Abstract
Objective
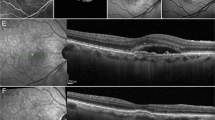
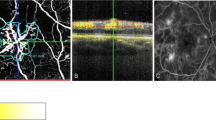
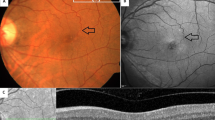
To evaluate the sensitivity and specificity of structural optical coherence tomography (OCT) in comparison to fluorescein angiography (FA) and OCT angiography (OCTA) in discerning between macular haemorrhages (MH) due to myopic choroidal neovascularization (m-CNV) and idiopathic macular haemorrhage (IMH) in myopic patients and to suggest a new OCT biomarker to discern these two entities.
Methods and analysis
In this longitudinal retrospective study, patients affected by MH and pathological myopia were included. All patients underwent OCTA and FA to discern bleeding from m-CNV or IMH. Furthermore, all patients underwent a structural OCT and 2 expert graders evaluated the presence of the myopic 2 binary reflective sign as a biomarker to discern between IMH and bleeding from m-CNV.
Results
Forty-seven eyes of 47 patients were enrolled. By means of angiographic examinations, 34 out of 47 eyes with MH (57%) were diagnosed as m-CNV, whereas 13 eyes (43%) as IMH. Using structural OCT, the graders identified the presence of the myopic 2 binary reflective sign in 13 out of 13 eyes with IMH. In 33 out of 34 cases with m-CNV, the 2 graders established the absence of the sign. This accounted for 100% of sensibility and 97% of specificity of structural OCT in discerning between MH from m-CNV and IMH.
Conclusion
Structural OCT can discern with good reliability between IMH and bleeding from m-CNV based on the presence/ absence of the myopic 2 binary reflective sign. This could be of paramount relevance in the clinical setting for the diagnosis and treatment of HM patients.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 18 print issues and online access
$259.00 per year
only $14.39 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
Data availability
The datasets generated and/or analysed during the current study, which were used for all statistical analyses and for the creation of all figures, as well as the Table 1, are available from the corresponding author upon reasonable request.
References
Ruiz-Medrano J, Montero JA, Flores-Moreno I, Arias L, García-Layana A, Ruiz-Moreno JM. Myopic maculopathy: current status and proposal for a new classification and grading system (ATN). Prog Retin Eye Res. 2019;69:80–115. https://doi.org/10.1016/J.PRETEYERES.2018.10.005
Corbelli E, Parravano M, Sacconi R, Sarraf D, Yu SY, Kim K, et al. Prevalence and phenotypes of age-related macular degeneration in eyes with high myopia. Invest Ophthalmol Vis Sci. 2019;60:1394–402. https://doi.org/10.1167/IOVS.18-25534
Neelam K, Cheung CMG, Ohno-Matsui K, Lai TYY, Wong TY. Choroidal neovascularization in pathological myopia. Prog Retin Eye Res. 2012;31:495–525. https://doi.org/10.1016/J.PRETEYERES.2012.04.001
Kumar A, Chawla R, Kumawat D, Pillay G. Insight into high myopia and the macula. Indian J Ophthalmol. 2017;65:85–91. https://doi.org/10.4103/IJO.IJO_863_16
Ohno-Matsui K, Ikuno Y, Lai TYY, Gemmy Cheung CM. Diagnosis and treatment guideline for myopic choroidal neovascularization due to pathologic myopia. Prog Retin Eye Res. 2018;63:92–106. https://doi.org/10.1016/J.PRETEYERES.2017.10.005
Ohno-Matsui K, Yoshida T, Futagami S, Yasuzumi K, Shimada N, Kojima A, et al. Patchy atrophy and lacquer cracks predispose to the development of choroidal neovascularisation in pathological myopia. Br J Ophthalmol. 2003;87:570–3. https://doi.org/10.1136/BJO.87.5.570
Hayashi K, Ohno-Matsui K, Shimada N, Moriyama M, Kojima A, Hayashi W, et al. Long-term pattern of progression of myopic maculopathy: a natural history study. Ophthalmology (2010);117. https://doi.org/10.1016/J.OPHTHA.2009.11.003
Wong TY, Ohno-Matsui K, Leveziel N, Holz FG, Lai TY, Yu HG, et al. Myopic choroidal neovascularisation: current concepts and update on clinical management. Br J Ophthalmol. 2015;99:289–96. https://doi.org/10.1136/BJOPHTHALMOL-2014-305131
Borrelli E, Battista M, Vella G, Sacconi R, Querques L, Grosso D, et al. Three-year OCT predictive factors of disease recurrence in eyes with successfully treated myopic choroidal neovascularisation. Br J Ophthalmol. 2022;106:1132–8. https://doi.org/10.1136/BJOPHTHALMOL-2020-318440
Parodi MB, Iacono P, Sacconi R, Iuliano L, Bandello F. Fundus autofluorescence changes after ranibizumab treatment for subfoveal choroidal neovascularization secondary to pathologic myopia. Am J Ophthalmol. 2015;160:322–27.e2. https://doi.org/10.1016/J.AJO.2015.04.030
