Abstract
Continuous cardiorespiratory physiological monitoring is a cornerstone of care in hospitalized children. The data generated by monitoring devices coupled with machine learning could transform the way we provide care. This scoping review summarizes existing evidence on novel approaches to continuous cardiorespiratory monitoring in hospitalized children. We aimed to identify opportunities for the development of monitoring technology and the use of machine learning to analyze continuous physiological data to improve the outcomes of hospitalized children. We included original research articles published on or after January 1, 2001, involving novel approaches to collect and use continuous cardiorespiratory physiological data in hospitalized children. OVID Medline, PubMed, and Embase databases were searched. We screened 2909 articles and performed full-text extraction of 105 articles. We identified 58 articles describing novel devices or approaches, which were generally small and single-center. In addition, we identified 47 articles that described the use of continuous physiological data in prediction models, but only 7 integrated multidimensional data (e.g., demographics, laboratory results). We identified three areas for development: (1) further validation of promising novel devices; (2) more studies of models integrating multidimensional data with continuous cardiorespiratory data; and (3) further dissemination, implementation, and validation of prediction models using continuous cardiorespiratory data.
Impact
-
We performed a comprehensive scoping review of novel approaches to capture and use continuous cardiorespiratory physiological data for monitoring, diagnosis, providing care, and predicting events in hospitalized infants and children, from novel devices to machine learning-based prediction models.
-
We identified three key areas for future development: (1) further validation of promising novel devices; (2) more studies of models integrating multidimensional data with continuous cardiorespiratory data; and (3) further dissemination, implementation, and validation of prediction models using cardiorespiratory data.
Similar content being viewed by others
Introduction
Continuous cardiorespiratory monitoring using bedside devices and sensor-based technology is pervasive in modern healthcare and a cornerstone of care in hospitalized children. Though in widespread use, the current state-of-the-art bedside monitoring would benefit from novel wireless, noninvasive, and non-contact sensing methods that could protect fragile skin, reduce interference in care, and promote caregiver-child interactions.1,2 In addition, the wealth of data generated by these devices needs to be saved and utilized in prediction models or clinical decision support tools, rather than automatically deleted from vendor servers soon after patient discharge. Preliminary data indicate that these continuous physiological cardiorespiratory data coupled with machine learning techniques could fundamentally transform the way we provide care.3 Machine learning models using continuous physiological data in children already show promise in early identification of sepsis,4,5,6,7,8,9,10 cardiac arrest,11,12 and risk of readmission.13 As we look to the future of continuous cardiorespiratory monitoring, we must improve monitoring technology, identify those patients who would benefit from beat-to-beat and breath-to-breath bedside monitoring data, and find new ways to use these data to improve the care and outcomes of hospitalized children.
In this scoping review, we summarize existing evidence on (1) the use of novel approaches to capture continuous cardiorespiratory physiological data in hospitalized children in order to identify key opportunities for the development of continuous cardiorespiratory monitoring technology; and (2) the use of machine learning to analyze continuous cardiorespiratory physiological data to improve the care of hospitalized children.
Methods
We conducted a scoping review of original research articles published on or after January 1, 2001, involving novel approaches to the capture and use of continuous cardiovascular and/or respiratory data in hospitalized neonates, children, and adolescents. “Novel” devices were defined as those not currently part of the standard of care. “Continuous” devices were those which acquired data in an automated way at a frequency of greater than one sample per minute for a duration of at least 5 min. “Physiological” data were defined as an observed variable measuring functioning of the human body. We excluded studies focused on: continuous biochemical information (e.g., glucose), intermittently collected imaging devices (e.g., ultrasound), alarm fatigue, drug monitoring, measurement accuracy in previously validated devices, and normal reference range definitions.
OVID Medline, PubMed, and Embase databases were searched. Abstract and full-text screening was completed in Covidence (Veritas Health Innovation Ltd, Melbourne, Australia) by six investigators (S.B.W., M.S.C., K.S.H., C.M.B., D.E.W.-M., L.N.S.-P.), with two reviewers required per article. Further details can be found in the Supplementary materials.
Results
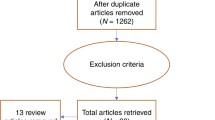
We screened 2909 articles and performed full-text extraction of 105: 58 describing novel continuous cardiorespiratory monitoring devices or measurement approaches and 47 describing prediction or inference models using continuous cardiorespiratory physiological data (Fig. 1).
Studies describing novel devices or measurement approaches were primarily small (<50 patients), single-center, observational trials or proof-of-concept studies in an intensive care unit (ICU) setting (Table 1 and Supplementary Tables 1 and 2). Articles describing prediction or inference models using continuous cardiorespiratory physiological data mostly involved a single physiological variable (31 of 47) and the majority of these studied heart rate variability (14 of 31). Sample size for these studies varied widely (<10 to >7000 patients). All studies took place at least partially in the ICU and only three were randomized control trials (Table 2 and Supplementary Tables 3 and 4).
Novel devices or measurement approaches to cardiovascular monitoring
Blood pressure (BP)
Six articles described novel methods to measure BP in hospitalized children. These aimed to provide data that are continuous, noninvasive, and usable to reconstruct features of arterial line waveforms (e.g., pulse pressure variation). All were prospective observational trials of 10–35 patients, all but one in pediatric ICU (PICU) patients, and all were compared to gold standard invasive arterial line measurements (Table 1 and Supplementary Table 1). Three articles described different proprietary noninvasive BP cuffs that are attached to fingers.14,15,16 Finger BP cuff use was feasible and well tolerated but noted erroneous values due to placement. None were specifically tested in hemodynamically unstable children. One method of BP prediction based on heart sounds resulted in predictions with high standard deviation.17 The most recent article described a noninvasive wireless skin interface sensor that had a good correlation with invasive arterial BP including after pharmacologic interventions known to cause hemodynamic change.18 Finally, a study comparing pulse oximeter waveforms to invasive arterial line waveforms in mechanically ventilated patients found a good correlation with waveform features.19
Heart rate (HR)
Novel methods to measure HR in hospitalized children are mostly neonatal ICU (NICU) based. These alternative methods were developed to: (1) avoid adhesive-based sensors to capture ECG data, which can be obtrusive and potentially harmful to the skin of neonates1 and (2) reduce motion artifacts that can affect sensor accuracy.20 Most of the 14 articles identified are small proof-of-concept or prospective observational cohorts of less than 80 patients (Table 1 and Supplementary Table 1). Five studies presented results of the use of cameras to detect HR, in some cases using machine learning techniques to identify and suppress artifacts.21,22,23,24,25 The correlation with standard measurements was generally good, although problems with artifacts were common, particularly during hands-on care. Two articles presented results of HR measurements based on the detection of chest movement, one using a radar signal26 and the other using laser Doppler.26,27 Two studies presented results from sensors embedded in the blankets or mattress of neonates: a capacitive sensor1 and a piezoelectric sensor.28
Four articles presented results of novel methods to reduce artifacts in HR captured in neonates, including forehead reflectance photoplethysmography,29 transesophageal measurement,30 transcutaneous diaphragm electromyography sensors,31 and spectrogram analysis of ECG data, instead of RR detection.32 While these approaches were generally successful at reducing artifacts, few considered implementation strategies that would make them feasible alternatives to traditional ECG.
