IV in mice. Eur. J. Pharmacol. 404, 239–245 (2000).
Luginbuhl, K. M. et al. Dataset for: One-week glucose control via zero-order release kinetics from an injectable depot of glucagon-like peptide-1 fused to a thermosensitive biopolymer. figsharehttp://dx.doi.org/10.6084/m9.figshare.4903931 (2017).
Acknowledgements
A.C. acknowledges the support of NIH through grant R01-DK091789. K.M.L. acknowledges the support of the NSF through a Graduate Research Fellowship. We thank D. Drucker for providing BHK cells for assaying in vitro activity, G. A. Johnson and Duke’s Center for In Vivo Microscopy for use of their U-SPECT-II/CT imaging equipment, and M. R. Zalutsky for allowing us to use his laboratory and equipment to conduct radiolabelling experiments. K.L. thanks C. Gilroy for productive discussions on in vitro and in vivo experiments. The authors all sincerely thank K. Gerken, who provided pathology expertise and helped to analyse and interpret injection site histology, as well as the Duke Research Immunohistology Shared Resource Lab who processed the skin samples. Finally, we would like to thank J. Jowett, D. Sendecki and C. Woods of PhaseBio Pharmaceuticals, who helped to express and purify fusion protein for the non-human primate experiment.
Author information
Authors and Affiliations
Contributions
K.M.L. and A.C. conceived and designed the research. K.M.L., J.L.S., X.L. and B.U. performed the experiments. S.B. provided materials for the imaging study. S.A. helped to plan and organize the non-human primate study. M.F. and D.D. provided expertise in endocrinology for the design of in vivo studies. E.M.M. assisted in statistical analysis and interpretation of in vivo results. K.M.L. and A.C. analysed the results and wrote the manuscript. J.L.S., E.M.M. and D.D. edited the manuscript.
Corresponding author
Ethics declarations
Competing interests
A.C. is a scientific advisor and is on the board of directors for PhaseBio Pharmaceuticals, which has licensed the ELP technology for drug delivery applications from Duke University.
Supplementary information
Supplementary Information
Supplementary methods, figures and tables (PDF 4067 kb)
Rights and permissions
About this article
Cite this article
Luginbuhl, K., Schaal, J., Umstead, B. et al. One-week glucose control via zero-order release kinetics from an injectable depot of glucagon-like peptide-1 fused to a thermosensitive biopolymer. Nat Biomed Eng 1, 0078 (2017). https://doi.org/10.1038/s41551-017-0078
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41551-017-0078
This article is cited by
-
The construction of elastin-like polypeptides and their applications in drug delivery system and tissue repair
Journal of Nanobiotechnology (2023)
-
Peptide-based liquid droplets as emerging delivery vehicles
Nature Reviews Materials (2023)
-
Fluid protein condensates for bio-inspired applications
Nature Reviews Bioengineering (2023)
-
Redox-responsive peptide-based complex coacervates as delivery vehicles with controlled release of proteinous drugs
Communications Chemistry (2023)
-
Designing and computational analyzing of chimeric long-lasting GLP-1 receptor agonists for type 2 diabetes
Scientific Reports (2023)