Abstract
Objectives:
The life-course development of body mass index (BMI) may be driven by interactions between genes and obesity-inducing social environments. We examined whether lower parental or own education accentuates the genetic risk for higher BMI over the life course, and whether diet and physical activity account for the educational differences in genetic associations with BMI.
Subjects/Methods:
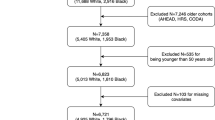
The study comprised 2441 participants (1319 women, 3–18 years at baseline) from the prospective, population-based Cardiovascular Risk in Young Finns Study. BMI (kg/m2) trajectories were calculated from 18 to 49 years, using data from six time points spanning 31 years. A polygenic risk score for BMI was calculated as a weighted sum of risk alleles in 97 single-nucleotide polymorphisms. Education was assessed via self-reports, measured prospectively from participants in adulthood and from parents when participants were children. Diet and physical activity were self-reported in adulthood.
Results:
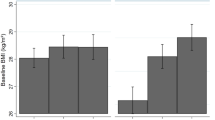
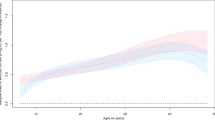
Mean BMI increased from 22.6 to 26.6 kg/m2 during the follow-up. In growth curve analyses, the genetic risk score was associated with faster BMI increase over time (b=0.02, (95% CI, 0.01–0.02, P<0.001)). The association between the genetic risk score and BMI was more pronounced among those with lower educational level in adulthood (b=−0.12 (95% CI, −0.23–0.01); P=0.036)). No interaction effect was observed between the genetic risk score and parental education (b=0.05 (95% CI, −0.09–0.18; P=0.51)). Diet and physical activity explained little of the interaction effect between the genetic risk score and adulthood education.
Conclusions:
In this prospective study, the association of a risk score of 97 genetic variants with BMI was stronger among those with low compared with high education. This suggests lower education in adulthood accentuates the risk of higher BMI in people at genetic risk.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
The Global BMI Mortality Collaboration. Body-mass index and all-cause mortality: Individual-participant-data meta-analysis of 239 prospective studies in four continents. Lancet 2016; 388: 776–786.
Kopelman PG . Obesity as a medical problem. Nature 2000; 404: 635–643.
Pi-Sunyer X . The medical risks of obesity. Postgr Med 2009; 121: 21–33.
Elks CE, Hoed M, den, Zhao JH, Sharp SJ, Wareham NJ, Loos RJF et al. Variability in the heritability of body mass index: a systematic review and meta-regression. Front Endocrinol (Lausanne) 2012; 3: 29.
Locke AE, Kahali B, Berndt SI, Justice AE, Pers TH, Day FR et al. Genetic studies of body mass index yield new insights for obesity biology. Nature 2015; 518: 197–206.
McLaren L . Socioeconomic status and obesity. Epidemiol Rev 2007; 29: 29–48.
Bann D, Johnson W, Li L, Kuh D, Hardy R . Socioeconomic inequalities in body mass index across adulthood: coordinated analyses of individual participant data from three british birth cohort studies initiated in 1946, 1958 and 1970. PLOS Med 2017; 14: e1002214.
Tyrrell J, Wood AR, Ames RM, Yaghootkar H, Beaumont RN, Jones SE et al. Gene–obesogenic environment interactions in the UK Biobank study. Int J Epidemiol 2017; 46: 559–575.
Speliotes EK, Willer CJ, Berndt SI, Monda KL, Thorleifsson G, Jackson AU et al. Association analyses of 249,796 individuals reveal 18 new loci associated with body mass index. Nat Genet 2010; 42: 937–948.
Liu H, Guo G . Lifetime socioeconomic status, historical context, and genetic inheritance in shaping body mass in middle and late adulthood. Am Sociol Rev 2015; 80: 705–737.
Darmon N, Drewnowski A . Does social class predict diet quality? Am J Clin Nutr 2008; 87: 1107–1117.
Drewnowski A, Specter SE . Poverty and obesity: the role of energy density and energy costs. Am J Clin Nutr 2004; 79: 6–16.
Lynch JW, Kaplan GA, Salonen J . Why do poor people behave poorly? Variation in adult health behaviors and psychosoocial characteristics by stages of the socioeconomic life course. Soc Sci Med 1997; 44: 809–819.
Hanson MD, Chen E . Socioeconomic status and health behaviors in adolescence: a review of the literature. J Behav Med 2007; 30: 263–285.
Pampel FC, Krueger P, Denney J . Socioeconomic disparities in health behaviors. Annu Rev Sociol 2010; 36: 349–370.
