Abstract
The mechanisms by which antidepressants regulate the hypothalamic-pituitary-adrenal (HPA) axis are still unknown. The ABCB1-type multiple drug resistance (MDR) p-glycoprotein (PGP) regulates the HPA axis by limiting the access of glucocorticoids to the brain in mice and humans. Previous work in cell cultures has found that antidepressants enhance glucocorticoid receptor (GR) function in vitro by inhibiting MDR PGP, and therefore by increasing the intracellular concentration of glucocorticoids—but this model has never been tested directly in animals. Here, the tricyclic antidepressant, desipramine (20 mg/kg/day, i.p., for seven days), was administered to abcb1ab MDR PGP knockout mice (congenic on the FVB/N background strain) and to FVB/N controls. The hippocampal mRNA expression of GR, mineralocorticoid receptor (MR), MDR (Mdr1a) PGP, and 11β-hydroxysteroid dehydrogenase type 1 (11β-HSD1) were measured, together with plasma corticosterone levels. In FVB/N controls, desipramine induced a significant upregulation of GR mRNA in the CA1 region (+31%; p=0.045); in contrast, in abcb1ab (−/−) mice, desipramine induced a significant downregulation of GR mRNA in the CA1 region (−45%; p=0.004). MR mRNA expression was unaltered. Desipramine decreased corticosterone levels in both FVB/N controls and in abcb1ab (−/−) mice, but in abcb1ab (−/−) mice the effects were smaller. Specifically, in FVB/N controls (but not in abcb1ab (−/−) mice), desipramine reduced corticosterone levels not only compared with saline-treated mice but also compared with the ‘physiological’ levels of untreated mice (−39%; p=0.05). Finally, desipramine reduced Mdr1a mRNA expression across all hippocampus areas (−9 to −23%), but had no effect on 11β-HSD1 mRNA expression. These data support the notion that the MDR PGP is one of the molecular targets through which antidepressants regulate the HPA axis.
Similar content being viewed by others
INTRODUCTION
Antidepressants normalize the hormonal stress response in patients with major depression, but the molecular mechanisms underlying this effect are still unknown (Holsboer, 2000; Pariante et al, 2004b; Neigh and Nemeroff, 2006; Pariante, 2006). Patients with major depression have a hyperactivity of the main hormonal stress response system, the hypothalamic-pituitary-adrenal (HPA) axis, as shown by increased levels of corticotropin-releasing factor (CRF) in the brain, and of the endogenous glucocorticoid hormone, cortisol, in the plasma (Holsboer, 2000; Pariante et al, 2004b; Neigh and Nemeroff, 2006; Pariante, 2006). Moreover, several lines of evidence indicate that these HPA axis abnormalities contribute to the development of the depressive symptoms. First, treatment with antidepressants reduces HPA axis activity, and this reduction is associated with the clinical response in depressed patients (Kunzel et al, 2003). Second, genes that regulate the HPA axis also influence the likelihood of developing depression (van West et al, 2006). Third, drugs that directly regulate HPA axis activity have therapeutic effects in affective disorders (Nemeroff and Owens, 2002; Young et al, 2004; Flores et al, 2006). Finally, and of particular relevance to this paper, antidepressants can directly regulate the function and the expression of the corticosteroid receptors (Pariante, 2004, 2006).
Antidepressants reduce HPA axis activity by increasing the negative feedback on the HPA axis by the endogenous glucocorticoids, cortisol in humans and corticosterone in rodents (Pariante, 2004, 2006). This feedback is mediated by intracellular corticosteroid receptors in the brain: the glucocorticoid receptor (GR) and the mineralocorticoid receptor (MR) (de Kloet et al, 1998). Although there is consensus that GR function is reduced in depressed patients (Pariante, 2006), MR function seems to remain intact (Young et al, 2003; Juruena et al, 2006). Indeed, antidepressants increase GR expression, GR function, and GR nuclear translocation in cellular and animal experimental systems; in turn, this is associated with enhanced negative feedback and thus with reduced HPA axis activity (Pariante, 2004, 2006). Moreover, in humans, we have shown that an increase in GR-mediated negative feedback is already present after as little as 4 days of antidepressant treatment (Pariante et al, 2004a). However, considering that the first paper describing this effect in cells was published in 1989 (Pepin et al, 1989), and the first papers in animals shortly afterward (Peiffer et al, 1991b; Seckl and Fink, 1992), it is perhaps surprising that we do not yet know how antidepressants increase GR expression and function. According to the classical model of antidepressant action, these drugs work by increasing the monoaminergic neurotransmission in the brain (Nemeroff and Owens, 2002), and in fact there is a direct cross talk between monoaminergic neurotransmission, glucocorticoid hormones, and corticosteroid receptors (Yau et al, 1997; Lai et al, 2003). However, the effects of antidepressants on GR can occur independently from this mechanism. For example, desipramine, a tricyclic antidepressant that increases noradrenaline neurotransmission, induces GR upregulation in rats even following neurotoxic lesioning of noradrenergic neurons with DSP4 (Rossby et al, 1995). Moreover, antidepressant-induced GR upregulation in cell cultures is not blocked by antagonists of α or β adrenergic receptors, or of 5HT1a or 5HT2 serotonergic receptors (Okugawa et al, 1999; Lai et al, 2003).
Recently, we have described in cell cultures that antidepressants control GR function by increasing the intracellular concentration of glucocorticoids (Pariante et al, 2001, 2003a, 2003b, 2004b). Glucocorticoids are excreted from fibroblasts, leukocytes, and epithelial cells by the ABCB1-type multiple drug resistance (MDR) p-glycoprotein (PGP) present in two isoforms in rodents (abcb1a and abcb1b) and one isoform only in humans (ABCB1). Interestingly, the MDR PGP is also localized at the luminal membrane of the endothelial cells of the blood–brain barrier (BBB), and limits the access of endogenous glucocorticoids to the mouse and human brain (de Kloet et al, 1998; Meijer et al, 1998; Karssen et al, 2001, 2002; Uhr et al, 2002; Muller et al, 2003). We have found that antidepressants enhance GR function in mouse fibroblast cells by inhibiting the MDR PGP, and thus increasing intracellular concentrations of glucocorticoids (Pariante et al, 2001, 2003a, 2003b); a similar effect is also present in rat cortical neurones (Pariante et al, 2003a). Consistent with this finding, pretreatment of cells with an MDR PGP inhibitor, or coincubation with a glucocorticoid that is not transported by MDR PGP in vitro, prevents these effects of antidepressants (Pariante et al, 1997, 2001, 2003a, 2003b). Although other researchers have independently replicated these in vitro findings (Budziszewska et al, 2000; Miller et al, 2002; Herr et al, 2003), this model has never been directly tested in animals.
