Abstract
Most governments have enacted physical or social distancing measures to control COVID-19 transmission. Yet little is known about the socio-economic trade-offs of these measures, especially for vulnerable populations, who are exposed to increased risks and are susceptible to adverse health outcomes. To examine the impacts of physical distancing measures on the most vulnerable in society, this scoping review screened 39,816 records and synthesised results from 265 studies worldwide documenting the negative impacts of physical distancing on older people, children/students, low-income populations, migrant workers, people in prison, people with disabilities, sex workers, victims of domestic violence, refugees, ethnic minorities, and people from sexual and gender minorities. We show that prolonged loneliness, mental distress, unemployment, income loss, food insecurity, widened inequality and disruption of access to social support and health services were unintended consequences of physical distancing that impacted these vulnerable groups and highlight that physical distancing measures exacerbated the vulnerabilities of different vulnerable populations.
Similar content being viewed by others
Introduction
The global COVID-19 pandemic had led to around 586.5 million cases and 6.4 million fatalities cumulatively by 10 August 2022, with the United States (US), Brazil, India, Russia, Mexico, Peru and the United Kingdoms (UK) being some of the countries that have been hardest hit in terms of the death toll1.
With the number of COVID-19 cases and fatalities worldwide still growing, governments have deployed various policy instruments to bring the pandemic under control and to reduce its impact on socio-economic systems. One widely implemented tool in governments’ arsenals that has been used to curb the spread of COVID-19 is the deployment of “physical distancing” (often used interchangeably with the term “social distancing”) measures. According to the World Health Organization (WHO), social distancing aims to maintain safe physical distancing through decreased crowding2. Social distancing (hereafter physical distancing) measures range from lockdowns and school closures to restrictions on social gatherings in homes and public places (Supplementary Text A1).
While policy measures to combat COVID-19 are implemented by governments with the deliberate intention of breaking the virus’s transmission chain and bringing the pandemic under control, there are costs involved, including in relation to unintended consequences. The nature of some of these measures, such as nationwide lockdowns, can be draconian and are likely to have some negative repercussions, especially for vulnerable populations.
Researchers have published several systematic reviews of the effectiveness and impacts of physical distancing measures3,4,5. However, a systematic effort to consolidate knowledge on how certain physical distancing measures targeting general populations affect vulnerable groups is lacking. In addition, there is insufficient understanding of how certain targeted physical distancing measures that are intended to ringfence vulnerable populations are designed and implemented in different countries, and how these measures have negatively impacted them. Essentially, ringfencing means protecting something by putting limits on it so that it can only be used for a particular purpose or by a particular group. In the context of this study ringfencing measures resemble “sectoral lockdown so that all the people within a sector or a location can minimise further interactions with the public”6. For instance, restricting external visitors to nursing homes and prisons during COVID-19 are some commonly deployed ringfencing measures during the pandemic. Essentially, ringfencing is a form of physical distancing strategy, which aims to limit COVID-19 transmission and contain their spread.
We conducted a scoping review to address the above knowledge gaps, to examine the negative impacts of physical distancing measures on vulnerable populations and identify ringfencing measures designed to counter these impacts.
Results
Study contexts and characteristics
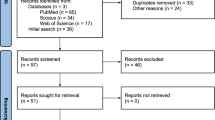
Figure 1 summarises the data selection and screening process, according to the PRISMA guidelines7,8,9. Of the total 39,816 records that were produced by searches, we identified 265 eligible studies for synthesis of their results in this review. The list of included studies is available in Supplementary Tables 1, 2, the detailed distribution of studies across countries and vulnerable groups is in Supplementary Tables 3, 4, and additional details of the findings can be found in Supplementary Text A4. Our data cover 49 countries spread across five continents (Fig. 2).
a Global map. b Data distribution around Europe. c Data distribution around Asia. Data listed in Supplementary Tables 5–7. QGIS version 3.16.12 was used to generate the map (Open Source Geographic Information System, http://www.qgis.org). Global map was downloaded from the OpenStreetMap © OpenStreetMap contributors. Available under the Open Database Licence from: openstreetmap.org.
The majority of studies in our dataset focus on children/students and low-income populations (96 studies and 58 studies, respectively). This is followed by studies on the older people (n = 37), victims of domestic violence (n = 16), people with disabilities (n = 15), migrant workers (n = 14), refugees (n = 14), the people from sexual and gender minorities (n = 11), ethnic minorities (n = 10), sex workers (n = 9), and people in prison (n = 7). There are five studies on vulnerable groups in general. The classification we apply is not exclusive, and vulnerabilities can be intertwined, such as children with disabilities or children who are vulnerable to domestic violence.
Older people: vulnerability and physical distancing
Older people, especially those with chronic diseases, exhibit health vulnerability, including having a high risk of developing severe COVID-19 symptoms if they contract the disease. They are also vulnerable to developing mental health problems, such as anxiety and depression, when isolated at home10,11,12,13,14,15. Some older people are also prone to economic vulnerability, which may exacerbate their health vulnerability due to the resulting decreased access to essential living needs or medical services16.
In most countries, physical distancing measures have been neutrally applied to all populations, even though they may have negative impacts on the older people. The review included 37 studies on older people. In these studies, physical distancing measures are found to be effective in mitigating COVID-19 infection and deaths among the older people17,18. However, at the same time they are found to further predispose older people to greater risks of cardiovascular, autoimmune and neurocognitive diseases14,19.
The literature also analyses alternatives policy measures to lockdowns, which are more cost-effective. As an example, distributing hygiene kits is considered effective in preventing the spread of COVID-19 while mitigating unintended policy consequences, especially in low- and middle-income countries20. To mitigate the risk of COVID-19 outbreaks within nursing homes and long-term care (LTC) facilities, early screening, detection and contact tracing are found to be effective21. The distribution of tools for detection and remote monitoring of cases is also found to facilitate COVID-19 control in LTC facilities22,23.
To address mental health issues faced by older people when socially isolated, the use of technology is considered useful22,23,24,25. Information and communication technologies are found to help the older people maintain social connections with their loved ones, including attending virtual recreational activities (e.g., playing games) to mitigate loneliness and maintain their wellbeing when they are isolated at home or in LTC facilities24.
Children/students: vulnerability and physical distancing
Children are subject to cognitive and communicative vulnerability because of their young age. They are dependent persons (subject to economic vulnerability), relying on their parents/guardians to meet their living needs and receive financial support26,27. Poor economic conditions, such as lack of access to schooling, health and social services, and inadequate clothing, contribute to children’s vulnerability27.
Among the 96 studies on children/students, most studies discuss school closing and remote learning. Unintended detrimental impacts of school closures that are identified in the studies include negative impacts on educational outcomes (differing across learning courses) and on children’s physical health (e.g., weight gain)28,29. School closures are found to cause widespread concerns about children’s suboptimal learning at home30. Remote learning is found to exert pressure on teachers’ technical capacities to operate digital teaching, and often increases their working hours31,32.
Across the world, the implementation of remote learning has sparked concerns about the widening of learning gaps between students from different socio-economic classes. Virtual learning environments cause inevitable disruptions. Children from low-income families are affected more significantly by disruptions in learning and being deprived of the services and support that they receive in schools33,34,35,36,37. They are likely to lack access to the internet and other digital resources, such as computers, and face issues such as a lack of regular meals and parental support, a home environment that is not conducive for learning, and a high risk of exposure to COVID-19 in crowded housing conditions33,34,36,38,39.
There have been debates on the extent to which school closures are effective in breaking the virus’s transmission, and the necessity of reopening schools to facilitate effective learning40,41,42,43,44,45,46,47,48. As indicated by the literature, decisions on school closures or reopening should consider the severity of COVID-19 infections in the community and the ability of schools to enforce physical distancing, as well as to detect and trace suspected cases on campus/in school facilities43,45. It has been shown that in many countries school reopening did not necessarily result in increases in COVID-19 transmission if health and safety protocols were adhered to. These protocols include the following: teaching children hygiene measures (e.g., washing hands), mandating mask-wearing, ensuring one- to two-metre distancing, screening at entry, grouping students and reducing class sizes, limiting after-school activities, moving to outdoor classrooms, testing and tracing suspected cases, quarantining confirmed cases, suggesting that parents do not congregate outside the campus gates, staggering drop-off and pick-up times, enhancing air circulation, shortening school hours, offering options for in-person, remote or hybrid learning, and disinfecting facilities47,49,50,51,52,53,54,55,56,57,58,59,60,61,62,63,64,65,66.
To address children’s mental health issues, studies67,68 suggested that parents communicate constructively with their children about the current COVID-19 pandemic situation, in accordance with their maturity level and ability to understand the crisis, and in some parts of the world scholars have advocated for schools and families to assess and identify children’s mental health needs and issues69,70.
To enhance remote learning, especially to support vulnerable students from low-income families, solutions that have been applied have ranged from circulating printed materials to be used in learning from home32, putting out television broadcasts related to courses or other media71, identifying children’s needs and offering target instructions72,73,74, and offering support such as helping people obtain laptops, providing helplines, providing free-of-charge data SIM cards and implementing food programmes75,76. Many governments have also established funds or fiscal stimulus packages to meet children’s educational needs during the COVID-19 pandemic35,73,74.
Low-income populations: vulnerability and physical distancing
As the term suggests, low-income populations face adverse financial conditions. They may also face less favourable employment conditions, such as temporary contracts, part-time employment, self-employment and employment in the low-income informal sector. Low-income levels also correlate with poor health77,78, poor housing conditions and even homelessness78. As low-income populations typically have few savings, the loss of their job or income can further worsen their financial situation, causing other health risks, such as food insecurity79.
Fifty-eight studies across 19 countries find similar results regarding the challenges faced by low-income populations in adhering strictly to various physical distancing measures. These include congregated living spaces, a dearth of sanitation facilities, an inability to work from home (e.g., if they work in the manufacturing and processing industries), a lack of access to job protection or paid leave, food shortages and food insecurity, worsened financial conditions and being forced to live off savings, a lack of regular access to basic hygiene, and a lack of resources and infrastructure for testing, isolation and contract tracing10,38,78,79,80,81,82,83,84,85,86,87,88,89,90,91,92,93,94,95,96,97,98,99,100,101. Lockdowns are reported to be less effective in containing and reducing new COVID-19 cases in low-income countries and communities97,102,103,104.
