Abstract
Background
To assess whether prior interventional treatment for benign prostatic hyperplasia (BPH) influences oncologic or functional outcomes following primary whole-gland prostate cryoablation.
Methods
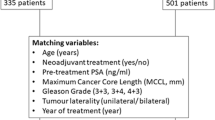
Among 3831 men with prostate cancer who underwent primary whole-gland prostate cryoablation, we identified 160 with a history of prior BPH interventional therapy including transurethral needle ablation (n = 6), transurethral microwave thermotherapy (n = 9), or transurethral resection of the prostate (n = 145). Patients with a history of medically treated or unspecified BPH therapy were excluded from the study. Oncological and functional outcomes were compared between men with and without prior BPH interventional therapy.
Results
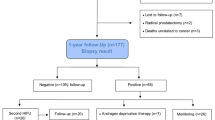
In unadjusted analyses, prior interventional BPH therapy was associated with higher risks of postoperative urinary retention (17.5% vs. 9.6%, p = 0.001) and new-onset urinary incontinence (39.9% vs. 19.4%, p > 0.001) compared with no prior therapy. Interventional BPH therapy was not correlated with the risk of developing a rectourethral fistula (p = 0.84) or new-onset erectile dysfunction (ED) at 12 months (p = 0.08) following surgery. On multivariable regression, prior interventional BPH therapy was associated with increased risk of urinary retention (OR 1.9, 95%, p = 0.015) and new-onset urinary incontinence (OR 2.13, p < 0.001). The estimated 5 years Kaplan–Meier survival analysis showed no statistically significant difference (p = 0.3) in biochemical progression free survival between those who underwent interventional BPH therapy compared with those who did not. Local disease recurrence assessed by post cryoablation positive for-cause prostate biopsy showed no significant difference between the two groups (25.4% vs. 28.7%, p = 0.59).
Conclusions
Prior interventional BPH therapy did not affect the oncologic outcomes nor did it increase the risk of rectourethral fistula or ED in sexually performing patients prior to cryosurgery. Prior interventional BPH therapy was associated with increased risk of urinary retention and incontinence after primary whole-gland prostate cryoablation for prostate cancer.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 4 print issues and online access
$259.00 per year
only $64.75 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Chang RT, Kirby R, Challacombe BJ. Is there a link between BPH and prostate cancer? Practitioner. 2012;256:13–2.
Vuichoud C, Loughlin KR. Benign prostatic hyperplasia: epidemiology, economics and evaluation. Can J Urol. 2015;22:1–6.
Bashir MN. Epidemiology of prostate cancer. Asian Pac J Cancer Prev. 2015;16:5137–41.
Sanda MG, Cadeddu JA, Kirkby E, Chen RC, Crispino T, Fontanarosa J, et al. Clinically localized prostate cancer: AUA/ASTRO/SUO Guideline. Part II: recommended approaches and details of specific care options. J Urol. 2018;199:990–7.
Biers S, Sievert KD, Thiruchelvam N. Overactive bladder syndrome and lower urinary tract symptoms after prostate cancer treatment. Curr Opin Urol. 2017;27:307–13.
Ishiyama H, Hirayama T, Jhaveri P, Satoh T, Paulino AC, Xu B, et al. Is there an increase in genitourinary toxicity in patients treated with transurethral resection of the prostate and radiotherapy? A systematic review. Am J Clin Oncol. 2014;37:297–304.
Cozzarini C, Rancati T, Palorini F, Avuzzi B, Garibaldi E, Balestrini D, et al. Patient-reported urinary incontinence after radiotherapy for prostate cancer: quantifying the dose-effect. Radiother Oncol. 2017;125:101–6.
Lodeizen O, de Bruin M, Eggener S, Crouzet S, Ghai S, Varkarakis I, et al. Ablation energies for focal treatment of prostate cancer. World J Urol. 2019;37:409–18.