Here, we examine the effects of the tricyclic antidepressant, desipramine, in mice that are knockout (−/−) for both the abcb1a and the abcb1b MDR PGP, and in FVB/N controls. The abcb1ab (−/−) mice have been previously shown to have increased access of corticosterone to the brain and a more effective HPA axis negative feedback because of the facilitated entry of endogenous and exogenous glucocorticoids to the brain (Uhr et al, 2002; Muller et al, 2003). Our hypothesis is that antidepressants increase GR expression and decrease HPA axis activity by modulating MDR PGP; and therefore that these effects of antidepressants would not be present in the abcb1ab (−/−) mice. To investigate further, the mechanism by which antidepressants regulate the HPA axis, we also examine the effects of desipramine on the expression of MDR PGP itself (Mdr1a, more expressed in the brain), and also on the expression of 11β-hydroxysteroid dehydrogenase type 1 (11β-HSD1). 11β-HSD1 is an intracellular enzyme which catalyzes the regeneration of active glucocorticoids from circulating inert 11-keto steroids, and therefore effectively amplifies glucocorticoid action in the brain (Seckl and Walker, 2001).
MATERIALS AND METHODS
Animals
Male FVB/N controls and abcb1ab (−/−) mice, originally created by Schinkel et al (1997), backcrossed 12 generations to the FVB/N background strain, 8–9 months of age, were obtained from Taconic (Germantown, NY, USA), housed individually and maintained on a 12:12 h light/dark cycle (lights on 0700 h) with standard chow (Special Diet Services, Essex, UK) and water available ad libitum. For the initial antidepressant dose–response and time–course study (see below), the male FVB/N mice (4 months of age) were from Harlan UK. All mice were killed by decapitation, in the morning, 16 h after the last injection. Brains were removed, snap frozen on soft dry ice, and stored at −80°C. Trunk blood was collected for corticosterone measurements. All studies were performed to the highest standard of animal care under the aegis of the UK Animals (Scientific Procedures) Act, 1986.
Antidepressant Administration
For the main experiments presented in this paper, the abcb1ab (−/−) mice and FVB/N controls were administered desipramine (Sigma, UK), 10 mg/kg, i.p., twice daily (total dose: 20 mg/kg/d) for 7 days (n=5–7 per group). This dose and length of treatment was chosen because we were interested in examining the shortest period of time needed by the antidepressant for inducing GR changes. In a preliminary time–course and dose–response study, we compared FVB/N controls treated with desipramine 20 mg/kg/day for 1 week, 20 mg/kg/day for 2 weeks, or 10 mg/kg/day for 3 weeks (see below for the methods). We found the greatest effects after 1 week of 20 mg/kg/day, with a significant upregulation of the GR in the CA1 area (+32%; p=0.011). After 2 weeks of 20 mg/kg/day, there were smaller, nonsignificant increases of GR in the CA1 (+10%), whereas after 3 weeks of 10/mg/kg/day, there was no evidence of GR upregulation. Therefore, we used the regime of 1 week of desipramine 20 mg/kg/day for our subsequent main experiments. The 20 mg/kg/day dose was administered in 2 separate i.p. injections, as described by Uhr et al (2000) in these mice. Desipramine was dissolved in sterile 0.9% saline at 1 mg/ml, and controls received saline, 10 ml/kg, i.p., twice daily. Untreated (ie naive mice that have not received any treatments) abcb1ab (−/−) and FVB/N (n=4 per group) were also included in the study, for comparison.
mRNA In Situ Hybridization Histochemistry in the Hippocampus
Brain sections (10 μm) at the level of the hippocampus (Bregma − 2.3 mm, plate 50 from Franklin and Paxinos, The Mouse Brain in Stereotaxic Coordinates) were mounted on silane-coated slides and postfixed in 4% paraformaldehyde followed by acetylation (0.25% acetic anhydride in 0.1 M triethanolamine, pH 8.0); the sections were then washed in phosphate-buffered saline, dehydrated through graded alcohols, and air-dried. The medial amygdaloid nucleus and retrosplenial agranular cortex were also analyzed on the same sections. Hybridization was carried out as described previously (Yau et al, 1997) using [35S]UTP-labeled cRNA antisense probes transcribed in vitro from cDNA clones encoding: rat MR and GR (kindly supplied by Drs R Evans, J Arriza, and R Miesfeld); the mouse Mdr1a (889 bp fragment excised from the original full length clone from Alfred Schinkel and subcloned into pBluescript, kindly supplied by Dr Onno Meijer) (Not1 cut plasmid and T3 RNA polymerase for antisense probes; EcoR1 cut plasmid and T7 RNA polymerase for sense probes); and the mouse 11β-HSD1 (160–615 bp PCR product inserted into a pCR™11 vector) (Not1 cut plasmid and SP6 RNA polymerase for antisense probes; kpn1 cut plasmid and T7 RNA polymerase for sense probes). Following hybridization, sections were treated with ribonuclease A (30 μg/ml, 45 min, 37°C) and washed to a final stringency of 0.1 × SSC at 60°C. Slides were dehydrated, dipped in photographic emulsion (NTB-2, Kodak, UK), and exposed at 4°C for 21 days before developing and counterstaining with 1% pyronine. Hybridization signal within hippocampal subregions was assessed by computer-assisted grain counting using an image analysis system (Imaging Associates Ltd, UK). Silver grains were counted in a fixed circular area, under bright-field illumination, over individual hippocampal cells within each hippocampal subfields (see Figure 1), except for the dentate gyrus, where it was difficult to define cell boundaries, and therefore the fixed circular area covered one cell and a fraction of neighboring cells). The analysis was carried out blind to drug treatment. For each animal, 15–18 cells per subregion were assessed (over three hippocampal sections per animal), and background, counted over areas of white matter, was subtracted.
Photomicrograph showing GR mRNA expression in CA1 pyramidal cells from FVB/N controls mice treated with saline, under × 40 light microscope objective. Silver grains, which appear black under bright field, represent GR mRNA expression. The black circle shows the size of the fixed area used on the image analysis program to measure the grain density per cell.