In addition, the social vulnerability of low-income populations intersects with economic vulnerability, and contributes to health vulnerability. For instance, in slums and informal settlements, residents are exposed to poor living conditions, a dearth of sanitation facilities and a lack of clean drinking water; moreover, the high population density in slums renders one- or two-metre distancing impractical10,38,86,96,104,105,106. These factors have negative repercussions for governments in terms of tracing, testing and treating COVID-19 infections. Those with low incomes also face barriers to accessing healthcare due to income loss and reduced employer-sponsored healthcare83,101, while their access to government aid or relief packages is limited84,104,107,108. The literature also records the mental distress suffered by low-income populations during the COVID-19 pandemic38,108,109,110.
According to the literature, to control the spread of COVID-19 among low-income communities, physical distancing measures should be context-specific90. Intensive screening, testing, and contract tracing, and the isolation of infected cases, are found to be useful to keep cases low80,111,112. Other measures, such as offering affordable masks, the availability of clean water, sanitiser and soaps, and easing crowding in low-income communities, are also necessary80,105,112.
Greater economic support has been called for to assist low-income populations35,87,93,96,99,113,114. It is argued that access to unemployment insurance, paid medical leave and reemployment services should also be strengthened for those on low incomes79,87,115.
More effective channels for communication between low-income populations and governments can be established87. Community-led efforts by non-governmental organisations are found to have been instrumental in aiding low-income populations during the pandemic. Their efforts include offering food, distributing COVID-19 information and education through social media or SMS, facilitating contract tracing and quarantine, delivering groceries and other essential items to patients in quarantine, and establishing longitudinal clinical and social support for them through the involvement of community health workers and public health specialists106,116,117,118.
Migrant workers: vulnerability and physical distancing
A migrant worker is defined as “a person who is to be engaged, is engaged or has been engaged in a remunerated activity in a state of which he or she is not a national”119. Migrant workers move away from their usual place of residence across an international border to a different country, or to a different place within the same country120. Migrant workers are exposed to economic vulnerability due to experiencing adverse employment conditions, such as precarious recruitment processes, an absence of accurate information on the terms and conditions of employment contracts, and a lack of labour law coverage in the destination state/location121. They may also face mental health vulnerability122, such as suffering from emotional distress due to social and cultural isolation, hardening migration policies and even the loss of accommodation in the destination state/location123,124,125,126.
Owing to lockdowns/stay-at-home orders implemented to control COVID-19, migrant workers (inter-state or inter-country) have faced a variety of challenges, including job losses and income loss127, food insecurity127,128, a high risk of exposure to the virus in crowded dormitories129,130, and limited access to primary healthcare and COVID-19 treatment107,130. A study in the UK reported that the pandemic has led to a deterioration in the housing stability of the migrant worker population, making them even more socially and economically isolated, which has created ripple impacts, such as preventing them from accessing remote healthcare services126. Migrant workers tend not to qualify for many COVID-19-related social benefits (e.g., food rations) provided by the destination country and are likely to be repatriated to their home countries131. Migrant workers also suffer significant mental stress and loneliness due to financial instability, the isolation of migrant worker dormitories, language and cultural barriers, an inability to send remittances to families, and barriers to returning home to see their family members92,122,129,130. These predicaments have resulted in some migrant workers adopting different survival strategies, such as reducing their expenses, consuming less food, and selling their jewellery, land and other possessions123.
A notable example of the drastic measures that have been taken to address COVID-19 transmission among migrant workers is Singapore. The initial COVID-19 outbreaks in migrant workers’ dormitories in the country put Singapore in the global limelight and the government and non-profit organisations responded swiftly by enhancing migrant workers’ access to medical support and public health information129,132. The government also employed extensive testing, established quarantine facilities, offered financial support for employers to pay migrant workers’ salaries, supported communication via facilitating internet connectivity and prepaid phone cards, and provided timely and free-of-charge medical care for infected migrant workers129. In addition to governmental efforts, online information about COVID-19 in native languages that were accessible to migrant workers, as well as hotline- and web-based counselling services, were provided by a local non-profit organisation for migrant workers132.
People in prison: vulnerability and physical distancing
The primary vulnerability faced by people in prison is institutional or deferential vulnerability, as they are deprived of their liberty. In addition, they are socially isolated and live in overcrowded spaces, which can lead to social vulnerability. Vulnerability to mental health issues133 and violence134 are also typical among inmates. The spatial density in prisons has been associated with outbreaks of infectious and communicable diseases135,136.
Enforcing social isolation or distancing in prisons has been shown to exacerbate inmates’ mental health issues and even suicide rates137. Poor communication about the COVID-19 pandemic from prison staff contributes to increased stress and anxiety among people in prison138. Prison escapes and riots have been reported in Brazil, Italy, Sudan and Nigeria due to increased social isolation measures imposed on people in prison, such as restrictions on receiving visitors80,137.
Some countries, such as Sweden139 and the UK138, have allowed virtual or video visits from families to mitigate the mental distress experienced by people in prison. For instance, in Sweden, the Swedish Prison and Probation Service (SPPS) has provided inmates with tablets to enable phone calls or video calls with their children or their other family members and friends139. Many prison units have also organised weekly information meetings to update inmates about the COVID-19 situation and the policy measures taken to preserve their safety in prisons139. These measures have been found to be helpful in mitigating inmates’ fear of contracting the virus and preserving their mental health.
To reduce population density and reduce the spread of COVID-19 in prisons, some governments have released a number of people from prisons, primarily to home confinement or community supervision, such as in the US, Portugal, Iran, Ireland, Morocco, Libya, Burkina Faso, Uganda and Nigeria80,137,140,141. Certain groups of people in prison have been considered for rapid release137, such as those who are approaching their actual release date, those eligible for medical release, those approved for community supervision, those held on minor charges, and those held pretrial on bail.
People with disabilities: vulnerability and physical distancing
A disability is defined as any physical or mental condition (impairment) that results in a limitation on a person’s activity (difficulty in undertaking certain activities, e.g., difficulty seeing, hearing, walking, or problem-solving) or a restriction on their participation (difficulty participating in normal daily activities, e.g., working, social activities, or accessing healthcare and preventive services)142. People with disabilities typically face health vulnerabilities. Economic vulnerability is also a prominent vulnerability reported among the people with disabilities as they often have less access to educational and employment opportunities, and are more likely to live in poverty or on a low income143,144.
When physical distancing measures are enforced, particularly during lockdowns, people with disabilities face challenges such as reduced social connections and reduced access to healthcare services145. For instance, in-person supportive services, such as community-based rehabilitation, may be disrupted146, and people with mental disabilities (e.g., children with autism) may face worse mental health outcomes due to increased social isolation and suspension of therapy68,147. The enforcement of physical distancing measures also inadvertently reduces access to medication, healthcare services and transportation for adults with mobility disabilities148. In addition, their reduced mobility and social connections limits their access to social welfare services, such as food rations109.
In this review, one of the populations with disabilities found to be worst affected is children with disabilities. When schools close during the pandemic, the lack of necessary technologies (e.g., braille readers) and services (e.g., help and support from special education teachers) at home may lead to their experiencing difficulties in participating in remote learning39. Studies from Egypt and India have reported that remote learning poses challenges to the caregivers of children who are intellectually challenged, as these children’s attention span, impulsivity, mood swings and hyperactivity worsen post-lockdown, thus reducing their performance149,150,151,152. By and large, it is found to be challenging to provide remote learning to students with disabilities because the services and the number of specialised instruction hours may differ for each student153.
The studies included in the review discuss solutions to help children with disabilities during the COVID-19 pandemic, such as allowing them to borrow learning devices from their school39, offering financial support to meet their educational needs154 and encouraging parents to help their children to understand the COVID-19 pandemic68.
Sex workers: vulnerability and physical distancing
By the nature of their occupation, sex workers face health vulnerability, due to their susceptibility to sexually transmitted infections, and social vulnerability, such as increased risk of being subjected to violence155. Some also face economic vulnerability due to adverse financial conditions156.
In the context of the COVID-19 pandemic, sex workers living with HIV are reported to have experienced a lack of access to testing and treatment for sexually transmitted infections during lockdown periods157,158,159. In addition, they also have limited access to COVID-19 social services and safety nets offered by governments160. A study in Singapore also revealed that sex workers have experienced greater economic hardship during the pandemic as a result of a reduction in the demand for sex workers. This phenomenon has also caused the out-migration of sex workers and a shift of sex work towards online spaces161.
To meet the basic needs of sex workers during the COVID-19 pandemic, community-based organisations have stepped up efforts to provide food, financial aid, COVID-19 safety guidance, and community-driven health interventions, including anti-retroviral therapy (ART)157,162. In India, considering that ART was disrupted, the organisation Ashodaya Samithi formed a community-led system to distribute ART at private and discreet sites and utilised WhatsApp messaging to share information related to the pandemic158. In Thailand, to secure the basic hygiene and personal protection needs of sex workers, community-led organisations, including the Raks Thai Foundation, Dannok Health and Development Community Volunteers, and SWING, provided food, hand sanitisers, condoms and face masks to the sex worker population157. In Africa, community-led outreach has distributed food packs to sex workers during the pandemic163.
Victims of domestic violence: vulnerability and physical distancing
When isolated at home, victims of domestic violence are more socially isolated and have reduced access to institutional support164. In many cases, having a disability can exacerbate a person’s vulnerability to domestic violence165,166.
Victims of domestic violence may face difficulties in leaving home to access institutional support during lockdowns. In Spain, the Democratic Republic of Congo, South Africa, Guatemala, India, and Bangladesh, lockdown periods saw increased incidence of, and police reports of, domestic violence against women167,168,169,170,171,172. Studies surmise that the official figures for such violence are under-reported as many formal and informal communication channels to access help for the victims, including transport to access shelters in some countries, either shut down or slowed down their operations during the pandemic, fostering change in help-seeking behaviour among abused women167,169,173. School closures that force children to be homebound also put them at a higher risk of violence174. A study in a city in Wales, in the UK, reported a significant increase in child protection medical examinations through self-referrals and third-party referrals in 2020 as compared to 2019175.
Remote counselling services through virtual platforms can be helpful for victims of domestic violence10. In the UK, due to alarming trends in domestic violence during the pandemic, several national campaigns were organised to raise awareness of domestic abuse and to highlight available help services176. Helpline services were extended for victims of domestic violence in the UK, and the government provided funds to support these helplines and other online support services from April 2020176. Victims of domestic violence have sometimes been allowed to bypass lockdown restrictions to travel to sheltered accommodation to seek refuge176. Schools and universities have also extended accommodation to students who are vulnerable to domestic violence and have ensured student counselling and support services are provided to support them176. In France and Italy, governments also commissioned hotels as shelters for victims of domestic violence164.
Refugees: vulnerability and physical distancing
The vulnerabilities faced by refugees, as identified in the literature, include economic vulnerability177, social vulnerability (e.g., social isolation, living in crowded informal refugee camps, a lack of water and sanitation facilities, and vulnerability to violent attacks)178,179, and health vulnerability, particularly mental health problems180.
