Abstract
To investigate the role of pancreatic (group I) secretory PLA2 (sPLA2-I) in the pathogenesis of meconium aspiration syndrome, human particulate meconium or its supernatant either before or after extraction of PLA2-I was insufflated into rat lungs. In addition, the pulmonary effects of intra-tracheal human and bovine PLA2-I were studied. Lungs with saline instillation served as controls. Intrapulmonary particulate meconium (both before and after PLA2-I extraction), unlike meconium supernatant, resulted in markedly elevated lung tissue PLA2 catalytic activity and human PLA2-I concentrations when compared with controls. On the other hand, tissue concentrations of the group II PLA2 remained unchanged in all meconium lungs. Pulmonary PLA2-I concentrations further correlated positively with lung injury scores. Instillation of meconium-derived human PLA2-I, at a concentration of one-third of that in particulate meconium, did not raise PLA2 activity or concentrations of PLA2-I or PLA2-II in the lung tissue from the control level, but still resulted in significantly elevated lung wet/dry ratio and injury score. In contrast, insufflation of bovine pancreatic PLA2 increased the lung tissue enzyme activity and wet/dry ratio from the control level, but had no effect on the type II PLA2 concentration or lung injury score. Our data thus indicate that human pancreatic PLA2, introduced in high amounts within aspirated meconium especially in particulate form, is a potent inducer of lung tissue inflammatory injury.
Similar content being viewed by others
Main
Perinatal aspiration of meconium may result in severe pulmonary failure with ventilation-perfusion mismatch in the lungs, hypoxemia and increase in pulmonary vascular resistance, associated with high morbidity and mortality in full- or post-term newborn infants (1). The pathophysiology of the neonatal meconium aspiration syndrome (MAS) is complex, but inflammation with pulmonary surge of cytokines, possibly through activation of alveolar macrophages, and accumulation of polymorphonuclear leukocytes in the pulmonary tissue is believed to be a central event in the development of acute tissue damage (1,2). This inflammatory reaction is connected with increased lung epithelial cell apoptosis, which may together with inactivation of the pulmonary surfactant and direct toxic effects of meconium significantly contribute to the lung injury process (1,3,4). Still, the clinical effects of anti-inflammatory therapeutic approaches are unsatisfactory and do not consistently improve the outcome of severe complications of this disease (1). New advances into the pathophysiology and therapy of MAS are therefore needed.
Phospholipase A2 (PLA2) represents a family of ubiquitous enzymes that generate, by hydrolysing membrane phospholipids, biologically active FFA and lysophospholipids (5). In the lungs, activation of PLA2 by direct or indirect insults may lead through arachidonic acid to formation of pro-inflammatory lipid mediators, including eicosanoids and platelet-activating factor (6,7). Since PLA2 may also directly damage alveolar cells and inactivate surfactant (8,9), its activity is proposed to be important in the pathogenesis of acute inflammatory lung injury (6,8,10). The PLA2 enzymes occur as cytosolic (cPLA2) and secretory (sPLA2) types. Among the mammalian secretory (extracellular) PLA2's two well-characterized enzymes have been identified: group I secreted by the pancreas (PLA2-I) and group II (synovial) detected in inflammatory fluids (PLA2-II) (5,10). High PLA2 activity in inflammatory lung injury is generally connected with increased release of PLA2-II originating from macrophages and platelets, but other types of PLA2 enzymes may also play a modulating role (6). Previous studies in our laboratory in fact demonstrate that human meconium contains high amount of PLA2-I and that the PLA2 activity and concentration of PLA2-I in the meconium-contaminated lung tissue is high (3). Although these results connected intra-tracheal insufflation of particulate meconium with pulmonary inflammation, there are also data suggesting an important role for the soluble fraction of human meconium in the initiation of acute inflammatory response in the insulted lungs (3,4). We hypothesized that PLA2-I is present in both particulate and soluble fraction of meconium and that it contributes to the inflammatory and apoptotic lung injury induced by meconium aspiration, and therefore decided to investigate the pulmonary effects of meconium before and after extraction of PLA2-I, and also the direct effects of intra-tracheal PLA2-I. We additionally evaluated the contribution of the pulmonary PLA2-II production on the meconium-induced lung injury.
