Abstract
Clinically, irreversible pulpitis is treated by the complete removal of pulp tissue followed by replacement with artificial materials. There is considered to be a high potential for autologous transplantation of human dental pulp stem cells (DPSCs) in endodontic treatment. The usefulness of DPSCs isolated from healthy teeth is limited. However, DPSCs isolated from diseased teeth with irreversible pulpitis (IP-DPSCs) are considered to be suitable for dentin/pulp regeneration. In this study, we examined the stem cell potency of IP-DPSCs. In comparison with healthy DPSCs, IP-DPSCs expressed lower colony-forming capacity, population-doubling rate, cell proliferation, multipotency, in vivo dentin regeneration and immunosuppressive activity, suggesting that intact IP-DPSCs may be inadequate for dentin/pulp regeneration. Therefore, we attempted to improve the impaired in vivo dentin regeneration and in vitro immunosuppressive functions of IP-DPSCs to enable dentin/pulp regeneration. Interferon gamma (IFN-γ) treatment enhanced in vivo dentin regeneration and in vitro T cell suppression of IP-DPSCs, whereas treatment with tumor necrosis factor alpha did not. Therefore, these findings suggest that IFN-γ may be a feasible modulator to improve the functions of impaired IP-DPSCs, suggesting that autologous transplantation of IFN-γ-accelerated IP-DPSCs might be a promising new therapeutic strategy for dentin/pulp tissue engineering in future endodontic treatment.
Similar content being viewed by others
Introduction
The dentin/pulp complex does not self-remodel/regenerate, but forms reparative dentin in response to diverse tissue injury1,2. Tumor necrosis factor alpha (TNF-α) and interferon gamma (IFN-γ) are involved in the pathogenesis of dental pulpitis3,4, which can be clinically categorized as either reversible or irreversible pulpitis5. In irreversible pulpitis, the injured dental pulp tissue does not recover once the pathogen(s) is removed completely. Therefore, clinically, pulp tissue with irreversible pulpitis is completely removed and replaced by artificial materials such as cements and gutta percha. Teeth that receive endodontic treatment lose their physiological bioactivity, including strength, sensitivity and immune defense and many ultimately require extraction because of fractures or caries. Therefore, regeneration of the bioactive dentin/pulp complex is considered an ideal endodontic therapy for pulpectomized teeth.
Dental pulp stem cells (DPSCs) have been identified in the healthy dental pulp tissue of human impacted third molars6 and are regarded as a subpopulation of mesenchymal stem cells (MSCs). Recent investigation of DPSCs has discovered various stem cell properties, including self-renewal, multipotency into odontoblasts, chondrocytes and adipocytes, an in vivo regenerative capacity of the dentin/pulp complex, heterogeneity and immunomodulatory functions6,7,8,9. Based on these unique properties of DPSCs, healthy dental pulp tissue has been considered a promising resource for pulp regeneration10.
Patient-derived pulpectomized pulp tissue is also considered to be a feasible and ideal source for DPSC-based pulp regeneration because of its dentinogenic capacity11,12. Although recent studies have attempted to isolate and characterize stem cells from inflamed dental pulp tissue that is clinically diagnosed with irreversible pulpitis11,12,13,14, many properties of pulpitis-derived DPSCs remain unclear. Recently, pulpitis-derived DPSCs have been shown to exhibit less efficacy for dental pulp regeneration and T cell immunosuppression13,14. However, a practical approach to improving the deficient functions of pulpitis-derived DPSCs has not been revealed.
In this study, to clarify the properties of pulpitis-derived DPSCs, we isolated stem cells from human dental pulp tissue with irreversible pulpitis, referred to as IP-DPSCs, using colony-forming unit-fibroblasts (CFU-Fs)15 and determined a variety of MSC properties including clonogenicity, self-renewal capacity, multidifferentiation ability into odontoblasts, adipocytes, endothelial cells and neural cells, in vivo dentin regenerative capacity, heterogeneity and immunomodulatory functions. Furthermore, we attempted to develop an ex vivo approach to improve IP-DPSCs by treatment with TNF-α and IFN-γ.
Results
Stemness of IP-DPSCs
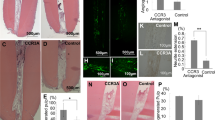
Histological analysis demonstrated that inflamed dental pulp tissue freshly obtained from teeth that were clinically diagnosed with irreversible pulpitis consisted of dense connective tissue supplied with blood vessels and nerve fibers (Fig. 1a). An early MSC marker, STRO-1, was detected on cells in the inflamed pulp tissue (Fig. 1b), suggesting that inflamed dental pulp tissue may contain MSCs, as reported in healthy human dental pulp tissue16.
Characterization of stem cells isolated from inflamed human dental pulp.
(a) Histochemical images of irreversible pulpitis tissue. H&E staining. BV: blood vessel. Arrowheads: nerve fibers. (b) Immunohistochemical localization of STRO-1-positive cells (arrows) in irreversible pulpitis tissue. Hematoxylin staining. (c–e) Capability of CFU-Fs of IP-DPSCs. Toluidine blue staining. Representative image of CFU-Fs on a culture dish (c left) and fibroblastic colony-forming cells (c right). Differences in colony size and density (d). Colony-forming efficiency (CFE) per 1 × 106 cells (e). (f) Immunophenotype assay by flow cytometric analysis. White area: histograms stained with control antibody; grey area: histograms stained with antibodies against cell surface antigens. Percentiles indicate the average of each antigen. PE: phycoerythrin. (g) Gene expression for embryonic stem and neural crest cell markers. Semi-quantitative RT-PCR assay. OCT4: octamer 4, GAPDH: glyceraldehyde 3-phosphate dehydrogenase. (h) Population-doubling assay. (i,j) Cell proliferation analysis by BrdU incorporation assay. Representative images of BrdU-positive cells. Hematoxylin staining (i). Percentiles of BrdU-positive nuclei to the total nuclear cells (j). (k) Telomerase activity test. TRAP-qPCR assay. HEK: Human Embryonic Kidney 293 cells, H.I. heat-inactivated treatment. (e,f,h,j,k): n = 3 per group. **P < 0.01 and ***P < 0.005. Graph bars show the means ± s.e.m.