Finally, one study compared methods for forecasting neonatal HR and found that an autoregressive moving average model could predict future HR values from historical values with reasonable accuracy.33
Heart rate variability (HRV)
HRV is defined as the fluctuation in time between consecutive heartbeats and may be altered when there is an imbalance in autonomic nervous system inputs to the heart.34 There are a variety of ways to look at these fluctuations, but most require complex waveform analysis.35 Many measures have shown promise in clinical prediction or inference models as described later, but none have been compared to other measurements of autonomic dysfunction (and thus are not included in Table 1). A simplified proxy of HRV using the standard deviation of HR, termed integer HRV (HRVi), has also shown promise in prediction models, although it has not been directly compared to traditional methods for deriving HRV. One article, however, did show that HRVi estimated using the pulse rate from photoplethysmography correlated well with HRVi calculated from ECG (Table 1 and Supplementary Table 1).36
Cardiac output (CO)
We found ten articles describing the estimation of CO using five different strategies (Table 1 and Supplementary Table 1). Four studies of <25 patients each studied the pulse index continuous cardiac output (PiCCO) device. PiCCO uses pulse contour analysis calibrated by thermodilution in order to estimate CO as well as ten additional proprietary measurements.37 The first article published showed poor agreement between markers of clinical assessment and measurements of hemodynamic status.38 However, it is unclear how much of this discrepancy results from variability in clinical assessment, as subsequent articles have shown estimates of PiCCO to have good agreement with thermodilution39 and transthoracic ultrasound measurements of cardiac index,40 as well as global perfusion.41
Two additional articles explored uncalibrated pulse contour analysis using the pressure recording analytical method (PRAM) with the Mostcare® device and compared it to transthoracic echocardiogram (TTE)42 or transpulmonary ultrasound dilution using COstatus®.43 PRAM had an excellent agreement with TTE measurements but lower agreement with COstatus® measurements. Given COstatus® has not been validated in hospitalized children, more studies are necessary to determine the usefulness of PRAM in this population.
Three articles described the use of two forms of bioimpedance to estimate CO. One study described the use of electrical cardiometry bioimpedance in two children with hypoplastic left heart syndrome, showing some correlation between estimated CO and clinical change.44 Two studies described the use of electrical velocimetry bioimpedance in critically ill children (pediatric, cardiac, and neonatal) using the AESCULON®.45,46 Generally, the AESCULON® had a good correlation with CO based on TTE but was associated with a large margin of error. Bioreactance, the most recently developed form of bioimpedance, has not been compared to a gold standard but has been used in a prediction model as described later.47
Finally, one article studied CO estimations using partial rebreathing of carbon dioxide measured via the noninvasive cardiac output (NICO) device (Novametrix Medical Systems Inc., Wallingford, CT) on hemodynamically stable, mechanically ventilated patients >15 kg and was found to have good agreement with TTE.48
Systemic vascular resistance (SVR)
No novel device or approach was specifically targeted toward measuring SVR alone; however, four of the five strategies used to measure CO also provide measurements of SVR (NICO cannot; AESCULON® requires a central venous pressure estimate). Despite the ability to measure SVR, measurements of SVR were only reported in three articles, all using thermodilution via the PiCCO device. These three articles found no association when comparing PiCCO-measured SVR to clinician assessment38 or markers of oxygen balance;41 but did demonstrate significantly higher SVR between low and normal-to-high cardiac index states.49 No article compared these novel SVR continuous measurements to a gold standard.
Perfusion
We found five articles describing the use of near-infrared spectroscopy (NIRS), a common noninvasive continuous monitoring device that estimates regional tissue saturation. In critically ill children, NIRS showed a good correlation with peripheral and central measurements of venous oxygenation saturation (SvO2),50 as well as weak but statistically significant correlations with BP.51 Among post-operative cardiac ICU (CICU) patients, NIRS demonstrated not only significant correlations with central SvO2 but also highly correlated with adverse events after Norwood procedure.52 NIRS has also been used as a proxy for intestinal perfusion in neonates at high risk for intestinal failure (Table 1 and Supplementary Table 1).53
Despite its promise in healthy newborn54 and adult populations,55 we did not find any articles comparing perfusion index, a measurement of the ratio of pulsatile flow to non-pulsatile flow derived from pulse oximeters, to a gold standard of perfusion. We did find one clinical prediction or inference model that will be described later.
Novel devices or measurement approaches to respiratory monitoring
Respiratory rate (RR)
Similar to novel methods for HR measurement previously discussed, the ten articles describing novel methods for RR detection come from the NICU and are focused on reducing artifacts (Table 1 and Supplementary Table 2). Seven studies presented data of simultaneous HR and RR detection using: chest wall movement detected via a radar signal26 or laser Doppler27 image analysis of video signal,21,23,25 piezoelectric sensor in the bedding of the crib,28 or leveraging transcutaneous diaphragm electromyography sensors.31 While the correlation with RR via airway flow or impedance was good, motion artifacts and implementation barriers limited the feasibility of these devices.
Two studies demonstrated the challenges of measuring RR in neonates when compared to adults, one using a fiber-optical monitoring device integrated into a nasal cannula56 and another using a video-based method.57 In both cases, the performance of the devices was suboptimal compared to adults.
Finally, a small proof-of-concept study in neonates studied the use of infrared thermography of the nares to detect changes in temperature related to breathing.58 While the results are promising, implementation would have to be validated in children with various respiratory devices and nasal pathology.
Oxygenation
Three articles described noninvasive tools to measure oxygenation. A large PICU study used machine learning approaches to demonstrate the potential use of noninvasive pulse oximetry and ECG-derived HR measurements to reliably estimate PaO2 and the oxygenation index.59 A NICU study examined continuous positive airway pressure for respiratory distress and demonstrated a correlation between a novel index, the saturation oxygen pressure index, and alveolar-arteriolar oxygen difference.60 Finally, a neonatal conjunctival pulse oximetry monitor was found to be effective, although it caused conjunctival edema in one neonate.61
Both oxygen saturation index and ratio of SpO2 to FiO2 are well studied, noninvasive ways to assess hypoxemia in children with acute lung injury.62 Although not considered novel for the purposes of this review, these methods could be transformed into continuous, noninvasive measures.