During the pandemic, precarious and overcrowding housing conditions have made it difficult for refugees to maintain physical distancing or self-isolation at home when required181. Owing to the shutting of government services and decreased numbers of volunteers working in refugee camps during the pandemic, refugees have experienced limited access to food, basic sanitation and medical care181,182,183. This situation exacerbates the mental health issues of refugees, who may already be living with post-traumatic stress disorders or other mental illnesses. For some refugees, owing to the sensitive nature of their trauma histories, their forced isolation may bring to the surface traumatic memories of the past181,182,183.
Solutions, such as encouraging mask-wearing, limiting mobility, sectoring and setting up quarantine areas, as well as quickly detecting and isolating suspected or confirmed cases, have been implemented to limit the spread of COVID-19 in refugee camps80,184,185,186. Mental health services have been provided for refugees through phone or video conferencing emotional therapies, as well as through other voluntary mental health services in a targeted attempt to reach out to refugee families182,187,188. The active deployment of social workers to areas where asylum-seekers reside has also helped to address the social and psychological vulnerabilities they face during the pandemic189.
Ethnic minorities: vulnerability and physical distancing
Ethnic minority groups typically face social vulnerability as they are socially isolated/marginalised. They tend to have less access to education and health services than the ethnic majority190. Ethnic minorities also face economic vulnerability. In any given country, members of an ethnic minority are more likely to live in poverty than the ethnic majority, on average, and are less likely to work in high- or semi-skilled jobs190.
Lockdowns may be particularly challenging for ethnic minority groups as they are less able to work from home or to self-isolate at home100. People from an ethnic minority background are more likely to work in adverse employment conditions and to face greater financial concerns than the ethnic majority93,113. Physical distancing measures are also found to substantially impact the mental health of ethnic minorities191. Language barriers experienced by ethnic minorities are also highlighted as an issue. These barriers can hamper their understanding of the pandemic and can hamper government efforts to enforce physical distancing measures192.
People from sexual and gender minorities: vulnerability and physical distancing
The people from sexual and gender minorities are socially isolated193 or vulnerable to violence;194 they also have health vulnerabilities, particularly vulnerability to HIV risks193,194 and mental health illnesses195. The marginalised social identities of sexual and gender minorities reinforce and intersect with their health vulnerability. This review finds that physical distancing measures to control COVID-19 may exacerbate the social and health vulnerabilities of the people from sexual and gender minorities195,196,197,198. Most importantly, enforcing physical distancing may limit their access to essential medical services, including HIV testing and treatment196,197. For those who are vulnerable to mental illnesses related to discrimination and lack of family acceptance, the enforcement of physical distancing measures directly cuts off their access to supportive friends and partners, reduces their sense of social connectedness and aggravates feelings of loneliness198. For instance, a study in Brazil revealed that transgender populations reported substantial mental health problems and challenges in accessing healthcare during the pandemic199. The stigma and social exclusion of the transgender population were exacerbated during the pandemic, especially those who were older, as their social and health needs were not properly addressed due to the small and dispersed nature of this population200.
Summary of results
Table 1 summarises the findings and specific examples mentioned in the literature (Supplementary Text A4.12).
Discussion
While there is a robust scientific basis for enforcing physical distancing measures to slow the transmission of COVID-19, little is known about the ethical implications and socio-economic trade-offs associated with such measures. Physical distancing measures may disproportionately and negatively impact the most vulnerable groups in society through job losses, reduction in incomes, a deterioration in mental health and a widened socio-economic gap between the richest and the poorest201,202,203.
The review has revealed the negative impacts that physical distancing measures can have on different vulnerable populations (Table 1). The enforcement of physical distancing affects the utilisation of and access to essential health services among the older people, people with disabilities and people from sexual and gender minorities. Mental distress caused by social isolation is found to be common among different vulnerable populations. Effective communication mechanisms should therefore be established to make public information regarding the COVID-19 pandemic and related policy measures accessible to socially isolated population groups, such as people in prison and ethnic minorities. For children/students, school closures lead to concerns about disruption to their learning and decreased social interactions with peers, especially for children from low-income families. For low-income populations and migrant workers, job losses and financial challenges are the most common challenges faced during lockdowns. Lockdowns or stay-at-home orders also hamper access to social support among refugees and people who are at high risk of domestic violence.
Various ringfenced measures have been taken by governments to address the diverse challenges faced by vulnerable populations and these have been discussed by scholars; they range from the use of technologies to telehealth services and financial support. To date, there has been limited evidence on the impacts of these measures. Evaluating these policy measures represents an important future research direction and is critical to inform policymakers, so that they can adopt an optimal set of ringfenced policy measures to enhance social inclusion for vulnerable populations.
Among the countries that have implemented physical distancing measures, few have ringfenced measures for vulnerable groups (e.g., income support for the low-income populations), which suffer from the unintended consequences of physical distancing204. Effective control of the COVID-19 pandemic requires packaging policy measures strategically to address multiple competing objectives and to balance the various conflicts and tensions that exist between controlling the virus’s transmission to save lives, supporting the economy and ensuring that the wellbeing of vulnerable groups is accounted for in policy processes. Physical distancing measures should be complemented by ringfenced measures to reduce the negative impacts of physical distancing measures on vulnerable groups and to enhance the overall policy effectiveness. More research is required to weigh the trade-offs between the benefits and unintended negative consequences of physical distancing measures, to improve their design and to minimise long-term socio-economic disparities.
Among studies of the experience of vulnerable groups during the COVID-19 pandemic, most studies focus on low-income populations, the older people and children/students, while other vulnerable groups receive much less attention. Each group may experience multiple forms of vulnerability that are mutually reinforcing. Here we identify their primary and secondary vulnerabilities (Table 2).
To safeguard vulnerable populations and meet their financial, health, education, food and housing needs during the COVID-19 pandemic, the following strategies have gained traction in the literature, that while speculative at this stage, merit policy considerations: (a) Leveraging technological prowess of autonomous systems and digital technologies through use of technologies such as social companion robots, to address social isolations faced by the older residents in care homes22,23,24,25 and ICT to deliver health services, such as online counselling services by mental health professionals10,22,23,24,25,132, (b) Ensuring continuity of essential health services129,132,157,162 and strengthening health service delivery capacity and use of telemedicine or home care services, to ensure treatment continuity for patients205,206,207, (c) Providing financial support for low-income populations in the forms of direct cash assistance, in-kind assistance, low-interest loans, tax reduction or rebates, and temporary relief funds or concessions for small businesses, and flexible payment options for utilities and other essential public services35,87,93,96,99,113,114, as well as rolling-out various unemployment benefits such as handouts or improving employability via upskilling and retraining79,87,115, (d) Establishing effective public communication for vulnerable populations who are socially isolated132,139,158,192 and a comprehensive support package for them to ensure reliable access to necessities, such as food, housing/shelter, electricity, water and sanitation85,93,104,106,157,162,208, (e) Enhancing the capacity of the education sector to deliver online or home-based learning31,32,33,34,35,36,37,75,76 and outreach services to support special needs students with learning difficulties153, and (f) Strengthening public finance to facilitate implementation of physical distancing measures35,39,73,74,176 and to weather the economic recession impacts caused by future pandemics35,73,74.
This scoping review has two potential limitations. First, we may have missed out a small subset of studies during the systematic evidence search process due to the various ways vulnerabilities and vulnerable populations are defined and conceptualised. Second, we did not attempt to tease out the jurisdictional differences pertaining to the negative impacts experienced by the 11 vulnerable populations examined in this review. This presents an opportunity for future research.
Broader impact
This scoping review represents a comprehensive effort to consolidate empirical insights regarding the impacts of COVID-19 physical distancing measures on the most vulnerable in society, and to identify strategies and actions that have been taken to address their vulnerabilities. Review studies have been conducted on physical distancing measures and their effectiveness3,4,5, but few reviews have focused specifically on vulnerable populations. By examining the extent to which universally applied physical distancing measures have negatively impacted the vulnerable populations, this scoping review fills a pertinent research gap and has significant policy implications for equity and human rights.
Our findings emphasise the need for policymakers and practitioners to pay more attention to addressing the needs and improving the welfare of the vulnerable populations as the world transits into endemicity. Furthermore, the insights and recommendations provided in this research would allow countries to put more efforts and resources into strengthening health provisions and social safety nets for vulnerable populations to better prepare for future public health emergencies.
In summary, this scoping review has identified more discussions of problems than solutions as regards addressing the needs of vulnerable population groups when imposing physical distancing policy measures to control the spread of COVID-19. The negative impacts of physical distancing measures for multiple vulnerable population groups include unemployment and income loss, prolonged social isolation (leading to loneliness and an increased mental health burden), as well as disruption to access to non-COVID-19-related health services and delayed treatment, such as for non-communicable diseases for the older people and sexually transmitted diseases for sex workers and the people from sexual and gender minorities.
We also find that physical distancing measures exacerbate the vulnerabilities of different vulnerable population groups. Adverse employment and financial conditions constitute the primary vulnerability of low-income populations and migrant workers. Health vulnerability is typical among the older people and the people with long-term disabilities. Sex workers and the people from sexual and gender minorities are more vulnerable to sexually transmitted diseases. Social vulnerability is the primary vulnerability faced by victims of domestic violence, refugees and ethnic minority population groups. Regarding children, cognitive/communicative vulnerability is a major concern, and they need help to keep up with online learning. People in prison primarily face institutional/deferential vulnerability, as their decisions and behaviour are supervised by prison wardens.
The aggravation of the state of vulnerability of these populations, which were already vulnerable prior to the COVID-19 pandemic, should not be overlooked by governments. Addressing these negative impacts is of paramount importance to many countries as they have ripple impacts that affect the larger general population. Ignoring or downplaying the plight of vulnerable populations affected by the COVID-19 pandemic can translate into higher social care and financial burdens for governments in future as the pandemic continues to ravage the global economy.
Methods
Types and descriptions of vulnerability
While the meaning of “vulnerability” may be defined somewhat differently in various fields, the term “vulnerable populations” commonly refers to social groups that are exposed to increased risks or susceptibility to adverse health outcomes or diminished quality of life209. Based on the categorisation of the National Bioethics Advisory Committee of the United States (NBAC)210 and Yale University211, and drawing insights from the Organisation for Economic Co-operation and Development (OECD)212, Mikolai et al.213 and Mishra et al.214 (Supplementary Text A2), we constructed the categorisation of vulnerabilities and vulnerable groups shown in Table 3. It should be noted that these categories of vulnerable groups or vulnerabilities are not mutually exclusive. Different types of vulnerability may intersect with one another. For instance, while people in prison face institutional or deferential vulnerability, since they are incarcerated, they are also subject to overcrowding and are vulnerable to violence, under the social vulnerability category. Lack of access to necessities (e.g., water and sanitation) or lack of access to information technology can be co-producers of social and economic vulnerabilities.
