Key Points
-
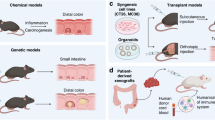
Colorectal cancer (CRC) is the second most common type of cancer in the Western world. Despite improvements in treatment, CRC recurs in up to 50% of patients and ultimately proves to be fatal.
-
CRC lends itself to various gene-therapy approaches, which include gene correction, virus-directed enzyme–prodrug therapy, immunogenetic manipulation and virotherapy.
-
CRC can be confined to organs (liver) or compartments (peritoneal cavity) for most of its natural history, allowing regional administration of the gene vector.
-
Gene-replacement trials have been initiated combining adenoviral TP53, which can act as a cytotoxic sensitizer, and conventional chemotherapy.
-
Virus-directed enzyme–prodrug therapy involves viral delivery of a transgene encoding an enzyme that can convert a non-toxic prodrug to a cytotoxic species. Early-phase clinical trials have been initiated with cytosine deaminase/fluorocytosine, herpes simplex virus thymidine kinase/gancyclovir and nitroimidazole reductase/CB1954.
-
Adenoviral transduction of allogeneic CRC cells with the gene encoding interleukin-2, vaccinia and fowl-pox vaccines aimed at inducing T-cell responses to carcinoembryonic antigen, and manipulation of MHC expression have all produced clinical immune responses in trials of immunogenetic therapies.
-
Virotherapy, with replication-competent adenoviruses engineered to proliferate in CRC cells with mutant p53 or RB, has been used to treat patients with hepatic metastases, in combination with 5-fluorouracil.
-
Randomized clinical trials are required to show the added value of gene therapy in the management of CRC; it is probable that combination gene therapy will be required to complement conventional chemotherapy.
Abstract
Colorectal cancer (CRC) is the second most common type of malignancy in Western nations. Improvements in surgical and radiotherapeutic techniques and the increased availability of new cytotoxic drugs have improved outcome, but 50% of patients still die from recurrent or metastatic disease. Several features of its natural history render CRC a good candidate for gene therapy. Techniques include gene replacement, virus-directed enzyme–prodrug therapy, immune manipulation and virotherapy, all of which have entered clinical trials.
Similar content being viewed by others
Main
Colorectal cancer (CRC) is a global concern, with approximately 950,000 new cases diagnosed and 500,000 deaths recorded worldwide in 2000 (Ref. 1). It is the second most common type of cancer in the Western world, and although there is an increasingly well-described genetic component (accounting for about 5% of disease burden), the dominant causative factors are environmental (diet and lifestyle)2,3,4. There is a recognized transition5 from premalignant adenomas to invasive carcinoma. It is therefore logical to screen asymptomatic populations, as early surgical intervention can completely remove premalignant adenomas, and early disease detection will lead to resection of stage I and II carcinomas, which carry a much better prognosis than stage III tumours (lymph-node metastasis). There have been significant improvements in reducing local recurrence rates from rectal cancer by optimizing surgical techniques (total mesorectal excision) and using radiotherapy, and overall survival rates have been improved by the use of systemic adjuvant chemotherapy (5–7% absolute improvement in 5-year survival rates in stage III colon cancer). However, despite these therapeutic advances, 20% of patients present with advanced disease, which is not amenable to surgery, and in those patients that are operated on, the cancer recurs in 50% of cases, providing a large number of patients with disease (metastatic and locally irresectable) who require chemotherapy6. Common sites of recurrence are the liver (80% of patients with CRC die from liver metastases) and locally within the peritoneal cavity.
Given the relatively low success rate of current treatments, several approaches are being taken to define new therapeutic avenues for CRC, in common with many other tumour types, including signal-transduction inhibitors, vaccines, antivascular drugs and gene therapy.
Each of these new treatments has a strong preclinical rationale, a mechanistic early-trials base and emerging evidence of clinical benefit. The other areas have been the subject of recent review7,8,9, but gene therapy deserves particular attention as it is the most logical extension of the information gained recently from the human genome project.
Gene therapy for CRC
There are several factors that make CRC a particularly attractive target for gene therapy. In common with other cancer types, a survival plateau has been reached with combinations of conventional cytotoxic drugs, increasing the demand for new approaches. In contrast to most cancers, which disseminate early in their natural history, CRC is often confined to specific organs (such as the liver) or compartments (such as the peritoneal cavity). As many as 30% of patients suffering from CRC have macroscopic relapses in the liver5, compared with, for example, breast cancer, in which metastases in multiple sites (such as bone, liver and lung) are much more likely to occur. This could offer an advantage through regional delivery of a genetic vector to maximize tumour exposure and minimize systemic toxicity. There is more information on the sequence of genetic and epigenetic events that characterize the transformation of colon epithelium to premalignant adenomas and then invasive carcinoma (Fig. 1) than there is for the development of other tumour types. These data can be used to construct rational gene vectors — for example, using tumour-suppressor pathways such as p53 and retinoblastoma (RB) — that might support cancer-selective virus replication. Similarly, there is a large database of CRC-associated ONCO-FETAL ANTIGENS10, the promoters of which might be used to restrict transgene expression to tumours and allow a further means of assessing tumour response to treatment. Finally, CRC and its adenoma precursors are more often amenable to biopsy of both early and late disease than other tumour types, which can add an important mechanistic element to proof-of-principle clinical trials, such as demonstration of viral replication, transgene expression, induction of apoptosis and tumour infiltration by lymphocytes.