Plasma Corticosterone Levels
Plasma corticosterone levels were measured by radioimmunoassay modified for microtitre plate scintillation proximity assay (Amersham Int., UK) with a highly specific antiserum (Dr C Kenyon, Centre for Cardiovascular Science, Queen's Medical Research Institute, Edinburgh, UK) and [3H]corticosterone (Amersham Int., UK). The detection limit of the RIA was 0.02 pmol corticosterone in 20 μl, or 0.03 μg/dl.
Statistical Analysis
Data are presented as mean and standard error of the mean (SEM). Data were analyzed using two-way analysis of variance (ANOVA) (multivariate when appropriate) with genotype (FVB/N controls vs abcb1ab (−/−) mice) and treatment (untreated vs saline vs desipramine) as main factors; this was followed by between-group Student's t-test comparisons when the ANOVA indicated a significant effect.
RESULTS
Effects of Desipramine on GR mRNA Expression in the Hippocampus, Amygdala, and Cortex
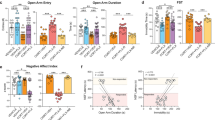
GR mRNA was measured in the hippocampus, amygdala, and cortex, as detailed in the methods. The analysis of hippocampal GR showed a significant interaction between hippocampal subregion, genotype, and treatment (two-way (multivariate) ANOVA; F6, 52=2.4; p=0.04; see Figure 2, panel a for FVB/N controls and panel b for abcb1ab (−/−) mice). Post hoc analysis showed that, compared to saline, desipramine induced a significant upregulation of GR mRNA in the CA1 region of FVB/N controls (+31%; p=0.045; see Figure 2, panel a, black vs white column), whereas it induced a significant downregulation of GR mRNA in CA1 of abcb1ab (−/−) mice (−45%; p=0.004; see Figure 2, panel b, black vs white column). The analysis of amygdala GR also showed a significant interaction between genotype and treatment (two-way ANOVA; F5, 27=4.4; p=0.022; see Figure 3). Post hoc analysis, however, showed opposite results than in the hippocampus: compared with saline, desipramine induced a significant upregulation of GR mRNA in abcb1ab (−/−) mice (+31%; black vs white columns on the right; p=0.04), whereas inducing a (nonsignificant) downregulation of GR mRNA in FVB/N controls mice (−27%; black vs white columns on the left; p=0.12). Finally, the analysis of cortical GR showed no interaction between genotype and treatment (two-way ANOVA; F5, 27=1.4; p=0.3; see Figure 4), nor any main effects of genotype (F1, 27=1.7; p=0.2) or treatment (F2, 27=1.2; p=0.3).
Expression of GR mRNA in the hippocampus of FVB/N controls (a) and abcb1ab (−/−) mice (b), measured by in situ hybridization histochemistry. Data are presented as mean±SEM of grains/cell. Compared to saline, desipramine induced a significant upregulation of the GR mRNA expression in the CA1 region of FVB/N controls (Panel a, black vs white column), whereas it induced a significant downregulation of GR mRNA expression in the CA1 region of the abcb1ab (−/−) mice (Panel b, black vs white column). There were no differences in GR expression between saline-treated and-untreated mice, for both strains (gray vs white columns in a and b). *p<0.05 vs saline in the same strain.
Expression of GR mRNA in the amygdala of FVB/N controls and abcb1ab (−/−) mice measured by in situ hybridization histochemistry. Data are presented as mean±SEM of grains/cell. Compared to saline, desipramine induced a significant upregulation of the GR mRNA expression in the CA1 region of abcb1ab (−/−) mice (black vs white column on the right). There were no differences in GR expression between saline-treated and untreated mice, for both strains (gray vs white columns). *p<0.05 vs saline in the same strain.
It is of note that there were no differences in GR mRNA levels between saline-treated and untreated mice, for all three brain areas and for both strains; this indicates that the i.p. injections had no effects on GR expression per se (gray vs white columns in Figures 2, 3 and 4).
Effects of Desipramine on MR mRNA Expression in the Hippocampus
The analysis of MR mRNA revealed no interaction between the hippocampal subregion, genotype, and treatment (two-way ANOVA; F8, 50=0.7; p=0.7; see Figure 5, panel a for FVB/N controls and panel b for abcb1ab (−/−) mice), nor any main effects of genotype (F1, 27=0.3; p=0.6) or treatment (F2, 27=0.1; p=0.9).
Effects of Desipramine on Plasma Corticosterone Levels
The analysis of corticosterone levels in the two strains of mice showed a significant interaction between genotype and treatment (two-way ANOVA; F5, 27=3.1; p=0.025; see Figure 6). Post hoc analyses showed that untreated abcb1ab (−/−) mice had lower corticosterone levels than untreated FVB/N mice (gray column on the right vs gray column on the left; p=0.02); this replicates the findings by Muller et al (2003). It is also of note that there was an increase of corticosterone levels in saline-treated abcb1ab (−/−) mice compared with untreated abcb1ab (−/−) mice (gray vs white columns on the right; p=0.053), whereas the same phenomenon did not occur in FVB/N controls (gray vs white columns on the left; p=0.7).
Corticosterone levels measured in the plasma of FVB/N controls (left) and abcb1ab (−/−) mice (right). Untreated abcb1ab (−/−) mice had lower corticosterone levels than untreated FVB/N mice (gray column on the right vs gray column on the left). There was an increase of corticosterone levels in saline-treated abcb1ab (−/−) mice compared with untreated abcb1ab (−/−) mice (gray vs white columns on the right; p=0.053). In FVB/N controls, desipramine decreased corticosterone levels not only compared with saline-treated mice (black vs white columns on the left), but also compared with untreated mice (black vs gray columns on the left). In contrast, in abcb1ab (−/−) mice, desipramine only reduced corticosterone levels compared with saline treatment (black vs white columns on the right), to levels that were equal to those of untreated mice (black vs gray columns on the right). #p⩽0.05 vs untreated FVB/N controls; *p⩽0.05 vs saline in the same strain.
Desipramine reduced corticosterone levels in both mice groups, but in abcb1ab (−/−) mice the effects were smaller. In FVB/N controls, desipramine decreased corticosterone levels not only compared with saline-treated mice (black vs white columns on the left; p=0.05), but also compared with naive mice (black vs gray columns on the left; p=0.05): ie after desipramine, corticosterone in FVB/N controls was lower (−39%) than the ‘physiological’ levels of naive mice. In contrast, in abcb1ab (−/−) mice, desipramine only reduced corticosterone levels compared with saline treatment (black vs white columns on the right; p=0.05) to levels that were equal to those of naive mice (black vs gray columns on the right; p=0.9).