DPSCs isolated from clinically healthy dental pulp tissue, referred to as healthy DPSCs, can be shared with MSC properties, including clonogenicity, self-renewal, MSC surface antigens, multidifferentiation, in vivo dentin regeneration and immunosuppression6,7,9. However, the properties of DPSCs isolated from irreversible pulpitis tissue, IP-DPSCs, have not yet been fully revealed11,12,14. To closely examine the properties of IP-DPSCs, at the beginning of this study, cells were isolated from fresh irreversible pulpitis tissue with a standard CFU-F method15. Single cells were independently attached to the plastic culture dishes and then formed cell clusters and CFU-Fs (Fig. 1c) with different sizes and varied density (Fig. 1d), but the IP-DPSCs showed significantly lower colony-forming efficacy when compared with healthy DPSCs (Fig. 1e). Flow cytometric analysis demonstrated that IP-DPSCs were positive to STRO-1, CD146, CD105, CD73 and CD90, but negative to hematopoietic cell markers CD34, CD45 and CD14, as seen in healthy DPSCs (Fig. 1f). Reverse transcription polymerase chain reaction (RT-PCR) demonstrated that IP-DPSCs expressed genes for embryonic stem cells, NANOG and octamer 4 and for neural crest cells, NESTIN, NOTCH1 and CD271 (Fig. 1g). IP-DPSCs expressed a markedly reduced CD271 when compared with healthy DPSCs. By population-doubling and bromodeoxyuridine (BrdU) assays, IP-DPSCs showed a significantly suppressed proliferation capacity when compared with healthy DPSCs (Fig. 1h–j). IP-DPSCs expressed lower telomerase activity than healthy DPSCs (Fig. 1k). Therefore, these data suggested that IP-DPSCs retained stemness as MSCs, but expressed different essential characteristics when compared with healthy DPSCs.
Multipotency of IP-DPSCs
When IP-DPSCs were cultured under a dentinogenic condition for 4 weeks, they were capable of forming calcium-deposited nodules positive to Alizarin Red staining (Fig. 2a,b). RT-PCR and quantitative RT-PCR (RT-qPCR) demonstrated that IP-DPSCs at 1 week after the induction expressed odontoblast-specific genes including runt-related gene 2 (Runx2), alkaline phosphatase (ALP), osteocalcin (OCN) and dentin sialophosphoprotein (DSPP) (Fig. 2c, Supplementary Figure 1a) and showed ALP activity (data not shown). IP-DPSCs were then cultured under an adipogenic condition for 6 weeks. Oil Red O staining assay demonstrated lipid accumulation in IP-DPSCs (Fig. 2d,e). RT-PCR and RT-qPCR confirmed the expression of adipocyte-specific genes, including lipoprotein lipase (LPL) and peroxisome proliferator-activated receptor γ2 (PPARγ2) (Fig. 2f, Supplementary Figure 1b). Immunofluorescence showed the expression of CD31 on IP-DPSCs that were cultured under an endothelial cell differentiation condition for seven days (Fig. 2g,h). We also treated IP-DPSCs under a neural cell induction condition for 7 days. Immunofluorescent analysis detected the expression of glial fibrillary acidic protein (GFAP), neurofilament M (NF-M) and tubulin βIII (βIII) on IP-DPSCs (Fig. 2i,j). IP-DPSCs also showed a reduced capability to differentiate into odontoblasts, adipocytes, endothelial cells and neural cells in comparison with healthy DPSCs (Fig. 2).
Multi-lineage differentiation capacity of IP-DPSCs.
(a–c) In vitro dentinogenic capacity (Den). Representative images of Alizarin Red staining (a). Percentiles of Alizarin Red-positive area to the total area (b). Ratio of odontoblast-specific genes to 18S rRNA (18S). RT-qPCR (c). (d–f) In vitro adipogenic capacity (Adipo). Representative images of Oil Red O staining (d). Measurement of Oil Red O content (e). Ratio of adipocyte-specific genes to 18S rRNA. RT-qPCR (e). (g,h) In vitro endothelial cell differentiation capacity (Endo). Immunofluorescent images of CD31-positive cells. DAPI staining (g). Percentiles of CD31-positive cells to total cells (h). (i,j) In vitro neural cell differentiation capacity (Neuro). Immunofluorescent images of neural marker-positive cells. DAPI staining (i). Percentiles of neural marker-positive cells to total cells (j). (b,c,e,f,h,j): n = 3 per group. Relative results to non-induced DPSC group. ***P < 0.005. Graph bars show the means ± s.e.m.
In vivo dentin/pulp complex regeneration of IP-DPSCs
IP-DPSCs were subcutaneously implanted with hydroxyapatite/tricalcium phosphate (HA/TCP) carriers under the dorsal skin of immunocompromised BALB/c nu/nu mice and left in place for 8 weeks (Supplementary Figure 2). Histological analysis showed that dentin/pulp complex-like structures were found in the implant tissues (Fig. 3a,b). This was similar to the findings of previous studies6,7. Immunofluorescence showed that human CD146- or DSPP-positive cells were arranged along the surface of the de novo mineralized matrix (Fig. 3c,d). In comparison, control transplants that received implantation of HA/TCP alone (without IP-DPSCs) did not show any mineralized tissue or human CD146 antibody-positive cells (data not shown). However, IP-DPSCs exhibited a reduced capacity for in vivo dentin/pulp complex regeneration in comparison with healthy DPSCs (Fig. 3e).
In vivo dentinogenic and self-renewal capacities and heterogeneity of IP-DPSCs.
(a–e) In vivo dentinogenic capacity assay. Representative images of transplants. H&E staining (a). Invert color images of H&E images (b). (c,d) Immunofluorescent localization of human CD146 (c) and DSPP (d). DAPI staining (c,d). (a–d): DSPP D: dentin, DP: dental pulp, HA: HA/TCP carrier. Percentiles of de novo dentin area to the total area. n = 3 per group. ***P < 0.005. Graph bars show the means ± s.e.m (e). (f–i) Self-renewal assay. Representative image of secondary transplants. H&E staining (f). Alinine blue collagen stainig (g). Immunohistochemical localization of human mitochondria (hMt)-positive cells (arrows). Hematoxylin staining (h). Immunofluorescent localization of DSPP. DAPI staining (i). (j–l) Heterogeneity. Single colony-derived cell assay. Population-doubling assay (j). Percentiles of BrdU-positive nuclei to total nuclear cells (k). Percentiles of Alizarin Red-positive area to the total area (l).
Self-renewal capability of IP-DPSCs
Sequential transplantation is the traditional and gold standard method to determine the self-renewal capacity of stem cells, including DPSCs6,7,8 (Supplementary Figure 2). IP-DPSCs were first transplanted with HA/TCP placed under the dorsal skin of immunocompromised mice. Cells were isolated from the primary transplants 8 weeks after the primary implantation and were then transplanted under the dorsal skin of different immunocompromised mice for a further 8 weeks. Histological investigation revealed that de novo structures in the secondary transplants expressed dentin/pulp complex-like structures in the primary transplants (Fig. 3f,g). Human mitochondria- or DSPP-positive cells were arranged on the de novo mineralized matrix in the secondary transplants (Fig. 3h,i). Population-doubling (Fig. 1h) and telomerase activity (Fig. 1k) in IP-DPSCs were associated with a self-renewal potential of stem cells17. Collectively, these results verified that IP-DPSCs have a self-renewal capacity.
