Abstract
Aim:
To investigate early insulin release (EIR) and late insulin release (LIR) upon glucose challenge as well as important insulin signaling factors in differentiated insulin-producing cells from embryonic stem cells(ESCs).
Methods:
A recently published protocol was modified by increasing the concentration of Exendin-4 (from 0.1 nmol/L to 10 nmol/L) together with an additional 5-day culture in low glucose (5.5 mmol/L) medium after differentiation. Gene expression profile, insulin content, C-peptide, EIR and LIR were determined.
Results:
Compared to a lower concentration of Exendin-4 (0.1 nmol/L), a higher concentration of Exendin-4 (10 nmol/L) increased glucose-responsive insulin secretion, especially EIR. Moreover, 10 nmol/L Exendin-4 increased the expression of the following genes: insulin 1, Pdx-1 (an important transcription factor, newly recognized insulin signaling factors), Epac1 and Epac2 (exchange proteins directly activated by cAMP 1 and 2), and sulfonylurea receptor 1 (SUR1, the subunit of the KATP channel).
Conclusion:
According to current knowledge, our modified protocol with a higher concentration of Exendin-4 (10 nmol/L) together with an additional 5-day 5.5 mmol/L glucose culture after differentiation improved the efficiency of differentiation toward the beta cell phenotype, which was possibly the result of stimulated expression of Pdx-1, Epac 1, and Epac 2, which in turn inhibited the K(ATP) channel through combination with SUR1, leading to increased EIR upon glucose challenge.
Similar content being viewed by others
Introduction
Beta cell replacement therapy research for diabetes has attracted much attention during recent years because the current therapy can not prevent the development of additional and severe complications resulting from chronic hyperglycemia1. Islet transplantation therapy as a strategy of cell replacement has been performed clinically; however, unavoidable problems, including lifelong use of immunosuppressive agents, donor shortage and risk of xenobiotic virus infection for the use of xenogeneic tissues, remain to be resolved2. Islet transplantation hence remains a therapeutic alternative only for a minority of patients who suffer from severe diabetes or end-stage complications. Therefore, current research on diabetes therapy emphasizes the production of an unlimited supply of surrogate cells that can function as beta cells.
Embryonic stem cells (ESCs) have been one of the main focuses of cell therapy research for diabetes because of their pluripotency, unlimited source and infinite proliferation. Various strategies have been developed to derive insulin-producing cells from ESCs. ESCs can be differentiated into insulin-producing and glucose-responsive cells by selecting nestin-positive cells. However, this five-stage induction protocol was challenged, because the insulin 2 gene is preferentially expressed in neuronal cells during development and neuronal cells express only insulin 2, whereas the pancreas expresses both insulin 1 and 23, 4. However, the insulin-producing cells in this study expressed only the insulin 2 gene, like neuronal cells5, or very weakly expressed the insulin 1 gene and exhibited disproportionately low C-peptide production compared to insulin content6. It is possible that these insulin-producing cells were mainly abnormal neurons, since they began the differentiation with nestin-positive cells, which could be differentiated to insulin-2-expressing neurons, and that insulin content may be the result of insulin uptake from the medium but not de novo synthesis7, 8, 9. Ku et al induced mouse ESCs (mESCs) into insulin–producing cells using a simple 3-step protocol based on a combination of Exendin-4, nicotinamide (NIC) and activin B10. They showed stronger insulin 1 gene expression and C-peptide immunoreactivity; however, insulin content and secretion were not described. Although subsequent in vitro studies reported the production of insulin-producing and glucose-responsive cells from ESCs using different factors combined with or without genetic modification11, 12, 13, 14, there are several common problems: relatively low insulin production; abnormal insulin secretion upon glucose stimulation; and high glucose medium (17.7–25 mmol/L) throughout the differentiation procedures, which may be one reason for impaired secretory function in beta cells15, 16.
Here we modified Ku's published protocol by increasing the concentration of Exendin-4 (10 nmol/L) and adding an additional 5 day culture in low glucose medium (5.5 mmol/L) to obtain more insulin1 and C-peptide expression and glucose-responsive cells from ESCs. We also investigated the early insulin release (EIR) and late insulin release (LIR) upon glucose challenge as well as important signaling factors to elucidate the secretion function of beta cells.
