Abstract
Menthol cigarettes are likely associated with greater risks of smoking dependence than non-menthol cigarettes. We sought to test the hypothesis that menthol increases the rate of brain nicotine accumulation (BNA) during smoking and thereby enhances its addictive effects. In a counter-balanced cross-over design, 10 menthol and 9 non-menthol smokers (10 females and 9 males; mean age 44.3) underwent two study phases. In each phase, the participant smoked exclusively either menthol or non-menthol research cigarettes for approximately 1 week prior to a positron emission tomography (PET) scan session, during which the subject’s head was scanned following inhalation of a single puff of smoke from a cigarette containing 11C-nicotine. No differences in initial slope, Cmax, area under curve (AUC), and T1/2 of BNA were found between menthol and non-menthol cigarettes across all subjects; however, menthol relative to non-menthol cigarettes were associated with steeper initial slopes in men (p=0.008). Unexpectedly, women had faster BNA as indicated by greater values of the initial slope, Cmax, AUC, and shorter T1/2 than men (all ps<0.04). The rates of BNA were significantly correlated with ratings of smoking motivations of getting a ‘rush’, getting relaxing effects and marginally with alleviation of craving. These results do not provide strong support for the putative role of menthol in enhancing BNA, although further studies should explore the apparent effect of menthol on BNA in men. Fast BNA during smoking and preference of sensory properties of menthol cigarettes may independently or jointly contribute to smoking dependence among women.
Similar content being viewed by others
INTRODUCTION
Menthol cigarettes represent approximately one-fourth of all cigarettes sold in the United States (Giovino et al, 2004). Menthol cigarette use is more common among smokers who are female, African American, young, and have low income (Food and Drug Administration, 2013). A recent comprehensive review by the U.S. Food and Drug Administration (FDA) has concluded that menthol cigarettes are likely associated with greater risks of smoking dependence and thereby a greater public health threat than non-menthol cigarettes (Food and Drug Administration, 2013). Despite substantial data to support this conclusion, there remain major gaps in knowledge of neuropharmacological mechanisms underlying the association of menthol and enhanced addictive effects of cigarette smoking. Among them, one unaddressed question is whether menthol enhances the rate of brain nicotine accumulation (BNA) during smoking, which is critical for its reinforcing and addictive properties (Benowitz, 1990; Henningfield and Keegan, 1993; Le Foll et al, 2007).
Menthol reduces the harshness and irritation of cigarette smoke owing to its cooling (Eccles, 1994) and local anesthetic (Green, 1992) effects in the respiratory tract of smokers. With these effects, menthol in cigarettes might allow smokers to puff more intensively as well as inhale deeper and thereby have greater and faster intake of nicotine than that from non-menthol cigarettes. Moreover, menthol may increase breath-holding time (Sloan et al, 1993). However, overall mixed findings have been reported on the effects of menthol on smoking topography and levels of nicotine exposure (Jarvik et al, 1994; McCarthy et al, 1995; Ahijevych and Parsley, 1999; Food and Drug Administration, 2013).
Aside from its putative effects on smoking intensity, menthol may enhance nicotine permeability in the respiratory tract. Menthol increased transdermal (Kobayashi et al, 1994; Kunta et al, 1997) and transbuccal (Shojaei et al, 1999) permeability of various drugs. Recently, menthol has been demonstrated to increase the penetration of nicotine through porcine oral mucosa (Squier et al, 2010). These findings are supportive of a proposition that menthol in cigarettes may increase the permeability of nicotine across the lungs (Jarvik et al, 1994; McCarthy et al, 1995; Clark et al, 1996; US Department of Health and Human Services, 1998). On the basis of the evidence for this proposition, we further hypothesized that menthol would enhance the rate of BNA by facilitating pulmonary absorption and transfer of smoke-delivered nicotine into the blood.
In this study, we sought to directly test the hypothesis that menthol increases the rate of BNA during smoking using high temporal resolution positron emission tomography (PET) and menthol and non-menthol cigarettes containing 11C-nicotine. Additional analyses were conducted to examine the role of individual variables (eg, sex and menthol preference) in moderating the effects of menthol on BNA kinetics and smoking behavior, and to assess the associations of the kinetics parameters with motivations of smoking. PET with 11C-nicotine loaded into cigarettes is currently the only technique available to directly assess the dynamics of smoking-delivered nicotine in the human brain. The approach was first used to characterize nicotine lung deposition (Lunell et al, 1996) and has recently been validated by two studies which demonstrated the rapid rates of BNA and their association with lung nicotine kinetics after smoke inhalation (Berridge et al, 2010; Rose et al, 2010).
MATERIALS AND METHODS
Participants
Participants were recruited through television advertisements and flyers. Inclusion criteria consisted of 18–65 years of age, being generally healthy, smoking⩾8 cigarettes per day (CPD), and expired CO of ⩾10 ppm. Exclusion criteria included respiratory disorders, psychiatric disorders, alcohol abuse, testing positive for illicit drug use, using non-cigarette tobacco or nicotine products, and presence of contraindications for PET scan (eg, pregnancy and lactation). Because Basic cigarettes (Philip Morris, USA) were chosen as the research cigarettes, individuals who smoked Basic brand cigarettes in the past 6 months were also excluded to avoid likely brand preference-related biases.
