Abstract
Background
Gene–obesogenic environment interactions influence body mass index (BMI) across the life course; however, limited research examines how these interactions may differ by race and sex.
Methods
Utilizing mixed-effects models, we examined the interaction effects of a polygenic risk score (PGS) generated from BMI-associated single-nucleotide polymorphisms, and environmental factors, including age, physical activity, alcohol intake, and childhood socioeconomic status on measured longitudinal BMI from the Health and Retirement Study (HRS). HRS is a population representative survey of older adults in the United States. This study used a subsample of genotyped Black (N = 1796) and White (N = 4925) men and women (50–70 years) with measured BMI.
Results
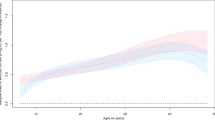
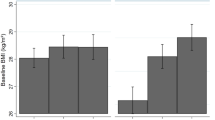
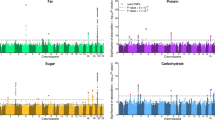
Higher PGS was associated with higher BMI. The association between PGS and BMI weakened as individuals aged among White men (Pinteraction = 0.0383) and White women (Pinteraction = 0.0514). The mean BMI difference between the 90th and 10th PGS percentile was 4.25 kg/m2 among 50-year-old White men, and 3.11 kg/m2 among the 70 years old’s, i.e., a 1.14 kg/m2 (95% CI: −0.27, 2.82) difference. The difference among 50- and 70-year-old White women was 1.34 kg/m2 (95% CI: 0.09, 2.60). In addition, the protection effect of physical activity was stronger among White women with higher PGS (Pinteraction = 0.0546). Vigorous physical activity (compared with never) was associated with 1.66 kg/m2 (95% CI: 1.06, 2.29) lower mean BMI among those in the 90th PGS percentile, compared with 0.83 kg/m2 (95% CI: 0.37, 1.29) lower among those in the 10th PGS percentile. Interactions were also observed between both PGS and alcohol intake among White men (Pinteraction = 0.0034) and women (Pinteraction = 0.0664) and Black women (Pinteraction = 0.0108), and PGS and childhood socioeconomic status among White women (Pinteraction = 0.0007).
Conclusions
Our findings reinforce the importance of physical activity among those with an elevated genetic risk; additionally, other detected interactions may underscore the influence of broader social environments on obesity-promoting genes.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Boles A, Kandimalla R, Reddy PH. Dynamics of diabetes and obesity: epidemiological perspective. Biochim Biophys Acta. 2017;1863:1026–36.
Bastien M, Poirier P, Lemieux I, Després J-P. Overview of epidemiology and contribution of obesity to cardiovascular disease. Prog Cardiovasc Dis. 2014;56:369–81.
Arnold M, Leitzmann M, Freisling H, Bray F, Romieu I, Renehan A, et al. Obesity and cancer: an update of the global impact. Cancer Epidemiol. 2016;41:8–15.
Bhaskaran K, Dos-Santos-Silva I, Leon DA, Douglas IJ, Smeeth L. Association of BMI with overall and cause-specific mortality: a population-based cohort study of 3.6 million adults in the UK. Lancet. 2018;6:944–53.
Tremmel M, Gerdtham U-G, Nilsson P, Saha S. Economic burden of obesity: a systematic literature review. Int J Environ Res Public Health. 2017;14:435.
Flegal KM, Kit BK, Orpana H, Graubard BI. Association of all-cause mortality with overweight and obesity using standard body mass index categories: a systematic review and meta-analysis. JAMA. 2013;309:71–82.
Flegal KM, Kruszon-Moran D, Carroll MD, Fryar CD, Ogden CL. Trends in obesity among adults in the united states, 2005 to 2014. JAMA. 2016;315:2284–91.
Dong SS, Zhang YJ, Chen YX, Yao S, Hao RH, Rong Y, et al. Comprehensive review and annotation of susceptibility SNPs associated with obesity‐related traits. Obes Rev. 2018;19:917–30.
Locke AE, Kahali B, Berndt SI, Justice AE, Pers TH, Day FR, et al. Genetic studies of body mass index yield new insights for obesity biology. Nature. 2015;518:197–206.
Speakman JR, Loos RJF, O’Rahilly S, Hirschhorn JN, Allison DB. GWAS for BMI: a treasure trove of fundamental insights into the genetic basis of obesity. Int J Obes. 2018;42:1524–31.
Celis-Morales CA, Lyall DM, Bailey MES, Petermann-Rocha F, Anderson J, Ward J, et al. The combination of physical activity and sedentary behaviors modifies the genetic predisposition to obesity. Obesity. 2019;27:653–61.
