Abstract
Bladder cancer is the most common malignant tumor of the urothelium and is classified into non-muscle-invasive bladder cancer (NMIBC) and muscle-invasive bladder cancer (MIBC). Stemness markers such as SOX2 and NANOG are frequently overexpressed in various aggressive cancers, including MIBC; epithelial–mesenchymal transition (EMT) has been proposed as a potential trigger of stemness in cancers. To determine whether cancer stemness is acquired via EMT in bladder cancer, we studied the effect of EMT on the expression of SOX2 and NANOG in bladder cancer cell lines. We also analyzed their expression in clinical tissue samples. Our results revealed that a potent EMT inducer (transforming growth factor β1) reduced the expression of the epithelial marker E-cadherin and increased expression of both SOX2 and NANOG in epithelial-type bladder cancer cells. As for clinical bladder cancer samples, in NMIBC, E-cadherin expression was slightly diminished, and the expression of both SOX2 and NANOG was negligible. In contrast, in MIBC, E-cadherin expression was highly and heterogeneously diminished, while the expression of both SOX2 and NANOG was increased. We also noticed that either E-cadherin or SOX2 (or NANOG) was expressed (ie, in a manner exclusive of each other). In addition, the concentration of E-cadherin showed a significant negative correlation with tumor grade and stage, while expression of SOX2 and NANOG positively correlated with those clinicopathological parameters. These findings suggest that EMT promotes stemness of bladder cancer cells, contributing to tumor aggressiveness. This EMT–cancer stemness axis may also play an important role in the pathogenesis of NMIBC and MIBC.
Similar content being viewed by others
Main
Bladder cancer, originating from the urothelial epithelium, is the most common cancer of the human urinary tract and is the ninth most common cancer worldwide; it is relatively frequent in developed countries.1 Bladder cancers are categorized into two subtypes based on their clinicopathology: non-muscle-invasive bladder cancer (NMIBC) and muscle-invasive bladder cancer (MIBC).2, 3 Approximately 80% of patients with bladder cancer present with NMIBC, which is associated with lower mortality despite a high risk of intravesical tumor recurrence.2, 3 The remaining 20% of patients present with MIBC, which frequently invades surrounding tissues and metastasizes to lymph nodes and distant organs and poses a higher mortality risk.2, 3
Epithelial–mesenchymal transition (EMT) is involved in cancer invasion and metastasis and is associated with poor prognosis of bladder cancer.4 Cancer cells that have undergone EMT share numerous molecular characteristics with cancer stem cells or cancer stem-like cells (CSCs).5 Notably, EMT was reported to have a role in the formation of CSCs in breast cancer.6 Thereafter, EMT has been known to be important for acquisition of the CSCs phenotype.7, 8, 9, 10 Bladder CSCs were first reported in 2009;11 since then, considerable evidence supporting the existence of bladder CSCs has been presented.12, 13, 14 Unlike other tumor cells, bladder CSCs likely emerge from pre-existing cancer cells at the late stages of bladder cancer,14 suggesting that bladder cancer cells acquire the phenotype of CSCs through EMT.15
Three transcription factors—SOX2, OCT3/4, and NANOG—coordinately determine self-renewal and differentiation in embryonic stem cells.16 These molecules also perform an important function in oncogenesis-related processes. The target genes activated by these molecules are more frequently overexpressed in poorly differentiated tumors than in well-differentiated ones.17 SOX2 and NANOG regulate self-renewal and maintenance in CSC populations.18, 19 SOX2 and NANOG expression levels have been reported to correlate well with the malignancy of bladder cancer.20, 21
Here, our hypothesis was that EMT increases the expression of stemness markers SOX2 and NANOG in bladder cancer cell lines. We assessed the associations between an epithelial marker, E-cadherin, and stemness markers SOX2 and NANOG in clinical tumor samples. Our findings further support the significance of EMT and CSCs in the pathogenesis of bladder cancer.