Roberts CB, Jang TL, Shao YH, Kabadi S, Moore DF, Lu-Yao GL. Treatment profile and complications associated with cryotherapy for localized prostate cancer: a population-based study. Prostate Cancer Prostatic Dis. 2011;14:313–9.
Shinohara K, Connolly JA, Presti JC Jr, Carroll PR. Cryosurgical treatment of localized prostate cancer (stages T1 to T4): preliminary results. J Urol. 1996;156:115–21.
Temml C, Haidinger G, Schmidbauer J, Schatzl G, Madersbacher S. Urinary incontinence in both sexes: prevalence rates and impact on quality of life and sexual life. Neurourol Urodyn. 2000;19:259–71.
Stephenson AJ, Kattan MW, Eastham JA, Bianco FJ Jr, Yossepowitch O, Vickers AJ, et al. Prostate cancer-specific mortality after radical prostatectomy for patients treated in the prostate-specific antigen era. J Clin Oncol. 2009;27:4300–5.
Colombo R, Naspro R, Salonia A, Montorsi F, Raber M, Suardi N, et al. Radical prostatectomy after previous prostate surgery: clinical and functional outcomes. J Urol. 2006;176:2459–63.
Teber D, Cresswell J, Ates M, Erdogru T, Hruza M, Gözen AS, et al. Laparoscopic radical prostatectomy in clinical T1a and T1b prostate cancer: oncologic and functional outcomes-a matched-pair analysis. Urology. 2009;73:577–81.
Devisetty K, Zorn KC, Katz MH, Jani AB, Liauw SL. External beam radiation therapy after transurethral resection of the prostate: a report on acute and late genitourinary toxicity. Int J Radiat Oncol Biol Phys. 2010;77:1060–5.
Nag S, Beyer D, Friedland J, Grimm P, Nath R. American Brachytherapy Society (ABS) recommendations for transperineal permanent brachytherapy of prostate cancer. Int J Radiat Oncol Biol Phys. 1999;44:789–99.
Moran BJ, Stutz MA, Gurel MH. Prostate brachytherapy can be performed in selected patients after transurethral resection of the prostate. Int J Radiat Oncol Biol Phys. 2004;59:392–6.
Stone NN, Ratnow ER, Stock RG. Prior transurethral resection does not increase morbidity following real-time ultrasound-guided prostate seed implantation. Tech Urol. 2000;6:123–7.
Brousil P, Hussain M, Lynch M, Laing RW, Langley SE. Modified transurethral resection of the prostate (TURP) for men with moderate lower urinary tract symptoms (LUTS) before brachytherapy is safe and feasible. BJU Int. 2015;115:580–6.
Babaian RJ, Donnelly B, Bahn D, Baust JG, Dineen M, Ellis D, et al. Best practice statement on cryosurgery for the treatment of localized prostate cancer. J Urol. 2008;180:1993–2004.
Ullal AV, Korets R, Katz AE, Wenske S. A report on major complications and biochemical recurrence after primary and salvage cryosurgery for prostate cancer in patients with prior resection for benign prostatic hyperplasia: a single-center experience. Urology. 2013;82:648–52.
Xu N, Chen SH, Xue XY, Wei Y, Zheng Q-S, Li X-D, et al. Older age and larger prostate volume are associated with stress urinary incontinence after plasmakinetic enucleation of the prostate. Biomed Res Int. 2017;2017:6923290.
Grossgold E, Given R, Ruckle H, Jones JS. Does neoadjuvant androgen deprivation therapy before primary whole gland cryoablation of the prostate affect the outcome? Urology. 2014;83:379–83.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
ElShafei, A., DeWitt-Foy, M., Calaway, A. et al. Does prior surgical interventional therapy for BPH affect the oncological or functional outcomes after primary whole-gland prostate cryoablation for localized prostate cancer?. Prostate Cancer Prostatic Dis 24, 507–513 (2021). https://doi.org/10.1038/s41391-020-00306-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41391-020-00306-z