Qi Q, Chu AY, Kang JH, Jensen MK, Curhan GC, Pasquale LR et al. Sugar-sweetened beverages and genetic risk of obesity. N Engl J Med 2012; 367: 1387–1396.
Qi Q, Chu AY, Kang JH, Huang J, Rose LM, Jensen MK et al. Fried food consumption, genetic risk, and body mass index: gene-diet interaction analysis in three US cohort studies. BMJ 2014; 348: g1610.
Kilpeläinen T, Qi L, Brage S, Sharp SJ, Sonestedt E, Demerath E et al. Physical activity attenuates the influence of FTO Variants on obesity risk : a meta-analysis of 218,166 adults and 19,268 children. PLoS Med 2011; 8: e1001116.
Johnson W, Krueger RF . Genetic effects on physical health: lower at higher income levels. Behav Genet 2005; 35: 579–590.
Dinescu D, Horn E, Duncan G, Turkheimer E . Socioeconomic modifiers of genetic and environmental influences on body mass index in adult twins. Heal Psychol 2016; 35: 157–166.
Silventoinen K, Huppertz C, van Beijsterveldt CEM, Bartels M, Willemsen G, Boomsma DI . The genetic architecture of body mass index from infancy to adulthood modified by parental education. Obesity 2016; 24: 2004–2011.
Clarke P, O’Malley PM, Johnston LD, Schulenberg JE . Social disparities in BMI trajectories across adulthood by gender, race/ ethnicity and lifetime socio-economic position: 1986-2004. Int J Epidemiol 2009; 38: 499–509.
El-Sayed AM, Scarborough P, Galea S . Unevenly distributed: a systematic review of the health literature about socioeconomoic inequalities in adult obesity in the United Kingdom. BMC Public Health 2012; 12: 18.
Langenberg C, Hardy R, Kuh D, Brunner E, Wadsworth M . Central and total obesity in middle aged men and women in relation to lifetime socioeconomic status: evidence from a national birth cohort. J Epidemiol Community Health 2003; 57: 816–822.
Power C, Manor O, Matthews S . Child to adult socioeconomic conditions and obesity in a national cohort. Int J Obes 2003; 27: 1081–1086.
Strand B, Murray E, Guralnik J, Hardy R, Kuh D . Childhood social class and adult adiposity and blood-pressure trajectories 36-53 years: gender-specific results from a British birth cohort. J Epidemiol Community Health 2012; 66: 512–518.
Senese LC, Almeida ND, Fath AK, Smith BT, Loucks EB . Associations between childhood socioeconomic position and adulthood obesity. Epidemiol Rev 2009; 31: 21–51.
Pehkonen J, Viinikainen J, Böckerman P, Lehtimäki T, Pitkänen N, Raitakari OT . Genetic endowments, parental resources and adult health: evidence from the Young Finns Study. Soc Sci Med 2017, https://doi.org/10.1016/j.socscimed.2017.04.030.
Laitinen TT, Pahkala K, Magnussen CG, Viikari JSA, Oikonen M, Taittonen L et al. Ideal cardiovascular health in childhood and cardiometabolic outcomes in adulthood: the Cardiovascular Risk in Young Finns Study. Circulation 2012; 125: 1971–1978.
Lloyd-Jones DM, Hong Y, Labarthe D, Mozaffarian D, Appel LJ, Van Horn L et al. Defining and setting national goals for cardiovascular health promotion and disease reduction: the American Heart Association’s Strategic Impact Goal through 2020 and beyond. Circulation 2010; 121: 586–613.
Laitinen TT, Pahkala K, Venn A, Woo JG, Oikonen M, Dwyer T et al. Childhood lifestyle and clinical determinants of adult ideal cardiovascular health: the Cardiovascular Risk in Young Finns Study, the Childhood Determinants of Adult Health Study, the Princeton Follow-up Study. Int J Cardiol 2013; 169: 126–132.
Singer JD, Willett JB . Applied longitudinal data analysis. Modeling change and event occurrence. Oxford University Press: NY, USA, 2003.
Ahmad S, Poveda A, Shungin D, Barroso I, Hallmans G, Renström F et al. Established BMI-associated genetic variants and their prospective associations with BMI and other cardiometabolic traits: The GLACIER Study. Int J Obes 2016; : 1346–1352.
Johnson W, Kyvik KO, Skytthe A, Deary IJ, Sørensen TIA . Education modifies genetic and environmental influences on BMI. PLoS ONE 2011; 6: e16290.