Materials and methods
Cell Lines and Reagents
Human bladder cancer cell lines RT4, T24, and UM-UC-3 were acquired from the American Type Culture Collection (Manassas, VA, USA). The establishment of JTC-30 cells has been previously reported.22, 23 Both RT4 and JTC-30 cells were derived from patients with NMIBC and showed an epithelial phenotype,22, 24 whereas T24 and UM-UC-3 cells were derived from patients with MIBC and had a mesenchymal phenotype.22, 24, 25 The cells were cultured in Dulbecco’s modified Eagle’s medium (DMEM; Nacalai Tesque, Kyoto, Japan) supplemented with 10% of fetal bovine serum (Life Technologies, CA, USA). All the cells were cultured with 1% penicillin/streptomycin (Life Technologies) at 5% CO2 and 37 °C. For induction of EMT, RT4 and JTC-30 cells were grown in serum-free DMEM for 24 h, and then cultured in the presence or absence of recombinant human transforming growth factor β1 (TGF-β1; Peprotech, NJ, USA) for additional 48 h.
Patients and Clinical Samples
The study protocol was reviewed and approved by the institutional review boards of the Tokyo Metropolitan Institute of Medical Science as well as the Tokyo Metropolitan Cancer and Infectious diseases Center Komagome Hospital. We analyzed surgical specimens obtained by transurethral resection or a biopsy from 63 patients with bladder cancer between 2013 and 2014. Histological types were determined according to the 2004 WHO classification of bladder cancers.26 All the patients received a diagnosis of urothelial carcinoma, except one, who had adenocarcinoma. The average age of the patients was 71 years (ranging from 39 to 94 years). Patients were subdivided into pairs of groups based on clinical parameters for statistical analysis (age, ≤70 and ≥71; sex, men and women; primary tumor and recurrence; TNM stage, ≤Stage I and ≥Stage II; tumor grade, low-grade and high-grade; Ki-67 labeling index (LI), <20% and ≥20%).
Real-Time PCR
Total RNA from the cultured cells was extracted using the ISOGEN II kit (Nippon Gene, Tokyo, Japan). First-strand cDNA was synthesized from the total RNA using the SuperScript VILO cDNA Synthesis Kit (Life Technologies). FastStart Universal SYBR Green Master Mix (Roche, Basel, Switzerland) and gene-specific primers were added, and real-time PCR for transcript quantification was conducted using the Stratagene Mx3005P multiplex quantitative PCR system. Sequences of the primers are given below (5′→3′):
E-cadherin, forward: 5′-CCCGGGACAACGTTTATTA-3′, reverse: 5′-GCTGGCTCAAGTCAAAGTCC-3′;
N-cadherin, forward: 5′-ACAGTGGCCACCTACAAAGG-3′, reverse: 5′-CCGAGATGGGGTTGATAATG-3′;
vimentin, forward: 5′-AAAGTGTGGCTGCCAAGAAC-3′, reverse: 5′-AGCCTCAGAGAGGTCAGCAA-3′;
and β-actin, forward: 5′-GTGGGGCGCCCCAGGCACCA-3′, reverse: 5′-TGGGTCATCTTCTCGCGGTT-3′.
Relative quantities of mRNA were calculated using the comparative CT method after normalization to β-actin. All the experiments were carried out in triplicate and repeated at least twice.
An Immunoblot Assay
For cell lysis, the cells were washed with phosphate-buffered saline and resuspended in RIPA buffer (150 mM NaCl, 1% Triton X-100, 0.5% DOC [deoxycholic acid], 0.1% SDS, 50 mM Tris-HCl [pH 7.5], and 5 mM EDTA) with protease inhibitor cocktail tablets (Roche) and Benzonase Nuclease (Santa Cruz Biotechnology, Dallas, TX, USA). The protein concentration in each lysate was determined using a BCA Protein Assay Kit (Thermo Fisher Scientific, Waltham, MA, USA). After SDS-PAGE, the proteins were transferred onto Immobilon-P transfer membranes (Millipore, Bedford, MA, USA). The membranes were blocked for 20 min in Blocking One buffer (Nacalai Tesque) and probed overnight with primary antibodies for E-cadherin, ZO-1, SOX2, NANOG, tubulin (all from Cell Signaling Technology, Danvers, MA), fibronectin (Novus Biologicals, Littleton, CO), and β-actin (Sigma-Aldrich, St. Louis, MO, USA). A horseradish peroxidase (HRP)-conjugated anti-rabbit or anti-mouse IgG antibody (GE Healthcare, Buckinghamshire, UK) served as the secondary antibody. Immunoreactive bands were visualized by means of Chemi-Lumi One (Nacalai Tesque). All the assays were performed at least three times. The protein levels were quantified by densitometry in the ImageJ software (National Institutes of Health, Bethesda, MD, USA) and were normalized to β-actin or tubulin.