Among 28 subjects enrolled, 10 menthol and 9 non-menthol smokers completed the study (Table 1) and were included for the current analysis. Nine subjects dropped out because of reasons including scheduling conflict (n=1), no show (n=2), non-compliance with study protocol (n=2), anxiety or other unsuitable mental status at PET scan sessions (n=2), and technical difficulties with PET scan (n=2). The study protocol was approved by the Duke University Health System Institutional Review Board. All participants provided informed consent at the screening visit.
Study Design
Smokers participated in two study phases in a cross-over design. Each phase consisted of an approximately 1-week adaptation period during which the participant smoked exclusively one type (menthol or non-menthol) of research cigarettes with smoking topography recorded via a pocket device, a behavioral evaluation session, and a PET scan session using the same type of cigarette but containing 11C-nicotine to measure BNA kinetics after smoke inhalation. The order of the two phases was randomized and counter-balanced across participants. The research cigarettes consisted of Basic Gold and Basic Menthol Gold 100’s hard pack cigarettes which had identical FTC yield of nicotine (0.8 mg), tar (11 mg), and CO (14 mg). The smoking adaptation periods allowed subjects to get accustomed to the unfamiliar research cigarettes so that they could inhale the smoke from them during PET scans without complications, such as incomplete inhalation and coughing, which would affect PET data acquisition and interpretation. Topography recording was implemented to assess possible differences in menthol and non-menthol cigarette smoking and also to promote participant compliance with smoking the research cigarettes during the adaptation periods.
Procedure
Smoking history including years of smoking and number of CPD was collected using a general questionnaire at the screening visit. Participants also completed the Fagerström Test of Nicotine Dependence (Heatherton et al, 1991) and a 13-item Reasons to Smoke questionnaire (see Supplementary Materials). Expired CO was measured to ascertain smoke inhalation.
Prior to the beginning of Phase 1, participants practiced smoking the research cigarettes via a pocket smoking device (CReSS, Borgwaldt KC, Richmond, VA) at the first study visit (data not analyzed). They were instructed to smoke one menthol and one non-menthol research cigarette 40 min apart through the CReSS device. Expired CO concentrations were measured immediately before and 1 min after smoking each cigarette. Participants also rated their sensory experience following smoking each of the cigarettes on the Duke Sensory Questionnaire (Behm and Rose, 1994). At the end of the visit, participants practiced taking and inhaling puffs in the supine position from a smoking delivery device identical to that which was later used in the PET sessions. They were also provided with research cigarettes of the assigned type (menthol or non-menthol; daily amount equivalent to 115% of self-reported numbers of usual brand CPD) along with smoking diary forms for their logging of numbers of CPD. They were asked to start smoking exclusively the assigned cigarettes and use the CReSS device on as many occasions as they could for about a week (5∼12 days) till the upcoming PET scan visit. A portable cigarette ashtray and Ziploc bags were also given to the subjects so that they could collect all cigarette butts smoked during the period of smoking adaptation. The collection of these butts, which differed in paper and font colors between the menthol and non-menthol cigarettes, was expected to ensure compliance. Research cigarettes and other study materials for Phase 2 were provided to the subjects following the first PET scan session.
Following the adaptation period during each phase, participants attended a lab visit on the day before the PET scan session. The procedure for these visits was the same as that for the first visit except that the participants first smoked a research cigarette of the type that they had been smoking during the preceding days and then a cigarette of the other type. Given a short plasma half-life of menthol (∼90 min), only a negligible fraction (⩽0.04%) of menthol from smoking the menthol cigarette during the lab visit (before 5 pm) would remain in the participant’s body at the time of PET scan on the following day (after 10 am) and therefore would have little impact on the PET scan following inhalation from a non-menthol cigarette. Additionally, smoking topography data and completed smoking diaries were collected at each of these visits.
PET Scanning Procedure
The PET scans were conducted using a GE Discovery VCT PET/CT scanner (GE Healthcare, Waukesha, WI, USA). The head of each participant was scanned for 12 min in a sequence of 25 1-s, 30 2-s, 120 3-s, and 70 4-s frames (field of view: 24.6 × 24.6 × 15.4 cm3, matrix size: 128 × 128 × 47). The scanning was initiated simultaneously while the participant took a puff of 30 ml smoke from a research cigarette containing 11C-nicotine followed by inhalation of the smoke with 550 ml air. Immediately before this scanning, each participant took five puffs (30 ml puff volume, 45 s interval) from a non-radioactively labeled cigarette of the same type. Thus, for the PET sessions with menthol cigarettes, a certain amount of menthol was present in the body of the participant during the inhalation of single-puff smoke from the labeled cigarette. After the dynamic head scanning, a full-body scan was conducted to measure total inhaled radioactivity. Smoke delivery during the PET sessions was achieved through a customized, programmable device. Immediately after a 30-ml puff of smoke was generated from the device, the subject was verbally instructed to press a button valve and take the puff from a Teflon tube containing the smoke.
11C-nicotine was synthesized following an established protocol (Halldin et al, 1992). Approximately 740 MBq 11C-nicotine, dissolved in 10 μl ethanol, was applied to the tip of the tobacco rod of the study cigarette. Both the tobacco rod and filter were shortened (to 10 mm and 5 mm, respectively) to ensure efficient 11C-nicotine delivery. After evaporation of the ethanol, the cigarette was placed in the combustion chamber of the smoke delivery device and ready for use.
