« Prev Next »

Cell Division and Cancer
How Do Cancer Cells Differ from Normal Cells?
In normal cells, hundreds of genes intricately control the process of cell division. Normal growth requires a balance between the activity of those genes that promote cell proliferation and those that suppress it. It also relies on the activities of genes that signal when damaged cells should undergo apoptosis.
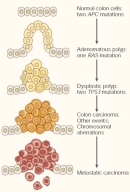
Cells become cancerous after mutations accumulate in the various genes that control cell proliferation. According to research findings from the Cancer Genome Project, most cancer cells possess 60 or more mutations. The challenge for medical researchers is to identify which of these mutations are responsible for particular kinds of cancer. This process is akin to searching for the proverbial needle in a haystack, because many of the mutations present in these cells have little to nothing to do with cancer growth.
Different kinds of cancers have different mutational signatures. However, scientific comparison of multiple tumor types has revealed that certain genes are mutated in cancer cells more often than others. For instance, growth-promoting genes, such as the gene for the signaling protein Ras, are among those most commonly mutated in cancer cells, becoming super-active and producing cells that are too strongly stimulated by growth receptors. Some chemotherapy drugs work to counteract these mutations by blocking the action of growth-signaling proteins. The breast cancer drug Herceptin, for example, blocks overactive receptor tyrosine kinases (RTKs), and the drug Gleevec blocks a mutant signaling kinase associated with chronic myelogenous leukemia.
Other cancer-related mutations inactivate the genes that suppress cell proliferation or those that signal the need for apoptosis. These genes, known as tumor suppressor genes, normally function like brakes on proliferation, and both copies within a cell must be mutated in order for uncontrolled division to occur. For example, many cancer cells carry two mutant copies of the gene that codes for p53, a multifunctional protein that normally senses DNA damage and acts as a transcription factor for checkpoint control genes.
How Do Cancerous Changes Arise?
Gene mutations accumulate over time as a result of independent events. Consequently, the path to cancer involves multiple steps. In fact, many scientists view the progression of cancer as a microevolutionary process.

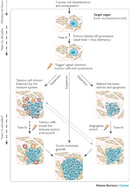
To understand what this means, consider the following: When a mutation gives a cancer cell a growth advantage, it can make more copies of itself than a normal cell can — and its offspring can outperform their noncancerous counterparts in the competition for resources. Later, a second mutation might provide the cancer cell with yet another reproductive advantage, which in turn intensifies its competitive advantage even more. And, if key checkpoints are missed or repair genes are damaged, then the rate of damage accumulation increases still further. This process continues with every new mutation that offers such benefits, and it is a driving force in the evolution of living things — not just cancer cells (Figure 1, Figure 2).
How Do Cancer Cells Spread to Other Tissues?
During the early stages of cancer, tumors are typically benign and remain confined within the normal boundaries of a tissue. As tumors grow and become malignant, however, they gain the ability to break through these boundaries and invade adjoining tissues.
Invasive cancer cells often secrete proteases that enable them to degrade the extracellular matrix at a tissue's boundary. Proteases also give cancer cells the ability to create new passageways in tissues. For example, they can break down the junctions that join cells together, thereby gaining access to new territories.Metastasis — literally meaning "new place" — is one of the terminal stages of cancer. In this stage, cancerous cells enter the bloodstream or the lymphatic system and travel to a new location in the body, where they begin to divide and lay the foundation for secondary tumors. Not all cancer cells can metastasize. In order to spread in this way, the cells must have the ability to penetrate the normal barriers of the body so that they can both enter and exit the blood or lymph vessels. Even traveling metastatic cancer cells face challenges when trying to grow in new areas (Figure 3).
Conclusion
eBooks
This page appears in the following eBook