Abstract
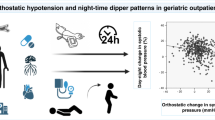
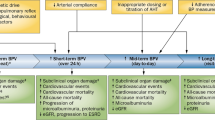
Orthostatic hypertension—a condition characterized by a hyperactive pressor response to orthostatic stress—is an emerging risk factor for cardiovascular disease and is associated with hypertensive target-organ damage (resulting in silent cerebrovascular disease, left ventricular hypertrophy, carotid atherosclerosis and/or chronic kidney disease) and cardiovascular events (such as coronary artery disease and lacunar stroke). The condition is also considered to be a form of prehypertension as it precedes hypertension in young, normotensive adults. Orthostatic blood pressure changes can be assessed using orthostatic stress tests, including clinic active standing tests, home blood pressure monitoring and the head-up tilting test. Devices for home and for ambulatory blood pressure monitoring that are equipped with position sensors and do not induce a white-coat effect have increased the sensitivity and specificity of diagnosis of out-of-clinic orthostatic hypertension. Potential major mechanisms of orthostatic hypertension are sympathetic hyperactivity (as a result of hypersensitivity of the cardiopulmonary and arterial baroreceptor reflex) and α-adrenergic hyperactivation. Orthostatic hypertension is also associated with morning blood pressure surge and extreme nocturnal blood pressure dipping, both of which increase the pulsatile haemodynamic stress of central arterial pressure and blood flow in patients with systemic haemodynamic atherothrombotic syndrome.
Key Points
-
Orthostatic hypertension is characterized by a hyper-reactive pressor response to orthostatic stress and is an emerging risk factor for organ damage and cardiovascular disease
-
The condition increases the pulsatile haemodynamic stress of central arterial pressure and blood flow, resulting in progression of systemic haemodynamic atherothrombotic syndrome
-
Orthostatic hypertension precedes hypertension and is considered to be a form of prehypertension and a biomarker of masked hypertension in patients with normal sitting blood pressure levels
-
Sympathetic hyperactivity (resulting from hypersensitivity of the cardiopulmonary and arterial baroreceptor reflex) and α-adrenergic hyper-reactive vascular disease are potential major mechanisms of orthostatic hypertension
-
Further studies are needed to demonstrate whether orthostatic hypertension is only a marker or one of the leading causes of target-organ damage and cardiovascular events
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout







Similar content being viewed by others
References
Ogihara, T. et al. The Japanese Society of Hypertension guidelines for the management of hypertension (JSH 2009). Hypertens. Res. 32, 3–107 (2009).
Mancia, G. et al. 2013 ESH/ESC guidelines for the management of arterial hypertension. The Task Force for the management of arterial hypertension of the European Society of Hypertension (ESH) and of the European Society of Cardiology (ESC). Eur. Heart J. 34, 2159–2219 (2013).
Kario, K. & Pickering, T. G. Blood pressure variability in elderly patients. Lancet 355, 1645–1646 (2000).
Parati, G., Ochoa, J. E., Lombardi, C. & Bilo, G. Assessment and management of blood-pressure variability. Nat. Rev. Cardiol. 10, 143–155 (2013).
Kario, K. Preceding linkage between a morning surge in blood pressure and small artery remodeling: an indicator of prehypertension? J. Hypertens. 25, 1573–1575 (2007).
Fedorowski, A. et al. Orthostatic hypotension predicts all-cause mortality and coronary events in middle-aged individuals (The Malmo Preventive Project). Eur. Heart J. 31, 85–91 (2010).
Task Force for the Diagnosis and Management of Syncope et al. Guidelines for the diagnosis and management of syncope (version 2009). Eur. Heart J. 30, 2631–2671 (2009).
Freeman, R. et al. Consensus statement on the definition of orthostatic hypotension, neurally mediated syncope and the postural tachycardia syndrome. Clin. Auton. Res. 21, 69–72 (2011).
Fessel, J. & Robertson, D. Orthostatic hypertension: when pressor reflexes overcompensate. Nat. Clin. Pract. Nephrol. 2, 424–431 (2006).
Kario, K. Orthostatic hypertension: a measure of blood pressure variation for predicting cardiovascular risk. Circ. J. 73, 1002–1007 (2009).