Study design
A scoping review was conducted to examine the types and nature of physical distancing measures implemented across the world, and the extent to which they have negatively impacted vulnerable populations. A consolidation of global evidence is timely due to the rapid emergence of evidence since the beginning of the pandemic, and the lack of focus on the invisible and hidden impacts of physical distancing interventions—which have been applied nearly universally—on vulnerable populations that are already prone to many disadvantages due to pre-existing socio-economic fault lines.
In this scoping review, we posed the following review questions: (i) What physical distancing measures or interventions have been implemented and have they negatively impacted vulnerable populations? (ii) What ringfenced measures have been designed to protect vulnerable populations during the COVID-19 pandemic and how have they been implemented?
Search strategy and data sources
From March 2021 to April 2021, we searched ten databases to identify articles that could potentially be relevant to the issue of physical distancing measures. The databases were PubMed, Scopus, Web of Science, ProQuest, ProQuest Coronavirus Research Database, Embase, Educational Resource Information Center database, LITCOVID, the Cochrane database of systematic reviews, and WHO’s database of global literature on coronavirus disease. We developed the search strategy and search strings (Table 4) with the help of an experienced information specialist. The key terms used for the literature search focused on the themes of COVID-19 and physical distancing policy measures.
During the peer review process, in June 2022 we updated the search to include new literature published after April 2021 for vulnerable populations (the strategy for the updated search is in Supplementary Text A3). We removed duplicate results from the updated searches against previous results to ensure records were accurate.
Eligibility criteria and screening processes
Table 5 summarises the eligibility criteria for the screening of the studies.
The screening process involved screening the titles and abstracts to select articles relevant to vulnerable population groups, following the full inclusion and exclusion criteria and referring to the categories of vulnerabilities listed in Table 3. The first author conducted the entire screening process independently to identify relevant studies, while the third author randomly selected more than half of the records to screen independently. Both authors went through two iterations to achieve less than 10% discrepancies. All discrepancies were resolved through a detailed discussion among all three authors. Thereafter, the third author again cross-checked the records chosen by the first author to achieve final agreement on the included studies. Full texts of the identified relevant articles were later retrieved for data extraction.
Data extraction
Data extraction followed a predesigned data extraction template created through ongoing discussion among all the authors. To ensure quality control, all three authors piloted the data extraction practices for the first 10% of the identified full-text articles. The authors then discussed the data extraction results to build a consistent understanding of the aim and scope of the review. Thereafter, the first author extracted data from the remaining articles, and the other two authors validated a random selection of the data extraction results to ensure consistency.
Data analysis
We managed extracted data using Excel 16 (Microsoft Corporation). The data synthesis involved intensive line-by-line reading of the extracted qualitative information by all the authors. We grouped the studies by categories of vulnerable population groups examined using a framework synthesis approach. Framework synthesis enables structured analysis to be done by following a five-stage approach (familiarisation of the issue, framework selection, indexing, charting and finally mapping and interpretation). It is a versatile analytical approach that accounts for heterogeneity in the types of study included (quantitative, qualitative and mixed method) and is a suitable approach when theory is nascent and emergent, which was the case in this review215. At every stage of the analysis, discussions were held to achieve final agreement on the results.
Reporting summary
Further information on research design is available in the Nature Portfolio Reporting Summary linked to this article.
Data availability
The authors declare that all data generated and analysed during the current research are included in this article. The studies included in this scoping review are listed in its supplementary files.
References
Dong, E., Du, H. & Gardner, L. An interactive web-based dashboard to track COVID-19 in real time. Lancet Infect. Dis. 20, 533–534 (2020).
WHO. Overview of Public Health and Social Measures in the Context of COVID-19 (Interim guidance). (World Health Organization, 2020).
Chu, D. K. et al. Physical distancing, face masks, and eye protection to prevent person-to-person transmission of SARS-CoV-2 and COVID-19: a systematic review and meta-analysis. Lancet 395, 1973–1987 (2020).
Fricke, L. M., Glöckner, S., Dreier, M. & Lange, B. Impact of non-pharmaceutical interventions targeted at COVID-19 pandemic on influenza burden–a systematic review. J. Infect. 82, 1–35 (2021).
Phuoc, T. et al. Effect of the social distancing measures on the spread of COVID-19 in 10 highly infected countries. Sci. Total Environ. 742, 140430 (2020).
Tan, C. Ring-fencing intensified to avoid second Covid-19 circuit breaker in S’pore. The Straits Times (2021).
Moher, D., Liberati, A., Tetzlaff, J. & Altman, D. G., The PRISMA Group. PRISMA 2009 flow diagram. PLoS Med. 6, e1000097 (2009).
Moher, D., Liberati, A., Tetzlaff, J. & Altman, D. G., The PRISMA Group. Preferred reporting items for systematic reviews and meta-analyses: The PRISMA statement. PLoS Med. 6, e1000097 (2009).
Liberati, A. et al. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: explanation and elaboration. PLoS Med. 6, e1000100 (2009).
Mishra, M. & Majumdar, P. Social distancing during COVID-19: Will it change the Indian society? J. Health Manag. 22, 224–235 (2020).
Robb, C. E. et al. Associations of social isolation with anxiety and depression during the early COVID-19 pandemic: a survey of older adults in London, UK. Front. Psychiatry 11, 591120 (2020).
García-Prado, A., González, P. & Rebollo-Sanz, Y. F. Lockdown strictness and mental health effects among older populations in Europe. Econ. Hum. Biol. 45, 101116 (2022).
Paccagnella, O. & Pongiglione, B. Depression deterioration of older adults during the first wave of the COVID-19 outbreak in Europe. Soc. Sci. Med. 299, 114828 (2022).
Sit, R. W. S. et al. Explaining the psychosocial effects of covid-19 among older Hong Kong Chinese people—a qualitative analysis. J. Geriatr. Psychiatry Neurol. 35, 206–214 (2022).
Mendez-Lopez, A., Stuckler, D., McKee, M., Semenza, J. C. & Lazarus, J. V. The mental health crisis during the COVID-19 pandemic in older adults and the role of physical distancing interventions and social protection measures in 26 European countries. SSM Popul. Heal. 17, 101017 (2022).
Tavares, A. I. Older Europeans’ experience of unmet health care during the COVID-19 pandemic (first wave). BMC Health Serv. Res. 22, 1–13 (2022).
Juhn, Y. J. et al. Adherence to public health measures mitigates the risk of COVID-19 infection in older adults: a community-based study. Mayo Clin. Proc. 96, 912–920 (2021).
Shen, J., Wang, C., Dong, C., Tang, Z. & Sun, H. Reductions in mortality resulting from COVID-19 quarantine measures in China. J. Public Health (Bangk.) 43, 254–260 (2021).
Callow, M. A., Callow, D. D. & Smith, C. Older adults’ intention to socially isolate once COVID-19 stay-at-home orders are replaced with “Safer-at-Home” public health advisories: a survey of respondents in Maryland. J. Appl. Gerontol. 39, 1175–1183 (2020).
Colebunders, R., Siewe Fodjo, J. N., Vanham, G. & Van den Bergh, R. A call for strengthened evidence on targeted, non-pharmaceutical interventions against COVID-19 for the protection of vulnerable individuals in sub-Saharan Africa. Int. J. Infect. Dis. 99, 482–484 (2020).
Park, S. Y. et al. Early intervention reduces the spread of covid-19 in long-term care facilities in the Republic of Korea. Osong Public Heal. Res. Perspect. 11, 259–264 (2020).
McArthur, C. et al. Evaluating the effect of COVID-19 pandemic lockdown on long-term care residents’ mental health: a data-driven approach in New Brunswick. J. Am. Med. Dir. Assoc. 22, 187–192 (2021).
Echeverría, P. et al. COVIDApp as an innovative strategy for the management and follow-up of COVID-19 cases in long-term care facilities in Catalonia: Implementation study. JMIR Public Heal. Surveill. 6, e21163 (2020).
Bakshi, T. & Bhattacharyya, A. Socially distanced or socially connected? Well-being through ICT Usage among the Indian Elderly during COVID-19. Millenn. Asia 12, 190–208 (2021).
Amundsen, D. Digital technologies as a panacea for social isolation and loneliness among older adults: an intervention model for flourishing and wellbeing visual technologies as a panacea for social isolation. Video J. Educ. Pedagog. 5, 1–14 (2021).
Skinner, D. et al. Towards a definition of orphaned and vulnerable children. AIDS Behav. 10, 619–626 (2006).
Skinner, D. Defining Orphaned and Vulnerable Children (HSRC press, 2004).
Takaku, R. & Yokoyama, I. What the COVID-19 school closure left in its wake: Evidence from a regression discontinuity analysis in Japan. J. Public Econ. 195, 104364 (2021).
Viner, R. M. et al. School closure and management practices during coronavirus outbreaks including COVID-19: a rapid systematic review. Lancet Child Adolesc. Heal. 4, 397–404 (2020).
Burzynska, K. & Contreras, G. Gendered effects of school closures during the COVID-19 pandemic. Lancet 395, 1968 (2020).
Prata-Linhares, M. M., Cardoso, T. D. S. G., Lopes-Jr, D. S. & Zukowsky-Tavares, C. Social distancing effects on the teaching systems and teacher education programmes in Brazil: reinventing without distorting teaching. J. Educ. Teach. 46, 554–564 (2020).
Huber, S. G. & Helm, C. COVID-19 and schooling: evaluation, assessment and accountability in times of crises—reacting quickly to explore key issues for policy, practice and research with the school barometer. Educ. Assess. Eval. Account. 32, 237–270 (2020).
Montacute, C. & Cullinane, R. Covid-19 and Social Mobility Impact Brief #1: School Shutdown. Sutton Trust. 1–11 ED605807 (2020).
Naimark, D. et al. Simulation-based estimation of Sars-cov-2 infections associated with school closures and community-based nonpharmaceutical interventions in Ontario, Canada. JAMA Netw. Open 4, 1–13 (2021).
Fitzpatrick, R., Korin, A. & Riggall, A. An International Review of Plans and Actions for School Reopening. (Education Development Trust, 2020).
Kaisara, G. & Bwalya, K. J. Investigating the e-learning challenges faced by students during COVID-19 in Namibia. Int. J. High. Educ. 10, 308–318 (2021).