There is a well-described sequence of mutational events that characterize the transition from normal colon epithelium to premalignant adenoma and then invasive adenocarcinoma. Loss of function of the adenomatous polyposis coli (APC) gene, which encodes a protein involved in cell adhesion and transcription, is found in up to 85% of all cases of colorectal cancer (CRC). KRAS, a GTP-ase that controls cell proliferation, is mutated in 50–60% of cases of CRC, and expression of the cell-adhesion transmembrane glycoprotein E-cadherin is downregulated in a similar number of patients. Mutations in the mismatch-repair genes MLH1 and MSH2 contribute to genetic instability. SMAD4 belongs to the SMAD family, which is involved in the transforming growth factor-β signalling pathway to suppress epithelial-cell growth. INK4A (also known as p16) is involved in the retinoblastoma tumour-suppressor pathway. TP53 mutations tend to be late events and increase the resistance of cancer cells to apoptosis. Reproduced from Ref. 56 © (2002) Oxford University Press.
Here, I provide some insight into current gene-therapy trials, highlighting the relevance of CRC as a target disease and how gene vectors have been adapted through understanding the molecular pathogenesis of CRC (Fig. 1). A summary of illustrative clinical trials for gene therapy of CRC that are in progress in the United States and the United Kingdom is provided in Box 1, showing the diversity of approaches, which can be subdivided into the following therapeutic strategies.
Gene correction or replacement
There is a large amount of literature detailing the genetic changes11,12,13 that occur in the adenoma–carcinoma transition, and their approximate sequence (Fig. 1). At its most basic level, gene-replacement therapy would involve the use of viral vectors to re-introduce wild-type genes for phenotypic correction. There are obvious stoichiometric flaws in this reasoning in that it would be impossible to correct all mutant genes (many of which are as yet undiscovered) in every cancer cell. However, common mutations in CRC, such as those of the tumour suppressor TP53 (45–60% of CRC cases) or the proto-oncogene KRAS (50–60%), have been assessed as therapeutic targets.
There are in vitro and in vivo data showing that exposure of CRC cells to recombinant adenovirus encoding wild-type p53 has a definite antiproliferative effect and can lead to increased survival following intratumoral administration to xenograft-bearing nude mice14. Further research has indicated that p53 replacement sensitizes CRC cells to conventional cytotoxic agents such as 5-fluorouracil (5-FU), presumably by reconstituting the apoptotic pathway15. Preclinical toxicology studies indicated that it was feasible to administer replication-deficient adenoviruses encoding p53, without evidence of significant toxicity, growth arrest or induction of apoptosis in normal cells. Venook et al.16 undertook a Phase I clinical trial of adenoviral administration of TP53 through hepatic arterial catheters to patients with CRC liver metastases. The virus was well tolerated, with the most frequent side effects being a short-lived pyrexia and ASYMPTOMATIC TRANSAMINITIS in 25% of patients. Of 12 patients who went on to receive arterial infusion of the cytotoxic drug 5-fluorodeoxyuridine, 11 had significant reduction (>50%) in tumour volume, paving the way for a randomized trial of hepatic arterial, infusional chemotherapy with or without adenoviral TP53.
KRAS has an important role in maintaining the uncontrolled proliferation that is characteristic of CRC and, therefore, its downregulation could be beneficial. Eggermont and colleagues17 developed a rat model of liver metastasis using a KRAS-mutated CRC cell line and showed that significant tumour regression occurred after hepatic arterial administration of a replication-deficient adenovirus encoding an intracellular antibody specific for KRAS.
Virus-directed enzyme–prodrug therapy (VDEPT)
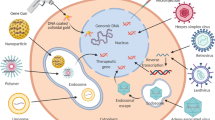
In this approach, cancer cells are transduced with an enzyme-encoding gene that, when transcribed, can convert an inactive, non-toxic prodrug to an effective cytotoxic species (Fig. 2). The ideal situation would be one in which the prodrug is completely inert and the activated cytotoxin is potent and short-lived (half-life of seconds), with the capacity to diffuse from the cancer cell in which it is produced to kill surrounding tumour cells (bystander effect) without entering the systemic circulation and causing side effects. There is a large body of work on the preclinical potential of three enzyme–prodrug systems for therapy of CRC, which was sufficiently compelling to warrant entry into clinical trials18,19,20,21. The earliest and most well-studied approach in VDEPT used thymidine kinase (TK) to activate ganciclovir, whereas nitroimidazole reductase (NTR)/CB1954 is a relatively new approach.
An adenovirus encoding the gene for an enzyme that can convert an inactive prodrug to a potent cytotoxic species is used to transfect tumour and normal cells. Examples of the enzymes used include thymidine kinase, which converts ganciclovir to phosphoganciclovir; cytosine deaminase, which converts 5-fluorocytosine to 5-fluorouracil; and nitroimidazole reductase, which converts CB1954 to a cytotoxic alkylating agent. Linkage of the gene to a tumour-specific promoter (such as the promoter for carcinoembryonic antigen or α-fetoprotein) ensures a higher level of enzyme transcription in tumour cells compared with normal cells. It is unlikely that the virus will infect all tumour cells, so an important aspect of virus-directed enzyme–prodrug therapy is the bystander effect. This involves diffusion of the activated cytotoxic drug from the cell expressing the enzyme to kill surrounding tumour cells. This might be mediated by diffusion through the lipid domain of the cell membrane or through gap junctions. If the activated drug has a short half-life, this further reduces the possibility of escape into the systemic circulation, which could cause side effects.