Buddineni, J. P., Chauhan, L., Ahsan, S. T. & Whaley-Connell, A. An emerging role for understanding orthostatic hypertension in the cardiorenal syndrome. Cardiorenal Med. 1, 113–122 (2011).
Robertson, D. Orthostatic hypertension: the last hemodynamic frontier. Hypertension 57, 158–159 (2011).
Streeten, D. H. et al. Orthostatic hypertension. Pathogenetic studies. Hypertension 7, 196–203 (1985).
Olga, V., Lucio, M., Giuseppe, G., Stefano, M. & Paolo, P. Blood pressure response to stress tests does not reflect blood pressure variability and degree of cardiovascular involvement in young hypertensives. Int. J. Cardiol. 48, 303–310 (1995).
Matsubayashi, K. et al. Postural dysregulation in systolic blood pressure is associated with worsened scoring on neurobehavioral function tests and leukoaraiosis in the older elderly living in a community. Stroke 28, 2169–2173 (1997).
Vriz, O. et al. Does orthostatic testing have any role in the evaluation of the young subject with mild hypertension?: an insight from the HARVEST study. Am. J. Hypertens. 10, 546–551 (1997).
Kario, K., Eguchi, K., Nakagawa, Y., Motai, K. & Shimada, K. Relationship between extreme dippers and orthostatic hypertension in elderly hypertensive patients. Hypertension 31, 77–82 (1998).
Nardo, C. J. et al. Descriptive epidemiology of blood pressure response to change in body position. The ARIC study. Hypertension 33, 1123–1129 (1999).
Kohara, K., Tabara, Y., Yamamoto, Y. & Miki, T. Orthostatic hypertension: another orthostatic disorder to be aware of. J. Am. Geriatr. Soc. 48, 1538–1539 (2000).
Yoshinari, M. et al. Orthostatic hypertension in patients with type 2 diabetes. Diabetes Care 24, 1783–1786 (2001).
Eguchi, K. et al. Greater change of orthostatic blood pressure is related to silent cerebral infarct and cardiac overload in hypertensive subjects. Hypertens. Res. 27, 235–241 (2004).
Hoshide, S. et al. Altered aortic properties in elderly orthostatic hypertension. Hypertens. Res. 28, 15–19 (2005).
Hoshide, S. et al. Orthostatic hypertension detected by self-measured home blood pressure monitoring: a new cardiovascular risk factor for elderly hypertensives. Hypertens. Res. 31, 1509–1516 (2008).
Wu, J. S., Yang, Y. C., Lu, F. H., Wu, C. H. & Chang, C. J. Population-based study on the prevalence and correlates of orthostatic hypotension/hypertension and orthostatic dizziness. Hypertens. Res. 31, 897–904 (2008).
Hirai, F. E., Moss, S. E., Klein, B. E. & Klein, R. Postural blood pressure changes and associated factors in long-term type 1 diabetes: Wisconsin Epidemiologic Study of Diabetic Retinopathy. J. Diabetes Complications 23, 83–88 (2009).
Fan, X. H. et al. Disorders of orthostatic blood pressure response are associated with cardiovascular disease and target organ damage in hypertensive patients. Am. J. Hypertens. 23, 829–837 (2010).
Fedorowski, A. et al. Orthostatic blood pressure response, carotid intima-media thickness, and plasma fibrinogen in older nondiabetic adults. J. Hypertens. 30, 522–529 (2012).
Barochiner, J. et al. Predictors of masked hypertension among treated hypertensive patients: an interesting association with orthostatic hypertension. Am. J. Hypertens. 26, 872–878 (2013).
Kario, K. et al. U-curve relationship between orthostatic blood pressure change and silent cerebrovascular disease in elderly hypertensives: orthostatic hypertension as a new cardiovascular risk factor. J. Am. Coll. Cardiol. 40, 133–141 (2002).
Thomas, R. J. et al. Positional change in blood pressure and 8-year risk of hypertension: the CARDIA Study. Mayo Clin. Proc. 78, 951–958 (2003).
Yatsuya, H. et al. Postural changes in blood pressure and incidence of ischemic stroke subtypes: the ARIC study. Hypertension 57, 167–173 (2011).
Hoshide, S. et al. Orthostatic hypertension: home blood pressure monitoring for detection and assessment of treatment with doxazosin. Hypertens. Res. 35, 100–106 (2012).