Ochs-Balcom HM, Preus L, Nie J, Wactawski-Wende J, Agyemang L, Neuhouser ML, et al. Physical activity modifies genetic susceptibility to obesity in postmenopausal women. Menopause. 2018;25:1131–7.
Wang TG, Heianza Y, Sun DJY, Huang T, Ma WJ, Rimm EB, et al. Improving adherence to healthy dietary patterns, genetic risk, and long term weight gain: gene-diet interaction analysis in two prospective cohort studies. BMJ. 2018;360:9.
Svendstrup M, Allin KH, Sorensen TIA, Hansen TH, Grarup N, Hansen T, et al. Genetic risk scores for body fat distribution attenuate weight loss in women during dietary intervention. Int J Obes. 2018;42:370–5.
Ding M, Ellervik C, Huang T, Jensen MK, Curhan GC, Pasquale LR, et al. Diet quality and genetic association with body mass index: results from 3 observational studies. Am J Clin Nutr. 2018;108:1291–300.
Celis-Morales C, Lyall DM, Guo YB, Steell L, Llanas D, Ward J, et al. Sleep characteristics modify the association of genetic predisposition with obesity and anthropometric measurements in 119,679 UK Biobank participants. Am J Clin Nutr. 2017;105:980–90.
Llewellyn C, Wardle J. Behavioral susceptibility to obesity: gene–environment interplay in the development of weight. Physiol. Behav. 2015;152:494–501.
Wang NJ, Lu M, Chen C, Xia FZ, Han B, Li Q, et al. Adiposity genetic risk score modifies the association between blood lead level and body mass index. J Clin Endocrinol Metab. 2018;103:4005–13.
Nagpal S, Gibson G, Marigorta UM. Pervasive modulation of obesity risk by the environment and genomic background. Genes. 2018;9:13.
Rask-Andersen M, Karlsson T, Ek WE, Johansson A. Gene-environment interaction study for BMI reveals interactions between genetic factors and physical activity, alcohol consumption and socioeconomic status. PLoS Genet. 2017;13:20.
Tyrrell J, Wood AR, Ames RM, Yaghootkar H, Beaumont RN, Jones SE, et al. Gene-obesogenic environment interactions in the UK Biobank study. Int J Epidemiol. 2017;46:559–75.
Song M, Zheng Y, Qi L, Hu FB, Chan AT, Giovannucci EL. Longitudinal analysis of genetic susceptibility and BMI throughout adult life. Diabetes. 2018;67:248.
Rohde JF, Angquist L, Larsen SC, Tolstrup JS, Husemoen LLN, Linneberg A, et al. Alcohol consumption and its interaction with adiposity-associated genetic variants in relation to subsequent changes in waist circumference and body weight. Nutr J. 2017;16:11.
Stryjecki C, Alyass A, Meyre D. Ethnic and population differences in the genetic predisposition to human obesity. Obes Rev. 2018;19:62–80.
Walter S, Mejia-Guevara I, Estrada K, Liu SY, Glymour MM. Association of a genetic risk score with body mass index across different birth cohorts. JAMA. 2016;316:63–69.
Zhao W, Ware E, He Z, Kardia S, Faul J, Smith J. Interaction between social/psychosocial factors and genetic variants on body mass index: a gene-environment interaction analysis in a longitudinal setting. Int J Environ Res Public Health. 2017;14:1153.
Calvin CM, Hagenaars SP, Gallacher J, Harris SE, Davies G, Liewald DC, et al. Sex-specific moderation by lifestyle and psychosocial factors on the genetic contributions to adiposity in 112,151 individuals from UK Biobank. Sci Rep. 2019;9:12.
Fisher GG, Ryan LH. Overview of the Health and Retirement Study and introduction to the special issue. Work Aging Retire. 2018;4:1–9.
Sonnega A, Faul JD, Ofstedal MB, Langa KM, Phillips JW, Weir DR. Cohort profile: the Health and Retirement Study (HRS). Int J Epidemiol. 2014;43:576–85.
Domingue BW, Belsky DW, Harrati A, Conley D, Weir DR, Boardman JD. Mortality selection in a genetic sample and implications for association studies. Int J Epidemiol. 2017;46:1285–94.
Steffick DE. Documentation of affective functioning measures in the Health and Retirement Study. Ann Arbor, MI: University of Michigan; 2000.
Drewnowski A, Specter SE. Poverty and obesity: the role of energy density and energy costs. Am J Clin Nutr. 2004;79:6–16.
Luppino FS, de Wit LM, Bouvy PF, Stijnen T, Cuijpers P, Penninx BWJH, et al. Overweight, obesity, and depression: a systematic review and meta-analysis of longitudinal studies. JAMA Psychiatry. 2010;67:220–9.