Materials and methods
Culture of mESCs — primary culture
Here we describe the culture of AB2.2 mESCs before differentiation as primary culture. STO/Neor/LIF (SNL) feeder cells, which were genetically manipulated to express neomycin (Neo) and leukemia inhibitory factor (LIF) to maintain the undifferentiated state of mESCs and promote proliferation, were seeded onto gelatinized culture dishes and treated with 10 μg/mL Mitomycin C(MMC) for 2.5 h two days before ESC plating, when SNL cells had achieved 90% confluence. Two days later, ESCs were thawed and added evenly to MMC-treated SNL feeders, which were changed to ESC medium with 85% DMEM (Invitrogen), 15% FBS (Gemini, Woodland, CA, USA), 2 mmol/L L-glutamine (Invitrogen), 49.5 U/mL Penicillin , 38.8 μg/mL streptomycin (Invitrogen), and 0.1 mmol/L β-mercaptoethanol (Sigma), at least 3 h prior. ESCs were fed with fresh ESC medium every day and achieved about 90% confluence on the third day. Then, ES cells were passaged for further expansion or additional differentiation experiments. Alkaline phosphatase (AP) staining was routinely performed to assess the undifferentiated and pluripotency states of ESCs. Cells were observed and photographed under a phase contrast microscope (Olympus TH4-200, Olympus Optical Co Ltd, Tokyo, Japan).
In vitro differentiation protocol
Generation of embryonic bodies (EBs) — secondary culture
ESCs were trypsinized and transferred to 10-cm culture dishes for two rounds to deplete feeder cells. Then AP staining was routinely performed in ESCs with another set of SNL feeders as negative control. DAPI was used for counterstaining the nucleus. Cells were observed under a fluorescence microscope (Olympus TH4-200, Olympus Optical Co Ltd, Tokyo, Japan). To introduce the generation of EBs, termed as the secondary culture, ESCs were transferred to differentiation medium containing IMDM (Mediatech, Inc, Herndon, VA), 50 μg/mL ascorbic acid (Sigma), 6×10−3 mol/L monothioglycerol (MTG, Sigma, St Louis) and 15% FBS, and ESCs were plated at a density of 5000 cells/mL on 10-cm Petri dishes to avoid adherence. From day 2 to day 6 of secondary culture, EBs were transferred to differentiation medium containing IMDM, 50 μg/mL ascorbic acid, 6×10−4 mol/L MTG and 15% FBS.
Inducing the differentiation toward insulin-producing cells — tertiary culture
EBs were plated without precoating on day 6 of secondary culture, thus initiating the onset of tertiary culture. The basic tertiary culture medium contained DMEM/F-12 (1:1) (Mediatech, Inc) and 15% serum replacement (SR, Invitrogen) for ESCs. The first change of medium occurred on day 5 of the tertiary culture to allow attachment of most EBs onto the plates; 10 mmol/L nicotinamide (Sigma) and 10 ng/mL activin B (R&D Systems) were added on day 7. Exendin-4 (Sigma) was also added at the same time, but at two different concentrations: 0.1 nmol/L and 10 nmol/L. The whole tertiary culture lasted for 15 days.
Further maturation of differentiated cells — quaternary culture
To promote further differentiation, the cells were switched to medium containing 15% SR with 5.5 mmol/L glucose for 5 days. The whole process was summarized in Figure 1.
The control group was prepared at the same time but cultured in the ESC culture medium from the beginning to the end of the experiment.
Analysis of differentiated cells at the end of the experiment
Morphological development during differentiation
During differentiation, morphological changes were observed and photographed at days 2 and 6 of secondary culture, day 15 of tertiary culture and day 5 of quaternary culture, using a phase contrast microscope.
RT-PCR
Total RNA was extracted from cells using the RNeasy Mini Kit (Qiagen, Courtaboeuf Cedex, France), and RT-PCR (Invitrogen) was performed according to the manufacturer's protocol. Genomic DNA was digested with DNaseI (BioLab) for 40 min at 37 °C. The forward and reverse primers of each PCR set were designed to be located in different exons to distinguish the PCR products from possible DNA contamination. Moreover, the final PCR products were generally designed to be less than 500 bp and the products from possible DNA contamination were generally designed to be larger than 1 kb or even higher, making the amplifying reactions from DNA contamination impossible to induce by the following PCR conditions. The PCR reactions were performed for 28 cycles for GAPDH first as follows: 40 s at 94 °C for denaturation, 30 s at 58 °C for annealing, and 30 s at 72 °C for extension. PCR products were separated on 1.5% agarose gels by electrophoresis and analyzed with a gel analyzer. The qualities of RNA for all samples were modulated and finally determined according to gel analysis so as to make the densities of GAPDH product bands for all samples similar. The qualities of RNA for other primers were determined according to the quality of RNA for GAPDH and PCR reactions were performed for 35 cycles with the same conditions as applied for GAPDH. Primer sequences and product sizes are summarized in Table 1.