PET Image Processing
PET image processing was conducted using PMOD (Version 3.17, PMOD Technologies, Adliswil, Switzerland). The head CT image from the second scan session was co-registered to that from the first session and then the same transformation parameters were applied for co-registration of the brain dynamic PET images. Individual whole-brain volume of interest was drawn on the average of time-averaged images from the two sessions and then applied to dynamic images. A cylinder-shaped volume of interest was generated to cover the entire body image of each subject. After decay correction to the brain scan start time, the radioactivity within the volume of interest was taken as the total dose of inhaled radioactivity. Whole-brain 11C-nicotine radioactivity over time was calculated as a percentage of the total dose of inhaled radioactivity. The resulting individual brain time activity curves were subject to three-exponential curve fitting with the following equation: Yi=a(1-exp(-k1ti)+b(1-exp(-k2ti)−c(1-exp(-k3ti), where Yi is the fitted value at time ti while values of a, b, c, k1, k2, and k3 are all constrained to⩾0. Initial rate of BNA was calculated as the linear slope of the fitted time activity curve over 15 s starting at the arrival of 11C-nicotine in the brain. Values of maximal concentration (Cmax), time to reach 50% of Cmax values (T1/2), and area under the curve (AUC; over 12 min starting from the time of inhalation) were also extracted from the fitted time activity curves.
Statistical Analysis
Paired t-tests were conducted to compare the kinetics parameters of BNA between menthol and non-menthol cigarettes. Additional analyses using repeated measures (menthol vs non-menthol phase) ANOVAs with each between-subjects factor (eg, sex) were conducted to examine its effect and interaction with cigarette mentholation. Years of smoking was entered as a covariate in these analyses given its possible impact on nicotine kinetics (Yamamoto et al, 2012). Similar analyses were performed on measures of smoking behavior which included self-reported CPD and a composite index of smoking intensity (puffing volume (ml)/min) averaged across the last 3 days of smoking adaptation, and CO boosts from smoking a study cigarette (COpost-smoking−COpre-smoking) after the adaptation. Partial correlations were calculated to evaluate the associations of BNA kinetics with smoking motivational measurements controlling for smoking years, sex, and menthol preference. Threshold for statistical significance was set at p<0.05. Group mean values (±SEM) are reported unless otherwise specified.
RESULTS
Sample Characteristics
Table 1 summarizes demographic and baseline smoking-related characteristics of the subjects. There were comparable numbers of males and females in menthol and non-menthol smoker groups. No significant group differences were found in mean age, years of smoking, Fagerström Test of Nicotine Dependence scores, and expired CO at the screening visit. Self-reported numbers of CPD tended to be larger among the non-menthol than menthol smokers. Despite extensive efforts towards recruiting participants comparable in race/ethnicity composition between the two groups, the completers in the non-menthol group were all White, while equal numbers of Blacks and Whites in the menthol group completed the study.
PET Results
Results of separate paired t-tests performed with the full sample (n=19) showed no significant differences in initial slope, Cmax, AUC, and T1/2 of BNA between inhalation from menthol and non-menthol study cigarettes (all p-values>0.23).
Exploratory analysis with repeated measures (menthol vs non-menthol phase) ANOVA with sex as a between-subjects factor and years of smoking as a covariate was conducted on each of the parameters of BNA. Results showed a main effect of sex (F(1,16)=6.373, p=0.023) and a significant sex × mentholation interaction (F(1,16)=9.993, p=0.006) on initial slopes (Figures 1 and 2a). Among men, the average initial slope was 26.2% steeper with menthol than non-menthol cigarettes (p=0.008), whereas slightly lower values were associated with menthol cigarettes in women. Mean initial slope across both cigarette types was 56.8% greater in women than in men. The analysis with Cmax revealed a main effect of sex (F(1, 16)=7.301, p=0.016). Averaged across the two types of cigarettes, Cmax values were 34.6% greater in women than in men (Figure 2b). Similarly, there was a significant main effect of sex (F(1,16)=7.347, p=0.015) on AUC. Average AUC was 33.2% larger in women vs men (Figure 2c). As to T1/2, there was a significant effect of sex (F(1, 16)=5.665, p=0.03) with longer mean T1/2 seen in men (Figure 2d). Years of smoking was found to be a significant covariate with T1/2 values only (F(1, 16)=6.417, p=0.022; partial correlation 0.54). Additionally, it interacted with study cigarette types such that its correlation with T1/2 values measured with non-menthol was higher than that with menthol cigarettes (F(1,16)=5.407, p=0.034; partial correlations 0.61 vs 0.41).
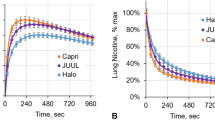
Average brain nicotine accumulation (BNA) curves after inhalation of a single puff of smoke from menthol and non-menthol cigarettes in male (left, a) and female (right, b) smokers depict faster BNA with menthol than non-menthol cigarettes in males and overall faster BNA in females (n=10) than in males (n=9). Brain nicotine accumulation per kg of tissue mass was expressed as a percentage of the total dose of inhaled 11C-nicotine. Data were calculated from fitted time activity curves for individual subjects. Gray straight line represents the time interval when the difference between inhaling from menthol and non-menthol cigarettes is statistically significant in male subjects (p<0.05) based on paired t-tests performed on the fitted brain nicotine measurements at each time frame. For visual clarity, only plus or minus error bars (SEM) are shown for each curve.