Effects of Desipramine on MDR PGP and 11β-HSD1 mRNAs
The analysis of Mdr1a in the hippocampus (of FVB/N controls only) showed a significant interaction between subregion and the treatment (multivariate ANOVA; F8, 20=2.7; p=0.03; see Figure 7). Specifically, compared to saline, desipramine induced a significant downregulation of Mdr1a mRNA across all five subregions (−9 to −23%; multivariate ANOVA, F1, 9=5.7; p=0.04; black vs white columns). It is of note that there were no differences between saline-treated and untreated mice, showing that the i.p. injections had no effects of Mdr1a (gray vs white columns).
Expression of MDR PGP mRNA in the hippocampus of FVB/N controls measured by in situ hybridization histochemistry. Data are presented as mean±SEM of grains/cell. Compared to saline, desipramine induced a significant downregulation of MDR PGP mRNA expression across all five subregions (black vs white columns). There were no differences between saline-treated and untreated mice (gray vs white columns). The dotted line marked by * indicates the significant (p=0.04) main difference between desipramine- and saline-treated mice.
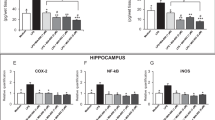
The analysis of hippocampal 11β-HSD1 revealed no interaction between hippocampal subregion, genotype, and treatment (two-way ANOVA; F8, 54=1.5; p=0.2; see Figure 8, panel a for FVB/N controls and panel b for abcb1ab (−/−) mice), nor any main effects of genotype (F1, 29=1.9; p=0.2) or treatment (F1, 29=1.0; p=0.4).
DISCUSSION
This is the first study to identify a mechanism through which antidepressants can induce GR upregulation and reduce HPA axis activity in vivo. We find that lack of the glucocorticoid transporters, MDR PGP abcb1a and 1b, prevents GR upregulation in the hippocampus induced by desipramine, and reduces the ability of desipramine to decrease plasma corticosterone levels. These findings are remarkably consistent with previous work in cell lines, by us and others, showing that antidepressants are unable to potentiate GR-mediated gene transcription in the presence of an MDR PGP inhibitor or of a glucocorticoid that is not transported by MDR PGP (Pariante et al, 1997, 2001, 2003a, 2003b, 2004b; Budziszewska et al, 2000; Miller et al, 2002; Herr et al, 2003). Moreover, we find that desipramine reduces MDR PGP (Mdr1a) expression in the hippocampus of FVB/N control controls, again consistent with previous work in cell lines (Varga et al, 1996; Szabo et al, 1999; Weiss et al, 2003; Pariante et al, 2003b; Weber et al, 2005). Finally, we replicate the previous finding by Muller et al (2003) showing that abcb1ab (−/−) mice have lower corticosterone levels than FVB/N controls. Indeed, desipramine treatment (in our model, a pharmacological ‘knockdown’ of MDR PGP) also lowers plasma corticosterone levels in controls, to levels indistinguishable from abcb1ab (−/−) mice. This confirms the notion that MDR PGP is indeed a barrier to corticosterone access to the brain, and that its absence leads to more corticosterone entering the brain, and thus to an increased negative feedback on the HPA axis. Taken together with previous in vitro work, the present study strongly supports our proposed model that one mechanism through which antidepressants regulate the HPA axis is by reducing the action of glucocorticoid transporters like MDR PGP on the endothelial cells of the BBB (and possibly in neurons), thus leading to enhanced entry of glucocorticoids into the brain and so to facilitated negative feedback (Pariante et al, 2001, 2003a, 2003b, 2004b; Pariante, 2006).
It is interesting that, in FVB/N controls, there were no effects of desipramine on GR expression in the cortex, and there was a tendency (although not significant) for a GR downregulation in the amygdala. Very few studies have examined the effects of tricyclic antidepressants on GR expression in these areas, and, consistent with our results, have found that GR is decreased (not significantly) in the amygdala (Peiffer et al, 1991b), and unchanged in the cortex (Seckl and Fink, 1992), in the presence of GR upregulation in the hippocampus (Peiffer et al, 1991b; Seckl and Fink, 1992). In contrast, one study in transgenic mice with decreased GR expression has found that desipramine increases GR expression in the cortex of these animals (Pepin et al, 1992). The desipramine-induced GR upregulation in the amygdala of abcb1ab (−/−) mice (as opposed to the tendency for a downregulation in the amygdala of FVB/N controls) is also puzzling, although is consistent with the notion that, as for the hippocampal GR, desipramine have opposite effects on the GR in these two mice groups. GR expression is differently regulated in the hippocampus, cortex, and amygdala, and powerful GR manipulations such as adrenalectomy, glucocorticoid treatment, and programming induce different effects on GR expression in these areas (Meaney et al, 1985; Sapolsky and McEwen, 1985; Pepin et al, 1990; Peiffer et al, 1991a; Welberg et al, 2001), although the molecular mechanisms underlying these localized differences are still unclear.
The second important finding of this study is that desipramine decreases corticosterone levels in both FVB/N controls and in abcb1ab (−/−) mice, but in abcb1ab (−/−) mice the effects are smaller. Specifically, in FVB/N controls (but not in abcb1ab (−/−) mice), desipramine reduces corticosterone levels not only compared with saline-treated mice, but also compared with the physiological levels of untreated mice. Interestingly, saline treatment seems to activate the HPA axis in the abcb1ab (−/−) mice, but not in FVB/N controls. This may be due to the fact that abcb1ab (−/−) mice suffer from spontaneous colitis (Banner et al, 2004) and, therefore, could be more sensitive to the manipulation associated with two daily i.p. injections for 1 week. Taken together, these results suggest that desipramine in abcb1ab (−/−) mice can reduce an activated HPA axis, but cannot reduce basal HPA axis activity, whereas in FVB/N controls, desipramine can also reduce basal HPA activity. This, of course, also emphasizes that MDR PGP is not the only mechanisms involved in the antidepressant-induced reduction in HPA axis activity (see below).