MATERIALS AND METHODS
Animal preparation.
Sixty-six male Sprague-Dawley rats (mean weight 320 g, SD 150 g) were studied. The animals were anesthetized with pentobarbital (60 mg/kg IP (intraperitoneal), Mebunat®, Orion-Farmos, Turku, Finland) and intubated through an incision in the neck. Lungs were then ventilated using a pressure-controlled ventilator (Baby-Bird, Bird Corp, Palm Springs, CA) for three hours (rate 30/min, peak inspiratory pressure 15 cmH2O, positive end-expiratory pressure 1–2 cmH2O, FiO2 0.70). The experiments were approved by the Committee of Animal Care in Research of the University of Turku.
Meconium preparation.
Human meconium was collected from the first stools of healthy full-term neonates. The samples were frozen, later pooled, lyophilised and irradiated for sterility. Before instillation, meconium was diluted with sterile saline to a concentration of 65 mg/mL (particulate meconium), clinically corresponding to thick meconium in amniotic fluid (3). To separate supernatant, this particulate solution of meconium was spun down at 5,000 rpm for 20 min. in room air. Endotoxin in meconium was quantified using the Limulus Amebocyte Lysate Assay (LAL Kinetic-QCL, 50-650U; BioWhittaker/Cambrex Bio Science, Walkersville, M.D., USA). The meconium batch was sterile in culture and its endotoxin content was 24 ng/mg of meconium.
Study protocols: Protocol I: The effects of PLA2-I in meconium.
Lung injury was produced in 18 rats by intra-tracheal instillation (3 mL/kg) of human particulate meconium (65 mg/mL) (Group MP, n = 8) or supernatant of meconium (Group MS, n = 10). To study the pulmonary effects of PLA2-I in meconium, two further groups of rats were instilled either with the same amount of particulate meconium after extraction of PLA2-I by immunoadsorption (Group MP/E, n = 10) or supernatant of meconium after extraction of PLA2-I (Group MS/E, n = 10). The mean concentration of PLA2-I in particulate human meconium before extraction was 2280 μg/L (341, SD), and after extraction 1286 μg/L (462), corresponding to a mean decrease of 44% (19%). Similarly, the mean concentration of PLA2-I in meconium supernatant before extraction was 2348 μg/L (1088), and 672 μg/L (591) after extraction, corresponding to a mean decrease of 71% (9%). Control animals received a bolus of sterile saline intra-tracheally (n = 7) (Control). To estimate the baseline PLA2 activity and PLA2-II enzyme concentration in rat lungs, five additional animals were anesthetized and the lungs studied without any insult or ventilation. All the instilled lungs were ventilated with 70% oxygen for 3 h. At the end of the experiments, thoracotomy was made and heparin was injected into the left ventricle to prevent blood from clotting. Subsequently, the lungs were perfused with 10 mL of sterile saline through a pulmonary artery catheter. The lungs were finally isolated and the lobes were separated for biochemical and histologic analysis and measurement of wet/dry ratio. The upper right lobe was deep frozen in liquid nitrogen and then put to the –70°C freezer.
Study protocols: Protocol II: The effects of meconium-derived or bovine group I PLA2.
To further study the pulmonary effects of PLA2-I, the enzyme was purified from samples of human meconium. Due to technical difficulties, the concentration of PLA2-I after purification from meconium remained on an average level of 840 μg/L (89). Three mL/kg of this solution was then instilled into the lungs of six rats (Group hPLA2). In comparison, two other groups received a similar bolus of bovine PLA2-I (Sigma Chemical Co. Chemicals). One group was given bovine PLA2-I intra-tracheally at a concentration of 4 mg/mL, corresponding to the catalytic activity found in the particulate (65 mg/mL) meconium (n = 5) (Group bPLA2/4). Catalytic activity of bovine PLA2-I [1 mg/mL] was 1804 U/L (868). The other group received an intrapulmonary bolus of double concentration, 8 mg/mL, of bovine PLA2-I (n = 5) (Group bPLA2/8). The rats were similarly ventilated with 70% oxygen for 3 h and the lungs were studied as above at the end of the study.