Kinetic parameters (mean+SEM) of brain nicotine accumulation after inhalation of a single puff of smoke from menthol and non-menthol cigarettes in males (n=9) and females (n=10). (a) initial slope over 15-s period after the initial appearance of radioactivity in the brain. (b) Cmax. (c) area under brain nicotine accumulation curve (AUC). (d) Time (s) to reach 50% of the value of Cmax (T1/2). Brain nicotine accumulation per kg of tissue mass was expressed as a percentage of the total dose of inhaled 11C-nicotine. *p<0.05; **p<0.01.
Similar ANOVAs with menthol preference and race (Black vs White) each as a between-subjects factor showed no significant main effects of either factor or their interactions with mentholation of study cigarettes (all ps⩾0.18). Separate analyses with order (menthol phase being the first or not) as a between-subjects factor revealed a significant order × mentholation interaction on T1/2 values (F(1,16)=5.188, p=0.037). Mean T1/2 was shorter after inhalation from menthol than non-menthol cigarettes (19.4 (3.1) vs 23.5 (3.6) s, p=0.019) among subjects who underwent the menthol cigarette study phase first, whereas no such difference was found in those who smoked non-menthol cigarettes first (23.9 (3.3) vs 22.8 (3.8), n.s.). Results from an additional repeated measures ANOVA with both sex and order as between-subject variables on T1/2 measures showed that sex remained a significant factor (F(1,14)=5.557, p=0.033) and there was no interaction between order and sex (p=0.48), suggesting that order is not a confounding factor for the observed effect of sex.
Behavioral Results
Participants smoked via the CReSS devices on average 50.1±7.0% of self-reported total numbers of menthol cigarettes and 59.2±7.0% of non-menthol cigarettes smoked over the last 3 days of the respective smoking adaptation period, indicating overall moderate compliance with using the devices in naturalistic smoking settings. One of the male participants who had unusually large mean puff volumes per min for both menthol and non-menthol cigarettes (> (group mean+3.5 SD)) was excluded as an outlier from statistical analyses on smoking intensity.
Paired t-tests indicated no significant differences in smoking intensity, numbers of CPD, and CO boosts between the two phases (all p-values>0.33). Separate repeated measures (menthol vs nonmenthol phase) ANOVAs with sex as a between-subjects factor revealed a sex × mentholation interaction (F(1,13)=7.310, p=0.018) on smoking intensity but not on CPD (Supplementary Figure S1A) and CO boosts. In men, lower smoking intensity was associated with menthol than non-menthol cigarettes (p=0.015), whereas women had slightly higher smoking intensity with menthol cigarettes (Supplementary Figure S1B). Similar ANOVAs with menthol preference as a between-subjects factor showed a menthol preference × mentholation interaction (F(1,17)=6.934, p=0.017) on numbers of CPD during smoking adaptation. Menthol smokers reported higher mean numbers of CPD while smoking menthol than non-menthol study cigarettes (18.4 (1.9) vs 15.3 (2.2), p=0.044), whereas non-menthol smokers tended to report lower numbers of CPD with menthol cigarettes (17.4 (2.0) vs 19.8 (2.3), n.s.). No main effects of sex or menthol preference were observed on these behavioral measures.
Relations between Brain Nicotine Kinetics and Smoking Motivations
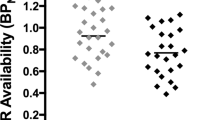
Partial correlations were also calculated between BNA kinetics measures, averaged across menthol and non-menthol study cigarettes, and ratings on the Reasons to Smoke questionnaire, controlling for the effects of sex, menthol preference, and years of smoking. Greater values of initial slope, Cmax, and AUC were significantly correlated with higher ratings of motivational value of getting a ‘rush’ and getting relaxing effects and marginally correlated with alleviation of craving (Table 2). Partial correlation plots in Figure 3 illustrate the associations of individual mean Cmax values with self-ratings of the former two motivations to smoke.
Partial correlations between values of Cmax of brain nicotine accumulation (BNA) after inhalation of a single puff of smoke from menthol and non-menthol cigarettes and ratings of the importance of getting a ‘rush’ (a) and getting better relaxation (b) from cigarette smoking, controlling for sex, menthol preference, and years of smoking (n=19). Subjects rated their motivations to smoke on the Reasons to Smoke questionnaire.
DISCUSSION
This study yielded three main findings: (i) menthol relative to non-menthol cigarettes were associated with faster initial rates of BNA after smoke inhalation in men but not women; (ii) women had overall faster BNA than men; and (iii) the rates of BNA correlated with ratings of some key aspects of smoking motivation. These results suggest that the impact of menthol on BNA and smoking dependence may vary by sex.