How can we reconcile that desipramine decreases corticosterone levels in both mice groups, but in the presence of hippocampal GR upregulation in FVB/N controls and hippocampal GR downregulation in abcb1ab (−/−) mice? Our preferred model is that desipramine initially increases hippocampal GR translocation and function in both mice groups; the increased GR translocation and function lead to both the reduced corticosterone levels (following enhanced negative feedback) and the GR downregulation (following GR internalization into cellular nuclei). This model is supported by studies in rats, where antidepressants decrease HPA axis activity and induce GR downregulation within the first few days of treatment (Reul et al, 1993; Yau et al, 2001), and by studies in vitro, where antidepressants induce GR translocation and GR downregulation within one or 2 days of treatment (Pariante et al, 1997, 2003a; Okugawa et al, 1999; Yau et al, 2001; Heiske et al, 2003). Indeed, Mukherjee et al (2004) found that one single dose of imipramine in mice induces GR translocation in the CA1 subregion, the same area where we find the GR downregulation. GR translocation and internalization into cellular nuclei may lead to GR downregulation via reduced GR protein half-life and inhibition of GR mRNA synthesis (Schmidt and Meyer, 1994). Of course, this model implies that GR activation by antidepressants is independent from inhibition of MDR PGP, as it seems to be present in the abcb1ab (−/−) mice. It is possible that abcb1ab (−/−) mice express other transporters that regulate the access of glucocorticoids to neuronal cells and that could be inhibited by antidepressants, like the MDR-associated protein (MRP or ABCC1) (Herr et al, 2000; Hirrlinger et al, 2002; Sisodiya et al, 2002). Indeed, we have recently described that the tricyclic antidepressant, clomipramine, increases the intracellular concentration of glucocorticoids in rat cortical neurons, where MDR PGP has not been described (Pariante et al, 2003a). Alternatively, or additionally, antidepressants can activate the GR by regulating a variety of second-messenger mechanisms (Maes et al, 1999; Budziszewska et al, 2000; Basta-Kaim et al, 2002, 2004, 2006; Budziszewska et al, 2004; Yehuda et al, 2004, 2006; Wang et al, 2005). Incidentally, we show here that one important pathway regulating glucocorticoid action in the brain, the enzyme 11β-HSD1 (Seckl and Walker, 2001), is not regulated by desipramine. Why then would the GR upregulation develop only in FVB/N mice, but not in the abcb1ab (−/−) mice? We propose that, in FVB/N mice only, the additional effects of desipramine on MDR PGP increase corticosterone access to the brain and thus further enhance the negative feedback, thus reducing plasma corticosterone beyond physiological levels and inducing GR upregulation as a consequence of the peripheral changes in HPA axis. Indeed, in rats, GR upregulation by antidepressants tends to occur after several days or weeks of treatment in the presence of reduced corticosterone levels and following the initial GR downregulation (reviewed in Pariante et al, 2004b).
In two recent papers, Weber et al (2005, 2006) have directly challenged our hypothesis that inhibition of MDR PGP function is relevant to the effects of antidepressants on the HPA axis. In the first paper, in mice, the authors have found that the tricyclic antidepressant, amitriptyline, had no effects on plasma or brain corticosterone levels (Weber et al, 2006). However, measuring endogenous corticosterone in the brain may not be appropriate to address this issue, because antidepressant-induced changes in plasma corticosterone would alter the levels in the brain and, hence, confound any inference on BBB permeability (Carroll et al, 1975). Measuring the access to the brain of radioactive glucocorticoids administered in the periphery (Meijer et al, 1998; Karssen et al, 2001 2002; Muller et al, 2003), or through brain perfusion (Pariante et al, 2004b), are more appropriate techniques to answer this kind of question. Moreover, these authors administered amitriptyline 10 mg/kg/d, a dose that may be too low to affect the HPA axis in mice. In the present study, we administered desipramine 20 mg/kg/day, and in our dose–response study, we found no effect of 10 mg/kg/day of desipramine on GR or MR in the hippocampus. Two other studies using tricyclic antidepressants in mice have also found that 20 mg/kg/day increase brain GR levels and reduce HPA axis activity (Pepin et al, 1992; Mukherjee et al, 2004). In the second paper, in vitro, the authors have confirmed previous work by us and others showing that the inhibiting effects of antidepressants on MDR PGP function occur at micromolar concentrations (Varga et al, 1996; Szabo et al, 1999; Weiss et al, 2003; Pariante et al, 2003b), but have concluded that these concentrations are ‘above therapeutically relevant plasma levels’ (Weber et al, 2005). However, micromolar concentration of antidepressants are achieved in the brain of animals treated with the doses used in this and similar studies showing HPA axis changes by antidepressants (Glotzbach and Preskorn, 1982), and, most importantly, are achieved in the brain of patients taking therapeutic doses of antidepressants. In fact, in vivo neuroimaging studies using spectroscopy, which are only possible with antidepressants containing fluorine atoms such as fluoxetine and fluvoxamine, have consistently described steady-state brain concentrations of these drugs in the micromolar range (Bolo et al, 2000). Moreover, brain concentrations of tricyclics in humans, largely derived from postmortem studies following overdoses, have described brain-to-plasma concentration ratios ranging from eightfold, at higher plasma concentrations, to 125-fold, at lower plasma concentrations (Sunshine and Baeumler, 1963; Bickel et al, 1967; Avella et al, 2004). Therefore, considering that the plasma concentrations of tricyclics in patients taking therapeutic doses range 100–250 ng/ml (ie approximately 0.4–0.9 μM for desipramine and amitryptiline, and 0.3–0.8 μM for clomipramine), even a conservative estimate of a brain-to-plasma concentration of 10 would lead to micromolar concentrations of tricyclic antidepressants in the brain of patients.
One limitation of our study is that we have not been successful in measuring the levels of desipramine in the brain (using high-performance liquid chromatography; data not shown): desipramine levels were below the limit of detection (ranging 150–300 ng/g in different samples). These would have been interesting data, as previous studies (Uhr et al, 2000, 2003; Uhr and Grauer, 2003) have shown, also using abcb1ab (−/−) mice, that MDR PGP limits the access to the brain of the tricyclic antidepressants, doxepine, amitriptyline, nortriptyline and trimipramine, after a single injection (although no data are available on desipramine). However, our study protocol was aimed at detecting persisting changes in the HPA axis, rather than the steady-state brain concentrations of antidepressants, and, therefore, the mice were killed 16 h after the last injection, whereas in previous studies measuring brain antidepressants levels, the animals were killed 15–60 min after single injections (Glotzbach and Preskorn, 1982; Uhr et al, 2000, 2003; Uhr and Grauer, 2003) or 4 h after the last injections in chronic-treatment studies (Grauer and Uhr, 2004); this could explain our negative findings. Theoretically, it is possible that abcb1ab (−/−) mice in our study have higher brain concentrations of desipramine, and that this might explain the differences in the GR expression. However, it is important to note that chronic treatment is different from a single injection; indeed, these same authors have found that after 10 days of administration (20 mg/kg/d in two i.p. injections, as in our study) only nortriptyline brain levels were elevated in abcb1ab (−/−) mice (approximately threefold), whereas amitriptyline brain levels were identical to those of FVB/N controls (Grauer and Uhr, 2004). Nevertheless, even if brain levels of desipramine were increased in abcb1ab (−/−) mice, there is no evidence that higher doses of tricyclic could lead to hippocampal GR downregulation rather than upregulation. In fact, one study in rats treated with amitriptyline (for 5 weeks) have found no evidence of hippocampal GR downregulation even using a dose that was 15-fold larger than the minimal dose able to induce GR upregulation (Reul et al, 1993).