Thymidine kinase/ganciclovir. Herpes simplex virus (HSV)-TK phosphorylates ganciclovir to produce phosphoganciclovir. This undergoes further metabolism by cellular kinases to the triphosphate, which inhibits DNA synthesis through competition with dGTP. Mouse studies indicate a large bystander effect22, as treatment with ganciclovir induced significant tumour regression in a syngeneic CRC model in which only 10% of tumour cells expressed HSV-TK. A Phase I trial of escalating doses of a replication-deficient adenovirus encoding HSV-TK administered by direct inoculation to hepatic metastatic CRC nodules, combined with a fixed intravenous dose of ganciclovir, has been completed23. Side effects were mild (self-limiting fever and reversible transaminitis), and although there were no objective tumour responses, median survival for the group was 11–15 months, which compares favourably with historic controls (9–12 months).
Cytosine deaminase/5-fluorocytosine. Enzymatic conversion of 5-fluorocytosine (5-FC) by cytosine deaminase yields the cytotoxic agent 5-FU, which has been the main chemotherapeutic agent for CRC for 40 years. Huber et al.24 showed that there was a marked bystander effect in a human CRC xenograft model, in which significant tumour regression was seen following intraperitoneal delivery of 5-FC when only 2% of the total tumour population had been transfected with cytosine deaminase. Phase I trials have been undertaken with direct intratumoral inoculation of a replication-deficient adenovirus encoding cytosine deaminase and oral administration of 5-FC, which is already in general clinical use as an antifungal agent. Initial reports indicate that the virus is well tolerated, and biopsies have indicated cancer-associated expression of cytosine deaminase25.
NTR/CB1954. NTR converts CB1954 (5-(aziridin-1-YL)-2,4-dinitrobenzamide) into a cytotoxic alkylating agent, which causes double-strand DNA crosslinks and induction of apoptosis and necrosis. This effect is cell-cycle independent, killing cells at G0, and conventional alkylating-agent-resistant cell lines are susceptible to CB1954, which indicates that the CB1954-induced DNA adducts are less prone to excision repair than those produced by conventional cytotoxic agents such as cisplatin and cyclophosphamide. There is a good bystander effect — 99% cell kill when only 10% of an ovarian cancer cell population26 expresses NTR — and NTR-transfected CRC cells were 1,000–10,000-fold more sensitive to CB1954 than wild-type cells20. Chung-Faye et al.27 reported a dose-escalating Phase I trial of CB1954 in patients with mainly CRC, showing the safety of intravenous administration of the prodrug. Side effects included diarrhoea and asymptomatic transaminitis. In a separate, proof-of-principle Phase I trial28, an E1- and E3-deleted replication-incompetent adenovirus encoding NTR is being administered to patients with liver metastasis from CRC and primary hepatocellular carcinoma by ultrasound-guided intratumoral injection, 48 hours before they undergo liver resection to remove the tumour (Fig. 3). Immunocytochemical studies to detect NTR expression in the surgically resected tumour have shown a dose-related effect, with up to 25% of cancer cells expressing the therapeutic transgene28. Combination studies of the virus and prodrug have just begun28. Other enzyme–prodrug systems in preclinical development that are relevant for the treatment of CRC include cyclophosphamide/ cytochrome P450 (Ref. 29), carboxypeptidase G2/CMDA30 and carboxylesterase/irinotecan31.
Ultrasound-guided placement of the needle allows accurate administration of the virus to the cancer nodule. Forty-eight hours later — the optimal time for expression of the therapeutic transgene — the patients undergo resection of the segment/lobe of the liver harbouring the cancer. The pathologists cut multiple histological sections from the tumour for immunohistochemical staining for nitroimidazole reductase (NTR). Collection of venous blood samples at intervals after virus injection allows measurement of viral DNA and the neutralizing antibody response. For further experimental details, see Ref. 28.
Immunogenetic strategies
CRC is being increasingly considered as a target for immunogenetic therapy, whether antibody or cell mediated. Whereas most of the gene-therapy approaches described so far have involved regional treatment, the great promise in stimulating a tumour-specific immune response is that although it can be delivered locally, it can generate a signal that can be amplified (for example, by T-cell proliferation) and disseminated through the vasculature and tissues by lymphocyte trafficking, thereby exposing tumour cells to the cytotoxic mediator at sites distant from the area of gene-vector inoculation (Fig. 4). This is the largest and most diverse programme in CRC gene-therapy development and includes the delivery of lymphoproliferative cytokines and tumour antigens, and attempts to enhance the immunogenicity of autologous tumours.