Heterogeneity of IP-DPSCs
Heterogeneity in MSCs18,19 is one of the unique characteristics of healthy DPSCs7. To examine heterogeneity in IP-DPSCs, a total of 12 clonogenic single colonies were obtained from irreversible pulpitis tissue. Each single colony-derived cells expressed a different population-doubling score (Fig. 3j), cell proliferation capacity (Fig. 3k) and in vitro calcium deposition (Fig. 3l). These findings indicated that IP-DPSCs were a heterogeneous population.
Immunosuppressive function of IP-DPSCs
Healthy DPSCs exhibit T cell suppression9. Different numbers of γ-irradiated IP-DPSCs were directly co-cultured with human peripheral blood mononuclear cells (PBMNCs) stimulated with or without concanavalin A (ConA) (10 μg/ml) (Supplementary Figure 3a). Under a ConA-free condition, any number of IP-DPSCs did not affect the cell viability of PBMNCs (Fig. 4a). In comparison, under a ConA-stimulated condition, the PBMNC viability was suppressed depending on the cell number of IP-DPSCs (Fig. 4b). However, IP-DPSCs exhibited a reduced suppressive function in response to ConA-activated PBMNCs when compared with healthy DPSCs (Fig. 4b). Next, PBMSCs were co-cultured indirectly with IP-DPSCs or healthy DPSCs in a transwell culture system (Supplementary Figure 3). Under concanavalin A (ConA)-free condition, PBMNCs exhibited similar cell viability between direct and indirect co-culture systems (Supplementary Figure 4a). However, under a ConA-stimulated condition, the PBMNC viability did not showed any reduction depending on the cell number of IP-DPSCs in the traswell system (Supplementary Figure 4b).
Immunomodulatory effects of IP-DPSCs.
(a–c) Cell viability of human PBMNCs cultured with different ratios of DPSCs (SC) (SC/PBMNC = 0.01, 0.1 and 1) in the absence (a) or presence (b) of ConA. Co-culture of PBMNCs with DPSCs (SC/PBMNC = 1) under ConA stimulation with varied inhibitors and neutralized antibodies. Anti-IL10: anti-IL-10 antibody, Anti-TGFβ: anti-TGF-β antibody (c). (d) Expression of IDO in DPSCs. RT-qPCR assay. Ratio of IDO mRNA to 18S rRNA (18S). (e) Expression of L-kynurenine in culture supernatants of DPSCs. (f) Expression of IL-10 in culture supernatants of DPSCs. ELISA. (g–i) Cell death assay of DPSCs co-cultured with anti-CD3 antibody (Anti-CD3)-activated PBMNCs for 3 days (g) or 1 day (h,i). Anti-FasL: anti-FasL antibody. Toluidine blue staining (g). TUNEL assay (h,i). Representative images of TUNEL-positive cells (h). Percentiles of TUNEL-positive cells to total nuclear cells (i). (a–f,i): n = 3 per group. *P < 0.05, **P < 0.01 and ***P < 0.005. Graph bars show the means ± s.e.m. c: † < 0.05 vs. culture of PBMNCs with DPSCs in the absence of inhibitors and antibodies, #P < 0.05 vs. culture of PBMNCs with DPSCs in the absence of inhibitors and antibodies.
Direct contact of MSCs with T cells regulates immune tolerance through the Fas/Fas ligand (FasL) pathway20. On the other hand, many soluble factors secreted from MSCs participate in the immunosuppression of T cells21,22,23,24. In this study, the co-culture of ConA-stimulated PBMNCs with IP-DPSCs or healthy DPSCs was treated with 1-methyl-L-tryptophan (1-MT) (indoleamine 2,3-dioxygenase [IDO] inhibitor), N-nitro-L-arginine methyl ester (L-NAME) (nitric oxide synthase [NOS] inhibitor), indomethacin (cyclooxygenase [COX] inhibitor) and antibodies neutralized to IL-10 and transforming growth factor (TGF)-β (Supplementary Figure 5a). L-NAME, indomethacin and anti-TGF-β antibody did not recover the suppressed PBMNC viability when co-cultured with IP-DPSCs or healthy DPSCs (Fig. 4c). Treatment with 1-MT or anti-IL-10 antibody effectively enabled the IP-DPSC- or healthy DPSC-mediated inhibition of ConA-activated PBMNC viability (Fig. 4c). RT-qPCR analysis demonstrated that IP-DPSCs expressed lower IDO mRNA than healthy DPSCs when co-cultured with ConA-stimulated PBMNCs (Fig. 4d). The IP-DPSC co-culture produced less L-kynurenine as a result of IDO catabolism than the healthy DPSC co-culture (Fig. 4e). Enzyme-linked immunosorbent assay (ELISA) showed that the IP-DPSC co-culture group secreted lower human IL-10 in the conditioned medium (CM) of the co-cultures when compared with the healthy DPSC co-culture group (Fig. 4f). These results suggested that IP-DPSCs retained immunosuppressive function, but IP-DPSCs expressed reduced immunosuppression in comparison with healthy DPSCs.
Cell survival of IP-DPSCs
Activated T cells induce apoptosis of MSCs through the Fas/FasL pathway25,26. When IP-DPSCs and healthy DPSCs were co-cultured with anti-CD3 antibody-activated PBMNCs for 3 days (Supplementary Figure 5b), the IP-DPSCs were also induced into cell death (Fig. 4g). However, the treatment with anti-Fas antibody inhibited cell death of the IP-DPSCs (Fig. 4g). The activated PBMNCs induced terminal deoxynucleotidyl transferase dUTP nick end labeling (TUNEL)-positive cells in IP-DPSCs one day after the co-culture (Fig. 4h). The number of TUNEL-positive cells was greater in IP-DPSCs than in healthy DPSCs (Fig. 4i).
IFN-γ treatment improved dentinogenic dysfunction of IP-DPSCs
TNF-α and IFN-γ have been known to participate in the immunomodulatory and dentinogenic functions of healthy DPSCs9,13. Here, we investigated whether TNF-α or IFN-γ improve the in vitro or in vivo impaired dentin formation of IP-DPSCs. IFN-γ-stimulated IP-DPSCs were capable of forming a significant number of calcium-deposited nodules positive to Alizarin Red staining 4 weeks after the induction (Fig. 5a,b). IFN-γ-stimulated IP-DPSCs showed higher ALP activity (Fig. 5c) and markedly upregulated the expression of odontoblast/osteoblast-specific genes, including Runx2, ALP, osteocalcin and DSPP (Fig. 5d,e) 1 week after the induction. On the other hand, TNF-α-treated IP-DPSCs showed a markedly reduced dentinogenic capacity in vitro when compared with non-stimulated (intact) and IFN-γ-stimulated IP-DPSCs (Fig. 5a–e).
