Abstract
Patients with magnetic-resonance-imaging (MRI)-negative (or ‘nonlesional’) pharmacoresistant focal epilepsy are the most challenging group undergoing presurgical evaluation. Few large-scale studies have systematically reviewed the pathological substrates underlying MRI-negative epilepsies. In the current study, histopathological specimens were retrospectively reviewed from MRI-negative epilepsy patients (n=95, mean age=30 years, 50% female subjects). Focal cortical dysplasia cases were classified according to the International League Against Epilepsy (ILAE) and Palmini et al classifications. The most common pathologies found in this MRI-negative cohort included: focal cortical dysplasia (n=43, 45%), gliosis (n=21, 22%), hamartia+gliosis (n=12, 13%), and hippocampal sclerosis (n=9, 9%). The majority of focal cortical dysplasia were ILAE type I (n=37) or Palmini type I (n=39). Seven patients had no identifiable pathological abnormalities. The existence of positive pathology was not significantly associated with age or temporal/extratemporal resection. Follow-up data post surgery was available in 90 patients; 63 (70%) and 57 (63%) attained seizure freedom at 6 and 12 months, respectively. The finding of positive pathology was significantly associated with seizure-free outcome at 6 months (P=0.035), but not at 12 months. In subgroup analysis, the focal cortical dysplasia group was not significantly correlated with seizure-free outcome, as compared with the negative-pathology groups at either 6 or 12 months. Of note, the finding of hippocampal sclerosis had a significant positive correlation with seizure-free outcome when compared with the negative-pathology group (P=0.009 and 0.004 for 6- and 12-month outcome, respectively). Absence of a significant histopathology in the resected surgical specimen did not preclude seizure freedom. In conclusion, our study highlights the heterogeneity of epileptic pathologies in MRI-negative epilepsies, with focal cortical dysplasia being the most common finding. The existence of positive pathology in surgical specimen may be a good indication for short-term good seizure outcome. There is a small subset of cases in which no pathological abnormalities are identified.
Similar content being viewed by others
Main
Patients with magnetic-resonance-imaging (MRI)-negative (or ‘nonlesional’) pharmacoresistant focal epilepsy constitute the most challenging group undergoing presurgical evaluation.1, 2, 3 The overall prevalence of nonlesional epilepsy in all surgical studies is ∼26%.4 At present, surgical management of MRI-negative pharmacoresistant focal epilepsy patients relies heavily on invasive intracranial electroencephalography, which is based on complimentary review of other noninvasive modalities including positron emission tomography, ictal single-photon emission computed tomography, and magnetoencephalography when available.5, 6, 7, 8 Despite substantial efforts, the lack of a lesion on MRI has consistently been shown to be one of the predictors for surgical failure.9, 10 Therefore, MRI-negative patients are usually considered unfavorable surgical candidates4 and are often denied epilepsy surgery. Yet, surgical resection can be effective in well-selected patients with no visible MRI abnormality. In order to improve surgical outcome of MRI-negative patients, it is important to understand the pathologies that these patients may demonstrate on examining their surgically resected tissues.
The pathologic substrates underlying pharmacoresistant focal epilepsy are well established and most commonly include hippocampal sclerosis, focal cortical dysplasia, tumors, and remote ischemic events/infarcts.11, 12 Studies specifically on the surgical pathology of MRI-negative patients, however, are limited to small-scale experiences of individual centers,13, 14, 15, 16 or cases buried in larger series containing both MRI-positive and -negative patients.17, 18 Moreover, with the advance in MRI technology over the last decade and the establishment of more uniform epilepsy MRI protocols, the definition of ‘MRI-negative’ cases in recent studies may not be equivalent to earlier ones. The purpose of this study is to systematically review one institution’s recent experience with the pathological substrates underlying strictly defined MRI-negative epilepsies.