Immunofluorescence staining of C-peptide
Cells were fixed in 4% paraformaldehyde O/N at 4 °C. The cells were incubated with the primary polyclonal goat anti-C-peptide (1:800, Santa Cruz Biotechnology, USA) O/N at 4 °C and then localized by anti-goat FITC (1:500, Sigma) for 30 min at room temperature. 4′,6-diamidine-2′-phenylindole dihydrochloride (DAPI) was used for counterstaining the nucleus. Cells were observed under a fluorescence microscope (Olympus TH4-200, Olympus Optical Co LTD, Tokyo, Japan).
Glucose challenge test
Before the test, the cells were changed to serum-free medium containing 5.5 mmol/L glucose for 2 h at 37 °C, followed by washing twice with additional serum-free medium to enable the detection of insulin secretion without interference from the serum. Glucose challenge test was performed by the addition of serum-free medium containing low (5.5 mmol/L) glucose for 2 h at 37 °C and then transferred to serum-free medium containing high (26 mmol/L) glucose for 2 h at 37 °C. The conditioned medium was collected 5 minutes and 2 h after the glucose challenge, and cells were washed and collected at the end of the high (26 mmol/L)-glucose challenge. All samples were frozen at −80 °C until assayed for insulin contents. Total protein content was determined with the BCA Protein Assay Reagent Kit (Pierce, Rockford, USA).
ELISA detection of insulin in medium and cell lysates
Insulin levels in the medium and cell lysates were detected with an insulin ELISA kit (Linco Research, USA) according to the provided protocol. The insulin secreted into the medium and cell lysates was expressed as ng/mg protein after being normalized to the total protein content of the cells.
Statistical analysis
Data were expressed as the mean±SEM. Statistical analyses of the data were performed using one-way ANOVA followed by Tukey's post-hoc test. A P value <0.05 was considered statistically significant.
Results
Undifferentiated and pluripotency state of mESCs
AP staining showed strong red signals in all clumps of mESCs from primary culture and mESCs after two rounds of feeder-free culture, suggesting the undifferentiated and pluripotency state of our ESCs (Figure 2).
Alkaline phosphatase (AP) staining of AB 2.2 mESCs from primary culture (A) and mESCs after two rounds of feeder-free culture (B). AP staining showed strong red signals in all ESC clumps, whereas SNL feeder cell control showed the absence of AP (C), suggesting the undifferentiated and pluripotency state of our ESCs.
Morphology observation during differentiation
mESCs consistently aggregated and formed simple EBs on day 2 after plating, largely composed of densely packed mESCs (Figure 3A). Then the EBs grew larger and the center of the bodies became cavitary; these turned into cystic EBs on day 6 of secondary culture (Figure 3B). The EBs were obviously larger in the control group than in the differentiation group.
Morphology of ESCs during differentiation toward insulin-producing cells. (A) Formation of simple embryonic bodies (EBs) on day 2 of secondary culture; these were largely composed of densely packed ES cells. (B) Formation of cystic EBs on day 6 of secondary culture. In the control group, the simple EBs on day 2 and cystic EBs on day 6 were larger than those in the differentiation group. (C) On day 3 of tertiary culture, EBs in the control group attached quickly and achieved 100% attachment on day 3 of tertiary culture, whereas the EBs in the differentiation group attached slowly and only about 50% had attached on day 3. After attachment, cells extended and scattered widely from the EBs in the control group, but extended within a certain limited range in the differentiation group. (D) On day 5 of the quaternary culture, cell populations in the control group became multi-layered and more crowded; it was difficult to distinguish the cell morphology. Cells in the differentiation group became more confluent than those in the tertiary culture, with various cell morphologies. Control: control group; Differentiation: Differentiation group.