Carbon dioxide (CO2)
Twelve articles described technology to estimate CO2 measures, primarily in observational trials of <75 PICU patients. Several studies correlated PaCO2 to end-tidal CO2 (EtCO2), transcutaneous CO2, or novel microstream capnometer devices.63,64,65,66,67 Three articles focused on the use of continuous measures of CO2 during mechanical ventilation. One study used bedside monitor data and ventilator measurements to identify deviations from pre-defined “trend templates” and made suggestions for the management of ventilator settings.68 Another study demonstrated strong correlations between EtCO2 and PaCO2 in a range of dead space to tidal volume ratios with the EtCO2-PaCO2 difference increasing predictably with increasing dead space to tidal volume ratio.69 Two studies used capnography to measure dead space, finding success with a novel EtCO2 monitor (CO2SMO Plus!™),70 but not with conventional time-based capnography.71
Investigators also studied measures of CO2 for applications outside of mechanical ventilation. One study demonstrated noninvasive EtCO2 monitoring to be a reliable tool to monitor acidosis in diabetic ketoacidosis.72 Another study demonstrated that cerebral NIRS measurements were a useful indicator of hypercapnia, though with low sensitivity.73 Finally, during apnea testing for the determination of neurologic death, transcutaneous CO2 monitoring demonstrated high correlation, accuracy, and minimal bias when compared with PaCO2.74
Regional lung ventilation measurements
Measurement of regional lung ventilation using electrical impedance tomography has been studied in children for over two decades.75 Electrical impedance tomography is a radiation-free functional modality that allows for bedside imaging and real-time monitoring of lung expansion, particularly useful for PEEP titration with avoidance of overdistension and collapse.76 Electrical impedance tomography has proven useful in both PICU and NICU patients, but most validation studies have limited sample sizes.77 Further studies are needed to determine the usefulness and cost-effectiveness of this method.
Prediction and/or inference models using cardiorespiratory physiological data
Models using HRV as a single physiological variable
Fourteen articles used HRV as a single continuous variable physiological variable within a clinical prediction or inference model. HRV has been studied as a single variable to predict clinical deterioration across a range of pathologies, most extensively in sepsis (Table 2 and Supplementary Table 3).4,7,78,79,80,81 HRV has also been used to identify neonates at risk for bradycardia,82 predict the duration of respiratory support,83 trace recovery during noninvasive respiratory support,84 and correlate with adverse outcomes at a 15-month follow-up in neonates after hypoxic-ischemic encephalopathy.85 Continuous bedside display of trended HRV and other HR characteristics integrated into a single score (the HeRO score) was associated with mortality reduction in a randomized trial of low birth weight neonates,86 mostly driven by patients with late-onset sepsis,87 and is now available as a commercial device. Subsequent validation of this device has shown a limited ability to predict bloodstream infections.88 The simplified proxy of HRV (HRVi) has also shown promise in predicting new or worsening organ dysfunction in PICU13 and oncology ward patients.36
Models using other single physiological variables
Seventeen studies described a prediction or inference model using a single physiological variable other than HRV, mostly pertaining to cardiac function (Table 2 and Supplementary Table 3). Variation in stroke volume with breathing measured through bioreactance using the NICOM device predicted an increase in stroke volume after fluid administration better than central venous pressure, but less accurately than intermittent ultrasound measurement.47 CO estimations using PRAM were associated with the duration of mechanical ventilation, tissue perfusion, vasoactive and diuretic drug requirements in children post-cardiac surgery.89 In PICU patients with viral respiratory failure, management of fluid status through PiCCO was associated with fewer ventilator days, although without a significant change in length of stay.90 The compensatory reserve index, a machine learning-based measure that continuously compares the arterial line waveform to a store of “normal” arterial line waveforms in order to predict cardiac deterioration, was found to be feasible and safe, with early changes in the index associated with length of stay.91 A study of CICU patients found estimations of normal cardiac index via PiCCO to be associated with shorter duration of mechanical ventilation and length of stay.49 Finally, EtCO2 was studied as a proxy of CO and CPR quality during in-hospital cardiac arrest, but was not associated with the return of circulation or survival to hospital discharge.92
Five articles described perfusion as a clinical predictor. One case report described how splanchnic NIRS measurements precipitously dropped and remained low until the time of necrotizing enterocolitis diagnosis.93 Cardiac conditions affecting systemic perfusion have also been discovered through NIRS changes, including large pericardial effusion94 and hemodynamically significant patent ductus arteriosus.95 These observational studies and case reports suggest that NIRS can alert clinicians to underlying changes in central and peripheral SvO2 and oxygen extraction –in some cases as the first signal that the patient is beginning to deteriorate (Table 2 and Supplementary Table 3). Although this trend in small studies is encouraging, the quality of evidence is low, and NIRS would benefit from larger, multicenter, randomized control trials.96 In addition, perfusion index was investigated in a single study of PICU patients, where it showed high sensitivity and specificity in diagnosing shock as defined by tachycardia with poor peripheral perfusion, but poor ability to predict hypotension.97
Four studies investigated respiratory variables. The ventilatory ratio, a variable dependent on CO2, body weight, and minute ventilation, was compared to alveolar dead space fraction, and only alveolar dead space fraction was associated with mortality.98 Various measures of time-based capnography were associated with extubation success in infants.99 Another study created an age-dependent index of the pulse oximeter waveform to predict episodic clinical deterioration.100 The pulse oximeter-based index had a number of false positives equal to the number of events, but performed better than clinical prediction alone.100
Finally, a study of critically ill children investigated the use of noninvasive thermal imaging to detect and/or predict shock 0–12 h before onset, and was found to have fair performance in critically ill children.101
Models using multiple continuous physiological variables
Most studies of prediction or inference using multivariable models only included continuously collected physiological variables rather than a combination of continuously collected physiological variables with intermittently collected multidimensional variables (e.g., electronic health record (EHR) or demographic data).
Six articles presented models to predict cardiorespiratory deterioration or arrest. Four of these articles were in the CICU and presented models using commonly monitored cardiorespiratory variables combined with novel variables, including beat-to-beat ST segment morphology,11,102 HRV,12 and systemic vascular resistance,103 with variable performance. Two PICU studies of models using commonly monitored cardiorespiratory variables alone, either from conventional means104 or through novel wireless sensors,105 reported varying sensitivity and specificity to predict cardiorespiratory deterioration and arrest. All models required an hour or longer of continuous physiological input for model training.