Immunohistochemistry (IHC)
IHC was performed on 5-μm-thick formalin-fixed paraffin-embedded tissue slices. Hematoxylin and eosin (HE) staining was performed on all the samples. Antigen retrieval was carried out by autoclaving for 20 min in 50 mM citrate buffer. The slides were then reacted with primary antibodies against E-cadherin, SOX2, NANOG, and the proliferation marker Ki-67 (MIB-1; Dako Corporation, Carpenteria, CA, USA). The slides were developed by means of the VECTASTAIN Elite ABC kit and 3,3′-diaminobenzidine tetrahydro-chloride (DAB; Vector Laboratories, CA, USA). Hematoxylin was used as the counterstain. The expression and staining intensity on tissue slices were scored semiquantitatively by three authors (TM, AU, and SH) who did not have knowledge of the patients’ clinical data. The scoring scale was as follows: 0=no; +1=weak; +2=moderate; and +3=strong. The Ki-67 labeling index (LI) was determined by enumerating more than 1000 tumor cells including Ki-67-positive and -negative cells, and was expressed as the percentage of cells positive for nuclear staining.
The Cancer Genomics Database
Gene expression datasets of E-cadherin, SOX2, and NANOG in bladder cancer were retrieved from the public database cBioPortal for cancer genomics (www.cbioportal.org). We obtained the profile of expression of these genes in bladder cancer from a study on Bladder Urothelial Carcinoma (TCGA, Provisional; 413 samples from 412 patients). The data from massively parallel high-throughput RNA sequencing (RNA-Seq) were processed by means of RNA Seq V2 RSEM (RNA-Seq by Expectation-Maximization) to estimate the abundance of the transcripts of these genes.
Statistical Analysis
Continuous variables were analyzed by two-tailed Student’s t test with unequal variance. The statistically significant differences among the IHC scores on E-cadherin, NANOG, and SOX2 were examined by the Wilcoxon rank-sum test or Spearman’s rank correlation coefficient test. The correlations between the clinicopathological parameters and the expression levels of E-cadherin, NANOG, and SOX2 were evaluated by Pearson’s χ2-test. The cBioPortal database provided Spearman’s correlation coefficients for the correlations between E-cadherin and SOX2 and those between E-cadherin and NANOG. All statistical analyses were conducted in the JMP software, version 10 (SAS Institute, Cary, NC, USA). In all the analyses, data with P<0.05 were considered statistically significant.
Results
EMT Induces Expression of Cancer Stemness Markers in Bladder Cancer Cells
Bladder cancer cell lines RT4, JTC-30, T24, and UM-UC-3 were cultured for 48 h, and cell morphology was examined by phase contrast microscopy. RT4 and JTC-30 cells proliferated while maintaining cell–cell adhesion, forming island-like colonies (Figure 1a, left two panels). By contrast, T24 and UM-UC-3 cells showed lesser adhesion and tended to proliferate individually (Figure 1a, right two panels). We next examined the expression levels of epithelial (E-cadherin) and mesenchymal markers (N-cadherin and vimentin) in these cells. RT4 and JTC-30 cells had high levels of the E-cadherin transcript; however, the N-cadherin and vimentin transcripts were undetectable (Figure 1b). This finding is consistent with other studies, which showed that both N-cadherin and vimentin are not expressed in these cell lines.22, 27, 28, 29 In contrast, T24 and UM-UC-3 cells had undetectable levels of the E-cadherin transcript but had plenty of N-cadherin and vimentin transcripts (Figure 1b). Furthermore, the E-cadherin, N-cadherin, and vimentin protein concentrations corresponded to the mRNA expression, as confirmed by the immunoblot assay (Figure 1c). These findings indicated that RT4 and JTC-30 cells had an epithelial phenotype, whereas T24 and UM-UC-3 cells had a mesenchymal phenotype.
Phenotypic classification of bladder cancer cell lines by epithelial or mesenchymal markers. (a) Morphology of bladder cancer cell lines RT4, JTC30, T24, and UM-UC-3 in culture dishes. Cells were examined by phase contrast microscopy. Original magnification: × 200. (b) cDNA was synthesized from total RNA of each cell line, and real-time PCR was conducted for E-cadherin, N-cadherin, and vimentin. β-Actin served as an internal control. (c) An immunoblot assay for E-cadherin, N-cadherin, vimentin, and β-actin expression was performed on all cell lines. Bar graphs represent the average levels of each protein normalized to β-actin, as determined by densitometry.