In conclusion, we have found that desipramine requires MDR PGP to induce GR upregulation in mice, and that this effect is associated with downregulation of MDR PGP. Although some effects on the HPA axis are present in abcb1ab (−/−) mice treated with desipramine, our study clearly indicates that decreasing MDR PGP function by downregulation (and possibly direct pharmacological inhibition) is at least one of the molecular mechanisms involved in the HPA axis regulation by antidepressants. We suggest that MDR PGP could be a novel pharmacological target for developing new drugs that can treat depression by normalizing HPA axis activity in depressed patients (Nemeroff and Owens, 2002).
References
Avella J, Lehrer M, Katz M, Minden E (2004). Two cases involving clomipramine intoxication. J Anal Toxicol 28: 504–508.
Banner KH, Cattaneo C, Le Net JL, Popovic A, Collins D, Gale JD (2004). Macroscopic, microscopic and biochemical characterisation of spontaneous colitis in a transgenic mouse, deficient in the multiple drug resistance 1a gene. Br J Pharmacol 143: 590–598.
Basta-Kaim A, Budziszewska B, Jaworska-Feil L, Tetich M, Kubera M, Leskiewicz M et al (2004). Mood stabilizers inhibit glucocorticoid receptor function in LMCAT cells. Eur J Pharmacol 495: 103–110.
Basta-Kaim A, Budziszewska B, Jaworska-Feil L, Tetich M, Kubera M, Leskiewicz M et al (2006). Antipsychotic drugs inhibit the human corticotropin-releasing-hormone gene promoter activity in neuro-2A cells-an involvement of protein kinases. Neuropsychopharmacology 31: 853–865.
Basta-Kaim A, Budziszewska B, Jaworska-Feil L, Tetich M, Leskiewicz M, Kubera M et al (2002). Chlorpromazine inhibits the glucocorticoid receptor-mediated gene transcription in a calcium-dependent manner. Neuropharmacology 43: 1035–1043.
Bickel MH, Brochon R, Friolet B, Herrmann B, Stofer AR (1967). Clinical and biochemical results of a fatal case of desipramine intoxication. Psychopharmacologia 10: 431–436.
Bolo NR, Hode Y, Nedelec JF, Laine E, Wagner G, Macher JP (2000). Brain pharmacokinetics and tissue distribution in vivo of fluvoxamine and fluoxetine by fluorine magnetic resonance spectroscopy. Neuropsychopharmacology 23: 428–438.
Budziszewska B, Jaworska-Feil L, Kajta M, Lason W (2000). Antidepressant drugs inhibit glucocorticoid receptor-mediated gene transcription—a possible mechanism. Br J Pharmacol 130: 1385–1393.
Budziszewska B, Jaworska-Feil L, Tetich M, Basta-Kaim A, Kubera M, Leskiewicz M et al (2004). Regulation of the human corticotropin-releasing-hormone gene promoter activity by antidepressant drugs in Neuro-2A and AtT-20 cells. Neuropsychopharmacology 29: 785–794.
Carroll BJ, Heath B, Jarrett DB (1975). Corticosteroids in brain tissue. Endocrinology 97: 290–300.
de Kloet ER, Vreugdenhil E, Oitzl MS, Joels M (1998). Brain corticosteroid receptor balance in health and disease. Endocr Rev 19: 269–301.
Flores BH, Kenna H, Keller J, Solvason HB, Schatzberg AF (2006). Clinical and biological effects of mifepristone treatment for psychotic depression. Neuropsychopharmacology 31: 628–636.
Glotzbach RK, Preskorn SH (1982). Brain concentrations of tricyclic antidepressants: single-dose kinetics and relationship to plasma concentrations in chronically dosed rats. Psychopharmacology (Berl) 78: 25–27.
Grauer MT, Uhr M (2004). P-glycoprotein reduces the ability of amitriptyline metabolites to cross the blood brain barrier in mice after a 10-day administration of amitriptyline. J Psychopharmacol 18: 66–74.
Heiske A, Jesberg J, Krieg JC, Vedder H (2003). Differential effects of antidepressants on glucocorticoid receptors in human primary blood cells and human monocytic u-937 cells. Neuropsychopharmacology 28: 807–817.
Herr AS, Tsolakidou AF, Yassouridis A, Holsboer F, Rein T (2003). Antidepressants differentially influence the transcriptional activity of the glucocorticoid receptor in vitro. Neuroendocrinology 78: 12–22.
Herr AS, Wochnik GM, Rosenhagen MC, Holsboer F, Rein T (2000). Rifampicin is not an activator of glucocorticoid receptor. Mol Pharmacol 57: 732–737.
Hirrlinger J, Konig J, Dringen R (2002). Expression of mRNAs of multidrug resistance proteins (Mrps) in cultured rat astrocytes, oligodendrocytes, microglial cells and neurones. J Neurochem 82: 716–719.
Holsboer F (2000). The corticosteroid receptor hypothesis of depression. Neuropsychopharmacology 23: 477–501.
Juruena MF, Cleare AJ, Papadopoulos AS, Poon L, Lightman S, Pariante CM (2006). Different responses to dexamethasone and prednisolone in the same depressed patients. Psychopharmacology (Berl) 189: 225–235.
Karssen AM, Meijer OC, van der Sandt I, de Boer AG, de Lange EC, de Kloet ER (2002). The role of the efflux transporter P-glycoprotein in brain penetration of prednisolone. J Endocrinol 175: 251–260.
Karssen AM, Meijer OC, van der Sandt I, Lucassen PJ, de Lange EC, de Boer AG et al (2001). Multidrug resistance P-glycoprotein hampers the access of cortisol but not of corticosterone to mouse and human brain. Endocrinology 142: 2686–2694.
