Host: Shamini Bundell
Welcome back to the Nature Podcast. This week, a potential vaccine for a neglected tropical disease…
Host: Benjamin Thompson
And the latest guidelines for human stem cell research. I’m Benjamin Thompson.
Host: Shamini Bundell
And I’m Shamini Bundell.
[Jingle]
Interviewer: Shamini Bundell
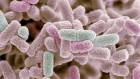
Trypanosomes are microscopic parasites – single-celled organisms that can cause serious diseases in humans and animals around the world. In livestock animals, certain species of trypanosomes can cause a disease called African animal trypanosomiasis (nagana) which causes significant economic impacts, primarily in sub-Saharan Africa. Researchers have been trying to develop a vaccine to protect animals against this disease, but trypanosome parasites have an array of tricks up their sleeve to outwit the immune system. Delphine Autheman is part of a team at the Sanger Institute in the UK who have been working on a way to identify potential antigens – proteins on the surface of the parasite that the host immune system can recognise and use to target the invasive cell. They’ve used this system to develop a vaccine candidate that targets the species Trypanosoma vivax, and it’s showing early promise. I wanted to find out more, so I gave Delphine a call and started by asking her how T. vivax affects livestock animals.
Interviewee: Delphine Autheman
So, for the animals it’s mainly loss of milk productivity, for example, and they have anaemia, so they are becoming weak. But if the animals are not treated, they die from nagana.
Interviewer: Shamini Bundell
So, what kind of treatments are available against the diseases, against the trypanosomes?
Interviewee: Delphine Autheman
So, it’s mainly old drugs which had been developed in the 50s. They are targeting some enzyme in the parasites, but there is more and more resistance, so we need new medication to continue controlling the disease.
Interviewer: Shamini Bundell
And so, your team has been working on a vaccine against a particular species of trypanosome. Why did you want to develop a vaccine rather than some sort of a treatment?
Interviewee: Delphine Autheman
Because it’s cost effective and because as trypanosomes are infecting wild animals, there is a reservoir for these parasites, so this means that your herd will always have to receive treatment drugs because they will be continually exposed to the parasites. So, if you vaccinate your animals, it will be more efficient than just having to treat continually your animals.
Interviewer: Shamini Bundell
And have people tried to develop vaccines to these organisms before?
Interviewee: Delphine Autheman
Oh, yes, there were a lot of attempts. So, some of them have shown passive protection but nothing which could be tested in clinical trials because the protection level was not enough.
Interviewer: Shamini Bundell
And what is it about these particular organisms that makes it so difficult to find a vaccine and develop something that allows our immune system to target them?
Interviewee: Delphine Autheman
They are extracellular parasites so they are continuously exposed to the immune system, so they have developed strategies to avoid host immune systems, which makes them very difficult to control the infection by the host.
Interviewer: Shamini Bundell
So, usually our immune system or an animal immune system would be looking for particular antigens on the surface of the cell of this parasite that it could bind to and that it would recognise as something to be destroyed. How does the parasite defend itself?
Interviewee: Delphine Autheman
So, they are expressing on the surface one variant of a protein which is VSG, but they express a very high number of these proteins, so it forms a coat to shield the parasite and to prevent the host antibody to access other surface proteins.
Interviewer: Shamini Bundell
So, the immune system is there, trying and failing to get past this sort of shield of VSG proteins, but when looking for a vaccine, you and your team wanted to find other potential targets. How did you go about looking for a target?
Interviewee: Delphine Autheman
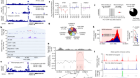
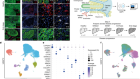
For a long time, it was thought that the VSG were only accessible by host antibody proteins, but now we know from bioinformatics that there is also other proteins in between this coat, so particularly we’re looking to the genome of the parasite, and we set up some criteria to just triage them. So, we looked for genes that are coding for proteins over 300 amino acids because it’s the size of the VSG protein, so we were thinking that maybe if the protein projects beyond the VSG, they would be more accessible to host antibodies, and we also look at genes for which we had evidence for expression on the surface of the parasites.
Interviewer: Shamini Bundell
So, once you had the sort of potential candidates for proteins which could be identified by the immune system, you then wanted to test them out as a vaccine, and what were the initial results when you tried this out in mice?