Four articles presented models of sepsis prediction using multiple cardiorespiratory physiological variables. Three were derived in NICU patients and despite slightly different features of physiological variables used, all had similar modest predictive value.5,9,106 Notably, two of these studies did not include HRV,9,106 one finding that HRV was not as useful for the subset of adults in their cohort.106 A PICU article included HRV in its model but likewise found it less important than other features.6
Two studies presented models predicting unplanned intubation in the NICU. The first found good prediction of urgent unplanned intubation, notably performing only slightly better than the HRV-based HeRO score alone.107 The second noted similar signatures of deterioration in urgent intubation and sepsis, although their model performed best when predicting urgent intubations.106
Models using continuous physiological variables and non-continuous clinical variables
It is likely that a multidimensional approach to modeling disease that includes continuous physiological variables, intermittently collected clinical variables (e.g., lab values, medication administrations), and patient factors (e.g., age, comorbidities) will result in better performing models through a more complete picture of an individual patient. However, we found only seven studies that integrated intermittently collected clinical variables or patient-level characteristics into continuous cardiorespiratory physiology-based models. Only one of those studies incorporated all three types of data, demonstrating that two machine learning models of sepsis prediction in a large PICU achieved good performance.8 Integrated laboratory results with the HRV-based HeRO score demonstrated an improved performance predicting sepsis in neonates when compared to HeRO score alone.10 A comparison of three machine learning models integrating continuous cardiorespiratory variables with respiratory support and medication data automatically generated asthma scores that were noninferior to expert-derived manual scores.108 A comparison of models to predict at least four mechanical ventilation days in PICU patients found that a model containing both patient-level factors and continuous data performed better than those containing continuous or patient-level factors alone.109 Three machine learning models with continuous versus non-continuous data in a small CICU population found that the best strategy for non-continuous, continuous, combination models had an equivalent performance.110 Finally, two studies investigated the commercially available oxygen delivery index (IDO2; Etiometry, Boston, MA), an index containing both continuous and non-continuous clinical variables (but not demographic data), finding IDO2 to be associated with failed vasoactive wean in CICU patients111 and improved specificity of clinical concern for cardiac arrest in PICU patients.112
Discussion
In this comprehensive scoping review we have summarized the existing evidence on novel approaches to the capture and use of continuous cardiorespiratory physiological data in hospitalized children. We identified 58 articles describing novel devices or measurement approaches and these were found to be primarily small, single-center, observational trials. Only three of these novel devices or measurement approaches were further explored in prediction or inference models in hospitalized children. We also identified 47 articles of prediction or inference modeling using continuous cardiorespiratory variables and these varied greatly in sample size. Most multivariable models did not incorporate multidimensional data (i.e., intermittently collected clinical variables or patient-level factors). Only two studies were randomized control trials in which a cardiorespiratory physiological variable-based model was implemented and tested in hospitalized children (in both cases neonates).67,86 Finally, no study in either section took place entirely outside of an ICU. Based on these findings, we identified three key areas for future development: (1) further external validation of promising novel devices and approaches to measure continuous cardiorespiratory physiological variables; (2) more studies of models integrating multidimensional data; and (3) further dissemination, implementation, and prospective validation of prediction models using continuous cardiorespiratory physiological data.
Though novel cardiorespiratory monitoring devices and approaches have been an important pediatric research focus for the last two decades, the majority of studies are small and single-center. It is difficult to assess the value of these novel devices without further study and external validation. Furthermore, we found only three devices (PiCCO, NICOM, PRAM) that were used in prediction or inference models in hospitalized children.47,89,90 All three systems showed clinical utility but all require proprietary devices and specialized training, and only NICOM is noninvasive. As such, despite availability for over 15 years, none have become routinely incorporated into standard of care. Most of the other novel devices described in this review were developed for neonates where a major motivator is to avoid wire-based sensors, which can be obtrusive and potentially harmful to delicate skin.1,2 It is unclear what the utility of these types of devices will have outside of the NICU, but they may gain more prominence as there is a movement toward higher patient mobility and fewer wires.2
Machine learning-based prediction models that use continuous cardiorespiratory physiological data are steadily emerging in the literature, with the majority of studies published after 2018. In general, we found that the integration of continuous cardiorespiratory physiological data with non-continuous clinical variables is associated with improved performance in various clinical deterioration models. Of the seven prediction models that performed this integration, all but one found that continuous physiological data improved model performance8,10,108,109,111,112 (and the outlier showed non-inferiority110). These types of integrated, dynamic physiological-clinical models will likely serve as a foundation for personalized medicine in the acute care setting.113 Machine learning will be an important tool in this endeavor, as more traditional statistical methods typically require data reduction steps that may discard useful information. However, for these models to be successful, we first need to: (1) identify which patients will benefit most from cardiorespiratory monitoring and the prediction models based on physiological data; (2) share data, resources, and methods to develop more accurate models; and (3) develop strategies to disseminate, implement, and prospectively validate these models.
Identifying the patients who will most benefit from continuous cardiorespiratory monitoring will be an essential step in the successful development and implementation of integrated, dynamic physiological-clinical models. All children with an acute illness may not need continuous cardiorespiratory monitoring. A recent multicenter RCT comparing intermittent versus continuous pulse oximetry in the first episode of bronchiolitis in stable children found no difference in clinical outcomes.114 Clinicians may not, however, be as good at predicting clinical deterioration as we would like–a recent study of emergent PICU transfers due to clinical deterioration found only 35% of patients were on continuous cardiorespiratory monitoring prior to the event requiring transfer.115 Perhaps we should first focus on assessing the pre-test probability of a patient benefitting from continuous cardiorespiratory monitoring to identify the “best” populations of hospitalized children to either escalate to continuous monitoring (with or without associated prediction models) or de-escalate to intermittent monitoring. These strategies may eventually apply to patients who would benefit from remote patient monitoring after discharge from the hospital13 or those who may avoid an admission altogether by being discharged from the emergency department with a wearable device.2
Advances in this field will hinge on our ability to share data, models, resources, and methods. Clinical data science has advanced considerably in the last few years thanks to EHR data-sharing initiatives that leverage common data models, standard terminologies, and data exchange resources.116,117 Indeed, automated sepsis alerts, clinical decision support tools, and real-time continuous vital sign visualization tools have already impacted the way we provide care. However, physiological data from monitoring devices have not seen this same level of sharing and collaboration, with few exceptions (e.g., the MIMIC dataset).118 This lack of collaboration is in large part due to three technical reasons: (1) physiological monitoring data is rarely stored by hospital systems beyond a few days; (2) there is a lack of standards to make physiological data more interoperable across institutions; and (3) the complexity and volume of physiological data makes sharing these data more complicated than other types of clinical data.119 The first problem is the most critical and urgent: we owe it to our patients to store any physiological data we collect to learn how to improve the care of future patients. The other two problems are more easily surmountable through the development of new standards and data collaboration approaches (e.g., federated learning).120
The final hurdle that we must overcome to take full advantage of continuous physiological data and machine learning models is the so-called last mile of artificial intelligence: dissemination, implementation, and prospective validation.121 We identified very few examples of successful implementation and prospective validation of models based on cardiorespiratory physiological data in children, including only two RCTs.67,86 A recent systematic review of real-time clinical analytics implementations found only 14 studies and identified 37 implementation challenges across people, processes, information, and technology.122 A few key steps may improve implementation success: (1) making the models informative, actionable, timely, and interpretable; (2) tailoring each intervention to the particular hospital environment in which the model will be implemented, both with buy-in and education; (3) integrating into routine clinical care without significantly impacting workflows; and (4) providing support and ongoing monitoring of performance after implementation.123,124,125
Conclusion
In this scoping review we have summarized the existing evidence on novel approaches to the capture and use of continuous cardiorespiratory physiological data in hospitalized children. We identified three key areas for future development: (1) further validation of promising novel devices; (2) more studies of models integrating multidimensional data with continuous cardiorespiratory data; and (3) further dissemination, implementation, and validation of prediction models using continuous cardiorespiratory data.