The EBs in the control group attached quickly and achieved 100% attachment, whereas the EBs in the differentiation group attached slowly and only partially attached on tertiary culture. After attachment, cells extended and scattered widely from the EBs in the control group but extended within a boundary outside the EBs in the differentiation group. At this stage, it was easy to distinguish the cells in different EBs because of the different locations (Figure 3C). Thereafter, the cells in the control group grew rapidly, while cells in the differentiation group grew more slowly. By day 15 of tertiary culture, the cells in the control group had achieved 100% confluence. However, cells only achieved about 50% confluence in the differentiation group, and some EBs still did not attach.
In quaternary culture, cell populations in the control group became multi-layered, and it was difficult to distinguish the cell morphology. However, cells in the differentiation group became more confluent than those in the tertiary culture with various cell morphologies, appearing to be neuron-like, epithelial-like, endodermal-like, small and round. A few EBs still did not attach (Figure 3D).
In summary, the control group showed rapid growth and attachment, while both differentiation groups grew and attached more slowly, with a few EBs floating even at the end of the experiment, suggesting that the differentiation group may be in the process of directed differentiation at the expense of proliferation.
Expression profiles of genes related to the beta cell phenotype
After calibrations and statistical analysis, there was no significant difference among GAPDH product bands for all samples as shown, respectively, in Figure 4A and Figure 4B. Gene expression was obviously higher in the 10 nmol/L Exendin-4 (E10) group compared to the 0.1 nmol/L Exendin-4 (E0.1) group and control group for the following: beta cell-specific hormone insulin-1; important transcription factors playing an important role in beta cell differentiation including Pdx-1, Ngn3, and NeuroD (as shown in Figure 4A); important factors related to glucose-dependent insulin secretion of beta cells (as shown in Figure 4B), including glucose transporter-2 (Glut-2, glucose transporter to transport glucose from outside the cell into the cytoplasm), SUR1, and newly recognized insulin signaling factors, exchange proteins directly activated by cAMP1 and 2 (Epac1, Epac2). These results indicated a higher extent of differentiation toward beta cell phenotype in the E10 group, suggesting that cells cultured at a higher concentration of the GLP-1 analogue, Exendin-4, are more likely to be differentiated to beta cells.
Gene expression profiles of important transcription factors (A) necessary for beta cell development and important factors involved in glucose-dependent insulin secretion (B). Ngn3: neurogenin 3, Pdx-1: pancreatic and duodenal homeobox gene 1, Glut-2: glucose transporter-2, SUR1: sulfonylurea receptor, Con: control group; E0.1: Exendin-4 at 0.1 nmol/L group; E10: Exendin-4 at 10 nmol/L group.
Immunofluorescence staining of C-peptide
As shown in Figure 5, a few small cell clusters with positive signals for C-peptide were observed in the control group. However, much larger cell clusters with positive signals for C-peptide were easily observed in both the E0.1 and the E10 groups. These clusters were mainly made up of small round cells. These results suggested more de novo insulin synthesis in both differentiation groups because C-peptide is the product of proinsulin during processing into mature insulin and thus has been accepted as a more specific marker for beta cells than insulin.
Immunostaining of C-peptide. Rare small cell clusters with positive signals for C-peptide were observed in the control group, whereas more and larger cell clusters with positive signals for C-peptide were easily observed in both E0.1 and E10 groups. DAPI (4′,6-diamidine-2′-phenylindole dihydrochloride, blue fluorescence) was used for nucleus counterstaining. Control: control group; E0.1: Exendin-4 at 0.1 nmol/L group; E10: Exendin-4 at 10 nmol/L group.
Insulin content in medium and cell lysates after glucose challenge
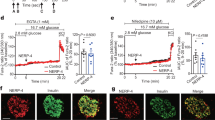
As seen in Figure 6, insulin levels in cell lysates from both E0.1 and E10 groups were significantly higher than those in the control group (P<0.05 for the E0.1 group and P<0.01 for the E10 group in Figure 6A) , but there was no significant difference between the E0.1 and E10 groups. The insulin levels in medium during both the first 5 min and the period from 5 min to 2 h after 5.5 mmol/L and 26 mmol/L glucose challenge in the E10 group was significantly higher than that in the E0.1 group and the control group (P<0.05 or P<0.01 as indicated in Figure 6B and 6C). Moreover, there was a significant difference in the insulin levels in the medium in the E10 group during the first 5 min when comparing 5.5 mmol/L and 26 mmol/L glucose challenges (P<0.05 as indicated in Figure 6B), but not in the E0.1 group or the period from 5 min to 2 h. These results suggest that Exendin-4 induced the differentiation of insulin-producing cells with increased insulin synthesis and secretion, whereas a higher dosage of Exendin-4 also induced the glucose-responsive characteristics of insulin-producing cells, but only for early not for late insulin release. These results indicate that the insulin-producing cells possessed some but not all characteristics of fully matured beta cells.