TGF-β1 treatment induces EMT in urothelial cancer cells showing epithelial features.30, 31 In RT4 cells, which had an epithelial phenotype, we induced EMT by TGF-β1 treatment. The protein expression of the epithelial makers, E-cadherin and ZO-1, was reduced by TGF-β1 treatment in a dose-dependent manner (0–5 ng/ml), whereas protein concentration of the mesenchymal maker fibronectin increased (Figure 2). Furthermore, expression of SOX2 and NANOG increased in response to TGF-β1 treatment in a dose-dependent manner (Figure 2). We also confirmed TGF-β1-mediated SOX2 and NANOG expression in another epithelial cell line, JTC30 (Supplementary Figure 1). These results suggested that TGF-β1-induced EMT promoted the expression of stemness markers in bladder cancer cells.
Transforming growth factor β1 (TGF-β1)-induced EMT increases the expression of SOX2 and NANOG. RT4 cells were cultured in the absence of serum for 24 h and then treated with the indicated concentrations of TGF-β1 for 48 h. Protein was extracted from the cells and an immunoblot assay for E-cadherin, ZO-1, Fibronectin, SOX2, NANOG, and β-actin was carried out. Bar graphs represent the average concentrations of each protein normalized to β-actin, as determined by densitometry. *Statistically significant. EMT, epithelial–mesenchymal transition.
Differential Expression Patterns of EMT and Stemness Markers in Clinical NMIBC and MIBC Samples
We next evaluated EMT and cancer stemness in clinical samples of bladder cancer tissues including NMIBC (pT1 or lesser) and MIBC (pT2 or greater) and performed IHC analysis for E-cadherin, SOX2, and NANOG.
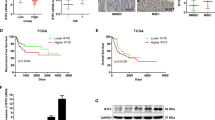
In normal urothelial cells, E-cadherin was localized to the cell membrane, and its expression was abundant although both NANOG and SOX2 expression levels were miniscule in serial sections (Supplementary Figure 2). In cancer cells, E-cadherin expression was slightly decreased in NMIBC cells and remarkably decreased in MIBC cells (Figure 3a, upper panels). Cytoplasmic and nuclear NANOG expression was low or undetectable in NMIBC cells; however, it was strong in MIBC cells (Figure 3a, middle panels). In concordance with this expression pattern of NANOG, cytoplasmic and nuclear SOX2 expression was also low or undetectable in NMIBC cells but strong in MIBC cells (Figure 3a, lower panels).
Differential expression of E-cadherin, NANOG, and SOX2 in NMIBC and MIBC. (a) A representative image from IHC analysis for E-cadherin, NANOG, and SOX2 in serial sections. Original magnification × 200. (b) E-cadherin, NANOG, and SOX2 expression levels were semiquantitatively scored in NMIBC and MIBC cells. Data are the percentages of patients with E-cadherin scores in each group. Statistical analysis was performed by the Wilcoxon rank-sum test. *Statistically significant. (c) Hematoxylin and eosin staining shows a noninvasive area (i) and invasive area (ii) in a single tumor. A representative image from IHC analysis of the noninvasive and invasive areas in serial sections. Original magnification: × 400. IHC, immunohistochemical; MIBC, muscle-invasive bladder cancer; NMIBC, non-muscle-invasive bladder cancer.
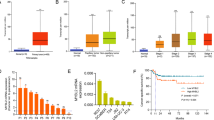
Statistical analysis revealed that E-cadherin expression was significantly lower in MIBC cells than in NMIBC cells (P<0.0001, Figure 3b). In contrast, the expression levels of NANOG and SOX2 were significantly higher in MIBC cells as compared to NMIBC cells (P<0.0001 and P<0.0001, respectively; Figure 3b). To confirm that the decreased level of E-cadherin and increased levels of NANOG (or SOX2) are generally observed in MIBC, we analyzed the mRNA expression of E-cadherin, NANOG, and SOX2 in tumor samples from 412 patients with bladder cancer using a public database cBioPortal for cancer genomics. Although the differences were not significant, decreased expression of E-cadherin and increased expression of NANOG (or SOX2) were clearly observed in tumors at stages II–IV compared with those with stage I (Supplementary Figure 3a).