Data availability
All data generated or analyzed during this study are included in this published article and its Supplementary information files.
References
Atallah, L. et al. Unobtrusive ECG monitoring in the NICU using a capacitive sensing array. Physiol. Meas. 35, 895–913 (2014).
Xu, S., Jayaraman, A. & Rogers, J. A. Skin sensors are the future of health care. Nature 571, 319–321 (2019).
Sanchez-Pinto, L. N., Luo, Y. & Churpek, M. M. Big data and data science in critical care. Chest 154, 1239–1248 (2018).
Amiri, P. et al. Potential prognostic markers in the heart rate variability features for early diagnosis of sepsis in the pediatric intensive care unit using convolutional neural network classifiers. Conf. Proc. IEEE Eng. Med. Biol. Soc. 2020, 5627–5630 (2020).
Cabrera-Quiros, L. et al. Prediction of late-onset sepsis in preterm infants using monitoring signals and machine learning. Crit. Care Explor. 3, e0302 (2021).
Kamaleswaran, R. et al. Applying artificial intelligence to identify physiomarkers predicting severe sepsis in the PICU. Pediatr. Crit. Care Med. 19, e495–e503 (2018).
Leon, C., Carrault, G., Pladys, P. & Beuchee, A. Early detection of late onset sepsis in premature infants using visibility graph analysis of heart rate variability. IEEE J. Biomed. Health Inf. 25, 1006–1017 (2021).
Spaeder, M. C. et al. Predictive analytics in the pediatric intensive care unit for early identification of sepsis: capturing the context of age. Pediatr. Res. 86, 655–661 (2019).
Stanculescu, I., Williams, C. K. I. & Freer, Y. Autoregressive hidden Markov models for the early detection of neonatal sepsis. IEEE J. Biomed. Health Inf. 18, 1560–1570 (2014).
Xiao, Y., Griffin, M. P., Lake, D. E. & Moorman, J. R. Nearest-neighbor and logistic regression analyses of clinical and heart rate characteristics in the early diagnosis of neonatal sepsis. Med. Decis. Mak. 30, 258–266 (2010).
Rusin, C. G. et al. Prediction of imminent, severe deterioration of children with parallel circulations using real-time processing of physiologic data. J. Thorac. Cardiovasc. Surg. 152, 171–177 (2016).
Bose, S. N. et al. Early identification of impending cardiac arrest in neonates and infants in the cardiovascular ICU: a statistical modelling approach using physiologic monitoring data. Cardiol. Young. 29, 1340–1348 (2019).
Badke, C. M., Swigart, L., Carroll, M. S., Weese-Mayer, D. E. & Sanchez-Pinto, L. N. Autonomic nervous system dysfunction is associated with re-hospitalization in pediatric septic shock survivors. Front. Pediatr. 9, 745844 (2021).
Yiallourou, S. R., Walker, A. M. & Horne, R. S. C. Validation of a new noninvasive method to measure blood pressure and assess baroreflex sensitivity in preterm infants during sleep. Sleep 29, 1083–1088 (2006).
Lemson, J. et al. The reliability of continuous noninvasive finger blood pressure measurement in critically ill children. Anesth. Analg. 108, 814–821 (2009).
Andriessen, P. et al. Feasibility of noninvasive continuous finger arterial blood pressure measurements in very young children, aged 0-4 years. Pediatr. Res. 63, 691–696 (2008).
Kapur, G. et al. Noninvasive determination of blood pressure by heart sound analysis compared with intra-arterial monitoring in critically ill children–a pilot study of a novel approach. Pediatr. Crit. Care Med. 20, 809–816 (2019).
Liu, C. et al. Wireless, skin-interfaced devices for pediatric critical care: application to continuous, noninvasive blood pressure monitoring. Adv. Healthc. Mater. 10, e2100383 (2021).
Chandler, J. R. et al. Pulse oximeter plethysmograph variation and its relationship to the arterial waveform in mechanically ventilated children. J. Clin. Monit. Comput. 26, 145–151 (2012).
Hay, W. W. Jr et al. Reliability of conventional and new pulse oximetry in neonatal patients. J. Perinatol. 22, 360–366 (2002).
Chaichulee, S. et al. Cardio-respiratory signal extraction from video camera data for continuous non-contact vital sign monitoring using deep learning. Physiol. Meas. 40, 115001 (2019).
Chen, Q. et al. Non-contact heart rate monitoring in neonatal intensive care unit using RGB camera. Conf. Proc. IEEE Eng. Med. Biol. Soc. 2020, 5822–5825 (2020).
Cobos-Torres, J.-C., Abderrahim, M. & Martínez-Orgado, J. Non-contact, simple neonatal monitoring by photoplethysmography. Sensors 18, 4362 (2018).
Mestha, L. K., Kyal, S., Xu, B., Lewis, L. E. & Kumar, V. Towards continuous monitoring of pulse rate in neonatal intensive care unit with a webcam. Conf. Proc. IEEE Eng. Med. Biol. Soc. 2014, 3817–3820 (2014).
Villarroel, M. et al. Non-contact physiological monitoring of preterm infants in the neonatal intensive care unit. NPJ Digit. Med. 2, 128 (2019).
Lee, W. H. et al. Feasibility of non-contact cardiorespiratory monitoring using impulse-radio ultra-wideband radar in the neonatal intensive care unit. PLoS One 15, e0243939 (2020).
Marchionni, P., Scalise, L., Ercoli, I. & Tomasini, E. P. An optical measurement method for the simultaneous assessment of respiration and heart rates in preterm infants. Rev. Sci. Instrum. 84, 121705 (2013).
Sato, S. et al. Assessment of a new piezoelectric transducer sensor for noninvasive cardiorespiratory monitoring of newborn infants in the NICU. Neonatology 98, 179–190 (2010).
Grubb, M. R. et al. Forehead reflectance photoplethysmography to monitor heart rate: preliminary results from neonatal patients. Physiol. Meas. 35, 881–893 (2014).
Simmen, P. et al. Multichannel esophageal heart rate monitoring of preterm infants. IEEE Trans. Biomed. Eng. 68, 1903–1912 (2021).
Kraaijenga, J. V., Hutten, G. J., de Jongh, F. H. & van Kaam, A. H. Transcutaneous electromyography of the diaphragm: a cardio-respiratory monitor for preterm infants. Pediatr. Pulmonol. 50, 889–895 (2015).