Obuaku-Igwe, C. ‘Umuntu ngumuntu ngabantu’ (a person is a person because of other people): reflections on student’s experiences of social isolation and the impact of a peer to peer mental health support group during covid-19 lockdown in South Africa. Youth Voice J. 2020, 58–71 (2020).
Nyashanu, M., Simbanegavi, P. & Gibson, L. Exploring the impact of COVID-19 pandemic lockdown on informal settlements in Tshwane Gauteng Province, South Africa. Glob. Public Health 15, 1443–1453 (2020).
Pellegrini, M. & Maltinti, C. “School never stops”: measures and experience in Italian schools during the COVID-19 lockdown. Best. Evid. Chin. Educ. 5, 649–663 (2020).
Loima, J. Socio-educational policies and Covid-19–a case study on Finland and Sweden in the Spring 2020. Int. J. Educ. Lit. Stud. 8, 59–75 (2020).
Iwata, K., Doi, A. & Miyakoshi, C. Was school closure effective in mitigating coronavirus disease 2019 (COVID-19)? Time series analysis using Bayesian inference. Int. J. Infect. Dis. 99, 57–61 (2020).
Rypdal, M. et al. Modelling suggests limited change in the reproduction number from reopening norwegian kindergartens and schools during the COVID-19 pandemic. PLoS ONE 16, e0238268 (2021).
Lo Moro, G. et al. Reopening schools during the COVID-19 pandemic: Overview and rapid systematic review of guidelines and recommendations on preventive measures and the management of cases. Int. J. Environ. Res. Public Health 17, 1–21 (2020).
Zimmerman, F. J. & Anderson, N. W. Association of the timing of school closings and behavioral changes with the evolution of the Coronavirus Disease 2019 Pandemic in the US. JAMA Pediatr. 175, 501–509 (2021).
Puntis, J. W. L. Is it really time to go back to school? Arch. Dis. Child. 106, e7 (2021).
Friedrich, F. et al. Early Impact of social distancing in response to COVID-19 on hospitalizations for acute bronchiolitis in infants in Brazil. Clin. Infect. Dis. 72, 2071–2075 (2021).
Esposito, S. & Principi, N. School closure during the Coronavirus Disease 2019 (COVID-19) Pandemic: An effective intervention at the global level? JAMA Pediatr. 174, 922–923 (2020).
Cheng, S. O. & Liu, A. Debates around the role of school closures in the Coronavirus 2019 Pandemic. JAMA Pediatr. 175, 105–106 (2021).
Formosinho, J. From schoolification of children to schoolification of parents?–educational policies in COVID times. Eur. Early Child. Educ. Res. J. 29, 141–152 (2021).
Krishnaratne, S. et al. Measures implemented in the school setting to contain the COVID-19 pandemic: a rapid scoping review. Cochrane Database Syst. Rev. 1–60 https://doi.org/10.1002/14651858.CD013812 (2020).
Pollock, A. M. Covid-19: Local implementation of tracing and testing programmes could enable some schools to reopen. BMJ 368, 1–2 (2020).
Fantini, M. P., Reno, C., Biserni, G. B., Savoia, E. & Lanari, M. COVID-19 and the re-opening of schools: a policy maker’s dilemma. Ital. J. Pediatr. 46, 1–3 (2020).
Melnick, H. & Darling-Hammond, L. Reopening Schools in the Context of COVID-19: Health and Safety Guidelines from Other Countries. Policy Brief. (Learning Policy Institute, 2020).
Rice, K., Wynne, B., Martin, V., Ackland, G. J. & Ackland Effect of school closures on mortality from coronavirus disease 2019: old and new predictions. BMJ 371, m3588 (2020).
Yui, L. Landscape measure: Animating the university campus to promote social distancing. N. Engl. J. High. Educ. EJ1265670 (2020).
Burns, A. A. C. & Gutfraind, A. Effectiveness of isolation policies in schools: evidence from a mathematical model of influenza and COVID-19. PeerJ 9, e11211 (2021).
Lee, B., Hanley, J. P., Nowak, S., Bates, J. H. T. & Hébert-Dufresne, L. Modeling the impact of school reopening on SARS-CoV-2 transmission using contact structure data from Shanghai. BMC Public Health 20, 1–9 (2020).
Panovska-Griffiths, J. et al. Determining the optimal strategy for reopening schools, the impact of test and trace interventions, and the risk of occurrence of a second COVID-19 epidemic wave in the UK: a modelling study. Lancet Child Adolesc. Heal 4, 817–827 (2020).
van den Berg, P. et al. Effectiveness of 3 versus 6 ft of physical distancing for controlling spread of coronavirus disease 2019 among primary and secondary students and staff: a retrospective, statewide cohort study. Clin. Infect. Dis. 02132, 1–8 (2021).
Krishnamachari, B. et al. The role of mask mandates, stay at home orders and school closure in curbing the COVID-19 pandemic prior to vaccination. Am. J. Infect. Control 49, 1036–1042 (2021).
Malkus, N. Reopening in the Shadow of Covid-19: Beginning the First Full Coronavirus School Year (American Enterprise Institute 2020).
Reykdal, C. Reopening Washington Schools 2020: District Planning Guide. (Washington Office of Superintendent of Public Instruction, 2020).
Donohue, J. M. & Miller, E. COVID-19 and school closures. J. Am. Med. Assoc. 324, 845–847 (2020).
von Schroeter, M., Weiss, N. & O’rourke, T. How Should Massachusetts Reopen its K-12 Schools in the Fall? Lessons from Abroad and Other States. (Pioneer Institute for Public Policy Research, 2020).
Southall, E. et al. An analysis of school absences in England during the Covid-19 pandemic. BMC Med. 19, 1–14 (2021).
Brooks-Pollock, E., Read, J. M., Mclean, A., Keeling, M. J. & Danon, L. Using social contact data to predict and compare the impact of social distancing policies with implications for school re-opening. medRxiv 8, https://doi.org/10.1101/2020.07.25.20156471 (2020).
Ghia, J.-E., Gaulin, S., Ghia, L., Garancher, L. & Flamand, C. Informing children citizens efficiently to better engage them in the fight against COVID-19 pandemic. PLoS Negl. Trop. Dis. 14, e0008828 (2020).
Singh, S. et al. Impact of COVID-19 and lockdown on mental health of children and adolescents: a narrative review with recommendations. Psychiatry Res. 293, 1–10 (2020).
Biswas, S. & Biswas, A. Anxiety level among students of different college and universities in India during lock down in connection to the COVID-19 pandemic. J. Public Heal. 31, 49–55 (2021).
Chitapure, T., Bhodaji, S., Zanwar, M. & Malani, R. Impact of covid-19 pandemic lockdown on mental and physical health of students: a cross-sectional study. Int. J. Res. Pharm. Sci. 11, 1710–1714 (2020).
Yayci, L. & Kendirci, A. Determination of educational/academic and some social behavioral trends of elementary school students in Turkey during Coronavirus (Covid-19) pandemic days. Int. Online J. Educ. Teach. 8, 358–380 (2021).
Wyse, A. E., Stickney, E. M., Butz, D., Beckler, A. & Close, C. N. The potential impact of COVID-19 on student learning and how schools can respond. Educ. Meas. Issues Pract. 39, 60–64 (2020).
Willis, J., Krausen, K. & Caparas, R. Managing Public Education Resources in California during and after the Coronavirus Crisis: Practical Tips and Considerations for School District and Charter School Leaders. Crisis Response Resource (WestEd, 2020).
Willis, J., Krausen, K. & Outlaw, L. Managing Public Education Resources during the Coronavirus Crisis: Practical Tips and Considerations for School District Leaders. Crisis Response Resource. (WestEd, 2020).
Grooms, A. A. & Childs, J. “We Need to Do Better by Kids”: changing routines in U.S. schools in response to COVID-19 school closures. J. Educ. Stud. Place. Risk 26, 135–156 (2021).
Seymour, K., Skattebol, J. & Pook, B. Compounding education disengagement: COVID-19 lockdown, the digital divide and wrap-around services. J. Child. Serv. 15, 243–251 (2020).
Rogers, A. C. Vulnerability, health and health care. J. Adv. Nurs. 26, 65–72 (1997).
Alderman, J. & Harjoto, M. COVID-19: US shelter-in-place orders and demographic characteristics linked to cases, mortality, and recovery rates. Transform. Gov. 15, 627–644 (2020).
Jay, J. et al. Neighbourhood income and physical distancing during the COVID-19 pandemic in the United States. Nat. Hum. Behav. 4, 1294–1302 (2020).
Oladimeji, O., Atiba, B. P., A Mbokazi, J. & Hyera, F. L. M. The homeless, inmates and refugees in Africa in the face of COVID-19 outbreak. Open Public Health J. 13, 306–308 (2020).
Agoramoorthy, G. & Hsu, M. J. How the Coronavirus lockdown impacts the impoverished in India. J. Racial Ethn. Heal. Disparities 8, 1–6 (2021).
Weill, J. A., Stigler, M., Deschenes, O. & Springborn, M. R. Social distancing responses to COVID-19 emergency declarations strongly differentiated by income. Proc. Natl Acad. Sci. USA 117, 19658–19660 (2020).
McIntosh, A. et al. Effect of COVID-19 lockdown on hospital admissions and mortality in rural KwaZulu-Natal, South Africa: Interrupted time series analysis. BMJ Open 11, 1–10 (2021).
Romero-Michel, J. C. et al. Health and economic measures in response to the COVID-19 pandemic-effect on street vendors. J. Infect. Dev. Ctries. 15, 198–203 (2021).
Barnett-Howell, Z., Mobarak, A. M. & Watson, O. J. The benefits and costs of social distancing in high- and low-income countries. Trans. R. Soc. Trop. Med. Hyg. 115, 807–819 (2021).
Quaife, M. et al. The impact of COVID-19 control measures on social contacts and transmission in Kenyan informal settlements. BMC Med. 18, 1–11 (2020).
Lou, J., Shen, X. & Niemeier, D. Are stay-at-home orders more difficult to follow for low-income groups? J. Transp. Geogr. 89, 102894 (2020).
Jorge, D. C. P. et al. Assessing the nationwide impact of Covid-19 mitigation policies on the transmission rate of SARS-CoV-2 in Brazil. Epidemics 35, 100465 (2021). (1–11).
Chang, H.-Y. et al. Differential impact of mitigation policies and socioeconomic status on COVID-19 prevalence and social distancing in the United States. BMC Public Health 21, 1–10 (2021).
Lau, L. L., Hung, N. & Wilson, K. COVID-19 response strategies: Considering inequalities between and within countries. Int. J. Equity Health 19, 1–3 (2020).