EMT frequently occurs at the invasive front of various cancers. As expected, E-cadherin expression was high in noninvasive areas, while that of both NANOG and SOX2 was low in the same areas of a serial section (Figure 3c, (i)). In contrast, at the invasive front, E-cadherin expression was found to be reduced, while both NANOG and SOX2 expression levels were increased (Figure 3c, (ii)). These findings suggested that EMT and cancer stemness were promoted in MIBC.
An Inverse Relation Between E-cadherin and SOX2 (or NANOG) Expression in Clinical Bladder Cancer
E-cadherin expression was likely to have an inverse correlation with NANOG or SOX2 expression (Supplementary Figure 4a). The expression of E-cadherin and NANOG was mutually exclusive in MIBC serial sections (Figure 4a). Similarly, the expression patterns of E-cadherin and SOX2 were also mutually exclusive in a patient with MIBC (Figure 4a). To assess the relation between E-cadherin and SOX2 (or NANOG), we compared the expression levels of E-cadherin and NANOG (SOX2) in clinical samples including NMIBC and MIBC. We found a significant inverse correlation between E-cadherin and NANOG expression (ρ=−0.3078, P=0.0141), and between E-cadherin and SOX2 expression (ρ=−0.4763, P<0.0001; Figure 4b). The public database cBioPortal also showed that although not significant, there was an inverse correlation between mRNA levels of E-cadherin and NANOG (ρ=−0.012) and between mRNA levels of E-cadherin and SOX2 (ρ=−0.057; Supplementary Figure 3b). In addition, there was a significant positive correlation between SOX2 and NANOG expression (ρ=0.4173, P=0.0007; Supplementary Figure 4b). These findings suggested that there was an inverse correlation between E-cadherin and SOX2 (or NANOG) expression in clinical bladder cancer.
Inverse correlation between E-cadherin and NANOG (or SOX2) expression in bladder cancer. Immunohistochemical analysis for E-cadherin, NANOG, and SOX2 was performed on serial sections of bladder cancer. (a) Left panels: representative images of E-cadherin and NANOG expression in a serial section of a patient with MIBC. Reduced E-cadherin expression corresponded to increased NANOG expression on the left side separated by dotted line, and vice versa on the right-hand side. (right) a representative image of E-cadherin and SOX2 expression in a serial section of another patient with MIBC. Reduced E-cadherin expression corresponded to increased SOX2 expression in the upper region separated by the dotted line, and vice versa in the lower region. Original magnification: × 200. (b) The left bar graph shows the percentages of patients with NANOG scores for each E-cadherin score. The right-hand bar graph shows the percentages of patients with SOX2 scores for each E-cadherin score. Statistical analysis was performed by Spearman’s rank correlation coefficient test; ρ: correlation coefficients. *Statistically significant. MIBC, muscle-invasive bladder cancer.
Expression of E-cadherin, NANOG and SOX2 Correlates with Tumor Aggressiveness in Bladder Cancer
The relations among E-cadherin, NANOG, SOX2, and clinicopathological features of all the studied cases are summarized in Table 1. E-cadherin expression significantly correlated with a lower TNM stage (P=0.0009) or lower tumor grade (p=0.0017). NANOG expression significantly correlated with a higher TNM stage (P=0.0109), higher tumor grade (P=0.0005), or higher Ki-67 LI (P=0.029). SOX2 expression was significantly higher in recurrent tumors (P=0.0303) and tumors with a higher TNM stage (P=0.0108), higher grade (P<0.0001), or higher Ki-67 LI (P<0.0001). In addition, Ki-67 LI was significantly higher in MIBC than in NMIBC (Supplementary Figure 5a). Ki-67 LI was negatively associated with the E-cadherin expression level and positively associated with both NANOG and SOX2 expression levels (Supplementary Figure 5b).
These findings suggested that bladder cancer progression involved decreased protein levels of E-cadherin and increased protein levels of NANOG (or SOX2).