Cabrera-Quiros, L. et al. Estimation of heart rate directly from ECG spectrogram in neonate intensive care units. Conf. Proc. IEEE Eng. Med. Biol. Soc. 2020, 320–323 (2020).
Abdel-Rahman, Y., Jeremic, A. & Tan, K. Neonatal heart rate prediction. 2009 Annual International Conference of the IEEE Engineering in Medicine and Biology Society. https://doi.org/10.1109/iembs.2009.5334205 (2009).
Badke, C. M., Marsillio, L. E., Weese-Mayer, D. E. & Sanchez-Pinto, L. N. Autonomic nervous system dysfunction in pediatric sepsis. Front. Pediatr. 6, 280 (2018).
Heart rate variability. Standards of measurement, physiological interpretation, and clinical use. Task Force of the European Society of Cardiology and the North American Society of Pacing and Electrophysiology. Eur. Heart J. 17, 354–381 (1996)..
Mayampurath, A., Volchenboum, S. L. & Sanchez-Pinto, L. N. Using photoplethysmography data to estimate heart rate variability and its association with organ dysfunction in pediatric oncology patients. NPJ Digit. Med. 1, 29 (2018).
Litton, E. & Morgan, M. The PiCCO monitor: a review. Anaesth. Intensive Care 40, 393–408 (2012).
Egan, J. R. et al. Clinical assessment of cardiac performance in infants and children following cardiac surgery. Intensive Care Med. 31, 568–573 (2005).
Fakler, U. et al. Cardiac index monitoring by pulse contour analysis and thermodilution after pediatric cardiac surgery. J. Thorac. Cardiovasc. Surg. 133, 224–228 (2007).
Aslan, N. et al. Comparison of cardiac output and cardiac index values measured by critical care echocardiography with the values measured by pulse index continuous cardiac output (PiCCO) in the pediatric intensive care unit: a preliminary study. Ital. J. Pediatr. 46, 47 (2020).
Gergely, M. et al. Assessment of global tissue perfusion and oxygenation in neonates and infants after open-heart surgery. Interact. Cardiovasc. Thorac. Surg. 18, 426–431 (2014).
Calamandrei, M. et al. Assessment of cardiac output in children: a comparison between the pressure recording analytical method and Doppler echocardiography. Pediatr. Crit. Care Med. 9, 310–312 (2008).
Saxena, R., Durward, A., Puppala, N. K., Murdoch, I. A. & Tibby, S. M. Pressure recording analytical method for measuring cardiac output in critically ill children: a validation study. Br. J. Anaesth. 110, 425–431 (2013).
Gatelli, I. F., Vitelli, O., Chiesa, G., De Rienzo, F. & Martinelli, S. Noninvasive cardiac output monitoring in newborn with hypoplastic left heart syndrome. Am. J. Perinatol. 37, S54–S56 (2020).
Blohm, M. E. et al. Impedance cardiography (electrical velocimetry) and transthoracic echocardiography for non-invasive cardiac output monitoring in pediatric intensive care patients: a prospective single-center observational study. Crit. Care 18, 603 (2014).
Schubert, S. et al. Continuous, non-invasive techniques to determine cardiac output in children after cardiac surgery: evaluation of transesophageal Doppler and electric velocimetry. J. Clin. Monit. Comput. 22, 299–307 (2008).
Lee, J. Y. et al. The ability of stroke volume variation measured by a noninvasive cardiac output monitor to predict fluid responsiveness in mechanically ventilated children. Pediatr. Cardiol. 35, 289–294 (2014).
Botte, A. et al. Evaluation of a noninvasive cardiac output monitor in mechanically ventilated children. Pediatr. Crit. Care Med. 7, 231–236 (2006).
Gil-Anton, J. et al. Cardiac index monitoring by femoral arterial thermodilution after cardiac surgery in children. J. Crit. Care 29, 1132.e1–4 (2014).
Bay-Hansen, R., Elfving, B. & Greisen, G. Use of near infrared spectroscopy for estimation of peripheral venous saturation in newborns: comparison with co-oximetry of central venous blood. Biol. Neonate 82, 1–8 (2002).
Massa-Buck, B., Amendola, V., McCloskey, R. & Rais-Bahrami, K. Significant correlation between regional tissue oxygen saturation and vital signs of critically ill infants. Front. Pediatr. 5, 276 (2017).
Dabal, R. J. et al. Inferior vena cava oxygen saturation monitoring after the Norwood procedure. Ann. Thorac. Surg. 95, 2114–2120 (2013). discussion 2120–2121.
Gillam-Krakauer, M. et al. Correlation of abdominal rSO2 with superior mesenteric artery velocities in preterm infants. J. Perinatol. 33, 609–612 (2013).
Piasek, C. Z., Van Bel, F. & Sola, A. Perfusion index in newborn infants: a noninvasive tool for neonatal monitoring. Acta Paediatr. 103, 468–473 (2014).
Coutrot, M. et al. Perfusion index: physical principles, physiological meanings and clinical implications in anaesthesia and critical care. Anaesth. Crit. Care Pain. Med. 40, 100964 (2021).
Roback, K., Nelson, N., Johansson, A., Hass, U. & Strömberg, T. A new fiberoptical respiratory rate monitor for the neonatal intensive care unit. Pediatr. Pulmonol. 39, 120–126 (2005).
Janssen, R., Wang, W., Moço, A. & de Haan, G. Video-based respiration monitoring with automatic region of interest detection. Physiol. Meas. 37, 100–114 (2016).
Abbas, A. K., Heimann, K., Jergus, K., Orlikowsky, T. & Leonhardt, S. Neonatal non-contact respiratory monitoring based on real-time infrared thermography. Biomed. Eng. Online 10, 93 (2011).
Sauthier, M., Tuli, G., Jouvet, P. A., Brownstein, J. S. & Randolph, A. G. Estimated Pao2: a continuous and noninvasive method to estimate Pao2 and oxygenation index. Crit. Care Explor. 3, e0546 (2021).
Thandaveshwara, D., Chandrashekar Reddy, A. H., Gopalakrishna, M. V. & Doreswamy, S. M. Saturation oxygenation pressure index: a non-invasive bedside measure for severity of respiratory disease in neonates on CPAP. Eur. J. Pediatr. 180, 1287–1292 (2021).
Isenberg, S. J., Neumann, D., Fink, S. & Rich, R. Continuous oxygen monitoring of the conjunctiva in neonates. J. Perinatol. 22, 46–49 (2002).
Pediatric Acute Lung Injury Consensus Conference Group. Pediatric acute respiratory distress syndrome: consensus recommendations from the Pediatric Acute Lung Injury Consensus Conference. Pediatr. Crit. Care Med. 16, 428–439 (2015).
Duyu, M. et al. Comparing the novel microstream and the traditional mainstream method of end-tidal CO2 monitoring with respect to PaCO2 as gold standard in intubated critically ill children. Sci. Rep. 10, 22042 (2020).
