Abstract
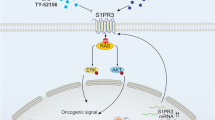
TAL1 is one of the most frequently dysregulated genes in T-ALL and is overexpressed in about 50% of T-ALL cases. One of the molecular mechanisms of TAL1 overexpression is abnormal mutations in the upstream region of the TAL1 promoter that introduce binding motifs for the MYB transcription factor. MYB binding at this location creates a 5’ TAL1 super-enhancer (SE), which leads to aberrant expression of TAL1 and is associated with unfavorable clinical outcomes. Although targeting TAL1 is considered to be an attractive therapeutic strategy for patients with T-ALL, direct inhibition of transcription factors is challenging. Here, we show that KLF4, a known tumor suppressor in leukemic cells, suppresses SE-driven TAL1 expression in T-ALL cells. Mechanistically, KLF4 downregulates MYB expression by directly binding to its promoter and inhibits the formation of 5’ TAL1 SE. In addition, we found that APTO-253, a small molecule inducer of KLF4, exerts an anti-leukemic effect by targeting SE-driven TAL1 expression in T-ALL cells. Taken together, our results suggest that the induction of KLF4 is a promising strategy to control TAL1 expression and could be a novel treatment for T-ALL patients with a poor prognosis.

This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 50 print issues and online access
$259.00 per year
only $5.18 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
Data availability
All data generated or analyzed during this study are included in this published article and its supplementary information files.
References
Aifantis I, Raetz E, Buonamici S. Molecular pathogenesis of T-cell leukaemia and lymphoma. Nat Rev Immunol. 2008;8:380–90.
Belver L, Ferrando A. The genetics and mechanisms of T cell acute lymphoblastic leukaemia. Nat Rev Cancer. 2016;16:494–507.
Look AT. Oncogenic transcription factors in the human acute leukemias. Science. 1997;278:1059–64.
Mansour MR, Abraham BJ, Anders L, Berezovskaya A, Gutierrez A, Durbin AD, et al. Oncogene regulation. An oncogenic super-enhancer formed through somatic mutation of a noncoding intergenic element. Science. 2014;346:1373–7.
Sanda T, Lawton LN, Barrasa MI, Fan ZP, Kohlhammer H, Gutierrez A, et al. Core transcriptional regulatory circuit controlled by the TAL1 complex in human T cell acute lymphoblastic leukemia. Cancer Cell. 2012;22:209–21.
Sanda T, Leong WZ. TAL1 as a master oncogenic transcription factor in T-cell acute lymphoblastic leukemia. Exp Hematol. 2017;53:7–15.
Berg T. Inhibition of transcription factors with small organic molecules. Curr Opin Chem Biol. 2008;12:464–71.
Rowland BD, Bernards R, Peeper DS. The KLF4 tumour suppressor is a transcriptional repressor of p53 that acts as a context-dependent oncogene. Nat Cell Biol. 2005;7:1074–82.
Morita K, Masamoto Y, Kataoka K, Koya J, Kagoya Y, Yashiroda H, et al. BAALC potentiates oncogenic ERK pathway through interactions with MEKK1 and KLF4. Leukemia. 2015;29:2248–56.
Noura M, Morita K, Kiyose H, Matsuo H, Nishinaka-Arai Y, Kurokawa M, et al. Pivotal role of DPYSL2A in KLF4-mediated monocytic differentiation of acute myeloid leukemia cells. Sci Rep. 2020;10:20245.
Noura M, Morita K, Kiyose H, Okuno Y, Matsuo H, Koyama A, et al. Albendazole induces the terminal differentiation of acute myeloid leukaemia cells to monocytes by stimulating the Krüppel-like factor 4-dihydropyrimidinase-like 2A (KLF4-DPYSL2A) axis. Br J Haematol. 2021;194:598–603.
Guan H, Xie L, Leithäuser F, Flossbach L, Möller P, Wirth T, et al. KLF4 is a tumor suppressor in B-cell non-Hodgkin lymphoma and in classic Hodgkin lymphoma. Blood. 2010;116:1469–78.
Shen Y, Park CS, Suppipat K, Mistretta TA, Puppi M, Horton TM, et al. Inactivation of KLF4 promotes T-cell acute lymphoblastic leukemia and activates the MAP2K7 pathway. Leukemia. 2017;31:1314–24.
Yasunaga J, Taniguchi Y, Nosaka K, Yoshida M, Satou Y, Sakai T, et al. Identification of aberrantly methylated genes in association with adult T-cell leukemia. Cancer Res. 2004;64:6002–9.
Li W, Jiang Z, Li T, Wei X, Zheng Y, Wu D, et al. Genome-wide analyses identify KLF4 as an important negative regulator in T-cell acute lymphoblastic leukemia through directly inhibiting T-cell associated genes. Mol Cancer. 2015;14:26.
Bagger FO, Kinalis S, Rapin N. BloodSpot: a database of healthy and malignant haematopoiesis updated with purified and single cell mRNA sequencing profiles. Nucleic Acids Res. 2019;47:D881–D885.
Brown L, Cheng JT, Chen Q, Siciliano MJ, Crist W, Buchanan G, et al. Site-specific recombination of the tal-1 gene is a common occurrence in human T cell leukemia. EMBO J. 1990;9:3343–51.
Janssen JW, Ludwig WD, Sterry W, Bartram CR. SIL-TAL1 deletion in T-cell acute lymphoblastic leukemia. Leukemia. 1993;7:1204–10.
Bieker JJ. Krüppel-like factors: three fingers in many pies. J Biol Chem. 2001;276:34355–8.