Discussion
EMT and CSCs share a molecular network and both are functionally linked to bladder cancer biology including transdifferentiation, resistance to treatment, tumor heterogeneity, and tumor progression.5, 32 As stated in our review focused on the origin of bladder CSC, bladder cancer may acquire the CSC phenotype later in tumor development.15 EMT may contribute to this process because of the following evidence: (1) stem-like characteristics of bladder cancer are not observed until late in tumor development;14 (2) most bladder CSCs have been identified in MIBC, which is frequently associated with EMT but not identified in NMIBC;11, 15 (3) some of NMIBCs (10–15%) eventually progress to MIBC but not the other way around; this situation corresponds to the process of EMT within solid tumors.3
We demonstrated that EMT is associated with the expression of stemness markers SOX2 and NANOG in bladder cancer. TGF-β1 treatment decreased the expression of epithelial markers (including E-cadherin) and increased SOX2 and NANOG expression in bladder cancer cell lines. NMIBC clinical samples showed a slight and homogeneous reduction in E-cadherin expression without any changes in SOX2 or NANOG expression. In contrast, a strong reduction in E-cadherin expression and increased SOX2 and NANOG expression were frequently observed in MIBC. Thus, there is likely a threshold of the E-cadherin level below which EMT and EMT-induced cancer stemness are initiated. It has been reported that a direct knockdown of E-cadherin increases the number of CSCs, drug resistance, and metastasis in breast epithelial cells33, 34 and enriches CSCs among colorectal cancer cells.35 Moreover, the E-cadherin knockdown enhances expression of pluripotency genes including SOX2 in A549 lung cancer cells.36 On the other hand, there is evidence that SOX2 and NANOG regulate EMT and inhibit E-cadherin expression in various types of cancers.37, 38, 39 Therefore, there is likely some reciprocal regulation between E-cadherin and SOX2 (or NANOG). A loss of E-cadherin may trigger the development of cancer stemness and tumor aggressiveness.
On the basis of our results as well as those of others, we hypothesized a mechanism of bladder cancer formation and progression (Figure 5). Bladder cancers are believed to arise from distinct types of cells in normal urothelium.40 Primary bladder cancer cells may have different amounts of E-cadherin depending on their site of origin. A small reduction in E-cadherin expression does not alter SOX2 and NANOG expression but allows cancer cells to form a relatively organized structure with loose cell–cell adhesion. These cancer cells take root and get implanted at other sites in the bladder mucosa and proliferate via clonal expansion, becoming a highly recurrent tumor of the NMIBC type. In contrast, a severe reduction in E-cadherin expression, some of which may develop from small downregulation of E-cadherin, may enable the upregulation of SOX2 and NANOG and subsequently enhance cancer stemness, contributing to tumor heterogeneity. These cancer cells proliferate via clonal expansion, becoming a highly invasive or metastatic tumor of the MIBC type. Further research is needed to determine whether this hypothesis is correct.
A hypothetical mechanism of the development of NMIBC and MIBC. Bladder cancer may originate from a different site of the bladder urothelium, which expresses E-cadherin at various magnitudes. There may be a mechanism of reciprocal inhibition between E-cadherin and SOX2 (or NANOG) expression. Strong downregulation of E-cadherin may lead to cancer stemness. Bladder cancer cells may develop into NMIBCs or MIBCs via clonal expansion. MIBC, muscle-invasive bladder cancer; non-muscle-invasive bladder cancer, NMIBC.
This study, to the best of our knowledge, is the first to show a relation between EMT and cancer stemness in bladder cancer; it also provides a rationale for a treatment strategy targeting EMT or cancer stemness. We believe that our findings will provide new insights into the pathogenesis of NMIBC and MIBC, and that EMT inhibitors may improve the clinical outcomes of bladder cancer treatment.
References
Ferlay J, Soerjomataram I, Dikshit R et al, Cancer incidence and mortality worldwide: sources, methods and major patterns in GLOBOCAN 2012. Int J Cancer 2015; 136: E359–E386.
Knowles MA, Hurst CD . Molecular biology of bladder cancer: new insights into pathogenesis and clinical diversity. Nat Rev Cancer 2015; 15: 25–41.
McConkey DJ, Lee S, Choi W et al, Molecular genetics of bladder cancer: Emerging mechanisms of tumor initiation and progression. Urol Oncol 2010; 28: 429–440.
Baumgart E, Cohen MS, Silva Neto B et al, Identification and prognostic significance of an epithelial-mesenchymal transition expression profile in human bladder tumors. Clin Cancer Res 2007; 13: 1685–1694.
Kong D, Li Y, Wang Z et al, Cancer stem cells and epithelial-to-mesenchymal transition (EMT)-phenotypic cells: are they cousins or twins? Cancers (Basel) 2011; 3: 716–729.