Wu, C.-H. et al. Good estimation of arterial carbon dioxide by end-tidal carbon dioxide monitoring in the neonatal intensive care unit. Pediatr. Pulmonol. 35, 292–295 (2003).
Hejlesen, O. K., Cichosz, S. L., Vangsgaard, S., Andresen, M. F. & Madsen, L. P. Clinical implications of a quality assessment of transcutaneous CO2 monitoring in preterm infants in neonatal intensive care. Stud. Health Technol. Inform. 150, 490–494 (2009).
Williams, E., Dassios, T., O’Reilly, N., Walsh, A. & Greenough, A. End-tidal capnography monitoring in infants ventilated on the neonatal intensive care unit. J. Perinatol. 41, 1718–1724 (2021).
Kugelman, A. et al. Impact of continuous capnography in ventilated neonates: a randomized, multicenter study. J. Pediatr. 168, 56–61.e2 (2016).
Belal, S. Y., Taktak, A. F. G., Nevill, A. & Spencer, A. An intelligent ventilation and oxygenation management system in neonatal intensive care using fuzzy trend template fitting. Physiol. Meas. 26, 555–570 (2005).
McSwain, S. D. et al. End-tidal and arterial carbon dioxide measurements correlate across all levels of physiologic dead space. Respir. Care 55, 288–293 (2010).
Riou, Y. et al. Reproducibility of the respiratory dead space measurements in mechanically ventilated children using the CO2SMO monitor. Intensive Care Med. 30, 1461–1467 (2004).
Bhalla, A. K. et al. Monitoring dead space in mechanically ventilated children: volumetric capnography versus time-based capnography. Respir. Care 60, 1548–1555 (2015).
Agus, M. S. D., Alexander, J. L. & Mantell, P. A. Continuous non-invasive end-tidal CO2 monitoring in pediatric inpatients with diabetic ketoacidosis. Pediatr. Diabetes 7, 196–200 (2006).
Erdoğan, S., Oto, A. & Boşnak, M. Reliability of cerebral oximeter in non-invasive diagnosis and follow-up of hypercapnia. Turk. J. Pediatr. 58, 389–394 (2016).
Sochet, A. A. et al. Transcutaneous carbon dioxide monitoring during apnea testing for determination of neurologic death in children: a retrospective case series. Pediatr. Crit. Care Med. 21, 437–442 (2020).
Frerichs, I., Schiffmann, H., Hahn, G. & Hellige, G. Non-invasive radiation-free monitoring of regional lung ventilation in critically ill infants. Intensive Care Med. 27, 1385–1394 (2001).
Davies, P., Yasin, S., Gates, S., Bird, D. & Silvestre, C. Clinical scenarios of the application of electrical impedance tomography in paediatric intensive care. Sci. Rep. 9, 5362 (2019).
Krause, U. et al. Monitoring of regional lung ventilation using electrical impedance tomography after cardiac surgery in infants and children. Pediatr. Cardiol. 35, 990–997 (2014).
Griffin, M. P. et al. Heart rate characteristics: novel physiomarkers to predict neonatal infection and death. Pediatrics 116, 1070–1074 (2005).
Griffin, M. P., Lake, D. E., O’Shea, T. M. & Moorman, J. R. Heart rate characteristics and clinical signs in neonatal sepsis. Pediatr. Res. 61, 222–227 (2007).
Griffin, M. P. & Moorman, J. R. Toward the early diagnosis of neonatal sepsis and sepsis-like illness using novel heart rate analysis. Pediatrics 107, 97–104 (2001).
Ellenby, M. S. et al. Uncoupling and recoupling of autonomic regulation of the heart beat in pediatric septic shock. Shock 16, 274–277 (2001).
Gee, A. H., Barbieri, R., Paydarfar, D. & Indic, P. Predicting bradycardia in preterm infants using point process analysis of heart rate. IEEE Trans. Biomed. Eng. 64, 2300–2308 (2017).
Jost, K., Datta, A. N., Frey, U. P., Suki, B. & Schulzke, S. M. Heart rate fluctuation after birth predicts subsequent cardiorespiratory stability in preterm infants. Pediatr. Res. 86, 348–354 (2019).
Perez–Zabalza, M. et al. Analysis of heart rate variability in children during high flow nasal cannula therapy. Biomed. Phys. Eng. Express 5, 045028 (2019).
Massaro, A. N. et al. Heart rate variability in encephalopathic newborns during and after therapeutic hypothermia. J. Perinatol. 34, 836–841 (2014).
Moorman, J. R. et al. Mortality reduction by heart rate characteristic monitoring in very low birth weight neonates: a randomized trial. J. Pediatr. 159, 900–906.e1 (2011).
Fairchild, K. D. et al. Septicemia mortality reduction in neonates in a heart rate characteristics monitoring trial. Pediatr. Res. 74, 570–575 (2013).
Coggins, S. A. et al. Heart rate characteristic index monitoring for bloodstream infection in an NICU: a 3-year experience. Arch. Dis. Child. Fetal Neonatal Ed. 101, F329–F332 (2016).
Favia, I. et al. Cardiac index assessment by the pressure recording analytical method in infants after paediatric cardiac surgery: a pilot retrospective study. Interact. Cardiovasc. Thorac. Surg. 23, 919–923 (2016).
Wang, F. et al. The fluid management and hemodynamic characteristics of PiCCO employed on young children with severe hand, foot, and mouth disease—a retrospective study. BMC Infect. Dis. 21, 208 (2021).
Ehrmann, D. E. et al. Lessons learned from the first pilot study of the compensatory reserve index after congenital heart surgery requiring cardiopulmonary bypass. World J. Pediatr. Congenit. Heart Surg. 12, 176–184 (2021).
Berg, R. A. et al. End-tidal carbon dioxide during pediatric in-hospital cardiopulmonary resuscitation. Resuscitation 133, 173–179 (2018).
Baserga, M., Reich, B. & Braski, K. Abnormal splanchnic regional saturations in a preterm infant that developed necrotizing enterocolitis following a red blood cell transfusion. Adv. Neonatal Care 20, 401–405 (2020).
Maher, K. O., Phelps, H. M. & Kirshbom, P. M. Near infrared spectroscopy changes with pericardial tamponade. Pediatr. Crit. Care Med. 10, e13–e15 (2009).
Chock, V. Y., Rose, L. A., Mante, J. V. & Punn, R. Near-infrared spectroscopy for detection of a significant patent ductus arteriosus. Pediatr. Res. 80, 675–680 (2016).
Hansen, M. L. et al. Cerebral near-infrared spectroscopy monitoring (NIRS) in children and adults: a systematic review with meta-analysis. Pediatr. Res. (2022) https://doi.org/10.1038/s41390-022-01995-z.
Sivaprasath, P., Mookka Gounder, R. & Mythili, B. Prediction of shock by peripheral perfusion index. Indian J. Pediatr. 86, 903–908 (2019).