Materials and methods
After approval from Institutional Review Board, the Cleveland Clinic Epilepsy Center’s surgical database was searched for patients with chronic epilepsy who underwent a surgical resection from 2002 to 2011. During this period, all patients underwent high-resolution 1.5- or 3-Tesla preoperative MRI studies using a standard epilepsy protocol. From this group, we selected patients with strictly defined negative MRI based on two criteria: (1) all MRI scans were evaluated prospectively by dedicated epilepsy neuroradiologists for possible epileptogenic abnormalities during the presurgical evaluation process and showed no lesions and (2) MRI scans were evaluated again by epileptologists, neurosurgeons, and dedicated epilepsy neuroradiologists after re-review of images during the patient management conference, taking into account the results of comprehensive noninvasive testing, and were still judged to be negative. Patients with MRIs that were initially interpreted as normal were excluded if a probable or questionable lesion was identified during re-review of the study in the patient management conference. Patients were excluded if they had poor MRI image quality, for example, motion artifacts hampering image interpretation. Patients with prior surgeries were excluded.
Available microscopic slides from surgical resections were reviewed in all cases (mean=7, range=1–20). In 40 cases, all the resected tissues were submitted and reviewed microscopically; a subtotal sampling of resected tissue was done in the remaining 55 cases. Focal cortical dysplasia was classified according to both the International League Against Epilepsy (ILAE) classification19 as well as Palmini et al20 classification; classification criteria are described in Table 1. Hippocampal sclerosis was defined by a characteristic loss of neurons and gliosis in the hippocampus, preferentially involving the dentate, CA4, CA3, and CA1 regions.21 Hamartias were defined as collections of small neurons marked by scant cytoplasm and pericellular clearing.22 Nodular heterotopia is marked by the presence of disordered gray matter tissue in the white matter. Positive pathology is defined by the finding of focal cortical dysplasia, heterotopia, hippocampal sclerosis, other hippocampal abnormalities, and dual osseous metaplasia. Negative pathology is defined by the finding of gliosis only, gliosis with hamartia, or no microscopic abnormality identified.
Based on location of surgical site, resections were classified as frontal, parieto-occipital, neocortical temporal, standard temporal lobectomies with removal of mesial temporal structures, and multilobar resections. We analyzed the outcome at 6 and 12 months. Outcome was classified into two groups: completely seizure-free (Engel’s class Ia) and not seizure-free (Engel’s class Ib–IV).23 Statistical significance was assessed using the Fisher’s exact test, with significance defined as a probability (P) value of ≤0.05.
Results
Patient Demographics
A total of 95 patients (median/mean age=29/30 years, range 4–64 years; 50% female subjects) fulfilled the selection criteria. Histological slides were available in all patients. Surgery included 21 frontal resections, 6 parieto-occipital resections, 34 neocortical temporal resections, 32 standard temporal lobectomies with removal of mesial structures, and 2 multilobar resections. Left-sided resections were performed in 49 (52%) patients.
Pathological Findings
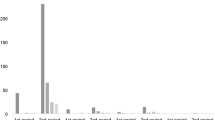
Table 2 summarizes the pathological findings observed in this MRI-negative cohort. The most commonly identified pathology was focal cortical dysplasia (n=43, including 2 coexisting with hippocampal sclerosis and 2 with nodular heterotopia). A majority of cortical dysplasias were ILAE type I (n=37), with the majority being Ic (n=28); using Palmini classification, the majority were type I as well (n=39), with type IA being most common (n=30). Examples of ILAE type Ic (Palmini type IA) and Ib (Palmini type IB) are shown in Figures 1 and 2, respectively. Two patients had nodular heterotopia in addition to focal cortical dysplasia (Figure 3). Nine patients had hippocampal sclerosis alone (Figure 4). Twenty-one patients only had gliosis, and an additional 12 patients showed gliosis accompanied by hamartia (Figure 5). In seven patients, no microscopic abnormality was identified.
Low-magnification view of the cortex showing a linear arrangement of neurons in central layers 2 and 3, consistent with ILAE type Ic focal cortical dysplasia (Palmini et al20 type IA). (Hematoxylin and eosin staining; original magnification × 100.)