Ward, M. South Africa’s COVID-19 lockdown dilemma. Emerald Emerg. Mark. Case Stud. 10, 1–10 (2020).
Kumar, S. et al. Socio-economic impact of first 21 days nationwide lockdown- 1 on the spread of SARS-COV-2 in India in relation to health. J. Fam. Med. Prim. Care 9, 4557–4562 (2020).
Singh, I., Singh, J. & Baruah, A. Income and employment changes under COVID-19 lockdown: a study of Urban Punjab. Millenn. Asia 11, 391–412 (2020).
Banerjee, T., Nayak, A. & Zhao, H. Y. A county-level study of the effects of state-mandated COVID-19 lockdowns on urban and rural restaurant visits using consumers’ cell phone geo-location data. J. Public Heal. Theory Pr. 31, 249–258 (2021).
Mandal, K. K., Alam, S., Ranjan, A., Dharanirajan, K. & Kumari, P. A review of India’s response to COVID-19 outbreak and impact of lockdown on Indian economy. J. Crit. Rev. 7, 402–408 (2020).
Wasdani, K. P. & Prasad, A. The impossibility of social distancing among the urban poor: the case of an Indian slum in the times of COVID-19. Local Environ. 25, 414–418 (2020).
Jung, J., Manley, J. & Shrestha, V. Coronavirus infections and deaths by poverty status: The effects of social distancing. J. Econ. Behav. Organ. 182, 311–330 (2021).
Yilmazkuday, H. COVID-19 and unequal social distancing across demographic groups. Reg. Sci. Policy Pract. 12, 1235–1248 (2020).
Bonaccorsi, G. et al. Economic and social consequences of human mobility restrictions under COVID-19. Proc. Natl Acad. Sci. USA 117, 15530–15535 (2020).
Singh, S., Shaikh, M., Hauck, K. & Miraldo, M. Impacts of introducing and lifting nonpharmaceutical interventions on COVID-19 daily growth rate and compliance in the United States. Proc. Natl Acad. Sci. USA 118, e2021359118 (2021).
Garnier, R., Benetka, J. R., Kraemer, J. & Bansal, S. Socioeconomic disparities in social distancing during the COVID-19 pandemic in the United States: Observational study. J. Med. Internet Res. 23, 1–8 (2021).
Alon, T., Kim, M., Lagakos, D. & Vanvuren, M. How should policy responses to the covid-19 pandemic differ in the developing world?. Natl. Bur. Econ. Res. Working Paper Series No. 27273. (2020).
Bennett, M. All things equal? Heterogeneity in policy effectiveness against COVID-19 spread in Chile. World Dev. 137, 105208 (2021).
Iwuoha, V. C. & Aniche, E. T. Covid-19 lockdown and physical distancing policies are elitist: towards an indigenous (Afro-centred) approach to containing the pandemic in sub-urban slums in Nigeria. Local Environ. 25, 631–640 (2020).
Mbogo, R. W. & Odhiambo, J. W. COVID-19 outbreak, social distancing and mass testing in Kenya-insights from a mathematical model. Afr. Mat. https://doi.org/10.1007/s13370-020-00859-1 (2021).
Sahu, M. & Dobe, M. How the largest slum in india flattened the covid curve? A case study. South East. Eur. J. Public Heal. 14, 1–15 (2020).
Silva, D. S. & Smith, M. J. Social distancing, social justice, and risk during the COVID-19 pandemic. Can. J. Public Heal. 111, 459–461 (2020).
Iwara, I. O., Musvipwa, F., Amaechi, K. E. & Raselekoane, R. COVID-19 lock-down socio-economic challenges faced by households in rural areas: A perspective from Vhembe district, South Africa. Sociol. Pregl. 54, 761–798 (2020).
Mathias, K., Rawat, M., Philip, S. & Grills, N. ‘We’ve got through hard times before’: acute mental distress and coping among disadvantaged groups during COVID-19 lockdown in North India-a qualitative study. Int. J. Equity Health 19, 1–12 (2020).
Pandey, G., Moghal, S., Barodia, R. & Carey, W. COVID-19 and its effects on the mental health of people living in urban slums in India. J. Inf. Knowl. Manag. 21, 2240003 (2022).
Khan, M., Roy, P., Matin, I., Rabbani, M. & Chowdhury, R. An adaptive governance and health system response for the COVID-19 emergency. World Dev. 137, 105213 (2021).
Jiang, X., Gong, W., Gao, Y., Fraser, C. & Holmes, C. Modelling the impact of rapid tests, tracing and distancing in lower-income countries suggest optimal policies varies with rural-urban settings. medRxiv https://doi.org/10.1101/2021.03.17.21253853 (2021).
Denford, S. et al. Understanding patterns of adherence to COVID-19 mitigation measures: a qualitative interview study. J. Public Health (Bangk.) 43, 508–516 (2021).
Arndt, C. et al. Covid-19 lockdowns, income distribution, and food security: an analysis for South Africa. Glob. Food Sec. 26, 100410 (2020).
Basu, P., Bell, C. & Edwards, T. H. COVID social distancing and the poor: An analysis of the evidence for England. B. E. J. Macroecon. 22, 211–240 (2022).
Dahab, M. et al. COVID-19 control in low-income settings and displaced populations: What can realistically be done? Confl. Health 14, 1–6 (2020).
Kerkhoff, A. D. et al. Evaluation of a novel community-based COVID-19 ‘Test-to-Care’ model for low-income populations. PLoS ONE 15, e0239400 (2020).
Nachega, J. B. et al. Contact tracing and the COVID-19 response in Africa: Best practices, Key Challenges, and lessons learned from Nigeria, Rwanda, South Africa, and Uganda. Am. J. Trop. Med. Hyg. 104, 1179–1187 (2021).
United Nations. International Convention on the Protection of the Rights of All Migrant Workers and Members of Their Families (adopted 18 December 1990, entered into force 1 July 2003). United Nations Treaty Ser. (Doc. A/RES/45/158) 2220, (United Nations, 2003).
United Nations. Researching the impact of the pandemic on internal migrant workers in India. United Nations: Academic Impact (United Nations, 2021). Available at: https://www.un.org/en/academic-impact/researching-impact-pandemic-internal-migrant-workers-india. (Accessed: 17th September 2021)
International Labour Organization (ILO). Migrant domestic workers. (International Labour Organization (ILO), 2021). Available at: https://www.ilo.org/global/topics/labour-migration/policy-areas/migrant-domestic-workers/lang–en/index.htm. (Accessed: 31st August 2021)
Choudhari, R. COVID 19 pandemic: mental health challenges of internal migrant workers of India. Asian J. Psychiatry J. 54, 102254 (2020).
Bojórquez, I., Odgers-Ortiz, O. & Olivas-Hernández, O. L. Psychosocial and mental health during the COVID-19 lockdown: a rapid qualitative study in migrant shelters at the Mexico-United States border. Salud Ment. 44, 167–175 (2021).
Singh, G. P. & Arun, P. Subjective well-being among migrant workers residing in a shelter home during lockdown: a pilot survey from North India. Prim. Care Companion CNS Disord. 24, 38916 (2021).
Crouzet, L. et al. Impact of the COVID-19 pandemic on vulnerable groups, including homeless persons and migrants, in France: a qualitative study. Prev. Med. Rep. 26, 101727 (2022).
Fu, L., Lindenmeyer, A., Phillimore, J. & Lessard-Phillips, L. Vulnerable migrants’ access to healthcare in the early stages of the COVID-19 pandemic in the UK. Public Health 203, 36–42 (2022).
Guha, P., Islam, B. & Hussain, M. A. COVID-19 lockdown and penalty of joblessness on income and remittances: a study of inter-state migrant labourers from Assam, India. J. Public Aff. 21, e2470 (2020).
Kumar, S. & Choudhury, S. Migrant workers and human rights: a critical study on India’s COVID-19 lockdown policy. Soc. Sci. Humanit. Open 3, 100130 (2021).
Yee, K. et al. Stressors and coping strategies of migrant workers diagnosed with COVID-19 in Singapore: a qualitative study. BMJ Open 11, 1–8 (2021).
Melillo, T. Public health measures to control the spread of COVID-19 amongst the migrant population in Malta. Eur. J. Public Health 30, ckaa165.429 (2020).
Nyamukamba, P., Mujuru, N. M. & Isaacs, S. Early impacts of covid-19 and government’s intervention and prevention actions in South Africa. J. Hum. Ecol. 71, 266–276 (2020).
Chan, L. G. & Kuan, B. Mental health and holistic care of migrant workers in Singapore during the Covid-19 pandemic. J. Glob. Health 10, 1–5 (2020).
Liebling, A. Vulnerability and prison suicide. Br. J. Criminol. 35, 173–187 (1995).
Morash, M., Jeong, S., Bohmert, M. N. & Bush, D. R. Men’s vulnerability to prisoner-on-prisoner sexual violence: a state correctional system case study. Prison J. 92, 290–311 (2012).
Simpson, P. L. & Butler, T. G. Covid-19, prison crowding, and release policies. BMJ 369, 1–2 (2020).
Simpson, P. L., Simpson, M., Adily, A., Grant, L. & Butler, T. Prison cell spatial density and infectious and communicable diseases: a systematic review. BMJ Open 9, e026806 (2019).
Henry, B. F. Social distancing and incarceration: policy and management strategies to reduce COVID-19 transmission and promote health equity through decarceration. Heal. Educ. Behav. 47, 536–539 (2020).
Maycock, M. & Dickson, G. Analysing the views of people in custody about the management of the COVID-19 pandemic in the Scottish Prison Estate. Int. J. Prison. Health https://doi.org/10.1108/IJPH-09-2020-0065 (2021).
Lindström, M., Ahlstrand, E. & Kärrholm, J. Sweden’s response to the COVID-19 outbreak. Vict. Offenders 15, 1203–1214 (2020).
Schotland, S. D. A plea to apply principles of quarantine ethics to prisoners and immigration detainees during the COVID-19 crisis. J. Law Biosci. 1–11 https://doi.org/10.1093/jlb/lsaa070 (2020).
Fróis, C. COVID-19 pandemic and social distancing in prisons. Anthropol. Today 36, 25–26 (2020).
Centers for Disease Control and Prevention (USA). Disability and health overview. (Centers for Disease Control and Prevention, 2020). Available at: https://www.cdc.gov/ncbddd/disabilityandhealth/disability.html. (Accessed: 31st August 2021)
World Health Organization (WHO). Disability. Available at: https://www.who.int/health-topics/disability#tab=tab_1. (Accessed: 17th September 2021)
Batavia, A. I. & Beaulaurier, R. L. The financial vulnerability of people with disabilities: assessing poverty risks. J. Sociol. Soc. Welf. 28, 139–162 (2001).