Bhalla, A. K., Dong, J., Klein, M. J., Khemani, R. G. & Newth, C. J. L. The association between ventilatory ratio and mortality in children and young adults. Respir. Care 66, 205–212 (2021).
Rasera, C. C., Gewehr, P. M. & Domingues, A. M. T. PET(CO2) measurement and feature extraction of capnogram signals for extubation outcomes from mechanical ventilation. Physiol. Meas. 36, 231–242 (2015).
Matam, B. R., Rajeswari Matam, B., Duncan, H. & Lowe, D. Automated prediction of deterioration of infants in paediatric intensive care using SpO2. Int. J. Biomed. Eng. Technol. 13, 341 (2013).
Nagori, A., Dhingra, L. S., Bhatnagar, A., Lodha, R. & Sethi, T. Predicting hemodynamic shock from thermal images using machine learning. Sci. Rep. 9, 91 (2019).
Rusin, C. G. et al. Automated prediction of cardiorespiratory deterioration in patients with single ventricle. J. Am. Coll. Cardiol. 77, 3184–3192 (2021).
Erez, E., Mazwi, M. L., Marquez, A. M., Moga, M.-A. & Eytan, D. Hemodynamic patterns before inhospital cardiac arrest in critically ill children: an exploratory study. Crit. Care Explor 3, e0443 (2021).
Matam, B. R., Duncan, H. & Lowe, D. Machine learning based framework to predict cardiac arrests in a paediatric intensive care unit. J. Clin. Monit. Comput. 33, 713–724 (2019).
Duncan, H. P., Fule, B., Rice, I., Sitch, A. J. & Lowe, D. Wireless monitoring and real-time adaptive predictive indicator of deterioration. Sci. Rep. 10, 11366 (2020).
Moss, T. J. et al. Signatures of subacute potentially catastrophic illness in the ICU: model development and validation. Crit. Care Med. 44, 1639–1648 (2016).
Clark, M. T. et al. Predictive monitoring for respiratory decompensation leading to urgent unplanned intubation in the neonatal intensive care unit. Pediatr. Res. 73, 104–110 (2013).
Messinger, A. I. et al. Novel pediatric-automated respiratory score using physiologic data and machine learning in asthma. Pediatr. Pulmonol. 54, 1149–1155 (2019).
Castiñeira, D. et al. Adding continuous vital sign information to static clinical data improves the prediction of length of stay after intubation: a data-driven machine learning approach. Respir. Care 65, 1367–1377 (2020).
Rooney, S. R. et al. Prediction of extubation failure in the paediatric cardiac ICU using machine learning and high-frequency physiologic data. Cardiol. Young 1–8 (2021).
Goldsmith, M. P. et al. Use of a risk analytic algorithm to inform weaning from vasoactive medication in patients following pediatric cardiac surgery. Crit. Care Explor. 3, e0563 (2021).
Dewan, M., Cooper, D. S. & Tegtmeyer, K. Low inadequate oxygen delivery index is associated with decreased cardiac arrest risk in high-risk pediatric ICU patients. Crit. Care Explor. 4, e0600 (2022).
Holder, A. L. & Clermont, G. Using what you get: dynamic physiologic signatures of critical illness. Crit. Care Clin. 31, 133–164 (2015).
Mahant, S. et al. Intermittent vs continuous pulse oximetry in hospitalized infants with stabilized bronchiolitis: a randomized clinical trial. JAMA Pediatr. 175, 466–474 (2021).
Kowalski, R. L., Lee, L., Spaeder, M. C., Moorman, J. R. & Keim-Malpass, J. Accuracy and monitoring of Pediatric Early Warning Score (PEWS) scores prior to emergent pediatric intensive care unit (ICU) transfer: retrospective analysis. JMIR Pediatr. Parent 4, e25991 (2021).
Forrest, C. B., Margolis, P., Seid, M. & Colletti, R. B. PEDSnet: how a prototype pediatric learning health system is being expanded into a national network. Health Aff. 33, 1171–1177 (2014).
Brant, E. B. et al. Developing a shared sepsis data infrastructure: a systematic review and concept map to FHIR. NPJ Digit. Med. 5, 44 (2022).
Johnson, A. E. W. et al. MIMIC-III, a freely accessible critical care database. Sci. Data 3, 160035 (2016).
Maslove, D. M., Elbers, P. W. G. & Clermont, G. Artificial intelligence in telemetry: what clinicians should know. Intensive Care Med. 47, 150–153 (2021).
Crowson, M. G. et al. A systematic review of federated learning applications for biomedical data. PLOS Digital Health 1, e0000033 (2022).
Coiera, E. The last mile: where artificial intelligence meets reality. J. Med. Internet Res. 21, e16323 (2019).
Lim, H. C. et al. Toward a learning health care system: a systematic review and evidence-based conceptual framework for implementation of clinical analytics in a digital hospital. Appl. Clin. Inform. 13, 339–354 (2022).
Moorman, L. P. Principles for real-world implementation of bedside predictive analytics monitoring. Appl. Clin. Inform. 12, 888–896 (2021).
Futoma, J., Simons, M., Panch, T., Doshi-Velez, F. & Celi, L. A. The myth of generalisability in clinical research and machine learning in health care. Lancet Digit Health 2, e489–e492 (2020).
Sanchez-Pinto, L. N. & Bennett, T. D. Evaluation of machine learning models for clinical prediction problems. Pediatr. Crit. Care Med. 23, 405–408 (2022).
McQuillen, P. S. et al. Regional and central venous oxygen saturation monitoring following pediatric cardiac surgery: concordance and association with clinical variables. Pediatr. Crit. Care Med. 8, 154–160 (2007).
Ong, T. et al. Higher pulmonary dead space may predict prolonged mechanical ventilation after cardiac surgery. Pediatr. Pulmonol. 44, 457–463 (2009).
Heskamp, L., Lansdorp, B., Hopman, J., Lemson, J. & de Boode, W.-P. Ventilator-induced pulse pressure variation in neonates. Physiol. Rep. 4, e12716 (2016).
Joshi, R. et al. Cardiorespiratory coupling in preterm infants. J. Appl. Physiol. 126, 202–213 (2019).
Author information
Authors and Affiliations
Contributions
All authors made substantial contributions to the conception and design of the study. S.B.W., C.M.B., K.S.H., M.S.C., D.E.W.-M., and L.N.S.-P. contributed to the acquisition, analysis, and interpretation of data. S.B.W., C.M.B., K.S.H., M.S.C., D.E.W.-M., and L.N.S.-P. helped draft the article, revise the manuscript critically for important intellectual content, and gave final approval of the version to be submitted for peer review.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Walker, S.B., Badke, C.M., Carroll, M.S. et al. Novel approaches to capturing and using continuous cardiorespiratory physiological data in hospitalized children. Pediatr Res 93, 396–404 (2023). https://doi.org/10.1038/s41390-022-02359-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41390-022-02359-3