The present finding that men had steeper initial slopes of BNA while inhaling from menthol than non-menthol cigarettes provides partial support for the prediction that menthol may enhance the rate of BNA during smoking. Rapid nicotine delivery through cigarette smoking has long been hypothesized to be crucial to its addictive liability (Benowitz, 1990; Henningfield and Keegan, 1993). The present study contributes new evidence for the hypothesis by demonstrating significant correlations between rates of BNA after smoke inhalation and self-ratings of motivational value of getting a rush which is a good indicator of the reinforcing effects of nicotine and other addictive drugs (Foltin and Fischman, 1991; Volkow et al, 1999). Given that reduction of stress and negative affect, along with relief of withdrawal, has a critical role in the maintenance of dependent smoking motivation and vulnerability to relapse after smoking cessation (Baker et al, 2004), the association between faster BNA and higher motivation to get relaxing effects from smoking further suggests that rapid pharmacokinetics of BNA is linked to a key element of negative reinforcement from smoking. Thus, menthol-induced increases in the rates of BNA may be involved in the neurobiological substrates underlying greater risks of smoking dependence associated with menthol than non-menthol cigarettes in men. One possibility is that faster rates of BNA result in greater nicotine binding and activation or desensitization of α4β2-containing nicotinic cholinergic receptors, which are essential for the rewarding effect of smoking (Dani and Bertrand, 2007). Given that smoking one to two puffs of a cigarette results in 50% occupancy of the α4β2-containing nicotinic cholinergic receptors, whereas smoking a full cigarette (or more) leads to over 88% receptor occupancy and a reduction of cigarette craving (Brody et al, 2006), the present results suggest that menthol is likely to increase the rate at which the receptor occupancy reaches a level that leads to significant behavioral effects in male smokers.
In contrast with the results in men, no significant differences in BNA kinetics were found between menthol and non-menthol cigarettes in women. This result suggests that the higher prevalence of menthol than non-menthol cigarette smoking in women cannot be explained by the impact of menthol on BNA kinetics and other factors have to be considered. Indeed, unlike men, women in this study tended to report stronger sensations in the back of the mouth/throat and windpipe in addition to their higher ratings of liking and satisfaction with menthol than non-menthol cigarettes (Supplementary Table S1). These observations indicate that sensitivity to and preference for sensory effects of menthol in cigarettes could be a factor that significantly contributes to the popularity of menthol cigarettes in women. Consistent with this notion, non-nicotine smoking stimuli such as olfactory/taste stimuli have been shown to be more potent conditioned reinforcers in female than male smokers (Perkins et al, 2001). Together with the current finding of markedly faster BNA after smoke inhalation in women than men, these data suggest that a combination of enhanced reinforcing effects from rapid BNA and greater satisfaction with the sensory properties of menthol cigarettes may perpetuate menthol cigarette smoking in women through strengthened conditioned reinforcements.
The finding of faster BNA in women in itself may be important for understanding sex differences in smoking dependence and cessation outcomes. Women have greater difficulties quitting smoking (Perkins, 2001; Scharf and Shiffman, 2004) and also have poorer cessation outcomes following many nicotine replacement treatments (Cepeda-Benito et al, 2004; Perkins and Scott, 2008). Although women’s vulnerability to nicotine/smoking dependence is likely determined by many factors (O’Dell and Torres, 2014; Perkins et al, 1999), considerable evidence suggests that women vs men are more sensitive to acute rewarding effects of smoking or nicotine administration. Some studies found that women experienced greater reductions in craving (Eissenberg et al, 1999) and tension-anxiety symptoms (Xu et al, 2008) immediately after cigarette smoking. Women reported stronger ‘drug strength’, ‘head rush’ from intravenous bolus nicotine (Sofuoglu and Mooney, 2009), and stimulant and mood-altering experiences after nicotine nasal spray (Myers et al, 2008). The current findings of markedly faster BNA in women than men after smoke inhalation and the correlations between the rates of BNA with ratings of some important aspects of smoking motivation may suggest a neuropharmacological mechanism underlying the sex differences in the reinforcement of nicotine/smoking. Women who become dependent on some stronger reinforcing effects associated with faster BNA during smoking may have greater difficulties quitting and also benefit less than men from nicotine replacement treatments that feature slower nicotine delivery.
What causes the sex differences in BNA during smoking is unclear. Fast BNA after smoke inhalation is critically determined by the fraction of inhaled nicotine that can rapidly deposit and then be transferred to the blood via the huge surface area of the alveoli and small airways in the lungs (Benowitz et al, 1988; Berridge et al, 2010; Rose et al, 2010). Therefore, structural differences in the respiratory system between sexes could lead to differences in nicotine deposition and transfer in the lungs and the rates of BNA. First, men have larger diameter upper and lower airways than women (Mead, 1980). As larger airways are more prone to turbulent air flow that enhances particle deposition (Ahmadi, 2009), there is likely to be a greater deposition of nicotine-containing smoke particles in the upper airways and consequently reduced pulmonary nicotine deposition for men than women. Second, given the fixed inhalation volume during PET imaging, one possibility may be that, as noted for non-smoke particles (Jaques and Kim, 2000), the inhaled nicotine penetrates more deeply into the lungs and reaches more alveoli in women because their lung volumes are smaller than that of men’s (Crapo et al, 1982). Besides these structural differences in the respiratory tract, female and male smokers might differ in capacity of pulmonary nicotine uptake (‘trapping’) because of smoke exposure-induced increases in alveolar macrophages (Yano et al, 2002) that may trap nicotine (pKa ca. 8.0) in their acid lysosomal bodies (pH 4.6∼5.0; Mellman et al, 1986). On the basis of evidence that female vs male smokers have overall lower nicotine/smoke exposure (Zeeman et al, 2002; Gan et al, 2008), it is likely that women might have on average fewer alveolar macrophages and thereby lower nicotine trapping in their lungs and faster rates of nicotine clearance into the blood. Notably, we previously found that dependent vs non-dependent smokers had slower rates of nicotine wash-out from the lungs after smoke inhalation (Rose et al, 2010), which further supports the likely association between the heaviness of smoke exposure and macrophage-mediated increases in pulmonary nicotine trapping.