Liu SY, Walter S, Marden J, Rehkopf DH, Kubzansky LD, Nguyen T et al. Genetic vulnerability to diabetes and obesity: does education offset the risk? Soc Sci Med 2015; 127: 150–158.
Lynch J, Kaplan G. Socioeconomic position. In: Berkman LF, Kawachi I (eds). Social epidemiology. Oxford University Press: NY, USA, 2000. pp 13–36.
Glymour M, Avendano M, Kawachi I. Socioeconomic status and health. In: Berkman LF, Kawachi I, Glymour M (eds). Social epidemiology. Oxford University Press: NY, USA, 2014. pp 17–62.
Chen E, Miller GE . Socioeconomic status and health : mediating and moderating factors. Annu Rev Clin Psychol 2013; 9: 723–749.
Marmot M, Wilkinson RG . Psychosocial and material pathways in the relation between income and health : a response to Lynch et al. BMJ 2001; 322: 1233–1236.
McEwen BS, Gianaros PJ . Central role of the brain in stress and adaptation: Links to socioeconomic status, health, and disease. Ann N Y Acad Sci 2010; 1186: 190–222.
Seeman T, Epel E, Gruenewald T, Karlamangla A, Mcewen BS . Socio-economic differentials in peripheral biology : Cumulative allostatic load. Ann N Y Acad Sci 2010; 1186: 223–239.
Zhang C, Rexrode KM, Van Dam RM, Li TY, Hu FB . Abdominal obesity and the risk of all-cause, cardiovascular, and cancer mortality: Sixteen years of follow-up in US women. Circulation 2008; 117: 1658–1667.
Acknowledgements
This study was supported by the Academy of Finland grants 265869 (Dr Keltikangas-Järvinen); 265977 (Dr Elovainio); 258578 (Dr Hintsanen); 286284, 134309 (Eye), 126925, 121584, 124282, 129378 (Salve), 117787 (Gendi), and 41071 (Skidi); the Social Insurance Institution of Finland; Kuopio, Tampere and Turku University Hospital Medical Funds (grant X51001); Juho Vainio Foundation; Paavo Nurmi Foundation; Finnish Foundation of Cardiovascular Research; Finnish Cultural Foundation; Tampere Tuberculosis Foundation; Emil Aaltonen Foundation; Yrjö Jahnsson Foundation; and Signe and Ane Gyllenberg Foundation (Dr Lehtimäki). The expert technical assistance in the statistical analyses by Irina Lisinen is gratefully acknowledged. The funding sources had no role in the design and conduct of the study; collection, management, analysis and interpretation of the data; preparation, review or approval of the manuscript; and decision to submit the manuscript for publication. This manuscript is an original contribution. Neither this manuscript or one with substantially similar content has been published or is being considered for publication elsewhere.
Author contributions
Ms Komulainen and Dr Pulkki-Råback had full access to all the data in the study and take responsibility for the integrity of the data and the accuracy of the data analysis; study concept and design: Komulainen, Pulkki-Råback, Jokela, Keltikangas-Järvinen; acquisition, analysis and interpretation of data: all authors; drafting of the manuscript: Komulainen, Pulkki-Råback, Jokela; critical revision of the manuscript for important intellectual content: all authors; statistical analysis: Komulainen, Jokela; obtained funding: Keltikangas-Järvinen, Elovainio, Hintsanen, Lehtimäki; study supervision: Raitakari, Lehtimäki, Keltikangas-Järvinen. All authors have given final approval of the submitted manuscript. All authors agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. The corresponding author (Pulkki-Råback) confirms to have the final responsibility for the decision to submit for publication.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies this paper on International Journal of Obesity website
Supplementary information
Rights and permissions
About this article
Cite this article
Komulainen, K., Pulkki-Raback, L., Jokela, M. et al. Education as a moderator of genetic risk for higher body mass index: prospective cohort study from childhood to adulthood. Int J Obes 42, 866–871 (2018). https://doi.org/10.1038/ijo.2017.174
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ijo.2017.174
This article is cited by
-
Healthy lifestyle practice correlates with decreased obesity prevalence in individuals with high polygenic risk: TMM CommCohort study
Journal of Human Genetics (2024)
-
Modeling Interaction and Dispersion Effects in the Analysis of Gene-by-Environment Interaction
Behavior Genetics (2022)
-
Genetic propensity for obesity, socioeconomic position, and trajectories of body mass index in older adults
Scientific Reports (2021)
-
Neighborhood deprivation index is associated with weight status among long-term survivors of childhood acute lymphoblastic leukemia
Journal of Cancer Survivorship (2021)