Insulin Content (ng/mg prot) in the cell extracts (A) and in the medium 5 min (B) and from 5 min to 2 h (C) after 26 mmol/L glucose challenge, as determined by ELISA. Con: control group; E0.1: Exendin-4 at 0.1 nmol/L group; E10: Exendin-4 at 10 nmol/L group. bP<0.05, cP<0.01 compared to control group. eP<0.05, fP<0.01 compared to E10 group at 26 mmol/L glucose challenge; hP<0.05, iP<0.01 compared to E10 group at 5.5 mmol/L glucose challenge.
Discussion
Exendin-4 is a dipeptidyl peptidase IV (DPP-IV)-resistant GLP-1 analog. It can increase insulin secretion in a dose-dependent and glucose-dependent manner in vivo or in isolated islets in vitro17, 18. In vivo treatment with Exendin-4 or overexpression of GLP-1 also promoted the differentiation of fetal pancreatic tissue, pancreatic progenitors or intestinal stem cells into insulin-producing cells and ameliorated hyperglycemia19, 20, 21. In vitro Exendin-4 treatment combined with activin B and NIC also induced the differentiation of mESCs into insulin–producing cells with stronger insulin 1 gene expression, but the insulin content and secretion were not described10. It is possible that the concentration of Exendin-4 used was too low, ie, 0.1 nmol/L. Another possible reason may be the presence of high-glucose culture (17.7–25 mmol/L) throughout the entire differentiation procedure. Hyperglycemia caused much lower insulin content and impaired glucose-regulatory insulin release, whereas this functional impairment induced by high glucose, or glucose toxicity, was significantly corrected by an additional 2-day culture at 5.5 mmol/L glucose following high-glucose culture15, 16. Therefore, in the current study, we used a more strict protocol to elucidate the function of differentiated cells, including adding a higher concentration of Exendin-4 (10 nmol/L), adding an additional 5-day culture in 5.5 mmol/L glucose culture at the end of the differentiation after high glucose culture (25 mmol/L); serum starvation before and during glucose challenge test to prevent the interference of serum insulin with the detection of insulin in cell extracts and medium; strict design of all primers for RT-PCR to prevent genomic DNA contamination and detection of EIR since EIR plays an important role in maintaining normal glucose homeostasis by suppressing hepatic glucose production and by increasing the glucose uptake of insulin-sensitive tissues22.
Our results indicated that both E0.1 and E10 groups showed much higher expression levels of insulin 1 and C-peptide immunoreactivity, and significantly higher insulin content in cell lysates compared to the control group, indicating a positive effect of the combination of Exendin-4, activin B, and NIC on differentiation toward the beta cell phenotype. Constitutive insulin secretion, EIR (at 5 min after 26 mmol/L glucose challenge) and LIR (at 2 h after 26 mmol/L glucose challenge) in the E10 group were significantly higher than in the E0.1 group, but there was no significant difference between the E0.1 group and the control group. Moreover, EIR after 26 mmol/L glucose challenge was significantly higher than in 5.5 mmol/L glucose medium in the E10 group, but not in the E0.1 group. These results suggest that Exendin-4 at a lower dosage (0.1 nmol/L) induced the differentiation of insulin-producing cells with increased insulin synthesis but without significant effect on insulin secretion, while Exendin-4 at a higher dosage (10 nmol/L) enhanced both insulin synthesis and glucose-responsive insulin secretion, especially EIR. A higher dosage of Exendin-4 appears to have potential for application in the clinic, since EIR plays an important role in inhibiting not only postprandial hyperglycemia, but also postprandial hyperlipidemia in type 2 diabetes, which is characterized by impaired EIR23, 24, 25.