The mechanisms underlying the sex-specific enhancement of BNA by menthol remain to be determined. As discussed above, faster BNA in women indicates that women probably have greater nicotine deposition in the alveoli after smoke inhalation. The absence of impact of menthol on BNA in women suggests that menthol is unlikely to enhance nicotine permeability through the alveoli to any significant level, presumably because nicotine transfer through them is extremely efficient as it is (Ingebrethsen, 2006). Assuming that men have considerably greater nicotine deposition in the small airways because of their larger diameters than that of women’s (Mead, 1980) and/or other unknown factors, we postulate that menthol may enhance nicotine permeability through membrane of these airways, similar to what it does to oral mucosa (Squier et al, 2010), to a greater extent for men than women. Because bronchial blood flow drains mostly into the pulmonary circulation (Charan et al, 2007), the increases of nicotine permeability in these small airways can contribute to faster rates of BNA after inhaling from menthol cigarettes as seen in men. Future investigations should evaluate these possibilities and other potential mechanisms for the sex differences in pulmonary nicotine deposition and clearance and their susceptibility to the influence of menthol.
Several limitations of the present study should be noted. First, there was a lack of African-American participants in the non-menthol smoker group. The total sample size was relatively modest, though not atypical for PET studies. Thus, the findings should be replicated in studies with larger, more balanced samples, which would also permit evaluation of whether any trends for selective attrition may introduce bias into the findings. Second, the lack of manipulation (eg, inhalation volume) or control of respiratory parameters (eg, inhalation flow rate and breath-holding time) might limit the generalizability of our findings. Although existing evidence is inconclusive with regard to the influence of menthol on puffing and inhaling patterns of smokers, it is still possible that the impact of menthol on BNA may be affected by certain respiratory parameters. Third, possible differences in tobacco blend and construction (eg, filter pressure drop) among other non-menthol factors between the menthol and non-menthol cigarettes could have affected their nicotine delivery. However, the comparable FTC nicotine/tar/CO yields of these two types of cigarettes seem to indicate a lack of overall impact of such differences, if they exist. Alternative experimental manipulations of menthol vs non-menthol cigarettes such as a use of encapsulated menthol cartridge cigarettes could permit better isolation of any impact of menthol from those of other factors on nicotine availability in future investigations. Another weakness of the study is a lack of a biomarker of menthol exposure during smoking adaptation periods which would have allowed objective verification of subject compliance in smoking assigned cigarettes.
In summary, this study provides only partial support for the hypothesis that menthol may physiologically enhance the rate of BNA during smoking. The findings suggest that the impact of menthol on BNA may have a role in promoting smoking dependence in men. For women, preference of the sensory properties of menthol cigarettes and fast BNA kinetics during smoking may independently or jointly contribute to smoking dependence. These results support the development of cessation treatments that target sex-specific effects of menthol on fast brain nicotine kinetics and the behavioral reinforcement of smoking. Further studies of the relations between menthol and sex differences in smoking behavior as well as pulmonary absorption and transfer of nicotine are warranted.
FUNDING AND DISCLOSURE
The project described was supported by Grant R03DA029676 (Dr Zuo) from the National Institute on Drug Abuse. It was also supported in part by a grant to Duke University from Philip Morris USA Inc. Dr Rose and Ms Behm hold patent purchase agreement/consultancy with Philip Morris International. The sponsors had no role in the planning or execution of the study, data analysis, or publication of results. The authors declare no conflict of interest.
References
Ahijevych K, Parsley LA (1999). Smoke constituent exposure and stage of change in black and white women cigarette smokers. Addict Behav 24: 115–120.
Ahmadi G (2009). Lagrangian versus Eulerian Method for Nano-Particles. Paper presented at the AVT-169 RTO AVT/VKI Lecture Series; 9–12 February 2009; von Karman Institute, Rhode St. Genèse, Belgium. http://www.cso.nato.int/pubs/rdp.asp?RDP=RTO-EN-AVT-169.
Baker TB, Brandon TH, Chassin L (2004). Motivational influences on cigarette smoking. Annu Rev Psychol 55: 463–491.
Behm FM, Rose JE (1994). Reducing craving for cigarettes while decreasing smoke intake using capasaicin-enhanced low-tar cigarettes. Exp Clin Pharmacol 2: 143–153.
Benowitz NL (1990). Clinical pharmacology of inhaled drugs of abuse: implications in understanding nicotine dependence. NIDA Res Monogr 99: 12–29.
Benowitz NL, Porchet H, Sheiner L, Jacob P 3rd (1988). Nicotine absorption and cardiovascular effects with smokeless tobacco use: comparison with cigarettes and nicotine gum. Clin Pharmacol Ther 44: 23–28.