Clarke TK, Hall LS, Fernandez-Pujals AM, MacIntyre DJ, Thomson P, Hayward C, et al. Major depressive disorder and current psychological distress moderate the effect of polygenic risk for obesity on body mass index. Transl Psychiatr. 2015;5:e592–e592.
Faith MS, Kral TVE. Social environmental and genetic influences on obesity and obesity-promoting behaviors: fostering research integration. In: Hernandez LM, Blazer DG, editors. Institute of Medicine (US) Committee on Assessing Interactions Among Social, Behavioral, and Genetic Factors in Health. Washington, DC: National Academies Press (US); 2006.
Johnson W, Ong KK, Elks CE, Wareham NJ, Wong A, Muniz-Terrera G, et al. Modification of genetic influences on adiposity between 36 and 63 years of age by physical activity and smoking in the 1946 British Birth Cohort Study. Nutr Diabetes. 2014;4:7.
Locke AE, Kahali B, Berndt SI, Justice AE, Pers TH, Day FR, et al. Genetic studies of body mass index yield new insights for obesity biology. Nature. 2015;518:197–206.
Ware E, Schmitz L, Gard A, Faul J. HRS polygenic scores—release 3: 2006–12 genetic data. Ann Arbor: Survey Research Center, University of Michigan; 2018.
Fitzmaurice GM, Laird NM, Ware JH. Applied longitudinal analysis, vol. 998. Hoboken, NJ: John Wiley & Sons; 2012.
McDonald L. Tests for the general linear hypothesis under the multiple design multivariate linear model. Ann Stat. 1975;3:461–6.
Efron B, Tibshirani RJ. An introduction to the bootstrap. Boca Raton, FL: CRC press; 1994.
Hosseini-Esfahani F, Koochakpoor G, Daneshpour MS, Sedaghati-khayat B, Mirmiran P, Azizi F. Mediterranean dietary pattern adherence modify the association between FTO genetic variations and obesity phenotypes. Nutrients. 2017;9:13.
Brunkwall L, Chen Y, Hindy G, Rukh G, Ericson U, Barroso I, et al. Sugar-sweetened beverage consumption and genetic predisposition to obesity in 2 Swedish cohorts. Am J Clin Nutr. 2016;104:809–15.
Casas-Agustench P, Arnett DK, Smith CE, Lai CQ, Parnell LD, Borecki IB, et al. Saturated fat intake modulates the association between an obesity genetic risk score and body mass index in two US populations. J Acad Nutr Diet. 2014;114:1954–66.
Goni L, Cuervo M, Milagro FI, Martinez JA. A genetic risk tool for obesity predisposition assessment and personalized nutrition implementation based on macronutrient intake. Genes Nutr. 2015;10:10.
Gilbert PA, Khokhar S. Changing dietary habits of ethnic groups in Europe and implications for health. Nutr Rev. 2008;66:203–15.
Kelly-Irving M, Lepage B, Dedieu D, Bartley M, Blane D, Grosclaude P, et al. Adverse childhood experiences and premature all-cause mortality. Eur J Epidemiol. 2013;28:721–34.
Brown DW, Anda RF, Tiemeier H, Felitti VJ, Edwards VJ, Croft JB, et al. Adverse childhood experiences and the risk of premature mortality. Am J Prevent Med. 2009;37:389–96.
Yengo L, Sidorenko J, Kemper KE, Zheng Z, Wood AR, Weedon MN, et al. Meta-analysis of genome-wide association studies for height and body mass index in approximately 700000 individuals of European ancestry. Hum Mol Genet. 2018;27:3641–9.
Shuey KM, Willson AE. Cumulative disadvantage and black-white disparities in life-course health trajectories. Res Aging. 2008;30:200–25.
Rothman KJ. BMI-related errors in the measurement of obesity. Int J Obes. 2008;32:S56.
Ferrucci L, Cooper R, Shardell M, Simonsick EM, Schrack JA, Kuh D. Age-related change in mobility: perspectives from life course epidemiology and geroscience. J Gerontol. 2016;71:1184–94.
Krieger N. Genders, sexes, and health: what are the connections—and why does it matter? Int J Epidemiol. 2003;32:652–7.
Acknowledgements
This study was supported by Ola HAWAII through the National Institute on Minority Health and Health Disparities (U54MD007601-31), National Institutes of Health.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Thompson, M.D., Pirkle, C.M., Youkhana, F. et al. Gene–obesogenic environment interactions on body mass indices for older black and white men and women from the Health and Retirement Study. Int J Obes 44, 1893–1905 (2020). https://doi.org/10.1038/s41366-020-0589-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41366-020-0589-4