Intermediate magnification view of the cortex showing an absence of a well-formed cortical layer 2 and neuronal cytomegaly, consistent with ILAE type Ib focal cortical dysplasia (Palmini et al20 type IB). (Hematoxylin and eosin staining; original magnification × 200.)
Overall, 12/19 (63%) children (17 years or younger) had positive pathology, compared with 43/76 (57%) adults. No difference in positive pathology was noted between these two age groups (P=0.8). Twenty-one of the 29 (72%) extratemporal lobe epilepsy patients had positive pathology compared with 34/66 (52%) of patients with temporal lobe epilepsy. The finding of positive pathology was not significantly associated with temporal/extratemporal lobe epilepsy groups (P=0.07). Seventeen of the 55 (31%) subtotally submitted specimens had negative pathology; 23/40 (58%) of totally submitted specimens had negative pathology.
Correlation With Outcome
Follow-up data were available in 90 patients. Outcome data grouped by pathology are shown in Table 3. At 6 months’ follow-up, 63 (ie, 70% of the entire cohort) attained seizure freedom (Engel class Ia). Overall, 42 of the 53 (79%) patients with positive pathology, and 21 of the 37 (57%) patients with negative pathology were seizure-free. The finding of positive pathology was significantly associated with seizure-free outcome (P=0.035). We further performed subgroup analysis. Although focal cortical dysplasia constituted the largest group of seizure-free patients (30/63, 48%), there was no significant correlation between the existence of focal cortical dysplasia in surgical specimen and seizure-free outcome, as compared with the negative-pathology group (P=0.16) or gliosis alone (P=0.09). Of note, the finding of hippocampal sclerosis (including nine hippocampal sclerosis only, and two hippocampal sclerosis+focal cortical dysplasia) had a significant positive correlation with seizure-free outcome when compared with the negative-pathology group (P=0.009). The ILAE Ib group trended towards being positively associated with seizure-free outcome when compared with the gliosis only plus no-identifiable-pathology group (P=0.06), but did not reach statistical significance. In the group where no pathology was identified, four out of the seven patients were seizure-free.
At 12-month follow-up, 57 (63%) were completely seizure-free (Engel class Ia outcome). Overall, 37 of the 53 (70%) patients with positive pathology, and 20 of the 37 (54%) patients with negative pathology were seizure-free. Different from the 6-month follow-up data, the finding of positive pathology was not significantly associated with seizure-free outcome 12 months after surgical resection (P=0.18). Other data trends are similar to the 6-month-outcome data. Patients with focal cortical dysplasia were still more likely to attain seizure-free outcome (27/57, 47%), but there was no significant correlation between the existence of focal cortical dysplasia in surgical specimen and seizure-free outcome, as compared with the negative-pathology group (P=0.35) or gliosis alone (P=0.27). The finding of hippocampal sclerosis still had a significant positive correlation with seizure-free outcome at 12 months when compared with the negative-pathology group (P=0.004). The ILAE Ib group trended toward being positively associated with seizure-free outcome when compared with the Ic group (P=0.056) and the gliosis plus no-identifiable-pathology group (P=0.06), but did not reach statistical significance for either. Four out of the seven patients with no-identifiable pathology remained seizure-free at 12 months.
Discussion
We present the pathologic results of a large single-center series of 95 patients with strictly defined MRI-negative focal epilepsy who underwent epilepsy surgery. Consistent with previous studies, our data show that focal cortical dysplasia is the most common pathological substrate of surgically treated nonlesional epilepsy. In addition, our results show that the presence of positive pathology is significantly associated with early seizure-free outcome. There was no significant correlation between the existence of focal cortical dysplasia in surgical specimens and seizure-free outcome, as compared with the negative-pathology groups in either 6- or 12 months’ outcome data. Of note, the finding of hippocampal sclerosis had a significant positive correlation with seizure-free outcome, when compared with the negative-pathology group. Absence of a significant histopathology in the resected surgical specimen did not preclude seizure freedom.