Effects of IFN-γ and TNF-α on dentinogenic capacity of IP-DPSCs.
(a–e) In vitro dentinogenic capacity. Representative images of Alizarin Red staining (a). Percentiles of Alizarin Red-positive area to the total area (b). ALP activity assay (c). Semi-quantitative RT-PCR for odontoblast-specific genes (d). Ratio of odontoblast-specific genes to 18S rRNA (18S). RT-qPCR Relative results to non-treated (intact) IP-DPSC group. (e). (f,g) In vivo dentinogenic capacity. Representative images of transplants. D: dentin, DP: dental pulp, HA: HA/TCP carrier (f). Percentiles of de novo dentin area to the total area (g). (h,i) In vivo dentin regeneration on human dentin. DP: dental pulp, ND: newly formed dentin. H&E staining (h). Immunohistochemical localization of hMt-positive cells (arrows). Hematoxylin staining (i). (b,c,e,g): n = 3 per group. *P < 0.05, **P < 0.01 and ***P < 0.005. Graph bars show the means ± s.e.m.
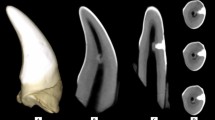
Next, TNF-α- or IFN-γ-pretreated IP-DPSCs were subcutaneously transplanted with HA/TCP into immunocompromised mice. Histological analysis demonstrated that IFN-γ-treatment enhanced the in vivo capability of dentin/pulp complex-like structures in the implant tissues (Fig. 5f,g). On the other hand, TNF-α-treatment reduced the in vivo capability (Fig. 5f,g). To further examine the effect of TNF-α and IFN-γ on IP-DPSC-mediated dentin/pulp regeneration, TNF-α and IFN-γ-treated IP-DPSCs were transplanted into human tooth root canals (Supplementary Figure 6). The IP-DPSCs formed a dentin-like structure directly on the surface of existing human tooth root dentin (Fig. 5h). IFN-γ-treatment abundantly deposited de novo dentin on a pre-existing human dentin surface, whereas TNF-α treatment did not (Fig. 5h). The newly formed dentin-like structure did not contain dentinal tubules and the charged cells arranged on its surface and embedded within it. Immunohistochemical assay with anti-human mitochondria antibody revealed that the lining and embedded cells were of human origin (Fig. 5i). These structural findings indicated that IP-DPSC-mediated dentin/pulp complex regeneration on human dentin may be controlled under a similar mechanism as reparative dentin formation occurring in the physiological human dentin/pulp system, suggesting that IFN-γ treatment improved the impaired dentinogenic function of IP-DPSCs.
IFN-γ treatment improved the impaired immunosuppressive efficacy of IP-DPSCs
We investigated the effect of TNF-α and IFN-γ treatment on STRO-1 expression. Flow cytometric analysis showed that TNF-α treatment significantly downregulated STRO-1 expression of IP-DPSCs, whereas IFN-γ treatment significantly upregulated STRO-1 expression, when compared with intact IP-DPSCs (Fig. 6a). BrdU incorporation assay demonstrated that TNF-α treatment markedly reduced the cell proliferation capacity of IP-DPSCs, whereas IFN-γ treatment significantly increased the IP-DPSC proliferation capacity, when compared with intact IP-DPSCs (Fig. 6b). Using the TUNEL method and under co-culture with anti-CD3 antibody-activated PBMNCs, TNF-α pretreatment markedly enhanced TUNEL-positive IP-DPSCs, whereas IFN-γ pretreatment suppressed TUNEL-positive IP-DPSCs, when compared with intact IP-DPSCs (Fig. 6c).
Effects of IFN-γ and TNF-α on STRO-1 expression, cell proliferation, cell death and immunomodulatory function of IP-DPSCs.
(a) Expression of STRO-1. Flow cytometry. (b) Percentiles of BrdU-positive nuclei to total nuclear cells. (c) Percentiles of TUNEL-positive cells to total nuclear cells. (d) Expression of IDO mRNA. RT-qPCR. Ratio of IDO to 18S rRNA (18S). (e) L-kynurenine in culture supernatants. (f) IL-10 in culture supernatants. ELISA. (g) Cell viability of human PBMNCs co-cultured with different ratios of IP-DPSCs (IP-DPSC/PBMNC = 0.01, 0.1 and 1). (h) Time-dependent expression of NF-κB. Western blotting. p-NF-κB: phosphorylated NF-κB. (i) Telomerase activity test. (a–g,i): n = 3 per group. *P < 0.05, **P < 0.01 and ***P < 0.005. Graph bars show the means ± s.e.m. F: #P < 0.05, ###P < 0.005 vs. culture of PBMNCs with DPSCs in the absence of inhibitors and antibodies.
Next, we examined the effects of TNF-α and IFN-γ on the immunosuppressive functions of IP-DPSCs under co-culture with ConA-stimulated PBMNCs. RT-qPCR analysis and L-kynurenine production assay demonstrated that IFN-γ enhanced IDO mRNA expression and L-kynurenine production in IP-DPSCs co-cultured with ConA-stimulated PBMNCs, whereas TNF-α did not (Fig. 6d,e). Similarly, ELISA showed that IFN-γ induced IL-10 production, whereas TNF-α did not (Fig. 6f). We then co-cultured a greater number of IP-DPSCs with ConA-stimulated PBMNCs under treatment with TNF-α and IFN-γ. The cell viability of the PBMNCs was markedly suppressed when the IP-DPSCs were under treatment with TNF-α or IFN-γ (Fig. 6g). IFN-γ-mediated suppression was more effective than TNF-α-mediated inhibition (Fig. 6g). PBMNC suppression through TNF-α- and IFN-γ-stimulated IP-DPSCs was significantly inhibited by 1-MT and anti-IL-10 antibody treatments (Fig. 6g). These findings suggested that IFN-γ treatment may restore the impaired immunoregulatory function of IP-DPSCs.
We then investigated the time-dependent expressional change of nuclear factor kappa-light-chain-enhancer of activated B cells (NF-κB) in IP-DPSCs after TNF-α and IFN-γ treatment. TNF-α-treated IP-DPSCs expressed enhanced phosphorylation of NF-κB, whereas IFN-γ-treated and non-treated IP-DPSCs did not (Fig. 6h). We also examined the effects of TNF-α and IFN-γ on telomerase activity in IP-DSPCs. TNF-α markedly reduced the telomerase activity of IP-DPSCs (Fig. 6i). In comparison, IFN-γ significantly enhanced the telomerase activity of IP-DPSCs, when compared with non-treated IP-DPSCs (Fig. 6i).