Dalise, S. et al. Psycho-social impact of social distancing and isolation due to the COVID-19 containment measures on patients with physical disabilities. Eur. J. Phys. Rehabil. Med. 57, 158–165 (2021).
Kim, J. Y., Han, J.-O. & Lee, H. Recommendation for response to the COVID-19 pandemic: Korean context of “distancing in daily life,” considering vulnerable population. Int. J. Equity Health 19, 1–5 (2020).
Solé, B. et al. Effects of the COVID-19 pandemic and lockdown in Spain: comparison between community controls and patients with a psychiatric disorder. Preliminary results from the BRIS-MHC STUDY. J. Affect. Disord. 281, 13–23 (2021).
Goddard, K. S., Schulz, J., Nzuki, I. & Hall, J. P. Examining the impacts of the coronavirus pandemic and social distancing on the health of people with mobility disabilities. Front. Public Heal. 10, 875880 (2022).
Gothwal, V. K., Kodavati, K. & Subramanian, A. Life in lockdown: impact of COVID-19 lockdown measures on the lives of visually impaired school-age children and their families in India. Ophthalmic Physiol. Opt. 42, 301–310 (2022).
Kaur, R., Boobna, T. & Kallingal, P. Effect of Covid-19 lockdown on Indian children with autism. Res. Dev. Disabil. 125, 104230 (2022).
Meguid, N. A. et al. Influence of COVID-19 pandemic lockdown on a sample of Egyptian children with Down syndrome. Egypt. J. Med. Hum. Genet. 23, 1–8 (2022).
Theis, N., Campbell, N., De Leeuw, J., Owen, M. & Schenke, K. C. The effects of COVID-19 restrictions on physical activity and mental health of children and young adults with physical and/or intellectual disabilities. Disabil. Health J. 14, 101064 (2021).
Nowicki, J. M. Distance learning: challenges providing services to K-12 English learners and students with disabilities during COVID-19. Government Accountability Office (GAO) Report to Congressional Committees (2020).
Yates, S., Dickinson, H., Smith, C. & Tani, M. Flexibility in individual funding schemes: how well did Australia’s National Disability Insurance Scheme support remote learning for students with disability during COVID-19? Soc. Policy Adm. 55, 906–920 (2020).
Pyett, P. M. & Warr, D. J. Vulnerability on the streets: female sex workers and HIV risk. AIDS Care Psychol. Socio-Med. Asp. AIDS/HIV 9, 539–547 (1997).
Ranebennur, V., Gaikwad, S., Ramesh, S. & Bhende, A. Addressing vulnerabilities of female sex workers in an HIV prevention intervention in Mumbai and Thane: experiences from the Aastha project. HIV/AIDS Res. Palliat. Care 6, 9–18 (2014).
Janyam, S. et al. Protecting sex workers in Thailand during the COVID-19 pandemic: opportunities to build back better. WHO South-East Asia J. public Heal 9, 100–103 (2020).
Reza-Paul, S. et al. Community action for people with HIV and sex workers during the COVID-19 pandemic in India. WHO South-East Asia J. public Heal. 9, 104–106 (2020).
Macharia, P. et al. Sexual health among Kenyan male sex workers in a time of COVID-19. Health Educ. J. 80, 119–127 (2021).
Adebisi, Y. A. et al. Sex workers should not be forgotten in Africa’s COVID-19 response. Am. J. Trop. Med. Hyg. 103, 1780–1782 (2020).
Tan, R. K. J. et al. COVID-19 and the shifting organisation of sex work markets in Singapore. Cult. Heal. Sex. https://doi.org/10.1080/13691058.2021.2014975 (2021).
Callander, D. et al. Sex workers are returning to work and require enhanced support in the face of COVID-19: results from a longitudinal analysis of online sex work activity and a content analysis of safer sex work guidelines. Sex. Health 17, 384–386 (2020).
Gichuna, S. et al. Access to healthcare in a time of COVID-19: Sex workers in crisis in Nairobi, Kenya. Glob. Public Health 15, 1430–1442 (2020).
Usher, K., Bhullar, N., Durkin, J., Gyamfi, N. & Jackson, D. Family violence and COVID-19: Increased vulnerability and reduced options for support. Int. J. Ment. Health Nurs. 29, 549–552 (2020).
Calderbank, R. Abuse and disabled people: vulnerability or social indifference? Disabil. Soc. 15, 521–534 (2000).
Hague, G., Thiara, R. & Mullender, A. Disabled women, domestic violence and social care: the risk of isolation, vulnerability and neglect. Br. J. Soc. Work 41, 148–165 (2011).
Vives-cases, C., La Parra-Casado, D., Estévez, J. F., Torrubiano-domínguez, J. & Sanz-barbero, B. Intimate partner violence against women during the COVID-19 lockdown in Spain. Int. J. Environ. Res. Public Health 18, 4698 (2021).
Ditekemena, J. D. et al. Intimate partners violence against women during a covid-19 lockdown period: Results of an online survey in 7 provinces of the Democratic Republic of Congo. Int. J. Environ. Res. Public Health 18, 5108 (2021).
Nduna, M. & Tshona, S. O. Domesticated poly-violence against women during the 2020 Covid-19 lockdown in South Africa. Psychol. Stud. (Mysore). 66, 347–353 (2021).
Iesue, L., Casanova, F. O. & Piquero, A. R. Domestic violence during a global pandemic: Lockdown policies and their impacts across Guatemala. J. Contemp. Crim. Justice 37, 589–614 (2021).
Tripathi, P., Dwivedi, P. S. & Sharma, S. Psychological impact of domestic violence on women in India due to COVID-19. Int. J. Hum. Rights Healthc. https://doi.org/10.1108/IJHRH-12-2021-0208 (2022).
Jahid, A. Unsafe at home: the increased trend of domestic violence during the COVID-19 pandemic in Bangladesh. J. Adult Prot. 24, 15–21 (2022).
Mahmood, N., Kamruzzaman, M., Rahman, A., Reidpath, D. D. & Akhter, S. Impact of the COVID-19 lockdown on intimate partner violence: Issues of non-reporting in Bangladesh. Women’s Heal. 18, https://doi.org/10.1177/17455057221087888 (2022).
Baron, E. J., Goldstein, E. G. & Wallace, C. T. Suffering in silence: How COVID-19 school closures inhibit the reporting of child maltreatment. J. Public Econ. 190, 104258 (2020).
Rengasamy, E. R. et al. Impact of COVID-19 lockdown: Domestic and child abuse in Bridgend. Child Abus. Negl. 130, 105386 (2022).
Universities UK. Beginning the conversation: responding to domestic violence and abuse in higher education communities during Covid-19 pandemic. (Universities UK, 2020).
Black, R. Livelihoods under stress: a case study of refugee vulnerability in Greece. J. Refug. Stud. 7, 360–377 (1994).
Johnson, R. A. I. Refugee camp security: decreasing vulnerability through demographic controls. J. Refug. Stud. 24, 23–46 (2011).
Dhesi, S., Isakjee, A. & Davies, T. Public health in the Calais refugee camp: Environment, health and exclusion. Crit. Public Health 28, 140–152 (2018).
Hameed, S., Sadiq, A. & Din, A. U. The increased vulnerability of refugee population to mental health disorders. Kans. J. Med. 11, 20–23 (2019).
Júnior, J. G. et al. A crisis within the crisis: the mental health situation of refugees in the world during the 2019 coronavirus (2019-nCoV) outbreak. Psychiatry Res. 288, 1–2 (2020).
Pinzón-Espinosa, J., Valdés-Florido, M. J., Riboldi, I., Baysak, E. & Vieta, E. The Covid-19 pandemic and mental health of refugees, asylum seekers, and migrants. J. Affect. Disord. 280, 407–408 (2021).
Peprah, P. Ageing out of place in COVID-19 pandemic era: how does the situation look like for older refugees in camps? Arch. Gerontol. Geriatr. 90, 104149 (2020).
Spernovasilis, N., Markaki, L. & Tsioutis, C. Challenges posed by covid-19 to refugee camps on the greek islands: We are all humans after all. Pneumon 33, 7–8 (2020).
Leiner, A., Sammon, M., Perry, H. & Dunavant, S. Facing COVID-19 and refugee camps on the U.S. Border. J. Emerg. Med. 59, 143–145 (2020).
Gilman, R. T., Mahroof-Shaffi, S., Harkensee, C. & Chamberlain, A. T. Modelling interventions to control COVID-19 outbreaks in a refugee camp. BMJ Glob. Heal. 5, 1–9 (2020).
Mattar, S. & Piwowarczyk, L. A. COVID-19 and U.S.-based refugee populations: Commentary. Psychol. Trauma 12, 228–229 (2020).
Alemi, Q., Stempel, C., Siddiq, H. & Kim, E. Refugees and covid-19: Achieving a comprehensive public health response. Bull. World Health Organ 98, 510–510A (2020).
Ceccon, C. & Moscardino, U. Impact of COVID-19 and lockdown on mental health and future orientation among young adult asylum seekers in Italy: A mixed-methods study. Transcult. Psychiatry https://doi.org/10.1177/13634615221098306 (2022).
United Nations. Indigenous peoples and ethnic minorities: Marginalization is the norm. In Promoting Inclusion through Social Protection: The Report on the World Social Situation. 2018 97–108 (United Nations, 2018).
Le, K. & Nguyen, M. The psychological consequences of COVID-19 lockdowns. Int. Rev. Appl. Econ. 35, 147–163 (2021).
Khan, S., Asif, A. & Jaffery, A. E. Language in a time of COVID-19: literacy bias ethnic minorities face during COVID-19 from online information in the UK. J. Racial Ethn. Heal. Disparities 1–7 https://doi.org/10.1007/s40615-020-00883-8 (2020).
Littlejohn, T., Poteat, T. & Beyrer, C. Sexual and gender minorities, public health, and ethics. in The Oxford Handbook of Public Health Ethics (eds. Mastroianni, A. C., Kahn, J. P. & Kass, N. E.) 231–244 (Oxford University Press, 2019).
Ganju, D. & Saggurti, N. Stigma, violence and HIV vulnerability among transgender persons in sex work in Maharashtra, India. Cult. Heal. Sex. 19, 903–917 (2017).
Salerno, J. P., Devadas, J., Pease, M., Nketia, B. & Fish, J. N. Sexual and gender minority stress amid the COVID-19 pandemic: implications for LGBTQ young persons’ mental health and well-being. Public Health Rep. 135, 721–727 (2020).