PLA2-I immunoadsorption.
Immunoadsorbtion was used to reduce the PLA2-I concentration in meconium. Particulate meconium was diluted in sterile saline in three steps to get the final concentration of 65 mg/mL. After every step diluted meconium was centrifuged [19 500 rpm (47 000 G)] for 30 min, and the supernatant was collected. Supernatant was then used for immunoadsorbtion in polystyrene tubes coated with rabbit anti-human PLA2-I antibody (11) (25 μg/mL). This antibody is highly specific to human PLA2-I (12), which is characterized and proved, e.g., in the immunoassay use (13). Incubation (45 min/tube) of the supernatant in the antibody-coated plastic tubes (1 mL/tube) was repeated 16 times and the solid (dry) phase of the meconium was finally diluted in the supernatant for measurement of the PLA2-I concentration.
PLA2-I purification from meconium.
An immunoaffinity column was prepared for immunoadsorbtion of human PLA2-I from the meconium. Briefly, a 5 mL sized HiTrap NHS-activated Sepharose column was prepared by immobilizing 13 mg of HiTrap protein A purified from human PLA2-I –immunized rabbit antiserum as instructed by the manufacturer of both columns (Amersham Pharmacia Biotech AB, Uppsala Sweden).
Clarified supernatant of meconium was applied into the column that was equilibrated with 0.05 M sodium phosphate buffer pH 7.5. The column was washed with the same buffer and the attached PLA2-I was released with 0.05 M glycine-hydrochloride buffer pH 2.7 containing 0.5 M NaCl. The purification was monitored with an UV-detector, 280 nm. The collected PLA2-I fraction was instantly neutralized by dialyzing against sodium phosphate buffer pH 7.5 overnight at + 4°C. For the animal experiments the purified PLA2-I was concentrated and the buffer changed to sterile saline solution with centrifugal filter device (Ultrafree-15, Millipore Bedford, MA).
PLA2 concentrations and catalytic activity.
The catalytic activity of PLA2 and concentrations of human group I PLA2 and rat group II PLA2 were measured using the same protocols as described earlier (3,11,14). Briefly, frozen lung tissues were homogenized, centrifuged for 20 min with 1000 G, and the supernatant was separated and used for PLA2 catalytic activity and concentration assays. In the activity measurement the substrate was prepared by mixing unlabelled 1,2-dipalmitoylphosphatidylcholine (Sigma Chemical Co., ST. Louis, MO) with 1-palmitoyl-2-[14C]-arachidonoylphosphatidylethanolamide (DuPont, Boston, MA) in a ratio of 6 mM/1.325 μM (250 nCi), dissolved in a mixture of chloroform and methanol (2:1), dried under a flow of nitrogen, and redissolved in 10 mL 0.1 M glycine buffer (pH 8.1). 10 μL samples of lung tissue supernatant were incubated with 100 μL of substrate buffer for three hours at 40°C. The reaction was stopped by adding 100 μL of Dole's reagent. Released [14C]-arachidonic acid was separated by SiO2/water/heptane phase extraction, and detected by a liquid scintillation spectrometer (Wallac, Turku, Finland).
The concentrations of PLA2-I and PLA2-II were measured by time-resolved fluoroimmunoassays. PLA2-I concentrations were measured in the used solutions of each animal group before experiments. After experiments, the human PLA2-I and rat PLA2-II concentrations were measured in the supernatant of the homogenized rat lung tissue. PLA2-I immunoassay uses MAb-coated microtitre plates and polyclonal (rabbit) antibody as tracer. Both antibodies were raised against purified human pancreatic group I PLA2. PLA2-II immunoassay utilizes a polyclonal antibody, raised in rabbits against rat recombinant PLA2-IIA, immobilized on the microtitre plate and also used as a detecting tracer antibody. Fluorescence was measured with an Arcus fluorometer (Wallac, Turku, Finland). Purified human pancreatic PLA2 and rat recombinant PLA2 were used as standards in the measurements. We have earlier shown that there is no cross-reaction between the human and rat group I PLA2 (3).