Mani SA, Guo W, Liao MJ et al, The epithelial-mesenchymal transition generates cells with properties of stem cells. Cell 2008; 133: 704–715.
Polyak K, Weinberg RA . Transitions between epithelial and mesenchymal states: acquisition of malignant and stem cell traits. Nat Rev Cancer 2009; 9: 265–273.
Singh A, Settleman J . EMT, cancer stem cells and drug resistance: an emerging axis of evil in the war on cancer. Oncogene 2010; 29: 4741–4751.
Abell AN, Johnson GL . Implications of mesenchymal cells in cancer stem cell populations: relevance to EMT. Curr Pathobiol Rep 2014; 2: 21–26.
Liu X, Fan D . The epithelial-mesenchymal transition and cancer stem cells: functional and mechanistic links. Curr Pharm Des 2015; 21: 1279–1291.
Chan KS, Espinosa I, Chao M et al, Identification, molecular characterization, clinical prognosis, and therapeutic targeting of human bladder tumor-initiating cells. Proc Natl Acad Sci USA 2009; 106: 14016–14021.
Shin K, Lim A, Odegaard JI et al, Cellular origin of bladder neoplasia and tissue dynamics of its progression to invasive carcinoma. Nat Cell Biol 2014; 16: 469–478.
Ho PL, Lay EJ, Jian W et al, Stat3 activation in urothelial stem cells leads to direct progression to invasive bladder cancer. Cancer Res 2012; 72: 3135–3142.
Bryan RT . Bladder cancer and cancer stem cells: basic science and implications for therapy. ScientificWorldJournal 2011; 11: 1187–1194.
Ohishi T, Koga F, Migita T . Bladder cancer stem-like cells: their origin and therapeutic perspectives. Int J Mol Sci 2016; 17: E43.
Wang J, Rao S, Chu J et al, A protein interaction network for pluripotency of embryonic stem cells. Nature 2006; 444: 364–368.
Ben-Porath I, Thomson MW, Carey VJ et al, An embryonic stem cell-like gene expression signature in poorly differentiated aggressive human tumors. Nat Genet 2008; 40: 499–507.
Weina K, Utikal J . SOX2 and cancer: current research and its implications in the clinic. Clin Transl Med 2014; 3: 19.
Jeter CR, Badeaux M, Choy G et al, Functional evidence that the self-renewal gene NANOG regulates human tumor development. Stem Cells 2009; 27: 993–1005.
Ruan J, Wei B, Xu Z et al, Predictive value of Sox2 expression in transurethral resection specimens in patients with T1 bladder cancer. Med Oncol 2013; 30: 445.
Zhang Y, Wang Z, Yu J et al, Cancer stem-like cells contribute to cisplatin resistance and progression in bladder cancer. Cancer Lett 2012; 322: 70–77.
Fukushima H, Koga F, Kawakami S et al, Loss of DeltaNp63alpha promotes invasion of urothelial carcinomas via N-cadherin/Src homology and collagen/extracellular signal-regulated kinase pathway. Cancer Res 2009; 69: 9263–9270.
Kakuya T, Yamada T, Yokokawa M et al, Establishment of cell strains from human urothelial carcinoma and their morphological characterization. In Vitro 1983; 19: 591–599.
Urist MJ, Di Como CJ, Lu ML et al, Loss of p63 expression is associated with tumor progression in bladder cancer. Am J Pathol 2002; 161: 1199–1206.
Rieger KM, Little AF, Swart JM et al, Human bladder carcinoma cell lines as indicators of oncogenic change relevant to urothelial neoplastic progression. Br J Cancer 1995; 72: 683–690.
Eble JN SG, Epstein JI et al, World Health Organization Classification of Tumours. Pathology and Genetics of Tumours of the Urinary System and Male Genital Organs. IARC Press: Lyon, France, 2014.
Rieger-Christ KM, Ng L, Hanley RS et al, Restoration of plakoglobin expression in bladder carcinoma cell lines suppresses cell migration and tumorigenic potential. Br J Cancer 2005; 92: 2153–2159.
Reyes-Mugica M, Meyerhardt JA, Rzasa J et al, Truncated DCC reduces N-cadherin/catenin expression and calcium-dependent cell adhesion in neuroblastoma cells. Lab Invest 2001; 81: 201–210.