Kunzel HE, Binder EB, Nickel T, Ising M, Fuchs B, Majer M et al (2003). Pharmacological and nonpharmacological factors influencing hypothalamic-pituitary-adrenocortical axis reactivity in acutely depressed psychiatric in-patients, measured by the Dex-CRH test. Neuropsychopharmacology 28: 2169–2178.
Lai M, McCormick JA, Chapman KE, Kelly PAT, Seckl JR, Yau JLW (2003). Differential regulation of corticosteroid receptors by monoamine neurotransmitters and antidepressant drugs in primary hippocampal culture. Neuroscience 118: 975–984.
Maes M, Song C, Lin AH, Bonaccorso S, Kenis G, De Jongh R et al (1999). Negative immunoregulatory effects of antidepressants: inhibition of interferon-gamma and stimulation of interleukin-10 secretion. Neuropsychopharmacology 20: 370–379.
Meaney MJ, Aitken DH, Bodnoff SR, Iny LJ, Tatarewicz JE, Sapolsky RM (1985). Early postnatal handling alters glucocorticoid receptor concentrations in selected brain regions. Behav Neurosci 99: 765–770.
Meijer OC, de Lange EC, Breimer DD, de Boer AG, Workel JO, de Kloet ER (1998). Penetration of dexamethasone into brain glucocorticoid targets is enhanced in mdr1A P-glycoprotein knockout mice. Endocrinology 139: 1789–1793.
Miller AH, Vogt GJ, Pearce BD (2002). The phosphodiesterase type 4 inhibitor, rolipram, enhances glucocorticoid receptor function. Neuropsychopharmacology 27: 939–948.
Mukherjee K, Knisely A, Jacobson L (2004). Partial glucocorticoid agonist-like effects of imipramine on hypothalamic-pituitary-adrenocortical activity, thymus weight, and hippocampal glucocorticoid receptors in male C57BL/6 mice. Endocrinology 145: 4185–4191.
Muller MB, Keck ME, Binder EB, Kresse AE, Hagemeyer TP, Landgraf R et al (2003). ABCB1 (MDR1)-type P-glycoproteins at the blood–brain barrier modulate the activity of the hypothalamic-pituitary-adrenocortical system: implications for affective disorder. Neuropsychopharmacology 28: 1991–1999.
Neigh GN, Nemeroff CB (2006). Reduced glucocorticoid receptors: consequence or cause of depression? Trends Endocrinol Metab 17: 124–125.
Nemeroff CB, Owens MJ (2002). Treatment of mood disorders. Nat Neurosci 5 (Suppl): 1068–1070.
Okugawa G, Omori K, Suzukawa J, Fujiseki Y, Kinoshita T, Inagaki C (1999). Long-term treatment with antidepressants increases glucocorticoid receptor binding and gene expression in cultured rat hippocampal neurones. J Neuroendocrinol 11: 887–895.
Pariante CM (2004). Glucocorticoid receptor function in vitro in patients with major depression. Stress 7: 209–219.
Pariante CM (2006). The glucocorticoid receptor: part of the solution or part of the problem? J Psychopharmacol 20: 79–84.
Pariante CM, Hye A, Williamson R, Makoff A, Lovestone S, Kerwin RW (2003a). The antidepressant clomipramine regulates cortisol intracellular concentrations and glucocorticoid receptor expression in fibroblasts and rat primary neurones. Neuropsychopharmacology 28: 1553–1561.
Pariante CM, Kim RB, Makoff A, Kerwin RW (2003b). Antidepressant fluoxetine enhances glucocorticoid receptor function in vitro by modulating membrane steroid transporters. Br J Pharmacol 139: 1111–1118.
Pariante CM, Makoff A, Lovestone S, Feroli S, Heyden A, Miller AH et al (2001). Antidepressants enhance glucocorticoid receptor function in vitro by modulating the membrane steroid transporters. Br J Pharmacol 134: 1335–1343.
Pariante CM, Papadopoulos AS, Poon L, Cleare AJ, Checkley SA, English J et al (2004a). Four days of citalopram increase suppression of cortisol secretion by prednisolone in healthy volunteers. Psychopharmacology (Berl) 177: 200–206.
Pariante CM, Pearce BD, Pisell TL, Owens MJ, Miller AH (1997). Steroid-independent translocation of the glucocorticoid receptor by the antidepressant desipramine. Mol Pharmacol 52: 571–581.
Pariante CM, Thomas SA, Lovestone S, Makoff A, Kerwin RW (2004b). Do antidepressants regulate how cortisol affects the brain? 2003 Curt Richter Award Paper. Psychoneuroendocrinology 29: 423–447.
Peiffer A, Lapointe B, Barden N (1991a). Hormonal regulation of type II glucocorticoid receptor messenger ribonucleic acid in rat brain. Endocrinology 129: 2166–2174.
Peiffer A, Veilleux S, Barden N (1991b). Antidepressant and other centrally acting drugs regulate glucocorticoid receptor messenger RNA levels in rat brain. Psychoneuroendocrinology 16: 505–515.
Pepin MC, Beaulieu S, Barden N (1989). Antidepressants regulate glucocorticoid receptor messenger RNA concentrations in primary neuronal cultures. Brain Res Mol Brain Res 6: 77–83.
Pepin MC, Beaulieu S, Barden N (1990). Differential regulation by dexamethasone of glucocorticoid receptor messenger RNA concentrations in neuronal cultures derived from fetal rat hypothalamus and cerebral cortex. Cell Mol Neurobiol 10: 227–235.
Pepin MC, Pothier F, Barden N (1992). Antidepressant drug action in a transgenic mouse model of the endocrine changes seen in depression. Mol Pharmacol 42: 991–995.
Reul JM, Stec I, Soder M, Holsboer F (1993). Chronic treatment of rats with the antidepressant amitriptyline attenuates the activity of the hypothalamic-pituitary-adrenocortical system. Endocrinology 133: 312–320.
Rossby SP, Nalepa I, Huang M, Perrin C, Burt AM, Schmidt DE et al (1995). Norepinephrine-independent regulation of GRII mRNA in vivo by a tricyclic antidepressant. Brain Res 687: 79–82.
Sapolsky RM, McEwen BS (1985). Down-regulation of neural corticosterone receptors by corticosterone and dexamethasone. Brain Res 339: 161–165.
Schinkel AH, Mayer U, Wagenaar E, Mol CA, van Deemter L, Smit JJ et al (1997). Normal viability and altered pharmacokinetics in mice lacking mdr1-type (drug-transporting) P-glycoproteins. Proc Natl Acad Sci USA 94: 4028–4033.