Histologic examinations.
Paraffin sections of the left lower lung lobe were stained with hematoxylin and eosin for light microscope analysis and assessed by a pathologist blinded to the grouping of rats. A score from 0 to 4 was assigned for three different characteristics: 1) the extent of leucocyte infiltration; 2) the amount of intra-alveolar leukocytes; and 3) the amount of exudative debris. The calculated total injury score means the sum of these scores (3).
In situ detection of TUNEL-positive cells.
Terminal deoxynucleodityl transferase-mediated nick end-labeling (TUNEL) for the detection of apoptotic cells was performed in paraffin wax sections, as described earlier (3,4,14). Lymphocytes undergoing apoptosis in the lymph nodes served as a positive control. TUNEL-positive cells were counted in lung sections stained with the antidigoxygenin antibody. A distinct color reaction within the cells was regarded to represent apoptotic DNA fragmentation. The results are expressed as the number of positive cells per mm2 of tissue section area in at least ten fields of view of a ×10 objective lens. The in situ detection of free DNA 3′: -ends is a well established method in the detection of apoptotic cellular changes and has been validated by simultaneous electrophoretic DNA analysis in pancreatic tissue (14).
Statistical analysis.
One-way analysis of variance (ANOVA) was used to compare the data in different groups. If the overall ANOVA was significant, comparisons between the groups were made using the Tukey's post hoc test. For comparison of nonparametric data, Kruskal-Wallis one-way ANOVA was used, followed by the Dunn's post hoc test. Differences between two groups were evaluated by unpaired 2-tailed t test. A level of p < 0.05 was considered statistically significant. The results are expressed as mean (SD).
RESULTS
The effects of PLA2-I in meconium.
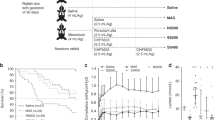
The PLA2 catalytic activity in the unventilated rat lungs was lower than in the saline-instilled control lungs [77 (16, SD) versus. 166 (53) mU/g lung tissue, p < 0.01], whereas pulmonary tissue PLA2-II concentrations were at the same level [160 (47) versus 126 (65) ng/g lung tissue, respectively]. Administration of particulate meconium (both before and after PLA2-I extraction) resulted in markedly elevated lung tissue PLA2 catalytic activity and PLA2-I concentrations, whereas insufflation of meconium supernatant (with or without PLA2-I extraction) had no significant effect on these parameters, when compared with saline controls (Fig. 1). On the other hand, the concentrations of PLA2-II in the lung tissue were not affected in any of the study groups (Fig. 1).
Tissue phospholipase A2 (PLA2) activity (mU/g lung tissue), and group I PLA2 (PLA2-I) and group II PLA2 (PLA2-II) concentrations (ng/g lung tissue) in rat lungs at 3 h after intra-pulmonary instillation of particulate meconium (MP, n = 8), particulate meconium after PLA2-I extraction (MP/E, n = 10), supernatant of meconium (MS, n = 10), meconium supernatant after PLA2-I extraction (MS/E, n = 10) and saline (control, n = 7). Mean(SD). ** p < 0.01 vs. saline.
The lung tissue wet/dry–ratio was not elevated from the control level after instillation of meconium, except after insufflation of meconium supernatant with PLA2 extraction (Table 1). In contrast, the pulmonary histologic injury scores in all meconium-insulted groups were increased, with the highest score, mainly due to elevated intrapulmonary leukocyte accumulation, after insufflation of particulate, non-manipulated meconium (Table 1). The lung injury score had further a direct correlation with pulmonary PLA2-I content (r = 0.426, p < 0.01), but not with PLA2 activity or PLA2-II concentrations in the lung tissue. On the other hand, pulmonary PLA2-I, unlike PLA2-II, concentration correlated significantly with the lung PLA2 activity (r = 0.826, p < 0.0001), whereas no correlations between these enzyme concentrations and lung tissue wet/dry ratio were found. The amount of TUNEL-positive cells in the lungs did not differ between the groups (Table 1).