Melin, K., Santiago Quiñones, D. & Rodríguez-Díaz, C. E. Socially distant and out of reach: Unintended consequences of COVID-19 prevention efforts on transgender and gender non-binary populations in Puerto Rico. J. Subst. Abus. Treat. 122, 108209 (2021).
Rhodes, S. D. et al. A rapid qualitative assessment of the impact of the COVID-19 pandemic on a racially/ethnically diverse sample of gay, bisexual, and other men who have sex with men living with HIV in the US South. AIDS Behav. 25, 58–67 (2021).
Nelson, K. M., Gordon, A. R., John, S. A., Stout, C. D. & Macapagal, K. “Physical Sex Is Over for Now”: impact of COVID-19 on the well-being and sexual health of adolescent sexual minority males in the U.S. J. Adolesc. Heal. 67, 756–762 (2020).
Torres, T. S. et al. Impact of COVID-19 pandemic on sexual minority populations in Brazil: An analysis of social/racial disparities in maintaining social distancing and a description of sexual behavior. AIDS Behav. 25, 73–84 (2021).
Toze, M., Westwood, S. & Hafford-Letchfield, T. Social support and unmet needs among older trans and gender non-conforming people during the COVID-19 ‘lockdown’ in the UK. Int. J. Transgend. Heal. https://doi.org/10.1080/26895269.2021.1977210 (2021).
Atchison, C. J. et al. Perceptions and behavioural responses of the general public during the COVID-19 pandemic: a cross-sectional survey of UK Adults. medRxiv https://doi.org/10.1101/2020.04.01.20050039 (2020).
Lewnard, J. A. & Lo, N. C. Scientific and ethical basis for social-distancing interventions against COVID-19. Lancet Infect. Dis. 20, 631–633 (2020).
Colbourn, T. COVID-19: extending or relaxing distancing control measures. Lancet Public Heal. 5, e236–e237 (2020).
Hale, T. et al. A global panel database of pandemic policies (Oxford COVID-19 Government Response Tracker). Nat. Hum. Behav. 5, 529–538 (2021).
Poteat, T. C., Reisner, S. L., Miller, M. & Wirtz, A. L. Vulnerability to COVID-19-related harms among transgender women with and without HIV infection in the Eastern and Southern U.S. J. Acquir. Immune Defic. Syndr. 85, e67–e69 (2020).
Jones, B. A., Bowe, M., McNamara, N., Guerin, E. & Carter, T. Exploring the mental health experiences of young trans and gender diverse people during the Covid-19 pandemic. Int. J. Transgender Heal. 1–13 https://doi.org/10.1080/26895269.2021.1890301 (2021).
Stephenson, R. et al. Sex in the time of COVID-19: results of an online survey of gay, bisexual and other men who have sex with men’s experience of sex and HIV prevention during the US COVID-19 epidemic. AIDS Behav. 25, 40–48 (2020).
Mukumbang, F. C., Ambe, A. N. & Adebiyi, B. O. Unspoken inequality: How COVID-19 has exacerbated existing vulnerabilities of asylum-seekers, refugees, and undocumented migrants in South Africa. Int. J. Equity Health 19, 1–7 (2020).
Flaskerud, J. H. & Winslow, B. J. Conceptualizing vulnerable populations health-related research. Nurs. Res. 47, 69–78 (1998).
NBAC (National Bioethics Advisory Commission of the United States). Ethical and policy issues in research involving human participants. Report and Recommendations of the National Bioethics Advisory Commission (NBAC, 2001).
Yale University. Categories of vulnerability–specific vulnerable populations. HSP Module 7: Protecting Vulnerable Subjects Available at: https://assessment-module.yale.edu/human-subjects-protection/categories-vulnerability-specific-vulnerable-populations. (Accessed: 27th July 2021).
OECD. COVID-19: Protecting people and societies. OECD Policy Responses to Coronavirus (COVID-19) (OECD, 2020). https://doi.org/10.1787/9870c393-en.
Mikolai, J., Keenan, K. & Kulu, H. Intersecting household-level health and socio-economic vulnerabilities and the COVID-19 crisis: An analysis from the UK. SSM Popul. Heal. 12, 100628 (2020).
Mishra, S. V., Gayen, A. & Haque, S. M. COVID-19 and urban vulnerability in India. Habitat Int. 103, 102230 (2020).
Brunton, G., Oliver, S. & Thomas, J. Innovations in framework synthesis as a systematic review method. Res. Synth. Methods 11, 316–330 (2020).
Venturieri, V. R., Goncalves, M. S. & Fuck, V. R. Mitigation of COVID-19 using social distancing of the elderly in Brazil The vertical quarantine effects in hospitalizations and deaths. medRxiv 2752, 1–28 (2021).
Claverie, J.-M. A scenario to safely ease the covid-19 lockdown while allowing economic recovery. Virologie 24, E23–E25 (2020).
Choi, E. Y., Farina, M. P., Wu, Q. & Ailshire, J. COVID-19 social distancing measures and loneliness among older adults. J. Gerontol. Ser. B 1–12 https://doi.org/10.1093/geronb/gbab009 (2021).
Michalowsky, B., Hoffmann, W., Bohlken, J. & Kostev, K. Effect of the COVID-19 lockdown on disease recognition and utilisation of healthcare services in the older population in Germany: a cross-sectional study. Age Ageing 50, 317–325 (2021).
Babu, T. A. & Selvapandiyan, J. The psychological effects of COVID-19 Pandemic related lockdown in children. Indian Pediatr. 57, 1087 (2020).
Nomura, K. et al. Cross-sectional survey of depressive symptoms and suicide-related ideation at a Japanese national university during the COVID-19 stay-home order. Environ. Health Prev. Med. 26, 30 (2021).
Thakur, K., Kumar, N. & Sharma, N. R. Effect of the Pandemic and Lockdown on Mental Health of Children. Indian J. Pediatr. 87, 552 (2020).
Caroppo, E. et al. Unequal effects of the national lockdown on mental and social health in Italy. Ann. Ist. Super. Sanita 56, 497–501 (2020).
DeArmond, M., Chu, L. & Gundapaneni, P. How Are School Districts Addressing Student Social-emotional Needs during the Pandemic? (Center on Reinventing Public Education, 2021).
The Lancet Child and Adolescent Health. Pandemic school closures: risks and opportunities. Lancet Child Adolesc. Heal. 4, 341 (2020).
Catling, J. C., Bayley, A., Begum, Z., Wardzinski, C. & Wood, A. Effects of the COVID-19 lockdown on mental health in a UK student sample. BMC Psychol. 10, 118 (2022).
Lindell-Postigo, D., Zurita-Ortega, F., Ortiz-Franco, M. & González-Valero, G. Cross-sectional study of self-concept and gender in relation to physical activity and martial arts in Spanish adolescents during the COVID-19 lockdown. Educ. Sci. 10, 1–10 (2020).
Yadav, R. K. et al. Anxiety and depression among health sciences students in home quarantine during the COVID-19 Pandemic in selected provinces of Nepal. Front. Public Heal. 9, 580561 (2021).
Ali, A., Siddiqui, A. A., Arshad, M. S., Iqbal, F. & Arif, T. B. Effects of COVID-19 pandemic and lockdown on lifestyle and mental health of students: A retrospective study from Karachi, Pakistan. Ann. Med. Psychol. (Paris). https://doi.org/10.1016/j.amp.2021.02.004 (2021).
Manjareeka, M. & Pathak, M. COVID-19 lockdown anxieties: Is student a vulnerable group? J. Indian Assoc. Child Adolesc. Ment. Heal. 17, 72–80 (2020).
Bahn, G. H. Coronavirus disease 2019, school closures, and children’s mental health. J. Korean Acad. Child Adolesc. Psychiatry 31, 74–79 (2020).
Duarte, C. et al. COVID-19 outbreak in a state prison: a case study on the implementation of key public health recommendations for containment and prevention. BMC Public Health 22, 977 (2022).
Hamadani, J. D. et al. Immediate impact of stay-at-home orders to control COVID-19 transmission on socioeconomic conditions, food insecurity, mental health, and intimate partner violence in Bangladeshi women and their families: an interrupted time series. Lancet Glob. Heal. 8, e1380–e1389 (2020).
Boserup, B., McKenney, M. & Elkbuli, A. Alarming trends in US domestic violence during the COVID-19 pandemic. Am. J. Emerg. Med. 38, 2753–2755 (2020).
O’Connell, C. & Lucić, L. An informal education intervention in response to the Covid-19 pandemic: homework mentorships in a Berlin refugee shelter. Hum. Arenas 4, 616–631 (2021).
Hamman, M. K. Disparities in COVID-19 mortality by county racial composition and the role of spring social distancing measures. Econ. Hum. Biol. 41, 100953 (2021).
Mathur, R., Bear, L., Khunti, K. & Eggo, R. M. Urgent actions and policies needed to address COVID-19 among UK ethnic minorities. Lancet 396, 1866–1868 (2020).
Eshareturi, C., Wareham, A., Rattray, M., Haith-Cooper, M. & McCarthy, R. An exploration of the impact of SARS-CoV-2 (COVID-19) restrictions on marginalised groups in the UK. Public Health 197, 6–10 (2021).
Priyadarshini, S. & Swain, S. C. Impact of covid-19 on the socioeconomic life and psychology of transgenders: Insights from india. Int. J. Res. Pharm. Sci. 11, 126–132 (2020).
Acknowledgements
This research is supported by Ministry of Education Singapore AcRF Tier 1 funding support through NUS ODPRT Reimagine Grant and the Lee Kuan Yew School of Public Policy, National University of Singapore with grant numbers A-0003291-01-00 (A.T.) and A-0003291-00-00 (A.T.). A.T. is grateful for the support provided by the NUS ODPRT Reimagine Research grant scheme and encouragements of Prof CHEN Tsuhan.
Author information
Authors and Affiliations
Contributions
Conceptualisation, A.T.; methodology, A.T. and S.-Y.T.; validation, A.T.; formal analysis, L.L., A.T. and S.-Y.T.; investigation, L.L., A.T. and S.-Y.T.; resources, A.T.; data curation: L.L. and S.-Y.T.; writing and editing L.L., A.T. and S.-Y.T.; supervision, A.T.; project administration, A.T.; funding acquisition, A.T. All authors read and agreed to the published version of the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Peer review
Peer review information
Nature Communications thanks Eran Bendavid, Giuliano Russo and the other, anonymous, reviewer(s) for their contribution to the peer review of this work. Peer reviewer reports are available.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Li, L., Taeihagh, A. & Tan, S.Y. A scoping review of the impacts of COVID-19 physical distancing measures on vulnerable population groups. Nat Commun 14, 599 (2023). https://doi.org/10.1038/s41467-023-36267-9
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41467-023-36267-9
This article is cited by
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.