Interviewee: Delphine Autheman
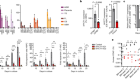
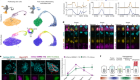
So, we have screened 39 proteins in mice and out of these 39, we found one which can reasonably delay the infection and one which gives a stable protection. It’s the first time that in a murine model we get this level of protection because before it was only partial protection, which means that the mice develop a delayed infection but in the end they still die. So, with the candidate we get we follow the mice for up to six months and they never developed parasitaemia after this.
Interviewer: Shamini Bundell
So, these candidates that you found have been way more successful than previous attempts at finding a vaccine, but this has been tested with a particular species of trypanosomes, so Trypanosoma vivax, and has also then obviously been tested in mice. Does this mean that these candidates that you have found could be used to make vaccines for cattle, for other kinds of livestock, even for humans?
Interviewee: Delphine Autheman
So, the candidate that we found to be protective against Trypanosoma vivax infection unfortunately will not be protective for all the trypanosome species, but the thing is we can use the approach we have used for Trypanosoma vivax for the other parasites. We can be reasonably optimistic to find another good vaccine candidate for the other species of trypanosomes.
Interviewer: Shamini Bundell
So, the idea is that your method, which is going through the genome, looking for these sort of key features and then testing it, could work for all the different trypanosome species. But T. vivax does impact livestock. Are the candidates that you found in the mice useful for that?
Interviewee: Delphine Autheman
Yes, I mean already, just if we can control T. vivax infection in the field, it would already decrease a lot of burden of the nagana in Africa and also in South America.
Interviewer: Shamini Bundell
And what are the next steps in order to get there, to get to a place where we can start vaccinating livestock?
Interviewee: Delphine Autheman
We need to test this vaccine candidate in cattle, which is a big step because cattle vaccine studies are really expensive and not easy to set up, so there is a big step before getting a proper vaccine, but we can be optimistic, I think.
Interviewer: Shamini Bundell
So, quite a lot of challenges, but you must be really pleased with the sort of leap forward of this particular finding?
Interviewee: Delphine Autheman
Yes, and especially because it’s opened the way for looking at vaccine candidates in other species and in particular the trypanosome species that are infecting humans.
Interviewer: Shamini Bundell
That was Delphine Autheman there. You can find a link to her paper in the show notes.
Host: Benjamin Thompson
Coming up in the podcast, we’ll be hearing how rapid advancements in developmental biology have spurred a top stem cell society to revise their guidelines for biomedical research. Before that, though, it’s time for the Research Highlights, read by Noah Baker.
[Jingle]
Noah Baker
What’s the secret to a long life? Well, for worker ants it might be getting infected with a tapeworm. A team of researchers investigating the long-term consequences of tapeworm infections placed 58 colonies of ants in observation nests and checked on them every ten days. In colonies that included ants infected with a tapeworm, the team showed that no uninfected workers were left alive when the experiment ended after three years, but half of the queens and infected workers were still kicking. The team are investigating the mechanism behind this parasite-triggered life extension. They think it may involve extra activity in some genes that help ant queens live longer. Infected ants also never left the nest, and that could be the tapeworm’s influence as well. You see, to complete its life cycle, the parasite must be consumed by woodpeckers, which prey on ant nests. Read that research in full in Royal Society Open Science.
[Jingle]
Noah Baker
Humanity has had a radical impact on life on Earth, but these changes may have started earlier than you think – not with factories but with farms. Scientists investigated how the abundance and composition of vegetation changed around the world after the last ice age. They analysed over 1,000 fossilised pollen samples from the past 18,000 years, which came from all continents except Antarctica. The team found that global vegetation has been transformed over this period, first by the climate change that accompanied the end of the last glacial period. Then, about 4,000 years ago, as agriculture intensified, the pace of change in global flora also accelerated, reaching or exceeding the rate of change seen at the end of the most recent ice age, showing that even before the Industrial Revolution, humans were capable of drastically affecting our environment. Read that research in full in Science.
[Jingle]
Interviewer: Benjamin Thompson
Next up on the show today, there’s some big news coming out in the world of stem-cell studies. Specifically, it’s that the International Society for Stem Cell Research (ISSCR) has today released the first update since 2016 to its well-respected set of guidelines for experiments involving stem cells. Now, this is a big deal, not just for the field but for ethics debates and the development of policy around the world. To find out how these guidelines have changed and what the recommendations might mean for stem-cell research, I gave Lauren Wolf, Nature’s Americas bureau chief, a call. Lauren, how are you doing? We haven’t had you on the show for a little while.