This figure indicates the potential of immunogenetic therapy, which involves stimulation of the cellular immune system to recognize and destroy cancer cells. a | Transfection of isolated tumour cells with genes encoding a variety of cytokines — such as interleukin-2 (IL-2) and granulocyte–macrophage colony-stimulating factor (GM-CSF) — or co-stimulatory molecules (such as CD80 and CD86). The transfected genes increase the immunogenicity of the autologous tumour cells, which potentially display a range of tumour-specific antigens, and increase the likelihood of generating a tumour-specific cytotoxic T-lymphocyte (CTL) response. b | Ex vivo transfection of antigen-presenting cells (APCs) with a gene encoding a tumour-specific antigen (such as carcinoembryonic antigen, CEA), which is presented by major histocompatibility complex (MHC) class I molecules to antigen-specific CTLs via the T-cell receptor (TCR). Stimulated CTLs can seek out and destroy residual CEA-expressing tumour cells. GM-CSF can increase the activation of APCs and their migration into the tumour tissue.
Manipulating MHC expression. Most cases of advanced CRC (60–70%) downregulate expression of MAJOR HISTOCOMPATIBILITY COMPLEX (MHC) class I molecules as one means of escaping immune surveillance. Following on from positive results in trials of patients with melanoma32, a Phase I study was completed in which a plasmid encoding HLA-B7 (in a lipid envelope) was injected directly into hepatic metastatic nodules of CRC in HLA-B7-negative patients. Of the 15 patients involved, it was possible to detect the HLA-B7 transcript or protein in tumour biopsies in 12 individuals. A total of 50% of patients mounted an HLA-B7-specific cytotoxic T-lymphocyte (CTL) response. There were few side effects but no tumour-regression responses were recorded33.
Delivery of interleukin-2 (IL-2). IL-2 infusion has been studied extensively as a single agent and in combination with other cytokines, such as interferon (IFN)-α, in CRC. Administered intravenously or subcutaneously, IL-2 proved to be toxic (causing CAPILLARY LEAK SYNDROME), with little consistent antitumour activity. Nevertheless, there are many reports of the activity of IL-2 when introduced genetically into autologous tumour cells, fibroblasts or immune effector cells in syngeneic mouse models34,35, prompting further exploration in humans. Clinical trials have involved ex vivo transduction of autologous fibroblasts36 with IL-2 (which were then mixed with autologous irradiated CRC cells before subcutaneous injection), transduction of autologous cytokine-induced killer cells with IL-2 and direct intra-tumoral injection of IL-2-encoding plasmid–lipid complexes37. These trials have been characterized by evidence of increased immune reactivity (IL-2 detection, CTL responses, and induction of cytokines such as IFN-γ and GM-CSF (granulocyte–macrophage colony-stimulating factor)), but no evidence of tumour regression.
Carcinoembryonic antigen vaccines. Carcinoembryonic antigen (CEA) is a cell-surface glycoprotein that might have a role in cell motility, but also functions as a relatively tumour-specific onco-fetal antigen. It is overexpressed in 85% of CRC cases. The gene encoding CEA has been incorporated into various vectors (such as DNA–lipid complexes, vaccinia virus and canary pox virus) for use as a vaccine, often in combination with other immune effector molecules that might enhance the probability of anti-CEA immune responses (co-stimulatory molecules such as CD86; and adhesion molecules such as ICAM1 and LFA3). There is some evidence to indicate that point mutation in the antigen produces a more immunogenic form (CEA/6D)38 and this gene has been incorporated into third-generation avian pox viruses. Multiple Phase I and II trials have been initiated and completed, with more than 100 patients treated. The vaccines38,39,40,41,42,43,44 are well tolerated and are most often delivered as a vaccinia prime followed by canary pox boost, sometimes with co-administration of subcutaneous GM-CSF. An HLA-A2-restricted epitope of CEA has been identified, allowing highly specific CTL responses after vaccination to be shown. Once again, there was no obvious correlation between immune end points and clinical outcome, and the vaccines have not been shown to be effective for the management of advanced CRC. One obvious step forward would be to take the immunogenetic vaccine strategy into an adjuvant setting with minimal residual disease — following surgical resection of the tumour and post-operative chemotherapy when tumour volume would be at its lowest level — but which vaccine would be the best to take forward? Clinical investigators had hoped that they could use the strength and duration of the specific immune response (such as epitope-specific CTL counts) to create a hierarchy of competing vaccines and use these immune data to select the optimal vaccine to enter a large trial (requiring up to 3,000 patients). However, the current clinical-trial database does not support this sort of ranking exercise.
Virotherapy
Three decades of clinical trials have used a wide range of attenuated, oncolytic viruses to treat cancer, such as adenoviruses, mumps virus, vaccinia virus, myxovirus and West Nile virus45. Increased understanding of the viral genes that are necessary for cellular replication led to successful attempts to engineer a degree of tumour selectivity. Deletion of the adenoviral gene encoding E1A-CR2, which inactivates RB-family members, confers replicative selectivity for cancer cells with defects in the RB pathway46. Loss of E1B, which normally binds to and inhibits p53 in complex with E40RF6 protein, produces an adenovirus (dl1520) that preferentially replicates in cancer cells with mutant or deleted p53 (Ref. 47). This dl1520 virus might have some p53-independent replication competency, but, in general, there is a consistent, significant differential cell kill of cancer cells compared with normal cells.