Kario, K. et al. Silent and clinically overt stroke in older Japanese subjects with white-coat and sustained hypertension. J. Am. Coll. Cardiol. 38, 238–245 (2001).
Pickering, T. G. et al. Call to action on use and reimbursement for home blood pressure monitoring: a joint scientific statement from the American Heart Association, American Society of Hypertension, and Preventive Cardiovascular Nurses Association. Hypertension 52, 10–29 (2008).
Parati, G. et al. European Society of Hypertension guidelines for blood pressure monitoring at home: a summary report of the Second International Consensus Conference on Home Blood Pressure Monitoring. J. Hypertens. 26, 1505–1526 (2008).
Imai, Y. et al. The Japanese Society of Hypertension guidelines for self-monitoring of blood pressure at home (second edition). Hypertens. Res. 35, 777–795 (2012).
Kario, K. et al. An α-adrenergic blocker titrated by self-measured blood pressure recordings lowered blood pressure and microalbuminuria in patients with morning hypertension: the Japan Morning Surge-1 Study. J. Hypertens. 26, 1257–1265 (2008).
Tochikubo, O., Ikeda, A., Miyajima, E. & Ishii, M. Effects of insufficient sleep on blood pressure monitored by a new multibiomedical recorder. Hypertension 27, 1318–1324 (1996).
Hui, X. et al. CKD and cardiovascular disease in the Atherosclerosis Risk in Communities (ARIC) Study: interactions with age, sex, and race. Am. J. Kidney Dis. 62, 691–702 (2013).
Carter, C. E. et al. Influence of urine creatinine concentrations on the relation of albumin:creatinine ratio with cardiovascular disease events: the Multi-Ethnic Study of Atherosclerosis (MESA). Am. J. Kidney Dis. 62, 722–729 (2013).
Kario, K. in Special Issues in Hypertension (eds Berbari, A. E. & Mancia, G.) 71–89 (Springer Inc., 2012).
Folkow, B. Physiological aspects of primary hypertension. Physiol. Rev. 62, 347–504 (1982).
Schiffrin, E. L. Vascular stiffening and arterial compliance. Implications for systolic blood pressure. Am. J. Hypertens. 17, 39S–48S (2004).
Rizzoni, D. et al. Morning rise of blood pressure and subcutaneous small resistance artery structure. J. Hypertens. 25, 1698–1703 (2007).
Nilsson, P. M. et al. Early vascular ageing in translation: from laboratory investigations to clinical applications in cardiovascular prevention. J. Hypertens. 35, 1517–1526 (2013).
Kario, K. Is vascular morning blood pressure surge in the elderly resistant to antihypertensives and more risky? Hypertension 60, e16 (2012).
Kario, K. Morning surge in blood pressure and cardiovascular risk: evidence and perspectives. Hypertension 56, 765–773 (2010).
Kario, K. et al. Nocturnal fall of blood pressure and silent cerebrovascular damage in elderly hypertensive patients. Advanced silent cerebrovascular damage in extreme dippers. Hypertension 27, 130–135 (1996).
Kario, K. et al. Stroke prognosis and abnormal nocturnal blood pressure falls in older hypertensives. Hypertension 38, 852–857 (2001).
Kario, K. et al. Morning surge in blood pressure as a predictor of silent and clinical cerebrovascular disease in elderly hypertensives: a prospective study. Circulation 107, 1401–1406 (2003).
Pickering, T. G., Eguchi, K. & Kario, K. Masked hypertension: a review. Hypertens. Res. 30, 479–488 (2007).
Kario, K. Proposal of a new strategy for ambulatory blood pressure profile-based management of resistant hypertension in the era of renal denervation. Hypertens. Res. 36, 478–484 (2013).
Mortensen, K. et al. Catheter-based renal sympathetic denervation improves central hemodynamics and arterial stiffness: a pilot study. J. Clin. Hypertens. (Greenwich) 14, 861–870 (2012).
Brandt, M. C. et al. Effects of renal sympathetic denervation on arterial stiffness and central hemodynamics in patients with resistant hypertension. J. Am. Coll. Cardiol. 60, 1956–1965 (2012).