The effects of meconium-derived or bovine PLA2-I. Instillation of meconium-derived human pancreatic PLA2, at a concentration of a third of that in particulate meconium, resulted in lung tissue-catalytic PLA2 activity, and concentrations of PLA2-I and PLA2-II that were on the control levels (Table 2). Still, the lung tissue wet/dry ratio and injury score, but not the count of TUNEL-positive cells, were significantly higher than in the controls (Table 2). Actually, the wet/dry ratio was similar than after intra-tracheal meconium instillation, but the injury score was significantly (p < 0.01) lower than observed in the meconium-contaminated lung tissue.
Insufflation of bovine PLA2-I with the activity corresponding to that in particulate meconium increased the lung tissue enzyme activity from the level observed in controls, but had no effect on the pulmonary PLA2-II concentration, lung tissue wet/dry ratio and injury score or number of TUNEL-positive cells (Table 2). Pulmonary instillation of a double amount of bovine PLA2-I resulted in even higher lung enzyme activity and wet/dry ratio, but again had no effect on the PLA2-II concentration, tissue injury score or number of TUNEL-positive cells (Table 2). In fact, the higher amount of intra-tracheal bovine PLA2-I resulted in a higher (p < 0.02) lung tissue wet/dry ratio than what was observed after insufflation of particulate meconium or meconium supernatant. Human PLA2-I concentrations were not measured in these lungs.
DISCUSSION
Our present data suggest that pancreatic PLA2 within aspirated meconium is related to the intense lung inflammatory, but not apoptotic, reaction in the development of the meconium aspiration-induced tissue injury (1–4). It is further evident that lung PLA2-II production is not stimulated after meconium contamination. Based on the present data, we cannot however totally exclude the influence of some other components of meconium on the present pulmonary findings. Especially the fact that PLA2-I seems to be attached very firmly to the solid particles of meconium complicated its extraction procedure and hence also the interpretation of the results. Moreover, despite of reduction of pancreatic PLA2 from particulate meconium (44%) and its supernatant (71%), enzyme activities and concentrations of PLA2-I were similar before and after manipulation in the meconium-contaminated lungs. This may be explained, at least in part, by absorption of the introduced enzyme into the pulmonary circulation. We have in fact previously observed elevated human PLA2-I concentrations in plasma during the first hours after intra-tracheal meconium administration in newborn piglets (P. Kääpä, unpublished observations). On the other hand, the pulmonary PLA2-I content correlated directly with the lung injury score. Although intra-tracheal endotoxin may also contribute to the pulmonary reactions, endotoxin content of meconium was in low nanomolar range, which remains well below the amount required for prompt induction of significant pulmonary neutrophil influx. Alike, even high amounts of intra-tracheal endotoxin do not affect pulmonary PLA2-I expression (15). Despite the experimental lung injuries in the present work were induced in fully developed lungs and the results therefore cannot be directly applied to neonatal pulmonary changes, the airway alterations in newborns tend to be more severe than those in adult lungs in response to a pulmonary insult (16). Thus, based on our present data, it may be suggested that meconium aspiration-induced lung damage is exacerbated by the high amount of pancreatic PLA2 in meconium.
Corroborating our present results, several lines of clinical and experimental evidence implicate that excess pulmonary PLA2 activity, through generation of pro-inflammatory lysophospholipids and eicosanoids, may contribute to the progression of various inflammatory lung disorders (5–8). Accordingly, lung PLA2 catalytic activity is significantly increased in adults with acute respiratory distress syndrome and after experimental pulmonary insults correlating with the severity of the pulmonary failure (15,17–19). High PLA2 activity in inflammatory lung injuries is commonly connected with increased release of secretory PLA2-II originating from macrophages and platelets (5,9,15). The present data in contrast indicate that meconium aspiration may provoke inflammatory lung damage through pulmonary introduction of high amount of PLA2-I with no influence on pulmonary PLA2-II production. Our earlier data accordingly indicate that high PLA2 catalytic activity found in human meconium is mainly (in > 90%) due to high concentration of human PLA2-I (3). Although some experimental studies propose that PLA2-I may induce, receptor-mediated, local PLA2-II expression (20), this was not obvious at least in the early phase of meconium-induced lung injury. The reason for the apparently lacking local production of PLA2-II and interaction between group I and II enzymes in our lung injury model remains unclear, but may be related to the short study period or varying catalytic or receptor-mediated interaction between these enzymes in the insulted lungs (17,20,21). On the other hand, we cannot exclude the involvement of other phospholipases within aspirated meconium (22) or products of pulmonary cytosolic PLA2 activation in the development of lung injury in our model (23).
