Abstract
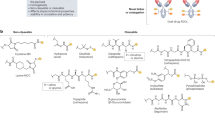
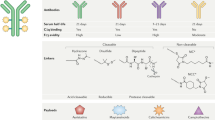
Antibody-Drug Conjugates (ADCs) represent a rapidly advancing category of oncology therapeutics, spanning the targeted therapy for both hematologic malignancies and solid cancers. A crucial aspect of ADC research involves the identification of optimal surface antigens that can effectively differentiate target cells from most mammalian cell types. Herein, we have devised an algorithm and compiled an extensive dataset annotating cell membrane proteins. This dataset is derived from comprehensive transcriptomic, proteomic, and genomic data encompassing 19 types of solid cancer as well as normal tissues. The aim is to uncover potential therapeutic surface antigens for precise ADC targeting. The resulting target landscape comprises 165 combinations of targets and indications, along with 75 candidates of cell surface proteins. Notably, 35 of these candidates possess characteristics suitable for ADC targeting, and have not been previously reported in ADC research and development. Additionally, we have identified a total of 159 ADCs from a pool of 760 clinical trials. Of these, 72 ADCs are presently undergoing interventional evaluation for a variety of solid cancer types, targeting 36 unique antigens. We conducted an analysis of their expression in normal tissues using this comprehensive annotation dataset, revealing a diverse range of profiles for the current ADC targets. Moreover, we emphasize that the biological impacts of target antigens have the potential to enhance their clinical effectiveness. We propose a comprehensive assessment of the drugability of target antigens, considering multiple facets. This study represents a thorough exploration of pan-cancer ADC targets over the past two decades, underscoring the potential of a comprehensive solid cancer target atlas to broaden the scope of ADC therapies.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
Data availability
The datasets generated during and/or analysed during the current study are available from the corresponding author on reasonable request.
Code availability
The custom computer codes utilized during the current study are available from the corresponding author upon reasonable request.
References
WHO. World cancer report. France: Imprimerie Faurite; 2020.
Davis C, Naci H, Gurpinar E, Poplavska E, Pinto A, Aggarwal A. Availability of evidence of benefits on overall survival and quality of life of cancer drugs approved by European Medicines Agency: Retrospective cohort study of drug approvals 2009-13. BMJ. 2017;359:j4530.
Beck A, Goetsch L, Dumontet C, Corvaïa N. Strategies and challenges for the next generation of antibody-drug conjugates. Nat Rev Drug Discov. 2017;16:315–37.
Chau CH, Steeg PS, Figg WD. Antibody–drug conjugates for cancer. Lancet. 2019;394:793–804.
Modi S, Saura C, Yamashita T, Park YH, Kim SB, Tamura K, et al. Trastuzumab Deruxtecan in Previously Treated HER2-Positive Breast Cancer. N. Engl J Med. 2020;382:610–21.
Lyon R. Drawing lessons from the clinical development of antibody-drug conjugates. Drug Discov Today Technol 2018;30:105–9.
Van Geel R, Wijdeven MA, Heesbeen R, Verkade JMM, Wasiel AA, Van Berkel SS, et al. Chemoenzymatic conjugation of toxic payloads to the globally conserved N-glycan of native mabs provides homogeneous and highly efficacious antibody-drug conjugates. Bioconjug Chem. 2015;26:2233–42.
Junutula JR, Raab H, Clark S, Bhakta S, Leipold DD, Weir S, et al. Site-specific conjugation of a cytotoxic drug to an antibody improves the therapeutic index. Nat Biotechnol. 2008;26:925–32.
Panowski S, Bhakta S, Raab H, Polakis P, Junutula JR. Site-specific antibody drug conjugates for cancer therapy. MAbs. 2014;6:34–45.
Strop P, Delaria K, Foletti D, Witt JM, Hasa-Moreno A, Poulsen K, et al. Site-specific conjugation improves therapeutic index of antibody drug conjugates with high drug loading. Nat Biotechnol. 2015;33:694–6.
Axup JY, Bajjuri KM, Ritland M, Hutchins BM, Kim CH, Kazane SA, et al. Synthesis of site-specific antibody-drug conjugates using unnatural amino acids. Proc Natl Acad Sci USA. 2012;109:16101–6.
Tsuchikama K, An Z. Antibody-drug conjugates: recent advances in conjugation and linker chemistries. Protein Cell. 2018;9:33–46.
Donaghy H. Effects of antibody, drug and linker on the preclinical and clinical toxicities of antibody-drug conjugates. MAbs. 2016;8:659–71.
Anami Y, Yamazaki CM, Xiong W, Gui X, Zhang N, An Z, et al. Glutamic acid-valine-citrulline linkers ensure stability and efficacy of antibody-drug conjugates in mice. Nat Commun. 2018;9:2512.
Devay RM, Delaria K, Zhu G, Holz C, Foletti D, Sutton J, et al. Improved Lysosomal Trafficking Can Modulate the Potency of Antibody Drug Conjugates. Bioconjug Chem. 2017;28:1102–14.
De Goeij BECG, Vink T, Ten Napel H, Breij ECW, Satijn D, Wubbolts R, et al. Efficient payload delivery by a bispecific antibody-drug conjugate targeting HER2 and CD63. Mol Cancer Ther. 2016;15:2688–97.
Tolcher AW. Antibody drug conjugates: lessons from 20 years of clinical experience. Ann Oncol. 2016;27:2168–72.