Limitations of the previous literature examining pathological substrates of nonlesional epilepsy include: small number of patients, variable definitions of ‘nonlesional’, and variable approaches to pathological diagnosis. Pathological findings are typically reported in small-scale studies from individual centers,13, 14, 15, 16 or buried in larger series containing a full spectrum of patients among which only a small number was MRI-negative.17, 18 A few attempts at meta-analysis have been performed to better understand surgical outcome and factors such as pathology, surgery type, and seizure semiology in MRI-negative patients. Ansari et al24 reported 95 pediatric extratemporal nonlesional epilepsy patients from 17 studies, and classified surgical pathology into three categories: cortical dysplasia, gliosis, and others (neuronal loss, encephalitis, polymicrogyria, ulegyria, chronic inflammation, and normal). Their analysis demonstrated that a positive histopathological finding has a favorable association with postoperative outcome: a majority of patients in the Engel class I outcome group harbored cortical dysplasia. In a parallel study, Ansari et al25 reported on 131 adult patients with extratemporal nonlesional epilepsy and found that none of the variables, including surgical pathology, had any significant association with outcome in the adult group. This study also found focal cortical dysplasia to be the most common substrate in patients with seizure-free outcome. Both meta-analysis studies defined ‘nonlesional’ epilepsies based on pathological substrates, whereas only mass-like lesions such as tumors, vascular lesions, multiple sclerosis, and heterotopias were considered ‘lesional’, and focal cortical dysplasia was considered ‘nonlesional’. From a practical, presurgical evaluation point of view, however, MRI findings are generally used to define a case as ‘nonlesional’. In our study, we only included patients with negative MRI based on consensus review of high-resolution MRI studies during a multidisciplinary patient management conference, in addition to an independent neuroradiology interpretation. This approach ensured the inclusion of a highly selected group of patients with negative MRI findings who underwent surgical resection of identified epileptic foci, followed by a blinded neuropathological examination of the resected specimens.
The high incidence of various focal cortical dysplasia types in the current study supports that the most common epileptic pathological correlate not visualized by MRI was indeed focal cortical dysplasia. These results are concordant with previous reports that showed that cortical dysplasia was identified in up to one-third of tissue specimens, following resective epilepsy surgery in both MRI-positive and -negative cases.24, 25, 26, 27 Among the focal cortical dysplasia subtypes, our data also show that focal cortical dysplasia type I (by either classification) is the most common substrate of MRI-negative epilepsy. There were only four cases of balloon cell cortical dysplasia. The higher prevalence of type I lesions than type II further illustrates the challenging nature of presurgical identification and mapping of this pathology, and highlights the need for more sensitive and accurate presurgical studies. Focal cortical dysplasia type I lesions have highly idiosyncratic presentations and are usually more diffuse than type II lesions, making them the most challenging ones to be detected by structural imaging methodology.28, 29, 30 In addition to the accurate definition, delineation of the boundaries of type I focal cortical dysplasia is also difficult, as the microscopically dysplastic lesion may extend well beyond the margins defined by the MRI-visible abnormality (in MRI-positive cases),30, 31, 32 even with the use of high-resolution dedicated epilepsy MRI protocols and review of the images by expert neuroradiologists.26, 32 Our finding of MRI-negative patients with hippocampal sclerosis is also consistent with previous literature that up to 30% of patients with hippocampal sclerosis may have normal findings on conventional MRI.33
Surgical outcome of MRI-negative patients can be hard to determine due to heterogeneity of patient populations, surgical techniques, follow-up time, and outcome definition in the literature. A recent meta-analysis showed only 34–45% long-term seizure-free rate, whereas MRI-positive (or ‘lesional’) surgical candidates may have a two times higher probability of attaining seizure freedom.4 Our MRI-negative cohort (comprised of temporal and extratemporal cases) had seizure-free rate of 59% at 12 months, this percentage is consistent with other studies from our center and can be anticipated to drop as follow-up durations increase.10, 34, 35 Overall, we found that positive pathology in surgical specimen positively associated with seizure-free outcome at 6 months, but not at 12 months. This finding is consistent with the hypothesis that immediate postoperative seizure recurrence may indicate a mislocalization and/or incomplete resection of the active epileptic focus, whereas long-term recurrence may be attributed to other factors such as the natural history of the disease and the postsurgical development of secondary epileptogenesis.36 Subgroup analysis revealed that focal cortical dysplasia did not positively correlate with seizure-free outcome, as the cortical dysplasia type I pathology (majority of the group) is generally more widespread, and often involves eloquent cortex in extratemporal cases, making it less amenable to resection. On the other hand, MRI-negative patients with hippocampal sclerosis appeared to have a better chance for seizure-free outcome, as these lesions are relatively more circumscribed, and temporal lobectomy with complete removal of the epileptic and histopathologically abnormal mesial structures is usually an effective approach.