Interviewee: Lauren Wolf
Oh, well, I’m hanging in there. I just got my second COVID shot so yeah, there seems to be a light at the end of this tunnel.
Interviewer: Benjamin Thompson
Well, Lauren, you’re here today to talk about the ISSCR’s new guidelines. Could you maybe give us a sense of what these are for?
Interviewee: Lauren Wolf
It’s basically a consensus from people in the field about what types of research should be done, what’s valuable in terms of stem cells, and what research still shouldn’t be done, ethics wise. So, it’s to keep up with advances in the field. We can do things we never used to be able to do before but that doesn’t necessarily mean we should do them.
Interviewer: Benjamin Thompson
Well, let’s maybe talk about some of those recommendations then. I think what will grab the headlines is maybe their recommendation about the 14-day rule.
Interviewee: Lauren Wolf
Yeah, that’s the big one. That’s the one that everybody will be talking about. So, the 14-day rule is a guideline that says that human embryos shouldn’t be grown in a dish in the lab for more than two weeks past when they were fertilised. Where that came from, it’s actually been around for decades and it came after the very first successful IVF experiment when people realised, ‘Oh, we can start doing things with embryos outside of a person’s body. I guess we should have some rules to guide this process.’ But what’s interesting about it is that back when it was put in place, nobody could even grow an embryo for 14 days outside of the body – it was more like five or six days – and in recent years, in 2016, two research teams figured out how to grow human embryos in a dish for up to 13 days, and then because of this 14-day rule they terminated the experiment. And so, now, we’re really in this time period where, okay, before we couldn’t do this, now we can. Should we revise these rules to enable us to look further into the future?
Interviewer: Benjamin Thompson
And why have there been calls then to extend this time period, and what are the new recommendations saying?
Interviewee: Lauren Wolf
What’s interesting is that because, well, I don’t know if it’s entirely because of this 14-day rule but we actually don’t know very much about what happens in terms of embryo development, human development, after 14 days, and I’ve read in a number of places that kind of this period where we don’t know much at all is the 14-28-day period. And so, the reason why scientists would like this rule extended is because that’s the period at which we could learn why certain pregnancies don’t work out, maybe why miscarriages happen, maybe why certain conditions go on to be developed in a baby. And I’ve also read if we knew more about that period, we might be able to help more IVF procedures be successful, and so that’s one reason why they want to extend this. And so, what the new recommendations are now saying is it’s not throw all caution to the wind and do whatever you want. They haven’t replaced the time frame. They haven’t said now it’s the 28-day rule. They’ve just said if anyone wants to do research with human embryos in the lab, there needs to be a bunch of different approval steps. Everyone needs to be taken on a case by case basis. When you apply for your research project grant, you need to lay this out and they kind of give recommendations about how regulatory authorities should look at these, establishing what the value of this particular experiment is, why do you want to do it, what can you learn from it, how far do you need to grow the embryo in order to get the answers that you want, those kinds of things.
Interviewer: Benjamin Thompson
And it’s not just embryos. There’s been a bunch of papers that have come out recently about researchers who have managed to coax stem cells into things that look like embryos but are really sort of complex models.
Interviewee: Lauren Wolf
That’s another one of those advances. People call them embryoids. The thought behind that is that people can learn even more because you can grow those structures as models and grow them for longer and test drugs on them and do more things with them, and so that’s one of the reasons why these were developed, and the 14-day rule doesn’t necessarily apply to these structures but I think there’s been a lot of uncertainty around them, and so a lot of researchers have actually stopped growing them at 14 days anyway. I think one of the reasons why this change to the 14-day rule is useful is that if you want to show that these structures are indeed good model systems and represent an embryo and that if you’re studying them whatever’s happening when you test them is reflective of what might happen to an embryo, you need to validate that, right? So, you need to grow an embryo long enough as long as you’re growing one of these structures, and then you’d be able to say, ‘Yes, they are mimicking each other at each step of this process,’ and then going forward you could use the model system rather than the embryo.
Interviewer: Benjamin Thompson
It is worth noting that these are the ISSCR’s recommendation for the 14-day rule, which has been put into law in some countries around the world and is used as a fairly sort of double-underlined guideline in others. Has there been any pushback, do we know, from this recommendation coming out?