The dl1520 virus has been administered to more than 300 patients with a range of cancer types (such as head and neck, colorectal and lung cancers). Trials in CRC have been carried out predominantly by intrahepatic arterial administration. This makes use of the liver's dual blood supply (portal vein and hepatic artery) and the knowledge that hepatic metastatic CRC nodules derive their blood supply from the hepatic artery, which allows the selective delivery of therapeutics. This can be further enhanced by vasoactive agents, such as angiotension II, that shunt blood from normal liver to the tumour. Having completed a Phase I trial48 to determine the dose of dl1520 that could be administered via the hepatic artery in combination with intravenous chemotherapy with 5-FU (in combination with the folic-acid derivative leucovorin), a Phase II trial was undertaken49. Twenty-seven patients were treated with hepatic arterial infusion of dl1520 on day 1 and 8, and thereafter, starting on day 22 in combination with intravenous 5-FU and leucovorin. Repeated viral infusions were possible. Two patients suffered reversible jaundice; seven (25%) patients showed tumour regression, nine (33%) patients had stable disease and the remaining eleven (42%) patients progressed. This study was too small to make any definite predictions about the efficacy of combination chemotherapy, but it did prove that hepatic arterial administration of a replication-competent virus was both feasible and safe, could be combined with conventional chemotherapy and could be repeated, with evidence of virus replication in vivo despite a strong host immune response and increased neutralizing antibody titres.
The problem of tumour tropism
Clinical gene-therapy trials for CRC reported so far have failed to show significant therapeutic efficacy, although most of them have recruited patients with advanced, drug-refractory disease. By contrast, in cell lines and animals, remarkable results, including complete regression of the tumour, have been shown. An important problem causing this discrepancy is the poor targeting selectivity of the vectors in humans, leading to low efficiency of gene transfer to tumour cells.
To confer tumour tropism on the vectors used for gene therapy of CRC, several strategies have been explored, including the use of tumour-specific promoters such as those of CEA or TCF (T-cell transcription factor, which is dysregulated in adenomatous polyposis coli ( APC )-mutated CRC cells) and delivery systems based on tumour-selective ligands such as fibroblast growth factor 2 (FGF2).
The use of the CEA promoter to express the transgene of interest provides a considerable degree of tumour specificity, as only cells expressing CEA (mainly CRC cells) would activate the promoter, but such promoters are often too weak for clinically effective gene therapy50. Development of stronger and more tumour-specific promoters is necessary and a Phase I trial (Box 1) of NTR under the control of the human telomerase promoter is planned51.
Fisher et al.52 reported a covalent coating and re-targeting strategy using adenoviral vectors in gene therapy. Adenovirus is often neutralized by pre-existing antibodies, or it binds to coxsackie and adenovirus receptors (CAR) that are distributed over a wide range of tissues, preventing tumour-selective and efficient delivery of adenoviral vector. When modified adenovirus is coated with a multivalent hydrophilic polymer to which FGF2 is covalently linked, CAR-independent binding of the virus to tumour cells bearing FGF2 receptors occurs. This strategy can be applied to many types of cancer, including those of colorectal origin, by the incorporation of specific targeting ligands into the vector.
To identify such tumour-specific ligands for CRC, a biopanning procedure using a peptide PHAGE DISPLAY library has been used in the vasculature of resected CRC, immediately after resection. PANNING with the library against specific receptors, cells or tissue allows identification of peptide sequences that bind to them. Using this technology, we identified a peptide that binds to FGF2 receptors expressed on CRC cells: the peptide motif, Met-Gln-Leu-Pro-Leu-Ala-Thr (MQLPLAT). Use of MQLPLAT to target polyelectrolyte gene-delivery vectors achieved 40-fold greater transgene transduction in CRC cells compared with the use of non-targeted vectors53.
Future directions
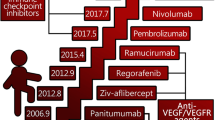
So far, clinical trials of gene therapy for CRC have focused predominantly on obtaining safety data and proof-of-principle, supporting the hypotheses underpinning development of the specific gene therapeutic agent. Side effects are mild and experimental measurements tend to indicate transgene expression, prodrug activation or specific T-cell activation; however, there has been relatively little evidence of tumour regression or other signs of efficacy. This relates predominantly to delivery and expression of an adequate dose of the relevant therapeutic gene. Building on clinical experience with virtually all other anticancer agents, it would seem probable that combination therapy, using different mechanisms of inducing CRC cell kill, is the most likely route to enhanced antitumour responses, improved quality of life and prolonged survival. Trials combining gene therapy and chemotherapy have been described earlier, but preliminary results of two large clinical studies indicate that there is likely to be an important role for anti-vascular endothelial growth factor (Avastin)54 and anti-epidermal growth factor (Cituximab)55 monoclonal antibodies in the management of advanced CRC, supporting the emergence of multi-modality therapy.
Although the search for new vectors (viral and non-viral), novel transgenes and more selective targeting moieties will continue, it is worthwhile considering what sort of clinical initiative might be undertaken to combine existing gene therapies at the most appropriate disease stage. I propose an adjuvant trial (Fig. 5) in which a replication-competent adenovirus engineered to deliver synergistic enzyme–prodrug systems (NTR/CB1954; cytosine deaminase/5-FC) and the gene encoding IL-2 would be administered via a portal venous catheter to hepatic micrometastases. Simultaneously, subcutaneous vaccination would commence using avipox-CEA and GM-CSF to generate an immune response to CEA. This could be integrated, using factorial trial design, with conventional systemic chemotherapy. This is not a trivial undertaking and such a trial would need to involve about 3,000 patients to demonstrate clinically meaningful improvements in overall survival. This is an order of magnitude larger than any existing trial of gene therapy but gives a sense of the challenges that are ahead in bringing gene therapy into mainstream treatment for CRC.