Lascombe I, Clairotte A, Fauconnet S et al, N-cadherin as a novel prognostic marker of progression in superficial urothelial tumors. Clin Cancer Res 2006; 12: 2780–2787.
Geng J, Fan J, Ouyang Q et al, Loss of PPM1A expression enhances invasion and the epithelial-to-mesenchymal transition in bladder cancer by activating the TGF-beta/Smad signaling pathway. Oncotarget 2014; 5: 5700–5711.
Fan Y, Shen B, Tan M et al, TGF-beta-induced upregulation of malat1 promotes bladder cancer metastasis by associating with suz12. Clin Cancer Res 2014; 20: 1531–1541.
McConkey DJ, Choi W, Marquis L et al, Role of epithelial-to-mesenchymal transition (EMT) in drug sensitivity and metastasis in bladder cancer. Cancer Metastasis Rev 2009; 28: 335–344.
Onder TT, Gupta PB, Mani SA et al, Loss of E-cadherin promotes metastasis via multiple downstream transcriptional pathways. Cancer Res 2008; 68: 3645–3654.
Gupta PB, Onder TT, Jiang G et al, Identification of selective inhibitors of cancer stem cells by high-throughput screening. Cell 2009; 138: 645–659.
Ye J, Wu D, Shen J et al, Enrichment of colorectal cancer stem cells through epithelial-mesenchymal transition via CDH1 knockdown. Mol Med Rep 2012; 6: 507–512.
Farmakovskaya M, Khromova N, Rybko V et al, E-Cadherin repression increases amount of cancer stem cells in human A549 lung adenocarcinoma and stimulates tumor growth. Cell Cycle 2016; 15: 1084–1092.
Herreros-Villanueva M, Zhang JS, Koenig A et al, SOX2 promotes dedifferentiation and imparts stem cell-like features to pancreatic cancer cells. Oncogenesis 2013; 2: e61.
Siu MK, Wong ES, Kong DS et al, Stem cell transcription factor NANOG controls cell migration and invasion via dysregulation of E-cadherin and FoxJ1 and contributes to adverse clinical outcome in ovarian cancers. Oncogene 2013; 32: 3500–3509.
Han X, Fang X, Lou X et al, Silencing SOX2 induced mesenchymal-epithelial transition and its expression predicts liver and lymph node metastasis of CRC patients. PLoS One 2012; 7: e41335.
Van Batavia J, Yamany T, Molotkov A et al, Bladder cancers arise from distinct urothelial sub-populations. Nat Cell Biol 2014; 16: 982–991.
Acknowledgements
This work was supported by grants from the Japan Society for the Promotion of Science KAKENHI, grant number 23659314 (to FS) and 15K06891 (to TM), and the Tokyo Metropolitan Government for the Tokyo Metropolitan Clinical Research Grant (2014A1-01). We are grateful to Michiko Imanishi (Tokyo Metropolitan Institute of Medical Science) for technical support.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies the paper on the Laboratory Investigation website
Epithelial-mesenchymal transition (EMT) has been suggested as a potential cancer stemness trigger. The authors found that TGF-β induced-EMT increased SOX2 and Nanog protein levels in bladder cancer cells. Immunohistochemistry showed a mutually exclusive expression of E-cadherin and SOX2/Nanog. These findings suggest that EMT promotes stemness of bladder cancer, contributing to tumor aggressiveness.
Rights and permissions
About this article
Cite this article
Migita, T., Ueda, A., Ohishi, T. et al. Epithelial–mesenchymal transition promotes SOX2 and NANOG expression in bladder cancer. Lab Invest 97, 567–576 (2017). https://doi.org/10.1038/labinvest.2017.17
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/labinvest.2017.17
This article is cited by
-
The role of stromal cells in epithelial–mesenchymal plasticity and its therapeutic potential
Discover Oncology (2024)
-
PEX26 Functions as a Metastasis Suppressor in Colorectal Cancer
Digestive Diseases and Sciences (2024)
-
Harnessing function of EMT in cancer drug resistance: a metastasis regulator determines chemotherapy response
Cancer and Metastasis Reviews (2024)
-
TrkB inhibition of DJ-1 degradation promotes the growth and maintenance of cancer stem cell characteristics in hepatocellular carcinoma
Cellular and Molecular Life Sciences (2023)
-
Rethinking the biology of metastatic melanoma: a holistic approach
Cancer and Metastasis Reviews (2021)