We further checked the gene expression of important factors related to the development and function of beta cells to provide further information about this differentiation promoted by high dosage of Exendin-4. Pdx-1 has been accepted as an essential and crucial transcription factor for pancreatic islet development since it is by far the first sign of differentiation detected in murine endoderm, as early as E8.5 (11–13 somites)26. Knockout of Pdx1 gene led to an arrest of pancreatic development at a very early stage and resulted in animals lacking pancreata. In mature beta cells, Pdx-1 also plays a critical role in normal function as a glucose-responsive regulator of insulin expression27, 28. Therefore, Pdx-1 expression was induced and examined in many different differentiation protocols, as were its downstream transcription factors, Ngn3 and NeuroD29, 31. Here we also detected an obviously higher expression level of Pdx-1 together with Ngn3 and NeuroD in the E10 group compared to the E0.1 group, suggesting that Exendin-4 at 10 nmol/L may induce a higher extent of differentiation toward the beta cell phenotype by promoting the expression of Pdx-1 and downstream transcription factors, which thus directed or promoted the further differentiation of mESCs toward the beta cell lineage.
Glucose-dependent insulin secretion is the most important function of mature beta cells for the body to maintain euglycemia after a meal or glucose intake, so the related factors were also examined to elucidate the function of differentiated insulin-producing cells as induced by high-dosage of Exendin-4. To briefly describe the process, glucose is taken up into the cytoplasm by the glucose sensor, Glut-2. Aerobic glycolysis produces increased ATP production. This signal causes the inhibition of K(ATP) channels, leading to the activation of voltage-dependent Ca2+ channels, Ca2+ influx, and finally Ca2+-dependent insulin exocytosis, while metabolism of glucose also generates metabolic coupling factors, such as cAMP, which facilitate the exocytosis of insulin through the PKA pathway and the newly recognized Epac pathway32, 33. GLP-1 has been shown to promote glucose-dependent ATP production, inhibit K(ATP)-channels and stimulate cAMP production to activate the PKA pathway and the Epac pathway for exocytosis of insulin32, 34. Expression of dominant-negative Epac 1 and Epac 2 in a beta cell line blocked the stimulatory effect of GLP-1 on exocytosis of insulin. Both Epac 1 and Epac 2 coimmunoprecipitated with SUR1, a subunit of the K(ATP) channel, suggesting that both Epac1 and Epac 2 are involved in a novel mechanism for insulin secretion35, 36. Exendin-4 shares insulinotropic actions with GLP-1 but at a much higher potency. Here we showed that the gene expression levels of Glut-2, SUR1, Epac 1, and Epac 2 were obviously higher in the E10 group than in the E0.1 group, suggesting that one of the mechanisms for our modified protocol with increased dosage of Exendin-4 may be the stimulation of Epac 1 and Epac 2 expression, which in turn inhibits K(ATP) channels through combinations with SUR1, leading to increased EIR upon 26 mmol/L glucose challenge.
Conclusions
In summary, our modified in vitro protocol for differentiation of mESCs with an increased concentration of Exendin-4 (10 nmol/L) and an additional 5-day low-glucose (5.5 mmol/L) culture at the end of the differentiation increased the differentiation efficiency of mESCs toward beta cell phenotype with increased insulin synthesis, constitutive insulin secretion and early insulin release upon glucose challenge, which may be mediated by increased expression of important transcription factors, such as Pdx-1, and glucose-induced insulin-secretion related factors, Epac 1, Epac 2, and SUR1. Recently Kroon et al showed that implantation of in vitro ESC-derived endocrine cells corrected hyperglycemia in diabetic mice37, which provides further solid support that ESCs are competent to generate glucose-responsive insulin-producing cells. However, differentiation of ESCs in vitro presents potential as well as a challenge. ESCs can be expanded without the passages limitation in vitro and are pluripotent, whereas the possibility of teratoma formation should be considered and immunosuppressive therapy is needed after transplantation back to the body. Since there is currently no perfect solution for cell replacement therapies for diabetes, the rapid growth in biomedical tools globally should allow the further development of a better ESC differentiation strategy for diabetes.
Author contribution
Hua LI: collection and assembly of data, manuscript writing; Amy LAM: collection and assembly of data; Ai-min XU: collection and assembly of data; Karen SL LAM: conception and design, manuscript writing; Sookja KIM CHUNG: conception and design, manuscript writing.
References
Yamagishi S, Nakamura K, Imaizumi T . Advanced glycation end products (AGEs) and diabetic vascular complications. Curr Diabetes Rev 2005; 1: 93–106
Zhou D, Sun YL, Vacek I, Ma P, Sun AM . Normalization of diabetes in cynomolgus monkeys by xenotransplantation of microencapsulated porcine islets. Transplant Proc 1994; 26: 1091.
Devaskar SU, Singh BS, Carnaghi LR, Rajakumar PA, Giddings SJ . Insulin II gene expression in rat central nervous system. Regul Pept 1993; 48: 55–63.