This trial scheme is an example of the potential for future investigation, using treatment of early-stage colorectal cancer (CRC) as the model. It combines current approaches to gene therapy that have distinct mechanisms of action. Replication-competent adenoviruses encoding enzymes and the prodrugs that they activate are administered via the portal vein, and an anti-CEA vaccination is given subcutaneously. By initiating therapy immediately after surgery, when residual tumour burden is minimal and there are fewer drug-resistant tumour-cell clones, there is an increase in the possibility of CRC cure. Avipox-CEA, fowl pox virus encoding carcinoembryonic antigen; CD, cytosine deaminase; 5-FC, 5-fluorocytosine; GM-CSF, granulocyte–macrophage colony-stimulating factor; IL-2, interleukin-2; NTR, nitroimidazole reductase; RB, retinoblastoma.
References
Ferlay, J., Bray, F., Pisani, P. & Parkin, D. M. Globocan 2000. Cancer incidence, mortality and prevalence worldwide, version 1.0. IARC Cancer Base No. 5. (IARC Press, Lyon, 2001).
Fearon, E. R. & Vogelstein, B. A genetic model for colorectal tumorigenesis. Cell 61, 759–767 (1990). Excellent summary of the pattern of mutations that characterize the transition from normal colon epithelium to adenoma and then adenocarcinoma.
Bodmer, W. F. et al. Localisation of the gene for familial adenomatous polyposis on chromosome 5. Nature 328, 614–616 (1987).
Cottrell, S., Bicknell, D., Kaklamanis, L. & Bodmer, W. F. Molecular analysis of APC mutations in familial adenomatous polyposis and sporadic colon carcinomas. Lancet 340, 626–630 (1992).
Midgley, R. & Kerr, D. J. Seminar in colorectal cancer. Lancet 353, 391–399 (1999). General background introduction to the natural history and modern management of colorectal cancer.
Douillard, J. Y. et al. Irinotecan combined with fluorouracil compared with fluorouracil alone as first-line treatment for metastatic colorectal cancer: a multicentre randomised trial. Lancet 355, 1041–1047 (2000).
Todryk, S. M., Chong, H., Vile, R. G., Pandha, H. & Lemoine, N. R. Can immunotherapy by gene transfer tip the balance against colorectal cancer? Gut 43, 445–449 (1998).
Mendelsohn, J. & Baselga, J. The EGF receptor family as targets for cancer therapy. Oncogene 19, 6550–6565 (2000).
Papamichael, D. Prognostic role of angiogenesis in colorectal cancer. Anticancer Res. 21, 4349–4354 (2001).
Thompson, J. A., Grunert, F. & Zimmermann, W. Carcinoembryonic antigen gene family: molecular biology and clinical perspectives. J. Clin. Lab. Anal. 5, 344–366 (1991).
Kinzler, K. W. & Vogelstein, B. The colorectal cancer gene hunt: current findings. Hosp. Prac. 27, 51–58 (1992).
Kinzler, K. W. & Vogelstein, B. Lessons from hereditary colorectal cancer. Cell 87, 159–170 (1996).
Houlston, R. S. & Tomlinson, I. P. M. Polymorphisms and colorectal tumour risk. Gastroenterology 121, 282–301 (2001).
Harris, M. P. et al. Adenovirus-mediated p53 gene transfer inhibits growth of human tumour cells expressing mutant p53 protein. Cancer Cell Ther. 3, 121–130 (1996).
Opalka, B., Dickopp, A. & Kirch, H. C. Apoptotic genes in cancer therapy. Cells Tissues Organs 172, 126–132 (2002).
Venook, P. et al. Gene therapy of colorectal liver metastasis using recombinant adenovirus encoding wt p53 (SCH58500) via hepatic artery infusion: a phase I study. Proc. Am. Soc. Clin. Oncol. 17, 431 (1998).
Van Etten, B. et al. Prerequisites for effective adenovirus mediated gene therapy of colorectal liver metastases in that rat using an intracellular neutralizing antibody of p21-Ras. Br. J. Cancer 86, 436–442 (2002).
Chung-Faye, G. A. et al. In vivo gene therapy for colon cancer using adenovirus-mediated, transfer of the fusion gene cytosine deaminase and uracil phosphoribosyltransferase. Gene Ther. 8, 1547–1554 (2001).
Rogulski, K. R., Kim, J. H., Kim, S. H. & Freytag, S. O. Glioma cells transduced with an Echerichia coli CD/HSV-1 TK fusion gene exhibit enhanced metabolic suicide and radiosensitivity. Hum. Gene Ther. 8, 73–85 (1997).
Green, N. K. et al. Sensitization of colorectal and pancreatic cancer cell lines to the prodrug 5 (aziridin-1-yl)-2, 4-dinitrobenzamide (CB1954) by retroviral transduction and expression of the E. coli nitroreductase gene. Cancer Gene Ther. 4, 229–238 (1997).
Green, N. K. et al. Gene therapy for cancer: in vivo killing of tumour cells expressing E-coli nitroreductase following administration of the prodrug CD1954. Gene Ther. 6, 33 (1999).
Burrows, F. J. et al. Purified herpes simplex virus thymidine kinase retroviral particles: III. Characterisation of bystander killer mechanisms in transfected tumour cells. Cancer Gene Ther. 9, 87–95 (2002).