Berridge MS, Apana SM, Nagano KK, Berridge CE, Leisure GP, Boswell MV (2010). Smoking produces rapid rise of [11C]nicotine in human brain. Psychopharmacology (Berl) 209: 383–394.
Brody AL, Mandelkern MA, London ED, Olmstead RE, Farahi J, Scheibal D et al (2006). Cigarette smoking saturates brain alpha 4 beta 2 nicotinic acetylcholine receptors. Arch Gen Psychiatry 63: 907–915.
Cepeda-Benito A, Reynoso JT, Erath S (2004). Meta-analysis of the efficacy of nicotine replacement therapy for smoking cessation: Differences between men and women. J Consult Clin Psychol 72: 712–722.
Charan NB, Thompson WH, Carvalho P (2007). Functional anatomy of bronchial veins. Pulm Pharmacol Ther 20: 100–103.
Clark PI, Gautam S, Gerson LW (1996). Effect of menthol cigarettes on biochemical markers of smoke exposure among Black and White smokers. Chest 110: 194–198.
Crapo RO, Morris AH, Gardner RM (1982). Reference values for pulmonary tissue volume, membrane diffusing capacity, and pulmonary capillary blood volume. Bull Eur Physiolopathol Respir 18: 893–899.
Dani JA, Bertrand D (2007). Nicotinic acetylcholine receptors and nicotinic cholinergic mechanisms of the central nervous system. Annu Rev Pharmacol Toxicol 47: 699–729.
Eccles R (1994). Menthol and related cooling compounds. J Pharm Pharmacol 46: 618–630.
Eissenberg T, Adams C, Riggins EC 3rd, Likness M (1999). Smokers' sex and the effects of tobacco cigarettes: subject-rated and physiological measures. Nicotine Tob Res 1: 317–324.
Foltin RW, Fischman MW (1991). Smoked and intravenous cocaine in humans: acute tolerance, cardiovascular and subjective effects. J Pharmacol Exp Ther 257: 247–261.
Food and Drug Administration (2013). Preliminary scientific evaluation of the possible public health effects of menthol versus nonmenthol cigarettes. http://www.fda.gov/downloads/scienceresearch/specialtopics/peerreviewofscientificinformationandassessments/ucm361598.pdf.
Gan WQ, Cohen SB, Man SF, Sin DD (2008). Sex-related differences in serum cotinine concentrations in daily cigarette smokers. Nicotine Tob Res 10: 1293–1300.
Giovino GA, Sidney S, Gfroerer JC, O’Malley PM, Allen JA, Richter PA et al (2004). Epidemiology of menthol cigarette use. Nicotine Tob Res 6: S67–S81.
Green BG (1992). The sensory effects of l-menthol on human skin. Somatosens Mot Res 9: 235–244.
Halldin C, Någren K, Swahn CG, Långström B, Nybäck H (1992). (S)- and (R) [11C]nicotine and the metabolite (R/S)-[11C]cotinine. Preparation, metabolite studies and in vivo distribution in the human brain using PET. Int J Rad Appl Instrum B 19: 871–880.
Heatherton TF, Kozlowski LT, Frecker RC, Fagerstrom KO (1991). The Fägerstrom Test for Nicotine Dependence: a revision of the Fagerstrom Tolerance Questionnaire. Br J Addict 86: 1119–1127.
Henningfield JE, Keegan RM (1993). Nicotine delivery kinetics and abuse liability. J Consult Clin Psychol 61: 743–750.
Ingebrethsen BJ (2006). Numerical simulation of the effects of dilution level, depth of inhalation, and smoke composition on nicotine vapor deposition during cigarette smoking. Inhal Toxicol 18: 1071–1076.
Jaques PA, Kim CS (2000). Measurement of total lung deposition of inhaled ultrafine particles in healthy men and women. Inhal Toxicol 12: 715–731.
Jarvik ME, Tashkin DP, Caskey NH, McCarthy WJ, Rosenblatt MR (1994). Mentholated cigarettes decrease puff volume of smoke and increase carbon monoxide absorption. Physiol Behav 56: 563–570.
Kobayashi D, Matsuzawa T, Sugibayashi K, Morimoto Y, Kimura M (1994). Analysis of the combined effect of l-menthol and ethanol as skin permeation enhancers based on a two-layer skin model. Pharm Res 11: 96–103.
Kunta JR, Goskonda VR, Brotherton HO, Khan MA, Reddy IK (1997). Effect of menthol and related terpenes on the percutaneous absorption of propranolol across excised hairless mouse skin. J Pharm Sci 86: 1369–1373.
Le Foll B, Wertheim C, Goldberg SR (2007). High reinforcing efficacy of nicotine in non-human primates. PLoS ONE 2: e230.
Lunell E, Bergström M, Antoni G, Långström B, Nordberg A (1996). Nicotine deposition and body distribution from a nicotine inhaler and a cigarette studied with positron emission tomography. Clin Pharmacol Ther 59: 593–594.
McCarthy WJ, Caskey NH, Jarvik ME, Gross TM, Rosenblatt MR, Carpenter C (1995). Menthol vs nonmenthol cigarettes: Effects on smoking behavior. Am J Public Health 85: 67–72.
Mead J (1980). Dysanapsis in normal lungs assessed by the relationship between maximal flow, static recoil, and vital capacity. Am Rev Respir Dis 121: 339–342.