Deltour L, Leduque P, Blume N, Madsen O, Dubois P, Jami J, et al. Differential expression of the two nonallelic proinsulin genes in the developing mouse embryo. Proc Natl Acad Sci USA 1993; 90: 527–31.
Lumelsky N, Blondel O, Laeng P, Velasco I, Ravin R, McKay R . Differentiation of embryonic stem cells to insulin-secreting structures similar to pancreatic islets. Science 2001; 292: 1389–94.
Bai L, Meredith G, Tuch BE . Glucagon-like peptide-1 enhances production of insulin in insulin-producing cells derived from mouse embryonic stem cells. J Endocrinol 2005; 186: 343–52.
Hansson M, Tonning A, Frandsen U, Petri A, Rajagopal J, Englund MC, et al. Artifactual insulin release from differentiated embryonic stem cells. Diabetes 2004; 53: 2603–9.
Rajagopal J, Anderson WJ, Kume S, Martinez OI, Melton DA . Insulin staining of ES cell progeny from insulin uptake. Science 2003; 299: 363.
Sipione S, Eshpeter A, Lyon JG, Korbutt GS, Bleackley RC . Insulin expressing cells from differentiated embryonic stem cells are not beta cells. Diabetologia 2004; 47: 499–508.
Ku HT, Zhang N, Kubo A, O'Connor R, Mao M, Keller G, et al. Committing embryonic stem cells to early endocrine pancreas in vitro. Stem Cells 2004; 22: 1205–17.
Jiang J, Au M, Lu K, Eshpeter A, Korbutt G, Fisk G, et al. Generation of insulin-producing islet-like clusters from human embryonic stem cells. Stem Cells 2007; 25:1940–53.
Li L, Li F, Qi H, Feng G, Yuan K, Deng H, et al. Coexpression of Pdx1 and betacellulin in mesenchymal stem cells could promote the differentiation of nestin-positive epithelium-like progenitors and pancreatic islet-like spheroids. Stem Cells Dev 2008; 17: 815–23.
Phillips BW, Hentze H, Rust WL, Chen QP, Chipperfield H, Tan EK, et al. Directed differentiation of human embryonic stem cells into the pancreatic endocrine lineage. Stem Cells Dev 2007; 16: 561–78.
Xu X, Kahan B, Forgianni A, Jing P, Jacobson L, Browning V, et al. Endoderm and pancreatic islet lineage differentiation from human embryonic stem cells. Cloning Stem Cells 2006; 8: 96–107.
Eizirik DL, Korbutt GS, Hellerstrom C . Prolonged exposure of human pancreatic islets to high glucose concentrations in vitro impairs the beta-cell function. J Clin Invest 1992; 90: 1263–8.
Jonas JC, Sharma A, Hasenkamp W, Ilkova H, Patane G, Laybutt R, et al. Chronic hyperglycemia triggers loss of pancreatic beta cell differentiation in an animal model of diabetes. J Biol Chem 1999; 274: 14112–21.
Buse JB, Henry RR, Han J, Kim DD, Fineman MS, Baron AD . Effects of exenatide (exendin-4) on glycemic control over 30 weeks in sulfonylurea-treated patients with type 2 diabetes. Diabetes Care 2004; 27: 2628–35.
Lupi R, Mancarella R, Del Guerra S, Bugliani M, Del Prato S, Boggi U, et al. Effects of exendin-4 on islets from type 2 diabetes patients. Diabetes Obes Metab 2008; 10: 515–9.
Liu MJ, Han J, Lee YS, Park MS, Shin S, Jun HS . Amelioration of hyperglycemia by intestinal overexpression of glucagon-like peptide-1 in mice. J Mol Med 2009;17: 1432–40
Movassat J, Beattie GM, Lopez AD, Hayek A . Exendin 4 up-regulates expression of PDX 1 and hastens differentiation and maturation of human fetal pancreatic cells. J Clin Endocrinol Metab 2002; 87: 4775–81.
Liu MJ, Shin S, Li N, Shigihara T, Lee YS, Yoon JW, et al. Prolonged remission of diabetes by regeneration of beta cells in diabetic mice treated with recombinant adenoviral vector expressing glucagon-like peptide-1. Mol Ther 2007; 15: 86–93.
Qian L, Xu L, Wang X, Fu X, Gu Y, Lin F, et al. Early insulin secretion failure leads to diabetes in Chinese subjects with impaired glucose regulation. Diabetes Metab Res Rev 2009; 25: 144–9.