Sung, M. W. et al. Intratumoural adenovirus-mediated suicide gene transfer for hepatic metastases from colorectal adenocarcinoma: results of a phase I clinical trial. Mol. Ther. 4, 182–191 (2001).
Huber, B. E., Austin, E. A., Richards, C. A., Davis, S. T. & Good, S. S. Metabolism of 5-fluorocytosine to 5-fluorouracil in human colorectal tumour cells transduced with cytosine deaminase gene: significant antitumour effects when only a small percentage of tumour cells express cytosine deaminase. Proc. Natl Acad. Sci. USA 91, 8302–8306 (1994). Early demonstration of the utility of virus-directed enzyme–prodrug therapy and the importance of the bystander effect in vivo.
Crystal, R. G. et al. Phase I study of direct administration of replication deficient adenovirus vector containing the E. coli cytosine deaminase gene to metastatic colon carcinoma of the liver in association with the oral administration of the pro-drug 5-fluorocytosine. Hum. Gene Ther. 8, 985–1001 (1997).
McNeish, I. A. et al. Virus directed enzyme prodrug therapy for ovarian and pancreatric cancer using retrovirally delivered E. coli nitroreductase and CB1954. Gene Ther. 5, 1061–1069 (1998).
Chung-Faye, G. et al. Virus-directed, enzyme prodrug therapy with nitroimidazole reductase: a phase I and pharmacokinetic study of its prodrug, CB1954. Clin. Cancer Res. 7, 2662–2668 (2001).
Palmer, D. H. et al. Virus-directed enzyme prodrug therapy (VDEPT) clinical trials with adenoviral nitroimidazole reductase (ad–ntr). Br. J. Cancer 86, S30 (2002).
Chang, T. K., Weber, G. F., Crespi, C. L. & Waxman, D. J. Differential activation of cyclophosphamide and ifosphamide by cytochromes P-450 2B and 3A in human liver microsomes. Cancer Res. 53, 5629–5637 (1993).
Marais, R., Spooner, R. A., Light, Y., Martin, J. & Springer, C. J. Gene-directed enzyme prodrug therapy with a mustard prodrug/carboxypeptidase G2 combination. Cancer Res. 56, 4735–4742 (1996).
Kojima, A., Hackett, N. R., Ohwada, A. & Crystal, R. G. In vivo human carboxylesterase cDNA gene transfer to activate the prodrug CPT-11 for local treatment of solid tumours. J. Clin. Invest. 101, 1789–1796 (1998).
Nabel, G. J. et al. Direct gene transfer with DNA-liposome complexes in melanoma: expression, biologic activity, and lack of toxicity in humans. Proc. Natl Acad. Sci. USA 90, 11307–11311 (1993).
Rubin, J. et al. Phase I study of immunotherapy of hepatic metastases of colorectal carcinoma by direct gene transfer of an allogeneic histocompatability antigen, HLA-B7. Gene Ther. 4, 419–425 (1997).
Fakhrai, H. et al. Cytokine gene therapy with interleukin-2 transduced fibroblasts: effects of IL-2 dose on anti-tumour immunity. Hum. Gene Ther. 6, 591–601 (1995).
Galanis, E. et al. Immunotherapy of advanced malignancy by direct gene transfer of an interleukin-2 DNA/DMRIE/DOPE lip complex: phase I/II experience. J. Clin. Oncol. 17, 3313–3323 (1999).
Sobol, R. E. et al. Interleukin 2 gene therapy of colorectal carcinoma with autologous irradiated tumour cells and genetically engineered fibroblasts: a phase I study. Clin. Cancer Res. 5, 2359–2365 (1999).
Schmidt-Wolf, I. G. et al. Phase I clinical study applying autologous immunological effector cells transfected with the interleukin-2 gene in patients with metastatic renal cancer, colorectal cancer and lymphoma. Br. J. Cancer 81, 1009–1016 (1999).
Tsang, K. Y. et al. Generation of human cytotoxic T cells specific for human carcinoembryonic antigen epitopes from patients immunized with recombinant vaccinia-CEA vaccine. J. Natl Cancer Inst. 87, 982–990 (1995). High-quality Phase I trial of a carcinoembryonic antigen (CEA) vaccine, showing that it was possible to detect human cytotoxic T cells specific for CEA epitopes.
Conry, R. M. et al. Phase I trial of a recombinant vaccinia virus encoding carcinoembryonic antigen in metastatic adenocarcinoma: comparison of intradermal versus subcutaneous administration. Clin. Cancer Res. 5, 2330–2337 (1999).
Conry, R. M. et al. Human autoantibodies to carcinoembryonic antigen (CEA) induced by a vaccinia-CEA vaccine. Clin. Cancer Res. 6, 34–41 (2000).
Hodge, J. W., McLaughlin, J. P., Kantor, J. A. & Scholm, J. Diversified prime and boost protocols using recombinant vaccinia virus and recombinant non-replicating avian pox virus to enhance T-cell immunity and antitumour responses. Vaccine 15, 759–768 (1997).
Marshall, J. L. et al. Phase I study in cancer patients of a replication-defective avipox recombinant vaccine that expresses human carcinoembryonic antigen. J. Clin. Oncol. 17, 332–337 (1999).