Mellman I, Fuchs R, Helenius A (1986). Acidification of the endocytic and exocytic pathways. Annu Rev Biochem 55: 663–700.
Myers CS, Taylor RC, Moolchan ET, Heishman SJ (2008). Dose-related enhancement of mood and cognition in smokers administered nicotine nasal spray. Neuropsychopharmacology 33: 588–598.
O'Dell LE, Torres OV (2014). A mechanistic hypothesis of the factors that enhance vulnerability to nicotine use in females. Neuropharmacology 76: 566–580.
Perkins KA (2001). Smoking cessation in women. Special considerations. CNS Drugs 15: 391–411.
Perkins KA, Donny E, Caggiula AR (1999). Sex differences in nicotine effects and self-administration: review of human and animal evidence. Nicotine Tob Res 1: 301–315.
Perkins KA, Gerlach D, Vender J, Grobe J, Meeker J, Hutchison S (2001). Sex differences in the subjective and reinforcing effects of visual and olfactory cigarette smoke stimuli. Nicotine Tob Res 3: 141–150.
Perkins KA, Scott J (2008). Sex differences in long-term smoking cessation rates due to nicotine patch. Nicotine Tob Res 10: 1245–1251.
Rose JE, Mukhin AG, Lokitz SJ, Turkington TG, Herskovic J, Behm FM et al (2010). Kinetics of brain nicotine accumulation in dependent and nondependent smokers assessed with PET and cigarettes containing 11C-nicotine. PNAS 107: 5190–5195.
Scharf D, Shiffman S (2004). Are there gender differences in smoking cessation, with and without bupropion? Pooled- and meta-analyses of clinical trials of Bupropion SR. Addiction 99: 1462–1469.
Shojaei AH, Khan M, Lim G, Khosravan R (1999). Transbuccal permeation of a nucleoside analog, dideoxycytidine: Effects of menthol as a permeation enhancer. Int J Pharm 192: 139–146.
Sloan A, DeCort SC, Eccles R (1993). Prolongation of breathhold time following treatment with an L-menthol lozenge in healthy man. J Physiol 473: 53P.
Sofuoglu M, Mooney M (2009). Subjective responses to intravenous nicotine: greater sensitivity in women than in men. Exp Clin Psychopharmacol 17: 63–69.
Squier CA, Mantz MJ, Wertz PW (2010). Effects of menthol on the penetration of tobacco carcinogens and nicotine across porcine oral mucosa ex vivo. Nicotine Tob Res 12: 763–767.
US Department of Health and Human Services (1998) Tobacco use among U.S. racial/ethnic groups—African Americans, American Indian and Alaska Natives, Asian Americans and Pacific Islanders, and Hispanics: A report of the surgeon general. US Department of Health and Human Services, Centers for Disease Control and Prevention: Atlanta, GA.
Volkow ND, Wang GJ, Fowler JS, Logan J, Gatley SJ, Wong C et al (1999). Reinforcing effects of psychostimulants in humans are associated with increases in brain dopamine and occupancy of D2 receptors. J Pharmacol Exp Ther 291: 409–415.
Xu J, Azizian A, Monterosso J, Domier CP, Brody AL, Fong TW et al (2008). Gender effects on mood and cigarette craving during early abstinence and resumption of smoking. Nicotine Tob Res 10: 1653–1661.
Yamamoto RT, Rohan ML, Goletiani N, Olson D, Peltier M, Renshaw PF et al (2012). Nicotine related brain activity: the influence of smoking history and blood nicotine levels, an exploratory study. Drug Alcohol Depend 129: 137–144.
Yano R, Hayakawa D, Emura S, Chen H, Ozawa Y, Taguchi H et al (2002). Effects of cigarette smoke exposure on the ultrastructure of the golden hamster parathyroid gland. Histol Histopathol 17: 375–381.
Zeman MV, Hiraki L, Sellers EM (2002). Gender differences in tobacco smoking: higher relative exposure to smoke than nicotine in women. J Womens Health Gend Based Med 11: 147–153.
Acknowledgements
We thank Al Salley, Tanaia Loeback, Wendy Roberts, and David Botts for subject recruitment, and Dena Hill-Cairnes, Alana Cataldo, and Kelsey Behrens for assistance in data collection and processing.
Author information
Authors and Affiliations
Corresponding author
Additional information
Supplementary Information accompanies the paper on the Neuropsychopharmacology website
Rights and permissions
About this article
Cite this article
Zuo, Y., Mukhin, A., Garg, S. et al. Sex-Specific Effects of Cigarette Mentholation on Brain Nicotine Accumulation and Smoking Behavior. Neuropsychopharmacol 40, 884–892 (2015). https://doi.org/10.1038/npp.2014.263
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/npp.2014.263
This article is cited by
-
Comparison of brain nicotine accumulation from traditional combustible cigarettes and electronic cigarettes with different formulations
Neuropsychopharmacology (2024)
-
Comparison of brain nicotine uptake from electronic cigarettes and combustible cigarettes
Neuropsychopharmacology (2022)
-
Sex differences in tobacco withdrawal and responses to smoking reduced-nicotine cigarettes in young smokers
Psychopharmacology (2018)
-
Sex Differences in Midbrain Dopamine D2-Type Receptor Availability and Association with Nicotine Dependence
Neuropsychopharmacology (2016)