In a subset of patients in the current study, no pathologic substrate was identified. One possible explanation is a presurgical mislocalization. In a recent study from our center,37 patients with multiple surgeries were examined in terms of their pathology: three of the 13 patients had no pathology on the first surgery, but focal cortical dysplasia was pathologically identified on the second surgery. Similarly, false localization could explain the pathological findings in patients with gliosis or no-identifiable pathology who were not seizure-free in this study. It is even more intriguing to speculate on the four patients who became seizure-free, but had no-identifiable pathology. Notably, with three of these four patients, resected tissue was totally submitted and examined. A number of possible explanations may include: evolving pathology due to neural plasticity and ongoing development of cortex38, 39 (given we could only sample surgically at one point of time), alterations at a neurotransmitter and/or neuromodulator level, mitochondrial level,40 genetics level,41, 42 or neurogenesis level.43, 44
One limitation of our study is the subtotal sampling of some specimens, which potentially could result in an underestimation of the epileptic pathologies. Another limitation is that we evaluated the relationship between pathology and outcome without the full consideration of the location and extent of resection. Patients who showed nonspecific gliosis or no-identifiable pathology may have focal cortical dysplasia pathology in an unresected lobe of the brain.
In conclusion, our study highlights the heterogeneity of epileptic pathologies in MRI-negative epilepsies, with focal cortical dysplasia being the most common finding. The existence of positive pathology in surgical specimen may be a good indication for short-term good seizure outcome, but does not necessarily predict long-term seizure freedom.
The subset of patients without any pathological findings is intriguing, and may indicate limitations of microscopic histopathological examination of resected human epileptic tissue, mislocalization/inadequate resection, or incomplete histopathological sampling of the resected specimens. Advanced imaging and neurophysiological modalities, invasive or noninvasive, are called for to adequately delineate the anatomical, functional, and epileptic extent of these lesions.
References
Alarcon G, Garcia Seoane JJ, Binnie CD et al. Origin and propagation of interictal discharges in the acute electrocorticogram. Implications for pathophysiology and surgical treatment of temporal lobe epilepsy. Brain 1997;120:2259–2282.
Semah F, Picot MC, Adam C et al. Is the underlying cause of epilepsy a major prognostic factor for recurrence? Neurology 1998;51:1256–1262.
Siegel AM, Jobst BC, Thadani VM et al. Medically intractable, localization-related epilepsy with normal MRI: presurgical evaluation and surgical outcome in 43 patients. Epilepsia 2001;42:883–888.
Tellez-Zenteno JF, Hernandez Ronquillo L, Moien-Afshari F et al. Surgical outcomes in lesional and non-lesional epilepsy: a systematic review and meta-analysis. Epilepsy Res 2010;89:310–318.
Schneider F, Alexopoulos AV, Wang Z et al. Magnetic source imaging in non-lesional neocortical epilepsy: additional value and comparison with ICEEG. Epilepsy Behav 2012;24:234–240.
Zakaria T, Noe K, So E et al. Scalp and intracranial EEG in medically intractable extratemporal epilepsy with normal MRI. ISRN Neurol 2012;2012:942849.
Funke ME, Moore K, Orrison WW Jr. et al. The role of magnetoencephalography in ‘nonlesional’ epilepsy. Epilepsia 2011;52:10–14.