Zhu, M. Z., Marshal, J., Cole, D., Scholm, J. & Tsang, K. Y. Specific cytolytic T-cell responses to human CEA from patients immunized with recombinant avipox-CEA vaccine. Clin. Cancer Res. 6, 24–33 (2000).
Horig, H. et al. Phase I clinical trial of a recombinant canarypoxvirus (ALVAC) vaccine expressing human carcinoembryonic antigen and the B7.1 co-stimulatory molecule. Cancer Immunol. Immunother. 49, 504–514 (2000).
Kirn, D. H. & McCormick, F. Replicating viruses as selective cancer therapeutics. Mol. Med. Today 2, 519–527 (1996).
Smith, E. R. & Chiocca, E. A. Oncolytic viruses as novel anticancer agents: turning one scourge against another. Exp. Opin. Invest. Drugs 9, 311–327 (2000).
Bischoff, J. R. et al. An adenovirus mutant that replicates selectively in p53-deficient human tumour cells. Science 274, 373–376 (1996). First description of tumour-specific replication-competent adenovirus in cancer cells with mutant TP53.
Reid, T. et al. Intra-arterial administration of a replication-selective adenovirus (dl1520) in patients with colorectal carcinoma metastatic to the liver: a phase I trial. Gene Ther. 8, 1618–1626 (2001).
Reid, T. et al. Hepatic arterial infusion of replication-selective adenovirus (dl1520): phase II viral, immunologic and clinical endpoints. Cancer Res. 62, 6070–6079 (2002).
Richards, C. A., Austin, E. A. & Huber, B. E. Transcriptional regulatory sequences of carcinoembryonic antigen: identification and use with cytosine deaminase for tumour-specific gene therapy. Hum. Gene Ther. 6, 881–893 (1995).
Bisland, A. E. et al. Selective ablation of human cancer cells by telomerase specific adenoviral suicide gene therapy vectors expressing bacterial nitroreductase. Oncogene 22, 370–380 (2003).
Fisher, K. D. et al. Polymer-coated adenovirus permits efficient retargeting and evades neutralizing antibodies. Gene Ther. 8, 341–348 (2001).
Maruta, F. et al. Identification of FGF receptor-binding peptides for cancer gene therapy. Cancer Gene Ther. 9, 543–552 (2002).
Benson, A. B. et al. Bevacizumab (anti–VEGF) plus FOLFOX 4 in previously treated advanced colorectal cancer patients. Proc. Am. Soc. Clin. Oncol. A39, A975 (2003).
Humbley, Y. et al. Cituximab alone or in combination with irinotecan in patients with epidermal growth factor receptor positive, irinotecan refractory colorectal cancer. Proc. Am. Soc. Clin. Oncol. A39, A1012 (2003).
Fearnhead, N. S., Wilding, J. L. & Bodmer, W. F. in Advances in Colorectal Cancer British Medical Bulletin Vol. 64 (eds Kerr, D. J., Bodmer, W. F., McArdle, C. S. & Pignatelli, M.) 27–43 (Oxford Univ. Press, Oxford, 2002).
Author information
Authors and Affiliations
Glossary
- ONCO-FETAL ANTIGENS
-
Cell-surface-associated antigens that are normally expressed during specific phases of embryogenesis but are not expressed at significant levels in adults. These can be dysregulated during carcinogenesis.
- ASYMPTOMATIC TRANSAMINITIS
-
The increase of liver enzymes (such as aspartate and alanine aminotransferases) that are measurable in the blood in response to tissue damage.
- MAJOR HISTOCOMPATIBILITY COMPLEX
-
(MHC). A genetic region encoding proteins that are involved in antigen presentation to T cells. MHC class I molecules bound to peptide are recognized by the T-cell receptors of CD8+ T cells.
- CAPILLARY LEAK SYNDROME
-
Involves damage to vascular endothelial cells, and the extravasation of fluids and proteins, resulting in weight gain and, in its most severe form, kidney damage and pulmonary oedema.
- PHAGE DISPLAY
-
Technology for displaying a protein (or peptide) on the surface of a bacteriophage, which contains the gene(s) that encodes the displayed protein(s), thereby physically linking the genotype and phenotype.
- PANNING
-
The process of separating target-binding clones from nonbinding clones for a phage display library.
Rights and permissions
About this article
Cite this article
Kerr, D. Clinical development of gene therapy for colorectal cancer. Nat Rev Cancer 3, 615–622 (2003). https://doi.org/10.1038/nrc1147
Issue Date:
DOI: https://doi.org/10.1038/nrc1147
This article is cited by
-
β-carboline derivative Z86 attenuates colorectal cancer cell proliferation and migration by directly targeting PI3K
Natural Products and Bioprospecting (2024)
-
CRISPR/Cas9: a powerful tool in colorectal cancer research
Journal of Experimental & Clinical Cancer Research (2023)
-
Assessment of murine colorectal cancer by micro-ultrasound using three dimensional reconstruction and non-linear contrast imaging
Molecular Therapy - Methods & Clinical Development (2016)
-
Autophagy inhibition sensitizes WYE-354-induced anti-colon cancer activity in vitro and in vivo
Tumor Biology (2016)
-
Clinical outcomes of active specific immunotherapy in advanced colorectal cancer and suspected minimal residual colorectal cancer: a meta-analysis and system review
Journal of Translational Medicine (2011)