Discussion
The present isolation approach reveals the existence of CFU-F clonal populations15 in human dental pulp tissues diagnosed with irreversible pulpitis. The isolated CFU-Fs also express multipotency and immunological features as MSCs. Moreover, the present sequential transplantation and single colony assays demonstrated that the isolated CFU-Fs express an in vivo dentin/pulp complex regeneration ability, self-renewal capacity and heterogeneity. Overall, these findings indicate that the present CFU-Fs isolated from irreversible pulpitis tissue display stem cell characteristics similar to MSCs and healthy DPSCs6,7,8. Furthermore, IP-DPSCs also demonstrated an immunosuppressive function similar to healthy DPSCs9. However, when compared with healthy DPSCs, the IP-DPSCs showed impaired colony-forming capacity, cell proliferation rate, multipotency, in vivo dentin regeneration and immunosuppressive functions.
Recent tissue engineering technology has shown that healthy DPSCs reconstruct a dentin/pulp-like structure on human dentin in a xenograft system using immunocompromised mice8,27. In dogs, autologous transplantation of DPSCs from freshly extracted teeth successively regenerates a vascularized dental pulp tissue in pulpectomized teeth28. The currently innovated preclinical grade of healthy human DPSCs combined with granulocyte colony-stimulating factor suggests that autologous healthy DPSC-based therapy may almost be ready for clinical application29,30. However, the opportunity to obtain healthy donor teeth is quietly limited at a general clinical situation. Therefore, IP-DPSCs isolated from diseased teeth might be a feasible source for dentin/pulp complex regeneration11,12. The present IFN-γ-mediated IP-DPSCs facilitated the regeneration of dysfunctional dentin/pulp and the immunosuppressive function of IP-DPSCs will aid in the development of autologous DPSC-based endodontic therapy.
Inflammatory pulp reactions including reversible and irreversible pulpitis are carried out by several etiologies/stimuli5. Human dental pulp tissue with irreversible pulpitis expresses high levels of TNF-α and IFN-γ4. Major inflammatory helper T cell cytokines, TNF-α and IFN-γ, have been known to affect the immunomodulatory and dentinogenic functions of healthy DPSCs9,13,31,32,33,34. However, the effects of TNF-α and IFN-γ on the immunomodulatory and dentinogenic capabilities of IP-DSPCs have not yet been clarified. Recent studies of short-term TNF-α exposure-enhanced dentinogenic activity in healthy DPSCs suggest that reparative dentin formation occurs in response to reversible pulpitis32,35,36. Meanwhile, prolonged and heavy exposure of TNF-α diminishes the mineralization potential of IP-DPSCs and healthy DPSCs13,37. In comparison, IFN-γ accelerates the osteoblastic differentiation of human MSCs in vitro and in vivo38. IFN-γ-treated bone marrow-derived mesenchymal stem cells (BMMSCs) and DPSCs also accelerated IDO production to enhance the suppressive effect on T cell proliferation9,39,40. The present IFN-γ treatment successfully recovered the dysfunction of IP-DPSC-mediated dentin regeneration in vitro and in vivo and the suppression of T cells via IDO, whereas TNF-α treatment did not. These data suggest that exogenous IFN-γ treatment to IP-DPSCs is a novel approach to improve its ability of dentin/pulp complex regeneration and immunosuppression.
BMMSCs derived from patients with systemic lupus erythematosus, which have impaired bone forming potential, express enhanced phosphorylation of NF-κB under accelerated TNF-α signaling41. The inhibition of NF-κB activation induces the osteogenic capacity of normal BMMSCs42. In healthy DPSCs, suppression of activated NF-κB also enhances odontogenic ability under TNF-α stimulation31,43. In the present study, TNF-α treatment caused NF-κB activation with improved dentin/pulp complex regeneration and T cell immunosuppression in IP-DPSCs13,14. On the other hand, IFN-γ treatment enhanced the ability for IP-DPSCs by activation of NF-κB independently. These findings suggest that a practical control for NF-κB activation may enable regulation of the impaired functions of IP-DPSCs, including dentin/pulp regeneration and T cell immunosuppression.
The ectopic human telomerase reverse transcriptase (TERT) gene in human BMMSCs induces bone formation in vitro and in vivo by enhancing a critical master transcription factor for osteoblast differentiation, Runx244,45. TERT modulates FasL expression on BMMSCs to induce T cell apoptosis46. Recently, the non-steroidal anti-inflammatory drug aspirin (acetylsalicylic acid) has been shown to enhance telomerase activity and stimulate bone formation in vitro and in vivo as well as induce T cell apoptosis in BMMSCs and stem cells derived from human deciduous teeth25,47,48. In this study, IFN-γ-treated telomerase activity in IP-DPSCs facilitated in vitro and in vivo dentin formation and T cell suppression, whereas TNF-α treatment in IP-DPSCs did not. Therefore, regulation of telomerase activity in IP-DPSCs may accelerate their impaired dentin/pulp regeneration and immunosuppressive functions.
In conclusion, the present findings indicated that IFN-γ treatment improved the impaired IP-DPSC functions of dentin/pulp regeneration and immunosuppressive regulation. These effects were modified by telomerase activity, but independent of the NF-κB pathway. This functional gain study of disease-derived DPSCs may contribute to achieving not only autologous stem cell-approached pulp tissue engineering, but also to develop novel pulp-capping agents targeted to recipient diseased stem cells in future endodontic therapy (Supplementary Figure 7).
Methods
Ethics statement and human participants
All human samples were obtained as discarded biological/clinical samples from systemically healthy donors (19–25 years old) in Kyushu University Hospital. Extracted dental pulp tissue (n = 4) from permanent teeth that were diagnosed with irreversible pulpitis was aseptically collected under pulpectomy. Healthy pulp tissue (n = 3) was obtained from participants with healthy impacted third molars (19–23 years old). Human PBMNCs were provided by healthy volunteers (26–38 years old). The procedures for using human samples were conducted in accordance with the Declaration of Helsinki and approved by the Kyushu University Institutional Review Board for Human Genome/Gene Research (Protocol Number: 393-01). Written informed consent was obtained from all subjects. All experimental protocols were approved by the Institutional Animal Care and Use Committee of Kyushu University (Protocol Number: A21-044-1). The methods were carried out in accordance with the approved guidelines.
Mice
BALB/cAJcl-nu/nu mice (female, 7–10 weeks old) were purchased from CLEA Japan (Tokyo, Japan) and used under an institutionally approved animal research protocol (Kyushu University protocol #A21-044-1).