Schmidt TJ, Meyer AS (1994). Autoregulation of corticosteroid receptors. How, when, where, and why? Receptor 4: 229–257.
Seckl JR, Fink G (1992). Antidepressants increase glucocorticoid and mineralocorticoid receptor mRNA expression in rat hippocampus in vivo. Neuroendocrinology 55: 621–626.
Seckl JR, Walker BR (2001). Minireview: 11β-hydroxysteroid dehydrogenase type 1- a tissue-specific amplifier of glucocorticoid action. Endocrinology 142: 1371–1376.
Sisodiya SM, Lin WR, Harding BN, Squier MV, Thom M (2002). Drug resistance in epilepsy: expression of drug resistance proteins in common causes of refractory epilepsy. Brain 125: 22–31.
Sunshine I, Baeumler J (1963). A fatal case of poisoning with amitriptyline. Nature 199: 1103–1104.
Szabo D, Szabo Jr G, Ocsovszki I, Aszalos A, Molnar J (1999). Anti-psychotic drugs reverse multidrug resistance of tumor cell lines and human AML cells ex-vivo. Cancer Lett 139: 115–119.
Uhr M, Grauer MT (2003). abcb1ab P-glycoprotein is involved in the uptake of citalopram and trimipramine into the brain of mice. J Psychiatr Res 37: 179–185.
Uhr M, Grauer MT, Holsboer F (2003). Differential enhancement of antidepressant penetration into the brain in mice with abcb1ab (mdr1ab) P-glycoprotein gene disruption. Biol Psychiatry 54: 840–846.
Uhr M, Holsboer F, Muller MB (2002). Penetration of endogenous steroid hormones corticosterone, cortisol, aldosterone and progesterone into the brain is enhanced in mice deficient for both mdr1a and mdr1b P-glycoproteins. J Neuroendocrinol 14: 753–759.
Uhr M, Steckler T, Yassouridis A, Holsboer F (2000). Penetration of amitriptyline, but not of fluoxetine, into brain is enhanced in mice with blood–brain barrier deficiency due to mdr1a P-glycoprotein gene disruption. Neuropsychopharmacology 22: 380–387.
van West D, Van Den EF, Del Favero J, Souery D, Norrback KF, Van Duijn C et al (2006). Glucocorticoid receptor gene-based SNP analysis in patients with recurrent major depression. Neuropsychopharmacology 31: 620–627.
Varga A, Nugel H, Baehr R, Marx U, Hever A, Nacsa J et al (1996). Reversal of multidrug resistance by amitriptyline in vitro. Anticancer Res 16: 209–211.
Wang X, Wu H, Lakdawala VS, Hu F, Hanson ND, Miller AH (2005). Inhibition of Jun N-terminal kinase (JNK) enhances glucocorticoid receptor-mediated function in mouse hippocampal HT22 cells. Neuropsychopharmacology 30: 242–249.
Weber CC, Eckert GP, Muller WE (2006). Effects of antidepressants on the brain/plasma distribution of corticosterone. Neuropsychopharmacology 31: 2443–2448.
Weber CC, Kressmann S, Ott M, Fricker G, Muller WE (2005). Inhibition of P-glycoprotein function by several antidepressants may not contribute to clinical efficacy. Pharmacopsychiatry 38: 293–300.
Weiss J, Dormann SM, Martin-Facklam M, Kerpen CJ, Ketabi-Kiyanvash N, Haefeli WE (2003). Inhibition of P-glycoprotein by newer antidepressants. J Pharmacol Exp Ther 305: 197–204.
Welberg LA, Seckl JR, Holmes MC (2001). Prenatal glucocorticoid programming of brain corticosteroid receptors and corticotrophin-releasing hormone: possible implications for behaviour. Neuroscience 104: 71–79.
Yau JL, Noble J, Hibberd C, Seckl JR (2001). Short-term administration of fluoxetine and venlafaxine decreases corticosteroid receptor mRNA expression in the rat hippocampus. Neurosci Lett 306: 161–164.
Yau JL, Noble J, Seckl JR (1997). Site-specific regulation of corticosteroid and serotonin receptor subtype gene expression in the rat hippocampus following 3,4-methylenedioxymethamphetamine: role of corticosterone and serotonin. Neuroscience 78: 111–121.
Yehuda R, Yang RK, Golier JA, Grossman RA, Bierer LM, Tischler L (2006). Effect of sertraline on glucocorticoid sensitivity of mononuclear leukocytes in post-traumatic stress disorder. Neuropsychopharmacology 31: 189–196.
Yehuda R, Yang RK, Golier JA, Tischler L, Liong B, Decker K (2004). Effect of topiramate on glucocorticoid receptor mediated action. Neuropsychopharmacology 29: 433–439.
Young AH, Gallagher P, Watson S, Del Estal D, Owen BM, Nicol FI (2004). Improvements in neurocognitive function and mood following adjunctive treatment with mifepristone (RU-486) in bipolar disorder. Neuropsychopharmacology 29: 1538–1545.
Young EA, Lopez JF, Murphy-Weinberg V, Watson SJ, Akil H (2003). Mineralocorticoid receptor function in major depression. Arch Gen Psychiatry 60: 24–28.
Acknowledgements
This research was supported by a Clinician Scientist Fellowship (2004–2009) from the UK Medical Research Council (MRC) to CM Pariante. Dr Pariante's research was also funded by the National Alliance for Research on Schizophrenia and Depression (NARSAD) and the Guy's & St Thomas' Charitable Foundation.
This paper is dedicated to the memory of Professor Robert Kerwin. He was highly regarded by all of his colleagues, and he will be much missed.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Yau, J., Noble, J., Thomas, S. et al. The Antidepressant Desipramine Requires the ABCB1 (Mdr1)-Type p-Glycoprotein to Upregulate the Glucocorticoid Receptor in Mice. Neuropsychopharmacol 32, 2520–2529 (2007). https://doi.org/10.1038/sj.npp.1301389
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.npp.1301389
Keywords
This article is cited by
-
Platinum anticancer agents and antidepressants: desipramine enhances platinum-based cytotoxicity in human colon cancer cells
JBIC Journal of Biological Inorganic Chemistry (2012)
-
Antidepressants increase human hippocampal neurogenesis by activating the glucocorticoid receptor
Molecular Psychiatry (2011)
-
Clomipramine In Vitro Reduces Glucocorticoid Receptor Function in Healthy Subjects but not in Patients with Major Depression
Neuropsychopharmacology (2008)