Querques G, Corvi F, Balaratnasingam C, Casalino G, Parodi MB, Introini U, et al. Lacquer cracks and perforating scleral vessels in pathologic myopia: a possible causal relationship. Am J Ophthalmol. 2015;160:759–66.e2. https://doi.org/10.1016/J.AJO.2015.07.017
Ohno-Matsui K, Ito M, Tokoro T. Subretinal bleeding without choroidal neovascularization in pathologic myopia. A sign of new lacquer crack formation. Retina. 1996;16:196–202. https://doi.org/10.1097/00006982-199616030-00003
Ren P, Lu L, Tang X, Lu H, Zhao Y, Lou D, et al. Clinical features of simple hemorrhage and myopic choroidal neovascularization associated with lacquer cracks in pathologic myopia. Graefes Arch Clin Exp Ophthalmol. 2020;258:2661–9. https://doi.org/10.1007/S00417-020-04778-6
Curtin BJ. Pathologic myopia. Acta Ophthalmol Suppl (Oxf). 1988;185:105–6. https://doi.org/10.1111/J.1755-3768.1988.TB02680.X
Battista M, Sacconi R, Borrelli E, Crepaldi A, Fantaguzzi F, Costanzo E, et al. Discerning between macular hemorrhages due to macular neovascularization or due to spontaneous bruch’s membrane rupture in high myopia: a comparative analysis between OCTA and fluorescein angiography. Ophthalmol Ther. 2022;11:821–31. https://doi.org/10.1007/S40123-022-00484-0
Spaide RF, Fujimoto JG, Waheed NK, Sadda SR, Staurenghi G. Optical coherence tomography angiography. Prog Retin Eye Res. 2018;64:1–55. https://doi.org/10.1016/j.preteyeres.2017.11.003
Senn S. Review of Fleiss, statistical methods for rates and proportions. Res Synth Methods. 2011;2:221–2. https://doi.org/10.1002/JRSM.50
Ohno-Matsui K, Lai TYY, Lai CC, Cheung CMG. Updates of pathologic myopia. Prog Retin Eye Res. 2016;52:156–87. https://doi.org/10.1016/J.PRETEYERES.2015.12.001
Yannuzzi LA, Rohrer KT, Tindel LJ, Sobel RS, Costanza MA, Shields et al. Fluorescein angiography complication survey. Ophthalmology. 1986;93:611–7. https://doi.org/10.1016/s0161-6420(86)33697-2
Laíns I, Wang JC, Cui Y, Katz R, Vingopoulos F, Staurenghi G, et al. Retinal applications of swept source optical coherence tomography (OCT) and optical coherence tomography angiography (OCTA). Prog Retin Eye Res (2021);84. https://doi.org/10.1016/J.PRETEYERES.2021.100951
Sacconi R, Forte P, Tombolini B, Grosso D, Fantaguzzi F, Pina A, et al. OCT predictors of 3-year visual outcome for Type 3 macular neovascularization. Ophthalmol Retin. 2022;6:586–94. https://doi.org/10.1016/J.ORET.2022.02.010
Marchese A, Carnevali A, Sacconi R, Centoducati T, Querques L, Bandello F, et al. Retinal pigment epithelium humps in high myopia. Am J Ophthalmol. 2017;182:56–61. https://doi.org/10.1016/J.AJO.2017.07.013
Asai T, Ikuno Y, Nishida K. Macular microstructures and prognostic factors in myopic subretinal hemorrhages. Invest Ophthalmol Vis Sci. 2014;55:226–32. https://doi.org/10.1167/IOVS.13-12658
Querques L, Giuffrè C, Corvi F, Zucchiatti I, Carnevali A, de Vitis LA, et al. Optical coherence tomography angiography of myopic choroidal neovascularisation. Br J Ophthalmol. 2017;101:609–15. https://doi.org/10.1136/BJOPHTHALMOL-2016-309162
Author information
Authors and Affiliations
Contributions
Conception or design of the work: GQ, FB, RS, MB. Acquisition, analysis, or interpretation of data: RS, MB, CM, AS, AC. Drafted the work or substantively revised it: GQ, FB, RS, LQ, EC, CM, AS, MB, AC.
Corresponding author
Ethics declarations
Competing interests
RS is consultant for Allergan Inc, Bayer Shering-Pharma, Medivis, Novartis, and Zeiss. FB is consultant for Alcon, Alimera Sciences, Allergan Inc, Farmila-Thea, Bayer Shering-Pharma, Baush and Lomb, Genentech, Hoffmann-La-Roche, Novagali Pharma, Novartis, Sanofi-Aventis, Thrombogenics, and Zeiss. GQ is consultant for Alimera Sciences, Allergan Inc, Amgen, Bayer Shering-Pharma, Heidelberg, KBH, LEH Pharma, Lumithera, Novartis, Sandoz, Sifi, Sooft-Fidea, and Zeiss. The authors have no other relevant affiliations or financial involvement with any organization or entity with a financial interest in or financial conflict with the subject matter or materials discussed in the manuscript apart from those disclosed.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Mularoni, C., Servillo, A., Sacconi, R. et al. ‘Structural OCT changes distinguishing between myopic macular haemorrhages due to choroidal neovascularization and spontaneous Bruch’s membrane rupture: the “myopic 2 binary reflective sign”. Eye 38, 792–797 (2024). https://doi.org/10.1038/s41433-023-02780-w
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41433-023-02780-w
This article is cited by
-
Differential diagnosis of myopic choroidal neovascularization (mCNV): insights from multimodal imaging and treatment implications
Graefe's Archive for Clinical and Experimental Ophthalmology (2023)