Interviewee: Lauren Wolf
I have not seen anything thus far from official government bodies or anything like that, and it is important to note that just because the ISSCR has made this recommendation, it doesn’t mean that tomorrow any of these countries are going to say, ‘Okay, never mind, no more 14-day rule.’ I’m sure that there’s going to be a lot of evaluation of these recommendations and decisions but as of now, I haven’t seen anyone pushing back against it entirely. Some of the researchers that we spoke to for this story have said they wish that there was more public participation involved in crafting these guidelines. Really, it was kind of the scientists did it themselves. The other arguments made against it that we’ve heard are, ‘Scientists are just going to keep pushing the limit as they’re able to do more things,’ and then I think on the other side of that, it’s that, ‘Well, we made this limit a long time ago and now we know a lot more about the science and we know enough to know that this 14-day rule could be extended,’ so I think there’s arguments on both sides of the debate.
Interviewer: Benjamin Thompson
If that’s the recommendation that’s going to get the headlines, it’s important not to gloss over that there are other important recommendations in these new guidelines as well. What are they saying about CRISPR editing embryos, for example, which we now know is possible after that hugely controversial story from 2018 of the researcher in China who did it.
Interviewee: Lauren Wolf
How the new ISSCR guidelines come down on gene editing of embryos is that we should not do it yet. There are a number of other panels that have looked at this issue too and I don’t think the ISSCR are saying anything different. They’re just saying the science is still too new and we don’t fully understand all of the safety of genome editing, so we shouldn’t be doing it in a cell that’s going to be implanted and potentially turned into a human being. They’re not saying we’ll never ever do this in 100 years from now, but they’re just saying for now we don’t know enough.
Interviewer: Benjamin Thompson
And so if that one is a qualified no-no until we fully understand the technology, it does seem that the recommendations are more positive about mitochondrial replacement therapy – this way of potentially alleviating these terrible metabolic diseases caused by incorrectly functioning mitochondria. Again, something not possible in 2016 but demonstrated since.
Interviewee: Lauren Wolf
So, yeah, researchers in the United Kingdom have since won approval to begin clinical trials of his method, this mitochondrial replacement therapy, and so where the ISSCR guidelines come down is that again, we can do these experiments but with lots of checks and balances and approvals. In the way that they said no on the CRISPR editing, they’re not saying no here, but they are acknowledging that this is a thing, it comes with its risks, they want some more evaluations. I think there’s lots of question about the therapy yet that they want answered.
Interviewer: Benjamin Thompson
Well, Lauren, I’m getting the sense here that it seems that these new recommendations are really getting the ethical and policy framework more into step with what’s actually possible in the lab. Have we heard from any sort of ethics experts about what they think about these new recommendations?
Interviewee: Lauren Wolf
Yeah, I think we’ve talked to some ethics experts who have said the revision of these guidelines is exactly what’s needed. We never had some of these debates before because there was nothing to debate because we couldn’t do these things. And now that we can, it’s the time to talk about this and to make some revisions because we don’t want to hold back innovation and science that could be helpful to people. But there are some ethics folks who aren’t quite sure. They think, ‘Well, maybe we haven’t exhausted all of our knowledge in the space that we have yet,’ and that ‘Maybe it’s not time to push forward into these new realms exactly yet.’ They thought that the public should be engaged a little bit more in the conversation before just changing these guidelines. But I think everybody agrees that it’s important to revisit these guidelines because of all of the developments that are happening and to kind of set standards so that you don’t have people going rogue and doing things that they shouldn’t be doing before it’s time to do them and we don’t know enough about the safety and everything.
Interviewer: Benjamin Thompson
Nature’s Lauren Wolf there. Head over to the show notes where you can find a link to more coverage of the ISSCR’s updated guidelines.
Host: Shamini Bundell
That’s all for this week’s show. We’ll be back next week. But in the meantime, you can drop us a line any time on email – we’re podcast@nature.com – or on Twitter – we’re @NaturePodcast. I’m Shamini Bundell.
Host: Benjamin Thompson
And I’m Benjamin Thompson. Thanks for listening.

 Read the paper: An invariant Trypanosoma vivax vaccine antigen induces protective immunity
Read the paper: An invariant Trypanosoma vivax vaccine antigen induces protective immunity