Aksoy I, Giudice V, Delahaye E, Wianny F, Aubry M, Mure M, et al. Klf4 and Klf5 differentially inhibit mesoderm and endoderm differentiation in embryonic stem cells. Nat Commun. 2014;5:3719.
Kulakovskiy IV, Medvedeva YA, Schaefer U, Kasianov AS, Vorontsov IE, Bajic VB, et al. HOCOMOCO: a comprehensive collection of human transcription factor binding sites models. Nucleic Acids Res. 2013;41:D195–202.
Li Z, Abraham BJ, Berezovskaya A, Farah N, Liu Y, Leon T, et al. APOBEC signature mutation generates an oncogenic enhancer that drives LMO1 expression in T-ALL. Leukemia. 2017;31:2057–64.
Huesca M, Lock LS, Khine AA, Viau S, Peralta R, Cukier IH, et al. A novel small molecule with potent anticancer activity inhibits cell growth by modulating intracellular labile zinc homeostasis. Mol Cancer Ther. 2009;8:2586–96.
Local A, Zhang H, Benbatoul KD, Folger P, Sheng X, Tsai CY, et al. APTO-253 stabilizes G-quadruplex DNA, inhibits MYC expression, and induces DNA damage in acute myeloid leukemia cells. Mol Cancer Ther. 2018;17:1177–86.
Clappier E, Cuccuini W, Kalota A, Crinquette A, Cayuela JM, Dik WA, et al. The C-MYB locus is involved in chromosomal translocation and genomic duplications in human T-cell acute leukemia (T-ALL), the translocation defining a new T-ALL subtype in very young children. Blood. 2007;110:1251–61.
Lahortiga I, De Keersmaecker K, Van Vlierberghe P, Graux C, Cauwelier B, Lambert F, et al. Duplication of the MYB oncogene in T cell acute lymphoblastic leukemia. Nat Genet. 2007;39:593–5.
O’Neil J, Tchinda J, Gutierrez A, Moreau L, Maser RS, Wong KK, et al. Alu elements mediate MYB gene tandem duplication in human T-ALL. J Exp Med. 2007;204:3059–66.
Cercek A, Wheler J, Murray PE, Zhou S, Saltz L. Phase 1 study of APTO-253 HCl, an inducer of KLF4, in patients with advanced or metastatic solid tumors. Invest N Drugs. 2015;33:1086–92.
Ohanian M, Arellano ML, Levy MY, O’Dwyer K, Babiker H, Mahadevan D, et al. A phase 1a/b dose escalation study of the MYC repressor Apto-253 in patients with relapsed or refractory AML or high-risk MDS. Blood. 2021;138:3411–3411.
Smith C, Touzart A, Simonin M, Tran-Quang C, Hypolite G, Latiri M, et al. Harnessing the MYB-dependent TAL1 5' super-enhancer for targeted therapy in T-ALL. Mol Cancer. 2023;22:12.
Edgar R, Domrachev M, Lash AE. Gene expression omnibus: NCBI gene expression and hybridization array data repository. Nucleic Acids Res. 2002;30:207–10.
Barrett T, Wilhite SE, Ledoux P, Evangelista C, Kim IF, Tomashevsky M, et al. NCBI GEO: archive for functional genomics data sets–update. Nucleic Acids Res. 2013;41:D991–995.
Livak KJ, Schmittgen TD. Analysis of relative gene expression data using real-time quantitative PCR and the 2(-Delta Delta C(T)) Method. Methods. 2001;25:402–8.
Chou TC, Talalay P. Quantitative analysis of dose-effect relationships: the combined effects of multiple drugs or enzyme inhibitors. Adv Enzym Regul. 1984;22:27–55.
Odaira K, Yasuda T, Okada K, Shimooka T, Kojima Y, Noura M, et al. Functional inhibition of MEF2 by C/EBP is a possible mechanism of leukemia development by CEBP-IGH fusion gene. Cancer Sci. 2023;114:781–92.
Matsuo H, Nakatani K, Harata Y, Higashitani M, Ito Y, Inagami A, et al. Efficacy of a combination therapy targeting CDK4/6 and autophagy in a mouse xenograft model of t(8;21) acute myeloid leukemia. Biochem Biophys Rep. 2021;27:101099.
Acknowledgements
This work was supported by JSPS KAKENHI Grant Numbers 21K19505 and 22H03102 (to FH) and 23K15298 (to MN); and Grants for Practical Research for Innovative Cancer Control Grant Numbers JP21ck0106607 (to FH) from the Japan Agency for Medical Research and Development (AMED). We sincerely thank all for their support.
Author information
Authors and Affiliations
Contributions
MN initiated the study, designed and performed the experiments, analyzed the data, and wrote the manuscript. HM performed the in vivo experiments. All others supervised the research and approved the final manuscript for submission.
Corresponding author
Ethics declarations
Competing interests
HK has received research funds from FUJIFILM, Kyowa Hakko Kirin, Otsuka, Perseus Proteomics, Daiichi Sankyo, AbbVie, CURED, Astellas Pharma, Bristol-Myers Squibb; and scholarship funds from Zenyaku Kogyo, Nippon Shinyaku, Chugai, Astellas Pharma, Kyowa Hakko Kirin, Takeda, Sumitomo Dainippon Pharma, Sanofi, Eisai, and Ono; and honoraria from AbbVie, Chugai, Astellas Pharma, and Novartis. All other authors have nothing to disclose.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Noura, M., Matsuo, H., Yasuda, T. et al. Suppression of super-enhancer-driven TAL1 expression by KLF4 in T-cell acute lymphoblastic leukemia. Oncogene 43, 447–456 (2024). https://doi.org/10.1038/s41388-023-02913-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41388-023-02913-1