Histology of dental pulp tissue of human teeth diagnosed with irreversible pulpitis
Histological analysis with hematoxylin and eosin (H&E) staining and immunohistochemistry for human dental pulp tissue was performed as described in Supplementary Methods49. Mouse anti-STRO-1 IgM antibody (R&D Systems, Minneapolis, MN, USA) and non-immune mouse IgM (R&D Systems) were used for immunohistochemical analysis.
Isolation and culture of DPSCs
Stem cells from the dental pulp tissue of human permanent teeth were isolated as described in Supplementary Methods7,50. Briefly, the dental pulp tissue was digested with 0.3% collagenase type I (Worthington Biochemicals, Lakewood, NJ, USA) and 0.4% dispase II (Sanko Junyaku, Tokyo, Japan) for 60 min at 37 °C. The single cells obtained were seeded. After 3 hours, the cultures were washed and cultured with a regular medium consisting of 15% fetal bovine serum (Equitech-Bio, Kerrville, TX, USA), 100 μM L-ascorbic acid 2-phosphate (Wako Pure Chemicals, Osaka, Japan), 2 mM L-glutamine (Nacalai Tesque, Kyoto, Japan) and antibiotics containing 100 U/ml penicillin and 100 μg/ml streptomycin (Nacalai Tesque) in Alpha Modification of Eagle’s Medium (Invitrogen, Waltham, MA, USA). After forming well-attached colonies, the cells were passed for expansion.
CFU-F assay
The CFU-F assay was analyzed as described in Supplementary Methods49,50,51.
Immunophenotype analysis
Cell surface antigens of IP-DPSCs and healthy DPSCs were assayed by flow cytometric analysis according to Supplementary Methods49,50,51. All primary antibodies are summarized in Supplementary Table 1.
Population-doubling and BrdU incorporation assays
Population-doubling and BrdU incorporation assays were performed as described in Supplementary Methods49,50,51.
Telomerase activity assay
Telomerase activity was measured by a telomere repeat amplification protocol (TRAP) assay using a quantitative telomerase detection kit (Allied Biotech, Ijamsville, MD, USA) with RT-qPCR as described in Supplementary Methods49,50,51.
In vitro multidifferentiation capacity assay
Assays for multipotency into odontoblasts/osteoblasts, adipocytes, endothelial cells and neural cells were performed as described in Supplementary Methods49,50.
Assays for in vivo dentinogenic ability and self-renewal capacity
To analyze in vivo dentinogenic capacity, the cells were implanted subcutaneously with HA/TCP ceramic powders (40 mg, Zimmer Inc., Warsaw, IN, USA) into BALB/cAJcl-nu/nu mice as described in Supplementary Methods49,50,51,52 (Supplementary Figure 2). Eight weeks after the surgery, the implants were analyzed histologically. For self-renewal assay, the cells were sequentially transplanted as described in Supplementary Methods49,50 (Supplementary Figure 2).
In vivo dentin regeneration on human dentin
In vivo dentin regeneration on human dentin was performed as described in Supplementary Methods8 (Supplementary Figure 6).
Histological assay for implant tissue
Harvested implant tissue was treated for histochemical, immunohistochemical and immunofluorescent assays as described in Supplementary Methods49,50,51. The newly formed mineralized tissue area in each field was measured and shown as a percentage of the total tissue area44,52.
Single colony-derived cell assay
Single colony-derived cells were assayed by population-doubling, BrdU incorporation and in vitro dentinogenesis as described in Supplementary Methods19,49,50.
Treatment with IFN-γ and TNF-α
IP-DPSCs were stimulated with IFN-γ (100 ng/ml; PeproTech, Rocky Hill, NJ, USA) or TNF-α (100 ng/ml; PeproTech) at 37 °C for 0, 30, 60 and 120 minutes before analyzing an expression of NF-κB and its phosphorylated NF-κB under a serum-depleted condition. IP-DPSCs were pretreated with either cytokine at 37 °C for 24 hours before the transplant experiments under a serum-added condition.
Gene expression assay
Semi-quantitative RT-PCR and RT-qPCR assays were performed as described in Supplementary Methods53,54. The specific primer pairs and TaqMan probes (Applied Biosystems, Foster City, CA, USA) are summarized in Supplementary Tables 2 and 3.
PBMNC viability assay
Cell viability of PBMNCs under co-culture with IP-DPSCs or healthy DPSCs was performed as described in Supplementary Methods9,24 (Supplementary Figure 5a). Some PBMNCs were stimulated with ConA (10 μg/ml; Sigma-Aldrich, St. Louis, MO, USA). IP-DPSCs and healthy DPSCs were also pretreated with inhibitors for COX, NOS, IDO, indomethacin (20 μM; Sigma-Aldrich), L-NAME (1 mM; Sigma-Aldrich) and 1-MT (500 μM; Sigma-Aldrich), as well as antibodies neutralized to human IL-10 (10 μg/ml; R&D Systems), human TGF-β1 (10 μg/ml; R&D Systems), or an isotype-matched monoclonal antibody (10 μg/ml; R&D Systems). The collected CM was used for L-kynurenine and IL-10 measurements.
IDO activity assay
IDO activity was analyzed by measuring L-kynurenine in CMs of IP-DPSCs or healthy DPSCs co-cultured with ConA-activated PBMNCs according to a previous study9.
IL-10 measurement
Human IL-10 in culture supernatant was analyzed by ELISA in fresh co-culture CMs of IP-DPSCs or healthy DPSCs with ConA-activated PBMNCs using the Human IL-10 Quantikine ELISA kit (R&D Systems) according to the manufacturer’s instructions.
Apoptosis assay
T cell-mediated apoptosis assay in IP-DPSCs and healthy DPSCs was performed as described in Supplementary Methods25,26,51 (Supplementary Figure 5b). IP-DPSC and healthy DPSCs was also treated with anti-FasL antibody (1 μg/mL; eBioscience, San Diego, CA, USA). Apoptosis was assayed by toluidine blue staining and the TUNEL method.
Western blot analysis
Western blot analysis was performed as described in Supplementary Methods51,52. The primary antibodies used in this assay were NF-κB p65 (Cell Signaling Technology, Danvers, MA, USA), phosphorylated NF-κB p65 (Cell Signaling Technology) and β-actin (Sigma-Aldrich).
Statistical analysis
All data are expressed as the mean ± s.e.m. of, at least, triplicate determinations. Comparisons between two groups were analyzed by independent two-tailed Student’s t-tests. Multi-group comparisons were analyzed by one-way repeated measures analysis of variance followed by Tukey’s post hoc test. P-values less than 0.05 were considered statistically significant.