PLA2-I, earlier considered as a digestive enzyme secreted from the pancreas, is today known to be expressed and to modulate cellular function in a variety of tissues, including rat and human lungs (24,25). This enzyme is further able to stimulate cytokine chemokine and eicosanoid production from pulmonary cells involved in inflammatory responses and it may also directly stimulate neutrophil secretory function (26–28). These effects are shown to be exerted by mechanisms that are independent of the catalytic enzyme activity and are mediated by the interaction of secretory PLA2s with specific membrane receptors (27,28). Mammalian PLA2-I unlike group II PLA2 enzyme, is further able to inactivate pulmonary surfactant concentration-dependently through hydrolysis of phosphatidylcholine (29). Experimental investigations have additionally shown that exogenously administered PLA2-I may induce most likely through enhanced pulmonary thromboxane A2 synthesis, receptor-mediated contractile responses in the airways (30). Similarly increased pulmonary thromboxane production may contribute to the development of vascular hypertension and edema formation in the meconium-insulted lungs (1,31). The observed challenge of the meconium-aspirated lungs with high exogenous activity of PLA2-I may thus participate in propagation of the pulmonary ventilation disturbances hypertensive response and inflammation with ensuing respiratory failure in newborns (1–3,22,26). The variation of PLA2-I content and enzyme activity in particulate meconium and its supernatant may further explain the observed differences in the lung inflammatory reactions after aspiration.
Due to technical difficulties in the extraction of PLA2-I from human meconium, the amount of this enzyme used for intra-tracheal instillation studies remained low, but was still able to induce significant edema formation and some histologic injury in the exposed lungs. In contrast, bovine PLA2-I, even though given at a concentration corresponding to a similar or even higher catalytic PLA2 activity than found in particulate meconium did not cause any histologic injury, but induced, in a concentration-dependent manner, lung edema formation. These data, again, strengthen the view that human PLA2-I, either in soluble form or within meconium, is able to promote not only edema formation, but also neutrophil influx in the insulted lungs. The reason for the different responses to human and bovine PLA2-I remains unclear, but may be related to varying histamine or eicosanoid release, connected to pancreatic PLA2-induced permeability increase, or divergent chemokine and cytokine production in the lungs (27,30,32,33). In fact, earlier investigations have shown that mammalian pancreatic PLA2s, despite having highly homologous structures, have different activity toward various lipid substrates (34).
In conclusion, our data indicate that intrapulmonary aspirated meconium challenges the lungs with high human pancreatic PLA2 concentration and activity and may thereby contribute to the pulmonary inflammatory, but not apoptotic damage. Especially aspiration of thick particulate meconium through its high concentration of PLA2-I may have the most deleterious pulmonary effects. These findings may be amenable to development of new modes of more specific therapeutic approaches.