Hart, E. C. et al. Translational examination of changes in baroreflex function after renal denervation in hypertensive rats and humans. Hypertension 62, 533–541 (2013).
Dauphinot, V. et al. Impaired baroreflex sensitivity and the risks of new-onset ambulatory hypertension, in an elderly population-based study. Int. J. Cardiol. 168, 4010–4014 (2013).
Okada, Y. et al. Morning blood pressure surge is associated with arterial stiffness and sympathetic baroreflex sensitivity in hypertensive seniors. Am. J. Physiol. Heart Circ. Physiol. 305, H793–H802 (2013).
Sanchez Gelós, D. F., Otero-Losada, M. E., Azzato, F. & Milei, J. Morning surge, pulse wave velocity, and autonomic function tests in elderly adults. Blood Press. Monit. 17, 103–109 (2012).
Ragot, S., Herpin, D., Siché, J. P., Poncelet, P. & Mallion, J. M. Relationship between short-term and long-term blood pressure variabilities in essential hypertensives. J. Hum. Hypertens. 15, 41–48 (2001).
Williams, B. Evaluating interventions to reduce central aortic pressure, arterial stiffness and morbidity--mortality. J. Hypertens. 30 (Suppl.), S13–S18 (2012).
Palatini, P. et al. Arterial stiffness, central hemodynamics, and cardiovascular risk in hypertension. Vasc. Health Risk Manag. 7, 725–739 (2011).
Kotsis, V., Stabouli, S., Karafillis, I. & Nilsson, P. Early vascular aging and the role of central blood pressure. J. Hypertens. 29, 1847–1853 (2011).
Nilsson, P. M. et al. Early vascular ageing in translation: from laboratory investigations to clinical applications in cardiovascular prevention. J. Hypertens. 31, 1517–1526 (2013).
Safar, M. E. Arterial aging--hemodynamic changes and therapeutic options. Nat. Rev. Cardiol. 7, 442–449 (2010).
Makowski, K. et al. Left ventricular diastolic dysfunction is associated with impaired baroreflex at rest and during orthostatic stress in hypertensive patients with left ventricular hypertrophy. J. Hum. Hypertens. 27, 465–473 (2013).
Milan, A. et al. Baroreflex sensitivity correlates with left ventricular morphology and diastolic function in essential hypertension. J. Hypertens. 25, 1655–1664 (2007).
Brisset, M. et al. Large-vessel correlates of cerebral small-vessel disease. Neurology 80, 662–669 (2013).
Briet, M., Pierre, B., Laurent, S. & London, G. M. Arterial stiffness and pulse pressure in CKD and ESRD. Kidney Int. 82, 388–400 (2012).
Muiesan, M. L. et al. Pulsatile hemodynamics and microcirculation: evidence for a close relationship in hypertensive patients. Hypertension 61, 130–136 (2013).
Caplan, L. R. Intracranial branch atheromatous disease: a neglected, understudied, and underused concept. Neurology 39, 1246–1250 (1989).
Tatsumi, S. & Yamamoto, T. An autopsied case of an apparent pontine branch atheromatous disease. Eur. Neurol. 63, 184–185 (2010).
Izzo, J. L. & Shykoff, B. E. Arterial stiffness: clinical relevance, measurement, and treatment. Rev. Cardiovasc. Med. 2, 29–34, 37–40 (2001).
Masoud, M., Sarig, G., Brenner, B. & Jacob, G. Orthostatic hypercoagulability: a novel physiological mechanism to activate the coagulation system. Hypertension 51, 1545–1551 (2008).
Hagan, R. D., Diaz, F. J. & Horvath, S. M. Plasma volume changes with movement to supine and standing positions. J. Appl. Physiol. 45, 414–417 (1978).
Lin, M. C. et al. Shear stress induction of the tissue factor gene. J. Clin. Invest. 99, 737–744 (1997).
Andrews, N. P., Goldstein, D. S. & Quyyumi, A. A. Effect of systemic α-2 adrenergic blockade on the morning increase in platelet aggregation in normal subjects. Am. J. Cardiol. 84, 316–320 (1999).
Ikeda, Y. et al. The role of von Willebrand factor and fibrinogen in platelet aggregation under varying shear stress. J. Clin. Invest. 87, 1234–1240 (1991).