Additional Information
How to cite this article: Sonoda, S. et al. Interferon-gamma improves impaired dentinogenic and immunosuppressive functions of irreversible pulpitis-derived human dental pulp stem cells. Sci. Rep. 6, 19286; doi: 10.1038/srep19286 (2016).
References
Murray, P. E. et al. Postoperative pulpal and repair responses. J. Am. Dent. Assoc. 131, 321–329 (2000).
About, I., Murray, P. E., Franquin, J. C., Remusat, M. & Smith, A. J. Pulpal inflammatory responses following non-carious class V restorations. Oper. Dent. 26, 336–342 (2001).
Pezelj-Ribaric, S., Anic, I., Brekalo, I., Miletic, I. & Hasan, M. Detection of tumor necrosis factor-α in normal and inflamed human dental pulps. Arch. Med. Res. 33, 482–484 (2002).
Elsalhy, M., Azizieh, F. & Raghupathy, R. Cytokines as diagnostic markers of pulpal inflammation. Int. Endod. J. 46, 573–580 (2013).
Torabinejad, M., Fouad, A. & Walton, R. E. Endodontics: Principles and Practice. 5th Edition [ Torabinejad M, Fouad A, Walton RE (ed)] (Saunders, Amsterdam, Netherlands, 2014)
Gronthos, S., Mancani, M., Brahim, J., Robey, P. G. & Shi, S. Postnatal human dental pulp stem cells (DPSCs) in vitro and in vivo. Proc. Natl. Acad. Sci. USA 97, 13625–13630 (2000).
Gronthos, S. et al. Stem cell properties of human dental pulp stem cells. J. Dent. Res. 81, 531–535 (2002).
Batouli, S. et al. Comparison of stem-cell-mediated osteogenesis and dentinogenesis. J. Dent. Res. 82, 976–981 (2003).
Wada, N., Menicanin, D., Shi, S., Bartold, PM. & Gronthos, S. Immunomodulatory properties of human periodontal ligament stem cells. J. Cell Physiol. 219, 667–676 (2009).
Sonoda, S., Tomoda, E., Tanaka, Y. & Yamaza, T. Properties and possibilities of human dental pulp-derived stem cells. Arch. Stem Cell. Res. 2, 1012 (2015).
Alongi, D. J. et al. Stem/progenitor cells from inflamed human dental pulp retain tissue regeneration potential. Regen. Med. 5, 617–631 (2010).
Pereira, L. O. et al. Comparison of stem cell properties of cells isolated from normal and inflamed dental pulps. Int. Endod. J. 45, 1080–1090 (2012).
Boyle, M. et al. Chronic inflammation and angiogenic signaling axis impairs differentiation of dental-pulp stem cells. PLOS One 9, e113419 (2014).
Yazid, F. B., Gnanasegaran, N., Kunasekaran, W., Govindasamy, V. & Musa, S. Comparison of immunodulatory properties of dental pulp stem cells derived from healthy and inflamed teeth. Clin. Oral Invest. 18, 2103–2112 (2014).
Friedenstein AJ. Stromal mechanisms of bone marrow: cloning in vitro and retransplantation in vivo. Haematol. Blood Transfus. 25, 19–29 (1980).
Shi, S. & Gronthos, S. Perivascular Niche of Postnatal Mesenchymal Stem Cells Identified in Human Bone Marrow and Dental Pulp. J. Bone Miner. Res. 18, 696–704 (2003).
Morrison, S. J., Prowse, K. R., Ho, P. & Weissman, I. L. Telomerase activity in hematopoietic cells is associated with self-renewal potential. Immunity 5, 207–216 (1996).
Gronthos, S. et al. Differential cell surface expression of the STRO-1 and alkaline phosphatase antigens on discrete developmental stages in primary cultures of human bone cells. J. Bone Miner. Res. 14, 47–56 (1999).
Gronthos, S. et al. Molecular and cellular characterization of highly purified stromal stem cells derived from human bone marrow. J. Cell Sci. 116, 1827–1835 (2003).
Akiyama K. et al. Mesenchymal-stem-cell-induced immunoregulation involves FAS-ligand-/FAS-mediated T cell apoptosis. Cell Stem Cell 10, 544–555 (2012).
Di Nicola, M. et al. Human bone marrow stromal cells suppress T-lymphocyte proliferation induced by cellular or nonspecific mitogenic stimuli. Blood 99, 3838–3843 (2002).
Meisel, R. et al. Human bone marrow stromal cells inhibit allogeneic T-cell responses by indoleamine, 3-dioxygenase-mediated tryptophan degradation. Blood 103:4619–4621 (2004).
Jones, B. J., Brooke, G., Atkinson, K. & McTaggart, S. J. Immunosuppression by placental indoleamine 2,3-dioxygenase: A role for mesenchymal stem cells. Placenta 28, 1174–1181 (2007).
Ren, G. et al. Mesenchymal stem cell-mediated immunosuppression occurs via concerted action of chemokines and nitric oxide. Cell Stem Cell 2, 141–150 (2008).
Yamaza, T. et al. Pharmacologic stem cell based intervention as a new approach to osteoporosis treatment in rodents. PLOS One 3, e2615 (2008).
Yamaza, T. et al. Mouse mandible contains distinctive mesenchymal stem cells. J. Dent. Res. 90, 317–324 (2011).
Huang, GT-J. et al. Stem/progeny cell-mediated de novo regeneration of dental pulp with newly deposited continuous layer of dentin in an in vivo model. Tissue Eng. Part A 16, 605–615 (2010).
Iohara, K. et al. Regeneration of dental pulp after pulpotomy by transplantation of CD31(-)/CD146(-) side population cells from a canine tooth. Regen. Med. 24, 377–385 (2009).
Murakami, M. et al. The use of granulocyte-colony stimulating factor induced mobilization for isolation of dental pulp stem cells with high regenerative potential. Biomaterials 34, 9036–9047 (2013).
Nakashima, M. & Iohara, K. Mobilized dental pulp stem cells for pulp regeneration: initiation of clinical trial. J. Endod. 40, S26–32 (2014).
Chang, J., Zhang, C., Tani-Ishii, N., Shi, S. & Wang, C. Y. NF-kappaB activation in human dental pulp stem cells by TNF and LPS. J. Dent. Res. 84, 994–998 (2005).
Paula-Silva, F. W., Ghosh, A., Silva, L. A. & Kapila, Y. L. TNF-alpha promotes an odontoblastic phenotype in dental pulp cells. J. Dent. Res. 88, 339–344 (2009).
Demircan, P. C. et al. Immunoregulatory effects of human dental pulp-derived stem cells on T cells: comparison of transwell co-culture and mixed lymphocyte reaction systems. Cytotherapy 13, 1205–1220 (2011).