Abbreviations
- MAS:
-
meconium aspiration syndrome
- PLA2:
-
phospholipase A2
- PLA2-I:
-
group I phospholipase A2 (pancreatic)
- PLA2-II:
-
group II phospholipase A2 (synovial)
- TUNEL:
-
terminal deoxynucleotidyl transferase-mediated nick end-labeling
References
Wiswell TE 2003 Meconium staining and the meconium aspiration syndrome. In: Stevenson D, Benitz, WE, Sunshine, P (ed) Fetal and neonatal brain injury. Mechanisms, Management and the Risks of Practice. Cambridge University Press, Cambridge, MA, pp 612–635
Davey AM, Becker JD, Davis JM 1993 Meconium asiration syndrome: physiological and inflammatory changes in a newborn piglet model. Pediatr Pulmonol 16: 101–108
Holopainen R, Aho H, Laine J, Peuravuori H, Soukka H, Kääpä P 1999 Human meconium has high phospholipase A2 activity and induces cellular injury and apoptosis in piglet lungs. Pediatr Res 46: 626–632
Lukkarinen H, Laine J, Lehtonen J, Zagariya A, Vidyasagar D, Aho H, Kääpä P 2004 Angiotensin II receptor blockade inhibits pneumocyte apoptosis in experimental meconium aspiration. Pediatr Res 55: 326–333
Dennis EA 1994 Diversity of group types, regulation, and function of phospholipase A2 . J Biol Chem 269: 13057–13060
Arbibe L, Koumanov K, Vial D, Rougeot C, Faure G, Havet N, Longacre S, Vargaftig BB, Bereziat G, Voelker DR, Wolf C, Touqui L 1998 Generation of lyso-phospholipids from surfactant in acute lung injury is mediated by type-II phospholipase A2 and inhibited by a direct surfactant protein A-phospholipase A2 protein interaction. J Clin Invest 102: 1152–1160
Liu LY, Sun B, Tian Y, Lu BZ, Wang J 1993 Changes of pulmonary glucocorticoid receptor and phospholipase A2 in sheep with acute lung injury after high dose endotoxin infusion. Am Rev Respir Dis 148: 878–881
Niewoehner DE, Rice K, Duane P, Sinha AA, Gebhard R, Wangensteen D 1989 Induction of alveolar epithelial injury by phospholipase A2 . J Appl Physiol 66: 261–267
Holm BA, Keicher L, Liu MY, Sokolowski J, Enhorning G 1991 Inhibition of pulmonary surfactant function by phospholipases. J Appl Physiol 71: 317–321
Vadas P, Pruzanski W 1986 Role of secretory phospholipases A2 in the pathobiology of disease. Lab Invest 55: 391–404
Nevalainen TJ, Kortesuo PT, Rintala E, Märki F 1992 Immunochemical detection of group I and group II phospholipase A2 in human serum. Clin Chem 38: 1824–1829
Eskola JU, Nevalainen TJ, Aho HJ 1983 Purification and characterization of human pancreatic phospholipase A2. Clin Chem 29: 1772–1776
Eskola JU, Nevalainen TJ, Lövgren TN 1983 Time-resolved fluoroimmunoassay of human pancreatic phospholipase A2. Clin Chem 29: 1777–1780
Laine VJ, Nyman KM, Peuravuori HJ, Henriksen K, Parvinen M, Nevalainen TJ 1996 Lipopolysaccharide induced apoptosis of rat pancreatic acinar cells. Gut 38: 747–752
Arbibe L, Vial D, Rosisnski-Chupin I, Havet N, Huerre M, Vargaftig BB, Touqui L 1998 Endotoxin induces expression of type-II phospholipase A2 in macrophages during acute lung injury in guinea pigs. Involvement of TNF-α in lipopolysaccharide-induced type-II phospholipase A2 synthesis. J Immunol 159: 391–400
Coalson JJ, Kuehl TJ, Prihoda TJ, deLemos RA 1988 Diffuse alveolar damage in the evolution of bronchopulmonary dysplasia in the baboon. Pediatr Res 24: 357–366
Touqui L, Arbibe L 1999 A role for phospholipase A2 in ARDS pathogenesis. Mol Med Today 5: 244–249
Vadas P 1984 Elevated plasma phospholipase A2 levels: correlation with the hemodynamic and pulmonary changes in gram-negative septic shock. J Lab Clin Med 104: 873–881
Terao Y, Haseba S, Nakamura H, Morooka H, Shibata O, Sumikawa K 2001 Activation of alveolar phospholipase A2 after hydrochloric acid aspiration in rats. J Crit Care 16: 42–6
Kishino J, Ohara O, Nomura K, Kramer RM, Arita H 1994 Pancreatic-type phospholipase A2 induces group II phospholipase A2 expression and prostaglandin biosynthesis in rat mesangial cells. J Biol Chem 269: 5092–5098