Kuba R, Tyrlikova I, Chrastina J et al. ‘MRI-negative PET-positive’ temporal lobe epilepsy: invasive EEG findings, histopathology, and postoperative outcomes. Epilepsy Behav 2011;22:537–541.
Bien CG, Szinay M, Wagner J et al. Characteristics and surgical outcomes of patients with refractory magnetic resonance imaging-negative epilepsies. Arch Neurol 2009;66:1491–1499.
Jeha LE, Najm I, Bingaman W et al. Surgical outcome and prognostic factors of frontal lobe epilepsy surgery. Brain 2007;130:574–584.
Frater JL, Prayson RA, Morris IH et al. Surgical pathologic findings of extratemporal-based intractable epilepsy: a study of 133 consecutive resections. Arch Pathol Lab Med 2000;124:545–549.
Sloviter RS . The functional organization of the hippocampal dentate gyrus and its relevance to the pathogenesis of temporal lobe epilepsy. Ann Neurol 1994;35:640–654.
Smith JR, Lee MR, King DW et al. Results of lesional vs. nonlesional frontal lobe epilepsy surgery. Stereotact Funct Neurosurg 1997;69:202–209.
Duchowny M, Jayakar P, Resnick T et al. Epilepsy surgery in the first three years of life. Epilepsia 1998;39:737–743.
Kuzniecky R, Gilliam F, Morawetz R et al. Occipital lobe developmental malformations and epilepsy: clinical spectrum, treatment, and outcome. Epilepsia 1997;38:175–181.
Sinclair DB, Aronyk K, Snyder T et al. Extratemporal resection for childhood epilepsy. Pediatr Neurol 2004;30:177–185.
Elsharkawy AE, Behne F, Oppel F et al. Long-term outcome of extratemporal epilepsy surgery among 154 adult patients. J Neurosurg 2008;108:676–686.
Elsharkawy AE, Pannek H, Schulz R et al. Outcome of extratemporal epilepsy surgery experience of a single center. Neurosurgery 2008;63:516–525 discussion 25-6.
Blümcke I, Thom M, Aronica E et al. The clinicopathologic spectrum of focal cortical dysplasias: a consensus classification proposed by an ad hoc Task Force of the ILAE Diagnostic Methods Commission. Epilepsia 2011;52:158–174.
Palmini A, Najm I, Avanzini G et al. Terminology and classification of the cortical dysplasias. Neurology 2004;62:S2–S8.
Blümcke I, Pauli E, Clusmann H et al. A new clinico-pathological classification system for mesial temporal sclerosis. Acta Neuropathol 2007;113:235–244.
Prayson RA . Diagnostic challenges in the evaluation of chronic epilepsy-related surgical neuropathology. Am J Surg Pathol 2010;34:e1–13.
Engel JJ, Van NP, Rasmussen TB et al. Outcome with respect to epileptic seizures. In: Engel JJ (ed). Surgical Treatment of the Epilepsies. Raven Press: New York, NY, USA, 1993.
Ansari SF, Maher CO, Tubbs RS et al. Surgery for extratemporal nonlesional epilepsy in children: a meta-analysis. Childs Nerv Syst 2010;26:945–951.
Ansari SF, Tubbs RS, Terry CL et al. Surgery for extratemporal nonlesional epilepsy in adults: an outcome meta-analysis. Acta Neurochir (Wien) 2010;152:1299–1305.
Widdess-Walsh P, Kellinghaus C, Jeha L et al. Electro-clinical and imaging characteristics of focal cortical dysplasia: correlation with pathological subtypes. Epilepsy Res 2005;67:25–33.
Wyllie E, Comair YG, Kotagal P et al. Seizure outcome after epilepsy surgery in children and adolescents. Ann Neurol 1998;44:740–748.
Krsek P, Maton B, Korman B et al. Different features of histopathological subtypes of pediatric focal cortical dysplasia. Ann Neurol 2008;63:758–769.
Krsek P, Pieper T, Karlmeier A et al. Different presurgical characteristics and seizure outcomes in children with focal cortical dysplasia type I or II. Epilepsia 2009;50:125–137.