Ai M, Tanaka A, Ogita K, Shimokado K . Favorable effects of early insulin secretion by nateglinide on postprandial hyperlipidemia in patients with type 2 diabetes. Diabetes Care 2006; 29: 1180.
Laaksonen DE, Niskanen L, Mykkänen H, Juntunen KS, Schwab U, Kolehmainen M, et al. Long-term repeatability of measures of early insulin secretion derived from an intravenous glucose tolerance test and conversion from impaired glucose tolerance to diabetes. Ann Med 2008; 40: 303–11.
Mori Y, Kitahara Y, Miura K, Mine T, Tajima N . Role of early insulin secretion in postglucose-loading hyperglycaemia and postfat-loading hyperlipidaemia: comparing nateglinide and glibenclamide for acute effects on insulin secretion in OLETF rats. Diabetes Obes Metab 2004; 6: 422–3.
Kaufmann RA, Armant DR . In vitro exposure of preimplantation mouse embryos to cocaine and benzoylecgonine inhibits subsequent development. Teratology 1992, 46: 85–89.
Jonsson J, Carlsson L, Edlund T, Edlund H . Insulin-promoter-factor 1 is required for pancreas development in mice. Nature 1994; 371: 606–9.
Le Lay J, Stein R . Involvement of PDX-1 in activation of human insulin gene transcription. J Endocrinol 2006; 188: 287–94.
Li H, Li X, Lam KS, Tam S, Xiao W, Xu R . Adeno-associated virus-mediated pancreatic and duodenal homeobox gene-1 expression enhanced differentiation of hepatic oval stem cells to insulin-producing cells in diabetic rats. J Biomed Sci 2008; 15: 487–97.
Chen S, Borowiak M, Fox JL, Maehr R, Osafune K, Davidow L, et al. A small molecule that directs differentiation of human ESCs into the pancreatic lineage. Nat Chem Biol 2009; 5: 258–65.
Cai J, Yu C, Liu Y, Chen S, Guo Y, Yong J, et al. Generation of homogeneous PDX1(+) pancreatic progenitors from human ES cell-derived endoderm cells. J Mol Cell Biol 2010; 2: 50–60.
Gloerich M, Bos JL . Epac: defining a new mechanism for cAMP action. Annu Rev Pharmacol Toxicol 2010; 50: 355–75.
Holz GG, Kang G, Harbeck M, Roe MW, Chepurny OG . Cell physiology of cAMP sensor Epac. J Physiol 2006; 577: 5–15
Yu Z, Jin T . New insights into the role of cAMP in the production and function of the incretin hormone glucagon-like peptide-1 (GLP-1). Cell Signal 2010; 22: 1–8.
Kang G, Chepurny OG, Holz GG . cAMP-regulated guanine nucleotide exchange factor II (Epac2) mediates Ca2+-induced Ca2+ release in INS-1 pancreatic beta-cells. J Physiol 2001; 536: 375–85.
Kang G, Chepurny OG, Malester B, Rindler MJ, Rehmann H, Bos JL, et al. cAMP sensor Epac as a determinant of ATP-sensitive potassium channel activity in human pancreatic beta cells and rat INS-1 cells. J Physiol 2006; 573: 595–609.
Kroon E, Martinson LA, Kadoya K, Bang AG, Kelly OG, Eliazer S, et al. Pancreatic endoderm derived from human embryonic stem cells generates glucose-responsive insulin-secreting cells in vivo. Nat Biotechnol 2008; 26: 443–52.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Li, H., Lam, A., Xu, Am. et al. High dosage of Exendin-4 increased early insulin secretion in differentiated beta cells from mouse embryonic stem cells. Acta Pharmacol Sin 31, 570–577 (2010). https://doi.org/10.1038/aps.2010.38
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/aps.2010.38
Keywords
This article is cited by
-
Exendin-4 enhances the differentiation of Wharton’s jelly mesenchymal stem cells into insulin-producing cells through activation of various β-cell markers
Stem Cell Research & Therapy (2016)
-
In vitro evaluation of different protocols for the induction of mesenchymal stem cells to insulin-producing cells
In Vitro Cellular & Developmental Biology - Animal (2015)
-
Maturation and function of human embryonic stem cell-derived pancreatic progenitors in macroencapsulation devices following transplant into mice
Diabetologia (2013)