Valentin E, Lambeau G 2000 Increasing molecular diversity of secreted phospholipases A(2) and their receptors and binding proteins. Biochim Biophys Acta 1488: 59–70
Schrama AJ, de Beaufort AJ, Sukul YR, Jansen SM, Poorthuis BJ, Berger HM 2001 Phospholipase A2 is present in meconium and inhibits the activity of pulmonary surfactant: an in vitro study. Acta Pediatr 90: 412–416
Nagase T, Uozumi N, Ishii S, Kume K, Izumi T, Ouchi Y, Shimizu T 2000 Acute lung injury by sepsis and acid aspiration: a key role for cytosolic phospholipase A2. Nat Immunol 1: 42–46
Sakata T, Nakamura E, Tsuruta Y, Tamaki M, Teraoka H, Tojo H, Ono T, Okamoto M 1989 Presence of pancreatic-type phospholipase A2 mRNA in rat gastric mucosa and lung. Biochim Biophys Acta 1007: 124–126
Seilhamer JJ, Randall TL, Yamanaka M, Johnson LK 1986 Pancreatic phospholipase A2: isolation of the human gene and cDNAs from porcine pancreas and human lung. DNA 5: 519–527
Pruzanski W, Vadas P 1991 Phospholipase A2 -a mediator between proximal and distal effectors of inflammation. Immunol Today 12: 143–146
Granata F, Petraroli A, Boilard E, Bezzine S, Bollinger J, DelVecchio L, Gelb MH, Lambeau G, Marone G, Triggiani M 2005 Activation of cytokine production by secreted phospholipase A2 in human lung macrophages expressing the M-type receptor. J Immunol 174: 464–474
Zallen G, Moore EE, Johnson JL, Tamura DY, Barkin M, Stockinger H, Silliman CC 1998 New mechanisms by which secretory phospholipase A2 stimulates neutrophils to provoke the release of cytotoxic agents. Arch Surg 133: 1229–1233
Hite RD, Seeds MC, Jacinto RB, Balasubramanian R, Waite M, Bass D 1998 Hydrolysis of surfactant-associated phosphatidylcholine by mammalian secretory phospholipases A2 . Am J Physiol 275: L740–747
Sommers CD, Bobbitt JL, Bemis KG, Snyder DW 1992 Porcine pancreatic phospholipase A2-induced contractions of guinea pig lung pleural strips. Eur J Pharmacol 216: 87–96
Soukka H, Viinikka L, Kääpä P 1998 Involvement of thromboxane A2 and prostacyclin in the early pulmonary hypertension after porcine meconium aspiration. Pediatr Res 44: 838–842
Beck GCh, Yard BA, Schulte J, Haak M, van Ackern K, van der Woude FJ, Kaszkin M 2003 Secreted phospholipases A2 induce the expression of chemokines in microvascular endothelium. Biochem Biophys Res Comm 300: 731–737
Lloret S, Moreno JJ 1993 Oedema formation and degranulation of mast cells by phospholipase A2 purified from porcine pancreas and snake venoms. Toxicon 31: 949–956
Han SK, Lee BI, Cho W 1997 Bacterial expression and characterization of human pancreatic phospholipase A2 . Biochim Biophys Acta 1346: 185–192
Author information
Authors and Affiliations
Corresponding author
Additional information
This study was supported by the Foundation for Pediatric Research, the Sigrid Juselius Foundation, and the Paulo Foundation, Finland
Rights and permissions
About this article
Cite this article
Sippola, T., Aho, H., Peuravuori, H. et al. Pancreatic Phospholipase A2 Contributes to Lung Injury in Experimental Meconium Aspiration. Pediatr Res 59, 641–645 (2006). https://doi.org/10.1203/01.pdr.0000214685.31232.6a
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/01.pdr.0000214685.31232.6a
This article is cited by
-
Secretory phospholipase A2 pathway in various types of lung injury in neonates and infants: a multicentre translational study
BMC Pediatrics (2011)
-
Role of distinct phospholipases A2 and their modulators in meconium aspiration syndrome in human neonates
Intensive Care Medicine (2011)
-
Bile acids cause secretory phospholipase A2 activity enhancement, revertible by exogenous surfactant administration
Intensive Care Medicine (2009)
-
Phospholipase A2 in meconium-induced lung injury
Journal of Perinatology (2008)