Gkaliagkousi, E., Passacquale, G., Douma, S., Zamboulis, C. & Ferro, A. Platelet activation in essential hypertension: implications for antiplatelet treatment. Am. J. Hypertens. 23, 229–236 (2010).
Kario, K. et al. Morning blood pressure surge, morning platelet aggregation, and silent cerebral infarction in older Japanese hypertensive patients. J. Hypertens. 29, 2433–2439 (2011).
Kario, K. et al. Additional impact of morning haemostatic risk factors and morning blood pressure surge on stroke risk in older Japanese hypertensive patients. Eur. Heart J. 32, 574–580 (2011).
Smith, J. J., Porth, C. M. & Erickson, M. Hemodynamic response to the upright posture. J. Clin. Pharmacol. 34, 375–386 (1994).
Persson, P. B. Modulation of cardiovascular control mechanisms and their interaction. Physiol. Rev. 76, 193–244 (1996).
Gordon, R. D., Kuchel, O., Liddle, G. W. & Island, D. P. Role of the sympathetic nervous system in regulating renin and aldosterone production in man. J. Clin. Invest. 46, 599–605 (1967).
Kario, K., Schwartz, J. E. & Pickering, T. G. Changes of nocturnal blood pressure dipping status in hypertensives by nighttime dosing of α-adrenergic blocker, doxazosin: results from the HALT study. Hypertension 35, 787–794 (2000).
Kario, K. et al. Morning blood pressure surge and hypertensive cerebrovascular disease: role of the α-adrenergic sympathetic nervous system. Am. J. Hypertens. 17, 668–675 (2004).
Kario, K. Blood pressure variability in hypertension: a possible cardiovascular risk factor. Am. J. Hypertens. 17, 1075–1076 (2004).
Fujimoto, S., Mizuno, R., Saito, Y. & Nakamura, S. Clinical application of wave intensity for the treatment of essential hypertension. Heart Vessels 19, 19–22 (2004).
Benarroch, E. E. Postural tachycardia syndrome: a heterogeneous and multifactorial disorder. Mayo Clin. Proc. 87, 1214–1225 (2012).
Kario, K., Mitsuhashi, T. & Shimada, K. Neurohumoral characteristics of older hypertensive patients with abnormal nocturnal blood pressure dipping. Am. J. Hypertens. 15, 531–537 (2002).
Kario, K. et al. Development of a disaster cardiovascular prevention network. Lancet 378, 1125–1127 (2011).
Ketch, T., Biaggioni, I., Robertson, R. & Robertson, D. Four faces of baroreflex failure: hypertensive crisis, volatile hypertension, orthostatic tachycardia, and malignant vagotonia. Circulation 105, 2518–2523 (2002).
Acknowledgements
This author's work was supported by the Foundation for Development of the Community, Tochigi, Japan, by a Grant-in-Aid for Scientific Research (B 21390247) from The Ministry of Education, Culture, Sports, Science and Technology (MEXT), Japan, and by a MEXT-Supported Program for the Strategic Research Foundation at Private Universities, 2011-2015 “Cooperative Basic and Clinical Research on Circadian Medicine” (S1101022).
Author information
Authors and Affiliations
Ethics declarations
Competing interests
The author declares no competing financial interests.
Rights and permissions
About this article
Cite this article
Kario, K. Orthostatic hypertension—a new haemodynamic cardiovascular risk factor. Nat Rev Nephrol 9, 726–738 (2013). https://doi.org/10.1038/nrneph.2013.224
Published:
Issue Date:
DOI: https://doi.org/10.1038/nrneph.2013.224
This article is cited by
-
Clinical Significance of Salivary Alpha-amylase Activity in Patients With Parkinson’s Disease
Ageing International (2024)
-
Short-chain fatty acids in diseases
Cell Communication and Signaling (2023)
-
Consensus statement on the definition of orthostatic hypertension endorsed by the American Autonomic Society and the Japanese Society of Hypertension
Hypertension Research (2023)
-
Consensus statement on the definition of orthostatic hypertension endorsed by the American Autonomic Society and the Japanese Society of Hypertension
Clinical Autonomic Research (2023)
-
Prevalence of orthostatic hypertension and its association with cerebrovascular diagnoses in patients with suspected TIA and minor stroke
BMC Cardiovascular Disorders (2022)