Takegawa, D. et al. Modulatory roles of interferon-γ through indoleamine 2, 3-dioxygenase induction in innate immune response of dental pulp cells. J. Endod. 40, 1382–1387 (2014).
Feng, X. et al. TNF-α triggers osteogenic differentiation of human dental pulp stem cells via the NF-κB signaling pathway. Cell Biol. Int. 37, 1267–1275 (2013).
Ueda, M. et al. A short-term treatment with tumor necrosis factor-alpha enhances stem cell phenotype of human dental pulp cells. Stem Cell Res. Ther. 5, 31 (2014).
Qin, Z. et al. High dose of TNF-α suppressed osteogenic differentiation of human dental pulp stem cells by activating the Wnt/β-catenin signaling. J. Mol. Histol. 46, 409–420 (2015).
Duque, G. et al. Autocrine regulation of interferon gamma in mesenchymal stem cells plays a role in early osteoblastogenesis. Stem Cells 27, 550–558 (2009).
Krampera, M. et al. Role for interferon-gamma in the immunomodulatory activity of human bone marrow mesenchymal stem cells. Stem Cells 24, 386–398 (2006).
English, K., Barry, F. P., Field-Corbett, C. P. & Mahon, B. P. IFN-gamma and TNF-alpha differentially regulate immunomodulation by murine mesenchymal stem cells. Immunol. Lett. 110, 91–100 (2007).
Tang, Y. et al. Activated NF-κB in bone marrow mesenchymal stem cells from systemic lupus erythematosus patients inhibits osteogenic differentiation through downregulating smad signaling. Stem Cells Dev. 22, 668–678 (2013).
Chang, J. et al. NF-κB inhibits osteogenic differentiation of mesenchymal stem cells by promoting β-catenin degradation. Proc. Natl. Acad. Sci. USA 110, 9469–9474 (2013).
Hozhabri, N. S. T. et al. Decreasing NF-κB expression enhances odontoblastic differentiation and collagen expression in dental pulp stem cells exposed to inflammatory cytokines. PLOS One 10, e0113334 (2015).
Shi, S. et al. Bone formation by human postnatal bone marrow stromal stem cells is enhanced by telomerase expression. Nat. Biotechnol. 20, 587–591 (2002).
Gronthos, S., Chen, S., Wang, C. Y., Robey, R. B. & Shi, S. Telomerase Accelerates Osteogenesis of Bone Marrow Stromal Stem Cells by Upregulation of CBFA1, Osterix and Osteocalcin. J. Bone Miner. Res. 18, 716–722 (2003).
Chen, C. et al. Telomerase governs immunomodulatory properties of mesenchymal stem cells by regulating FAS ligand expression. EMBO Mol. Med. 6, 322–334 (2014).
Liu, Y. et al. Mesenchymal stem cell-based tissue regeneration is governed by recipient T lymphocytes via IFN-γ and TNF-α. Nat. Med. 17, 1594–1601 (2011).
Liu, Y. et al. Acetylsalicylic Acid Treatment Improves Differentiation and Immunomodulation of SHED. J. Dent. Res. 94, 209–218 (2015).
Ma, L. et al. Cryopreserved dental pulp tissues of exfoliated deciduous teeth is a feasible stem cell resource for regenerative medicine. PLOS One 7, e51777 (2012).
Makino, Y. et al. Immune therapeutic potential of stem cells from human supernumerary teeth. J. Dent. Res. 92, 609–615 (2013).
Yamaza, T. et al. Immunomodulatory properties of stem cells from human exfoliated deciduous teeth. Stem Cell Res. Ther. 1, 5 (2010).
Yamaza, T. et al. Mesenchymal stem cell-mediated ectopic hematopoiesis alleviates aging-related phenotype in immunocompromised mice. Blood 113, 2595–2604 (2009).
Ma, L. et al. Transplantation of mesenchymal stem cells ameliorates secondary osteoporosis through interleukin-17-impaired functions of recipient bone marrow mesenchymal stem cells in MRL/lpr mice. Stem Cell Res. Ther. 6, 104 (2015).
Yamaza, T., et al. In vivo hepatogenic capacity and therapeutic potential of stem cells from human exfoliated deciduous teeth in liver fibrosis in mice. Stem Cell Res. Ther. 6, 171 (2015).
Acknowledgements
We are very thankful to Drs. Keitaro F. Masuda, Yusuke Makino and Yoshihiro Hoshino (Kyushu University Hospital) for their technical support in this study. We also thank Ms. Megumi Ogawa (Department of Molecular Cell Biology and Oral Anatomy, Kyushu University) for her excellent assistance in this study. We are also thankful to Edanz Group Japan (Fukuoka, Japan) for their English language editing service to our manuscript. This work was supported by grants from the Japan Society for the Promotion of Science, including Grants-in-Aid for Scientific Research (B) (Grant Number 25293405 to TY) and Scientific Research (C) (Grant Number 25463187 to HY), Grant-in-Aid for Challenging Exploratory Research Project (Grant Number 24659815 to TY) and the Program for Advancing Strategic International Networks to Accelerate the Circulation of Talented Researchers (Grant Number S2605 to FN).
Author information
Authors and Affiliations
Contributions
Soi. S. generation, collection, assembly and interpretation of data and statistical analysis. L.M., H.Y., Y.T., E.T. and R.A. collection and assembly of data and statistical analysis. K.N., T.K., Son. S. and F.N. interpretation of data and study supervision. T.Y. study conception and design, manuscript drafting, critical revision of the manuscript for important intellectual content and study supervision. All of the authors approved the final version of the manuscript.
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Electronic supplementary material
Rights and permissions
This work is licensed under a Creative Commons Attribution 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/
About this article
Cite this article
Sonoda, S., Yamaza, H., Ma, L. et al. Interferon-gamma improves impaired dentinogenic and immunosuppressive functions of irreversible pulpitis-derived human dental pulp stem cells. Sci Rep 6, 19286 (2016). https://doi.org/10.1038/srep19286
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/srep19286
This article is cited by
-
Superior protective effects of PGE2 priming mesenchymal stem cells against LPS-induced acute lung injury (ALI) through macrophage immunomodulation
Stem Cell Research & Therapy (2023)
-
Oral cavity-derived stem cells and preclinical models of jaw-bone defects for bone tissue engineering
Stem Cell Research & Therapy (2023)
-
Stem cell-based bone and dental regeneration: a view of microenvironmental modulation
International Journal of Oral Science (2019)
-
Comparison of immunomodulatory properties of exosomes derived from bone marrow mesenchymal stem cells and dental pulp stem cells
Immunologic Research (2019)
-
Pamidronate decreases bilirubin-impaired cell death and improves dentinogenic dysfunction of stem cells from human deciduous teeth
Stem Cell Research & Therapy (2018)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.