Widdess-Walsh P, Diehl B, Najm I . Neuroimaging of focal cortical dysplasia. J Neuroimaging 2006;16:185–196.
Rosenow F, Luders H . Presurgical evaluation of epilepsy. Brain 2001;124:1683–1700.
Najm IM, Ying Z, Babb T et al. Epileptogenicity correlated with increased N-methyl-D-aspartate receptor subunit NR2A/B in human focal cortical dysplasia. Epilepsia 2000;41:971–976.
Smith AP, Sani S, Kanner AM et al. Medically intractable temporal lobe epilepsy in patients with normal MRI: surgical outcome in twenty-one consecutive patients. Seizure 2011;20:475–479.
Jeha LE, Morris HH, Burgess RC . Coexistence of focal and idiopathic generalized epilepsy in the same patient population. Seizure 2006;15:28–34.
Bulacio JC, Jehi L, Wong C et al. Long-term seizure outcome after resective surgery in patients evaluated with intracranial electrodes. Epilepsia 2012;53:1722–1730.
Jehi L, Sarkis R, Bingaman W et al. When is a postoperative seizure equivalent to ‘epilepsy recurrence’ after epilepsy surgery? Epilepsia 2010;51:994–1003.
Cruz VB, Prayson RA . Neuropathology in patients with multiple surgeries for medically intractable epilepsy. Ann Diagn Pathol 2012;16:447–453.
Leite JP, Neder L, Arisi GM et al. Plasticity, synaptic strength, and epilepsy: what can we learn from ultrastructural data? Epilepsia 2005;46 (Suppl 5):134–141.
Schwartzkroin PA, Wenzel HJ . Are developmental dysplastic lesions epileptogenic? Epilepsia 2012;53 (Suppl 1):35–44.
Gao J, Chi ZF, Liu XW et al. Mitochondrial dysfunction and ultrastructural damage in the hippocampus of pilocarpine-induced epileptic rat. Neurosci Lett 2007;411:152–157.
Gleeson JG, Walsh CA . Neuronal migration disorders: from genetic diseases to developmental mechanisms. Trends Neurosci 2000;23:352–359.
Winden KD, Karsten SL, Bragin A et al. A systems level, functional genomics analysis of chronic epilepsy. PLoS One 2011;6:e20763.
Liu YW, Mee EW, Bergin P et al. Adult neurogenesis in mesial temporal lobe epilepsy: a review of recent animal and human studies. Curr Pharm Biotechnol 2007;8:187–194.
Scharfman HE, McCloskey DP . Postnatal neurogenesis as a therapeutic target in temporal lobe epilepsy. Epilepsy Res 2009;85:150–161.
Acknowledgements
Financial support of this project is provided by the Cleveland Clinic Epilepsy Center.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
Andreas V Alexopoulos serves on the editorial board of Epileptic Disorders, and has received research support from UCB, Pfizer Inc, and from the American Epilepsy Society. Imad M Najm is on the Speakers’ Bureau of UCB Inc and receives research funding from the US Department of Defense. The remaining authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Wang, Z., Alexopoulos, A., Jones, S. et al. The pathology of magnetic-resonance-imaging-negative epilepsy. Mod Pathol 26, 1051–1058 (2013). https://doi.org/10.1038/modpathol.2013.52
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/modpathol.2013.52
Keywords
This article is cited by
-
White matter alterations in MR-negative temporal and frontal lobe epilepsy using fixel-based analysis
Scientific Reports (2023)
-
Diagnostic Accuracy of Epilepsy-dedicated MRI with Post-processing
Clinical Neuroradiology (2023)
-
The clinical application of neuro-robot in the resection of epileptic foci: a novel method assisting epilepsy surgery
Journal of Robotic Surgery (2023)
-
Imaging in medically refractory epilepsy at 3 Tesla: a 13-year tertiary adult epilepsy center experience
Insights into Imaging (2022)
-
MRI of focal cortical dysplasia
Neuroradiology (2022)