Saleh MN, Sugarman S, Murray J, Ostroff JB, Healey D, Jones D, et al. Phase I trial of the anti-Lewis Y drug immunoconjugate BR96-doxorubicin in patients with Lewis Y-expressing epithelial tumors. J Clin Oncol. 2000;18:2282–92.
Tijink BM, Buter J, De Bree R, Giaccone G, Lang MS, Staab A, et al. A phase I dose escalation study with anti-CD44v6 bivatuzumab mertansine in patients with incurable squamous cell carcinoma of the head and neck or esophagus. Clin Cancer Res. 2006;12:6064–72.
Damelin M, Zhong W, Myers J, Sapra P. Evolving Strategies for Target Selection for Antibody-Drug Conjugates. Pharm Res. 2015;32:3494–507.
Perna F, Berman SH, Soni RK, Mansilla-Soto J, Eyquem J, Hamieh M, et al. Integrating Proteomics and Transcriptomics for Systematic Combinatorial Chimeric Antigen Receptor Therapy of AML. Cancer Cell. 2017;32:506–19.
Love MI, Huber W, Anders S. Moderated estimation of fold change and dispersion for RNA-seq data with DESeq2. Genome Biol. 2014;15:550.
Hu Y, Yan C, Hsu CH, Chen QR, Niu K, Komatsoulis GA, et al. Omiccircos: A simple-to-use R package for the circular visualization of multidimensional Omics data. Cancer Inf. 2014;13:13.
Fehrmann RSN, Karjalainen JM, Krajewska M, Westra HJ, Maloney D, Simeonov A, et al. Gene expression analysis identifies global gene dosage sensitivity in cancer. Nat Genet. 2015;47:115–25.
Hänzelmann S, Castelo R, Guinney J. GSVA: Gene set variation analysis for microarray and RNA-Seq data. BMC Bioinforma. 2013;14:7.
Arora S, Pattwell SS, Holland EC, Bolouri H. Variability in estimated gene expression among commonly used RNA-seq pipelines. Sci Rep. 2020;10:2734.
Wang Q, Armenia J, Zhang C, Penson AV, Reznik E, Zhang L, et al. Data Descriptor: Unifying cancer and normal RNA sequencing data from different sources. Sci Data. 2018;5:180061.
Bagger FO, Kinalis S, Rapin N. BloodSpot: A database of healthy and malignant haematopoiesis updated with purified and single cell mRNA sequencing profiles. Nucleic Acids Res. 2019;47:881–5.
Uhlen M, Zhang C, Lee S, Sjöstedt E, Fagerberg L, Bidkhori G, et al. A pathology atlas of the human cancer transcriptome. Science. 2017;357:eaan2507.
Sweeney SM, Cerami E, Baras A, Pugh TJ, Schultz N, Stricker T, et al. AACR project genie: Powering precision medicine through an international consortium. Cancer Discov. 2017;7:818–31.
Junttila TT, Li G, Parsons K, Phillips GL, Sliwkowski MX. Trastuzumab-DM1 (T-DM1) retains all the mechanisms of action of trastuzumab and efficiently inhibits growth of lapatinib insensitive breast cancer. Breast Cancer Res Treat. 2011;128:347–56.
Smit EF, Nakagawa K, Nagasaka M, Felip E, Goto Y, Li BT, et al. Trastuzumab deruxtecan (T-DXd; DS-8201) in patients with HER2-mutated metastatic non-small cell lung cancer (NSCLC): Interim results of DESTINY-Lung01. J Clin Oncol. 2020;38:9504.
Staudacher AH, Brown MP. Antibody drug conjugates and bystander killing: is antigen-dependent internalisation required. Br J Cancer. 2017;117:1736–42.
Perrino E, Steiner M, Krall N, Bernardes GJL, Pretto F, Casi G, et al. Curative properties of noninternalizing antibody-drug conjugates based on maytansinoids. Cancer Res. 2014;74:2569–78.
Gébleux R, Stringhini M, Casanova R, Soltermann A, Neri D. Non-internalizing antibody–drug conjugates display potent anti-cancer activity upon proteolytic release of monomethyl auristatin E in the subendothelial extracellular matrix. Int J Cancer. 2017;140:1670–9.
Giansanti F, Capone E, Ponziani S, Piccolo E, Gentile R, Lamolinara A, et al. Secreted Gal-3BP is a novel promising target for non-internalizing Antibody–Drug Conjugates. J Control Release. 2019;294:176–84.
Acknowledgements
The authors would like to acknowledge the American Association for Cancer Research and its financial and material support in the development of the AACR Project GENIE registry, as well as members of the consortium for their commitment to data sharing. Interpretations are the responsibility of study authors. The authors thank Dr. Simon Wang at the Language Centre, HKBU, for help with an improvement to the linguistic presentations of the manuscript.
Author information
Authors and Affiliations
Contributions
JF: conceptualization, investigation, methodology, data curation, data visualization, writing—original draft, writing—review and editing; LG: supervision, project administration, funding acquisition; YZ: investigation, methodology, software; QG: data curation, software; MW, XW: supervision, methodology, project administration.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Fang, J., Guo, L., Zhang, Y. et al. The target atlas for antibody-drug conjugates across solid cancers. Cancer Gene Ther 31, 273–284 (2024). https://doi.org/10.1038/s41417-023-00701-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41417-023-00701-3